Abstracts
OBJECTIVE: The avoidance of pressure ulcers development in critically ill patients is a major nursing challenge. Prevention is thus relevant for assurance of high quality care. This study aimed to evaluate the applicability of the Braden scale in intensive care unit patients. METHODS: This was a prospective study based which evaluated all adult patients staying in the intensive care unit from July 14 to August 10, 2009. The data were collected using the Braden's scale by three examiners who identified the pressure ulcer development risk. The data were analyzed using the SAS Statistical Software. For determination of the examiners' rates degree of coincidence, the Kappa value was used (95%CI). RESULTS: Regarding the related risk factors: 36.4% had mild sensory perception impairment; 50.9% had occasionally moist skin; 97.3% bedfast; 39.1% had very limited mobility; 45% probably had inappropriate nutrition; 61.8% had friction and shear problems. An agreement between the examiners was identified for nutrition and physical activity (38.1% to 100.0%); the Kappa population zero hypothesis was rejected; a paired examiners agreement (41.7% to 100.0%) was identified for the items humidity and physical activity, and the Kappa values ranged from 0.13 to 1. CONCLUSIONS: These intensive care patients were identified to have increased risk of developing pressure ulcers. This tool was considered appropriate to support the implementation of preventive measures.
Validation studies; Protocols; Pressure ulcers; Pressure ulcers; Pressure ulcer; Intensive care
OBJETIVO: O não desenvolvimento da úlcera de pressão de pacientes graves em terapia intensiva é um grande desafio para a enfermagem. Portanto, é relevante a prevenção para que se garanta um cuidado de boa qualidade. O objetivo da pesquisa foi avaliar a aplicabilidade da escala de Braden em pacientes de terapia intensiva. MÉTODOS: Estudo prospectivo baseado na avaliação de todos os pacientes internados na unidade de terapia intensiva adulto, no período 14 de Julho a 10 de Agosto de 2009. A coleta de dados foi realizada através da aplicação da escala de Braden por três juízes, identificando os riscos para o desenvolvimento da úlcera de pressão. Para a análise dos dados foi utilizado o Software estatístico SAS Na avaliação do grau de coincidência entre os juízes utilizou-se valor kappa (IC=95%). RESULTADOS: Quanto aos fatores de risco relacionados: 36,4% apresentavam leve limitação à percepção sensorial, 50,9% pele ocasionalmente úmida; 97,3% restritos ao leito; 39,1% muito limitados à mobilidade, 45% nutrição provavelmente inadequada, 61,8% apresentaram problema quanto à fricção e cisalhamento. Quanto à concordância entre os juízes (38,1% a 100,0%) foram registradas em nutrição e atividade física; a hipótese do Kappa populacional nulo foi rejeitada; análise entre pares de examinadores de coincidência (41,7% a 100,0%) foi registrada no item umidade e atividade física, os valores de Kappa variaram de 0,13 a 1. CONCLUSÕES: Observou-se elevado risco para ulcera de pressão em pacientes de terapia intensiva. Esse instrumento parece ser adequado para auxiliar na implementação de medidas de prevenção.
Estudos de validação; Protocolos; Úlcera de pressão; Úlcera de pressão; Úlcera de pressão; Terapia intensiva
ORIGINAL ARTICLE
IResident Nurse in Intensive Care of Hospital da Restauração da Secretaria Estadual de Saúde, Recife (PE), Brazil
IINurse of the Intensive Care Unit of Hospital da Restauração da Secretaria Estadual de Saúde - Recife (PE), Brazil
IIIMSc, Vice-Director of Faculdade de Enfermagem Nossa Senhora das Graças FENSG UPE, Recife (PE), Brazil
Author for correspondence
ABSTRACT
OBJECTIVE: The avoidance of pressure ulcers development in critically ill patients is a major nursing challenge. Prevention is thus relevant for assurance of high quality care. This study aimed to evaluate the applicability of the Braden scale in intensive care unit patients.
METHODS: This was a prospective study based which evaluated all adult patients staying in the intensive care unit from July 14 to August 10, 2009. The data were collected using the Braden's scale by three examiners who identified the pressure ulcer development risk. The data were analyzed using the SAS Statistical Software. For determination of the examiners' rates degree of coincidence, the Kappa value was used (95%CI).
RESULTS: Regarding the related risk factors: 36.4% had mild sensory perception impairment; 50.9% had occasionally moist skin; 97.3% bedfast; 39.1% had very limited mobility; 45% probably had inappropriate nutrition; 61.8% had friction and shear problems. An agreement between the examiners was identified for nutrition and physical activity (38.1% to 100.0%); the Kappa population zero hypothesis was rejected; a paired examiners agreement (41.7% to 100.0%) was identified for the items humidity and physical activity, and the Kappa values ranged from 0.13 to 1.
CONCLUSIONS: These intensive care patients were identified to have increased risk of developing pressure ulcers. This tool was considered appropriate to support the implementation of preventive measures.
Keywords: Validation studies; Protocols; Pressure ulcers/prevention & control; Pressure ulcer/nursing; Intensive care
INTRODUCTION
Pressure ulcer (PU) in defined as any change in the skin integrity, due to not-relieved soft tissues compression between bony prominences and a hard surfaces,(1) and is a common complication in severely ill patients, causing and high impacts to the quality of life recovery.
PU development risk factors are: immobility, malnutrition, anemia, edema, drug vasoconstriction, consciousness level changes, incontinences and vasculopathies. Pressure ulcer leads to additional problems such as pain, suffering and increased morbidity and mortality, prolongs the time of stay in the hospital and increases the hospitalization expenditures.(2)
The job of intensive care unit (ICU) nursing is focused on the severely ill patient care and evaluation from a humanistic quality of life driven perspective including the condition diagnosis, interventions and specific nursing measures. Identification of patients in risk of developing PU depends not only on the professional's clinical ability, but also on measuring instruments, such as an evaluation scale which have appropriate predictive, sensitivity and specificity values.(1)
Aiming to provide additional support for constant professional care improvement and ability increase for PU risk evaluation and prevention, several authors have proposed measuring instruments or risk evaluation scales. The scales of Norton, Gosnell, Waterlow and Braden are the most frequently used in the Americas and Europe; these have different scope, complexity and use easiness.(3)
In Brazil, the Braden's scale was translated into Brazilian Portuguese and validated in 1999 according to the work by Paranhos and Santos, and is the best operationally defined, with a high predictive value of PU development, allowing the evaluation of several PU-related factors, and its use requires the evaluator to thoroughly evaluate the patient's condition.(1)
In this context, this study aimed to evaluate the Braden's scale applicability, considering that the instrument implementation by nurses can make possible best evaluation of pressure ulcers risk, which in turn may determine changes in the care measures and lower de novo cases incidence (Appendix 1).
METHODS
This was a transversal descriptive study developed in a Public Hospital's ICU located in Recife city (Brazilian Northeast) from July 14 to August 10, 2009. The data were collected using an ICU pressure ulcer prevention protocol (Appendix 2) based on the Braden's scale (Appendix 3). To verify the instrument reproducibility, it was decided to use three experienced professional examiner nurses as judges, evaluating the instrument's content, presentation, clarity and understanding.
The completed forms were identified with the characters A, B or C, in order to differentiate among the evaluators. The assessment was made in a two-day pre-established routine, always by the same time (by the morning, at the bath time) when the examiners applied the protocol simultaneously but individually, so the results could be as reliable as possible. The examiners had no access to each other evaluation. A 70% value was established for reliability determination, to allow its evaluation by an agreement analysis.
In the data analysis were calculated the absolute distributions, percents and the statistical measurements: mean, median, standard deviation, variation coefficient (minimal and maximal values), the Kappa value for evaluation of the degree of agreement between the examiners (descriptive statistics techniques) and inferential statistics for the Kappa value confidence interval determination. By means of this, it was possible to check the hypothesis that the population Kappa would be or not equal to zero. This test is useful to check if two examiners' evaluations are different. The Kappa score ranges between -1.0 and +1.0, and when it is equal to one this indicates a perfect agreement between the examiners and zero means random categorization or examiners' independence; the closer to 1, more coincidental are the evaluations, and the closer to -1, less coincidental. When this index is equal to -1.00, no evaluation is coincident.(4)
For the Kappa scores interpretation the following scale was suggested: < 0.20: poor; 0.21 0.40: weak; 0.41 0.60: moderate; 0.61 0.80: good; 0.81 0.99: excellent; 1.00: perfect. The significance level for the statistical tests was 5%. The data were entered in an Excel sheet and the SAS 8.0 software was used for the statistical calculations.
The data collection was only started after receiving the Institution's Ethics Committee approval, document number 071/08. Signature of an Informed Consent Form was also required, either by the patient or a family member, according to the Resolution 196/96 of the Brazilian National Health Council.
RESULTS
During the study period, 34 patients were admitted to the ICU, and 13 of them (38.24%) already had PU by the admission time, thus being excluded from the sample, leaving remainder 21 patients (61.76%). The table 1 shows that the predominant age was 51 years or more (38.1%); 42.9% patients were male, and 57.1% female. The studied patients were shown to have high (57.3%) and moderate risks (28.2%) of PU development, according to the Braden's scale PU risk evaluation (Table 2).
Regarding sensory perception of appropriate response to pressure-related discomfort, most of the patients were completely limited (29.0%) or slightly limited (36.4%). Most of the studied patients had occasionally (50.9%) or rarely (26.4%) moist skin. Regarding the degree of physical activity, most of the patients were bedfast (97.3%), as expected for an ICU patients' sample. Regarding mobility, most of the patients were very limited (39.1%) or completely immobile (34.6%). Probable inappropriate nutrition was seen for 45% of the patients. Regarding friction and shear, most needed moderate or maximum assistance to move (61.8%).
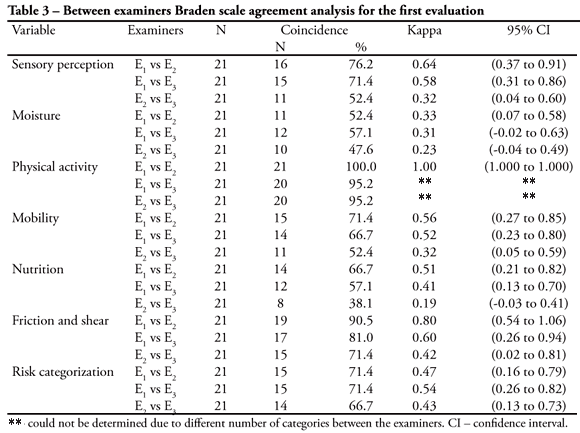
Among the 21 responses for each of the Braden's scale items, on each examiner's first evaluation, it was possible to identify a coincidences frequency ranging from 8 (38.1%) to 21 (100.0%). The most frequent coincidences were found for the "physical activity" item, with at least 20 coincidences and the less frequent coincidence was seen for the examiners 2 and 3 on the nutrition item. For the items where the Kappa could be calculated, the values ranged from 0.19 to 1.00. Except for an interval including the 0.00 value, for the remainder intervals the hypothesis of a null population Kappa was rejected for the adopted significance level (Table 3).
The table 4 shows the agreement results for the pairs of examiners, including the subsequent evaluations performed in 15 of the 21 patients, totalizing 36 evaluations. The coincidences frequency ranged from 15 (41.7%) to 36 (100.0%), being the higher frequency for physical activity, with at least 20 coincidences. The lower coincidence was between examiners 2 and 3 for moisture. The Kappa values for the items that could be determined ranged from 0.13 to 1.00. Except for an interval including the 0.00 value, for the remainder intervals the hypothesis of null population Kappa value was rejected.
DISCUSSION
The results show that the patients' age distribution was similar to the findings of Feijó,(5) who conducted a study in an University Hospital ICU in the Ceará state (Brazilian Northeast), with high prevalence of patients above 60 years old. Studies have shown that the skin becomes drier with age due to reduced number of sweat and sebaceous glands, and also hemodynamic changes and muscle atrophy rendering bony structures more prominent.(6)
Regarding the larger prevalence in females, demographic data have show that women live longer than men, and thus have longer chronic diseases courses. Additionally, there are differences in the attitudes towards diseases and physical incapacities. Women are generally more attentive to symptoms, know more about diseases and use more intensively the healthcare services than men. The early medical care is considered as one of the factors for best chronic diseases outcomes in women,(7) and this could explain the larger females proportion.
To evaluate the risk of developing PU in a given patient, the several predisposing factors should be taken into account. As highlighted by Fernandes,(8) "all aspects should be considered, since a pressure ulcer is not consequence of one single risk factor, but of the relationship between several risk factors and the patient", stressing the relevance of a validated risk-evaluation tool.
The lack of sensory perception leads these patients to require special attention, as they are frequently unable to communicate their discomfort and thus become more vulnerable to pressure ulcer development. The nurse should be able to diagnose this group of patients early, and to implement actions to reduce complications.
Skin moisture may be related to consciousness level changes and other peripheral nervous system complications. Among these, urinary and fecal incontinence and excessive perspiration are important, requiring serious healthcare team attention. Other factors also contributing to expose patients to moisture are secretions of drainage tubes, sores and food residues.(9) A direct connection was identified for PU and moisture, as prolonged moisture exposure may lead to skin maceration and rupture. Thus, the nursing team should be aware of secretions in the patient's bed, always making sure it is clean and dry.(10)
Regarding the degree of physical activity, the study shows that a large portion of the studied population was bedfast. This is concerning, as patients lying in bed are more prone to PU, and need special attention from the care team regarding decubitus change, skin care, bony prominences protection and special cushions use.(11)
The immobility is one of the most important risk factors for PU, due to the pressure on bony prominences areas, causing tissue destruction.(12) PU prevention is mainly dependent on the nursing team, caring 24 hours daily of the patient. Thus, appropriate decubitus change and bed positioning are indispensable.(13)
A deficient nutrition status is one of the main PU factors as leads to anemia and reduced tissue oxygen, contributing to reduce tissue tolerance to pressure. PU develop faster and is more treatment-resistant in poorly nourished patients. Malnutrition impairs the wounds healing, increases the subject's susceptibility to infection, and contributes to increased complications rate, longer hospitalizations and prolonged bed rest.(10) It is necessary that the nursing team realize their important role on malnourished patients identification, and also other known nutrition-associated aspects identification.(14)
Authors(9) indicate friction and shear as significant PU risk factors. Friction occurs when two surface forces glide against each other, with resulting abrasion and frequently blistering. Shear force is a consequence of inappropriate mobilization or positioning, and causes deeper tissues damage. This is seen when a patient is kept with raised bed head above 30 degrees, allowing the patient to slide down in the bed, injuring specially the sacrum and coccyx regions.(9) The nursing team should early identify and prevent these conditions and this makes continued education a daily practice ally.
Several studies have demonstrated that PU prevention is as important as risk identification. Thus, the creation of prevention scales and protocols appropriate to each risk level is relevant, as well as promoting its full implementation.
The tools should be simple, easy to use, and in order to be validated be objective-specific, in addition to outcomes anticipation. For PU risk patients' evaluation tools, its is proposed a frequent application in order to provide as early as possible interventions.
The examiners agreement test is used to assess the tool reliability. This reliability may be evaluated by the instrument's accuracy to measure its attribute. The smaller variation it produces on repeated measures, more reliable is the tool. A given tool is reliable when its measure accurately reflects the investigated attributes.
The accurate risk evaluation description, according to the Braden scale 6 subscales, depends on the observer's ability to recognize the patient's PU risks. The different knowledge level between different professionals developing this activity may lead to variable interpretations.
The protocol is based on the PU risk evaluation, using the Braden's scale, and its score define the measures to take (Appendix 4). Thus, a categorization system may look simple and easy for data acquisition, however inappropriate categorization may lead to unnecessary procedures.
In this study, the examiners had high levels of agreement, and showed similar categorizations; so, this protocol can be used to categorize the sores. The lowest coincidence frequency was seen between the examiners 2 and 3 for the items nutrition and moisture, showing requirement of specific training to qualify the nursing team for appropriate protocol implementation.
This simple measurement system was described by several authors as easy to perform, practical and affordable, although inaccurate. According to Santos,(15) some tools require for their application both training and time availability, in addition to the need of at least once a week continued evaluation. The PU categorization scales are deemed subject to biases due to the interpretation subjectivity, as well as the need of previous clinical knowledge, but this is also applicable for any evaluation tool.
The PU prevention protocol implementation has the meaning of a strategic decision to strengthen the care practices. This nurses leaded initiative may mean an institutional endeavor that includes several professional teams. Considering this PU prevention tool effectiveness and feasibility, the relevance of its insertion in the nursing prescription was demonstrated. However, the nurse's technical competence and clinical ability to evaluate the scale's items are indispensable for optimized care.
CONCLUSIONS
The PU risk evaluation with the Braden's scale evidenced that most of these ICU studied patients had high or moderate risk of developing PU. The Braden's scale-based items showed positive responses in the examiners evaluation. The population Kappa null hypothesis was rejected, suggesting that the tool was well interpreted and understood by the examiners in regard of its content, presentation and clearness, allowing the protocol to be safely used for appropriate diagnosis of PU risk patients.
REFERENCES
- 1. Menegon DB, Bercini RR, Brambila MI, Scola ML, Jansen MM, Tanaka RY. Implantação do protocolo assistencial de prevenção e tratamento de úlcera de pressão do Hospital de Clínicas de Porto Alegre. Rev Hosp Clin Porto Alegre. 2007;27(2):61-4.
- 2. D'Arco C, Sassine SW, Costa MLM, Silva LMG. Úlcera de pressão em UTI. In: Knobel E. Condutas no paciente grave. 3a. ed. São Paulo: Atheneu; 2006. Vol. 2. p. 2491-501.
- 3. Jorge SA, Dantas SRPE. Abordagem multiprofissional do tratamento de feridas. São Paulo: Atheneu; 2003.
- 4. Cohen J. A coefficient of agreement for nominal scales. Educ Psychol Meas. 1960;20:37-46.
- 5. Feijó CAR, Leite Júnior FO, Martins ACS, Furtado Júnior AH, Cruz LCS, Meneses FA. Gravidade dos pacientes admitidos à unidade de terapia intensiva de um hospital universitário brasileiro. Rev Bras Ter Intensiva. 2006;18(1):18-21.
-
6Universidade Estadual de Campinas. Hospital das Clínicas. Grupo de Estudos de Feridas. Tratamento de feridas. Campinas: UNICAMP; 1999.
- 7. Veras RP. Considerações acerca de um jovem país que envelhece. Cad Saúde Pública. 1988;4(4):382-97.
- 8. Fernandes LM. Úlcera de pressão em pacientes críticos hospitalizados: uma revisão integrativa da literatura [dissertação]. Ribeirão Preto: Escola de Enfermagem de Ribeirão Preto da Universidade de São Paulo; 2000.
- 9. Braden B, Bergstrom N. A conceptual schema for the study of the etiology of pressure sores. Rehabil Nurs. 1987;12(1):8-12.
- 10. Smeltzer SC, Bare BG. Brunner & Suddarth: tratado de enfermagem médico-cirúrgica. 10a. ed. Rio de Janeiro: Guanabara Koogan; 2005. vol. 1.
- 11. Aguiar JM, Paiva SS. Escala de Braden: avaliação dos fatores de risco para úlcera de pressão em pacientes internados em uma Unidade de Terapia Intensiva. Rev Hosp Univ UFMA. 2003;1(1/2):39-44.
- 12. Marin MJS, Pereira EACS, Paula MIR, Mesquita SRM, Laluna MC. Avaliando o risco para úlcera de pressão em uma população do município de Marília. Enferm Atual. 2002;2(7):28-33.
- 13. Silva EMP, Cruz ICF. Altered skin integrity as a nursing diagnosis ICU: literature review for an evidenced based nursing practice. J Spec Nurs Care. 2008;1(1).
- 14. Dreyer E, Brito S. Terapia nutricional. Cuidados de enfermagem: procedimentos padronizados para pacientes adultos. Campinas: Grupo de Apoio Nutricional; Equipe Multiprofissional de Terapia Nutricional do Hospital das Clínicas da UNICAMP; 2003.
- 15. Santos VLCG, Azevedo MAJ, Silva TS, Carvalho VMJ, Carvalho VF. Adaptação transcultural do Pressure Ulcer Scale for Healing (PUSH) para a língua portuguesa. Rev Latinoam Enferm. 2005;13(3):305-13.
- 16. Fernandes LM, Caliri MHL. Using the Braden and glasgow scales to predict pressure ulcer risk in patients hospitalized in Intensive Care Units. Revista Latinoam Enferm. 2008;16:973-8.
Applicability of a pressure ulcers protocol in intensive care unit
Publication Dates
-
Publication in this collection
05 Aug 2010 -
Date of issue
June 2010
History
-
Accepted
24 May 2010 -
Received
25 Feb 2010