Abstract
The goal of this study was to evaluate in vitro the effect of the photoinitiator phenylpropanedione (PPD), alone or combined with camphorquinone (CQ), on color stability of photoactivated resin cements and their bond strength to ceramics using a micro-shear test. Four resin cements were used: a commercial brand cement (RelyX Veneer®) and 3 experimental cements with different types and concentration of photoinitiators. For color analysis, ceramic discs were cemented on bovine dentin specimens to simulate indirect restorations (n=8) and were exposed to UV for 120 h and tested for color alteration using a reflectance spectrophotometer and the CIEL*a*b* system. Data were analyzed by Anova and Tukey’s test at 5% significance level. The color test results did not present statistically significant difference for the ∆E for all the studied cements, neither for ∆L, ∆a and ∆b. For the bond strength, all the studied cements showed statistically significant differences to each other, with the highest result for the RelyX Veneer® (29.07 MPa) cement, followed by the cement with CQ (21.74 MPa) and CQ+PPD (19.09 MPa) cement; the lowest result was obtained by the cement using only PPD as a photoinitiator (13.99 MPa). So, based on the studied parameters, PPD was not advantageous as photoinitiator of resin cements, because it showed a low value of bond strength to the ceramics and no superior color stability.
Key Words:
photoinitiator; cements; colors; bond strength
Resumo
O objetivo deste estudo foi avaliar in vitro o efeito do fotoiniciador fenilpropanodiona (PPD), isoladamente ou em associação com a CQ, sobre a estabilidade de cor de cimentos resinosos fotoativados e sua resistência de união adesiva à cerâmica, por teste de microcisalhamento. Foram utilizados 4 cimentos resinosos, sendo um comercial (RelyX Veneer®) e 3 experimentais, diferindo entre si quanto ao tipo e concentração dos fotoiniciadores. Para a análise de cor foram cimentados discos cerâmicos sobre dentina bovina, simulando restaurações indiretas (n=8), sendo expostos a 120 h de UV e testados quanto às alterações de cor, que foram mensuradas empregando a escala CIEL*a*b*, por meio de espectrofotômetro de reflectância. Os dados obtidos foram verificados quanto à distribuição normal, submetidos a Anova e ao teste complementar Tukey, todos com significância de 5%. Os resultados do teste de cor não apresentam diferença estatisticamente significante para o ∆E dos 4 cimentos estudados, tampouco para ∆L, ∆a e ∆b. Para a resistência de união, todos os cimentos estudados apresentaram diferenças estatisticamente significantes entre si, com o maior resultado para o cimento comercial RelyX Veneer® (29,07 MPa), seguido pelo cimento com CQ (21,74 MPa), e cimento de CQ+PPD (19,09 MPa); o menor resultado foi obtido com o cimento utilizando apenas o PPD como fotoiniciador (13,99 MPa). Portanto, para os parâmetros estudados, o PDD não se mostrou vantajoso como fotoiniciador de cimentos resinosos, pois apresentou baixo valor de resistência de união à cerâmica e não demonstrou superioridade quanto à estabilidade de cor.
Introduction
Resin cements are fundamental steps of the indirect restoration procedure. Light-cured cements are commonly used for fixation of caps and ceramic veneers in anterior teeth, due to the relative ease for light passing through the ceramics, warranting good retention. Polymer conversion was shown to be unaffected by light curing through ceramic thickness up to 2 mm 11 Akgungor, G; Akkayan, B; Gaucher, H. Influence of ceramic thickness and polymerization mode of a resin luting agent on early bond strength and durability with a lithium disilicate-based ceramic system. J Prosthet Dent 2005;94:234-241..
Camphorquinone (CQ) is the most used photoinitiator in light-cured composed resins, but it has some disadvantages, like a low polymerization rate and toxicity 22 Chae K, H; Sun G, J. Phenylpropanedione;A new visible light photosensitizer for dental composite resin with higher efficiency than camphorquinone. Bull Korean Chem Soc 1998;19,152-154.. Furthermore, the CQ is a solid substance that contains in its molecular structure a yellow chromatic association, which even in small amounts may compromise the final aesthetic result of the restorations causing an undesirable yellow hue 33 Schneider, LFJ; Pfeifer, CS; Consani, S; Prahl, SA; Ferracane, JL. Influence of photoinitiator type on the rate of polymerization, degree of conversion, hardness and yellowing of dental resin composites. Dent Mater 2008;24:1169-1177..
Another problem is that the a-dicetone group, derivative from CQ, which has an absorption peak of visible light (468 nm), resulting in fast light curing under room light (fluorescent and reflector light bulbs), which results in a short working time 44 Lührs, AK; De Munck, J; Geurtsen, W; Van Meerbeek, B. Composite cements benefit from light-curing. Dent Mater 2014;30: 292-301..
In order to circumvent the undesirable effect of the yellowish color produced by CQ, enhancing its use in cleared or naturally clearer teeth and also to optimize the polymerization of these cements, substitution of camphorquinone (CQ) as a photoinitiator agent has been studied by alternative chemical compounds 55 Aguiar, TR; Francescantonio, MD; Arrais, CA; Ambrosano, GMB; Davanzo, C; Giannini, M. Influence of curing mode and time on degree of conversion of one conventional and two self-adhesive resin cements. Oper Dent 2010;35:295-299..
Phenylpropane (PPD) is a photoinitiator with potential to reduce yellowing problems of the dental resinous composites. It may act alone or in combination with CQ, characterizing a synergetic and simultaneous action on formation of free radicals, which could favor the performance of materials with resinous base 66 Park, YJ; Chae, KH; Rawls, HR. Development of a new photoinitiation system for dental light-cure composite resins. Dent Mater 1999;15:120-127., since the PPD presents maximum peak of absorption in the ultraviolet region (UV - 390 nm) 77 Schneider, LFJ; Cavalcante, LM; Consani, S; Ferracane, JL. Effect of co-initiator ratio on the polymer properties of experimental resin composites formulated with camphorquinone and phenyl-propanedione. Dent Mater 2009;25:369-375.. In this way, composites with PPD as initiator tend to reach the maximum values of polymerization slower than the ones with camphorquinone, because the rate and the speed of polymerization depend on the energy density absorbed by the composite 88 Oliveira, KM; Consani,S; Gonçalves, LS; Brandt, WC; Ccahuana-Vásquez, RA. Photoelastic evaluation of the effect of composite formulation on polymerization shrinkage stress. Braz Oral Res 2012, 26:202-208..
Inappropriate polymerization results in inferior physicomechanical properties, like low resistance to attrition, low color stability, adverse reaction of pulp tissue, increase in water sorption, solubility and consequently, secondary decay and premature failure of the restoration 99 Brandt, WC; Schneider, LFJ; Frollini, E; CorrerSobrinho, L; Sinhoreti, MAC. Effect of different photo-initiators and light curing units on degree of conversion of composites. Braz Oral Res2010;24:263-270..
However, little is known about the efficiency of the PPD on the reduction of yellowing and the influence on the bond strength of the composites, mainly because the performed studies with PPD were made in composite resin 77 Schneider, LFJ; Cavalcante, LM; Consani, S; Ferracane, JL. Effect of co-initiator ratio on the polymer properties of experimental resin composites formulated with camphorquinone and phenyl-propanedione. Dent Mater 2009;25:369-375.,1010 Segreto, DR; Naufel, FS; Brandt, WC; Guiraldo, RD; Correr, Sobrinho, L; Sinhoreti, MAC. Influence of photoinitiators and light sources on the degree of conversion of experimental resin cements. Braz Dent Sci 2015;18:65-72., without influence of PPD on resin cements.
Improved understanding of photoactivation and the resources of polymerization, color stability and the adhesive resistance of the resin cements tends to rise, favoring the clinical longevity of the procedure. Thus, it may be stated that the longevity of indirect restorations is determined by the resistance, color stability and bond durability formed by the three different components: dental substrate, resin cements and ceramics 1111 Peumans, M; Van Meerbeek ,B; Lambrechts, P; Vanherle, G. Porcelain veneers: a review of the literature. J Dent 2000;28:163-177..
Based on these considerations, it is appropriate to evaluate the PPD influence as a photoinitiator on the color stability of light-curing resin cements, on the cementation of laminated ceramics to bovine dentin and the bond strength of these cements to ceramics.
The goal of this study was to evaluate in vitro the effect of the phenylpropanedione (PPD) photoinitiator, alone or in combination with camphorquinone (CQ), on color stability of photoactivated resin cements and their bond strength to ceramics using a micro-shear test. The null hypotheses tested in this study were: i) the PPD photoinitiator does not influence the color alteration of resin cements after the aging caused by extended exposure to UV light and ii) the PPD photoinitiator does not interfere on the adhesive bond strength of the resin cements to ceramics.
Material and Methods
A batch of seventy bovine incisives free of cracks or any lesions were selected and stored frozen in a solution of Chloramine T at 5% in a conventional freezer at -4 ºC until use. To obtain the samples, the roots were sliced 1 mm below the cementoenamel junction with a #7020 double face diamond wheel (KG Sorensen, Cotia, SP, Brazil) adapted on a mandrel and a straight hand piece (Kavo, Joinville, SC, Brazil) under constant irrigation, discarding all the roots.
For enamel removal of the vestibular surface were used #240 dental polishing stripes until exposure of the dentin, and #600, to standardize the smear layer 1212 Heydecke, G; Zhang, F; Razzoog, ME. In vitro color stability of double-layer veneers after accelerated aging. J Prosthet Dent 2001;85:551-557., in a metallographic polishing machine (Aropol 2V; Arotec, Cotia, SP) under constant irrigation.
After the standardized dentin exposure, the dentin blocks (7x7x2) were obtained with the double face diamond wheel (Dia. Wafer Blade 12205, Extec Corp. Enfield, CT, USA) mounted on a water cooled low speed cutting machine (Labcut 1010, Extec). The standardized dimensions of the samples were measured by a digital pachymeter (Mytutoyo, Suzano, SP, Brazil).
The initial color of the dentin blocks was standardized for color analysis 1313 Oliveira, DCRSD; Souza, Júnior, EJ; Prieto LT; Coppini EK; Maia RR; Paulillo, LAMS. Color stability and polymerization behavior of direct esthetic restorations. J Esthet Rest Dent 2014;26:288-295. by a spectrophotometer (CM 700d; Konica Minolta), using a sample holder of white Teflon with a 7x7x2 mm central depression, which was later deepened to 7x7x3.4 mm, due to the thickness of the ceramics (1.4 mm). For color measurement the edge was positioned directly at the center of the sample. The spectrophotometer used the CIE L*a*b* scale of color as reference. For the measurement of color was used controlled illumination with a D65 light box (GTI MiniMatcher, Gti Grafic Tecnology Inc., Newburgh, NY, USA).
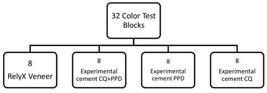
The color standardization of the dentin blocks was performed according to the L-values of the CIE L*a*b* system and the blocks with discrepant values (±10%) from the average were discarded. After the color standardization, were obtained 32 blocks of dentin with similar color, randomly assigned to the 4 experimental groups (n=8) (Fig. 1).
Thirty-two disks with ceramic glass reinforced by leucite (IPS Empress Esthetic/Ivoclar/Vivadent, Liechtenstein) were manufactured in ETC1 color, measuring 7 mm diameter and 1.4 thick 1010 Segreto, DR; Naufel, FS; Brandt, WC; Guiraldo, RD; Correr, Sobrinho, L; Sinhoreti, MAC. Influence of photoinitiators and light sources on the degree of conversion of experimental resin cements. Braz Dent Sci 2015;18:65-72.. Four resin cements were used, one of them the commercial Relyx Veener, 3M/ESPE, USA) with hexafluorophosphate diphenyl iodonium (DPIH) as photoinitiator, used as control group and 3 experimental cements developed at the FOP-UNICAMP Dent Mater Lab, with the formulations presented in Table 1.
Among the experimental cements, one had camphorquinone as photoinitiator (positive control). The experimental cements were made with a concentration pre-tested by previous studies of the same research team 1010 Segreto, DR; Naufel, FS; Brandt, WC; Guiraldo, RD; Correr, Sobrinho, L; Sinhoreti, MAC. Influence of photoinitiators and light sources on the degree of conversion of experimental resin cements. Braz Dent Sci 2015;18:65-72..
For cementation, the ceramic disks were conditioned by 10% hydrofluoric acid for 1 min, washed by water jet for 15 s and dried with oil-free air jet and water for 15 s. Next, they were treated with Silano Silano (Relyx Ceramic Primer - 3M/ESPE), applied with Microbrush® and volatilized for 1 min. Then was applied an adhesive system layer (Single Bond Universal, 3M/ESPE) with a Microbrush®, the solvent volatilized for 10 s. The dentin was conditioned with 37% phosphoric acid for 20 s, washed with air and water jet for 40 s and dried with absorbent paper. Next was applied an adhesive system layer with Microbrush®, dried with soft air jet for around 10 s to increase the solvent volatilization. The resin cement was applied on the already treated ceramic disc, positioned on the dentin block by uniform pressure, equivalent to the weight of a glass plate positioned on the ceramic disk and photoactivated for 60 s with LED curing light (Bluephase G2, Ivoclair).
After cementation, the specimens were stored in 100% relative humidity in a greenhouse at 37 ºC, for 24 h. Next was made the reading of initial color on all samples by a spectrophotometer (CM 700d, Konica Minolta), previously calibrated and controlled illumination with a D65 light box.
After reading the initial color, the samples were packed on the turnable of the photoaging machine at 10 cm distance from the lights 1414 De Oliveira DCRS; Rocha, MG; Gatti, A; Correr, AB; Ferracane, JL; Sinhoret, MAC. Effect of different photoinitiators and reducing agents on cure efficiency and color stability of resin-based composites using different LED wavelengths. J Dent 2015;43:1565-1572., to initiate the process of ultraviolet irradiation UV-b (EQ-UV-B 313, Equilam, Diadema, SP, Brazil), for 120 consecutive hours at 37 °C, which corresponds approximately to the photoaging of daily exposures to UV-b light at 37ºC for one year in the mouth 1515 Oliveira, DCRS; Ayres, APA; Rocha, MG; Giannini, M; Puppin Rontani, RM; Ferracane, JL; et al.. Effect of different in vitro aging methods on color stability of a dental resin-based composite using CIELAB and CIEDE2000 color-difference Formulas. J Esthet Rest Dent 2015;27:322-330.. After hydrated in 100% relative humidity at 37 ºC for 24 h, the final color reading was made, allowing to calculate the color variation (ΔE) and its coordinates (Δa, Δb e ΔL), and then the statistical analysis.
Bond Strength
Twenty-eight slices were made from lithium disilicate (E-Max CAD, Ivoclar/Vivadent, Liechtenstein), color HT A2, with 7x65x1.4 mm. These slices were cut with a double face diamond wheel (Dia. Wafer Blade 12205, Extec Corp.) mounted in a water cooled cutting machine at low speed (Labcut 1010, Extec Corp,),. The slices had their surfaces regularized with #600 tooth polishing strips (Extec Corp.) mounted in a polishing machine (Aropol 2V, Arotec, Cotia, SP) for 30 s, followed by cleaning in a ultrasonic vat with deionized water for 5 min, then sintered in a Programmat EP 3000 oven (Ivoclar/Vivadent, Liechtenstein) at 850 ºC for 25 min.
The same cements were used, with a similar protocol to the one used on the ceramic cementation for color analysis Therefore, the ceramic slices were conditioned with 5% hydrofluoric acid for 20 s, washed with a water jet for 40 s and dried with oil-free air jet and water for 20 s. Next, the silane (Relyx Ceramic Primer, 3M/ESPE)was applied with Microbrush® and volatilized for 1 min. The adhesive areas were delimited, with adhesive tape (Adere Tapefix, São Paulo, SP, Brazil) perforated with a smaller diameter of an Ainsworth perforator (Golgran, São Paulo, SP, Brazil.).
The adhesive application (Single Bond Universal, 3M/ESPE) was made with a Microbrush®. Before the adhesive photoactivation, cylindrical matrixes 1 mm high and 0.9 mm internal diameter were positioned perpendicularly to the ceramics, in a way that the matrix orifice coincided with the delimited adhesive area. The adhesive system was photoactivated for 40 s (Bluephase G2, Ivoclar). Then the matrixes were filled with the resin cements defined to each group, with syringes for insulin application (0,5 mL) and photoactivated for 1 min.
The matrix was removed by a #5 exploratory probe (Golgran) and the tape for adhesive delimitation was removed with a #15 scalpel blade 5, exposing the cement cylinders for the mechanical test.
The cement cylinders passed a visual evaluation with a magnifying glass with 4x magnification, in order to detect any problems that could influence the test results, like cylinders non-perpendicular to the ceramics, bubbles or cements out of the delimited area. All specimens with such problems were removed. After a 48-hour storage in deionized water at 37 ºC, the specimens were fixed in a PVC matrix with a self-curing acrylic resin for adaptation in a micro shear device adapted to an universal testing machine (Model 4411, Canton, MA, USA). The shearing load was applied with an orthodontic archwire (Morelli Ortodontia, Sorocaba, SP, Brazil), 0.1 mm thick, positioned exactly on the interface between the ceramic and the cement, at a 1 mm/min speed, until the adhesive rupture. The kgf values were converted to MP after measuring the adhesive area with a digital pachymeter (Starrett), according to the mathematical formula: Rs=F x 0.098/A where: Rs is the resistance to the shearing; F is the applied force in kgf and A is the union area in cm2.
Failure Mode
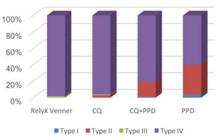
Failure mode after debonding was determined by a scanning electron microscope (LEO 435 VP; LEO Electron Microscopy Ltd., Cambridge, UK) at 100x magnification. The fractured surfaces were classified according to the prevailing remaining structure as Type I, adhesive; Type II, cohesive within cement; Type III, cohesive within dentin; or Type IV, mixed, involving at least two structures (ceramic, cement, bonding agent, hybrid layer or dentin).
Statistical Analysis
After verifying normality and homogeneity of the sample, data were analyzed statistically by Anova and Tukey’s test at a 5% significance level.
Results
Table 2 presents the means and standard deviations (SD) of ∆E and the 4 studied cements after the photoaging by UV-b. ANOVA did not demonstrate statistically significant differences (p>0.05) among the studied groups.
Table 3 presents the means and the standard deviation (SD) of ∆L, ∆a and ∆b of the 4 studied cements after photoaging by UV-b. ANOVA did not demonstrate statistically significant differences among the studied groups.
The micro shear test results are on Table 4. The bond strength of the RelyX Veneer cement was greater than all the others, followed by the CQ-based cement, then by the CQ+PPD-based one and the lowest result was obtained for the PPD cement; all with statistically significant difference (p>005).
Failure Mode Distribution
Failure mode distribution is shown in Figure 2. The SEM analysis identified 4 different fracture types in a sample of 182 microspecimens. The most frequent fractures were Type IV (mixed). For RelyX Veneer, which showed the highest BS values, 98% of the specimens had Type IV fractures and for CQ, which showed the highest BS values among experimental cements, 96% had Type IV fractures. In the group with the lowest BS values (PPD), 60% of the specimens had Type IV fractures, 36% Type II and 4% Type I.
Discussion
The first tested null hypothesis, that the PPD does not interfere on the color stability of the resin cements; was not rejected, because the results showed that there was neither difference on the color variation of all the 4 studied cements nor for ∆L, ∆a and ∆b; so, the use of PPD to avoid the yellowing of the composites could not be verified. The second null hypothesis tested, that the PPD does not interfere on the bond strength of the resin cements, was rejected, because the studied cements showed differences to each other, since the commercial cement RelyXVeneer® was the one that presented the greatest bond strength, followed by the CQ-based cement; then by the CQ+PPD cement and the lowest result was obtained by the cement using PPD only as photoinitiator.
The failure analysis mode revealed a higher prevalence of Type IV fractures. The RelyX Veneer and CQ groups resulted in 98% and 96% mixed fractures, respectively, and produced the highest mean bond strength, confirming the efficiency of these photoinitiators. Thus, the majority of fractures occurred cohesively in both cement and adhesive, showing a morphological appearance in relief on cement surface, characterized by a dense resin matrix with no pores around the inorganic silanized particles. These results indicated that the desired bond strength was achieved and were thus feasible for clinical use.
As PPD and CQ have absorption in different specters of wavelength, the PPD was chosen because it would be a better initiator alternative to specters in the UV region (390 nm), compared to CQ (470 nm). However, this could be a disadvantage for the conversion of C=C, because low energy would be concentrated on UV specter 99 Brandt, WC; Schneider, LFJ; Frollini, E; CorrerSobrinho, L; Sinhoreti, MAC. Effect of different photo-initiators and light curing units on degree of conversion of composites. Braz Oral Res2010;24:263-270.. The PPD is used in the composites because it has a greater molar extinction coefficient than the CQ; given that the probability that one molecule will absorb the light. The photoinitiators with great molar extinction coefficient are capable of absorbing more photons, produce more free radicals and contribute to high degree values of conversion 1616 Shin, DH; Rawls, HR. Degree of conversion and color stability of the light curing resin with new photoinitiator systems. Dent Mater 2009;25:1030-1038.,1717 Brandt, WC; Silva, CG; Frollini, E; SouzaJunior, EJC; Sinhoreti, MAC. Dynamic mechanical thermal analysis of composite resins with CQ and PPD as photo-initiators photoactivated by QTH and LED units. J Mech Behav Biomed Mater 2013;24:21-29.. Since both polywave LED and QTH curing units exhibited effectiveness in curing the resin cements containing PPD or CQ 1010 Segreto, DR; Naufel, FS; Brandt, WC; Guiraldo, RD; Correr, Sobrinho, L; Sinhoreti, MAC. Influence of photoinitiators and light sources on the degree of conversion of experimental resin cements. Braz Dent Sci 2015;18:65-72., in this study was used the Valo LED curing light with a spectrum in the range of 395-480 nm.
To improve the photoinitiators efficiency in lower concentration, was used 1.0% wt of co-initiator (DMAEMA), in a fixed dose (2:1 of co-initiator for photoinitiator, adjusted to 0,5% wt of initiator), based on the Teshima et al. protocol 1818 Teshima, W; Nomura, Y; Tanaka, N; Urabe, H; Okazaki, M; Nahara, Y. ESR study of camphorquinone/amine photoinitiator systems using blue light-emitting diodes. Biomater2003;24:2097-2103..
The CQ with DMAEMA or EDMAB effects 1919 Musaje, L; Ferracane, JL; Sakagushi, RL. Determination of the optimal photoinitiator concentration in dental composites based on essential material properties. Dent Mater 2009;25:994-1000. on GC showed that many combinations of CQ and amine (DMAEMA/EDMAB) can produce greater GC. In relation to the number of CQ mol to amine, maximum GC was not obtained, given the differences in the resin formations and the kind of accelerated amines used in both studies. The Yoshida and Greener’s study 2020 Yoshida, K; Greener, EH. Effects of two amine reducing agents on the degree of conversion and physical properties of an unfilled light-cured resin. Dent Mater1993;9:246-251. suggested a plateau on GC after the ideal proportion of CQ and amine was obtained and the Musage study showed a tendency to the decrease on GC or Knoop hardness, with concentrations above the ideal concentration of CQ to amine.
It must be considered that 1.4 mm ceramic between the light source and the cementation agent, can reduce the final irradiance of the curing light and thicker or darker ceramic restorations are obstacles to light and may reduce the quality and quantity of light incident on the resin cement, compromising many times the final polymerization 2121 Runnacles, P; Correr, GM; Baratto, Filho F; Gonzaga, CC; Furuse, AY. Degree of conversion of a resin cement light-cured through ceramic veneers of different thicknesses and types. Braz Dental J 2014;25:38-42., or even masking the cement’s color variation.
Schneider et al. 77 Schneider, LFJ; Cavalcante, LM; Consani, S; Ferracane, JL. Effect of co-initiator ratio on the polymer properties of experimental resin composites formulated with camphorquinone and phenyl-propanedione. Dent Mater 2009;25:369-375. studied the yellowing of composites containing PPD in concentrations similar to this study and concluded that the PPD-based composite yellowed significantly more than CQ; however, since it was about restoring composites, the reading of the color was made directly on the composite surface. Thus, the ceramic in this study is a possible justification for differences not being detected in the color variation of the cements containing photoinitiators associated to amine.
The color variation observed in all the studied cements was inferior to the power of detection of the human eye, considering that all the studied cements are acceptable when employed to the ceramics cementation more than 1.4 mm thick. New studies can be performed using more exposure to light, to verify the color variation of these cements with time.
The bond strength of cements to ceramics was evaluated by the micro shear test. The lowest bond strength of the cements containing PPD and PPD+CQ, according to Denis et al. 2222 Denis, AB; Diagone, CA; Plepis, AM; Viana, RB. The effect of the polymerization initiator and light source on the elution of residual Bis-GMA and TEGDMA monomers: A study using liquid chromatography with UV detection. Spectrochim Acta A Mol Biomol Spectrosc 2015;151:908-915. occurs because of the residual monomers on the composite. When studying a composite TEGDMA-based and BIS-GMA-based, manipulated with PPD, CQ or CQ+PPD, those authors verified that there are more residual monomers in the composite with PPD, which compromises the physico-mechanical properties of the material, besides increasing its toxicity.
Employing a LED luminous source, Segreto et al. 1010 Segreto, DR; Naufel, FS; Brandt, WC; Guiraldo, RD; Correr, Sobrinho, L; Sinhoreti, MAC. Influence of photoinitiators and light sources on the degree of conversion of experimental resin cements. Braz Dent Sci 2015;18:65-72. observed that the manipulated cement with CQ+PPD showed greater bond strength, compared to manipulated cements with only CQ or PPD. This difference may be ascribed to the fact that the authors have performed the microtensile test, which tests simultaneously the dentin/cement and the cement/ceramic interfaces.
A chemical difference of the experimental cements in relation to the commercial one, is that the experimental ones contain the UDMA monomer and according to Walterns et al. 2323 Walters NJ; Xia W; Salih V; Ashley PF; Young, AM. Poly (propylene glycol) and urethane dimethacrylates improve conversion of dental composites and reveal complexity of cytocompatibility testing. Dent Mater 2016;32:264-277., when the UDMA is incorporated with Bis-GMA or TEG-DMA, forming a stronger and more homogeneous polymers trio, it improves the physico-mechanical composite properties.
The fact that the commercial cement (RelyX Veneer®), which has the photoinitiator Hexafluorophosphate diphenyl iodonium (DPIH) in its formulation, exhibits greater bond strength can be assigned to the kinetic differences and the polymerization rate, on the conversion degree and on the temperature of vitreous transition 99 Brandt, WC; Schneider, LFJ; Frollini, E; CorrerSobrinho, L; Sinhoreti, MAC. Effect of different photo-initiators and light curing units on degree of conversion of composites. Braz Oral Res2010;24:263-270..
In addition to the limitations of the in vitro tests, it may be concluded that the PPD is not an option for CQ substitution in resinous composites, since its bond strength was inferior and did not exhibit superiority in color stability, compared to the other tested cements.
References
-
1Akgungor, G; Akkayan, B; Gaucher, H. Influence of ceramic thickness and polymerization mode of a resin luting agent on early bond strength and durability with a lithium disilicate-based ceramic system. J Prosthet Dent 2005;94:234-241.
-
2Chae K, H; Sun G, J. Phenylpropanedione;A new visible light photosensitizer for dental composite resin with higher efficiency than camphorquinone. Bull Korean Chem Soc 1998;19,152-154.
-
3Schneider, LFJ; Pfeifer, CS; Consani, S; Prahl, SA; Ferracane, JL. Influence of photoinitiator type on the rate of polymerization, degree of conversion, hardness and yellowing of dental resin composites. Dent Mater 2008;24:1169-1177.
-
4Lührs, AK; De Munck, J; Geurtsen, W; Van Meerbeek, B. Composite cements benefit from light-curing. Dent Mater 2014;30: 292-301.
-
5Aguiar, TR; Francescantonio, MD; Arrais, CA; Ambrosano, GMB; Davanzo, C; Giannini, M. Influence of curing mode and time on degree of conversion of one conventional and two self-adhesive resin cements. Oper Dent 2010;35:295-299.
-
6Park, YJ; Chae, KH; Rawls, HR. Development of a new photoinitiation system for dental light-cure composite resins. Dent Mater 1999;15:120-127.
-
7Schneider, LFJ; Cavalcante, LM; Consani, S; Ferracane, JL. Effect of co-initiator ratio on the polymer properties of experimental resin composites formulated with camphorquinone and phenyl-propanedione. Dent Mater 2009;25:369-375.
-
8Oliveira, KM; Consani,S; Gonçalves, LS; Brandt, WC; Ccahuana-Vásquez, RA. Photoelastic evaluation of the effect of composite formulation on polymerization shrinkage stress. Braz Oral Res 2012, 26:202-208.
-
9Brandt, WC; Schneider, LFJ; Frollini, E; CorrerSobrinho, L; Sinhoreti, MAC. Effect of different photo-initiators and light curing units on degree of conversion of composites. Braz Oral Res2010;24:263-270.
-
10Segreto, DR; Naufel, FS; Brandt, WC; Guiraldo, RD; Correr, Sobrinho, L; Sinhoreti, MAC. Influence of photoinitiators and light sources on the degree of conversion of experimental resin cements. Braz Dent Sci 2015;18:65-72.
-
11Peumans, M; Van Meerbeek ,B; Lambrechts, P; Vanherle, G. Porcelain veneers: a review of the literature. J Dent 2000;28:163-177.
-
12Heydecke, G; Zhang, F; Razzoog, ME. In vitro color stability of double-layer veneers after accelerated aging. J Prosthet Dent 2001;85:551-557.
-
13Oliveira, DCRSD; Souza, Júnior, EJ; Prieto LT; Coppini EK; Maia RR; Paulillo, LAMS. Color stability and polymerization behavior of direct esthetic restorations. J Esthet Rest Dent 2014;26:288-295.
-
14De Oliveira DCRS; Rocha, MG; Gatti, A; Correr, AB; Ferracane, JL; Sinhoret, MAC. Effect of different photoinitiators and reducing agents on cure efficiency and color stability of resin-based composites using different LED wavelengths. J Dent 2015;43:1565-1572.
-
15Oliveira, DCRS; Ayres, APA; Rocha, MG; Giannini, M; Puppin Rontani, RM; Ferracane, JL; et al.. Effect of different in vitro aging methods on color stability of a dental resin-based composite using CIELAB and CIEDE2000 color-difference Formulas. J Esthet Rest Dent 2015;27:322-330.
-
16Shin, DH; Rawls, HR. Degree of conversion and color stability of the light curing resin with new photoinitiator systems. Dent Mater 2009;25:1030-1038.
-
17Brandt, WC; Silva, CG; Frollini, E; SouzaJunior, EJC; Sinhoreti, MAC. Dynamic mechanical thermal analysis of composite resins with CQ and PPD as photo-initiators photoactivated by QTH and LED units. J Mech Behav Biomed Mater 2013;24:21-29.
-
18Teshima, W; Nomura, Y; Tanaka, N; Urabe, H; Okazaki, M; Nahara, Y. ESR study of camphorquinone/amine photoinitiator systems using blue light-emitting diodes. Biomater2003;24:2097-2103.
-
19Musaje, L; Ferracane, JL; Sakagushi, RL. Determination of the optimal photoinitiator concentration in dental composites based on essential material properties. Dent Mater 2009;25:994-1000.
-
20Yoshida, K; Greener, EH. Effects of two amine reducing agents on the degree of conversion and physical properties of an unfilled light-cured resin. Dent Mater1993;9:246-251.
-
21Runnacles, P; Correr, GM; Baratto, Filho F; Gonzaga, CC; Furuse, AY. Degree of conversion of a resin cement light-cured through ceramic veneers of different thicknesses and types. Braz Dental J 2014;25:38-42.
-
22Denis, AB; Diagone, CA; Plepis, AM; Viana, RB. The effect of the polymerization initiator and light source on the elution of residual Bis-GMA and TEGDMA monomers: A study using liquid chromatography with UV detection. Spectrochim Acta A Mol Biomol Spectrosc 2015;151:908-915.
-
23Walters NJ; Xia W; Salih V; Ashley PF; Young, AM. Poly (propylene glycol) and urethane dimethacrylates improve conversion of dental composites and reveal complexity of cytocompatibility testing. Dent Mater 2016;32:264-277.
Publication Dates
-
Publication in this collection
Jan-Feb 2018
History
-
Received
13 Mar 2017 -
Accepted
16 Oct 2017