Resumos
O objetivo do estudo foi determinar se o anel de tensão capsular (ATC), isoladamente ou associado à implantação de uma lente intraocular, poderia diminuir a ocorrência de opacificação da cápsula posterior (OCP) após a cirurgia de catarata por facoemulsificação em cães. Para tanto, cães portadores de catarata imatura ou madura foram avaliados, perfazendo um total de vinte olhos. Em todos os animais, foram excluídas quaisquer doenças oftálmicas e sistêmicas concomitantes. Os olhos foram selecionados aleatoriamente para receber o anel (ATC) isolado ou em associação com a lente. Flaremetria a laser e avaliações clínicas foram realizadas aos 2, 7, 14, 21, e 28 dias de pós-operatório. Fotografias foram tomadas aos 28 e a seguir a cada 30 dias, até os 180 dias. Os resultados mostraram inflamação mais importante nos olhos com IOL, embora, entre os parâmetros avaliados, apenas nas sinéquias houve diferença estatisticamente significativa. No entanto, em ambas as técnicas, quase nenhuma OCP ocorreu até o momento final das avaliações. Tais resultados sugerem que os anéis de tensão capsular (ATC) podem ser úteis na prevenção da opacidade capsular pós-operatória, sem complicações decorrentes
anel de tensão capsular; catarata, cães; lente intraocular; opacidade de cápsula posterior; facoemulsificação
The purpose of the study was to determine whether capsular tension ring (CTR) alone or associated with the implantation of an intraocular lens (IOL) could decrease the occurrence of posterior capsular opacification (PCO) after phacoemulsification cataract surgery in dogs. Twenty eyes of client-owned dogs with immature or mature cataracts were included in this study. In all the animals, any ophthalmic or systemic concurrent disease was excluded. The eyes were randomly selected to receive CTR alone or in association with the IOL. Laser flaremetry and clinical evaluations were conducted on post-operative days 2, 7, 14, 21 and 28. Fundus photographs were taken at the 28th and then every 30 days, up to 180 days. The results showed more inflammatory response on eyes with IOLs, although among the parameters evaluated, solely the synechiae showed significant statistical differences. Nevertheless, in both techniques almost no PCOs occurred at the end of the evaluations. These results suggest that the CTRs can be useful in the prevention of the post-operative capsular opacities, with minor complications
capsular tension ring; cataract, dog; intraocular lens; posterior capsular opacification, facoemulsification
INTRODUCTION:
Cataract is the main cause of vision impairment both in humans and in dogs.
Phacoemulsification with intraocular lens (IOL) implantation is the best method for
restoring sight. The most common long-term postoperative complication in both humans and
dogs is posterior capsule opacification (PCO) (GIFT et
al., 2009GIFT, B.W. et al. Comparison of capsular opacification and refractive
status after placement of three different intraocular lens implants following
phacoemulsification and aspiration of cataracts in dogs. Veterinary, Ophthalmology
v.12, p.13-21, 2009. Available from:
<http://www.ncbi.nlm.nih.gov/pubmed/19152593>. Accessed: Sept. 4, 2012. doi:
10.1111/j.1463-5224.2009.00667.x.
http://www.ncbi.nlm.nih.gov/pubmed/19152...
). Prevention of posterior capsule opacification is especially
important for dogs, which present high PCO rates, about 69 to 100% up to one year after
surgery (BRAS et al., 2006BRAS, I.D. et al. Posterior capsular opacification in diabetic and
non-diabetic canine patients following cataract surgery. Veterinary, Ophthalmology
v.9, p.317-327, 2006. Avaiable from:
<http://onlinelibrary.wiley.com/doi/10.1111/j.1463-5224.2006.00458.x/full>.
Accessed: Aug. 22, 2014. doi: 10.1111/j.1463-5224.2006.00458.x.
http://onlinelibrary.wiley.com/doi/10.11...
). The severity of PCO
in canine patients is also greater and may be related to the differences in inflammatory
and fibrous response (GERARDI et al., 1999GERARDI, J.G. et al. Immunohistochemical analysis of lens
epithelial-derived membranes following cataract extraction in the dog. Veterinary,
Ophthalmology v.2, p.163-168, 1999. Available from:
<http://onlinelibrary.wiley.com/doi/10.1046/j.1463-5224.1999.00071.x/full>.
Accessed: Aug. 22, 2014. doi: 10.1046/j.1463-5224.1999.00071.x.
http://onlinelibrary.wiley.com/doi/10.10...
).
PCO is caused by a regenerative response of residual lens epithelial cells (LEC) that
proliferate and undergo epithelial mesenchymal transformation (EMT), that is, change
from normal cuboidal epithelial cells into spindle shaped fibroblast-like cells that
expresses α-smooth muscle actin (MEDVEDOVIC et al.,
2006MEDVEDOVIC, M. et al. Gene expression and discovery during lens
regeneration in mouse: regulation of epithelial to mesenchymal transition and lens
differentiation. Molecular Vision, v.12, p.422-440, 2006. Avaiable from:
<http://www.molvis.org/molvis/v12/a49/>. Accessed: Aug. 29,
2014.
http://www.molvis.org/molvis/v12/a49/...
). These cells can migrate along the posterior face of lens capsule
leading to various degrees of visual impairment. The current treatment of PCO in humans,
using Nd:YAG laser, is expensive and not free from complications (HAZRA et al., 2012HAZRA, S. et al. Comparison of design of intraocular lens versus the
material for PCO prevention. Internationa.l Journal of, Ophthalmology v.5, p.59-63,
2012. Avaiable from:
<http://www.ijo.cn/gjyken/ch/reader/view_abstract.aspx?file_no=201201012&flag=1>.
Accessed: Aug. 29, 2014. doi: 10.3980/j.issn.2222-3959.2012.01.12.
http://www.ijo.cn/gjyken/ch/reader/view_...
). Laser capsulotomy is less successful in canine
patients due to the presence of dense capsular plaques, residual lens material and thick
inflammatory membranes requiring greater energy to achieve a capsular hole (NASISSE & DAVIDSON, 1988NASISSE, M.P.; DAVIDSON, M.G. Laser therapy in veterinary ophthalmology:
perspective and potential. Seminars in Veterinary Medicine and Surgery (Small
Animal), v. 3, n.1, p.52-54, 1988. Avaiable from:
<http://www.ncbi.nlm.nih.gov/pubmed/3283889>. Acessed: Aug. 29,
2014.
http://www.ncbi.nlm.nih.gov/pubmed/32838...
).
Although lens implantation is considered one of the main choices in the prevention of
PCO in both species, it is not sufficient to effectively prevent the opacities in both.
Studies in dogs using different types of lenses demonstrate only partial control of PCO
months after the surgery (YI et al., 2006YI, N.Y. et al. Phacoemulsification and acryl foldable intraocular lens
implantation in dogs: 32 cases. Journal of Veterinary Science, v.7, n.3, p. 281-285,
2006. Avaiable from <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3242129/>.
Accessed: Aug. 22, 2014. doi: 10.4142/jvs.2006.7.3.281.
http://www.ncbi.nlm.nih.gov/pmc/articles...
; GIFT et al., 2009GIFT, B.W. et al. Comparison of capsular opacification and refractive
status after placement of three different intraocular lens implants following
phacoemulsification and aspiration of cataracts in dogs. Veterinary, Ophthalmology
v.12, p.13-21, 2009. Available from:
<http://www.ncbi.nlm.nih.gov/pubmed/19152593>. Accessed: Sept. 4, 2012. doi:
10.1111/j.1463-5224.2009.00667.x.
http://www.ncbi.nlm.nih.gov/pubmed/19152...
). Many trials have been performed
to test the IOL materials and shapes in animals and in humans (YI et al., 2006YI, N.Y. et al. Phacoemulsification and acryl foldable intraocular lens
implantation in dogs: 32 cases. Journal of Veterinary Science, v.7, n.3, p. 281-285,
2006. Avaiable from <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3242129/>.
Accessed: Aug. 22, 2014. doi: 10.4142/jvs.2006.7.3.281.
http://www.ncbi.nlm.nih.gov/pmc/articles...
; KUGELBERG et al.,
2008KUGELBERG, M. et al. Two-year follow-up of posterior capsule
opacification after implantation of a hydrophilic or hydrophobic acrylic intraocular
lens. Acta Ophthalmologica, v.86, p.533-536, 2008. Available from:
<http://www.ncbi.nlm.nih.gov/pubmed/18081899>. Acessed: Out. 5,
2012.
http://www.ncbi.nlm.nih.gov/pubmed/18081...
; GIFT et al., 2009GIFT, B.W. et al. Comparison of capsular opacification and refractive
status after placement of three different intraocular lens implants following
phacoemulsification and aspiration of cataracts in dogs. Veterinary, Ophthalmology
v.12, p.13-21, 2009. Available from:
<http://www.ncbi.nlm.nih.gov/pubmed/19152593>. Accessed: Sept. 4, 2012. doi:
10.1111/j.1463-5224.2009.00667.x.
http://www.ncbi.nlm.nih.gov/pubmed/19152...
). The theory
that the shape of the square edge is more important than the IOL materials has gained
popularity and the IOLs have been modified in an attempt to effectively reduce PCO
formation. Some studies have reported that a sharp posterior optic edge is the main
factor in preventing PCO (KOHNEN et al., 2008KOHNEN, T. et al. Optic edge design as long-term factor for posterior
capsular opacification rates. Ophthalmology, v.115, n.8, p.1308-1314, 2008. Avaiable
from: <http://www.aaojournal.org/article/S0161-6420(08)00004-3/fulltext>.
Accessed: Aug. 29, 2014. doi:
http://dx.doi.org/10.1016/j.ophtha.2008.01.002.
http://www.aaojournal.org/article/S0161-...
)
due to the "barrier effect" against lens epithelial migration (APPLE et al., 2001APPLE, D.J. et al. Eradication of posterior capsule opacification.
Ophthalmology, v.108, n.3, p.505-518, 2001. Avaliabre from:
<http://www.sciencedirect.com/science/article/pii/S0161642000005893>. Accessed:
Aug. 22, 2014. doi: 10.1016/S0161-6420(00)00589-3.
http://www.sciencedirect.com/science/art...
).
It has also been shown that the use of the endocapsular tension ring can reduce
secondary lens epithelial cell (LEC) proliferation (NISHI et al., 2001NISHI, O. et al. Capsular bending ring to prevent posterior capsule
opacification: 2 year follow-up. Journal of Cataract and Refractive Surgery, v.27,
p.1359-1365, 2001. Avaiable from:
<http://www.jcrsjournal.org/article/S0886-3350(01)00892-6/fulltext>. Accessed:
Aug. 22, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(01)00892-6.
http://www.jcrsjournal.org/article/S0886...
). Capsular tension rings were first reported to be used to
maintain the shape of the capsular bag after the insertion of IOLs (HARA et al., 1991HARA, T. et al. "Equator Ring" for maintenance of the completely
circular contour of the capsular bag equator after cataract removal. Ophthalmic
Surgery, v.22, p.358-359, 1991. Avaiable from:
<http://www.ncbi.nlm.nih.gov/pubmed/1896178>. Accessed: Aug. 29,
2014.
http://www.ncbi.nlm.nih.gov/pubmed/18961...
). It has also been used to
reinforce the zonule in cases of zonular dehiscence or to facilitate the
phacoemulsification in traumatic cataracts (MARQUES et
al., 2007MARQUES, D.M. et al. Avaliação do uso do anel endocapsular modificado em
casos de subluxação traumática do cristalino. Arquivos Brasileiros de Oftalmologia,
v.70, p.746-751, 2007. Avaiable from:
<http://www.scielo.br/scielo.php?pid=S0004-27492007000500004&script=sci_arttext>.
Accessed: Aug. 29, 2014. doi:
http://dx.doi.org/10.1590/S0004-27492007000500004.
http://www.scielo.br/scielo.php?pid=S000...
). It was then observed that the secondary cataract was significantly
lower in those eyes that have received the ring implantation (KIM et al., 2005KIM, J.H. et al. The effect of capsular tension ring on posterior
capsular opacity in cataract surgery. Korean Journal of, Ophthalmology v.19, p.23-28,
2005. Avaiable from:
<http://synapse.koreamed.org/DOIx.php?id=10.3341/kjo.2005.19.1.23>. Accessed:
Aug. 29, 2014. doi: org/10.3341/kjo.2005.19.1.23.
http://synapse.koreamed.org/DOIx.php?id=...
). Some authors have proposed to modify its shape to
improve PCO prevention (NISHI et al., 2001NISHI, O. et al. Capsular bending ring to prevent posterior capsule
opacification: 2 year follow-up. Journal of Cataract and Refractive Surgery, v.27,
p.1359-1365, 2001. Avaiable from:
<http://www.jcrsjournal.org/article/S0886-3350(01)00892-6/fulltext>. Accessed:
Aug. 22, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(01)00892-6.
http://www.jcrsjournal.org/article/S0886...
).
The data show that the lens alone is not able to prevent PCO as expected. Nevertheless, the real need is to prevent PCO formation after canine cataract surgery, and few studies about it have been carried out. This study aims to investigate the role of the CTR alone and associated with IOL implantation in the control of PCO in dogs after phacoemulsification.
MATERIALS AND METHODS:
Animals
A total of 20 eyes of client-owned dogs of multiple breeds, aging between 3 and 10 years old, with immature or mature cataracts, were enrolled in the study. All the dogs underwent a complete ophthalmic and physical examination in order to exclude any other ophthalmic or systemic disease. Ocular ultrasound (UltraScan Imaging System - Alcon do Brasil, SP, Brazil) and electroretinogram (Handheld Multi-species ERG - Retvetcorp, Columbia, MO, USA) were performed to rule out vitreal or retinal pathologies. The globes were also measured by ultrasonography to estimate CTR and IOL sizes. All dogs were pre-treated with topical tobramicyn and dexametasone association (Tobradex, Alcon do Brasil, SP, Brazil) every six hours and 1mgkg of oral prednisolone (Meticorten, MSD Saúde Animal, SP, Brazil) every 24 hours, starting 3 days prior to surgery. Topical 1% atropine (Atropina 1% - Allergan Produtos Farmacêuticos, SP, Brazil) was applied 12 hours and again 30 minutes before the surgery.
General anesthesia was induced using routine procedures and maintained with isoflurane (Isoforine - Cristália, SP, Brazil) inhalation. Trypan blue (Azul de Tripan - Ophthalmos, SP, Brazil) was used to show the anterior capsule lens. A continuous curvilinear capsulorhexis was performed and all of the eyes received intracameral injections of two viscoelastic substances (Viscoat - Alcon labs, SP, Brazil; Metilcelulose 2% - Ophthalmos, SP, Brazil) to maintain the chamber and protect the endothelium. Hydrodissection was also performed on all eyes. Surgery was carried out using an Alcon phacoemulsification machine (Facoemulsificador Universal II - Alcon do Brasil, SP, Brazil). All eyes received a 12 or 14mm silicon CTR (Acri.Ring VR 125, VR 145 - Acrivet, Hennigsdorf, Germany) applied with an appropriate inserter (Tension Ring Injector - Acrivet, Hennigsdorf, Germany) and 10 of these eyes were randomly selected to receive also a squared edge foldable acrylic IOL (Posterior chamber lens 30-V 12, 30-V 14 - Acrivet, Hennigsdorf, Germany). If present, pre-existing capsular plaques were graduated and registered on the patient surgical record. The corneal incision was closed with interrupted 9-0 nylon sutures (Mononylon 9-0 - Ethicon, SP, Brazil).
A post-surgical medical protocol included oral prednisone (Meticorten, MSD Saúde Animal, SP, Brazil), 1mgkg SID for 2 weeks and then tapering the regimen within the following 2 weeks; topical association of 0.3% tobramycin and dexametasone (Tobradex, Alcon do Brasil, SP, Brazil) q4h for 2 weeks, q6h for 2 weeks; 1% brinzolamide (Azopt, Alcon do Brasil, SP, Brazil) q12h for one week and 1% tropicamide (Mydriacyl, Alcon do Brasil, SP, Brazil) q8h for one week completed the protocol. All the patients wore an Elizabethan collar for 2 weeks.
Reexamination period
Complete ophthalmic evaluations were conducted on post-operative days 2, 7, 14, 21, 28
and 60. Clinical parameters were graduated from 0-4 (0 = absent, 1 = slight, 2 = medium,
3 = intense, 4 = strong) and submitted to statistical analysis. Laser flaremetry
(FC-2000 Laser flare Meter - Kowa, Japan) was performed on post-operative days 2, 7, 14,
21 and 28. PCO was recorded by the examiners via slit-lamp biomicroscopy (SL-450 - Nidek
Co, Japan) and indirect ophthalmoscopy (OHC - 3.3 - Opto Eletrônica S.A., São Carlos,
SP, Brazil) on a scale of 0-4 as previously described (BRAS et al., 2006BRAS, I.D. et al. Posterior capsular opacification in diabetic and
non-diabetic canine patients following cataract surgery. Veterinary, Ophthalmology
v.9, p.317-327, 2006. Avaiable from:
<http://onlinelibrary.wiley.com/doi/10.1111/j.1463-5224.2006.00458.x/full>.
Accessed: Aug. 22, 2014. doi: 10.1111/j.1463-5224.2006.00458.x.
http://onlinelibrary.wiley.com/doi/10.11...
). Fundus photographs were also taken at the 28th
and then every 30 days, up to 180 days (TOPCON TRC 50DX - Topcon Medical Systems, Inc.,
Oakland, NJ, USA).
Image processing
In order to evaluate the PCO formation, the images were processed by software (Angioimage 1.5.1.0 - Copyright 2004-2007 DIGI-NET. Corp.) and then evaluated by two different examiners.
Statistical analysis
Mean values and standard deviations were calculated and the data were submitted to analysis of variance (ANOVA) followed by Tukey test. A P value <0.05 was considered significant.
RESULTS:
Return of vision was reported in all eyes. Synechiae were present since the 14th day in two eyes with IOL/CTR and in one eye with CTR in a slight level. However, during the observation time it increased in both groups. At the end of the 180 days, it was observed in four out of the ten eyes with CTR in slight and medium levels. In the group with IOL and CTR, it was seen in nine of the ten eyes, from slight to intense levels. Vascular congestion was observed in almost every eye of both groups. It lessened throughout the observation time, but remained for longer periods and in greater intensity in the eyes with IOL. Nevertheless, the statistic analysis showed that this apparent difference was not significant between the groups. Corneal edema was present only in few eyes and in a slight level, except for one eye from the IOL group, which became opaque since the 7th day and remained intensely opaque until the 180th day. On the other hand, photophobia occurred only until the 2nd day, and only slightly in both groups, although in more eyes with IOL.
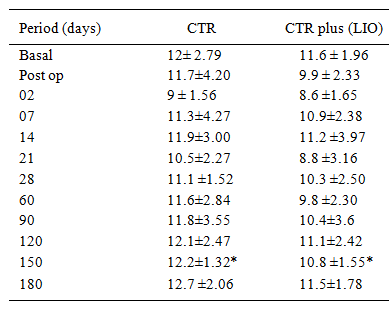
Although clinical inflammation seemed to be more evident in the eyes that received the CTR plus IOL, there were no statistical differences between techniques regarding the main parameters evaluated, including flare measurements by the laser cell flaremeter technique (Table 1). The mean IOP decreased during the earlier periods of observation, in a similar pattern in both groups (Table 2). IOP values showed statistical difference only on the 150th post-operative day (P<0.05). Otherwise, synechiae were more evident on those eyes that received the CTR plus the IOL from the 21 day (P<0.01) until the end of the period of the evaluations (180 days) (P<0.05). PCO occurred only in 1/10 (10%) of the eyes with IOL and CTR and a slight opacification was observed in one eye (10%) with the CTR alone up to the 180th post-operative day. Two eyes presented previous OCP, recorded as a grade 1, immediately after the surgery. This opacity showed little or no progress during the subsequent evaluations. Another eye that presented previous grade 1 OCP had the opacity reduced during the period (Figure 1).
: Means±SD the flare values (ph/ms), by laser flaremeter method, of the dogs that underwent surgery according to the follow-up periods.
: Image of posterior capsules. Left: From 2 (C) to 7 (A,F) and 14 (B,D,E) post-operative days. Right: On the 180th day. A. No PCO formation, note regular pupil and visible papilla (CTR). B. No PCO formation, regular pupil (CTR plus LIO). C. Lessening of PCO, note grade 1 synechia on the 180th day (CTR). D. Subtle PCO formation, note regular pupil, visible papilla and congestion on the 2nd day (CTR). E. Subtle PCO formation, note grade 2 sinechia since the 14th day and congestion (CTR plus LIO). F. With grade 1 previous PCO, no worsening of opacity, note pupil slightly irregular in both periods and congestion on the 7th day (CTR plus LIO).
DISCUSSION:
Results of this study indicate that within 180 days post-implantation, eyes with capsular tension ring alone and with capsular tension ring plus intraocular lens showed almost no posterior capsular opacities formation, so there were no sufficient data to establish a statistical analysis. The differences were subtle between the groups regarding inflammation parameters, being the synechiae the only one that were significantly greater on those eyes that received CTR and IOL together. This can happen because of the greater manipulation used to insert the IOLs. Basal flaremetry was higher in the first post-operative days because of the increased inflammation after the surgery, but it returned to lower values along the period with the lessening of the inflammation.
Posterior capsular opacification (PCO) is caused by proliferation and migration of
residual LEC, fibroblasts, macrophages, and iris-derived pigment cells on the posterior
capsule (KAPPELHOF & VRENSEN, 1992KAPPELHOF, J.; VRENSEN, G. The pathology of after-cataract. ACTA
Ophthalmologica, v.205, Suppl., p.13-24, 1992. Avaiable from:
<http://onlinelibrary.wiley.com/doi/10.1111/j.1755-3768.1992.tb02176.x/abstract>.
Accessed: Aug. 29, 2014. doi: 10.1111/j.1755-3768.1992.tb02176.x
http://onlinelibrary.wiley.com/doi/10.11...
).These
residual LECs differentiate into fibroblast-like cells via EMT, resulting in fibrous
plaque formation. Some authors believe that it is the anterior LECs that re-colonize the
anterior capsule, and then migrate to the posterior lens capsule (WORMSTONE, 2002WORMSTONE, M. Posterior capsule opacification: a cell biological
perspective. Experimental Eye Research, v.74, p.337-347, 2002. Avaiable from:
<http://www.sciencedirect.com/science/article/pii/S0014483508003564>. Accessed:
Aug. 22, 2014. doi: 10.1016/j.exer.2008.10.016.
http://www.sciencedirect.com/science/art...
), while others believe that the equatorial LECs are
the primary source of PCO formation (APPLE et al.,
2001APPLE, D.J. et al. Eradication of posterior capsule opacification.
Ophthalmology, v.108, n.3, p.505-518, 2001. Avaliabre from:
<http://www.sciencedirect.com/science/article/pii/S0161642000005893>. Accessed:
Aug. 22, 2014. doi: 10.1016/S0161-6420(00)00589-3.
http://www.sciencedirect.com/science/art...
).
It is also believed that sharp-edged IOLs and capsular rings can produce a "barrier
effect" preventing the migration of these cells and, consequently, the PCO formation
(APPLE et al., 2001APPLE, D.J. et al. Eradication of posterior capsule opacification.
Ophthalmology, v.108, n.3, p.505-518, 2001. Avaliabre from:
<http://www.sciencedirect.com/science/article/pii/S0161642000005893>. Accessed:
Aug. 22, 2014. doi: 10.1016/S0161-6420(00)00589-3.
http://www.sciencedirect.com/science/art...
; KUGELBERG et al., 2008KUGELBERG, M. et al. Two-year follow-up of posterior capsule
opacification after implantation of a hydrophilic or hydrophobic acrylic intraocular
lens. Acta Ophthalmologica, v.86, p.533-536, 2008. Available from:
<http://www.ncbi.nlm.nih.gov/pubmed/18081899>. Acessed: Out. 5,
2012.
http://www.ncbi.nlm.nih.gov/pubmed/18081...
; KOHNEN et
al., 2008KOHNEN, T. et al. Optic edge design as long-term factor for posterior
capsular opacification rates. Ophthalmology, v.115, n.8, p.1308-1314, 2008. Avaiable
from: <http://www.aaojournal.org/article/S0161-6420(08)00004-3/fulltext>.
Accessed: Aug. 29, 2014. doi:
http://dx.doi.org/10.1016/j.ophtha.2008.01.002.
http://www.aaojournal.org/article/S0161-...
). Histopathology studies showed that a sharp capsular bend was
formed at the sharp posterior optic edge of the IOLs and that the migration of lens was
inhibited at this site. Experimental and clinical studies suggest that the sharper the
edge is, the greater the preventive effect (NISHI et
al., 2001NISHI, O. et al. Capsular bending ring to prevent posterior capsule
opacification: 2 year follow-up. Journal of Cataract and Refractive Surgery, v.27,
p.1359-1365, 2001. Avaiable from:
<http://www.jcrsjournal.org/article/S0886-3350(01)00892-6/fulltext>. Accessed:
Aug. 22, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(01)00892-6.
http://www.jcrsjournal.org/article/S0886...
; NAGAMOTO & FUGIWARA,
2003NAGAMOTO, T.; FUJIWARA, T. Inhibition of lens epithelial cell migration
at the intraocular lens optic edge. Role of capsule bending and contact pressure.
Journal of Cataracts and Refractive Surgery, v.29, p.1605-1612, 2003. Avaiable from:
<http://www.jcrsjournal.org/article/S0886-3350(03)00050-6/fulltext>. Accessed:
Aug. 29, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(03)00050-6.
http://www.jcrsjournal.org/article/S0886...
).
Pharmacologic attempts to inhibit mitosis and metaplasia of the LECs have not been
successful or result in corneal endothelial toxicity (NISHI et al., 2001NISHI, O. et al. Capsular bending ring to prevent posterior capsule
opacification: 2 year follow-up. Journal of Cataract and Refractive Surgery, v.27,
p.1359-1365, 2001. Avaiable from:
<http://www.jcrsjournal.org/article/S0886-3350(01)00892-6/fulltext>. Accessed:
Aug. 22, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(01)00892-6.
http://www.jcrsjournal.org/article/S0886...
). Moreover, the use of the lens alone is also not able to
prevent PCO formation as expected in dogs, with the findings showing only a partial
control of PCO months after the surgery (YI et al.,
2006YI, N.Y. et al. Phacoemulsification and acryl foldable intraocular lens
implantation in dogs: 32 cases. Journal of Veterinary Science, v.7, n.3, p. 281-285,
2006. Avaiable from <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3242129/>.
Accessed: Aug. 22, 2014. doi: 10.4142/jvs.2006.7.3.281.
http://www.ncbi.nlm.nih.gov/pmc/articles...
; GIFT et al., 2007). What is noteworthy in this study is the almost
complete absence of PCO formation in both groups 6 months after surgery. Others studies
in dogs showed much more PCO after shorter periods of time. YI et al (2006YI, N.Y. et al. Phacoemulsification and acryl foldable intraocular lens
implantation in dogs: 32 cases. Journal of Veterinary Science, v.7, n.3, p. 281-285,
2006. Avaiable from <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3242129/>.
Accessed: Aug. 22, 2014. doi: 10.4142/jvs.2006.7.3.281.
http://www.ncbi.nlm.nih.gov/pmc/articles...
) found PCO as the main complication on the follow up
of dogs that received foldable acrylic lens, with 30% of the dogs presenting PCO up to
post- operative day 90. BRAS et al. (2006BRAS, I.D. et al. Posterior capsular opacification in diabetic and
non-diabetic canine patients following cataract surgery. Veterinary, Ophthalmology
v.9, p.317-327, 2006. Avaiable from:
<http://onlinelibrary.wiley.com/doi/10.1111/j.1463-5224.2006.00458.x/full>.
Accessed: Aug. 22, 2014. doi: 10.1111/j.1463-5224.2006.00458.x.
http://onlinelibrary.wiley.com/doi/10.11...
) showed
higher rates, with 100% of the patients developing time dependent PCO in both diabetic
and non-diabetic canine patients with PMMA lens implantation up to one year after
surgery.
It is important to consider that the PCO scores in this study were subjective and it was
not possible to establish a statistical analysis because of the almost absence of the
opacities. However, the photographs taken every 30 days were sufficiently reliable to
compare the slow evolution of the few PCOs that developed. Subjective methods of grading
PCO scores in humans have been compared to quantitative methods and have been found to
be a reliable method of measuring PCO (FINDL et al.,
2003FINDL, O. et al. Comparison of four methods for quantifying posterior
capsule opacification. Journal of Cataract and Refractive Surgery, v.29, p.106-111,
2003. Available from:
<http://www.sciencedirect.com/science/article/pii/S0886335002015092>. Accessed:
Aug. 22, 2014. doi: 10.1016/S0886-3350(02)01509-2
http://www.sciencedirect.com/science/art...
).
As far as the authors are aware, this is the first report showing the role of CTR in PCO prevention in dogs. According to another experimental study employing capsular bending rings, the bend could be better in preventing PCO, but it can also produce much more uveitis. Since the dog is much more prone to develop post-operatory uveitis, the benefit of using these devices in the species should be evaluated. In any case, studies employing bending rings could be another important alternative in preventing PCO in dogs. For now, it is possible to admit that the use of CTR can play an important role in the prevention of OCP, without major complications. The CTR have the additional advantage of stabilizing the lens when there is a zonule fragility.
Although in this study the period of evaluation stopped at the 180th day and more PCO can be formed during the following months or years after surgery, it is a critical period for PCO to begin. The results of this study are promising. However, a long-term follow-up will be needed because PCO may develop several years after cataract surgery.
ACKNOWLEDEGMENTS
Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP) (Process n. 2009/51773-4), Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq) (Process n. 300833/2010-5).
- APPLE, D.J. et al. Eradication of posterior capsule opacification. Ophthalmology, v.108, n.3, p.505-518, 2001. Avaliabre from: <http://www.sciencedirect.com/science/article/pii/S0161642000005893>. Accessed: Aug. 22, 2014. doi: 10.1016/S0161-6420(00)00589-3.
» https://doi.org/10.1016/S0161-6420(00)00589-3» http://www.sciencedirect.com/science/article/pii/S0161642000005893 - BRAS, I.D. et al. Posterior capsular opacification in diabetic and non-diabetic canine patients following cataract surgery. Veterinary, Ophthalmology v.9, p.317-327, 2006. Avaiable from: <http://onlinelibrary.wiley.com/doi/10.1111/j.1463-5224.2006.00458.x/full>. Accessed: Aug. 22, 2014. doi: 10.1111/j.1463-5224.2006.00458.x.
» https://doi.org/10.1111/j.1463-5224.2006.00458.x» http://onlinelibrary.wiley.com/doi/10.1111/j.1463-5224.2006.00458.x/full - FINDL, O. et al. Comparison of four methods for quantifying posterior capsule opacification. Journal of Cataract and Refractive Surgery, v.29, p.106-111, 2003. Available from: <http://www.sciencedirect.com/science/article/pii/S0886335002015092>. Accessed: Aug. 22, 2014. doi: 10.1016/S0886-3350(02)01509-2
» https://doi.org/10.1016/S0886-3350(02)01509-2» http://www.sciencedirect.com/science/article/pii/S0886335002015092 - GERARDI, J.G. et al. Immunohistochemical analysis of lens epithelial-derived membranes following cataract extraction in the dog. Veterinary, Ophthalmology v.2, p.163-168, 1999. Available from: <http://onlinelibrary.wiley.com/doi/10.1046/j.1463-5224.1999.00071.x/full>. Accessed: Aug. 22, 2014. doi: 10.1046/j.1463-5224.1999.00071.x.
» https://doi.org/10.1046/j.1463-5224.1999.00071.x» http://onlinelibrary.wiley.com/doi/10.1046/j.1463-5224.1999.00071.x/full - GIFT, B.W. et al. Comparison of capsular opacification and refractive status after placement of three different intraocular lens implants following phacoemulsification and aspiration of cataracts in dogs. Veterinary, Ophthalmology v.12, p.13-21, 2009. Available from: <http://www.ncbi.nlm.nih.gov/pubmed/19152593>. Accessed: Sept. 4, 2012. doi: 10.1111/j.1463-5224.2009.00667.x.
» https://doi.org/10.1111/j.1463-5224.2009.00667.x» http://www.ncbi.nlm.nih.gov/pubmed/19152593 - GOLDIM, J.R. Pesquisa em saúde e direito dos animais. Porto Alegre: HCPA, 1995. 28p.
- HARA, T. et al. "Equator Ring" for maintenance of the completely circular contour of the capsular bag equator after cataract removal. Ophthalmic Surgery, v.22, p.358-359, 1991. Avaiable from: <http://www.ncbi.nlm.nih.gov/pubmed/1896178>. Accessed: Aug. 29, 2014.
» http://www.ncbi.nlm.nih.gov/pubmed/1896178 - HAZRA, S. et al. Comparison of design of intraocular lens versus the material for PCO prevention. Internationa.l Journal of, Ophthalmology v.5, p.59-63, 2012. Avaiable from: <http://www.ijo.cn/gjyken/ch/reader/view_abstract.aspx?file_no=201201012&flag=1>. Accessed: Aug. 29, 2014. doi: 10.3980/j.issn.2222-3959.2012.01.12.
» https://doi.org/10.3980/j.issn.2222-3959.2012.01.12» http://www.ijo.cn/gjyken/ch/reader/view_abstract.aspx?file_no=201201012&flag=1 - KAPPELHOF, J.; VRENSEN, G. The pathology of after-cataract. ACTA Ophthalmologica, v.205, Suppl., p.13-24, 1992. Avaiable from: <http://onlinelibrary.wiley.com/doi/10.1111/j.1755-3768.1992.tb02176.x/abstract>. Accessed: Aug. 29, 2014. doi: 10.1111/j.1755-3768.1992.tb02176.x
» https://doi.org/10.1111/j.1755-3768.1992.tb02176.x» http://onlinelibrary.wiley.com/doi/10.1111/j.1755-3768.1992.tb02176.x/abstract - KIM, J.H. et al. The effect of capsular tension ring on posterior capsular opacity in cataract surgery. Korean Journal of, Ophthalmology v.19, p.23-28, 2005. Avaiable from: <http://synapse.koreamed.org/DOIx.php?id=10.3341/kjo.2005.19.1.23>. Accessed: Aug. 29, 2014. doi: org/10.3341/kjo.2005.19.1.23.
» https://doi.org/org/10.3341/kjo.2005.19.1.23» http://synapse.koreamed.org/DOIx.php?id=10.3341/kjo.2005.19.1.23 - KOHNEN, T. et al. Optic edge design as long-term factor for posterior capsular opacification rates. Ophthalmology, v.115, n.8, p.1308-1314, 2008. Avaiable from: <http://www.aaojournal.org/article/S0161-6420(08)00004-3/fulltext>. Accessed: Aug. 29, 2014. doi: http://dx.doi.org/10.1016/j.ophtha.2008.01.002.
» https://doi.org/http://dx.doi.org/10.1016/j.ophtha.2008.01.002» http://www.aaojournal.org/article/S0161-6420(08)00004-3/fulltext - KUGELBERG, M. et al. Two-year follow-up of posterior capsule opacification after implantation of a hydrophilic or hydrophobic acrylic intraocular lens. Acta Ophthalmologica, v.86, p.533-536, 2008. Available from: <http://www.ncbi.nlm.nih.gov/pubmed/18081899>. Acessed: Out. 5, 2012.
» http://www.ncbi.nlm.nih.gov/pubmed/18081899 - MARQUES, D.M. et al. Avaliação do uso do anel endocapsular modificado em casos de subluxação traumática do cristalino. Arquivos Brasileiros de Oftalmologia, v.70, p.746-751, 2007. Avaiable from: <http://www.scielo.br/scielo.php?pid=S0004-27492007000500004&script=sci_arttext>. Accessed: Aug. 29, 2014. doi: http://dx.doi.org/10.1590/S0004-27492007000500004.
» https://doi.org/http://dx.doi.org/10.1590/S0004-27492007000500004» http://www.scielo.br/scielo.php?pid=S0004-27492007000500004&script=sci_arttext - MEDVEDOVIC, M. et al. Gene expression and discovery during lens regeneration in mouse: regulation of epithelial to mesenchymal transition and lens differentiation. Molecular Vision, v.12, p.422-440, 2006. Avaiable from: <http://www.molvis.org/molvis/v12/a49/>. Accessed: Aug. 29, 2014.
» http://www.molvis.org/molvis/v12/a49/ - NAGAMOTO, T.; FUJIWARA, T. Inhibition of lens epithelial cell migration at the intraocular lens optic edge. Role of capsule bending and contact pressure. Journal of Cataracts and Refractive Surgery, v.29, p.1605-1612, 2003. Avaiable from: <http://www.jcrsjournal.org/article/S0886-3350(03)00050-6/fulltext>. Accessed: Aug. 29, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(03)00050-6.
» https://doi.org/http://dx.doi.org/10.1016/S0886-3350(03)00050-6» http://www.jcrsjournal.org/article/S0886-3350(03)00050-6/fulltext - NASISSE, M.P.; DAVIDSON, M.G. Laser therapy in veterinary ophthalmology: perspective and potential. Seminars in Veterinary Medicine and Surgery (Small Animal), v. 3, n.1, p.52-54, 1988. Avaiable from: <http://www.ncbi.nlm.nih.gov/pubmed/3283889>. Acessed: Aug. 29, 2014.
» http://www.ncbi.nlm.nih.gov/pubmed/3283889 - NISHI, O. et al. Capsular bending ring to prevent posterior capsule opacification: 2 year follow-up. Journal of Cataract and Refractive Surgery, v.27, p.1359-1365, 2001. Avaiable from: <http://www.jcrsjournal.org/article/S0886-3350(01)00892-6/fulltext>. Accessed: Aug. 22, 2014. doi: http://dx.doi.org/10.1016/S0886-3350(01)00892-6.
» https://doi.org/http://dx.doi.org/10.1016/S0886-3350(01)00892-6» http://www.jcrsjournal.org/article/S0886-3350(01)00892-6/fulltext - WORMSTONE, M. Posterior capsule opacification: a cell biological perspective. Experimental Eye Research, v.74, p.337-347, 2002. Avaiable from: <http://www.sciencedirect.com/science/article/pii/S0014483508003564>. Accessed: Aug. 22, 2014. doi: 10.1016/j.exer.2008.10.016.
» https://doi.org/10.1016/j.exer.2008.10.016» http://www.sciencedirect.com/science/article/pii/S0014483508003564 - YI, N.Y. et al. Phacoemulsification and acryl foldable intraocular lens implantation in dogs: 32 cases. Journal of Veterinary Science, v.7, n.3, p. 281-285, 2006. Avaiable from <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3242129/>. Accessed: Aug. 22, 2014. doi: 10.4142/jvs.2006.7.3.281.
» https://doi.org/10.4142/jvs.2006.7.3.281» http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3242129/
-
1
COMMITTEE OF ETHICS AND ANIMAL WELFARE The study protocol was submitted to and approved by the Committee of Ethics and Animal Welfare of the College of Agricultural and Veterinarian Sciences - UNESP - Jaboticabal (Protocol 025303/12). Bioethics cares follow the guidelines from Association for Research in Vision and Ophthalmology - ARVO (National Institutes of Health Publications No 85-23: Revised 1985) (GOLDIM, 1995GOLDIM, J.R. Pesquisa em saúde e direito dos animais. Porto Alegre: HCPA, 1995. 28p.).
Datas de Publicação
-
Publicação nesta coleção
Mar 2015
Histórico
-
Recebido
12 Abr 2013 -
Aceito
12 Maio 2014