ABSTRACT
Objective:
to identify what is discussed in studies published in Brazilian and international literature in the last ten years on Primary Health Care management.
Method:
an integrative review with a search carried out from 2006 to 2016, in the SciELO®, LILACS®, Scopus®, PubMed® and CINAHL® databases in the Portuguese, English and Spanish languages. The review followed the steps: formulation of the research question, definition of the inclusion and exclusion criteria, identification and selection of the studies, and summary of the subjects found in the studies. Resources from The Atlas.ti® software was used for data organization and analysis.
Results:
the corpus include 90 studies which predominantly originated from LILACS® and were performed in Brazil. The themes covered in the publications were: health policy and management in Primary Health Care, material resources management, human resources management, financial management, quality management, planning, characterization of managers, management role/ activities, challenges/difficulties in management, potentialities/facilities in management. There was a prevalence of studies that dealt with Primary Health Care management in the context of reflections on health policies and those dealing with the challenges/difficulties faced in Primary Health Care management. These findings demonstrate that the Primary Health Care model is complex and challenging, both for policymakers and for those managing it.
Conclusion:
the number of studies on Primary Health Care management is significant in the current literature and the predominance of health policy and difficulties in performing management issues reinforce the recognition of the centrality of the management for effective Primary Health Care.
DESCRIPTORS:
Health management; Health administration; Administration of health services; Primary health care; Family health strategy
RESUMEN
Objetivo:
identificar lo que abordan los estudios publicados en la literatura nacional e internacional, en los últimos diez años, sobre gestión en la Atención Primaria a la Salud.
Método:
revisión integradora con la búsqueda realizada en el período de 2006 a 2016, en bases de datos, SciELO® LILACS®, Scopus®, PubMed y CINAHL, en portugués, Inglés y Español. Se siguiron las etapas: elaboración de la pregunta de investigación, definición de los criterios de inclusión y exclusión, identificación y selección de los estudios, y síntesis de los asuntos encontrados en los estudios. Para la organización y análisis de datos se utilizaron recursos del software Atlas.ti®.
Resultados:
el corpus de la encuesta totalizó 90 estudios, predominando los oriundos del LILACS® y realizados en Brasil. Los temas tratados en las publicaciones fueron: política de salud y gestión en la Atención Primaria a la Salud, gestión de recursos materiales, gestión de personas, gestión financiera, gestión de la calidad, planificación, caracterización de los gestores, papel/actividades de la gestión, desafíos/dificultades en gestión, potencialidades/facilidades en la gestión. En el contexto de las reflexiones sobre política de salud y los que se ocupan de los desafíos/dificultades enfrentadas en la gestión en la Atención Primaria a la Salud, los hallazgos señalan que el modelo de atención en la Atención Primaria a la Salud es complejo y desafiador, tanto para formuladores de políticas y para quien realiza la gestión.
Conclusión:
el número de estudios sobre gestión en la Atención Primaria a la Salud ha sido significativo en la literatura actual y la predominancia de los temas políticos de salud y dificultades para la realización de la gestión refuerza el reconocimiento de la centralidad de la misma para la efectividad de la Atención Primaria a la Salud.
DESCRIPTORES:
Gestión en salud; Administración en salud; Administración de servicios de salud; Atención primaria a la salud; Estrategia de salud familiar
RESUMO
Objetivo:
identificar o que abordam os estudos publicados na literatura nacional e internacional, nos últimos dez anos, sobre gestão na Atenção Primária à Saúde.
Método:
revisão integrativa com busca realizada no período de 2006 a 2016, nas bases de dados SciELO®, LILACS®, Scopus®, PubMed® e CINAHL®, nos idiomas português, inglês e espanhol. Seguiram-se as etapas: elaboração da pergunta de pesquisa, definição dos critérios de inclusão e exclusão, identificação e seleção dos estudos, e síntese dos assuntos encontrados nos estudos. Para organização e análise de dados utilizou-se recursos do software Atlas.ti®.
Resultados:
o corpus da pesquisa totalizou 90 estudos, predominando os oriundos do LILACS® e realizados no Brasil. Os temas tratados nas publicações foram: política de saúde e gestão na Atenção Primária à Saúde, gestão de recursos materiais, gestão de pessoas, gestão financeira, gestão da qualidade, planejamento, caracterização dos gestores, papel/atividades da gestão, desafios/dificuldades na gestão, potencialidades/facilidades na gestão. Predominaram estudos que trataram da gestão na Atenção Primária Saúde no contexto das reflexões sobre política de saúde e os que tratam dos desafios/dificuldades enfrentadas na gestão na Atenção Primária à Saúde. Esses achados sinalizam que o modelo de atenção na Atenção Primária à Saúde é complexo e desafiador, tanto para formuladores de políticas quanto para quem realiza a gestão.
Conclusão:
o número de estudos sobre gestão na Atenção Primária à Saúde tem sido significativo na literatura atual e a predominância dos temas políticas de saúde e dificuldades para a realização da gestão reforçam o reconhecimento da centralidade da mesma para a efetividade da Atenção Primária à Saúde.
DESCRITORES:
Gestão em saúde; Administração em saúde; Administração de serviços de saúde; Atenção primária à saúde; Estratégia saúde da família
INTRODUCTION
Primary Health Care (PHC) has been presented as the best form of organization for healthcare services, and the main entrance point for the Brazilian population to access health care. Its objective is to meet the needs of the population by considering efficiency and effectiveness.11. Mendes EV. O cuidado das condições crônicas na Atenção Primária à Saúde: o imperativo da consolidação da estratégia da saúde da família. [Internet] Brasília, DF: Organização Pan-americana da Saúde; 2012. [cited 2016 Apr 10], Available from: Available from: http://bvsms.saude.gov.br/bvs/publicacoes/cuidado_condicoes_atencao_primaria_saude.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
-22. Cueto M. Atenção Primária à Saúde. In: Cueto M. Saúde Global: uma breve história. Rio de Janeiro (RJ): Fiocruz; 2015: 53-76.
Positive results are constantly being achieved due to the conception and formulation of PHC such as: greater community participation in health care; reduction of mortality and diseases related to the lack of sanitary and economic conditions; and the development of preventive and health promotion measures.22. Cueto M. Atenção Primária à Saúde. In: Cueto M. Saúde Global: uma breve história. Rio de Janeiro (RJ): Fiocruz; 2015: 53-76.-55. Mendes EV. A construção social da Atenção Primária à Saúde. [Internet] Brasília, DF: Conselho Nacional de Secretários de Saúde - Conass; 2015. [cited 2016 Apr 10], Available from: Available from: http://www.conass.org.br/biblioteca/a-construcao-social-da-atencao-primaria-a-saude/
http://www.conass.org.br/biblioteca/a-co...
These results made PHC a reference in the modification of the health services, in Brazil and internationally. However, a number of challenges still exist regarding its effectiveness as a strategy to achieve health for all and remain cost-efficient for countries, ensuring comprehensive care at all levels of care, achieving a broader understanding of the population's health needs and reducing disparities between regions.66. Matta GC, Morosini MVG. Atenção Primária à Saúde. In: Fundação Oswaldo Cruz, Escola Politécnica de Saúde Joaquim Venâncio. Dicionário da Educação Profissional em Saúde. Rio de Janeiro: Fiocruz; 2009.
PHC in some European countries is identified as an outpatient service which aims to meet the acute health needs of people.7 In others, such as Brazil, it integrates a national policy aimed at organizing services to meet the needs of the population in the health area.11. Mendes EV. O cuidado das condições crônicas na Atenção Primária à Saúde: o imperativo da consolidação da estratégia da saúde da família. [Internet] Brasília, DF: Organização Pan-americana da Saúde; 2012. [cited 2016 Apr 10], Available from: Available from: http://bvsms.saude.gov.br/bvs/publicacoes/cuidado_condicoes_atencao_primaria_saude.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
While not requiring material technological resources that are excessively expensive, such as in secondary (medical specialties and complex exams) and tertiary (hospital) levels, the services performed in PHC are complex. It involves human relations, between workers in health care teams, between these and managers, between teams and users, between managers and the community.11. Mendes EV. O cuidado das condições crônicas na Atenção Primária à Saúde: o imperativo da consolidação da estratégia da saúde da família. [Internet] Brasília, DF: Organização Pan-americana da Saúde; 2012. [cited 2016 Apr 10], Available from: Available from: http://bvsms.saude.gov.br/bvs/publicacoes/cuidado_condicoes_atencao_primaria_saude.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
,88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015.
The terms management/administration are related to the knowledge applied in the management of health organizations and this management involves the actions of managing / administering care networks and care units in public and private spheres. Managing involves providing direct, unique care which often involves multiprofessional teams, and the various requirements necessary for health organizations to work.99. Lorenzetti J, Lanzoni GMM Assuiti LFC, Pires DEP, Ramos FRS. Health management in Brazil: dialogue with public and private managers. Texto Contexto Enferm [Internet]. 2014 [cited 2016 Apr 10]; 23(2):417-25. Available from: Available from: http://dx.doi.org/10.1590/0104-07072014000290013
http://dx.doi.org/10.1590/0104-070720140...
PHC is a challenge for management since it also involves typical dimensions of health management: people management (provision of workforce in number and qualification, and management of work relations); management of materials and processes (including structure, organizational flows, work processes, materials and equipment); and financial management; assumes the responsibility of providing universal, comprehensive, equitable, efficient and effective care that meets the health needs of the population.88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015.
PHC management in Brazil is the responsibility of the municipality and it is essential that it is organized in a way that guarantees the quality and resolution of health care.44. Lacaz FAC, Cortizo CT, Junqueira V, Santos APL, Vieira NP, Santos FS. Gestão do trabalho e tecnologia na Atenção Básica do Sistema Único de Saúde em municípios do Estado de São Paulo. In: Assunção AÁ, Brito J. Trabalhar na Saúde: experiências cotidianas e desafios para a gestão do trabalho e do emprego. Rio de Janeiro (RJ): Fiocruz ; 2011: 73-93.,88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015. The effective functioning of PHC, in part, is related to the understanding of the health needs of the population, the work processes involved, the management of the resources required and the provision of effective results.88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015.
A study conducted in Brazil with managers from the public and private sector highlights the insufficiency of financial resources and weaknesses in health management. It also highlighted that this last point is related to the professional inexperience in the area of management, the delay in the inclusion of new technologies that contribute to management processes and work organization; and even more significantly in the public sector, is related to the difficulties in overcoming impediments imposed by the legislation that hinders the necessary agility, and to the party and electoral influences on managers, which generates turnover and discontinuity of initiated processes, and demotivation of workers and professionals.99. Lorenzetti J, Lanzoni GMM Assuiti LFC, Pires DEP, Ramos FRS. Health management in Brazil: dialogue with public and private managers. Texto Contexto Enferm [Internet]. 2014 [cited 2016 Apr 10]; 23(2):417-25. Available from: Available from: http://dx.doi.org/10.1590/0104-07072014000290013
http://dx.doi.org/10.1590/0104-070720140...
According to the Alma-Ata Declaration and the Federal Constitution in 1988, health is recognized as a fundamental right of the population and must be guaranteed by the involvement of the three governmental spheres: federal, state and municipal.88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015.,1010. Conselho Nacional de Secretários de Saúde (BR). Direito à Saúde. Brasília, DF: Conass ; 2015. However, the adequate financing and professional training focused on social and health practices did not accompany this expansion nor the management, which has made it difficult to offer quality and effective services to the population.1010. Conselho Nacional de Secretários de Saúde (BR). Direito à Saúde. Brasília, DF: Conass ; 2015.
PHC management is complex due to the specificity of health and primary health care itself, as well as the characteristics that it shares with many works in the service sector involving intangibility, simultaneity between production and consumption, impossibility of storage, difficulty in standardization, importance of the human factor and difficulty in evaluating costs.1111. Spiller ES, ed. Gestão dos serviços de saúde. Rio de Janeiro: FGV; 2009.
With the intention of promoting knowledge on PHC management, this review aimed to identify what studies published in Brazilian and international literature discuss in relation to Primary Health Care management in the last ten years.
METHOD
An integrative literature review1212. Ganong L. Integrative reviews of nursing research. Res Nurs Health. 1987;10(1):1-11.Available from: https://doi.org/10.1002/nur.4770100103
https://doi.org/10.1002/nur.4770100103...
-1414. Mendes KDS, Silveira RCC, Galvão CM. Revisão integrativa: método de pesquisa para a incorporação de evidencias na saúde e na enfermagem. Texto Contexto Enferm. 2008;17(4):758-764. Available from: https://doi.org/10.1590/S0104-07072008000400018
https://doi.org/10.1590/S0104-0707200800...
whose purpose is to select and analyze scientific studies on a given theme.
The methodological process consists of five stages: formulation of the research question; definition of the inclusion and exclusion criteria of the studies; identification and selection of studies; evaluation of selected studies and final inclusion; preparation of the summary of the studies and the subjects found in them. In order to ensure the integrity of the integrative review, a protocol1212. Ganong L. Integrative reviews of nursing research. Res Nurs Health. 1987;10(1):1-11.Available from: https://doi.org/10.1002/nur.4770100103
https://doi.org/10.1002/nur.4770100103...
,1515. Forte ECN. A satisfação no trabalho de enfermeiros/as em dois modelos assistenciais na atenção básica no Brasil. [dissertação] Florianópolis, SC: Programa de Pós-Graduação em Enfermagem, Universidade Federal de Santa Catarina; 2013. which was validated by an external researcher. Data collection was performed by two independent researchers (double blind modality), guided by the research question: what do the national and international studies discuss regarding the theme of Primary Health Care management?b
The initial search for identification of the studies occurred between April 26 and 30, in 2016 in Public/Publish Medline (PubMed) ®, Latin American and Caribbean Literature in Health Sciences (LILACS) ®, Scientific Electronic Library Online (SciELO)®, Scopus ® and Cumulative Index to Nursing and Allied Health Literature (CINAHL) ®. Search keys were developed for advanced research, based on the Health Sciences Descriptors (DeCS) and the Medical Subject Headings (MeSH) using the Boolean operators AND and OR. The terms used were: Gestão em Saúde/Health Management/Gestión en Salud; Administração em Saúde/Health Administration/Administración en Salud; Administração de Serviços de Saúde/Health Services Administration/ Administración de los Servicios de Salud; Atenção Primária à Saúde /Primary Health Care/Atención Primaria de Salud; Estratégia Saúde da Família/Family Health Strategy/Estrategia de Salud Familiar.
Full original scientific articles that contained the search terms in the title and/or abstract; published in the English, Spanish or Portuguese languages from 2006 to 2016; and which could be accessed by the Virtual Private Network (VPN) via the Federal University of Santa Catarina were included. The period of ten years from April 2006 to April 2016 is justified by the time that Primary Health Care became national policy in Brazil, under Ordinance No. 648, dated March 28, 2006, updated in 2011 and 2017.1616. Ministério da Saúde (BR). Portaria Nº 2.436, de 21 de setembro de 2017. Aprova a Política Nacional de Atenção Básica, estabelecendo a revisão de diretrizes para a organização da Atenção Básica, no âmbito do Sistema Único de Saúde (SUS). Diário Oficial da União 2017 Set 22 [cited 2017 Oct 18]. Available from: Available from: http://bvsms.saude.gov.br/bvs/saudelegis/gm/2017/prt2436_22_09_2017.html
http://bvsms.saude.gov.br/bvs/saudelegis...
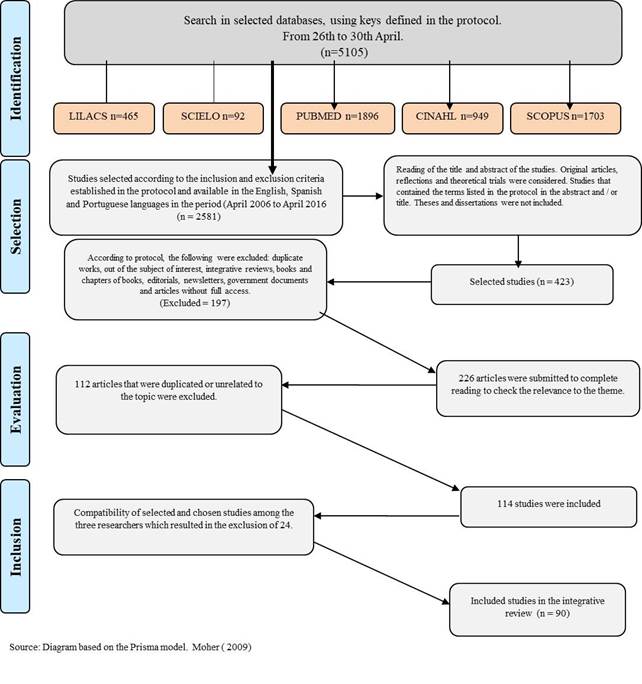
The first stage of the search resulted in 5105 articles from the five databases. When applying the language filters (English, Spanish or Portuguese) and period (2006 to 2016) the number of articles reduced to 2581, which then went to the study selection stage. At this point, the titles and abstracts were read and 423 articles were selected. Among these 423 articles, 197 were excluded as they were duplicated; outside the subject of interest; integrative reviews, editorials, newsletters, government documents or annals of congresses; and because they were not accessible in full, which resulted in a total of 226 articles.
In the evaluation stage, the 226 studies were submitted to a complete reading for the purpose of verification and relevance to the study theme, which resulted in 114 studies.
In the inclusion stage, the independent researchers agreed on the findings and concluded the final selection. In this stage, 24 papers were excluded because they were duplicated or did not answer the research question. The final corpus contained 90 articles.
The search process, selection and constitution of the corpus is shown in Figure 1
Methodological process of survey research in the integrative review, Florianópolis-SC, Brazil, 2017.1717. Moher DLA, Tetzlaff J, Altman DG. The PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009 Jul 21 [cited 2016 Apr 10]; 6(7): e1000097. Available from: Available from: https://doi.org/10.1371/journal.pmed.1000097
https://doi.org/10.1371/journal.pmed.100...
The submitted articles included in this review were organized according to article title, author, year, database, periodical and study site. For the last methodological step, the 90 articles included in the review, were stored in the Atlas.ti® software version 7.6.1, a tool that assists in the organization and qualitative analysis of data (Qualitative Research and Solutions), as primary documents in pdf format, and were evaluated and coded based on the purpose of this review.
For the analysis of each document, codes previously written in the software were formulated in order to help categorize the themes and subjects that the studies covered. The categories were: Health Policy; Material Resources Management; Characterization of Managers; People management; Financial management; Quality management; Planning; Paper/Management activities; Challenges/Difficulties in Management; Potentialities/Facilities in Management. Each document was then read and quotations were selected that identify each theme and sub-theme or subjects covered in each theme.
RESULTS
Regarding the type of study, the majority were descriptive qualitative studies, followed by mixed approach studies. Regarding the source, most articles were from the LILACS database, with 60%, followed by SciELO® with 17.78%, Scopus® with 12.22%, PubMed® with 7.78% and CINAHL® with 2.22%.
As for the publication period of the studies, there were more publications in the year 2014 with 18.89%; followed by the year 2010 with 16.67% and 2015 with 14.44%. The years 2009, 2011, 2012 and 2013 accounted for 10% for each year. The lowest number of publications occurred in the 2006, 2007, 2008, and 2016, respectively, with 1.11%, 2.22%, 3.33% and 3.33%. It should be observed, that the data for 2016 were only collected until April. Regarding the language, the Portuguese language predominated with 78.89%, followed by the English language with 11.11% articles, and the Spanish language with 10%.
Regarding the analysis of the study locations, the majority of the researches were performed in the American continent 86.67%. South America accounted for 85.56% of the publications, with 71 articles produced in Brazil, followed by Colombia with four, and Chile and Venezuela with one study in each country. 6.67% were produced and published in Europe, two of them originated in Portugal and two in Spain; England and Serbia produced one study each. Among the total of the studies, 3.33% were produced in the Asian continent, two originating from Lebanon and one from Pakistan. In addition, 2.22% of the productions came from the African continent. The lowest number of productions originated in Oceania region, 1.11%.
The results of the themes discussed in the literature on PHC management in the last ten years are organized in Box 1 and describe the thematic categories with the subjects related to them.
Subjects covered according to thematic category, in the period 2006-2016, Florianópolis-SC, Brazil, 2017
DISCUSSION
With regard to the publications on PHC management, it was verified that the number of manuscripts found in the last ten years was significant, reaffirming its importance in the health sector.99. Lorenzetti J, Lanzoni GMM Assuiti LFC, Pires DEP, Ramos FRS. Health management in Brazil: dialogue with public and private managers. Texto Contexto Enferm [Internet]. 2014 [cited 2016 Apr 10]; 23(2):417-25. Available from: Available from: http://dx.doi.org/10.1590/0104-07072014000290013
http://dx.doi.org/10.1590/0104-070720140...
,108108. Torres SFS, Belisario SA, Melo EM. The emergency network in the northern macro-region of Minas Gerais, Brazil: a case study. Saude Soc [Internet]. 2015 [cited 2017 Sep 04]; 24(1):361-73. Available from: Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-12902015000100361&lng=pt&nrm=iso
http://www.scielo.br/scielo.php?script=s...
-109109. Pires DEP, Machado RR, Soratto J, Scherer MA, Gonçalves ASR, Trindade LL. Nursing workloads in family health: implications for universal access. Rev Latino-am Enfermagem [Internet]. 2016 [cited 2017 Sep 04]; 24:e2682. Available from: Available from: https://doi.org/10.1590/1518-8345.0992.2682
https://doi.org/10.1590/1518-8345.0992.2...
This issue is relevant since policy-making and the healthcare practice are mediated by management. It involves aspects related to the coordination of collective work, as well as the provision of practice environments, including a complex range of elements that influence the efficiency and effectiveness of services.
The health policy category was the one that most stood out in the articles published on PHC management in the studied period. This finding can be explained by increasingly intense international debate on the universalization of access to health and the centrality that has been given to PHC in order to countries achieve this goal.109109. Pires DEP, Machado RR, Soratto J, Scherer MA, Gonçalves ASR, Trindade LL. Nursing workloads in family health: implications for universal access. Rev Latino-am Enfermagem [Internet]. 2016 [cited 2017 Sep 04]; 24:e2682. Available from: Available from: https://doi.org/10.1590/1518-8345.0992.2682
https://doi.org/10.1590/1518-8345.0992.2...
-112112. Frenk J. Leading the way towards universal health coverage: a call to action. Lancet. 2015;385(9975):1352-1358. https://doi.org/10.1016/S0140-6736(14)61467-7
https://doi.org/10.1016/S0140-6736(14)61...
The profile of publications highlights the significant number of articles found in the LILACS database and articles performed in Brazil. This prominence can be explained by the growth of PHC in the last decade.
The Family Health Program, established in 1994, was later named the Family Health Strategy, which became a national policy in 2006, reaffirmed in the new editions of the National Policy on Primary Care (PNAB) in 20111616. Ministério da Saúde (BR). Portaria Nº 2.436, de 21 de setembro de 2017. Aprova a Política Nacional de Atenção Básica, estabelecendo a revisão de diretrizes para a organização da Atenção Básica, no âmbito do Sistema Único de Saúde (SUS). Diário Oficial da União 2017 Set 22 [cited 2017 Oct 18]. Available from: Available from: http://bvsms.saude.gov.br/bvs/saudelegis/gm/2017/prt2436_22_09_2017.html
http://bvsms.saude.gov.br/bvs/saudelegis...
and 2017.
In Brazil, after the Federal Constitution of 1988, which defined health as a universal right and duty of the state, tension began between advocates of neoliberal policy and of constitutional precept, influencing the sense of universal access. It is worth highlighting that, as of 2006, the creation and significant investment in PNAB, a Brazilian expression for PHC, expanded to cover 64.6% of the population in 2016113113. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Histórico de cobertura da saúde da família [Internet] [cited 2017 Sep 04]. Available from: Available from: http://dab.saude.gov.br/dab/historico_cobertura_sf/historico_cobertura_sf_relatorio.php
http://dab.saude.gov.br/dab/historico_co...
incorporating precepts which approached a new healthcare model.114114. Soratto J, Pires DEP, Dornelles S, Lorenzetti J. Family health strategy: a technological innovation in health. Texto Contexto Enferm [Internet]. 2015 [cited 2017 Ago 28]; 24(2):584-92. Available from: Available from: https://doi.org/10.1590/0104-07072015001572014
https://doi.org/10.1590/0104-07072015001...
There is a significant agreement in relation to the importance of PHC to the universalization of the right to health. However, its implementation has been difficult, which is similar to that found by PHC scholars as well as the scholars of this research.115115. Santos NR. SUS, política pública de Estado: seu desenvolvimento instituído e instituinte e a busca de saídas. Ciênc Saúde Coletiva [Internet]. 2013 [cited 2017 Ago 28]; 18(1):273-80. Available from: Available from: https://doi.org/10.1590/S1413-81232013000100028
https://doi.org/10.1590/S1413-8123201300...
Many publications discuss management in the context of historical analyses and how PHC is being organized, how policies are included and what the repercussions of these policies are regarding the access of users to the health system.
Studies that discussed the analysis of the implementation of PHC and its evaluation as a policy, those that addressed policy evaluation instruments, those that dealt with comprehensiveness assessment and the health care network, and those that addressed the issue of financing are highlighted.
Another highlight in the publications was the category of challenges and difficulties in PHC management, including human resources and material health deficits and the difficulties in offering access to healthcare services. The management of the services of public organizations is already a challenge,116116. Savassi LCM. Qualidade em serviços públicos: os desafios da Atenção Primária. Rev Bras Med Fam Comunidade [Internet]. 2012 [cited 2017 Ago 28]; 7(23):69-74. Available from: Available from: http://dx.doi.org/10.5712/rbmfc7(23)392
http://dx.doi.org/10.5712/rbmfc7(23)392...
coupled with the lack of human and material resources that influences the provision of health services.117117. Villela WV, Araújo EC, Ribeiro SA, et al. Desafios da atenção básica em saúde: a experiência de Vila Mariana, São Paulo, Brasil. Cad Saude Publica. 2009;25(6):1316-1324. Available from: https://doi.org/10.1590/S0102-311X2009000600014
https://doi.org/10.1590/S0102-311X200900...
-119119. Pinheiro ALS, Andrade KTS, Silva DO, Zacharias FCM, Gomide MFS, Pinto IC. Health management: the use of information systems and knowledge sharing for the decision making process. Texto Contexto Enferm [Internet]. 2016. Available from: https://doi.org/10.1590/0104-07072016003440015
https://doi.org/10.1590/0104-07072016003...
Other challenging factors for PHC management are inexperienced managers and training deficits in this area that influence the achievement of efficient and effective management; problems in the implementation of PHC itself and problems in the organization and working relationships; deficits in the availability of work instruments, especially those necessary for management work; and difficulties in evaluating the quality of services.
Another category found was quality management, highlighting studies that discuss instruments and models used for quality evaluation in health services, as well as studies that address the importance and challenges of implementing a quality assessment and evaluation policy within the scope of PHC including the evaluation of the performance of these services. These studies highlight the need for internal restructuring of the service and the creation of new methods of work organization or even new policies to improve the quality of care. The issue of quality evaluation in PHC has also been a concern in the macro-level of health management represented by the implementation of the National Program for Improving Access and Quality of Primary Health Care, under Ordinance No. 1,654 as of July 19, 2011 and 1,645 as of October 1, 2015.88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015..1010. Conselho Nacional de Secretários de Saúde (BR). Direito à Saúde. Brasília, DF: Conass ; 2015.
Studies that address the role and activities involved in health management, with an emphasis on the coordination of collectives, work organization, planning, team management and articulation of the local units work in the health care network are also identified in the publications included in this review. As well as a reference related to the use of the traditional management model in PHC, based on verticalized and bureaucratized relationships.
With regard to the profile of PHC managers, the presence of nurses and females predominated. In Brazil, although the National Policy of Basic Attention (Política Nacional de Atenção Básica -PNAB, in Portuguese) does not dictate that the management activity belongs to this professional, the same assumes these activities due to the technical-scientific foundation that the nursing undergraduate degree in the country provides. However, the presence of women and the nurse in this activity is not restricted to the findings in Brazilian studies.
Key managerial competencies in this area were identified such as communication, team management, planning with prioritization, problem solving, performance evaluation and leadership. This is also mentioned by other authors and in official documents.55. Mendes EV. A construção social da Atenção Primária à Saúde. [Internet] Brasília, DF: Conselho Nacional de Secretários de Saúde - Conass; 2015. [cited 2016 Apr 10], Available from: Available from: http://www.conass.org.br/biblioteca/a-construcao-social-da-atencao-primaria-a-saude/
http://www.conass.org.br/biblioteca/a-co...
,88. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015.
Not one of the 90 studies included in this review focused on Primary Health Care management, focused on the set of aspects inherent to management, including methods and models of planning, the various aspects involved in material and people management, quality management, financial management and care processes.
With regard to personnel management in PHC, the studies deal with the composition and qualification of the workforce, the work process and the organization of the professionals and show how the conditions and how the work is carried out influences the effectiveness of PHC. The workforce profile in PHC, as well as factors that influence the retention and turnover of professionals contributing to PHC instability, were also mentioned in a study performed in Lebanon.120120. Alameddine M, Saleh S, El-Jardali F, Dimassi H, Mourad Y. The retention of health human resources in primary healthcare centers in Lebanon: a national survey. BMC Health Serv Res [Internet]. 2012. Available from: https://doi.org/10.1186/1472-6963-12-419
https://doi.org/10.1186/1472-6963-12-419...
In relation to material and financial resources, the studies address the presence of technological deficits and deficits of work instruments, including the PHC environment, as well as financing deficits. Regarding planning, studies that addressed planning models and instruments used in planning management were identified.
The planning, material management, personnel management and financial management categories, reveal important aspects of management and are fundamental for the quality of PHC services. Although these categories do not appear to be the most prominent in this review, they are indispensable for the proper management and organization of healthcare services.
One article addressed the potentialities/facilities in management focusing on the strategies that facilitate the PHC service, such as the Family Health Support Center. The implementation of the Family Health Support Center in the scope of the Family Health Strategy aims to support the consolidation of PHC and has the potential to promote changes in work processes in the production of health care reflecting in primary health care management.
As a limitation of the study, we can cite the thematic categorization, as one of the articles could be put into different categories and, in this case, we chose to categorize by the predominant theme in each article that is part of the corpus of the research. In addition, the time frame, the chosen languages and databases are highlighted as possible limitations of the study.
CONCLUSION
The publications analysed demonstrate that the theme of PHC management is the subject of research and concerns in academia, reinforcing what has been mentioned by policymakers and health systems managers in Brazil and worldwide. Ultimately, good management in primary health care can increase access, the comprehensiveness of care and the best use of available resources.
This review identified a variation in the number of publications over the analysed years, highlighting 2014 as the year with the highest number of articles. The results also reveal that PHC management has been portrayed in national and international scientific articles, mainly in relation to its aspects related to health policy and the challenges of management practice.
On the other hand, the study identified gaps in the knowledge produced in this area, in particular: the absence of writings that approach primary health care management in a conceptual manner; the weaknesses of information systems as strategic resources for decision-making and for the instrumentalisation of social control.
REFERENCES
- 1. Mendes EV. O cuidado das condições crônicas na Atenção Primária à Saúde: o imperativo da consolidação da estratégia da saúde da família. [Internet] Brasília, DF: Organização Pan-americana da Saúde; 2012. [cited 2016 Apr 10], Available from: Available from: http://bvsms.saude.gov.br/bvs/publicacoes/cuidado_condicoes_atencao_primaria_saude.pdf
» http://bvsms.saude.gov.br/bvs/publicacoes/cuidado_condicoes_atencao_primaria_saude.pdf - 2. Cueto M. Atenção Primária à Saúde. In: Cueto M. Saúde Global: uma breve história. Rio de Janeiro (RJ): Fiocruz; 2015: 53-76.
- 3. Starfield B. Atenção primária: equilíbrio entre necessidade de saúde, serviços e tecnologia. Brasília (DF): UNESCO: Ministério da Saúde; 2004.
- 4. Lacaz FAC, Cortizo CT, Junqueira V, Santos APL, Vieira NP, Santos FS. Gestão do trabalho e tecnologia na Atenção Básica do Sistema Único de Saúde em municípios do Estado de São Paulo. In: Assunção AÁ, Brito J. Trabalhar na Saúde: experiências cotidianas e desafios para a gestão do trabalho e do emprego. Rio de Janeiro (RJ): Fiocruz ; 2011: 73-93.
- 5. Mendes EV. A construção social da Atenção Primária à Saúde. [Internet] Brasília, DF: Conselho Nacional de Secretários de Saúde - Conass; 2015. [cited 2016 Apr 10], Available from: Available from: http://www.conass.org.br/biblioteca/a-construcao-social-da-atencao-primaria-a-saude/
» http://www.conass.org.br/biblioteca/a-construcao-social-da-atencao-primaria-a-saude/ - 6. Matta GC, Morosini MVG. Atenção Primária à Saúde. In: Fundação Oswaldo Cruz, Escola Politécnica de Saúde Joaquim Venâncio. Dicionário da Educação Profissional em Saúde. Rio de Janeiro: Fiocruz; 2009.
- 7. Giovanella L. A atenção primária à saúde nos países da União Européia: configurações e reformas organizacionais na década de 1990. Cad Saude Publica. 2006;22(5):951-63. Available from: https://doi.org/10.1590/S0102-311X2006000500008
» https://doi.org/10.1590/S0102-311X2006000500008 - 8. Conselho Nacional de Secretários de Saúde (BR). A Atenção Primária e as Redes de Atenção à Saúde. Brasília, DF: Conass; 2015.
- 9. Lorenzetti J, Lanzoni GMM Assuiti LFC, Pires DEP, Ramos FRS. Health management in Brazil: dialogue with public and private managers. Texto Contexto Enferm [Internet]. 2014 [cited 2016 Apr 10]; 23(2):417-25. Available from: Available from: http://dx.doi.org/10.1590/0104-07072014000290013
» http://dx.doi.org/10.1590/0104-07072014000290013 - 10. Conselho Nacional de Secretários de Saúde (BR). Direito à Saúde. Brasília, DF: Conass ; 2015.
- 11. Spiller ES, ed. Gestão dos serviços de saúde. Rio de Janeiro: FGV; 2009.
- 12. Ganong L. Integrative reviews of nursing research. Res Nurs Health. 1987;10(1):1-11.Available from: https://doi.org/10.1002/nur.4770100103
» https://doi.org/10.1002/nur.4770100103 - 13. Whittemore R, Knafl K. The integrative review: updated methodology. J Adv Nurs. 2005;52(5):546-53. Available from: https://doi.org/10.1111/j.1365-2648.2005.03621.x
» https://doi.org/10.1111/j.1365-2648.2005.03621.x - 14. Mendes KDS, Silveira RCC, Galvão CM. Revisão integrativa: método de pesquisa para a incorporação de evidencias na saúde e na enfermagem. Texto Contexto Enferm. 2008;17(4):758-764. Available from: https://doi.org/10.1590/S0104-07072008000400018
» https://doi.org/10.1590/S0104-07072008000400018 - 15. Forte ECN. A satisfação no trabalho de enfermeiros/as em dois modelos assistenciais na atenção básica no Brasil. [dissertação] Florianópolis, SC: Programa de Pós-Graduação em Enfermagem, Universidade Federal de Santa Catarina; 2013.
- 16. Ministério da Saúde (BR). Portaria Nº 2.436, de 21 de setembro de 2017. Aprova a Política Nacional de Atenção Básica, estabelecendo a revisão de diretrizes para a organização da Atenção Básica, no âmbito do Sistema Único de Saúde (SUS). Diário Oficial da União 2017 Set 22 [cited 2017 Oct 18]. Available from: Available from: http://bvsms.saude.gov.br/bvs/saudelegis/gm/2017/prt2436_22_09_2017.html
» http://bvsms.saude.gov.br/bvs/saudelegis/gm/2017/prt2436_22_09_2017.html - 17. Moher DLA, Tetzlaff J, Altman DG. The PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009 Jul 21 [cited 2016 Apr 10]; 6(7): e1000097. Available from: Available from: https://doi.org/10.1371/journal.pmed.1000097
» https://doi.org/10.1371/journal.pmed.1000097 - 18. Melo LMF, Martiniano CS, Guimarães J, Souza MB, Rocha PM. Análises das diretrizes para o apoio institucional das gestões da Atenção Básica das capitais brasileiras. Saúde debate[Internet]. 2016 Mar [cited 2017 Oct 18]; 40(108):8-22. Available from: Available from: https://doi.org/10.1590/0103-1104-20161080001
» https://doi.org/10.1590/0103-1104-20161080001 - 19. Cardoso JR, Oliveira GN, Furlan PG. Gestão democrática e práticas de apoio institucional na Atenção Primária à Saúde no Distrito Federal, Brasil. Cad Saúde Pública [Internet]. 2016 [cited 2017 Oct 18]; 32(3):e00009315. Available from: Available from: http://dx.doi.org/10.1590/0102-311X00009315
» http://dx.doi.org/10.1590/0102-311X00009315 - 20. Santos AM, Giovanella L. Gestão do cuidado integral: estudo de caso em região de saúde da Bahia, Brasil. Cad Saúde Pública [Internet]. 2016 [cited 2016 Apr 10]; 32(3). Available from: Available from: http://dx.doi.org/10.1590/0102-311X00172214
» http://dx.doi.org/10.1590/0102-311X00172214 - 21. Cardoso AVL, Chain APN, Mendes RIP, Ferreira e Ferreira E, Vargas AMD, Martins AMEBL, et al. Assessment of the management of the Family Health Strategy via the tool Assessment for Quality Improvement in municipalities of Minas Gerais, Brazil. Ciênc Saúde Coletiva [Internet]. 2015 Apr [cited 2017 Oct 18]; 20(4):1267-84. Available from: Available from: http://dx.doi.org/10.1590/1413-81232015204.01832014
» http://dx.doi.org/10.1590/1413-81232015204.01832014 - 22. Ditterich RG, Zermiani TC, Moysés ST, Moysés SJ. A contratualização como ferramenta da gestão na Atenção Primária à Saúde na percepção dos profissionais da Secretaria Municipal de Saúde de Curitiba, Brasil. Saúde debate [Internet]. 2015 Dec [cited 2017 Oct 18]; 39(spe):207-20. Available from: Available from: http://dx.doi.org/10.5935/0103-1104.2015S005323
» http://dx.doi.org/10.5935/0103-1104.2015S005323 - 23. Fernandes JA, Figueiredo MD. Apoio institucional e cogestão: uma reflexão sobre o trabalho dos apoiadores do SUS Campinas. Physis [Internet]. 2015 Mar [cited 2017 Oct 18]; 25(1):287-306. Available from: Available from: https://doi.org/10.1590/S0103-73312015000100016
» https://doi.org/10.1590/S0103-73312015000100016 - 24. Lima SAV, Silva MRF, Carvalho EMF, Pessoa EÂC, Brito ESV, Braga JPR. Elementos que influenciam o acesso à atenção primária na perspectiva dos profissionais e dos usuários de uma rede de serviços de saúde do Recife. Physis [Internet]. 2015 Jun [cited 2017 Oct 18]; 25(2):635-56. Available from: Available from: https://doi.org/10.1590/S0103-73312015000200016
» https://doi.org/10.1590/S0103-73312015000200016 - 25. Magnago C, Pierantoni CR. Dificuldades e estratégias de enfrentamento referentes à gestão do trabalho na Estratégia Saúde da Família, na perspectiva dos gestores locais: a experiência dos municípios do Rio de Janeiro (RJ) e Duque de Caxias (RJ). Saúde debate [Internet]. 2015 Mar [cited 2017 Oct 18]; 39(104):9-17. Available from: Available from: http://dx.doi.org/10.1590/0103-110420151040194
» http://dx.doi.org/10.1590/0103-110420151040194 - 26. Miclos PV, Calvo MCM, Colussi CF. Avaliação do desempenho da Atenção Básica nos municípios brasileiros com indicador sintético. Saúde debate [Internet]. 2015 Dec [cited 2017 Oct 18]; 39(107):984-96. Available from: Available from: https://doi.org/10.1590/0103-110420151070386
» https://doi.org/10.1590/0103-110420151070386 - 27. Oliveira CM, Cruz MM, Kanso S, Reis AC, Lima A, Torres RMC, et al. Avaliabilidade do Programa de Valorização do Profissional da Atenção Básica (PROVAB): desafios para gestão do trabalho. Ciênc Saúde Coletiva [Internet]. 2015 Oct [cited 2017 Oct 18]; 20(10):2999-3010. Available from: Available from: http://dx.doi.org/10.1590/1413-812320152010.13322014
» http://dx.doi.org/10.1590/1413-812320152010.13322014 - 28. Volponi PRR, Garanhani ML, Carvalho BG. Núcleo de Apoio à Saúde da Família: potencialidades como dispositivo de mudança na Atenção Básica em saúde. Saúde debate[Internet]. 2015 Dec [cited 2017 Oct 18]; 39(spe):221-31. Available from: Available from: https://doi.org/10.5935/0103-1104.2015S005418
» https://doi.org/10.5935/0103-1104.2015S005418 - 29. Duarte MLC, Boeck JN. O trabalho em equipe na enfermagem e os limites e possibilidades da Estratégia Saúde da Família. Trab Educ Saúde [Internet]. 2015 [cited 2017 Oct 18]; 13(3):709-20. Available from: Available from: http://dx.doi.org/10.1590/1981-7746-sip00054
» http://dx.doi.org/10.1590/1981-7746-sip00054 - 30. Schimith MD, Brêtas ACP, Budó MLD, Alberti GF, Beck CLC. Gestión del trabajo: implicaciones para el cuidado en la Atención Primaria de Salud. Enferm Global [Internet]. 2015 [cited 2017 Oct 18]; 14(2). Available from: Available from: http://scielo.isciii.es/pdf/eg/v14n38/administracion2.pdf
» http://scielo.isciii.es/pdf/eg/v14n38/administracion2.pdf - 31. Sulti A DC, Lima RCD, Freitas PSS, Felsky CN, Galavote HS. O discurso dos gestores da Estratégia Saúde da Família sobre a tomada de decisão na gestão em saúde: desafio para o Sistema Único de Saúde. Saúde debate [Internet]. 2015 Mar [cited 2017 Oct 18]; 39(104):172-82. Available from: Available from: http://dx.doi.org/10.1590/0103-110420151040238
» http://dx.doi.org/10.1590/0103-110420151040238 - 32. Nyikuri M, Tsofa B, Barasa E, Okoth P, Molyneux S. Crises and resilience at the frontline-public health facility managers under devolution in a sub-county on the Kenyan Coast. PLoS One [Internet]. 2015 Dec 22 [cited 2017 Oct 18]; 10(12):e0144768. Available from: Available from: http://dx.doi.org/10.1371/journal.pone.0144768
» http://dx.doi.org/10.1371/journal.pone.0144768 - 33. Ney MS, Pierantoni CR, Lapão LVz. Sistemas de avaliação profissional e contratualização da gestão na Atenção Primária à Saúde em Portugal. Saúde debate [Internet]. 2015 Mar [cited 2017 Oct 18]; 39(104):43-55. Available from: Available from: http://dx.doi.org/10.1590/0103-110420151040266
» http://dx.doi.org/10.1590/0103-110420151040266 - 34. Bazzo-Romagnolli AP, Gimenez-Carvalho B, Polo de Almeida-Nunes EFP. Gestão de unidade básica de saúde em municípios de pequeno porte: instrumentos utilizados, facilidades e dificuldades relacionadas. Rev Gerenc Polit Salud [Internet]. 2014 [cited 2017 Oct 18]; 13(27):168-80. Available from: Available from: https://doi.org/10.11144/Javeriana.rgyps13-27.gubs
» https://doi.org/10.11144/Javeriana.rgyps13-27.gubs - 35. Castanheira ERL, Nemes MIB, Zarili TFT, Sanine PR, Corrente JE. Avaliação de serviços de Atenção Básica em municípios de pequeno e médio porte no estado de São Paulo: resultados da primeira aplicação do instrumento QualiAB. Saúde debate [Internet]. 2014 Dec [cited 2017 Oct 18]; 38(103):679-91. Available from: Available from: https://doi.org/10.5935/0103-1104.20140063
» https://doi.org/10.5935/0103-1104.20140063 - 36. Carvalho BG, Peduzzi M, Nunes EFPA, Leite FS, Silva JAM. Gerência de unidade básica de saúde em municípios de diferentes portes: perfil e instrumentos gerenciais utilizados. Rev Esc Enferm USP [Internet]. 2014 Oct [cited 2017 Oct 18]; 48(5):907-14. Available from: Available from: http://dx.doi.org/10.1590/S0080-623420140000500018
» http://dx.doi.org/10.1590/S0080-623420140000500018 - 37. Maerschner RL, Bastos ENE, Gomes AMA, Jorge MSB, Diniz SAN. Apoio institucional - reordenamento dos processos de trabalho: sementes lançadas para uma gestão indutora de reflexões. Interface (Botucatu) [Internet]. 2014 [cited 2017 Oct 18]; 18(Suppl 1):1089-98. Available from: Available from: http://www.scielo.br/pdf/icse/v18s1/1807-5762-icse-18-1-1089.pdf
» http://www.scielo.br/pdf/icse/v18s1/1807-5762-icse-18-1-1089.pdf - 38. Ohira RHF, Cordoni Junior L, Nunes EFPA. Perfil dos gerentes de Atenção Primária à Saúde de municípios de pequeno porte do norte do Paraná, Brasil. Ciênc Saúde Coletiva [Internet]. 2014 Feb [cited 2017 Oct 18]; 19(2):393-400. Available from: Available from: http://www.scielo.br/pdf/csc/v19n2/1413-8123-csc-19-02-00393.pdf
» http://www.scielo.br/pdf/csc/v19n2/1413-8123-csc-19-02-00393.pdf - 39. Ohira RHF , Cordoni Junior L, Nunes EFPA . Análise das práticas gerenciais na Atenção Primária à Saúde nos municípios de pequeno porte do norte do Paraná, Brasil. Ciênc Saúde Coletiva [Internet]. 2014 Nov [cited 2017 Oct 18]; 19(11):4439-48. Available from: Available from: http://www.scielosp.org/pdf/csc/v19n11/1413-8123-csc-19-11-4439.pdf
» http://www.scielosp.org/pdf/csc/v19n11/1413-8123-csc-19-11-4439.pdf - 40. Rizzotto MLF, Gil CRR, Carvalho M, Fonseca ALN, Santos MF. Força de trabalho e gestão do trabalho em saúde: revelações da Avaliação Externa do Programa Nacional de Melhoria do Acesso e da Qualidade da Atenção Básica no Paraná. Saúde Debate [Internet]. 2014 Oct [cited 2017 Oct 18]; 38(spe):237-51. Available from: Available from: https://doi.org/10.5935/0103-1104.2014S018
» https://doi.org/10.5935/0103-1104.2014S018 - 41. Rolim-Ensslin S, Dutra A, Souza-Duarte C, Bortoluzzi SC, Ripoll-Feliu VM. A avaliação de desempenho como proposta para gestão das equipes do programa brasileiro “Estratégia da Saúde da Família”. Rev Gerenc Polit Salud [Internet]. 2014 [cited 2017 Oct 18]; 13(26):10-25 Available from: Available from: Available from: Available from: http://www.scielo.org.co/pdf/rgps/v13n26/v13n26a02.pdf
» http://www.scielo.org.co/pdf/rgps/v13n26/v13n26a02.pdf - 42. Sales NC, Silva MGC, Pinto FJM. Competências essenciais desenvolvidas por coordenadores de Centros de Saúde da Família. Rev Bras Promo Saúde [Internet]. 2014 [cited 2017 Sep 04]; 27(3). Available from: Available from: http://periodicos.unifor.br/RBPS/article/view/2473/pdf
» http://periodicos.unifor.br/RBPS/article/view/2473/pdf - 43. Costa e Silva V, Escoval A, Hortale VA. Contratualização na Atenção Primária à Saúde: a experiência de Portugal e Brasil. Ciênc Saúde Coletiva [Internet]. 2014 Aug [cited 2017 Oct 18]; 19(8):3593-604. Available from: Available from: https://doi.org/10.1590/1413-81232014198.11822013
» https://doi.org/10.1590/1413-81232014198.11822013 - 44. Fracolli LA, Gomes MFP, Gryschek ALFPL. Percepções de gestores municipais sobre ações de promoção da saúde: em foco os agentes comunitários de saúde. Saude Soc [Internet]. 2014 Sep [cited 2017 Oct 18]; 23(3):919-27. Available from: Available from: https://doi.org/10.1590/S0104-12902014000300015
» https://doi.org/10.1590/S0104-12902014000300015 - 45. Pereira LP, Nery AA. Planning, management and actions of men’s health in the family health strategy. Esc Anna Nery [Internet]. 2014 Dec [cited 2017 Oct 18]; 18(4):635-43. Available from: Available from: Available from: Available from: https://doi.org/10.5935/1414-8145.20140090
» https://doi.org/10.5935/1414-8145.20140090 - 46. Visagie S, Schneider M. Implementation of the principles of primary health care in a rural area of South Africa. Afr J Prim Health Care Fam Med [Internet]. 2014 Feb 18 [cited 2017 Oct 18]; 6(1):E1-E10. Available from: Available from: https://doi.org/10.4102/phcfm.v6i1.562
» https://doi.org/10.4102/phcfm.v6i1.562 - 47. El-Jardali F, Hemadeh R, Jaafar M, Sagherian L, El-Skaff R, Mdeihly R, Jamal D, Ataya N. The impact of accreditation of primary healthcare centers: successes, challenges and policy implications as perceived by healthcare providers and directors in Lebanon. BMC Health Serv Res[Internet]. 2014 Feb 25 [cited 2017 Oct 18];14:86Available from: Available from: https://doi.org/10.1186/1472-6963-14-86
» https://doi.org/10.1186/1472-6963-14-86 - 48. Casanova AO, Teixeira MB, Montenegro E. O apoio institucional como pilar na cogestão da atenção primária à saúde: a experiência do Programa TEIAS - Escola Manguinhos no Rio de Janeiro, Brasil. Ciênc Saúde Coletiva [Internet]. 2014 Nov [cited 2017 Oct 18]; 19(11):4417-26. Available from: Available from: http://www.scielo.br/pdf/csc/v19n11/1413-8123-csc-19-11-4417.pdf
» http://www.scielo.br/pdf/csc/v19n11/1413-8123-csc-19-11-4417.pdf - 49. Nickel DA, Calvo MCM, Natal S, Freitas SFT, Hartz ZMA. Desenvolvimento da capacidade avaliativa na gestão da atenção básica: um estudo de caso exemplar em Santa Catarina, Brasil, de 2008 a 2011. Cad Saúde Pública [Internet]. 2014 Apr [cited 2017 Oct 18]; 30(4):839-50. Available from: Available from: http://www.scielo.br/pdf/csp/v30n4/0102-311X-csp-30-4-0839.pdf
» http://www.scielo.br/pdf/csp/v30n4/0102-311X-csp-30-4-0839.pdf - 50. Nickel Daniela Alba, Natal Sonia, Hartz Zulmira Maria de Araújo, Calvo Maria Cristina Marino. O uso de uma avaliação por gestores da atenção primária em saúde: um estudo de caso no Sul do Brasil. Cad Saúde Pública [Internet]. 2014 Dec [cited 2017 Oct 18]; 30(12):2619-30. Available from: Available from: http://www.scielo.br/pdf/csp/v30n12/0102-311X-csp-30-12-02619.pdf
» http://www.scielo.br/pdf/csp/v30n12/0102-311X-csp-30-12-02619.pdf - 51. Feitosa RMM, Almeida ANS, Silva WF, Xavier MSM, Ramalho SKL, Rocha DJF. Enfermagem e gerenciamento da situação de saúde na Estratégia de Saúde da Família. Rev Baiana Enferm [Internet]. 2013 cited 2017 Oct 18]; 27(2). Available from: Available from: https://portalseer.ufba.br/index.php/enfermagem/article/view/6935/7159
» https://portalseer.ufba.br/index.php/enfermagem/article/view/6935/7159 - 52. Melo RC, Machado MÉ. Coordenação de unidades de saúde da família por enfermeiros: desafios e potencialidades. Rev Gaúcha Enferm [Internet]. 2013 Dec [cited 2017 Oct 18]; 34(4):61-7. Available from: Available from: https://doi.org/10.1590/S1983-14472013000400008
» https://doi.org/10.1590/S1983-14472013000400008 - 53. Pinto JM, Gerhardt TE. Práticas avaliativas na gestão da Atenção Básica à Saúde: estudo de caso em Camaquã e Canguçu. Rev Adm Pública [Internet]. 2013 [cited 2017 Oct 18]; 47(2):305-26. Available from: Available from: https://doi.org/10.1590/S0034-76122013000200002
» https://doi.org/10.1590/S0034-76122013000200002 - 54. Pedrosa JI, Sousa MF, Hamann EM, Rocha DG, Oliveira MAA. Quem participa em quê?: experiências de construção compartilhada no âmbito da cooperação Brasil - Canadá para o aperfeiçoamento da gestão na Atenção Primária à Saúde. Saude Soc [Internet]. 2013 Jun [cited 2017 Oct 18]; 22(2):629-41. Available from: Available from: http://www.scielo.br/pdf/sausoc/v22n2/v22n2a30.pdf
» http://www.scielo.br/pdf/sausoc/v22n2/v22n2a30.pdf - 55. Viegas SF, Penna CMM. Implicações da integralidade na gestão municipal em saúde. Rev Aps [Internet]. 2013 [cited 2017 Sep 04]; 16(2). Available from: Available from: https://aps.ufjf.emnuvens.com.br/aps/article/view/1802/713
» https://aps.ufjf.emnuvens.com.br/aps/article/view/1802/713 - 56. Aguilera SLVU, Franca BHS, Moyses ST, Moyses SJ. Articulação entre os níveis de atenção dos serviços de saúde na Região Metropolitana de Curitiba: desafios para os gestores. Adm Pública [Internet]. 2013 [cited 2017 Sep 04]; 47(4). Available from: Available from: https://doi.org/10.1590/S0034-76122013000400010
» https://doi.org/10.1590/S0034-76122013000400010 - 57. Akhtar-Danesh N, Valaitis R, O’Mara L, Austin P, Munroe V. Viewpoints about collaboration between primary care and public health in Canada. BMC Health Serv Res [Internet]. 2013 Aug 14 [cited 2017 Sep 04]; 13:311. Available from: Available from: https://doi.org/10.1186/1472-6963-13-311
» https://doi.org/10.1186/1472-6963-13-311 - 58. Goldstein RA, Barcellos C, Magalhães MAFM, Gracie R, Viacava F. A experiência de mapeamento participativo para a construção de uma alternativa cartográfica para a ESF. Ciênc Saúde Coletiva [Internet]. 2013 [cited 2017 Sep 04]; 18(1). Available from: Available from: https://doi.org/10.1590/S1413-81232013000100006
» https://doi.org/10.1590/S1413-81232013000100006 - 59. Mosquera PA, Hernández J, Vega R, Martínez J, Sebastián MS. Performance evaluation of the essential dimensions of the primary health care services in six localities of Bogota-Colombia: a cross-sectional study. BMC Health Serv Res [Internet]. 2013 Aug 15 [cited 2017 Sep 04]; 13:315. Available from: Available from: https://doi.org/10.1186/1472-6963-13-315
» https://doi.org/10.1186/1472-6963-13-315 - 60. Almeida DB, Melob CMM. Avaliação da gestão na Atenção Básica nas dimensões da integralidade. Rev Baiana Saúde Pública [Internet]. 2010 [cited 2017 Sep 04]; 24:75-80. Available from: Available from: https://portalseer.ufba.br/index.php/enfermagem/article/view/5530
» https://portalseer.ufba.br/index.php/enfermagem/article/view/5530 - 61. Scaratti D, Calvo MCM. Indicador sintético para avaliar a qualidade da gestão municipal da atenção básica à saúde. Rev Saúde Pública [Internet]. 2012 Jun [cited 2017 Oct 18]; 46(3):446-55. Available from: Available from: https://doi.org/10.1590/S0034-89102012000300006
» https://doi.org/10.1590/S0034-89102012000300006 - 62. Souza, RG. Rivemales MCC, Souza MKB. Sistema de Informaciónde laAtención Básica como instrumento de gestión: elstudo de caso em Santo Antônio de Jesus/BA. Online Br J Nurs [Internet]. 2012 [cited 2017 Sep 04]; 11(1). Available from: Available from: http://www.objnursing.uff.br/index.php/nursing/article/view/3552/html
» http://www.objnursing.uff.br/index.php/nursing/article/view/3552/html - 63. Vergara M, Bisama L, Moncada P. Competencias esenciales para la gestión en red. Rev méd Chile [Internet]. 2012 Dec [cited 2017 Oct 18]; 140(12):1593-605. Available from: Available from: https://doi.org/10.4067/S0034-98872012001200013
» https://doi.org/10.4067/S0034-98872012001200013 - 64. Pimenta AL. A construção de colegiados de gestão: a experiência de gestão da Secretaria Municipal de Saúde analisada por um ator político implicado. Saude soc [Internet]. 2012 May [cited 2017 Oct 18]; 21(Suppl 1):29-45. Available from: Available from: https://doi.org/10.1590/S0104-12902012000500003
» https://doi.org/10.1590/S0104-12902012000500003 - 65. Araújo CEL, Pontes RJS. Constituição de sujeitos na gestão em saúde: avanços e desafios da experiência de Fortaleza (CE). Ciênc Saúde Coletiva [Internet]. 2012 Sep [cited 2017 Oct 18]; 17(9):2357-65. Available from: Available from: http://www.scielo.br/pdf/csc/v17n9/a16v17n9.pdf
» http://www.scielo.br/pdf/csc/v17n9/a16v17n9.pdf - 66. Guimarães-Ximenes Neto FR, Coelho-Sampaio JJ. Análise do processo de trabalho dos gerentes no território da Estratégia Saúde da Família. Gerenc Polit Salud [Internet]. 2012 [cited 2017 Sep 04]; 11(22): Available from: Available from: http://www.scielo.org.co/pdf/rgps/v11n22/v11n22a07.pdf
» http://www.scielo.org.co/pdf/rgps/v11n22/v11n22a07.pdf - 67. Castelltort AL. ¿Autogestión o autonomía de gestión? Informe SESPAS 2012. Gaceta Sanitaria [Internet]. 2012 [cited 2017 Sep 04]; 26(10). Available from: Available from: http://www.gacetasanitaria.org/es/autogestion-o-autonomia-gestion-informe/articulo/S0213911111003918/
» http://www.gacetasanitaria.org/es/autogestion-o-autonomia-gestion-informe/articulo/S0213911111003918/ - 68. Andrade MCi, Castanheira ERL. Cooperação e apoio técnico entre estado e municípios: a experiência do programa articuladores da atenção básica em São Paulo. Saude Soc [Internet]. 2011 Dec [cited 2017 Oct 18]; 20(4):980-90. Available from: Available from: http://www.scielo.br/pdf/sausoc/v20n4/15.pdf
» http://www.scielo.br/pdf/sausoc/v20n4/15.pdf - 69. Berretta IQ, Lacerda JT, Calvo MCM. Modelo de avaliação da gestão municipal para o planejamento em saúde. Cad Saúde Pública [Internet]. 2011 Nov [cited 2017 Oct 18]; 27(11):2143-54. Available from: Available from: https://doi.org/10.1590/S0102-311X2011001100008
» https://doi.org/10.1590/S0102-311X2011001100008 - 70. Jonas LT, Rodrigues HC, Resck ZMR. A função gerencial do enfermeiro na Estratégia Saúde da Família: limites e possibilidades. Rev Aps [Internet]. 2011 [cited 2017 Sep 04]; 14(1): Available from: Available from: https://aps.ufjf.emnuvens.com.br/aps/article/view/977/443
» https://aps.ufjf.emnuvens.com.br/aps/article/view/977/443 - 71. Melo FAB, Goulart BF, Tavares DMS. Gerência em saúde: a percepção de coordenadores da estratégia saúde da família, em Uberaba-MG. Cienc Cuid Saúde [Internet]. 2011 [cited 2017 Sep 04]; 10(3). Available from: Available from: http://periodicos.uem.br/ojs/index.php/CiencCuidSaude/article/view/13261/pdf
» http://periodicos.uem.br/ojs/index.php/CiencCuidSaude/article/view/13261/pdf - 72. Trigueiro JVS, Nogueira JA, Sá LD, Palha PF, Villa TCS, Trigueiro DRSG. Controle da tuberculose: descentralização, planejamento local e especificidades gerenciais. Rev Latino-Am Enfermagem [Internet]. 2011 Dec [cited 2017 Oct 18]; 19(6):1289-96. Available from: Available from: http://www.scielo.br/pdf/rlae/v19n6/pt_03.pdf
» http://www.scielo.br/pdf/rlae/v19n6/pt_03.pdf - 73. Heimann LS, Ibanhes LC, Boaretto RC, Castro IEN, Telesi JúniorE, Cortizo CT, et al. Atenção primária em saúde: um estudo multidimensional sobre os desafios e potencialidades na Região Metropolitana de São Paulo (SP, Brasil). Ciênc Saúde Coletiva [Internet]. 2011 Jun [cited 2017 Oct 18]; 16(6):2877-87. Available from: Available from: http://www.scielo.br/pdf/csc/v16n6/25.pdf
» http://www.scielo.br/pdf/csc/v16n6/25.pdf - 74. Ruiz-Rodríguez M, Acosta-Ramírez N, Villamizar LAR, Uribe LM, León-Franco M. Experiencia de implementación de ver modelo de Atención Primaria. Rev Salud Pública [Internet]; 2011 [cited 2017 Sep 04]; 13(6):885-869. Available from: Available from: https://doi.org/10.1590/S0124-00642011000600002
» https://doi.org/10.1590/S0124-00642011000600002 - 75. shfaq M, Lodhi BK. Role of GIS in social sector planning: can developing countries benefit from the examples of Primary Health Care (PHC) planning in Britain? J Community Health [Internet]. 2012 Apr [cited 2017 Oct 18]; 37(2):372-82. Available from: Available from: https://link.springer.com/article/10.1007%2Fs10900-011-9454-7
» https://link.springer.com/article/10.1007%2Fs10900-011-9454-7 - 76. Alameddine M, Saleh S, El-Jardali F, Dimassi H, Mourad Y. The retention of health human resources in primary healthcare centers in Lebanon: a national survey. BMC Health Serv Res [Internet]. 2012 Nov 22 [cited 2017 Oct 18]; 12:419. Available from: Available from: https://doi.org/10.1186/1472-6963-12-419
» https://doi.org/10.1186/1472-6963-12-419 - 77. Rocha PM, Sá AB. Reforma da Saúde Familiar em Portugal: avaliação da implantação. Ciênc Saúde Coletiva [Internet]. 2011 Jun [cited 2017 Oct 18]; 16(6):2853-63. Available from: Available from: https://doi.org/10.1590/S1413-81232011000600023
» https://doi.org/10.1590/S1413-81232011000600023 - 78. Bosi MLM, Pontes RJS, Vasconcelos SM. Dimensões da qualidade na avaliação em saúde: concepções de gestores. Rev Saúde Pública [Internet]. 2010 Apr [cited 2017 Oct 18]; 44(2):318-24. Available from: Available from: https://doi.org/10.1590/S0034-89102010000200012
» https://doi.org/10.1590/S0034-89102010000200012 - 79. Bursztyn I, Kushnir R, Giovanella L, Stolkiner A, Sterman-Heimann L, Riveros MI, et al. Notas para el estudio de la Atención Primaria en contextos de sistemas de salud segmentados. Rev Salud Pública [Internet]. 2010;12(1):77-88. Available from: https://revistas.unal.edu.co/index.php/revsaludpublica/article/view/33500
» https://revistas.unal.edu.co/index.php/revsaludpublica/article/view/33500 - 80. Fernandes APP, Alexandre AMC, Dezoti AP, Mazza VA. A percepção do gestor sobre a organização da Atenção Básica à saúde da criança. Cogitare Enferm [Internet]. 2010 [cited 2017 Sep 04]; 15(1): Available from: Available from: http://revistas.ufpr.br/cogitare/article/viewFile/17140/11283
» http://revistas.ufpr.br/cogitare/article/viewFile/17140/11283 - 81. Müller EPL, Cubas MR, Bastos LC. Georreferenciamento como instrumento de gestão em unidade de saúde da família. Rev Bras Enferm [Internet]. 2010 Dec [cited 2017 Oct 18]; 63(6):978-82. Available from: Available from: https://doi.org/10.1590/S0034-71672010000600017
» https://doi.org/10.1590/S0034-71672010000600017 - 82. Pinto IC, Bulgarelli AF, Gomes TS, Figueiredo LA, Forster AC, Puime AO. Os sistemas de informação em atenção primária como instrumento de gestão em saúde: análise de experiências na Espanha. Cad Saúde Colet [Internet]. 2010 [cited 2017 Oct 18]; 18(2):291-7. Available from: Available from: http://www.cadernos.iesc.ufrj.br/cadernos/images/csc/2010_2/artigos/CSCv18n2_291-297.pdf
» http://www.cadernos.iesc.ufrj.br/cadernos/images/csc/2010_2/artigos/CSCv18n2_291-297.pdf - 83. Scalco SV, Lacerda JT, Calvo MCM. Modelo para avaliação da gestão de recursos humanos em saúde. Cad Saúde Pública [Internet]. 2010 Mar [cited 2017 Oct 18]; 26(3):603-14. Available from: Available from: https://doi.org/10.1590/S0102-311X2010000300017
» https://doi.org/10.1590/S0102-311X2010000300017 - 84. Silveira DS, Facchini LA, Siqueira FV, Piccini RX, Tomasi E, Thumé E, et al. Gestão do trabalho, da educação, da informação e comunicação na atenção básica à saúde de municípios das regiões Sul e Nordeste do Brasil. Cad Saúde Pública [Internet]. 2010 Sep [cited 2017 Oct 18]; 26(9):1714-26. Available from: Available from: https://doi.org/10.1590/S0102-311X2010000900005
» https://doi.org/10.1590/S0102-311X2010000900005 - 85. Junqueira TS, Cotta RMM, Gomes RC, Silveira SFR, Siqueira-Batista R, Pinheiro TMM, et al. As relações laborais no âmbito da municipalização da gestão em saúde e os dilemas da relação expansão/precarização do trabalho no contexto do SUS. Cad Saúde Pública [Internet]. 2010 May [cited 2017 Oct 18]; 26(5):918-28. Available from: Available from: http://www.scielo.br/pdf/csp/v26n5/14.pdf
» http://www.scielo.br/pdf/csp/v26n5/14.pdf - 86. Moura BLA, Cunha RC, Fonseca ACF, Aquino R, Medina MG, Vilasbôas ALQ, et al. Atenção primária à saúde: estrutura das unidades como componente da atenção à saúde. Rev Bras Saude Mater Infant [Internet]. 2010;10(Supl.1):S69-S81. Available from: https://doi.org/10.1590/S1519-38292010000500007
» https://doi.org/10.1590/S1519-38292010000500007 - 87. Barrêto AJR, Sá LD, Silva CC, Santos SR, Brandão GCG. Experiências dos enfermeiros com o trabalho de gestão em saúde no estado da Paraíba. Texto Contexto Enferm [Internet]. 2010 Jun [cited 2017 Oct 18]; 19(2):300-8. Available from: Available from: https://doi.org/10.1590/S0104-07072010000200011
» https://doi.org/10.1590/S0104-07072010000200011 - 88. Felisberto E, Freese E, Bezerra LCA, Alves CKA, Samico Ia. Análise da sustentabilidade de uma política de avaliação: o caso da atenção básica no Brasil. Cad Saúde Pública [Internet]. 2010 June [cited 2017 Oct 18]; 26(6):1079-95. Available from: Available from: http://www.scielo.br/pdf/csp/v26n6/03.pdf
» http://www.scielo.br/pdf/csp/v26n6/03.pdf - 89. Vieira JMR, Garnelo Luíza, Hortale Virginia Alonso. Análise da atenção básica em cinco municípios da amazônia ocidental, com ênfase no Programa Saúde da Família. Saude soc. [Internet]. 2010 Dec [cited 2017 Oct 18]; 19(4):852-65. Available from: Available from: http://www.scielo.br/pdf/sausoc/v19n4/12.pdf
» http://www.scielo.br/pdf/sausoc/v19n4/12.pdf - 90. Santric Milicevic MM, Bjegovic-Mikanovic VM, Terzic-Supic ZJ, Vasic V.2010 Competencies gap of management teams in primary health care. Eur J Public Health [Internet]. 2011 Apr [cited 2017 Oct 18]; 21(2):247-53. Available from: Available from: https://academic.oup.com/eurpub/article/21/2/247/495991/Competencies-gap-of-management-teams-in-primary
» https://academic.oup.com/eurpub/article/21/2/247/495991/Competencies-gap-of-management-teams-in-primary - 91. Silva NC, Garnelo L, Giovanella L. Extensão de cobertura ou reorganização da atenção básica? A trajetória do Programa de Saúde da Família de Manaus-AM. Saude soc. [Internet]. 2010 Sep [cited 2017 Oct 18]; 19(3):592-604. Available from: Available from: http://www.scielo.br/pdf/sausoc/v19n3/11.pdf
» http://www.scielo.br/pdf/sausoc/v19n3/11.pdf - 92. Castro ALB, Machado CV. A política de atenção primária à saúde no Brasil: notas sobre a regulação e o financiamento federal. Cad Saúde Pública [Internet]. 2010 Apr [cited 2017 Oct 18]; 26(4):693-705. Available from: Available from: https://doi.org/10.1590/S0102-311X2010000400012
» https://doi.org/10.1590/S0102-311X2010000400012 - 93. Fernandes LCL, Machado RZ, Anschau GO. Gerência de serviços de saúde: competências desenvolvidas e dificuldades encontradas na atenção básica. Ciênc Saúde Coletiva [Internet]. 2009 Oct [cited 2017 Oct 18]; 14(Suppl1):1541-52. Available from: Available from: https://doi.org/10.1590/S1413-81232009000800028
» https://doi.org/10.1590/S1413-81232009000800028 - 94. Soares RS, Rau B. Gestão compartilhada: Análise e reflexões sobre o processo de implementação em uma Unidade de Atenção Primária à Saúde do SUS. Rev Aps [Internet]. 2009 [cited 2017 Sep 04]; 12(4): Available from: Available from: https://aps.ufjf.emnuvens.com.br/aps/article/view/534/268
» https://aps.ufjf.emnuvens.com.br/aps/article/view/534/268 - 95. Sousa MF, Merchán-Hamann E. Saúde da Família no Brasil: estratégia de superação da desigualdade na saúde? Physis [Internet]. 2009 [cited 2017 Oct 18]; 19(3):711-29. Available from: Available from: http://www.scielo.br/pdf/physis/v19n3/a09v19n3.pdf
» http://www.scielo.br/pdf/physis/v19n3/a09v19n3.pdf - 96. Villela WV, Araújo EC, Ribeiro SA, Cuginotti AP, Hayana ET, Brito FC, et al. Desafios da atenção básica em saúde: a experiência de Vila Mariana, São Paulo, Brasil. Cad Saúde Pública [Internet]. 2009 Jun [cited 2017 Oct 18]; 25(6):1316-24. Available from: Available from: http://www.scielo.br/pdf/csp/v25n6/14.pdf
» http://www.scielo.br/pdf/csp/v25n6/14.pdf - 97. Bittar TO, Meneghim MC, Mialhe FL, Pereira AC, Fornazari DH. O Sistema de Informação da Atenção Básica como ferramenta da gestão em saúde. RFO [Internet]. 2009 [cited 2017 Sep 04]; 14(1). Available from: Available from: http://seer.upf.br/index.php/rfo/article/view/675/434
» http://seer.upf.br/index.php/rfo/article/view/675/434 - 98. Weirich CF, Munari DB, Mishima SM, Bezerra ALQ. O trabalho gerencial do enfermeiro na Rede Básica de Saúde. Texto Contexto Enferm [Internet]. 2009 Jun [cited 2017 Oct 18]; 18(2):249-57. Available from: Available from: http://www.scielo.br/pdf/tce/v18n2/07.pdf
» http://www.scielo.br/pdf/tce/v18n2/07.pdf - 99. Giovanella L, Mendonça MHM, Almeida PF, Escorel S, Senna MCM, Fausto MCR, et al. Saúde da família: limites e possibilidades para uma abordagem integral de atenção primária à saúde no Brasil. Ciênc Saúde Coletiva [Internet]. 2009 Jun [cited 2017 Oct 18]; 14(3):783-94. Available from: Available from: https://doi.org/10.1590/S1413-81232009000300014
» https://doi.org/10.1590/S1413-81232009000300014 - 100. Saliba NA, Moimaz SAS, Gonçalves PE, Lima DC, Santos JG. Gestión en salud em Brasil: La percepción de gestores y trabajadores de la salud sobre modelo de gestión y aspectos gerenciales Acta Odont Venez [Internet]. 2009 [cited 2017 Sep 04]; 47(2). Available from: Available from: https://www.actaodontologica.com/ediciones/2009/2/art-6/
» https://www.actaodontologica.com/ediciones/2009/2/art-6/ - 101. Bagley P, Lin V. The development and pilot testing of a rapid assessment tool to improve local public health system capacity in Australia. BMC Public Health [Internet]. 2009 Nov 15 [cited 2017 Oct 18]; 9:413. Available from: Available from: https://doi.org/10.1186/1471-2458-9-413
» https://doi.org/10.1186/1471-2458-9-413 - 102. Ramírez NA, Romero RV. El caso de la implementación de la estrategia de Atención Primaria Integral em la Salud (APIS) en la localidad de Suba, Bogotá - Colombia. Rev Gerenc Polit Salud [Internet]. 2008 [cited 2017 Oct 18]; Available from: Available from: http://revistas.javeriana.edu.co/index.php/gerepolsal/article/view/2684/12579
» http://revistas.javeriana.edu.co/index.php/gerepolsal/article/view/2684/12579 - 103. Ronzani TM, Silva CM. O Programa Saúde da Família segundo profissionais de saúde, gestores e usuários. Ciênc Saúde Coletiva [Internet]. 2008 Feb [cited 2017 Oct 18]; 13(1):23-34. http://www.scielo.br/pdf/csc/v13n1/06.pdf
» http://www.scielo.br/pdf/csc/v13n1/06.pdf - 104. Macq J, Martiny P, Villalobos LB, Solis A, Miranda J, Mendez HC, Collins C. Public purchasers contracting external primary care providers in Central America for better responsiveness, efficiency of health care and public governance: Issues and challenges. Health Policy [Internet]. 2008 Sep [cited 2017 Oct 18]; 87(3):377-88. Available from: Available from: https://doi.org/10.1016/j.healthpol.2008.01.007
» http://www.sciencedirect.com/science/article/pii/S0168851008000286 - 105. Vanderlei MIG, Almeida MCP. A concepção e prática dos gestores e gerentes da estratégia de saúde da família. Ciênc Saúde Coletiva [Internet]. 2007 Apr [cited 2017 Oct 18]; 12(2):443-53. Available from: Available from: https://doi.org/10.1590/S1413-81232007000200021
» https://doi.org/10.1590/S1413-81232007000200021 - 106. Ximenes Neto FRG, Sampaio JJC. Gerentes do território na Estratégia Saúde da Família: análise e perfil de necessidades de qualificação. Rev Bras Enfem [Internet]. 2007 [cited 2016 Apr 10]; 60(6). Available from: Available from: https://doi.org/10.1590/S0034-71672007000600013
» https://doi.org/10.1590/S0034-71672007000600013 - 107. Shaw S, Ashcroft J, Petchey R. Barriers and opportunities for developing sustainable relationships for health improvement: The case of public health and primary care in the UK. Critical Public [Internet]. 2006 [cited 2017 Sep 04]; 16(1):17-88. Available from: Available from: http://www.tandfonline.com/doi/abs/10.1080/09581590600602229?journalCode=ccph20
» http://www.tandfonline.com/doi/abs/10.1080/09581590600602229?journalCode=ccph20 - 108. Torres SFS, Belisario SA, Melo EM. The emergency network in the northern macro-region of Minas Gerais, Brazil: a case study. Saude Soc [Internet]. 2015 [cited 2017 Sep 04]; 24(1):361-73. Available from: Available from: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-12902015000100361&lng=pt&nrm=iso
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-12902015000100361&lng=pt&nrm=iso - 109. Pires DEP, Machado RR, Soratto J, Scherer MA, Gonçalves ASR, Trindade LL. Nursing workloads in family health: implications for universal access. Rev Latino-am Enfermagem [Internet]. 2016 [cited 2017 Sep 04]; 24:e2682. Available from: Available from: https://doi.org/10.1590/1518-8345.0992.2682
» https://doi.org/10.1590/1518-8345.0992.2682 - 110. World Health Organization (WHO). Global Health Workforce Alliance. Strategy 2013 - 2016: advancing the health workforce agenda within universal health coverage [Internet]. 2012 [cited 2017 Sep 04]. Available from: Available from: http://www.who.int/workforcealliance/en/
» http://www.who.int/workforcealliance/en/ - 111. Buss PM, Magalhães DP, Setti AFF, et al. Saúde na Agenda de Desenvolvimento pós-2015 das Nações Unidas. Cad Saude Publica. 2014;30(12):2555-2570. https://doi.org/10.1590/0102-311xat011214
» https://doi.org/10.1590/0102-311xat011214 - 112. Frenk J. Leading the way towards universal health coverage: a call to action. Lancet. 2015;385(9975):1352-1358. https://doi.org/10.1016/S0140-6736(14)61467-7
» https://doi.org/10.1016/S0140-6736(14)61467-7 - 113. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Histórico de cobertura da saúde da família [Internet] [cited 2017 Sep 04]. Available from: Available from: http://dab.saude.gov.br/dab/historico_cobertura_sf/historico_cobertura_sf_relatorio.php
» http://dab.saude.gov.br/dab/historico_cobertura_sf/historico_cobertura_sf_relatorio.php - 114. Soratto J, Pires DEP, Dornelles S, Lorenzetti J. Family health strategy: a technological innovation in health. Texto Contexto Enferm [Internet]. 2015 [cited 2017 Ago 28]; 24(2):584-92. Available from: Available from: https://doi.org/10.1590/0104-07072015001572014
» https://doi.org/10.1590/0104-07072015001572014 - 115. Santos NR. SUS, política pública de Estado: seu desenvolvimento instituído e instituinte e a busca de saídas. Ciênc Saúde Coletiva [Internet]. 2013 [cited 2017 Ago 28]; 18(1):273-80. Available from: Available from: https://doi.org/10.1590/S1413-81232013000100028
» https://doi.org/10.1590/S1413-81232013000100028 - 116. Savassi LCM. Qualidade em serviços públicos: os desafios da Atenção Primária. Rev Bras Med Fam Comunidade [Internet]. 2012 [cited 2017 Ago 28]; 7(23):69-74. Available from: Available from: http://dx.doi.org/10.5712/rbmfc7(23)392
» http://dx.doi.org/10.5712/rbmfc7(23)392 - 117. Villela WV, Araújo EC, Ribeiro SA, et al. Desafios da atenção básica em saúde: a experiência de Vila Mariana, São Paulo, Brasil. Cad Saude Publica. 2009;25(6):1316-1324. Available from: https://doi.org/10.1590/S0102-311X2009000600014
» https://doi.org/10.1590/S0102-311X2009000600014 - 118. Aguilera SLVU, França BHS, Moysés ST, Moysés SJ. Articulação entre os níveis de atenção dos serviços de saúde na Região Metropolitana de Curitiba: desafios para os gestores. Rev Adm Pública. 2013;47(4):1021-1040. Available from: https://doi.org/10.1590/S0034-76122013000400010
» https://doi.org/10.1590/S0034-76122013000400010 - 119. Pinheiro ALS, Andrade KTS, Silva DO, Zacharias FCM, Gomide MFS, Pinto IC. Health management: the use of information systems and knowledge sharing for the decision making process. Texto Contexto Enferm [Internet]. 2016. Available from: https://doi.org/10.1590/0104-07072016003440015
» https://doi.org/10.1590/0104-07072016003440015 - 120. Alameddine M, Saleh S, El-Jardali F, Dimassi H, Mourad Y. The retention of health human resources in primary healthcare centers in Lebanon: a national survey. BMC Health Serv Res [Internet]. 2012. Available from: https://doi.org/10.1186/1472-6963-12-419
» https://doi.org/10.1186/1472-6963-12-419
-
FUNDING INFORMATIONThis study was financed in part by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior - Brasil (CAPES) - Finance Code 001
Publication Dates
-
Publication in this collection
29 Apr 2019 -
Date of issue
2019
History
-
Received
29 Sept 2016 -
Accepted
09 Nov 2017