Abstracts
BACKGROUND: Gianotti-Crosti syndrome (GCS) is a rare, self-limited disease characterized by a symmetrical erythematopapulous, acral-based eruption. In most cases a definite relationship with a viral infection can be established, especially when hepatitis B or Epstein-Barr viruses are involved. However, few case reports on associations between GCS and human herpesvirus 6 (HHV6) have been published to date. OBJECTIVE: To study clinical and laboratorial aspects as well as to investigate the role of viral pathogens in the etiology of GCS cases from Belem (PA), Brazil. PATIENTS AND METHODS: From August 1996 to December 2002, ten children with a clinical diagnosis of GCS were investigated through routine laboratory exams and serologically screened for several virus specific antibodies. A diagnosis of GCS was considered for cases that presented clinical aspects considered suggestive, together with one or more of the following criteria: elevated titers of hepatic enzymes, lymphocytosis, positive viral serology or history of a prior vaccination. RESULTS: Six out of 10 children (60%) showed evidence of HHV6 primary infection, as demonstrated through specific IgM-antibody positivity. CONCLUSION: Anti-HHV6-IgM antibody positivity in 6/10 patients suggests that the pathogen can play a role in the etiology of GCS. Consequently, the authors recommend that this virus is added to the routine serological tests when exanthematous processes are concerned, especially those with a morphology suggestive of GCS.
acrodermatitis; hepatitis C antibodies; exanthema; herpesvirus 6, human
FUNDAMENTOS: A síndrome de Gianotti-Crosti (SGC) é uma doença rara e autolimitada caracterizada por erupção eritematopapulosa acrolocalizada e simétrica. Relaciona-se, na maioria das vezes, com infecção pelos vírus da hepatite B e Epstein-Barr, porém há poucas publicações relacionando a SGC com herpesvírus humano tipo 6 (HHV6). OBJETIVO: Estudar aspectos clínicos e laboratoriais e investigar a participação de patógenos virais na etiologia de casos de SGC procedentes de Belém-PA. PACIENTES E MÉTODOS: Dez crianças com diagnóstico clínico de SGC foram investigadas no período de agosto de 1996 a dezembro de 2002, utilizando-se provas laboratoriais de rotina e pesquisa de anticorpos séricos específicos para determinados vírus. O diagnóstico de SGC estabeleceu-se quando, além de aspectos clínicos considerados compatíveis, um ou mais dos seguintes critérios estavam presentes: elevação das enzimas hepáticas, linfocitose, positividade sorológica para um ou mais agentes virais ou história de vacinação prévia. RESULTADOS: Seis pacientes (60%) apresentaram evidência de infecção primária pelo HHV6 demonstrada pela presença de anticorpos específicos da classe IgM. CONCLUSÃO: A detecção de anticorpos anti-HHV6 da classe IgM em seis dos pacientes apresentados sugere um possível papel etiológico desse vírus na doença, recomendando-se que seja acrescentado ao painel sorológico rotineiramente pesquisado em processos exantemáticos com morfologia sugestiva de SGC.
acrodermatite; anticorpos anti-hepatite C; exantema; herpesvirus 6 humano
CLINICAL, EPIDEMIOLOGICAL, LABORATORY AND THERAPEUTIC INVESTIGATION
Gianotti-Crosti syndrome: clinical, laboratorial features, and serologic profiles of 10 cases from Belém, State of Para, Brazil* * Work done at Dermatology Service, Federal University of Pará (UFPA) and Hospital da Fundação Santa Casa de Misericórdia do Pará (HFSCMP) Av. Generalíssimo Deodoro, no 1, 66055-240 Belém-PA, Brazil.
Daniela A. LimaI; Daniela M. RochaII; Mario F. R. MirandaIII
IMD, Resident R3 of Dermatology, UFPA/HFSCMP
IIMD, dermatologist, ex-resident of Dermatology, UFPA/HFSCMP
IIIAdjunct professor 4 of Dermatology, UFPA
Correspondence Correspondence to Daniela Alves Lima Rua dos Pariquis no 1880 apt-302, Batista Campos Belém PA 66033 590 Tel: (91) 222-1741 Fax: (91) 224-6632 E-mail: danielaalveslima@ig.com.br
ABSTRACT
BACKGROUND: Gianotti-Crosti syndrome (GCS) is a rare, self-limited disease characterized by a symmetrical erythematopapulous, acral-based eruption. In most cases a definite relationship with a viral infection can be established, especially when hepatitis B or Epstein-Barr viruses are involved. However, few case reports on associations between GCS and human herpesvirus 6 (HHV6) have been published to date.
OBJECTIVE: To study clinical and laboratorial aspects as well as to investigate the role of viral pathogens in the etiology of GCS cases from Belem (PA), Brazil.
PATIENTS AND METHODS: From August 1996 to December 2002, ten children with a clinical diagnosis of GCS were investigated through routine laboratory exams and serologically screened for several virus specific antibodies. A diagnosis of GCS was considered for cases that presented clinical aspects considered suggestive, together with one or more of the following criteria: elevated titers of hepatic enzymes, lymphocytosis, positive viral serology or history of a prior vaccination.
RESULTS: Six out of 10 children (60%) showed evidence of HHV6 primary infection, as demonstrated through specific IgM-antibody positivity.
CONCLUSION: Anti-HHV6-IgM antibody positivity in 6/10 patients suggests that the pathogen can play a role in the etiology of GCS. Consequently, the authors recommend that this virus is added to the routine serological tests when exanthematous processes are concerned, especially those with a morphology suggestive of GCS.
Key-words: acrodermatitis; hepatitis C antibodies; exanthema; herpesvirus 6, human.
INTRODUCTION
Gianotti-Crosti syndrome (GCS) was described for the first time in 1955 by Gianotti as a papular, monomorphic eruption, self-limited, and symmetrically distributed in the face, in the gluteal area and in the extremities. It occurs in children from two to six years of age.1 In 1970, Gianotti and Crosti reported a relationship of this infection with hepatitis B virus.2 Later, cutaneous eruptions identical to those of GCS were observed without evidence of acute infection by hepatitis B virus. During the etiological investigation of the cases presented here, it was verified that these eruptions may be caused by various infectious agents, mainly viral (Table 1).2-18 In the literature consulted, there were only two references 5,7 to HHV6 as a cause of the disease.
The course of GCS is benign and self-limited, the manifestations disappearing within two to eight weeks, with no recurrence.3,4,6,7,10,14-16 The cutaneous lesions are generally asymptomatic, but exceptionally pruriginous.4,7,8,10,13,14,16 At times there are prodromes suggestive of an upper respiratory tract infection. General health status usually remains unaffected, although symptoms may occur such as indisposition, fever, nausea, vomiting, hepatosplenomegaly, lymphadenopathy and/or a picture of acute anicteric hepatitis. Lymphocytosis, with occasional presence of atypical lymphocytes in the peripheral blood, may also be observed.3,7-10,13-15
MATERIAL AND METHODS
From August 1996 to December 2002, a study was made of ten children in the city of Belem, with ages ranging between one month and ten years (mean: 2 years and 2 months), presenting acral-based papular eruptions with morphologic aspects compatible with GCS. Seven were boys and three, girls. The following laboratory exams were performed in each case: hemogram, ESR and hepatic function tests. Serology was performed for antibodies specific to the viruses EBV, HHV6, parvovirus B19, CMV, HBV, HAV, HCV, syncytial respiratory virus and rubella virus. Any exceptions to these procedures are described in Table 3. In six cases, biopsies of cutaneous lesions were collected and stained with hematoxylin and eosin (H-E). Histopathological aspects were not considered as diagnostic criteria, serving rather to exclude the possibility of other diseases. The diagnosis of GCS was established by a correlation between clinical and laboratorial factors. In addition to the clinical aspects considered compatible with this diagnosis, one or more of the following criteria were present: increase in hepatic enzyme levels, lymphocytosis with or without atypical lymphocytes or a mononucleosis-like syndrome, positive serologic results for one or more viral agents with indices of recent infection, and/or a history of recent vaccination. In the case attributed to HCV, it was considered to be a vertical transmission from mother to fetus, confirmed serologically, as a valid isolated criterion. Due to a lack of resources, molecular tests were not accomplished.
RESULTS
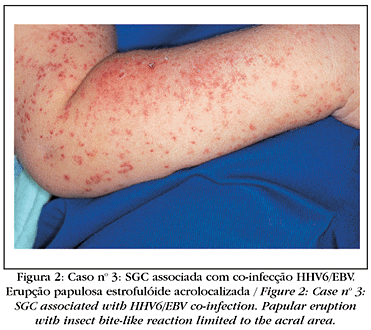
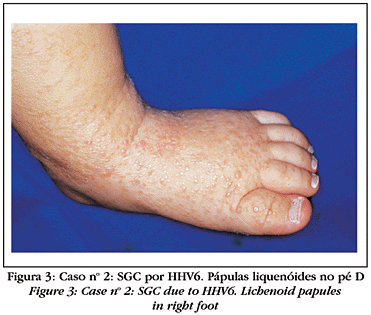
All the patients presented symmetrical cutaneous monomorphic eruptions, consisting of erythematous papules, brownish and at times lichenoid, with a diameter varying from 1 to 5 mm. These were predominantly located in the face (Figure 1) and limbs (Figures 2 and 3). The trunk was involved in nine cases, but generally with less intensity. Five patients complained of pruritus. Fever was observed in seven cases, lymphadenopathy in four and respiratory catarrhal manifestations in one. In all of the cases, spontaneous remission of the condition occurred within one week to six months (Table 2). During the course of the disease only systemic symptomatic medications were prescribed; including antihistaminic and antipyretic agents, when necessary. Lymphocytosis, occasionally with atypical lymphocytes, was observed in five cases. Transaminases presented a discreet elevation in four patients. An increase of bilirubin occurred only in the case related to hepatitis C. In two patients, high levels of alkaline phosphatase were also found. Microcytic and hypochromic anemia was observed in seven patients.
Table 3 shows the results of the serological viral tests. Antibodies against HHV6 of IgM class were present in six patients, one of which was associated with positivity to anti-EBV-IgM, suggesting a recent co-infection. In two cases, the serology was positive only to anti-EBV-IgM. Another child, with a HCV infected mother, presented a positive anti-HCV reaction. Patient number 5, whose possible etiology was attributed to the triple DPT vaccine, was only submitted to serologic testing for viral hepatitis. It is notable that, in all the patients, the tests for HBsAg and anti-HBc IgM lead to negative results.
DISCUSSION
A wide spectrum of infectious agents has been suspected to cause GCS (Table 1), with EBV figuring as the most frequent pathogen, followed by hepatitis B virus.3,7,13 Draelos19 did not observe any association of GCS with infection by HBV or EBV in nine children. Taieb17 studied a case attributed to an acute infection by HBV, three by coxsackie B, and seven cases by EBV among 26 children with GCS. Hofmann and col.9 observed five cases of infection by EBV among seven children with GCS. The results reported herein clearly support the role of a recent or acute infection by HHV6 in the etiology of GCS in 6/10 cases studied.
In the literature consulted, only two references were found associating HHV6 with GCS: Chuh and col., 20025 and Fölster-Holst, 1999.7 Chuh and col.5 investigated antibodies against HHV6 and HHV7, as well as molecular tests (PCR for viral DNA and RT-PCR for detection of mRNA transcriptions in the U91 gene of HHV6). This was done using the plasma and leukocytes from the peripheral blood of 10 patients diagnosed with GCS. Those authors observed that two patients (both children) presented evidence of an active infection by HHV6 and concluded that a primary HHV6 infection can be associated with this syndrome in children. In that same study, the serologic tests showed negative results for any recent infection by EBV or HBV.
The current spectrum of infectious agents associated with GCS may be influenced by epidemiological factors linked to the distribution of the viruses. Most of the patients with GCS produced by HBV, for instance, come from countries with a high prevalence of that pathogen, such as the Mediterranean Basin and Japan. Whereas investigations accomplished in areas with a relatively low prevalence of HBV, such as Eastern Europe and North America, have demonstrated a smaller role for HBV in the etiology of GCS.9
Salahuddin and col.20 isolated HHV6 for the first time in 1986, from the peripheral blood of patients with lymphoproliferative diseases and of those with acquired immunodeficiency syndrome. Since that time, serologic exams in several countries have demonstrated that infection by HHV6 is common and occurs both in children and in adults, with a serologic prevalence that varies from 45 to 63% in children and 52 to 97% in adults.21 Current knowledge relating to the epidemiology of HHV6 indicates that the primary infection occurs in childhood, usually before two years of age. Its form may be subclinical or it may cause exanthemas and lymphoproliferative disturbances. Freitas and col.,22 investigating the serologic prevalence (IgG) of HHV6 in 497 inhabitants of the urban area of Belem, with ages between seven months and 70 years, observed that infection by HHV6 is highly prevalent in that region. More than 90% of the children less than three years old presented antibodies for HHV6, which suggested that the primary infection had been acquired in early childhood. In another publication, those same authors, having accompanied, between January and December 1997, a total of 730 children under seven years of age registered at eight community day care centers in Belem, observed that infection by HHV6 had occurred in five out of every eight children during the studied period. They concluded that HHV6 infection is frequent among children in the area of Belem.21 Taking into consideration that epidemiological data, the authors of this work consider that tests for this pathogen should be included in the serologic panel alongside others considered to be possible agents. The fact that 60% of the cases presented here tested positive for anti-HHV6 IgM could, at least partly, reflect the high serologic prevalence levels in Belem observed by Freitas and col.22 However, considering the small number of examples in this report, future investigations will be necessary to validate these findings.
Case 1, a one-month-old infant, was born of a mother who was a carrier of HCV and presented positive serology for anti-HCV. The diagnosis of GCS in the infant, verified in a clinical-laboratorial correlation, suggested a probable vertical transmission of the infection. In this regard, three reports in the consulted literature relate hepatitis C virus with GCS.4,9,14 For another patient, a six-year-old boy, presenting an acute clinical picture that lasted five weeks, a possible causal relationship with DPT vaccine was suggested. The vaccine had been applied three months prior to the appearance of the symptoms. Such an association with vaccines shows strong corroboration in several published works, reporting that the cutaneous eruption occurs on average two to six weeks after the vaccination.3,8,9,11,13,18 However, this does not exclude the occasional participation of some other agent in the etiology of this case, since the serologic investigation was not complete, being restricted to hepatitis A, B and C.
Caputo and col.23 performed a retrospective analysis of 308 children diagnosed with GCS over a period of 35 years. They observed that the cases associated with HBV were clinically indistinguishable from those produced by any other agent. They suggested that clinical variations depended on the patients' individual characteristics rather than on different pathogens. In this way it is not possible a priori to attribute an etiological agent for each case, which in fact occurred in this series, in that six patients, with HHV6 as the cause, presented a certain diversity in the clinical-laboratorial manifestations.
The differential diagnosis should be made with the following: acute prurigo, scabies and other ectoparasitisms, granuloma annulare, atopic dermatitis, lichen planus, lichenoid drug eruption, lichen striatus, lichen nitidus, histiocytosis of Langerhans' cells, pityriasis lichenoides et varioliformis acuta (PLEVA), pityriasis rosea, papular urticaria, erythema multiforme, Henoch-Schönlein purpura, among others.7,8,13,15,16 Garcia and Vazquez8 do not agree with the statement that GCS is frequent in Europe and rare in Latin America. They suggest that pediatricians and dermatologists are possibly under-diagnosing the disease, since it can be easily confused with other papulovesicular illnesses of childhood.
The histopathological alterations are nonspecific and include focal parakeratosis, spongiosis, edema of the papillary dermis with leakage of erythrocytes and a superficial perivascular inflammatory lymphohistiocytic infiltrate; eventually a dermatitis of the superficial interface may be observed.4,7,8,13-16 In six patients, cutaneous biopsies were performed. The histopathological findings for three of these were in agreement with the available data in the consulted literature.
CONCLUSION
Several infectious agents have been proven to be capable of producing GCS, now HHV6 is an emerging pathogen. The association of this virus predominated in the research series presented here. The fact that this pathogen is highly prevalent in children, as shown by the results in the present work, indicates that it should be added to the panel of routine serologic tests in cases with a clinical picture suggestive of GCS.
ACKNOWLEDGEMENTS
To Dr. Ronaldo B. Freitas and Dr. Alexandre C. Linhares Virology Sector, Evandro Chagas Institution, Secretary of Health, Health Ministry, Belem, PA for the serological viral tests.
REFERENCES
Received on January 19, 2004
Approved by the Consultive Council and accepted for publication on October 30, 2004
- 1. Gianotti F. Rilievi di una particolare casistica tossinfettiva caratterizzata da un 'eruzione eritemato-infiltrativa desquamativa a focolai lenticolari, a sede elettiva acroposta. G Ital Dermatol. 1955;96:678-697.
- 2. Gianotti F. L'acrodermatite papulosa infantile "malattia". Gazz Sanitaria. 1970;41:271-274.
- 3. Baldari U, Monti A, Righini MG. An epidemic of infantile papular acrodermatitis (Gianotti-Crosti syndrome) due to Epstein-Barr virus. Dermatology. 1994;188:203-4.
- 4. Blauvelt A, Turner ML. Gianotti-Crosti Syndrome and human immunodeficiency virus infection. Arch Dermatol. 1994;130:481-3.
- 5. Chuh AA, Chan HH, Chiu SS, et al A prospective case control study of the association of Gianotti-Crosti syndrome with human herpesvirus 6 and human herpesvirus 7 infections. Pediatr Dermatol. 2002;19:492-7.
- 6. Drago F, Crovato F, Rebora A. Gianotti-Crosti syndrome as a presenting sign of EBV-induced acute infectious mononucleosis. Clin Exp Dermatol. 1997;22:301-2.
- 7. Fölster-Holst R, Christophers E. Exantheme im Kindesalter. Hautarzt. 1999;50:515-31.
- 8. Magaña-Garcia M, Vazquez R. Síndrome de Gianotti-Crosti. Bol Med Hosp Infant Mex. 1993;50:880-4.
- 9. Hofmann B, Schuppe HC, Adams O, et al Gianotti-Crosti syndrome associated with Epstein-Barr virus infection. Pediatr Dermatol. 1997;14:273-7.
- 10. Lendínez RH, Garcia LP, Garcia AA, et al Síndrome de Gianotti-Crosti debido a infección mixta producida por el vírus de la parotiditis y el virus parainfluenza tipo 2. An Esp Pediatr. 1996;44:65-6.
- 11. Mooney E, Kempf W. Gianotti-Crosti Syndrome (GCS) associated with poxvirus infection. Am J Dermatopathol. 2001;23:542.
- 12. Parsons ME, Russo GG, Millikan LE. Dermatologic disorders associated with viral hepatitis infections. Int J Dermatol. 1996;35:77-81.
- 13. Schopf RE. Gianotti-Crosti-Syndrom bei Epstein-Barr-Virus-Infektion. Hautarzt. 1995;46:714-6.
- 14. Smith KJ, Skelton H. Histopathologic features seen in Gianotti-Crosti syndrome secondary to Epstein-Barr virus. J Am Acad Dermatol. 2000;43:1076-9.
- 15. Stefanato CM, Goldberg LJ, Andersen WK, et al Gianotti-Crosti Syndrome presenting as lichenoid dermatitis. Am J Dermatopathol. 2000;22:162-5.
- 16. Stratte EG, Esterly NB. Human immunodeficiency virus and the Gianotti-Crosti syndrome. Arch Dermatol. 1995;131:108-9.
- 17. Taieb A. Gianotti-Crosti syndrome: a study of 26 cases. Br J Dermatol. 1986;115:49-59.
- 18. Velangi SS, Tidman MJ. Gianotti-Crosti syndrome after measles, mumps and rubella vaccination. Br J Dermatol. 1998;139:1122-3.
- 19. Draelos ZK. Gianotti-Crosti syndrome associated with infections other than hepatitis B. JAMA. 1986;259:2386-88.
- 20. Salahuddin SZ, Ablashi DV, Markham PD, et al Isolation of a new virus, HBLV, in patients with lymphoproliferative disordes. Science. 1986;234:596-601.
- 21. Freitas RB, Monteiro TAF, Linhares AC. Outbreaks of human-herpes virus 6 (HHV-6) infection in day-care centers in Belém, Pará, Brazil. Rev Inst Med trop S Paulo. 2000;42:305-311.
- 22. Freitas RB, Linhares AC. Prevalence of human herpesvírus 6 antibody in the population of Belém, Pará, northen Brazil. Trans roy Soc trop Med Hyg. 1997;91:538-40.
- 23. Caputo R, Gelmetti C, Ermacora E, et al Gianotti-Crosti syndrome: a retrospective analysis of 308 cases. J Am Acad Dermatol. 1992;26:207-210.
- 24. Campadelli-Fiume G, Mirandola P, Menotti L. Human herpesvirus 6: an emerging pathogen. Emerg Infect Dis. 1999;5:353-66.
- 25. Chuh AA. Diagnostic criteria for Gianotti-Crosti syndrome: a prospective case-control study for validity assessment. Cutis. 2001;68:207-13.
- 26. Freitas RB, Freitas MR, Linhares AC. Evidence of active herpesvirus 6 (variant-A) infection in patients with lymphadenophathy in Belém, Pará, Brazil. Rev Inst Med trop S Paulo. 2003;45:283-288.
- 27. Freitas RB, Linhares AC, Oliveira CS, et al Association of human herpesvirus 6 infection with exanthem subitum in Belém, Brazil. Rev Inst Med trop S Paulo. 1995;37:489-492.
- 28. Le Cleach L, Fillet AM, Agut H, et al Human herpesviruses 6 and 7: new roles yet to be discovered?. Arch Dermatol. 1998;134:1155-7.
Publication Dates
-
Publication in this collection
30 Mar 2005 -
Date of issue
Dec 2004
History
-
Accepted
30 Oct 2004 -
Received
19 Jan 2004