Abstracts
Background: Discoid lesion is the commonest cutaneous finding in lupus erythematosus and chronic types have their own immunological features, with Th1 inflammation profile. Although many diseases have association with blood-group systems, this fact was not enlightened in discoid lupus erythematosus. Objective: To investigate the association between blood groups (ABO and Rh) and discoid lupus erythematosus. Methods: A prospective cross-sectional study assessing clinical information, blood group systems (ABO and Rh), FAN and C4 serum levels from discoid lupus patients without characteristics of systemic disease, was carried out at a clinic from a Brazilian university hospital. Results: Sixty-nine patients were enrolled in the study, 71.0% were females (p1:160 in 31.9%, and low levels of C4 in 8.7%. There was no significant difference between the frequency of blood groups from discoid lupus patients and local population, however, blood group A was associated to disseminate forms of the disease (OR 4.1 and p < 0.05). Conclusions: Discoid lupus erythematosus patients with ABO and Rh blood groups exhibit similar frequencies as in the general population; nevertheless, disseminate clinical forms were more prevalent among group A patients.
ABO blood-group system; Epidemiology; Lupus erythematosus, discoid; Rh-Hr blood-group system
FUNDAMENTOS: Lesão discoide é a manifestação cutânea mais comum do lúpus eritematoso, e formas cutâneas crônicas apresentam características imunológicas próprias, direcionadas ao polo Th1. Diversas doenças possuem associação com grupos sanguíneos, o que não foi ainda estudado no lúpus discoide. OBJETIVO: Investigar a associação entre tipos sanguíneos (ABO e Rh) e lúpus eritematoso discoide. MÉTODOS: Estudo prospectivo tipo transversal envolvendo tipagem sanguínea ABO e Rh, inquérito de dados clínicos e dosagem de FAN e C4 de portadores de lúpus discoide sem critérios de doença sistêmica, atendidos em hospital universitário. RESULTADOS: Foram incluídos no estudo 69 pacientes, sendo 71,0% do sexo feminino (p 1:160, em 31,9%; e níveis baixos de C4, em 8,7%. Não houve diferença significativa entre as frequências dos grupos sanguíneos dos pacientes e da população local; entretanto, o grupo A foi associado às formas disseminadas da doença (OR 4,1 e p < 0,05). CONCLUSÕES: Grupos sanguíneos de pacientes com lúpus discoide apresentam frequência semelhante à da população; porém, formas clínicas disseminadas foram mais prevalentes entre portadores do grupo A.
Epidemiologia; Lúpus eritematoso discoide; Sistema do grupo sanguíneo ABO; Sistema do grupo sanguíneo Rh-Hr
INVESTIGATION
Blood groups and discoid lupus erythematosus
Andréia de Almeida TamegaI; Lílian Valéria Guerra da Silva Pinto BezerraII; Fabíola de Paula PereiraIII; Hélio Amante MiotIV
IIIResident Physician, Service of Dermatology, Faculdade de Medicina de Botucatu da Universidade Estadual Paulista (FMB-Unesp) Botucatu (SP), Brazil
IIIResident Physician, Service of Dermatology, Faculdade de Medicina de Botucatu da Universidade Estadual Paulista (FMB-Unesp) Botucatu (SP), Brazil
IVPh.D., Assistant Professor, Department of Dermatology and Radiotherapy, Faculdade de Medicina de Botucatu da Universidade Estadual Paulista (FMB-Unesp) Botucatu (SP), Brazil
Mailing AddressMailing Address: Hélio Amante Miot Departamento de Dermatologia, S/N Faculdade de Medicina da Unesp Campus Universitário de Rubião Jr. 18618 000 Botucatu SP Tel./fax: (14) 3882-4922 E-mail: heliomiot@fmb.unesp.br
ABSTRACT
BACKGROUND: Discoid lesion is the commonest cutaneous finding in lupus erythematosus and chronic types have their own immunological features, with Th1 inflammation profile. Although many diseases have association with blood-group systems, this fact was not enlightened in discoid lupus erythematosus.
OBJECTIVE: To investigate the association between blood groups (ABO and Rh) and discoid lupus erythematosus.
METHODS: A prospective cross-sectional study assessing clinical information, blood group systems (ABO and Rh), FAN and C4 serum levels from discoid lupus patients without characteristics of systemic disease, was carried out at a clinic from a Brazilian university hospital.
RESULTS: Sixty-nine patients were enrolled in the study, 71.0% were females (p< 0.01), mean age of disease onset was 32.8±13.1 years, and disseminate form occurred in 47.8%, smoking was related in 59.4%, FAN>1:160 in 31.9%, and low levels of C4 in 8.7%. There was no significant difference between the frequency of blood groups from discoid lupus patients and local population, however, blood group A was associated to disseminate forms of the disease (OR 4.1 and p < 0.05).
CONCLUSIONS: Discoid lupus erythematosus patients with ABO and Rh blood groups exhibit similar frequencies as in the general population; nevertheless, disseminate clinical forms were more prevalent among group A patients.
Keywords: ABO blood-group system; Epidemiology; Lupus erythematosus, discoid; Rh-Hr blood-group system
INTRODUCTION
Chronic discoid lupus erythematosus (CDLE) is the most common cutaneous manifestation that affects about 0.3% of the dermatological patients and presents epidemiological and immune specificities in comparison with the systemic forms. However, to present, its etiology is not completely known 1-3.
It is classically characterized by papules and erythematous infiltrate plaques that progress with central atrophy and desquamation and formation of hyperkeratotic spicules 2.
It affects primarily photoexposed areas of the face, neck region and upper limbs, but also the scalp, pinna, mucosa and extremities 1,2,4.
Cutaneous chronic forms occur more frequently in the age range between 20 and 40 years of age. There is predominance in female gender, in the proportion of 2-3:1, without preference for race 3.
The classification of CDLE, located and disseminated in the skin, was originally made by O'Leary in 1934 and it has been accepted by modern authors. It is considered to be localized if lesions are restricted to the head and neck and disseminated or generalized when, in addition to these, there are lesions on the trunk or limbs, regardless of the number. The importance of this classification is the observation of a greater risk of progression to systemic lupus erythematosus (SLE) in patients with lesions widely disseminated on the skin 4,5.
Serological exams, such as the investigation of circulating autoantibodies, which are extremely valuable in the diagnosis of SLE, are not important for the diagnosis of CDLE, used only for differential diagnosis with systemic forms and to detect possible manifestations of SLE 4,6,7.
As a model of cutaneous autoimmune disease pattern TH1, CDLE presents multifactorial etiological foundations of genetic basis 8. As phenotypic expressions may be studied to assess the gene segregation patterns, one of the characteristics that may be assessed are blood groups.9
Blood groups are cell surface antigens expressed according to well determined heritage patterns and are associated with incidence or prognosis of different diseases such as gastric carcinoma, small cell lung tumor, esophagus carcinoma, susceptibility to dermatophytosis, lichen planus, seborrheic dermatitis, systemic lupus erythematosus, breast cancer, among others 9-14.
There are over 30 proteins and sugars acknowledged as markers of blood groups, but the most antigenic ones comprise those that belong to system ABO and Rh(D), independently segregated in genes located in chromosomes 9q34 and 1p36.13-16
The authors intended to study the expression of blood groups (ABO and Rh) in patients with CDLE.
MATERIAL AND METHODS
We performed a prospective transversal study involving blood typing ABO and Rh, clinical history and FAN and C4 dosing in patients with CDLE without criteria for systemic disease, seen in the ambulatory of dermatology, Hospital das Clinicas, FMB-Unesp de Botucatu.17
Categorical data were represented as proportions, tested by chi-square test and residual analysis. The associations between variables were represented by odds ratio (OR) 18. Later, the co-variables were tested by a model of conditional multiple logistic regression using a stepwise-backward reduction algorithm adopted for the inclusion and exclusion criteria of variables p=0.2.
Data were compiled in MS Excel 2003 and analyzed with software SPSS 15.0.19 We considered as significant p value < 0.05.
RESULTS
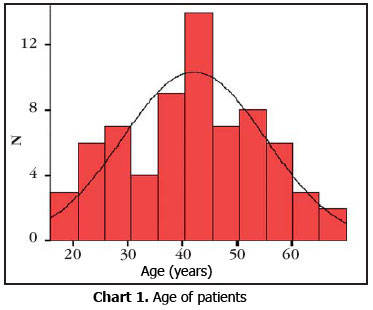
The study included 6 patients - 71% female (p < 0.01), producing a gender ratio of 2.5:1. Ages of patients and ages at onset of the disease are shown in Graphs 1 and 2, and the main clinical, epidemiological and laboratory data are shown in Table 1. As to topographical distribution of the lesion, we observed similar frequency between the localized and the disseminated forms (p>0.1), but the head was the most affected site in both clinical forms.
Smoking during the disease was detected in 59.4% of the patients, but there was no gender preference (p>0.1).
Positive FAN titles (>1:160) were associated with the disseminated form of the disease (OR 3.5; CI95% 1.2 to 9.9; p=0.01).
The frequency of blood types compared to regional expectation is shown in (Table 2)T. There was no statistically significant difference among blood group distribution in the patients and in the local population (p>0.1), even when stratified for groups ABO or Rh; however, group A was associated with the disseminated forms of the disease (OR 3.1; CI95% 1.2 to 8.3; p<0.05). We did no observe association between the blood groups and gender, smoking, FAN or C4 (p>0.1).
After multivariate analysis, positive Rh was associated with later onset of the disease (OR 1.3; CI95% 1.1 to 1.5; p < 0.01) and blood group A maintained its association with the disseminated forms (OR 4.1; CI95% 1.4 to 12. 3; p < 0.05).
DISCUSSION
We analyzed epidemiological, clinical and laboratory data of patients with CDLE seen in a teaching center in the countryside of Brazil, and the values we found were in agreement with the Brazilian literature 20-22.
Investigations of phenotypic expression in relation to diseases were preferably compared to local population standards, because regional genetic aspects may present differences among the people and even in different moments of history of the same given population 15,21,23.
In this study, blood types in the studied population who had European influence, showed proportions of positive Rh group and group A more frequent than reported in the literature; however, they were equivalent to the inquiries among regional blood donors 2,23.
The hypothesis of concomitant segregation of genes (genetic imbalance) or even antigenic expression and production of antibodies may be an explanation for the associations between blood types and many different diseases .9,11,13,15,24
Antigen A, identified in this study in association with disseminated disease, is expressed not only in red blood cells, but also on the surface of tissue nucleated cells. Patients in Group A still produce antibodies (isoagglutinins) against antigen B. Isoagglutinin produced as protein expression of cell membrane may justify the phenotypic patterns that are related with the more severe forms of discoid lupus 24.
Further studies should be carried out to assess the characteristics of discoid lupus in relation to other genes of chromosome 9q34, next to group A locus, as well as homology of oligossacharide A with nuclear antigens recognized in lupus erythematosus.
Disseminated forms are described as related with the greater prevalence of autoantibodies, greater therapeutic resistance and greater risk for systemic manifestation, configuring worse diagnosis .4-6, 21, 25
According to the literature, low levels of C4 are correlated with severity of lupus erythematosus and frequency of smoking, elements that were not confirmed with the sample in this study 21,26.
Finally, positive Rh groups were associated with late onset of the disease, indirectly indicating a factor of greater resistance to the development of lupus. The great predominance of positive groups Rh may result from the European descendant that characterizes the region 22. However, this aspect needs to be carefully assessed with a larger sample and adjusted to other confounding variables given that for example, socio-economic aspects are related with ethnic and professional characteristics in the country, and indirectly with the risk of chronic premature sun exposure.
CONCLUSION
Blood groups of patients with CDLE present frequency similar to that of the local population, but disseminated clinical forms were more prevalent among people with group A, suggesting a possible indicator of prognosis of the disease.
New studies should be carried out to assess the frequency of blood groups in different populations, assessing other variables as well as other subtypes of cutaneous lupus erythematosus.
REFERENCES
How to cite this article: Tamega AA, Bezerra LVGSP, Pereira FP, Miot HA. Grupos sanguíneos e lúpus eritematoso crônico discoide. An Bras Dermatol. 2009;84(5):477-81.
- 1. Werth VP. Clinical manifestations of cutaneous lupus erythematosus. Autoimmun Rev. 2005;4:296-302
- 2. Pramatarov KD. Chronic cutaneous lupus erythematosusclinical spectrum. Clin Dermatol. 2004;22:113-20
- 3. Prystowsky SD, Herndon JH Jr, Gilliam JN. Chronic cutaneous lupus erythematosus (DLE)--a clinical and laboratory investigation of 80 patients. Medicine (Baltimore) 1976;55:183-91
- 4. Patel P, Werth V. Cutaneous lupus erythematosus: a review. Dermatol Clin 2002;20:373-85
- 5. Prystowsky SD, Gilliam JN. Discoid lupus erythematosus as part of a larger disease spectrum. Correlation of clinical features with laboratory findings in lupus erythematosus. Arch Dermatol. 1975;111:1448-52
- 6. Prystowsky SD, Gilliam JN. Antinuclear antibody studies in chronic cutaneous discoid lupus erythematosus. Arch Dermatol. 1977;113:183-6
- 7. Millard LG, Rowell NR. Abnormal laboratory test results and their relationship to prognosis in discoid lupus erythematosus. A long-term follow-up study of 92 patients. Arch Dermatol. 1979;115:1055-8
- 8. Wenzel J, Wörenkämper E, Freutel S, Henze S, Haller O, Bieber T, et al Enhanced type I interferon signalling promotes Th1-biased inflammation in cutaneous lupus erythematosus. J Pathol. 2005;205:435-42
- 9. Macsween MP, Syme UA. Abo Blood Groups and Skin Diseases. Br J Dermatol 1965;77:30-4
- 10. Balajee SA, Menon T, Ranganathan S. ABO blood groups in relation to the infection rate of dermatophytosis. Mycoses. 1996;39:475-8
- 11. Holdsworth PJ, Thorogood J, Benson EA, Clayden AD. Blood group as a prognostic indicator in breast cancer. Br Med J (Clin Res Ed). 1985;290:671-3
- 12. Lee JS, Ro JY, Sahin AA, Hong WK, Brown BW, Mountain CF, Hittelman WN, et al Expression of blood-group antigen A-a favorable prognostic factor in non-small-cell lung cancer. N Engl J Med. 1991;324:1084-90
- 13. Tursen U, Tiftik EN, Unal S, Gunduz O, Kaya TI, Camdeviren H, et al Relationship between ABO blood groups and skin cancers. Dermatol Online J. 2005;11:44
- 14. Chakravartti MR. A statistical appraisal on the relationship between non-ABO blood group systems and diseases. Humangenetik. 1967;5:1-27
- 15. Kanbay M, Gür G, Arslan H, Yilmaz U, Boyacioglu S. The relationship of ABO blood group, age, gender, smoking, and Helicobacter pylori infection. Dig Dis Sci. 2005;50:1214-7
- 16. Ayatollahi H, Rafatpanah H, Khayyami ME, Sayyadpour D, Ravarian M, Sadeghian MH, et al Association between ABO and rhesus blood group systems among confirmed human T lymphotropic virus type 1-infected patients in northeast iran. AIDS Res Hum Retroviruses. 2008;24:1155-8
- 17. Albrecht J, Werth VP. Development of the CLASI as an outcome instrument for cutaneous lupus erythematosus. Dermatol Ther. 2007;20:93-101
- 18. Miot HA, Medeiros LM, Siqueira CRS, Cardoso LC, Gumieiro JH, Pandini Filho MA, et al Associação entre doença arterial coronariana e as pregas lobular diagonal e anterotragal em homens. An Bras Dermatol. 2006;81:29-33
- 19. Mushquash C, O'Connor BP. SPSS and SAS programs for generalizability theory analyses. Behav Res Methods. 2006;38:542-7
- 20. Freitas THP, Proença NG. Chronic cutaneous Lupus erythematosus: study of 290 patients. An Bras Dermatol. 2003;78:703-12
- 21. Miot HA, Bartoli Miot LD, Haddad GR. Association between discoid lupus erythematosus and cigarette smoking. Dermatology. 2005;211:118-22
- 22. Bortolozzi J, de Lucca EJ. [Distribution of ABO and Rh blood groups in Botucatu (Sao Paulo)]. Rev Paul Med. 1971;78:173-6
- 23. Curi PR, Kroll LB. [Determination of the sample size and distribution of the ABO and Rh blood groups in Botucatu, São Paulo, Brazil (author's transl)]. Rev Bras Pesqui Med Biol. 1976;9:129-35
- 24. Ottensooser F, Leon N, de Almeida TV. ABO blood groups and isoagglutinins in systemic lupus erythematosus. Rev Bras Pesqui Med Biol. 1975;8:421-5
- 25. Lipsker D, Boeckler P, Hauptmann G. Cigarette smoking and lupus erythematosus. Dermatology. 2006;212:262
- 26. Boeckler P, Milea M, Meyer A, Uring-Lambert B, Heid E, Hauptmann G, et al The combination of complement deficiency and cigarette smoking as risk factor for cutaneous lupus erythematosus in men; a focus on combined C2/C4 deficiency. Br J Dermatol. 2005;152:265-70
Publication Dates
-
Publication in this collection
07 Jan 2010 -
Date of issue
Oct 2009
History
-
Accepted
08 Dec 2009 -
Received
18 Aug 2009