Abstracts
BACKGROUND: Telemedicine can be defined as the use of telecommunication technologies for the transmission of health data. It has been described in different medical specialties, especially those in which interpretation of images represents a fundamental key in formulating diagnosis. OBJECTIVE: To evaluate the role of teledermatology in primary care system. METHODS: A prospective analysis included 60 patients seen in a primary care unit. All patients were seen by a dermatologist as regular outpatient dermatology consultation. A medical student obtained digital images and a brief clinical history of all patients. Using a Telemedicine system these data were reviewed by two dermatologists for distance diagnosis. Agreement between the diagnoses was assessed. RESULTS: Good agreement, ranging from 86.6% to 91.6%, was achieved between direct observation and teleconsultation. Good agreement was also achieved between two telemedicine diagnosis (Kappa = 0.62). CONCLUSION: Teledermatology is a form of care with great potential for use in dermatology, and could represent a useful tool in cases of low complexity from primary health units.
Diagnosis; Remote consultation; Telemedicine
FUNDAMENTOS: O termo telemedicina faz referência ao uso de tecnologias de comunicação para a transmissão a distância de informações relacionadas à saúde. Esse recurso é utilizado em várias especialidades médicas, principalmente naquelas em que a interpretação de imagens representa uma etapa fundamental na formulação diagnóstica. OBJETIVO: Avaliar a concordância entre o diagnóstico presencial e o diagnóstico a distância de lesões cutâneas, utilizando a teledermatologia, em pacientes atendidos em uma unidade básica de saúde. MÉTODOS: Foi realizado um estudo prospectivo envolvendo pacientes atendidos no serviço de dermatologia da clínica FTC em Salvador - BA. Participaram do estudo um dermatologista responsável pela consulta presencial e dois dermatologistas responsáveis pela consulta a distância. Os diagnósticos obtidos através da teleconsulta foram avaliados quanto à concordância e comparados com os diagnósticos da consulta presencial. RESULTADOS: Foram incluídos neste estudo 60 pacientes. Observou-se um grau de concordância total variando de 86,6% a 91,6% com índice Kappa de 0,62. CONCLUSÃO: A teledermatologia é uma forma de assistência com um grande potencial de uso na dermatologia, podendo representar uma ferramenta útil principalmente em casos clínicos de baixa complexidade, oriundos de unidades básicas de saúde.
Consulta remota; Diagnóstico; Telemedicina
INVESTIGATION
Teledermatology: diagnostic correlation in a primary care service
Cristiana Silveira SilvaI; Murilo Barreto SouzaII; Isabelle Ary DuqueIII; Luciana Molina de MedeirosIV; Nayra Rodrigues MeloV; Cecília de Almeida AraújoVI; Paulo Ricardo CriadoVII
IDermatologist, Master studies under course, Hospital das Clínicas, Medical School, Universidade de São Paulo (HCFMUSP) São Paulo (SP), Brazil
IIProfessor of Medical Computer Technology, Faculdade de Tecnologia e Ciências FTC - Salvador (BA), Brazil
IIIDermatologist Fortaleza (CE), Brazil
IVDermatologist São Paulo (SP), Brazil
VDermatologist Teresina (PI), Brazil
VIUndergraduate, School of Medicine, FTC - Salvador (BA), Brazil
VIIPh.D. in Dermatology, Universidade de São Paulo (USP) São Paulo (SP) - Brazil
Mailing Address Mailing Address: Cristiana Silveira Silva Rua da Graça, nº 374. Bairro Graça 40080 410 Salvador BA Tel.:/fax: 71 3336 2850 E-mail: silveira.cristiana@gmail.com
ABSTRACT
BACKGROUND: Telemedicine can be defined as the use of telecommunication technologies for the transmission of health data. It has been described in different medical specialties, especially those in which interpretation of images represents a fundamental key in formulating diagnosis.
OBJECTIVE: To evaluate the role of teledermatology in primary care system.
METHODS: A prospective analysis included 60 patients seen in a primary care unit. All patients were seen by a dermatologist as regular outpatient dermatology consultation. A medical student obtained digital images and a brief clinical history of all patients. Using a Telemedicine system these data were reviewed by two dermatologists for distance diagnosis. Agreement between the diagnoses was assessed.
RESULTS: Good agreement, ranging from 86.6% to 91.6%, was achieved between direct observation and teleconsultation. Good agreement was also achieved between two telemedicine diagnosis (Kappa = 0.62).
CONCLUSION: Teledermatology is a form of care with great potential for use in dermatology, and could represent a useful tool in cases of low complexity from primary health units.
Keywords: Diagnosis; Remote consultation; Telemedicine
INTRODUCTION
Telemedicine makes reference to the use of communication technologies for distance transmission of health-related information 1,2. In recent years, there has been an exponential growth of interest in the area. The number of published and indexed articles by Medline approached by telemedicine went from over 60 in the 90's to approximately 9,000 currently 3,4.
The use of Telemedicine has been described in many medical specialties, mainly in those in which imaging interpretation is a key step for diagnostic purposes 5,6,7. The use of this resource may provide a series of potential advantages, especially in situations such as the one observed in Brazil, a country of major geographic dimensions and with irregular distribution of healthcare professionals 8, especially dermatologists, which concentrate in the regions with highest purchasing power, such as the Southeast and the South of the country. This fact hinders access to dermatological consultation to different population groups distributed in areas far away from metropolitan centers 8.
Dermatology is a specialty with significant visual component, in a particularly favorable field to the use of telemedicine 9. The application of teledermatology, as the use of telemedicine in dermatology is named, has been studied mainly as a form of distance medical care, modality known as teleconsultation 7,10,11.
The use of teledermatology for distance consultation may be classified into two main groups 5,6,7,11,12 In the modality store-and-forward-system data referring to distance consultation, once sent, are stored in a database and are accessed after a variable time interval. In this modality, communication between the agents involved in the process occurs in a synchronic way. In the real time modality, exchange of information and interaction between agents takes place in real time 8,12.
The purpose of the present study was to assess the agreement level between live direct consultation and distance diagnosis of skin lesions using teledermatology in patients seen in a primary healthcare center, using the store and forward system (SFS).
MATERIAL AND METHOD
After approval of the Research Ethics Committee, we performed a retrospective study involving patients seen in the dermatology unit of Medical School, FTC, Salvador/BA, between January and April 2007. To enable sending and receiving distance data we created an internet environment using ASP (Active Server Pages), coupled to a database Microsoft SQL Server.
The study had a dermatologist responsible for the live consultation in Salvador-BA and two dermatologists responsible for the distance consultation (teleconsultation), physically located in two different Brazilian capital cities: São Paulo -SP and Fortaleza -CE.
All patients seen in the ambulatory of dermatology, Medical School, FTC, Salvador/BA, between January and April 2007, were invited to participate. Before the live consultation and after signing the informed consent term, an undergraduate took the clinical history and took pictures of the lesions. Together with the photos, the following data were collected and later submitted for the teleconsultation: gender, age, main complaint, summarized history of the current disease, duration of the condition and description of the elementary characteristics of the physical examination. Before the beginning of the study, the medical undergraduate was instructed on how to take the picture and describe the observed lesions. The study included only patients who had visible dermatological lesions.
Digital photos of cutaneous lesions were acquired under artificial light (fluorescent light) in the medical office, using digital care Sony Cyber-Shot with 7.2 megapixel resolution. On average, 10 pictures were taken per patient, including panoramic photos and macro mode. After initial photos, 3 to 4 best quality photos were sent to the teleconsultation.
Images were transferred from the camera to the computer using a USB cable and stored in JPEG format (Joint Photographic Experts Group), with 3072 x 2304 pixels resolution.
To send data referring to each patient, we used an internet environment exclusively to that end. Whenever a new case was included, a message was sent via email to the participating physicians informing that a new distant teleconsultation request had been sent. Through limited access to physicians responsible for the teleconsultation, they had access to the dada referring to each case.
After accessing the data, each physician responsible for the teleconsultation provided his independent diagnosis. All physicians made their diagnoses independently, based on the clinical information provided and the photos. In addition to the diagnosis, they could send comments about the cases to obtain information and suggestions that could explain any difficulties they had faced with each case.
After data collection, the failures and difficulties in operation of the system and the level of agreement between the clinical diagnoses of the involved physicians were assessed. The diagnosis considered as a reference was made by the physician responsible for the live care. It was considered to be in complete agreement (TC) when the distance diagnosis was identically described to what the physician had said in the live consultation. It was considered as partially in agreement (PC) when the diagnosis made by the distance physician corresponded to a differential diagnosis of that initially provided by the live visit and was considered as disagreeing diagnosis (DD) when the teleconsultation diagnosis differed from the main diagnosis and the differential diagnoses provided by the physician in the live visit.
The present study adopted the significance level of 5%. The agreement between diagnostic hits of dermatologists in teleconsultation was assessed based on Kappa test. Statistical analysis was made using software BioEstat 5.0 .
RESULTS
This pilot project included 60 patients. The patients' age ranged from 14 to 62 years, being 44% female and 56% male patients. The list with diagnoses obtained during the live visit is shown in Table 1.
In addition to the diagnosis from the live visit, two other main diagnoses were generated for each patient, made by the physicians in the teleconsultation, reaching a total of 120 responses.
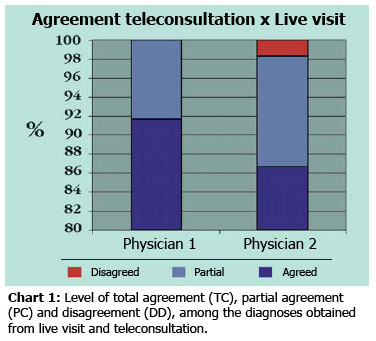
The level of total agreement between the diagnoses obtained through teleconsultation and live visit ranged from 86.6% to 91.6% (Chart 1). By grouping the diagnoses considered as TC and PC, the agreement ranged from 96% to 100% (Chart 1). Considering only the diagnoses obtained through teleconsultation, we observed good agreement between dermatologists in the teleconsultation (Kappa=0. 62, p< 0.01).
Concerning the comments made in the 120 responses, poor quality of the photo was reported in 20 cases (16.6%) and the need for additional data for diagnostic conclusion was reported in 24 cases (20%). Data insufficiency related to the need for further information such as clinical pathology results, dermatoscopy and/or data about consistency and/or texture of the skin.
DISCUSSION
When using Telemedicine in the teleconsultation modality there are two main ways of exchanging data: store-and-forward - when transmitted information is stored until they are accessed, and real time, in which there is real time interaction between the involved parties 4,7,9.
Despite the fact that real time modality has advantages when compared to SFS modality, such as greater interactivity between the patient and the physician and shorter response time, difficulties such as greater complexity, higher cost and the need to have synchronous access between the involved parties to exchange information ended up favoring the SFS modality 8,12. Because of these characteristics, modality SFS was adopted in this study.
The total agreement rate referred in the medical literature ranges from 54 to 95% 13,14 and partial agreement ranges from 76 to 100% 12. In the present study, the total agreement rate between the live diagnosis and the distant diagnosis was considered high, ranging from 86. 6% to 91.6%. When we consider partial agreement, the figures went up to 98.3% - 100%. This high level of agreement between live and distant diagnosis and the low rate of disagreement between the physicians in teleconsultation may be explained by the fact that the cases were from a primary healthcare center, which normally have low complexity cases with typical presentation. This association between the high hit rate and low complexity of clinical cases had been shown by other studies 15. Another factor that may have influenced the level of agreement is the fact that all dermatologists involved in the work presented similar education and experience in dermatological practice.
Concerning safety and operation of the system used for transmitting and storing data, there were no problems. There were no difficulties in handling the created interface, and its use had been easily incorporated by all participants of the study.
The technical quality of the photos directly influences the level of correct diagnosis and the agreement between the observers 8,12. To minimize problems with quality of photos we took on average 10 photos per patient, including panoramic photos and macro mode, and among them all, we selected 3 to 4 photos with the best quality, considering focus and lighting, before sending them through the system. Even taking it into account, the complaint of poor quality of the photo was identified in 16.6% of the cases. This complaint was more frequent in photos that identified regions such as pinna and hair scalp, regions that are normally considered of difficult visualization 12.
In the present study, in order to simulate information obtained through a healthcare professional who is not a specialist in dermatology, the information used to request a teleconsultation were collected by a medical undergraduate. The performance of the system in this study suggests that, provided that there was the appropriate training, there would be the possibility of a professional not specialized in dermatology to become responsible for information collection to be used when requesting the teleconsultation, towards maintaining satisfactory results.
CONCLUSION
Teledermatology supported by internet is one of the most disseminated forms of telesupport in the world, representing a viable option owing to its low cost and technological simplicity in application 13.
Cases of low complexity or those coming from primary healthcare centers may be particularly benefited by the teledermatology system 13.
Telemedicine is a valid resource to improve healthcare coverage 13, especially in such large country as Brazil. Applications and possibilities of teledermatology are multiple 8, but some challenges are posed especially concerning ethical and legal issues of distant medical care 13.
REFERENCES
Conflict of interest: None
Financial funding: None
How to cite this article: Silva CS, Souza MB, Duque IA, Medeiros LM, Melo NR, Araújo CA, Criado PR. Teledermatologia: correlação diagnóstica em serviço primário de saúde. An Bras Dermatol. 2009;84(5):489-93.
- 1. Wootton R. Telemedicine. BMJ. 2001; 323: 557-60
- 2. Perednia DA, Brown NA. Teledermatology: one application of telemedicine. Bull Med Libr Assoc. 1995: 83: 42-7
- 3. Demartines N, Mutter D, Vix M, Leroy J, Glatz D, Rösel F, et al Assessment of Telemedicine in Surgical Education and Patient Care. Ann Surg. 2000; 231: 282-91
- 4. Romero G, Cortina P, Vera E. Telemedicina y teledermatologia (II): estado actual de la investigación en teleconsulta dermatológica. Actas Dermosifiliogr. 2008; 99: 586-97
- 5. Eedy DJ, Wootton R. Teledermatology: a review. Br J Dermatol. 2001: 144: 696-707
- 6. D'Elia PB, Fisher PD, Bordin R, Harzheim E, Ramos MC. Concordância entre diagnósticos dermatológicos feitos presencialmente e por imagens digitais. An Bras Dermatol. 2007; 82: 521-7
- 7. Perednia DA, Brown NA. Teledermatology: one application of telemedicine. Bull Med Libr Assoc. 1995: 83: 42-7
- 8. Miot HA. Desenvolvimento e sistematizaçăo da interconsulta dermatológica ŕ distância [tese]. Săo Paulo (SP): Universidade de Săo Paulo; 2005. 144 p
- 9. Romero G, Garrido JA, García-Arpa M. Telemedicine and teledermatology (I): concepts and applications. Actas Dermosifiliogr 2008; 99: 506-22
- 10. Taylor P, Goldsmith P, Murray K, Harris D, Barkley A. Evaluating a telemedicine system to assist in the management of dermatology referrals. Br J Dermatol. 2001: 144: 328-33
- 11. Whited JD. Teledermatology research review. Int J Dermatol. 2006: 45: 220-9
- 12. Miot HA, Paixăo MP, Wen CL. Teledermatologia: passado, presente e futuro. An Bras Dermatol. 2005; 80: 523-32
- 13. Wootton R, Bloomer SE, Corbett R, Eedy DJ, Hicks N, Lotery HE, et al Multicentre randomised control trial comparing real time dermatology with conventional outpatient dermatological care: societal cost-benefit analysis. BMJ. 2000; 320: 1252-6
- 14. Chao LW, Cestari TF, Bakos L, Oliveira MR, Miot HA, Zampese M, et al Evaluation of an Internet-based teledermatology system. J Telemed Telecare. 2003; 9 (Suppl1): S9-12
- 15. Vidmar DA, Cruess D, Hsieh P, Dolecek Q, Pak H, Gwynn M, et al The effect of decreasing digital image resolution on teledermatology diagnosis. Telemed J. 1999; 5: 375-83
Mailing Address:
Publication Dates
-
Publication in this collection
07 Jan 2010 -
Date of issue
Oct 2009
History
-
Accepted
31 July 2009 -
Received
30 Dec 2008