Abstracts
Lipedematous scalp is a rare disease of unknown cause characterized by increased scalp thickness with a soft consistence. We report the case of a 13-year-old female with pruriginous soft thickening of the scalp vertex and slow growth of hair in the affected area. Anatomopathological examination showed edema, sparse mononuclear inflammatory perifollicular infiltrate, and ectatic lymphatic vessels. Ultrasonography confirmed thickening of the subcutaneous tissue. This is the second report of the disorder in a patient younger than 18 years old.
Edema; Scalp; Subcutaneous tissue
Escalpe lipedematoso é uma rara doença de origem desconhecida, caracterizada pelo aumento amolecido do couro cabeludo. Apresentamos um caso em paciente feminina de 13 anos de idade, com espessamento amolecido do vértex, prurido e crescimento lento dos fios na região afetada. O anatomopatológico revelou edema, infiltrado mononuclear esparso e perifolicular discretos, vasos linfáticos ectásicos e aumento do tecido subcutâneo, o qual foi ratificado pela ultrassonografia. Este é o segundo relato antes dos 18 anos de idade.
Couro cabeludo; Edema; Tecido subcutâneo
CASE REPORT
Lipedematous scalp with early onset
Roberto Rheingantz da Cunha FilhoI; Hiram Larangeira de Almeida JrII; André CartellIII
IM.S. in Health and Behavior at Universidade Catolica de Pelotas (UCPel) - Rio Grande do Sul, Dermatologist in a private clinic in Joaçaba (SC), Brazil
IIPh.D. in Dermatology, Professor and Coordinator of the Postgraduate Program in Health and Behavior, Universidade Catolica de Pelotas (UCPel) - Rio Grande do Sul. Professor of Dermatology at Universidade Catolica de Pelotas (UCPel) - and Universidade Federal de Pelotas (UFPel) - Pelotas (RS), Brazil
IIIDermatopathologist and Professor of Pathology at Universidade Federal do Rio Grande do Sul (UFRGS) - cidade (RS), Brasil
Mailing Address
ABSTRACT
Lipedematous scalp is a rare disease of unknown cause characterized by increased scalp thickness with a soft consistence. We report the case of a 13-year-old female with pruriginous soft thickening of the scalp vertex and slow growth of hair in the affected area. Anatomopathological examination showed edema, sparse mononuclear inflammatory perifollicular infiltrate, and ectatic lymphatic vessels. Ultrasonography confirmed thickening of the subcutaneous tissue. This is the second report of the disorder in a patient younger than 18 years old.
Keywords: Edema; Scalp; Subcutaneous tissue
INTRODUCTION
Lipedematous Scalp (LS) is an extremely rare disorder of unknown cause characterized increased edematous non-tumorigenic scalp thickness with a soft consistence, being more palpable than visible. Lipedematous Alopecia (LA) is a similar disorder associated with hypotrichosis or shortening of hair.There is no consensus, but both can be spectrums of the same disease.1 A rare case, of early onset, described by means of a histological and ultrasonographical study, is reported. It is the first in Latin America.
CASE REPORT
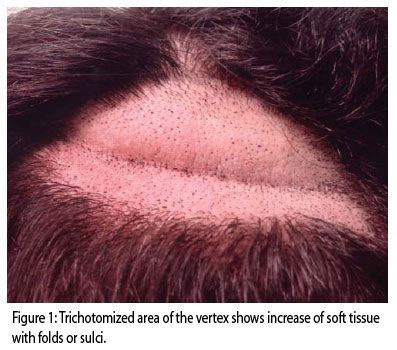
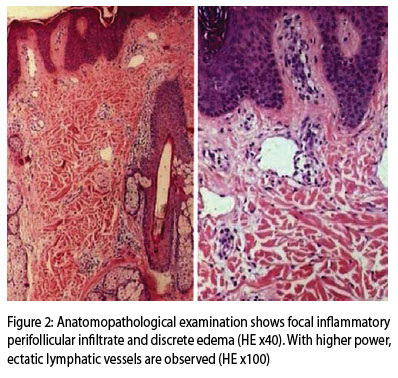
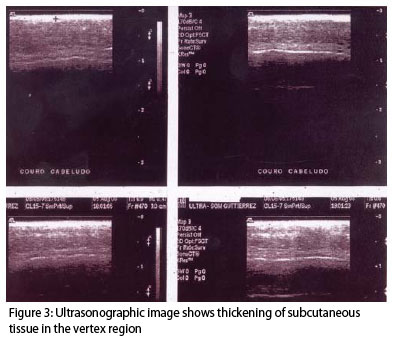
Female patient, brown, student, 13 years old, presents progressive thickening of the scalp vertex, more palpable than visible, that has gradually developed over the period of a year. It is sometimes pruriginous, and hair in the affected area grows slower. The area was trichotomized for photographic documentation and biopsy (Figure 1). Hair in the affected area was slightly shorter; however, finer hair or hypotrichosis were not identified. The patient's menarche occurred when she was 13 years old. She denies previous trauma and family history of the disease. Laboratorial and physical exams did not show other alterations (complete hemogram, hepatic and renal function tests, ASO, FAN, VDRL, total IgE, fasting glycemia, lipid profile, and thyroid hormones). Anatomopathological examination revealed ectatic capillary in the dermis, perifollicular mononuclear infiltrate and discrete edema, subcutaneous tissue increase and absence of mucin (Figure 2). Ultrasound showed an increase in the thickness of subcutaneous tissue, ranging from 6.2 mm to 9.1 mm. The expected range for the vertex region in normal individuals is 5-6 mm. (Figure 3).
DISCUSSION
There are about 30 cases of LS and LA reported in the world; most of them are cases of LA. The disorder affects individuals aged between 9 and 77 years, with no predilection for race. There is only one report of the disease in a male patient. The following occur in order of frequency: pruritus, absence of symptoms, pain, irritation, and paresthesia.1,2 The associations described occur with superficial lipomatous nevus and hyperelastic skin, affecting mainly the vertex and parietal region.3 Scalp measurement can be done with ultrasonography, magnetic resonance imaging, tomography or needle.4 The case reported is in accordance with the literature; however, it has an early onset, being the second case in a patient younger than 18 years old.5 It is more adequately classified as LS, despite the complaint that the hair grows slower and is apparently shorter in the affected area.
The etiology of the disorder is unknown, but hormonal factors may play a role due to its absolute predominance among women. Light microscopy is unspecific. It can be discrete, including edema, thickening of subcutaneous tissue, hyperkeratosis, sparse, perifollicular or perivascular inflammatory infiltrate, follicular alterations, ectatic lymphatic vessels, and reduction in the number of follicles. Anatomoclinical correlation is recommended. Elastic fibers are preserved. Studies may be conducted in an attempt to clarify the physio-pathogenia of the disease, including associated symptoms. Production and release of chemical mediators and cytokines should be explored in these studies.6,7
Treatment is challenging because it is a rare disorder and most reports do not refer to interventions. There is one report of improvement with systemic corticoid.
REFERENCES
- 1. El Darouti MA, Marzouk SA, Mashaly HM, El Nabarawi EA, Abdel-Halim MR, El Komy MM, et al. Lipedema and lipedematous alopecia: report of 10 news cases. Eur J Dermatol. 2007:17;351-2.
- 2. Martín JM, Monteagudo C, Montesinos E, Guijarro J, Llombart B, Jordá E. Lipedematous scalp and lipedematous alopecia: a clinical and histologic analysis of 3 cases. J Am Acad Dermatol. 2005:52;152-6.
- 3. Mansur AT, Yasar S, Aydingöz IE, Göktay F, Ozdemir N, Sungurlu F. Colocalization of lipematous scalp and nevus lipomatosus superficialis: a case report. J Cutan Pathol. 2006;34:342-5.
- 4. Yasar S, Mansur AT, Göktay F, Sungurlu F, Vardar Aker F, Ozkara S. Lipedematous scalp and lipedematous alopecia: report of three cases in white adults. J Dermatol. 2007:34;124-30.
- 5. Rowan DM, Simpson A, Wong KP. Lipedematous scalp in child. Pediatr Dermatol. 2006;23:276-8.
- 6. Scheufler O, Kania NM, Heinrichs CM, Exner K. Hyperplasia of the subcutaneous adipose tissue is the primary histopathologic abnormality in lipedematous scalp. Am J Dermatopathol. 2003;25:248-52.
- 7. Kavak A, Yuceer D, Yildirim U, Baykal C, Sarisoy HT. Lipedematous scalp: a rare entity. J Dermatol. 2008;35:102-5.
- 8. González-Guerra E, Haro R, Angulo J, Del Carmen Fariña M, Martín L, Requena L. Lipedematous alopecia: an uncommon clinicopathologic variant of nonscarring but permanent alopecia. Int J Dermatol. 2008:47;605-9.
Publication Dates
-
Publication in this collection
06 May 2010 -
Date of issue
Feb 2010
History
-
Received
20 Mar 2009 -
Accepted
31 July 2009