Abstracts
Papular mucinosis or lichen myxedematosus is an idiopathic disorder characterized by papules, nodules or plaques caused by mucin deposition in the dermis, in the absence of thyroid disease. The present report describes an atypical case with exuberant lesions in the form of plaques, associated with subclinical hypothyroidism. In cutaneous mucinosis, there is an abnormal quantity of mucin in the dermis. In traditional classifications of papular mucinosis, an absence of thyroid disease constitutes a diagnostic criterion. A few cases of the disease have been reported in association with hypothyroidism constituting, as in the present case, atypical lichen myxedematosus. It is therefore suggested that the presence of thyroid disease should not be considered an exclusion criterion for the diagnosis of this condition.
Hypothyroidism; Mucins; Scleromyxedema
A mucinose papulosa ou líquen mixedematoso é doença idiopática, manifestada por pápulas, nódulos ou placas por depósito de mucina na derme, na ausência de doença tireoidiana. Apresentamos um caso atípico, com lesões exuberantes em placas, associado ao hipotireoidismo subclínico. Nas mucinoses cutâneas há quantidade anormal de mucina na pele. Tradicionalmente as classificações consideram critério diagnóstico para mucinose papulosa a ausência de doença tireoidiana. Poucos casos associados ao hipotireoidismo são descritos e, assim como o nosso, constituem líquen mixedematoso atípico, sugerindo que a presença de doença tireoidiana não deva ser critério de exclusão para essa doença.
Escleromixedema; Hipotireoidismo; Mucinas
CASE REPORT
IPhysician, postgraduate student in Dermatology, State University of Rio de Janeiro (UERJ), Rio de Janeiro, RJ, Brazil
IIPhysician, postgraduate student in Dermatology, State University of Rio de Janeiro (UERJ), Rio de Janeiro, RJ, Brazil
IIIPhysician, postgraduate student in Dermatology, State University of Rio de Janeiro (UERJ), Rio de Janeiro, RJ, Brazil
IVAssistant Professor, Dermatology Department, State University of Rio de Janeiro (UERJ); Master's Degree in Dermatology from the Fluminense Federal University (UFF), Rio de Janeiro, RJ, Brazil
VAdjunct Professor, Dermatology Department, State University of Rio de Janeiro (UERJ); PhD in Dermatology from the Federal University of Rio de Janeiro (UFRJ), Rio de Janeiro, RJ, Brazil
Mailing Address
ABSTRACT
Papular mucinosis or lichen myxedematosus is an idiopathic disorder characterized by papules, nodules or plaques caused by mucin deposition in the dermis, in the absence of thyroid disease. The present report describes an atypical case with exuberant lesions in the form of plaques, associated with subclinical hypothyroidism. In cutaneous mucinosis, there is an abnormal quantity of mucin in the dermis. In traditional classifications of papular mucinosis, an absence of thyroid disease constitutes a diagnostic criterion. A few cases of the disease have been reported in association with hypothyroidism constituting, as in the present case, atypical lichen myxedematosus. It is therefore suggested that the presence of thyroid disease should not be considered an exclusion criterion for the diagnosis of this condition.
Keywords: Hypothyroidism; Mucins; Scleromyxedema
INTRODUCTION
Papular mucinosis or lichen myxedematosus is a chronic idiopathic disorder characterized by papules, nodules or lichenoid plaques resulting from a deposit of mucin in the skin, and a varying degree of fibrosis, without the presence of thyroid disease.1,2 The condition consists of two clinicopathological subtypes. The type referred to as scleromyxedema is a more widespread, sclerodermoid form, which is accompanied by monoclonal gammopathy and systemic manifestations that may be lethal. On the other hand, the localized papular form, which includes a range of more restricted conditions, is usually benign and chronic.3 Overlapping of the two different forms of the disease may occasionally occur and even cases with unique characteristics, unlike those described for any of the subtypes, may arise. These are referred to as atypical cases.2,3 The classification of cutaneous mucinosis is based on criteria that include the clinical appearance of the skin lesions, their histopathological characteristics and whether or not they are associated with systemic changes. According to the most recent classification, absence of thyroid disease is a diagnostic criterion for lichen myxedematosus; however, the classification of cutaneous mucinosis is considerably complex and remains controversial.3,4 Here, we report a case of atypical papular mucinosis with an exuberant presentation of plaques in the presence of symptomatic subclinical hypothyroidism.
CASE REPORT
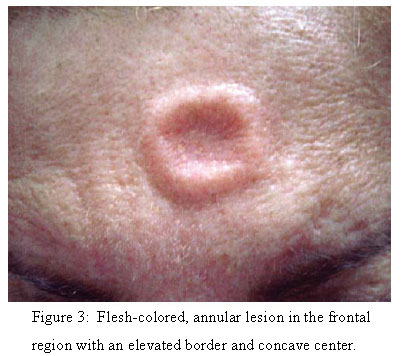
A 55 year old woman from Rio de Janeiro sought medical care at this service following a history of asymptomatic yellowish erythematous plaques on her upper back of around six years' duration. She reported that the lesions had been smaller and that around two years previously they had become infiltrated and more erythematous. In the past six months a new, flesh-colored lesion had appeared in the frontal region, with raised borders and a concave center. The patient had a past medical history of hypothyroidism, diagnosed around six years previously, and reported having undergone treatment with levothyroxine, which she, herself, decided to stop taking. She remains untreated to the present date. In addition to the skin lesions, the patient complained of fatigue, drowsiness, and arthralgia in her hands, wrists, elbows and shoulders. At the dermatological examination, yellowish erythematous, infiltrated, clearly defined, roundish plaques were found, measuring 4-6 cm at their largest diameter and spread across the upper back (Figure 1 and Figure 2). Another flesh-colored, annular lesion with a raised border and concave center, measuring around 1.5 cm in diameter, was found in the frontal region (Figure 3). Biopsy of a dorsal lesion revealed intense dissociation of collagen fibers in the middle and upper dermis with discrete perivascular mononuclear inflammatory infiltrate (Figure 4). Colloidal iron stain was positive, confirming the presence of a large amount of mucin between the fibers (Figure 5). Histopathological diagnosis was papular mucinosis. Laboratory findings consisted of: TSH 15.45 (normal range 0.27-4.2) and free T4 1.02 (normal range 0.93-1.7). A diagnosis of symptomatic subclinical hypothyroidism was made and treatment was initiated with 50 mcg/day of levothyroxine. After 15 days of treatment, the patient's systemic symptoms improved but her skin condition has remained unchanged up to the present date. The other laboratory tests such as complete blood count, renal function tests, serology for HIV and hepatitis, and protein electrophoresis were normal, the only abnormality being a higher than normal erythrocyte sedimentation rate (ESR) (48 mm; normal range < 10). the patient was referred for hematological evaluation, which excluded the presence of monoclonal gammopathy. she was also evaluated by a rheumatologist, who diagnosed synovitis of the wrist, metacarpophalangeal, interphalangeal and ankle joints, with a history of morning stiffness that lasted for more than two hours.
DISCUSSION
Cutaneous mucinosis refers to a heterogenous spectrum of disorders characterized by an abnormal amount of mucin in the skin.2 These disorders are traditionally classified as: primary, when the mucin is the principal histological characteristic, and secondary, when mucin represents merely an additional finding.2 Lichen myxedematosus or papular mucinosis is a primary form of mucinosis.2 There are two subtypes of lichen myxedematosus: a generalized papular, sclerodermoid form (also referred to as scleromyxedema) with monoclonal gammopathy, systemic manifestations and no thyroid abnormalities, and a localized papular form.3 The localized form is characterized by papules, nodules and plaques that are generally flesh-colored and located on the upper and lower limbs and trunk, with none of the characteristics of sclerosis, paraproteinemia, systemic involvement or thyroid disease.3 This type is divided into five subtypes: 1) the discrete papular form; 2) acral persistent papular mucinosis; 3) cutaneous mucinosis with spontaneous healing; 4) cutaneous mucinosis of infancy; and 5) the purely nodular form.1,3 A third group refers to patients with lichen myxedematosus with atypical characteristics or characteristics midway between the generalized and localized forms.1-3 The current classifications consider the absence of thyroid disease to constitute a diagnostic criterion for papular mucinosis.3 There are reports in the literature of three cases associated with hypothyroidism which, as in the present report, represent cases of atypical lichen myxedematosus. 4-6 The reason for the formation of papular depositions of mucin in hypothyroidism is unknown but may represent an exaggerated response of the local tissue to a generalized abnormality of the connective tissue metabolism induced by thyroid hormone deficiency. 7 There is evidence that in hypothyroidism the excess accumulation of hyaluronic acid in the skin and other tissues results from a proportionally greater reduction in its degradation compared to its synthesis.7 In two previously reported cases, thyroid hormone replacement therapy led to an improvement in cutaneous mucinosis, reinforcing the association between these conditions in which papular mucinosis may be considered a dermatological manifestation of hypothyroidism.5,6 In agreement with the findings of Archibald et al. 4, we believe that the presence of thyroid disease should not constitute an exclusion criterion for a diagnosis of lichen myxedematosus.
REFERENCES
- 1. Rongioletti F. Lichen mixedematosus (papular mucinosis): new concepts and perspectives for an old disease. Semin Cutan Med Surg. 2006;25:100-4.
- 2. Rebora A, Ronglioletti F. Mucinoses. In: Bolognia JL, Jorizzo JL, Rapini RP, editors. Dermatology. Spain: Mosby/Elsevier; 2004. p. 647-58.
- 3. Rongioletti F, Rebora A. Updated classification of papular mucinosis, lichen myxedematosus, and scleromyxedema. J Am Acad Dermatol. 2001;44:273-81.
- 4. Archibald GC, Calvert HT. Hypothyroidism and lichen myxoedematosus. Arch Dermatol. 1977;113:684.
- 5. Schaeffer D, Bruce S, Rosen T. Cutaneous mucinosis associated with thyroid dysfunction. Cutis. 1983;32:449-52,454,456.
- 6. Martin-Ezquerra G, Sanchez-Regaña M, Massana-Gil J, Umbert-Millet P. Papular mucinosis associated subclinical hypothyroidism: improvement with thyroxine therapy. J Eur Acad Dermatol Venereol. 2006;20:1340-1.
- 7. Jakubovic HR, Salama SS, Rosenthal D. Multiple cutaneous focal mucinoses with hypothyrodism. Ann Intern Med. 1982;96:56-8.
Papular mucinosis associated with hypothyroidism
Publication Dates
-
Publication in this collection
06 May 2010 -
Date of issue
Feb 2010
History
-
Accepted
30 Oct 2008 -
Received
08 Aug 2008