Abstracts
BACKGROUNDS: ultibacillary patients are the major source of infection in leprosy. Nevertheless, the risk is higher in household contacts between multibacillary patients than paucibacillary patients and in the general population. Household contacts are in close genetic relationship with the index case-patient. OBJECTIVE: To evaluate epidemiological data of the following variables: age, gender, education level, genetic proximity, and type of contact with the index case-patient (household or not) in 107 families with leprosy. METHODS: Home visits were conducted to clinically examine family members. The medical charts of index case-patients and co-prevalent cases were reviewed. RESULTS: The controlled analysis of variables such as type of contact and genetic proximity revealed that household contacts and first-degree kinship are independently associated with a higher chance of contracting the disease. CONCLUSION: Household contacts are often genetically closer to the index case-patient. To investigate the independent relevance of these risks in leprosy surveillance contact studies has been a challenge. Our results confirm literature data that show the influence of genetics in the susceptibility to leprosy per se.
Epidemiology; Genetics; Leprosy; Leprosy
FUNDAMENTOS - Os pacientes multibacilares (MB) são a principal fonte de infecção na hanseníase e esse risco é maior nos contatos domiciliares dos pacientes MB do que nos contatos dos paucibacilares (PB) e na população em geral. Entretanto, os contatos domiciliares são os mais próximos do caso-índice (CI), em termos genéticos. OBJETIVO: Analisar dados epidemiológicos das variáveis: sexo, idade, anos de estudo, grau de parentesco com o CI e tipo de contato residencial (intradomiciliar ou peridomiciliar) com o CI em 107 famílias de hanseníase. MÉTODOS: Foram realizadas visitas domiciliares para exame clínico dos familiares. Os prontuários dos CIs e de seus coprevalentes (contatos familiares que também tiveram hanseníase) foram revistos. RESULTADOS: A análise controlada das variáveis tipo de contato e grau de parentesco revelou que o contato domiciliar e o parentesco de primeiro grau estão independentemente associados a uma probabilidade maior de adoecer. CONCLUSÃO: Os contatos domiciliares, em geral, são os mais próximos do caso, em termos genéticos, e aferir a magnitude desses riscos separadamente tem sido um desafio nos estudos de vigilância de contatos em hanseníase. Os resultados deste estudo confirmam os dados da literatura, demonstrando a influência genética no desfecho da hanseníase per se.
Epidemiologia; Genética; Hanseníase; Hanseníase
INVESTIGATION
Epidemiologic study of 107 cases of families with leprosy in Duque de Caxias, Rio de Janeiro, Brazil*
Sandra Maria Barbosa DurãesI; Luiza Soares GuedesII; Mônica Duarte da CunhaIII; Monica Maria Ferreira MagnaniniIV; Maria Leide Wand Del Rey de OliveiraV
IM.S; Ph.D. student in Dermatology - Federal University of Rio de Janeiro (UFRJ); Assistant Professor - Federal Fluminense University (UFF) - Rio de Janeiro (RJ), Brazil
IIM.S. Student in Dermatology - Federal University of Rio de Janeiro (UFRJ) - Rio de Janeiro (RJ), Brazil
IIIPh.D. Student, Manager of the Leprosy Control Program of Duque de Caxias - Rio de Janeiro (RJ), Brazil
IVPh.D. Student; Statistician from the Collective Health Institute - Federal University of Rio de Janeiro (UFRJ) - Rio de Janeiro (RJ), Brazil
VM.S.; Professor (Ph.D.) at the Federal University of Rio de Janeiro (UFRJ) - Rio de Janeiro (RJ), Brazil
Mailing Address
ABSTRACT
BACKGROUNDS: ultibacillary patients are the major source of infection in leprosy. Nevertheless, the risk is higher in household contacts between multibacillary patients than paucibacillary patients and in the general population. Household contacts are in close genetic relationship with the index case-patient.
OBJECTIVE: To evaluate epidemiological data of the following variables: age, gender, education level, genetic proximity, and type of contact with the index case-patient (household or not) in 107 families with leprosy.
METHODS: Home visits were conducted to clinically examine family members. The medical charts of index case-patients and co-prevalent cases were reviewed.
RESULTS: The controlled analysis of variables such as type of contact and genetic proximity revealed that household contacts and first-degree kinship are independently associated with a higher chance of contracting the disease.
CONCLUSION: Household contacts are often genetically closer to the index case-patient. To investigate the independent relevance of these risks in leprosy surveillance contact studies has been a challenge. Our results confirm literature data that show the influence of genetics in the susceptibility to leprosy per se.
Keywords: Epidemiology; Genetics; Leprosy; Leprosy/epidemiology
INTRODUCTION
Studies about familial aggregation in leprosy indicate a relationship between the forms of the disease and kinship degree. Beiguelman (1972)1 observed that, in families in which the father and the mother were virchowian, relatives related by blood had a higher risk of developing the same polar type of the disease. In addition, the author noticed that the risk of contracting other forms of the disease was higher in non-consanguineous members of the household. Morton (1974) does not confirm these findings in Micronesia, but the rate of virchowian cases in that population (22%) was half of that observed in Brazil (45%), despite the fact that the world prevalence of leprosy is higher than in Brazil.2 The development of methods of segregation analysis made possible the investigation about the role of hereditarianism in familial aggregation to establish the form of inheritance.3,4 In 1979, Smith studied 91 families from the Philippines and verified that virchowian leprosy was three times more prevalent when one of the parents presented this clinical form of the disease, as compared to when none of them presented this form of the disease or presented no disease whatsoever. Nonetheless, the author argues that the multifactorial hypothesis correlates better with epidemiological data than any type of Mendelian inheritance.5
Serjeantson et al. (1979) analyzed 340 families from New Guinea and favored multifactorial inheritance for susceptibility to both virchowian and non-virchowian leprosy.6 Haile (1985) studied 75 families from India and suggested an autosomal recessive inheritance for susceptibility to tuberculoid leprosy.7 Shields et al. (1987) studied 269 families from New Guinea and were unable to differentiate between Mendelian inheritance and a purely environmental hypothesis as a risk factor.8 Wagener et al., in 1988, evaluated 63 families with at least 2 cases of leprosy and concluded that their data pointed to an autosomal dominant genetic hypothesis when the entire sample was considered. When only tuberculoid patients were included, the recessive model was more likely. 9
Abel et al. (1989) analyzed 27 pedigrees from the Caribbean island âDesirade' and accepted the hypothesis of autosomal recessive inheritance for susceptibility to both leprosy and Virchowian leprosy.10,11 In 1995, Abel et al. studied 285 families from Vietnam and 117 Chinese families who lived in Vietnam. The authors could not establish a Mendelian inheritance pattern for the distribution of cases in the Chinese families, whereas in the Vietnamese a larger co-dominant gene could be associated with leprosy per se.12
These studies were important because they strengthened the familial aggregation aspect of the disease. However, the authors did not arrive at a consensus about the form of inheritance of the disease due to its non-Mendelian character, in which the relationship with the genetic factor is complex, and there is likely more than one gene involved, with the need of various risk alleles to overcome the susceptibility threshold barrier.
OBJECTIVE
To analyze the clinical epidemiological profile of co-prevalent cases and identify the risk factors for leprosy among contacts.
MATERIAL AND METHODS
Details about the cases studied
The sample was defined based on a database from the Duque de Caxias Municipal Health Secretariat, with cases notified between 1998 and 2002 (520) in the 2nd district. Of the 520 index-case patients (IC), only 400 were found due to unavailable addresses. Initially 103 families were included in the study in a co-prevalence status (more than one case of leprosy in the family). Four more families from the same district of Duque de Caxias were included after the initial analysis period: two with co-prevalence cases and two with only one case of leprosy. A descriptive epidemiological study was conducted with these 107 families.
Home visits
Home visits were conducted in the municipality of Duque de Caxias for clinical dermato-neurological examination of family members to diagnose leprosy and to fill out prepared questionnaires. The visits occurred from June 2004 to September 2007.
Medical record review
Medical records of index and co-prevalent (family contacts who also had leprosy)-case patients were reviewed for certification about the contraction of the disease, data of diagnosis, treatment frequency, and level of disability.
Variables studied
The following variables were analyzed for indexcase patients: gender, age, ethnicity, clinical form of the disease, and educational level. For contacts, the following were evaluated: gender, age, ethnicity, degree of kinship with the index-case patient, dermato-neurological examination results, and educational level.
The clinical classification of index and co-prevalent- case patients was based on data from medical records of basic health units, where the Madrid and operational classifications are applied.
Degrees of kinship were defined as: 1- firstdegree kinship (father, mother, son/daughter, sibling); 2- second-degree kinship (uncle/aunt, nephew/niece, grandparents); 3 spouse; 4 others non-consanguineous (son/daughter-in-law, brother/sister-in-law, uncle's wife, friend, etc).
The type of contact with the index-case patient was defined as household (when the contact lived in the same house as the index-case patient, and non-household (when the contact lived in the same backyard).
Data from the descriptive epidemiological study of the 107 families were consolidated and analyzed using the computer programs EPIINFO 6.04d and STATA 9.0. Associations between categorical variables were evaluated with the Chi-square test or Fisher's exact test, when necessary. Student's t test was used to compare continuous variables between two groups. The endpoint variable considered was the contraction of the disease by contacts. Odds ratio (OR) and its respective reliability rate of 95% were estimated. A multifactor logistic regression analysis was conducted to investigate the factors associated with the chance of contracting the disease among contacts and determine the independent effect of each variable on the endpoint. The significance level for statistical tests was 0.05.
This study was approved by the Research Ethics Committee of HUCFF, UFRJ (protocol 187/04) and by the National Committee on Research Ethics (CONEP). All the participants signed a Free and Informed Consent Form (FICF). Two consent forms were prepared: one for index-case patients and one for their contacts to preserve the patients' anonymity, since their family members not always knew about their disease.
RESULTS
The 107 families were constituted by 1,205 individuals (107 index-case patients (IC) and 1,098 contacts); of this total, 1,098 were found (index-case patients and contacts). The other 107 (8.8%) were losses (61 missing (not found), 28 deceased, and 18 refused to participate) (Table 1).
The analysis of considered variables only examined contacts (829) and all the co-prevalent cases (211) because information was available in their medical records (including those missing and deceased), totaling 1,040 contacts. Index-case patients were all included. Losses of index and co-prevalent-case patients were not considered in the analysis of variables subject to clinical examination (such as ethnicity).
Table 2 shows the number of patients in each family and the distribution of cases based on the operational classification of the disease (paucibacillary or multibacillary). Three fourths of the families had two or three patients with the disease.
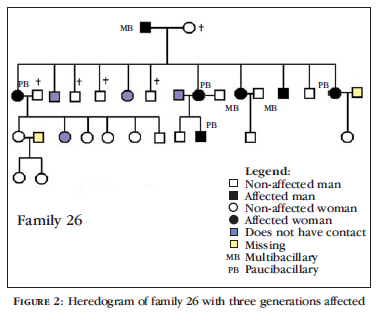
The disease appeared in one generation in 31 families, in two generations in 68 families and in 3 generations in 8 families. Figures 1 and 2 show family heredograms in which the disease affected two and three generations, respectively.
Bivariate Analysis
The sample studied did not show a statistical significant difference in relation to gender and ethnicity. Table 3 presents the distribution of gender, ethnicity and operational classification of the cases.
The educational level was similar for all index, co-prevalent and non-co-prevalent-cases, with an average of 4 years of study. Nevertheless, the age average was significantly lower among the non-co-prevalent cases. The average age among co-prevalent-case patients was 44.5 and among the non-co-prevalent, 30. 5 years (p-value = 0.002). The average age of index-case patients was 45.1 years old, similar to that of co-prevalent-case patients.
Degrees of kinship were defined as: 1- firstdegree kinship (father, mother, son/daughter, sibling); 2- second-degree kinship (uncle/aunt, nephew/niece, grandparents); 3 spouse; 4 others non-consanguineous (son/daughter-in-law, brother/sister-in-law, uncle's wife, friend, etc). The occurrence of the disease among first-degree consanguineous relatives (kinship degree 1- father, mother, sibling, daughter/son) and second-degree consanguineous relatives (kinship degree 2 uncle/aunt, nephew/niece, grandparents) in a single group was compared to the occurrence of the disease in the nonconsanguineous group (kinship degrees 3 and 4), and a significant association was not found (Table 4). However, when we compared only first-degree kinship with other degrees or types of kinship (other consanguineous relatives, spouses, and non-consanguineous contacts), the association with the disease was statistically significant (Table 5).
Contacts that lived in the same household as index-case patients had a higher chance of contracting the disease (x 2.4) than those that lived in the same backyard (Table 6).
A significant association between the clinical form of the disease presented by the index-case patient and the contraction of the disease was not found (Table 7).
Multivariate Analysis
Variables associated with the endpoint (contraction of the disease by contacts) with a 10% significance level were selected for multivariate analysis. The multivariate logistic regression analysis, involving type of contact and first-degree kinship, revealed that the chance of first-degree relatives contracting the disease is 2.05 times higher than that of contacts with other kinship degrees, controlling for type of contact. Moreover, the chance of contracting the disease among household contacts is 2 times higher than among non-household contacts, controlling for degree of kinship (Table 8).
DISCUSSION
Results from this epidemiological study indicate that the contact population (co-prevalent and non-coprevalent cases) did not show significant differences in relation to gender, ethnicity, and educational level. The higher age average of index and co-prevalent-case patients could be explained by the fact that the Brazilian population is young (56% younger than 30 years old) 13 and by the fact that the patients who contract leprosy are older due to BCG immunization or due to specific characteristics of the endemic disease in the study region.
In multifactor diseases, the risk of occurrence of a phenotype decreases as we move down the kinship distance ladder, differently from monogenic disorders, which always follow the same pattern. Considering the same type of contact, the higher incidence of the disease among consanguineous members of the nuclear family than among other consanguineous relatives shows the genetic susceptibility component of leprosy, widely reported in the literature.1,5,14,15 The association between the disease and the nuclear family in this epidemiological study was possible due to its sample size (n=1,147).
Household contacts of patients with leprosy have a higher chance of contracting the disease, even in an endemic urban area.16 However, only about 15 to 30% of the incident cases report contact with leprosy patients. 17 Upon extending the definition of contact to beyond household, Van Beers found the following incidence of new cases: 28% were household contacts; 36% lived in the same neighborhood of a case and 15% had social contacts with leprosy patients. In other words, in 79% of the cases some type of contact can be reported.18
CONCLUSION
Household contacts are often genetically closer to the index-case patient. To investigate the dimension of risks in isolation has been a challenge for researchers that conduct surveillance contact studies in leprosy. In this study the controlled analysis of the variable kinship degree 1 (first-degree kinship) and of the variable type of contact indicated the independent risk of the two exposures, with similar OR. In one of the largest cohort studies ever conducted, which followed 21,870 contacts of 1,037 leprosy patients in Bangladesh, physical and genetic proximity were also independently associated with the risk of contracting the disease.18 Even though we do not have the refinement of the data about independent association, our results confirm previous data from Moet showing that genetics influences the endpoint of leprosy per se. We did not find risk associations for clinical forms of the disease; however, this is of difficult analysis in this sample. Of the 33 paucibacillary cases, there was multibacillary Hansen's disease in the family of 19.
In the future we intend to research polymorphisms of susceptibility to leprosy, with various study designs in the Brazilian population. We believe that in the near future we may have access to very reliable susceptibility markers. Thus, the identification of susceptible genotypes may lead to greater knowledge about the pathogenic molecular mechanisms of leprosy and serve as a useful tool in the optimization of prophylactic actions as a strategy in the eradication and control of the disease.
REFERENCES
- 1. Rotberg, A. Some aspects of immunity in leprosy and their importance in epidemiology, pathogenesis, and classification of forms of the disease. Rev Bras Leprol. 1937;5:45-97.
- 2. Frost WH. The Familial Aggregation of Infectious Diseases. American Jour Pub Health. 1938;28:7-13.
- 3. Beiguelman B. An appraisal of genetic studies in leprosy. Acta Genet Med Gemello. 1972;17:21-52.
- 4. Morton NE, MacLean CJ. Analysis of family resemblance 3. Complex segregation analysis of quantitative traits. Am J Hum Genet. 1974;26:489-503.
- 5. Elston RC, Stewart J. A general model for the genetic analysis of pedigree data. Human Hered. 1971;21:523-42.
- 6. Lalouel JM, Rao DC, Morton NE, Elston RC. A unified model for complex segregation analysis. Am J Hum Genet. 1983;35:816-26.
- 7. Smith DG. The genetic hypothesis for susceptibility lepromatous leprosy. Human Genet. 1979;50:163-77.
- 8. Serjeantson S, Wilson SR, Keats BJ. The genetics of leprosy. Ann Hum Biol. 1979;6:375-93.
- 9. Haile RW, Iselius L, Fine PE, Morton NE. Segregation and linkage analyses of 72 leprosy pedigrees. Human Hered. 1985;35:43-52.
- 10. Shields ED, Russell DA, Pericak-Vance MA. Genetic epidemiology of the susceptibility to leprosy. J Clin Invest. 1987;79:1139-43.
- 11. Wagener DK, Schauf V, Nelson KE, Scollard D, Brown A, Smith T. Segregation analysis of leprosy in families of northern Thailand. Genet Epidemiol. 1988;5:95-105.
- 12. Abel L, Demenais F. Detection of major genes for susceptibility to leprosy and its subtypes in a Caribbean island: Desirade island. Am J Hum Genet. 1988;42:256-66.
- 13. Genetic susceptibility to leprosy on a Caribbean Island: linkage analysis with five markers. Int J Lepr Other Mycobact Dis. 1989;57:465-71.
- 14. Abel L, Vu DL, Oberti J, Nguyen VT, Van VC, Guilloud- Bataille M, et al. Complex segregation analysis of leprosy in southern Vietnam. Genet Epidemiol. 1995;12:63-82.
- 15. Casanova JL, Abel L. Genetic dissection of immunity to mycobacteria: The human model. Annu Rev Immunol. 2002;20:581-620.
- 16. Mira MT, Alcais A, Thuc NV, Moraes MO, Di Flumeri C, Thai VH et al. Susceptibility to leprosy is associated with PARK2 and PACRG. Nature. 2004;427(12):636-640.
-
17IBGE [homepage]. [acesso em 03 Ago 2008]. Disponível em: http://www.ibge.gov.br
» link - 18. Moet FJ, Pahan D, Schuring RP, Oskam L, Richardus JH. Physical distance, genetic relationship, age, and leprosy classification are independent risk factors for leprosy in contacts of patients with leprosy. J Infect Dis. 2006;193:346-53.
- 19. Durães SMB, Guedes LS, Cunha MD, Cavalliere FAM, Oliveira MLW. Estudo de 20 focos familiares de haseníase no município de Duque de Caxias - Rio de Janeiro. An Bras Dermatol. 2005;80:S295-300.
- 20. Matos HJ, Duppre N, Alvim MF, Machadovieira LM, Sarno EN, Struchiner CJ. Epidemiologia da hanseníase em coorte de contatos intradomiciliares no Rio de Janeiro (1987-1991). Cad Saude Publica. 1999;15:533-42.
- 21. Fine PE, Sterne JA, Pönnighaus JM, Bliss L, Saui J, Chihana A, et al. Household and dwelling contact as risk factors for leprosy in northern Malawi. Am J Epidemiol. 1997;146:91-102.
- 22. van Beers SM, Hatta M, Klatser PR. Patient contact is the major determinant in incident leprosy: implications for future control. Int J Lepr Other Mycobact Dis. 1999;67:119-28.
Publication Dates
-
Publication in this collection
24 Sept 2010 -
Date of issue
June 2010
History
-
Received
27 Aug 2008 -
Accepted
09 Dec 2008