Abstracts
Lymphogranuloma venereum is an infection caused by a variety of the bacterium Chlamydia trachomatis. Both genital and extragenital manifestations of the disease can cause serious differential diagnostic difficulties, indirectly leading to progression and dissemination of the infection. This work describes cases of patients with lymphogranuloma venereum showing atypical clinical and/or histopathological findings. It also focuses on alternative therapeutic approaches, such as surgical excision at stage 1, that may lead to a positive outcome. It is not completely clear whether histopathological findings of lymphogranuloma venereum can reveal progression or changes in the course of the disease over time, as is the case in other diseases. We conclude that both clinical and histopathological observations in a larger number of patients are needed in order to further evaluate the findings presented in this article.
Chlamydia trachomatis; Lymphogranuloma venereum; Neoplasms; Surgery, plastic
Linfogranuloma venéreo é uma infecção causada por um tipo específico da bactéria Chlamydia trachomatis. Manifestações genitais e extragenitais da doença podem causar uma série de dificuldades no diagnóstico diferencial, indiretamente levando a progressão ou disseminação da infecção. Este trabalho apresenta casos de pacientes com linfogranuloma venéreo cujos achados clínicos e/ou histopatológicos são atípicos, além de abordar métodos de terapia alternativos, tais como excisão cirúrgica na fase 1, os quais podem trazer um resultado positivo. Ainda não se sabe se achados histopatológicos do linfogranuloma venéreo podem revelar progressão ou mudanças no curso da doença ao longo do tempo, como ocorre com outras enfermidades. Concluímos que observações clínicas e histopatológicas devem envolver um número maior de pacientes a fim de avaliar os resultados clínicos deste trabalho.
Chlamydia trachomatis; Cirurgia plástica; Linfogranuloma venéreo; Neoplasias
CASE REPORT
Lymphogranuloma venereum - "a clinical and histopathological chameleon?"
Linfogranuloma venéreo - "um camaleão clínico e histopatológico?"
Georgi TchernevI; Cristina SalaroII; Mariana Carvalho CostaIII; James W. PattersonIV; Pietro NenoffV
IM.D., Ph.D., Specialist in Dermatology and Venereology, Department of Dermatology, Venereology and Dermatologic Surgery - Kirchheim, Germany. Associated professor - Bulgaria
IIM.D., Specialist in Dermatology, Professor Rubem David Azulay Institute of Dermatology - Santa Casa de Misericordia of Rio de Janeiro - Rio de Janeiro (RJ), Brazil
IIIM.D., Postgraduate student at Professor Rubem David Azulay Institute of Dermatology - Santa Casa de Misericordia of Rio de Janeiro - Rio de Janeiro (RJ), Brazil
IVM.D., Professor of Pathology and Dermatology, Division of Surgical Pathology & Cytopathology - University of Virginia Hospital; Director of Dermatopathology, University of Virginia Health System - Virginia, USA
VM.D., Ph.D., Laboratory for Medical Microbiology, Partnership Dr. Jürgen Herrmann, Prof. Dr. Pietro Nenoff & Dr. Constanze Krüger - Mölbis, Germany
Mailing address Mailing address: Georgi Tchernev Georgi Benkovski street 4a Sofia - Bulgaria E-mail: georgi_tchernev@yahoo.de
ABSTRACT
Lymphogranuloma venereum is an infection caused by a variety of the bacterium Chlamydia trachomatis. Both genital and extragenital manifestations of the disease can cause serious differential diagnostic difficulties, indirectly leading to progression and dissemination of the infection. This work describes cases of patients with lymphogranuloma venereum showing atypical clinical and/or histopathological findings. It also focuses on alternative therapeutic approaches, such as surgical excision at stage 1, that may lead to a positive outcome. It is not completely clear whether histopathological findings of lymphogranuloma venereum can reveal progression or changes in the course of the disease over time, as is the case in other diseases. We conclude that both clinical and histopathological observations in a larger number of patients are needed in order to further evaluate the findings presented in this article.
Keywords: Chlamydia trachomatis; Lymphogranuloma venereum; Neoplasms; Surgery, plastic
RESUMO
Linfogranuloma venéreo é uma infecção causada por um tipo específico da bactéria Chlamydia trachomatis. Manifestações genitais e extragenitais da doença podem causar uma série de dificuldades no diagnóstico diferencial, indiretamente levando a progressão ou disseminação da infecção. Este trabalho apresenta casos de pacientes com linfogranuloma venéreo cujos achados clínicos e/ou histopatológicos são atípicos, além de abordar métodos de terapia alternativos, tais como excisão cirúrgica na fase 1, os quais podem trazer um resultado positivo. Ainda não se sabe se achados histopatológicos do linfogranuloma venéreo podem revelar progressão ou mudanças no curso da doença ao longo do tempo, como ocorre com outras enfermidades. Concluímos que observações clínicas e histopatológicas devem envolver um número maior de pacientes a fim de avaliar os resultados clínicos deste trabalho.
Palavras-chave: Chlamydia trachomatis; Cirurgia plástica; Linfogranuloma venéreo; Neoplasias
INTRODUCTION
According to the New York State Department of Health, the incidence of lymphogranuloma venereum (LGV) is highest among sexually active people living in tropical or subtropical climates, including some areas in the southern U.S.1,2 This disease is endemic in East and West Africa, Southeast Asia, India, the Caribbean basin, and South America, including Brazil. Indeed, a recent Brazilian study coordinated by proctologists indicates that LGV has been diagnosed with increasing frequency in European countries, North America and Australia, mainly in men who have sex with men. The study also suggests an increasing incidence of LGV in Brazil.3
The diagnosis is often made serologically and by exclusion of other causes of inguinal lymphadenopathy or genital ulcers.2,4 The differential diagnosis of LGV is often difficult because other causes of genital ulceration have to be ruled out. Even when LGV is suspected, investigations of potentially co-existing sexually transmitted infections or other tumoral lesions must be undertaken.2
CASE REPORT
CASE 1
Anamnesis
A 36-year-old HIV-negative homosexual man complained of skin problems on his face and enlargement of cervical lymph nodes of three weeks duration (Figure 1). He had been in Libya for three months before the onset of cutaneous manifestations.
Clinical examination revealed an asymptomatic erythematous, erosive nodule on his right lower lip, approximately 12 mm in diameter, together with other two similar smaller lesions located on the ipsilateral cheek and zygoma.
Histopathological findings:
The epidermis showed hyperkeratosis, with both ortho- and parakeratosis. Within the dermis: inflammatory infiltrate containing many neutrophils; plasma and giant cells were identified in the deeper dermis. Microabscesses could also be noted (Figure 2).
Other complementary exams
A microbial smear from lesional tissue was negative for Staphylococus aureus and Clostridium spp, and culture of lesional tissue was negative for Gonococcus (Neisseria gonorrhoea). A Chlamydia smear from the urethra was also negative.
Laboratory findings
Leukocytosis of 15,000/mm3 before treatment; white cell count was 6,400/mm3 after treatment.
CRP (C-reactive protein) 75; level 8 after treatment.
Erythrocyte Sedimentation Rate - 60/78.
PCR in lesional tissue: Chlamydia trachomatis-DNA-positive; Chlamydia pneumoniae-DNA-negative; Chlamydia Psittaci-DNA-negative; Leishmania-DNA-negative.
ELISA: Chlamydia-AK (Autoantibodies) IgG (++) 6.77; IgA ++ (8.11) IgM ++ (4.36); HIV 1.2-AK: negative; TPHA negative, VDRL negative; Hepatitis B/C antibodies negative.
Other Diagnostic Studies
Roentgenography (Rx): no pathological findings.
Sonography-Abdomen: splenomegaly.
Sonography-Lymph nodes: multiple enlarged lymph nodes, regionally and peripherally located (axillary).
CT-Computer tomography of the neck area: asymmetrical oropharyngeal structures on the right side of the neck; cervical lymph node involvement with asymmetrical subcutaneous tissue structures on the right in comparison with the left; massive infiltration of the dermis and subcutis.
Treatment and Outcome
Surgical excision of the affected lymph nodes was performed under local anaesthesia. Histopathological examination of the excised cervical lymph nodes was negative for metastatic tumor (Figure 3). Treatment was initiated with pentamidine (Pentacarinat®) 200mg intramuscularly (2x) plus oral Doxycycline 2x100 mg for three weeks, leading to complete remission.
CASE 2
Anamnesis
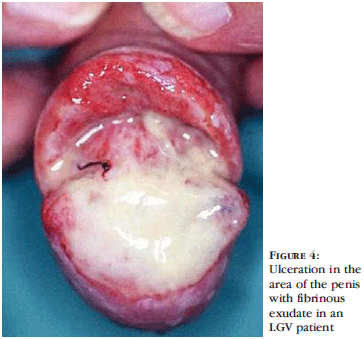
An 82-year-old male had a two-month history of a progressively indurating papule of the gland penis, followed by ulceration. The initial clinical suspicion was of a cutaneous neoplasm (Figure 4). His history was positive for internal diseases, including a positive serology for rheumatoid arthritis, diabetes mellitus type II, glaucoma, heart failure (status after bypass intervention), and hypertension. The patient's systemic medication included: ISDN (isosorbide dinitrate) 120 mg 1-0-0, captopril 25/25 (1-0-1), Torasemide 10 mg 1-0-0, Kalinor (potassium chloride) 1-0-0, and methotrexate 10 mg 1-0-0.
Histopathological findings
A bone marrow biopsy showed plasma cells and gammopathy of uncertain significance. Skin biopsy showed lymphocytic infiltrates with some eosinophils (Figure 5). Immunohistochemically, there was evidence of a chronic histiocytic (macrophagic) and fibrosing balanitis. Direct immunofluorescence studies were negative.
Laboratory findings
Erythrocyte Sedimentation Rate: 90/99, 76/88, 32/80.
Ferritin: 1.225 (normal: 20-400 ng/ml).
Transferin: 1.52 (normal: 3-3.6 g/l).
Haemoglobin: 8.2 (normal: 8.7-11.2 mmol/l).
Creatinine: 129 (normal: 53-133 μmol/l).
Urea: 12.6 (normal: 1.7-8.5 mmol/l).
LDH: 4.1 (normal up to 3.75 mmol/l).
Immunofixation electrophoresis from the serum: paraproteinemia type Kappa IgG could be observed.
Immunofixation electrophoresis from the urine: no Bence Jones proteinuria.
Serum protein electrophoresis: albumin- 54.5 (normal 60-71%) / alpha 1 - 3.7 (normal 1.4-2.9%) / gamma globulin - 20.9 (normal 9-16%).
Immunologic parameters:
ANA: 1.640 with fine speckled muster.
Autoantibodies against CCP: 8.2 (normal under 1).
Rheumatoid factor: 92: (normal under 14 U/ml).
pANCA, cANCA: negative.
ENA: negative.
Lymphocytic subpopulations: all data in normal issues.
Quantitative Immunoglobulins: IgG and Ig-Anormal, IgM-5.88 (normal 0.4-2.3 g/l).
Serologies for Infectious Diseases
TPHA test: negative.
Chlamydia serology: IgA (Ratio 1.47), IgM positive (Ratio 1.08); IgG negative.
Chlamydia smear, lesional tissue of the penis: negative.
VZV (Varicella zoster virus): IgG 3.4 (normal up to 1.1), IgM 1.3 (normal up to 1.1).
Herpes simplex virus serology (HSV1, HSV 2): IgG positive - 4.2, IgM negative.
Fungal smear of the penis: negative.
Bacterial smear of the penis: negative.
Other Diagnostic Studies
Roentgenography of thorax: right-sided lesion suspicious for tuberculoma.
Ultrasonography of lymph nodes and abdomen: steatosis hepatis, left band: many enlarged, conflating lymph nodes up to 15 mm; right band: a number of solitary painful lymph nodes.
Treatment and outcome
Administration of doxycycline 2x100 mg for 3 weeks and Octenisept® (antiseptic solution) 2-3 times a day resulted in complete remission of skin lesions (Figure 6).
DISCUSSION
An initial consideration of skin cancer is not unreasonable in patients such as those discussed above, since clinical findings can be quite similar and histopathology is not always conclusive.1 Therefore, an important first step in the differential diagnosis of an ulceration of the penis is to consider the possibility of LGV.1,2,4 A delay in diagnosis increases the chance of complications and misunderstandings.4
The personal data in case 1 (homosexuality and a recent time spent in Libya) provides the clinician important information and enhances the differential diagnosis by raising the possibility of rare and atypical cutaneous manifestations of tropical and subtropical infections, such as LGV. The enlarged lymph nodes in the cervical area could have been mistaken for locoregional metastases (patient 1). The lesion in the infralabial area was removed in toto and the defect closed by single skin sutures. As a supporting procedure, extirpation of single lymphatic nodes from the submandibular area was performed, and histopathological findings were identical. The exclusion of squamous cell carcinoma in patient 1 was of prime importance for the patient (Figure 2). However, microscopic findings yielded surprising results: abscessed inflammation with neutrophils and a partially granulomatous infiltrate (Figure 2). PCR performed on lesional tissue confirmed the presence of LGV -DNA (L1-L3) infection. Chlamydial serology was positive for IgM, as well as for IgG and IgA. A rare manifestation of cutaneous leishmaniasis was excluded by PCR methodology. The cause of the hepatosplenomegaly, discovered by ultrasonography, remained unclear; the patient's hepatic parameters were normal, arguing against the possibility of an infectious etiology.
In addition to the good therapeutic results achieved by systemic medication, surgical excision of the entire lesion quickly led to full remission (patient 1). An excellent cosmetic effect was also achieved in the facial area (Figure 3).
Evidently, LGV is a disease that, within the socalled initial papule or stage 1a, can also be surgically treated. In cases where lymphadenopathy due to infection is suspected (confirmed by positive serology for IgM and/or PCR-DNA for Chlamydia trachomatis in lesional tissue), additional antibiotic therapy is also recommended.4
It is assumed that each stage of LGV has a different clinical and histopathological morphology.4 Frequently, in their clinical practice, dermatologists have to face serious diagnostic dilemmas provoked by the non-specific clinical and, sometimes, histopathological findings in patients with LGV.2
For example, genital ulcers may be present in sexually transmitted diseases other than LGV, including syphilis, chancroid, genital herpes simplex, ulcerative herpes zoster, donovanosis; they may also occur in non-sexually transmitted disorders such as Behçet's syndrome, Crohn's disease, pemphigus vulgaris, and erosive lichen planus.1
The ulcerative genital form of LGV presented in case 2 is not characteristic of stage 1b, in which the ulcerations are mainly superficially located and lack fibrous coatings (Figure 4). The patient was hospitalized because of the ulcerated tumor in the genital area. Such a presentation, in an 82-year-old patient (sexually inactive, according to the clinical history) is quite unusual. Due to the positive serology for Chlamydia trachomatis, systemic therapy with doxycycline was instituted, leading to complete remission (Figure 6). PCR for chlamydial DNA in the lesional tissue was not performed at the hospital.
The Kappa type paraproteinemia found in this patient could suggest a disorder of the cutaneous microcirculation due to sedimentation of paraproteins (combined with thrombocytes, erythrocytes, and fibrinogen) in the form of cryoglobulins and cryofibrinogen. However, in that case, clinical remission would not have been achieved with antibiotic therapy within 2-3 weeks, but possibly with therapy directed towards hemodilution or vasodilatation. Indirectly, the diagnosis of a specific form of paraproteinemia could not be confirmed.
The critically increased values of IgM serology do not eliminate the possibility of a localized, superinfected, macerated, genital form of varicella-zoster viral infection. However, the non-specific histology eliminates the diagnosis of zoster involving the genital area and minimizes the critical positive values of IgM with respect to VZV infection. In addition, the negative immunofluorescence on lesional tissue argues against an immunologically initiated lesion within the framework of seropositive, active rheumatoid arthritis. The positive serology with respect to Chlamydia trachomatis and the rapid response to antimicrobial therapy indisputably lead to the interpretation of a rare form of LGV infection.
The question of whether histopathological findings in this LGV-suffering patient could evolve to an image similar to that of other granulomatous diseases, such as pyoderma gangrenosum, remains unanswered.5 As a disease of unclear etiology, pyoderma gangrenosum initially shows neutrophilic infiltrates (acute stage), followed by lymphocytic infiltrates (subacute stage), and granulomatous infiltrates (chronic stage).5
After a detailed analysis of all the bibliographic sources, we cannot entirely exclude the hypothesis that histopathological findings in LGV-patients can also evolve, in concert with the clinicopathologic findings. At the acute stage (case 1), neutrophilic infiltrates prevail; at the subacute stage, histiocytes (macrophages) most likely predominate (case 2), whereas at the chronic stage, granulomatous infiltrates probably prevail.
CONCLUSIONS
1) A rare form of extragenital lymphogranuloma venereum stage 1a is presented, clinically simulating squamous cell carcinoma with metastases to the cervical lymph nodes (Figure 1). The role of dermatosurgery as an important supporting method at the initial stages of this disease is evaluated.
2) Another rare case of lymphogranuloma venereum localized in the glans penis area is described, with the atypical presentation of a non-specific ulcerating balanitis (Figure 4).
3) A rare and new specific histopathological finding of ulcerating balanitis is described: a histiocytic (macrophagic) and sclerosing reaction at LGV stage 1b. This shared finding is probably specific to the subacute stages of this disease. We do not exclude the possibility that an ulcerating balanitis could be generated within the context of seropositive, active rheumatoid arthritis, which is frequently able to initiate nonspecific skin and mucosal ulcerations. In that case, partial improvement could in theory be achieved through the anti-inflammatory and immunomodulatory effects of the antibiotic doxycycline.
4) Probably, dermatosurgery should not be used as a primary or adjuvant method in patients suffering from LGV stage 1b or in patients with genital localization of the initial ulcer papule, in view of the genital location and the infiltrative plaque-like or endophytic growth of the lesions.
Received on 18.11.2010.
Approved by the Advisory Board and accepted for publication on 23.02.10
Conflict of interest: None / Conflito de interesse: Nenhum
Financial funding: None / Suporte financeiro: Nenhum
* This study was conducted at the Department of Dermatology, Venereology and Dermatologic Surgery - Kirchheim, Germany.
- 1. Tchernev G. Lymphogranuloma venereum of the penis mimicking clinically gangrenous pyoderma and presenting histologically as macrophagocytic-histiocytic balanitis. [Medical Review]. 2007;43:90-4.
- 2. Tchernev G, Trebing D, Goring HD. Genitale Manifestation eines Lymphogranuloma venereum unter dem klinischen Bild einer ulzerierenden makrophagozytären Balanitis Praktische Dermatologie DERM -HAMBURG. 2007;13:140-7.
- 3. Hernani BL, Nadal SR. Linfogranuloma venério: aumento na incidência sugere surto mundial da doença / Lymphogranuloma venereum: increased incidence suggests diseases world outbreak. Rev Bras Coloproct. 2007:27:224-7.
- 4. Tchernev G, Nenoff P, Costa M, Salaro C. Uncommon Extragenital Form of Lymphogranuloma venereum: A "New" Therapeutic Option for An "Ancient Disease"? [Medical Review]. 2009;45:77-82.
- 5. Tchernev G, Trebing D, Göring H-D, Steinhoff M, Zouboulis CC, Orfanos C. Pyoderma gangrenosum in Crohn's disease - The role of immunologic parameters and histological data in diagnosis and differential diagnosis. Bulg J Hepatogastroenterol. 2005;7:56-60.
Mailing address:
Publication Dates
-
Publication in this collection
01 Oct 2010 -
Date of issue
Aug 2010
History
-
Received
18 Nov 2010 -
Accepted
23 Feb 2010