Abstracts
Tufted angioma is a rare acquired vascular tumor. It is characterized by painful purplish macules that may progress to plaques containing angiomatous papules. The condition is benign; however, it often affects extensive areas of the skin, leading to functional disability of the affected limb if painful. The present report describes a case of a tufted angioma associated with myofascial pain syndrome in which the predisposing element was the presence of this tumor since childhood. Pain at the site of the lesion affected muscle use and led to the onset of the associated syndrome. Complete relief from symptoms was achieved by blocking the trigger points of the affected limb with anesthesia.
Local anesthesia; Hemangioma; Myofascial pain syndrome
O Angioma em tufo é considerado um raro tumor vascular cutâneo adquirido. Caracteriza-se por máculas purpúrico-violáceas, dolorosas que podem evoluir para placas com pápulas angiomatosas. Tem natureza benigna, mas o envolvimento extenso é comum, gerando alteração funcional do membro afetado em caso de dor. Os autores relatam um caso de angioma em tufo associado à síndrome dolorosa miofascial, em que o elemento predisponente foi a presença deste tumor desde a infância. A dor local prejudicou a utilização da musculatura e possibilitou o surgimento da síndrome relatada. A realização de bloqueio anestésico de pontos-gatilhos no membro afetado, levou à melhora total dos sintomas.
Anestesia local; Hemangioma; Síndrome da dor miofascial
CASE REPORT
Tufted angioma and myofascial pain syndrome*
Roberto Souto da SilvaI; Aline Lopes BressanII; Lívia Barbosa NascimentoIII; Bernard Kawa KacIV; Luna Azulay-AbulafiaV
IPhD in Dermatology. Adjunct Professor of Dermatology, State University of Rio de Janeiro (UERJ). Preceptor of the postgraduate courses in Dermatology at the State University of Rio de Janeiro (UERJ) and the Professor Rubem David Azulay Institute of Dermatology at the Santa Casa da Misericórdia in Rio de Janeiro. Professor at the Gama Filho University (UGF), Rio de Janeiro, Brazil.
IIPhysician currently participating in the medical residency program in Dermatology at the Pedro Ernesto Teaching Hospital, State University of Rio de Janeiro (UERJ), Rio de Janeiro, Brazil
IIISpecialist in Clinical Medicine. Currently participating in the postgraduate program in Dermatology at the Pedro Ernesto Teaching Hospital, State University of Rio de Janeiro (UERJ), Rio de Janeiro, Brazil
IVDermatologist certified by the Brazilian Society of Dermatology, Rio de Janeiro, Brazil
VPreceptor of the postgraduate course at the Professor Rubem David Azulay Institute of Dermatology at the Santa Casa da Misericórdia in Rio de Janeiro, Brazil
Mailing address
ABSTRACT
Tufted angioma is a rare acquired vascular tumor. It is characterized by painful purplish macules that may progress to plaques containing angiomatous papules. The condition is benign; however, it often affects extensive areas of the skin, leading to functional disability of the affected limb if painful. The present report describes a case of a tufted angioma associated with myofascial pain syndrome in which the predisposing element was the presence of this tumor since childhood. Pain at the site of the lesion affected muscle use and led to the onset of the associated syndrome. Complete relief from symptoms was achieved by blocking the trigger points of the affected limb with anesthesia.
Keywords: Local anesthesia; Hemangioma; Myofascial pain syndrome
INTRODUCTION
Tufted angioma was first described by Nakagawa in 1949. It is considered a rare, acquired, vascular tumor of the skin that generally occurs prior to five years of age.1 Nevertheless, congenital cases have been described, 1,2 as well as cases developing during adolescence, pregnancy and in adults. It is usually located on the neck, the upper part of the chest or the shoulders, but may affect the proximal portion of the limbs, the face or the scalp. Clinically, it presents as purplish macules that may progress to plaques with superimposed angiomatous papules. In the majority of cases, tufted angioma is painful, hard and incompressible. It grows slowly and may present with overlying hypertrichosis and hyperhidrosis. 3 Although benign, the area affected is often extensive, resulting in a disfiguring appearance and impaired function if the condition is painful. Growth is slow and progressive, stabilizing in the majority of cases, and spontaneous involution may even occur. 4,5 Histopathologically, the condition presents with vessels in the superficial and deep dermis distributed in a cannonball pattern (Figure 1). 6 Various forms of treatment have been attempted; however, none are considered first line. Therapeutic options include: surgical excision, topical and oral corticosteroids, alpha-interferon and pulsed dye laser.
CASE REPORT
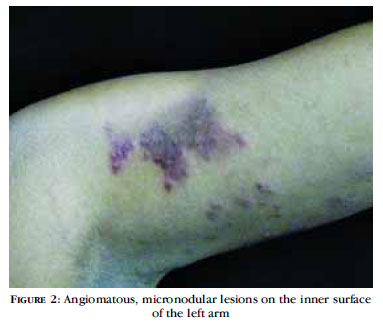
A 20-year old woman with a purplish erythematous lesion on her left arm (Figure 2), which had been present since she was one year old. 7 It grew slowly until she reached ten years of age (Figure 3). The principal symptom was spontaneous pain and pain to the touch, which had intensified in the previous five years, together with dysesthesia in her left arm. She had been followed up at another service, where a biopsy had been performed, resulting in a histopathology report of tufted angioma. She was treated with topical clobetasol and oral amitriptyline, albeit without any improvement. She came to this clinic and was prescribed topical 0.025% capsaicin, which resulted in an initial improvement. Despite this favorable response, the patient had a recurrence of the symptomatology and was referred to the pain clin-ic. At this time, she was diagnosed with myofascial pain syndrome and treatment was initiated with amitriptyline and gabapentin, and an anesthetic block was made at the trigger points in the upper dorsal region ipsilateral to the affected limb. After two infiltrations, pain at the site disappeared. Prior to receiving the third infiltration, the patient became pregnant. Although infiltration is not contraindicated for pregnant women, pregnancy renders systemic treatment of the angioma impossible.
DISCUSSION
In this patient, the age at the time of appearance of the vascular lesion and its site is compatible with the data in the literature. 2,3 As the years went by, the lesion increased in size; however, it stabilized at puberty. Nevertheless, the pain intensified, making it difficult to move the affected limb, 8 which was already slightly hypotrophic. The therapy selected consisted of 0.025% topical capsaicin cream. Despite an initial improvement, the pain returned and the patient was referred to the pain clinic, where she was diagnosed with myofascial pain syndrome. 9 This is characterized by the presence of regional pain, i.e. pain that affects only one member or one part of the body and is associated with trigger points. 10 The principal factor leading to this condition is misuse of the musculature due to a lack of physical activity, to trauma or compressions. In this patient, the predisposing factor was the presence since infancy of a tufted angioma, which hampered muscle use as a result of the localized pain. The most important part of the diagnostic process is the physical examination, in which the physician must carefully palpate the painful region to identify the trigger points. 9,10 During treatment, some basic steps should be followed: administration of drugs, local therapy and correction of the perpetuating factors. 11 In the present case, the difficulty in managing the tufted angioma by ablative procedures 12 and the added complication of the patient being unable to use interferon during her pregnancy made it impossible to exclude the perpetuating factor. 2,8 The fact that the lesion was stabilized and that no major structures were affected permitted expectant management to be implemented. The drugs indicated range from analgesics to tricyclic antidepressants, depending on the severity of the condition. 11 Local interventions are more effective in inactivating the trigger points. Improvements in muscle function may be achieved by exercise or procedures such as lidocaine infiltration performed directly into the trigger points. In this patient, treatment was initiated with tricyclic antidepressants and an anesthetic block was performed, resulting in an improvement in pain and in the movement of the affected limb after two applications. In certain situations, exclusion of the precipitating factor is impossible and pain relief is the only form of control. 9
The case presented here consisted of a rare coexistence of two conditions: tufted angioma and myofascial pain syndrome. The difficult diagnosis of this syndrome highlights the importance of consultations with other specialists. Since tufted angioma is a chronic, generally painful condition that usually begins in childhood, although it may stabilize soon after puberty, it may result in the development of myofascial pain syndrome. Based on the fact that definitive treatment is difficult, oral and local analgesia, as used in this patient up to the time she became pregnant, represents an excellent therapeutic option and should be considered whenever major structures are unaffected.
REFERENCES
-
1Heagerty AH, Rubin A, Robinson TW. Familial tufted angioma. Clin Exp Dermatol. 1992;17:344-5.
-
2Wong S-N, Tay YK. Tufted angioma: a report of five cases. Pediatr Dermatol. 2002;19:388-93.
-
3Herron MD, Coffin CM, Vanderhooft SL. Tufted angiomas: variability of the clinical morphology. Pediatr Dermatol. 2002;19:394-401.
-
4McKenna KE, McCusker G. Spontaneous regression of a tufted angioma. Clin Exp Dermatol. 2000;25:656-658.
-
5Jang KA, Choi JH, Sung KJ, Moon KC, Koh JK. Congenital linear tufted angioma with spontaneous regression. Br J Dermatol. 1998;138:912-4.
-
6Lam WY, Mac-Moune Lai F, Look CN, Choi PC, Allen PW. Tufted angioma with complete regression. J Cutan Pathol. 1994;21:461-6.
-
7Satter EK, Graham BS, Gibbs NF. Congenital tufted angioma. Pediatr Dermatol. 2002;19:445-7.
-
8Bernstein EF, Kantor G, Howe N, Savit RM, Koblenzer PJ, Uitto J. Tufted angioma of the thigh. J Am Acad Dermatol. 1994;31:307-11.
-
9Yeng LT, Kazyiama H. Síndrome dolorosa miofascial. Rev Med. 2001;80:94-110.
-
10Sande LP, Parizzoto N, Castro CES. Síndrome dolorosa miofascial - Artigo de Revisão. Rev Bras Fisioter. 1999;4:1-9.
-
11Simons DG. Understanding e effective treatments of myofascial trigger points. J Bodyw Mov Ther. 2002;6:81-8.
-
12Cardoso AEO, Tayti T, Oliveira JP, Torezan LA, Sotto MN, Vilela MA, et al. Angioma em tufos: relato de um caso tratado com laser corante pulsado. An. Bras. Dermatol. 2006;81(5 Supl 3):S273-6.
Publication Dates
-
Publication in this collection
21 Mar 2011 -
Date of issue
Feb 2011
History
-
Accepted
11 May 2010 -
Received
07 Oct 2009