Abstracts
It is reported the case of a 21-year-old female bather with a skin lesion, heart-shaped ,characteristic of attack by jellyfish
Cnidaria; Cnidarian venoms; Heart; Hydrozoa
Demonstra-se lesão dermatológica, em caprichoso formato de coração, característica de ataque por caravela-portuguesa, em banhista do sexo feminino, 21 anos
Cnidários; Coração; Hidrozoários; Venenos de cnidários
ICONOGRAPHY
Comparative dermatology: skin lesion produced by attack of jellyfishes (Physalia physalis)*
Maria do Carmo Araújo Palmeira QueirozI; Juliana Nascimento de Andrade Rabelo CaldasII
ISpecialist - Dermatologist from the Dermatology Service at the Onofre Lopes University Hospital - Federal University of Rio Grande do Norte (UFRN) - Natal (RN), Brazil
IISpecialist - Dermatologist - Natal (RN), Brazil
Mailing address
ABSTRACT
It is reported the case of a 21-year-old female bather with a skin lesion, heart-shaped ,characteristic of attack by jellyfish.
Keywords: Cnidaria; Cnidarian venoms; Heart; Hydrozoa
The jellyfish (Physalia physalis), (Figure 1)1 belongs to the animal kingdom, phylum Cnidaria (cnida = nettle in greec), class Hydrozoa.2 The phylum Cnidaria is composed of aquatic animals with radial structure that present tentacles around the oral cavity. There are, in each tentacle, inumerous oval bodies nameded nematocysts, capable of injecting venom by a stinging filament that is triggered when the cell is touched.3 The jellyfish is responsible for the the greatest and most serious number of accidents of this type in Brazil, specially in the summmer.4
The attack by Physalia physalis can lead to toxic damages (erythema, edema, necrosis, direct action to the myocardium, nervous tissue, hepatic and renal) and allergic damages (early and late), including anaphylaxis, urticaria and granuloma formation.3 Pain begins immediately after exposure. Delayed reactions can present increased levels of IgG, responses mediated by T cells and cross reaction with all types of jellyfish venom.2
In case of an accident it is essential to ask how it happened, the elapsed time, description of the jellyfish and local and systemic symptoms. The seriousness depends on many factors such as : number of nematocysts discharged, health and age of the patient, weight, affected body area, impairment of the extremities (50% more severe), location and tickness of the affected skin (near the head and chest, absorption of the poison is faster). Medical literature reports two deaths caused by this type of jellyfish.2
Treatment consists of deactivation of nematocysts, pain control, support to the vital organs affected and, if necessary, use of antidote againt jellyfish poisoning. The laboratories that produce these immuno derivatives in Brazil are: Butantan Institute -SP, Ezequiel Dias Foundation - MG and Vital Brazil Institute - RJ.4
Deactivation of nematocysts is carried out through physiological saline washing and/or immersion of the injury in 5% acetic acid or 70% isoprophyl alcohol, from 15 to 30 minutes. As a last resort, sea water can be used knowing that it can bring marine pathogens to the wound. Removal of nematocysts can be made covering the area with shaving cream, talcum powder and sodium bicabornate for a period of one hour. After that, one should use a blunt object to remove the lesion.5 A powerful adhesive tape can be put on the lesion and it should be immediately removed. Pain tends to decrease with the use of cold compress from 5 to 10 minutes. Avoid using ice directely on the area as hypotonic ice water stimulates non removed nematocysts. Do not use hot compresses as they increases systemic absorption of the venom. Clean the area three times a day and apply topical antibiotics such as chloramphenicol or erythromycin, effective for marine pathogens.2 Use antihistamines and topical or systemic steroids in case of important local reactions and to minimize adverse reaction to the antidote. Use muscle relaxants in case of serious spasms and tetanus prophylaxis and systemic antibiotics in case of secondary infection.
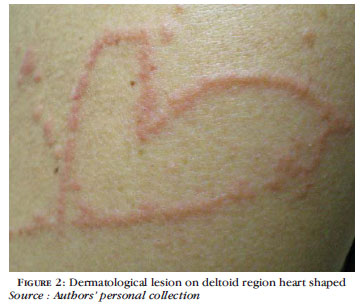
The dermatological lesion observed on the right deltoid region of the patient (Figure 2), resembles a heart (Figure 3). The heart is a muscular organ that pumps the blood and makes it circulates in the body. Figuratively it refers to sensibility, affection and love.
REFERENCES
- 1. Olhares fotografia on line [Internet] - Foto de Ribeiro R.; publicado em 28 de novembro de 2004. [acesso 19 Dez. 2009]. Disponível em: http://br.olhares.com/caravela_portuguesa_foto72332.html
- 2. Cristián VK, Marianne KR, María Soledad ZT, Francisco VK, Juan Pedro LJ. Picadura de medusas: actualización. Rev Méd Chile. 2004;132:233-41.
- 3. Haddad V, Lupi O, Lonza JP, Tyring SK. Tropical dermatology: Marine and aquatic dermatology. J Am Acad Dermatol. 2009;61:733-59.
- 4. Saude.gov.br [Internet]. Manual de Diagnóstico e Tratamento de Acidentes por Animais Peçonhentos, 2001 [acesso 04 Out. 2009]. Disponível em: http://portal.saude.gov.br/portal/arquivos/pdf/manu_peconhentos.pdf
- 5. Fischer AA. Atlas of Aquatic Dermatology. New York: Grune & Stratton; 1978.
Publication Dates
-
Publication in this collection
21 June 2011 -
Date of issue
June 2011
History
-
Accepted
13 Sept 2010 -
Received
23 July 2010