Abstracts
Acute Hemorrhagic Edema of Infancy is an infrequent leukocytoclastic vasculitis which occurs almost exclusively in children between 4 months and 2 years of age. It is clinically characterized by the triad fever, purpuric lesions on the face, auricular pinna and extremities, and edema. Although the cutaneous findings are dramatic and of rapid onset, the prognosis is favorable, with spontaneous resolution within 1 to 3 weeks. Three cases are described in which clinical and histopathological findings are characteristic of acute hemorrhagic edema of infancy.
Edema; Purpura, Schoenlein-Henoch; Vasculitis
O Edema Agudo Hemorrágico da Infância é uma vasculite leucocitoclástica pouco frequente, que ocorre, quase exclusivamente, em crianças entre 4 meses e 2 anos de idade. Caracteriza-se, clinicamente, pela tríade febre, lesões purpúricas na face, pavilhões auriculares e extremidades e edema. Embora os achados cutâneos sejam dramáticos e de surgimento rápido, o prognóstico é favorável, com resolução espontânea dentro de 1 a 3 semanas. Descrevem-se três casos cujos achados clínicos e histopatológicos são característicos de edema agudo hemorrágico da infância.
Edema; Púrpura de Schoenlein-Henoch; Vasculite
CASE REPORT
Acute hemorrhagic edema of infancy: report of three cases*
Paulo Sergio EmerichI; Patricia Almeida PrebianchiII; Luciene Lage da MottaIII; Elton Almeida LucasIV; Leonardo Mello FerreiraV
IDermatologist - Medical Preceptor and physician in charge of the Dermatological Clinic at the Children's Hospital (Clínica Dermatológica, Hospital Infantil Nossa Senhora da Glória - HINSG) - Vitória (ES), Brazil
IIPediatrician Infectologist at the Children's Hospital (Hospital Infantil Nossa Senhora da Glória - HINSG) - Vitória (ES), Brazil
IIIPathologist at the Children's Hospital (Hospital Infantil Nossa Senhora da Glória - HINSG) - Vitória (ES), Brazil
IVPathologist - Adjunct Professor IV of Pathology at the Federal University of Espírito Santo (Universidade Federal do Espírito Santo - UFES) - Vitória (ES), Brazil
VDermatologist at the Federal University of Espírito Santo (Universidade Federal do Espírito Santo - UFES) - Vitória (ES), Brazil
Mailing address
ABSTRACT
Acute Hemorrhagic Edema of Infancy is an infrequent leukocytoclastic vasculitis which occurs almost exclusively in children between 4 months and 2 years of age. It is clinically characterized by the triad fever, purpuric lesions on the face, auricular pinna and extremities, and edema. Although the cutaneous findings are dramatic and of rapid onset, the prognosis is favorable, with spontaneous resolution within 1 to 3 weeks. Three cases are described in which clinical and histopathological findings are characteristic of acute hemorrhagic edema of infancy.
Keywords: Edema; Purpura, Schoenlein-Henoch; Vasculitis
INTRODUCTION
Acute Hemorrhagic Edema of Infancy (AHEI) is a rare cutaneous illness that affects almost exclusively children between 4 months and 2 years of age.1
It was initially described in the United States by Snow, in 1913, under the title of "Purpura, urticaria and angioneurotic edema of the hands and feet in a nursing baby".2 Since then, some cases have been also reported in Europe, as Finkelstein's Disease and Seidlmayer Syndrome. It is rarely reported in American literature, probably because in the United States AHEI is called Henoch-Schönlein Purpura (HSP) in infants.3
The causes of AHEI are unknown; some authors consider the disease as a purely cutaneous form of HSP, while others believe it is a distinct entity within the leukocytoclastic vasculites spectrum.4
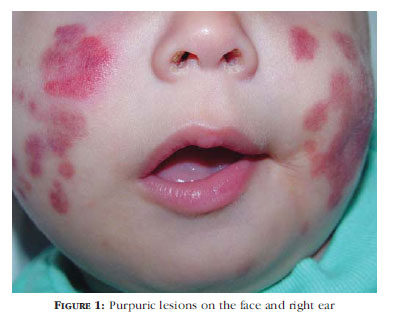
It is clinically characterized by the triad fever, purpuric lesions and edema. The purpuric lesions are located on the face, auricular pinna and extremities, sparsely on the trunk and accompanied by edema of the scalp, extremities and occasionally the genital region.5
Although the cutaneous findings are dramatic and of rapid onset, the prognosis is favorable, with spontaneous resolution within 1 to 3 weeks.1
The association of fever and purpuric lesions is a challenge to the physician. In the universe of diseases that develop with this association we should always think of Henoch-Schönlein Purpura, meningococcemia and septicemia, the main differential diagnosis of AHEI.
The authors report three clinical cases of AHEI treated at the Children's Hospital (Hospital Infantil Nossa Senhora da Glória) in Vitória/ES. As it is a rare illness whose differential diagnosis is made with potentially severe systemic diseases, we emphasize the importance of its early recognition.
CASE REPORTS
Case 1
A 5-month-old male nursing baby, white, born and resident in Alfredo Chaves /ES presented erythematous-violaceous lesion on the face, ears and extremities accompanied by edema for three days (Figure 1). The patient had low fever, irritability and good overall health, with upper respiratory tract infection antecedents.
Supplementary tests: the leukogram showed leukocytosis accompanied by a left shift and thrombocytosis; urinalysis was normal, antistreptolysin O (ASO) was 200 U Todd.
Case 2
A 22-month-old male child of mixed race (mulatto, was brought to the Emergency Department with purpuric cutaneous lesions on upper limbs, lower limbs and face accompanied by periorbital, extremities and scrotum edema, as well as low fever for 24 hours (Figure 2). Upper respiratory tract infection for 20 days was reported.
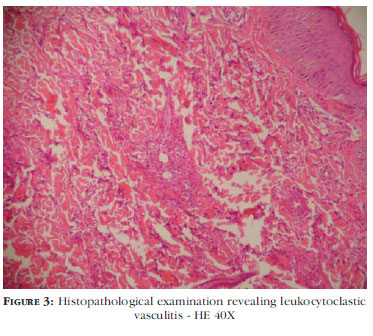
Supplementary tests: normal leukogram, moderate anemia and thrombocytosis; urinalysis normal; coagulation tests normal. The histopathological test revealed leukocytoclastic vasculitis (Figures 3 and 4).
Case 3
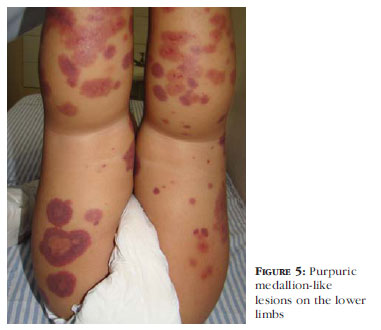
A 10-month-old male nursing baby presented purpuric cutaneous lesions on face and limbs for 2 days, with irritability and good overall health. Upper respiratory tract infection antecedents (Figure 5). The patient had low fever.
Supplementary tests: erythrogram, leukogram and platelets normal, ASO 200 U Todd, urinalysis normal; coagulation tests normal.
DISCUSSION
AHEI is a rare leukocytoclastic vasculitis. Ever since it was first described in 1913, approximately 100 cases of this illness have been reported worldwide.6 Most cases occur in the winter, probably precipitated by upper respiratory tract infections, immunizations and hypersensitivity to drugs. Staphylococci, streptococci, adenoviruses, Escherichia coli and mycobacteria have also been implicated as probable triggering agents.1,7
The marked characteristic of the disease is the aspect of the lesions, similar to medallions: annular purpuric plaques with well-defined borders and central vascular patterns, located on the face and extremities. The lesions reach up to 5 centimeters in diameter, are not pruritic and a painful subjacent edema is observed mainly on feet, hands, scalp and scrotum. Some may present areas of necrosis. There is contrast between the important cutaneous affection and the child's good overall health.8-13
The diagnosis is essentially clinical. Eosinophilia, leukocytosis and thrombocytosis may be found in peripheral blood. Erythrocyte sedimentation rate is normal or slightly elevated. Serum complement levels are normal.14 Other exams, such as coagulation tests, urine sediments, kidney and liver function, ASO, immunoglobulin A (IgA) and immunoglobulin M (IgM), antinuclear factor, VDRL are normal. Systemic affection is rare, as well as lesion recurrence.15
The histopathological findings are leukocytoclastic vasculitis affecting small dermal vessels, rarely extending to the subcutaneous, fibrinoid necrosis, red blood cell leakage and interstitial edema. Direct immunofluorescence (DIF) reveals deposits of complement 3 (C3), fibrinogen and IgM. Immunoglobulin A, immunoglobulin G and immunoglobulin E may be observed at a much lower frequency.9
Henoch-Schönlein Purpura is the main differential diagnosis of AHEI, with significant differences between the two illnesses: HSP affects with greater frequency children between 3 and 7 years of age, the lesions are mainly papular/petechial, located on lower limbs and rarely present subjacent edema. Systemic involvement is more common in HSP, with an average duration of 30 days and frequent recidivism. Fibrinoid necrosis rarely occurs and DIF reveals IgA deposits. Other important differential diagnoses of AHEI include: neonatal lupus erythematosus, Sweet's syndrome, erythema multiforme, Gianotti-Crosti disease and Kawasaki disease.15
There is no specific treatment for AHEI. Antibiotics are used when there is secondary infection. Corticosteroids and antihistaminics may be used, but there is no evidence that these medications bring any benefit.7
ACKNOWLEDGEMENT
Our grateful acknowledgment to Drs. Eloísa Targueta, Valéria Ceotto and Isabel Machado Carvalho for referring patients to the Dermatological Clinic Service of HINSG.
REFERENCES
- 1. Lernia VDI, Lombardi M, Scocco GL. Infantile Acute Hemorrhagic Edema and Rotavirus infection. Pediatr Dermatol. 2004; 21:548-50.
- 2. Caksen H, Odabas D, Kösen M, Arslan S, Ö.ner AF, Atas B, et al. Report of eight infants with Acute Infantile Hemorrhagic Edema and review of the literature. J Dermatol. 2002;29:290-5.
- 3. Amitai Y, Gillis D, Wasserman D, Kochman RH. Henoch-Schöenlein purpura in infants. Pediatrics. 1993;92:865-67.
- 4. Paradisi M, Annessi G, Corrado A. Infantile Acute Hemorrhagic Edema of the skin. Cutis. 2001;68:127-9.
- 5. Cabrera Roca G, Domínguez Ortega F, Perdomo Mesa E, Medina Calvo F, Báez Marrero O. Acute hemorrhagic edema in a nursing infant: a report of 5 cases. An Esp Pediatr. 1998;48:73-5.
- 6. Roh MR, Chung HJ, Lee JH. A case of acute hemorrhagic edema of infancy. Yonsei Med J. 2004;45:523-26.
- 7. Gonggryp LA, Todd G. Acute hemorrahagic edema of childhood. Pediatr Dermatol. 1998;15:91-6.
- 8. Legrain V, Lejean S, Taïeb A, Guillard JM, Battin J, Maleville J. Infantile acute hemorrhagic edema of skin: study of ten cases. J Am Acad Dermatol. 1991;24:17-22.
- 9. Krause I, Lazarov A, Rachmel A, Grunwald MM, Metzker A, Garty BZ, et al. Acute haemorrhagic oedema of infancy, a benign variant of leucocytoclastic vasculitis. Acta Paediatr. 1996;85:114-7.
- 10. Lon D, Helm KF. Acute hemorrhagic edema of infancy: Finkelstein disease. Cutis. 1998;61:283-4.
- 11. Caliskan S, Tasdan Y, Kasapcopur O, Sever L, Tunnessen WW. Acute hemorrhagic edema of infancy. Arch Pediatr Adolesc Med. 1995;149:1267-8.
- 12. Emerich P, Neves A, Machado I, Fagundes S, Almeida P. Edema agudo hemorragico de la infancia .Dermatol Pediatr Lat. 2005;3:234-38.
- 13. Criado PR, Valente NYS, Criado RFJ, Sittart JA, Sawaya S. Edema Agudo Hemorrágio do lactente. An Bras Dermatol. 1996;71:403-6.
- 14. Lantner RR, Simon PR. Acute hemorrhagic edema of unfancy. Pediatr Emerg Care. 1996;12:111-2.
- 15. Goulart FB, Lage KST, Quintero MV, Pádua PM. Edema Agudo Hemorrágico da Infância. Rev Bras Reumatol. 2004;44:251-4.
Publication Dates
-
Publication in this collection
23 Jan 2012 -
Date of issue
Dec 2011
History
-
Received
04 Sept 2010 -
Accepted
12 Sept 2010