Abstracts
Diffuse plane normolipemic xanthomatosis (DPNX) is a rare, non-inherited disease that is often associated with systemic diseases, mainly malignant hematological (especially multiple myeloma) or lymph proliferative disorders. The DPNX can precede the appearance of such conditions by several years, so careful follow-up and periodic laboratory examinations are recommended even for patients that seemed to have no underlying disease. We describe a case associated with monoclonal gammopathy. This case shows that dermatological lesions can be the first manifestation of important hematological diseases and so physicians should be familiarized with this entity
multiple Myeloma; Paraproteinemias; Xanthomatosis
A xantomatose plana difusa normolipêmica (XPDN) é uma dermatose adquirida rara, muitas vezes associada a doenças sistêmicas, nomeadamente neoplasias hematológicas(sobretudo o mieloma múltiplo) ou a processos linfoproliferativos. A XPDN pode preceder o aparecimento dessas doenças em vários anos, sendo por isso recomendada uma vigilância clínica e laboratorial periódica, mesmo para os doentes que aparentemente não apresentam uma doença associada. Descrevemos um caso associado à gamopatia monoclonal. Este caso demonstra a importância das manifestações cutâneas como primeira manifestação de doenças hematológicas importantes e por isso os clínicos devem estar familiarizados com esta entidade
Mieloma múltiplo; Paraproteinemias; Xantomatose
CASE REPORT
Diffuse plane xanthomatosis associated with monoclonal gammopathy* * Work performed at Centro Hospitalar do Porto, EPE - Hospital Santo António (HSA) - Porto, Portugal.
Xantomatose plana difusa associada a gamopatia monoclonal
Aristóteles RosmaninhoI; Iolanda FernandesI; Arlindo GuimasII; Isabel AmorimIII; Manuela SeloresIV
IPhysician, Intern in Dermatovenereology - Centro Hospitalar do Porto, EPE - Hospital Santo António (HSA) - Porto, Portugal
IIPhysician, Specialist in Internal Medicine - Centro Hospitalar do Porto, EPE - Hospital Santo António (HSA) - Porto, Portugal
IIIPhysician, Graduated Hospital Assistant in Dermatovenereology - Centro Hospitalar do Porto, EPE - Hospital Santo António (HSA) - Porto, Portugal
IVPhysician, Director of the Dermatovenereology Service - Centro Hospitalar do Porto, EPE - Hospital Santo António (HSA) - Porto, Portugal
Mailing address Mailing address: Aristóteles Rosmaninho Rua D. Manuel II, s/nº Edifício das Consultas Externas EX-CICAP 4099-001 Porto, Portugal E-mail: arisrosmaninho@gmail.com
ABSTRACT
Diffuse plane normolipemic xanthomatosis (DPNX) is a rare, non-inherited disease that is often associated with systemic diseases, mainly malignant hematological (especially multiple myeloma) or lymph proliferative disorders. The DPNX can precede the appearance of such conditions by several years, so careful follow-up and periodic laboratory examinations are recommended even for patients that seemed to have no underlying disease. We describe a case associated with monoclonal gammopathy. This case shows that dermatological lesions can be the first manifestation of important hematological diseases and so physicians should be familiarized with this entity.
Keywords: multiple Myeloma; Paraproteinemias; Xanthomatosis
RESUMO
A xantomatose plana difusa normolipêmica (XPDN) é uma dermatose adquirida rara, muitas vezes associada a doenças sistêmicas, nomeadamente neoplasias hematológicas(sobretudo o mieloma múltiplo) ou a processos linfoproliferativos. A XPDN pode preceder o aparecimento dessas doenças em vários anos, sendo por isso recomendada uma vigilância clínica e laboratorial periódica, mesmo para os doentes que aparentemente não apresentam uma doença associada. Descrevemos um caso associado à gamopatia monoclonal. Este caso demonstra a importância das manifestações cutâneas como primeira manifestação de doenças hematológicas importantes e por isso os clínicos devem estar familiarizados com esta entidade.
Palavras-chave: Mieloma múltiplo; Paraproteinemias; Xantomatose
INTRODUCTION
Diffuse plane normolipemic xanthomatosis (DPNX) is a rare, non-inherited disease first recognized by Altman and Winkelman in 1962.1 Clinically the dermatosis is characterized by the presence of symmetric yellowish flat or slightly elevated plaques distributed in the tegument. Sites of predilection are the face (mainly periocular areas), neck, upper trunk and flexural folds.2,3,4 Usually extensive xanthelasma palpebrum is present at the time of diagnosis and serum lipids are in the normal levels.1 DPXN has been associated with systemic diseases, particularly multiple myeloma and monoclonal gammopathy.3 However, other malignant hematological or lymph proliferative disorders, such as acute monoblastic leukemia, chronic myelomonocytic leukemia, chronic myeloid leukemia, chronic lymphatic leukemia, lymphoma, adult T-cell lymphoma/leukemia, Sézary syndrome, histiocytosis X, Waldenstrom's macroglobulinaemia, cryoglobulinemia and Castleman's disease have been reported in association with DPNX.3,5,6 The skin lesions can occur simultaneously with or after the diagnosis of such conditions but it can precede it in several years.3,7
CASE REPORT
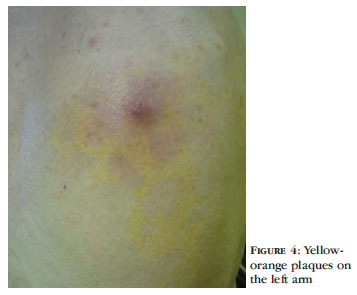
An 84-year-old man presented with a 2-year history of well-demarcated, flat, soft, slightly infiltrated yellow-orange plaques localized to his upper back and proximal arms (Figures 1, 2, 3 and 4). The lesions began in the arms and extended to his back. Otherwise he was asymptomatic. The lesions were not recognized as being significant by his physicians at its onset. He denied systemic symptoms. On physical examination there were no palpable adenomegalies and no xanthelasma palpebrarum was observed. His medical history consisted only of hypertension. His personal and familiar history was negative for hyperlipidemia and xanthoma.
The diagnosis of DPNX was suspected and further work-up was done to rule out a paraneoplastic underlying disease. Laboratory investigations revealed a platelet count of 138 000/uL, ESR of 45 mm/h (< 30), serum Ig G of 1650 mg/dl (< 1590). Values for liver, renal, thyroid function tests, auto-antibodies, cryogobulins, total cholesterol, low-density lipoprotein, high-density lipoprotein, triglycerides, IgA, IgM and total protein were within the normal range. Serum protein immunoelectrophoresis showed an IgG k monoclonal gammopathy. There was no Bence-Jones proteinuria. Bone marrow biopsy revealed a normocellular population and 4% of plasma cells. A skin biopsy from an arm lesion was performed and hematoxylin - eosin stains showed in the superficial dermis histiocytes with vacuolated foamy cytoplasm and an admixture of inflammatory cells, mainly lymphocytes (Figure 5). All the above was consistent with the diagnosis of DPNX associated with a monoclonal gammopathy of undetermined significance (MGUS).
DISCUSSION
DPNX is strongly associated with hematological disorders and for some authors, only some cases can be regarded as idiopathic.3 Thus, whenever the disease is suspected further work-up should be done in order to exclude malignancy, mainly multiple myeloma. A predominant association of DPNX with paraproteinemia of light-chain immunoglobulins seems to occur with the λ isotype prevailing.8,9 As in our case, an extensive cutaneous involvement is in favor of an underlying systemic disease; multiple myeloma as well as other hematological, lymph proliferative disorders were ruled out and a MGUS was considered the underlying cause of DPNX. MGUS is an asymptomatic genetically malignant but clinically premalignant clonal plasma cell proliferative disorder. 3 It is typically detected as an incidental finding when patients undergo a protein electrophoresis as part of a work up for a wide variety of clinical symptoms and disorders such as vasculitis or skin rashes. MGUS is diagnosed by meeting the following three criteria: the presence of a serum monoclonal protein, at a concentration <3 g/dL; fewer than 10 percent clonal plasma cells in the bone marrow and absence of lithic bone lesions, anemia, hypocalcaemia, and renal insufficiency related to the plasma cell proliferative process. The proposed pathogenic mechanism for DPNX associated with gammopathy is that lipids abnormalities are produced because of a specific interaction between a monoclonal immunoglobulin and lipoprotein metabolism occurs. In result, paraprotein-lipoprotein complexes (IgG-LDL) are formed and deposited around the dermal vessels. Those complexes may be recognized as modified LDL by scavenger macrophages leading to development of cutaneous xanthomas.7,8 For this reason, DPNX is considered a histiocytosisderived xanthomatosis (histiocytic lipidization).5 Since the first time that the association between paraproteins and DPNX has been suggested, 21 cases with multiple myeloma and xanthomatosis have been confirmed as having lipoprotein-paraprotein complexes. 8 The deposition of the complexes seems to be influenced more by the properties of the complexes rather than the lipid levels, explaining why most of the patients have normal serum lipid levels.10,11 Histopathological examination shows histiocytic foamy cells diffusely spread in the upper dermis with and an admixture of histiocytes and lymphocytes. The histopathology features have no correlation with the underlying systemic disease.3 DPNX can precede the appearance of the hematopoietic disorders by several years, so careful follow-up and periodic laboratory examinations are recommended even for patients that seemed to have no underlying disease.3,7 The development of multiple myeloma or a related malignance associated with MGUS seems to occur at the rate of 1% per year.12 Our patient is still under follow-up. Moreover, this case shows that dermatological lesions can be the first manifestation of important hematological diseases and so physicians should be familiarized with this rare entity. 
Recebido em 22.10.2010.
Aprovado pelo Conselho Consultivo e aceito para publicação em 06.10.2010.
Conflict of interest: None
Financial funding: None
-
1Altman J. Winkelmann RK. Diffuse normolipemic plane xanthoma. Arch Dermatol. 1962;85:633-40.
-
2Stockman A, Delanghe J, Geerts M, Naeyaert JM. Diffuse normolipidemic plane xanthomas in a patient with chronic lymphatic leukaemia and monoclonal gammopathy. Dermatology. 2002;204:351-4.
-
3Marcoval J, Moreno A, Bordas X, Gallardo F, Peyrí J. Diffuse plane xanthoma: Clinicopathologic study of 8 cases. J Am Acad Dermatol. 1998;39:439-42.
-
4Silva DM, Chacha JJ, Wiziack NC, Takita LC, Hayashi FK. Xantoma plano difuso normolipêmico idiopático com hiperesplenismo. An Bras Dermatol. 2010;85:73-6.
-
5Lynch PJ, Winkelmann RK. Generalized plane xanthoma and systemic disease. Arch Dermatol. 1996;93:639-49.
-
6Kim KJ, Lee DP, Suh HS, Lee MW, Choi JH, Moon KC, Koh JK. Diffuse plane xanthomas in a patient with chronic myeloid leukaemia. J Dermatol. 2004;31:503-5.
-
7Loo DS, Kang S. Diffuse normolipidemic plane xanthomas with monoclonal gammopathy presenting as urticarial plaques. J Am Acad Dermatol. 1996;35:829-32.
-
8Taylor JS, Lewis LA, Battle JD Jr, Butkus A, Robertson AL, Deodhar S, et al. Plane xanthoma and multiple myeloma with lipoprotein-paraprotein complexing. Arch Dermatol. 1978;114:425-31.
-
9Lorenz S, Hohenleutner S, Hohenleutner U, Landthaler M. Treatment of diffuse plane xanthoma of the face with the erbium:YAG laser. Arch Dermatol. 2001;137:1413-5.
-
10Hofmann M, Zappel K, Trefzer U, Audring H, Albrecht-Nebe H, Sterry W, et al. Diffuse normolipemic plane xanthoma in a 9-year old boy. Pediatr Dermatol. 2005;22:127-9
-
11Modiano P, Gillet-Terver MN, Reichert S, François-Griffaton A, Beaumont JL, Weber M, et al. Normolipemic plane xanthoma, monoclonal gammapathy, antilipoprotein activity, hypocomplementemia. Ann Dermatol Venereol. 1995;122:507-8.
-
12Kyle RA, Therneau TM, Rajkumar SV, Larson DR, Plevak MF, Offord JR, et al. Prevalence of monoclonal gammopathy of undetermined significance. N Engl J Med. 2006;354:1362-9.
Publication Dates
-
Publication in this collection
08 Nov 2011 -
Date of issue
Aug 2011
History
-
Received
22 Oct 2010 -
Accepted
06 Oct 2010