Abstracts
Subcutaneous fat necrosis of the newborn is an uncommon disorder occurring during the prenatal stage. Generally occurring in full-term neonates or during the first four weeks after a traumatic delivery, the disorder is characterized by the appearance of hard subcutaneous nodules or plaques on the trunk, buttocks or thighs. It is normally a benign and transient condition, although it may be complicated by hypocalcemia, which requires close monitoring until skin lesions are cured. The authors describe two cases of subcutaneous fat necrosis of the newborn, one occurring in a full-term neonate and the other in a premature newborn, both related to traumatic delivery and fetal distress
Dystocia; Infant, newborn, diseases; Fat necrosis; Hypocalcemia
A necrose adiposa subcutânea do recém-nascido é uma paniculite rara do período neonatal. Surge, geralmente, em recém-nascidos de termo ou pós-termo, nas primeiras 4 semanas de vida, e em associação com trauma obstétrico. Caracteriza-se pelo aparecimento de placas ou nódulos subcutâneos duros, localizados ao tronco, nádegas ou coxas. O seu curso é, geralmente, benigno e autolimitado, embora possa acompanhar-se de hipercalcemia, o que obriga a uma vigilância periódica até à resolução das lesões cutâneas. Os autores descrevem 2 casos de necrose adiposa subcutânea do recém-nascido, um num recémnascido de termo, outro num prematuro, ambos associados a partos traumáticos e a sofrimento fetal
Distocia; Doenças do recém-nascido; Hipercalcemia; Necrose gordurosa
CASE REPORT
Fat necrosis of the newborn: report on two cases*
Ana Cristina Santos OliveiraI; Manuela SeloresII; Olga PereiraIII
IMD, Specialist Internist, Dermatology Department, Santo António Hospital, Porto, Portugal
IIMD, Graduate Hospital Assistant, Dermatology Department, Santo António Hospital, Porto, Portugal
IIIMD, Dermatology Department, Alto Chave Hospital Centre (CHAA), Guimarães, Portugal
Mailing address
ABSTRACT
Subcutaneous fat necrosis of the newborn is an uncommon disorder occurring during the prenatal stage. Generally occurring in full-term neonates or during the first four weeks after a traumatic delivery, the disorder is characterized by the appearance of hard subcutaneous nodules or plaques on the trunk, buttocks or thighs. It is normally a benign and transient condition, although it may be complicated by hypocalcemia, which requires close monitoring until skin lesions are cured. The authors describe two cases of subcutaneous fat necrosis of the newborn, one occurring in a full-term neonate and the other in a premature newborn, both related to traumatic delivery and fetal distress.
Keywords: Dystocia; Infant, newborn, diseases; Fat necrosis; Hypocalcemia.
INTRODUCTION
Subcutaneous fat necrosis of the newborn is an uncommon dermatosis first described by Harrison and McNee in 1926 1. It is a panniculitis which affects newborn infants, manifested by necrosis and calcification of subcutaneous fat caused by a traumatic birth resulting in hypoperfusion of the subcutaneous tissue. 2 It is a benign self-limited condition normally resolved during the first year of life. It can however be complicated by hypocalcemia, which requires affected patients to be regularly monitored. 3
CASE REPORTS
Case 1:
Female newborn of healthy, non-consanguineous parents. Pregnancy complicated by gestational diabetes, controlled with dietary measures. The newborn was macrosomic (weight 4850g, length 52cm, head circumference 38cm) and had been subjected to a traumatic delivery involving shoulder dystocia and vacuum extraction, with Apgar scores of 4 and 6 at 1 and 5 minutes respectively and the need for endotracheal intubation in the first hour of life. Hospitalized for the first week due to perinatal asphyxia and right side brachial plexus injury.
Hard subcutaneous nodules on the back and bilateral cervical region, developed over approximately 5 days, were observed in the hospital emergency room at 13 days after birth. Physical examination revealed the presence of hard oval-shaped subcutaneous nodules measuring approximately 4x2 cm in the cervical region bilaterally and a 10 cm long string of nodules on the upper right part of the back. The overlying skin was normal (Figures 1 and 2). The remaining physical examination of the child was normal.
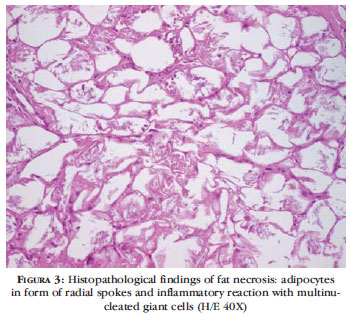
Ultrasonography of soft tissues of the neck and back showed thickening and homogeneous hyperechogenicity of the subcutaneous tissue of the neck and upper back. A skin biopsy showed fat necrosis lesions with areas of dystrophic calcification at the adipose tissue level, confirming the diagnosis of subcutaneous fat necrosis in the newborn. The analytical study revealed no changes, including in the serum calcium values (Figure 3).
Infant kept under observation and showed gradual regression of skin lesions. The serum calcium levels remained within the normal range.
Case 2:
Male newborn, normal delivery at 35 weeks, weighing1840g (light for gestational age), with Apgar scores of 3, 6 and 8 at 1, 5 and 10 minutes respectively and the need for peripartum assisted ventilation.
At 4 weeks two 15mm-diameter well-circumscribed hard nodules with central ulceration were observed in the left parieto-temporal region. Histopathology revealed foci of fat necrosis in the hypodermis. The lesions regressed spontaneously over the following months, leaving atrophic scarring. The serum calcium levels remained within normal limits during the process. 2
DISCUSSION
Subcutaneous fat necrosis of the newborn is a rare form of panniculitis, manifesting in necrosis of the fat tissue of newborn infants at term or post-term following a traumatic delivery.4 This generally occurs during the first 4 weeks of life and resolves spontaneously during the baby's first year. 5
The disorder generally occurs as the result of traumatic delivery, complicated by dystocia, hypothermia, hypoxia/asphyxia or meconium aspiration. 6 It is known that gestational diabetes, cocaine abuse during pregnancy, pre-eclampsia and Rh incompatibility may also be involved 7. The pathogenesis is still not known, but it is presumed that the hypoperfusion of the subcutaneous tissue of the newborn, whose enzymatic system responsible for the desaturation of fatty acids is immature, augments the deposits of saturated fatty acids leading to solidification and necrosis of the fatty tissue. On the other hand, cooling the tissues leads to crystallization of adipocytes, resulting in necrosis. Local pressure arising from delivery-related trauma (distocia or macrosomy) also increases the risk of fat necrosis.
Clinically characterized by areas of edema and erythema that progress to clearly- defined, hard, mobile and painless plaques or subcutaneous nodules in areas subjected to trauma during delivery such as the back, buttocks, thighs, arms and malar regions or more diffuse when associated separately with fetal distress.
The differential diagnoses for consideration include neonatal scleroderma, dermohypodermitis bacterial infections (erysipelas, cellulitis), CMV infection, deep hemangiomas, lipogranulomatosis (Farber disease) and sarcomas, including rhabdomyosarcomas.2,5
Clinical diagnosis reveals a typical history of maternal complications such as gestational diabetes associated with obstetric trauma (usually dystocia) or fetal distress, coupled with typical clinical findings. Imaging tests are usually not required for diagnosis, although they may play an important role in excluding other differential diagnoses. 9,10 The diagnosis can be confirmed by aspiration cytology or skin biopsy. The histology is typical, showing areas of fat necrosis surrounded by a granulomatous reaction consisting of histiocytes, macrophages and giant cells and associated with calcification foci. 2
Clinical case 1 reported above accords with the descriptions in the literature, namely a macrosomic baby born to a mother with gestational diabetes and subjected to a dystocic delivery resulting in a right side brachial plexus injury and perinatal hypoxia. The second clinical case is an unusual case given that it concerns a premature newborn. The fact that light for gestational age was relevant in that it conditioned the peripartum fetal distress and asphyxia. Although rare cases of NASRN are described in preterm infants. 11 The fact that the baby was light for its gestational age was of importance since peripartum fetal distress and asphyxia were involved. Although rare, cases of NASRN have been reported in preterm infants.11
The subcutaneous fat necrosis diagnoses were based on clinical history, typical clinical findings and histopathological examination.
Fat necrosis is a benign pathology which tends to resolve spontaneously in less than a year. It may however be accompanied by extracutaneous changes which, although rare, should be investigated. These changes include hypoglycemia, anemia, thrombocytopenia and hypercalcaemia. Hypercalcaemia (true incidence unknown) is the main complication of this disease and appears on average six months after fat necrosis. 5 It is often accompanied by a refusal to eat, lethargy, irritability, hypotonia, vomiting, polydipsia or polyuria. Some newborn infants nevertheless remain asymptomatic. This complication can lead to high morbidity (and possibly mortality) levels and should always be considered even in the absence of symptoms. Its etiology is not yet known, but it appears to be due to the excessive production of 1.25-dihydroxy-vitamin D by the macrophages, regardless of renal absorption and parathyroid hormone (PTH) levels. 6,12 Infants with this condition must be monitored regularly, both clinically and analytically, until the skin lesions have completely disappeared.
When not associated with hypercalcemia, treatment of this dermatosis is symptomatic.
REFERENCES
-
1Gu LL, Daneman A, Binet A, Kooth SW. Nephrocalcinosis and nephrolithiasis due to subcutaneous fat necrosis with hipercalcemia in two full-termasphyxiated neonates: sonographic findings. Pediatr Radiol. 1995;25:142-4.
-
2Fenniche S, Daoud L, Benmously R, Ben Ammar F, Khelifa I, Chaabane S, et al. Subcutaneous fat necrosis: report of two cases. Dermatol Online J. 2004;10:12.
-
3Corrêa M, Zaniboni MC, Ypiranga S, Arruda LHF. Caso para diagnóstico. Necrose gordurosa. An Bras Dermatol. 2008;83:269-70
-
4Lum CK, Solomon I, Bachrach LK. Asymptomatic hypercalcemia in subcutaneous fat necrosis. Clin Pediatr (Phila). 1999;38:547-50
-
5Canto-Costa MHS, Simão SP, Maas BS, Victório RS. Hipercalcemia secundária à necrose de tecido adiposo subcutâneo. Arq Bras Endocrinol Metab. 2003;47:198-202
-
6Ladoyanni E, Moss C, Brown RM, Ogboli M. Subcutaneous fat necrosis in a newborn associated with asymptomatic and uncomplicated hipercalcemia. Pediatr Dermatol. 2009;26:217-9
-
7Perrotta R, Virzi D, Tarico MS. A rare case of congenital ulcerated subcutaneous fat necrosis of the newborn. J Plast Reconstr Aesthet Surg. 2010;63;e801-2
-
8Dudink J, Walther FJ, Beekman RP. Subcutaneous fat necrosis of the newborn: hiper calcemia with hepatic and atrial myocardial calcification. Arch Dis Child Fetal Neonatal Ed. 2003;88:F343-5
-
9Srinath G, Cohen M. Imaging findings in subcutaneous fat necrosis in a newborn. Pediatr Radiol. 2006;36:361-3
-
10Vasireddy S, Long SD, Sacheti B; Mayforth RD. MRI and US findings of subcuta neous fat necrosis of the newborn. Pediatr Radiol. 2009;39:73-6
-
11Mather MK, Sperling LC, Sau P. Subcutaneous fat necrosis of the newborn. Int J Dermatol 1997;36:435-52
-
12Farooque A, Moss C, Zehnder D, Hewison M, Shaw NJ. Expression of 25-hydroxyvitamin D3-1alpha-hydroxylase in subcutaneous fat necrosis. Br J Dermatol. 2009;160:423-5.
Publication Dates
-
Publication in this collection
08 Nov 2011 -
Date of issue
Aug 2011
History
-
Received
09 Jan 2011 -
Accepted
30 Jan 2011