Abstracts
The umbilicus can be affected by various skin diseases including metastasis of internal malignancies, at which point it is known as Sister Mary Joseph's Nodule. The authors report a case of Sister Mary Joseph's Nodule as the first sign of internal malignancy and highlight the importance for the dermatologist to recognize the condition
Neoplasm metastasis; Ovarian neoplasms; Umbilicus
A cicatriz umbilical pode ser acometida por diversas dermatoses inclusive metástase de neoplasias internas quando então recebe a denominação de nódulo da Irmã Maria José. Os autores relatam um caso de nódulo da Irmã Maria José como primeiro sinal de neoplasia interna destacando desta forma a importância do dermatologista no reconhecimento desta entidade
Metástase Neoplásica; Neoplasias Ovarianas; Umbigo
CASO CLÍNICO
Sister Mary Joseph's nodule: a sign of internal malignancy* * Study undertaken at: Hospital do Servidor Publico Municipal de São Paulo (HSPM - SP), São Paulo (SP), Brazil
Nódulo da Irmã Maria José: um sinal de neoplasia maligna interna
Walter Augusto PereiraI; Caio Rosa HumaireII; Camila Simon SilvaII; Lucia Helena Gomes FernandesII
IAssistant Physician, Dermatology Clinic, Hospital do Servidor Publico Municipal de São Paulo (HSPM-SP), São Paulo (SP), Brazil
IIResident, Dermatology Clinic, Hospital do Servidor Publico Municipal de São Paulo (HSPM-SP), São Paulo (SP), Brazil
Mailing address Mailing address: Caio Rosa Humaire Rua Theo Dutra 90 - Jardim Colombo CEP: 05628-000 São Paulo (SP) - Brazil
ABSTRACT
The umbilicus can be affected by various skin diseases including metastasis of internal malignancies, at which point it is known as Sister Mary Joseph's Nodule. The authors report a case of Sister Mary Joseph's Nodule as the first sign of internal malignancy and highlight the importance for the dermatologist to recognize the condition.
Keywords: Neoplasm metastasis; Ovarian neoplasms; Umbilicus
RESUMO
A cicatriz umbilical pode ser acometida por diversas dermatoses inclusive metástase de neoplasias internas quando então recebe a denominação de nódulo da Irmã Maria José. Os autores relatam um caso de nódulo da Irmã Maria José como primeiro sinal de neoplasia interna destacando desta forma a importância do dermatologista no reconhecimento desta entidade.
Palavras-chave: Metástase Neoplásica; Neoplasias Ovarianas; Umbigo
INTRODUCTION
Sister Mary Joseph, Superintendent Nurse at St. Mary's Hospital in Rochester, found that patients with abdominal and pelvic malignant neoplasm occasionally have an umbilical nodule indicating umbilical metastasis. 1, 2
Hamilton Bailey, an English surgeon, first described this as Sister Mary Joseph's Nodule in 1949 in his book Demonstrations of Physical Signs in Clinical Surgery.2
The first survey of cancer relating to the umbilical area was conducted in 1846 by W H Walshe, who studied 9118 cancer and mortuary registers. This survey identified only two cases. 3
CASE REPORT
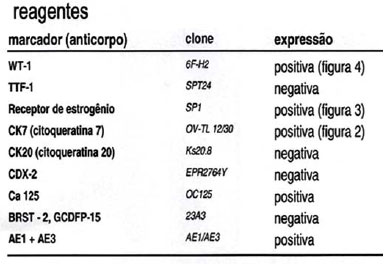
81-year-old female patient with a history of having started bleeding in the umbilical region one month previously (associated with the appearance of a local tumor). Received emergency care and was prescribed cephalexin and acetaminophen for seven days. Failed to improve and was sent to the Dermatology Department. Examination revealed a painless ulcerated erythematous-violaceous umbilical nodule measuring 2x1cm. No bleeding was observed during the examination (Figure 1). A biopsy was performed with anatomopathology, which revealed an infiltrating carcinoma. An immunohistochemistry examination was next performed which showed positive for AE1, AE3, Cytokeratin 7, WT-1, estrogen receptor and CA 125, suggesting a tumor of the genital tract (uterus or ovaries) as the primary site (Figure 2). A transvaginal ultrasound showed the left-side adnexal region with a heterogeneous hypoechoic lesion with cystic and solid components (Figure 3). A contrast CT scan of the abdomen and pelvis showed a complex solid and cystic mass with heterogeneous enhancement located in the region of the uterus and ovary, with 103x96 mm displacement of the posterior bladder wall and thickening of the skin in the abdominal region (Figures 4 and 5). The patient was referred to the gynecology-oncology service where she is still being followed up.
DISCUSSION
Sister Mary Joseph's Nodule is a form of metastasis to the umbilical region where the majority of cases are metastatic adenocarcinoma malignancies. 4 These account for 83% of all malignant tumors in the umbilical region5. Cutaneous metastases occur in between 1% and 9% of cases of malignancies, with around 10% affecting the umbilical region.6 Sister Mary Joseph's Nodule suggests widespread internal neoplasia, usually of the abdominal cavity.The most common primary sites are the gastrointestinal tract (52%) or are gynecological (28%)7. In around 15-29% of cases the primary site is unknown. 8
Clinically characterized by an irregular nodule, painful or not, the nodule may present with ulceration and bloody discharge, purulent or serous. It may also present as an induration of the subcutaneous tissue.9
Three hypotheses for the metastases in the umbilical region exist. The most common form results from contiguity of the internal neoplasia as well as from lymphatic or hematogenous dissemination.
Discovery of this nodule on physical examination may be the first sign of internal malignant neoplasm. Symptoms such as nausea, epigastric pain, weight loss and abdominal distension are often present. 4
Differential diagnoses include umbilical hernia, cutaneous endometriosis, pyogenic granuloma, melancocytic nevus, keloid, melanoma, squamous cell carcinoma and basal cell carcinoma. 2,10,11
In cases where an internal malignancy resection cannot generally be performed the average survival rate is 11 months. Fewer than 15% patients survive after two years. 12 Treatment usually involves palliative care, but the possibility does exist of surgical resection and radiotherapy/chemotherapy. 4
Benign umbilical nodules are called 'pseudo-Sister Mary Joseph's nodules'. 2,13
In this case, the Sister Mary Joseph's Nodule was considered to be the first sign of internal neoplasia, highlighting the need for dermatologists to be vigilant.
The umbilical metastatic cutaneous nodule and anti-CA-125 positivity revealed in the immunohistochemical test, together with the imaging methods employed (ultrasound and CT scan procedures), enabled us to diagnose metastatic ovarian adenocarcinoma.
Received on 01.04.2011.
Approved by the Advisory Board and accepted for publication on 26.04.11.
Conflict of interest: None
Financial funding: None
-
1Pure B, Meirovitz M, Bayme M, Shaco-Levy R. Sister Mary Joseph's nodule originating from endometrial carcinoma incidentally detected during surgery for an umbilical hernia: a case report. Arch Gynecol Obstet. 2006;274:385-8.
-
2Aich RK, Karim R, Chakraborty B, Dasgupta S, Deb AR. Sister Mary Joseph's nodule. Indian J Med Paediatr Oncol. 2008;2:40-3.
-
3Shetty MR. Metastatic tumors of the umbilicus: a review 1830-1989. J Surg Oncol. 1990;45:212-5.
-
4Urbano FL. Sister Mary Joseph Nodule. Hosp Physician May. 2001;44:33-35.
-
5Durieux C, Muysoms F, Claeys D. Sister Joseph's nodule umbilical manifestation of intraperitoneal carcinomatosis. Acta Chir Belg. 2008;108:444-6.
-
6Gabriele R, Conte M, Egidi F, Borghese M. Umbilical metastases: current viewpoint. World J Sur Oncol. 2005;3:13.
-
7Fogaça HS, Chagas VLA, Tolentino YFM, Ribeiro VCM, Ximenes LLL. Sister Mary Joseph's nodule: a warning sign for intra-abdominal malignant tumors: A case report. Rev Bras Ginecol Obstet. 2003;25:449-52.
-
8Dar IH, Kamili MA, Dar SH. Kuchhai FA. Mary Joseph nodule-A case report with review of literature. J Res Med Sci. 2009;14:385-7.
-
9Dubreuil A, Dompmartin A, Barjot P, Louvet S, Leroy D. Umbilical metastasis or Sister Mary Joseph's nodule. Int J Dermatol. 1998;37:7-13.
-
10Limmathurotsakul D, Rerknimitr P, Korkij W, Noppakun N, Kullavanijaya P, Rerknimitr R. Metastatic mucinous cystic adenocarcinoma of the pancreas presenting as Sister Mary Joseph's nodule. JOP. 2007;8:344-9.
-
11Ramirez P , Sendagorta E, Feito M, Gonzalez-Beato M, Mayor M, Pizarro A. Letter: Umbilical basal cell carcinoma in a 21-year-old man: Report of an exceptional case and dermatoscopic evaluation. Dermatol Online J. 2011;17:16.
-
12Shen Z, Yang X, Chen L, Hao F, Zhong B. Sister Mary Joseph's Nodule As a Diagnostic Clue to Metastatic Colon Carcinoma. J Clin Oncol. 2009;27:e1-2.
-
13Aich RK, Karim M, Chakraborty B, Dasgupta S, Deb AR. Sister Mary Joseph's nodule. Indian J Med Paediatr Oncol. 2008;29:40-3.
Publication Dates
-
Publication in this collection
08 Nov 2011 -
Date of issue
Aug 2011
History
-
Accepted
26 Apr 2011 -
Received
01 Apr 2011