Abstracts
The authors report a case (in Itajai, Santa Catarina State, Brazil) of tinea nigra in a 4-year-old female child which spontaneously healed. We discuss the clinical and epidemiological aspects of the mycosis and this rare case of spontaneous healing.
Dermatomycoses; Epidemiology; Mycoses
Os autores relatam um caso de Tinea nigra, observada em uma criança de 4 anos, do sexo feminino, que evoluiu para cura espontânea, ocorrido em Itajaí, Estado de Santa Catarina, Brasil. Discutem-se os aspectos clínicos e epidemiológicos da micose e a rara observação de cura espontânea.
Dermatomicoses; Epidemiologia; Micoses
COMMUNICATION
Spontaneous cure in a case of Tinea nigra* * Study undertaken at the Dermatology Clinic, Vale do Itajai University (UNIVALI), Itajai (SC), Brazil.
Cura espontânea em um caso de Tinea nigra
André Luiz RossettoI; Rosana Cé Bella CruzII
IProfessor of Dermatology at the Vale do Itajai University - UNIVALI, Itajai (SC), Brazil
IIMaster's Degree in Pharmaceutical Biochemistry, Vale do Itajai University - UNIVALI, Itajai (SC), Brazil
Mailing address Mailing address: Dr. André Luiz Rossetto Av. Alvin Bauer, 655 - Sala 203 Centro Médico Vida 88330 643 Balneário Camboriú, SC, Brazil Tel.:/Fax 47 3367 3407 E-mail: rossettovida@terra.com.br
ABSTRACT
The authors report a case (in Itajai, Santa Catarina State, Brazil) of tinea nigra in a 4-year-old female child which spontaneously healed. We discuss the clinical and epidemiological aspects of the mycosis and this rare case of spontaneous healing.
Keywords: Dermatomycoses; Epidemiology; Mycoses
RESUMO
Os autores relatam um caso de Tinea nigra, observada em uma criança de 4 anos, do sexo feminino, que evoluiu para cura espontânea, ocorrido em Itajaí, Estado de Santa Catarina, Brasil. Discutem-se os aspectos clínicos e epidemiológicos da micose e a rara observação de cura espontânea.
Palavras-chave: Dermatomicoses; Epidemiologia; Micoses
INTRODUCTION
Tinea nigra (TN) is a rare chronic and asymptomatic dermatomycosis caused by the fungus Hortae werneckii. 1,2,3 The disorder is known worldwide and is more prevalent in tropical and subtropical coastal areas. 1,3,4 It mainly affects young adults under 20, with a marked tendency to affect females. 1,4 TN usually manifests as a single brownish-blackish asymptomatic macula located on the palmar region, gradually extending to the undersurface of the foot and atypical areas. 1,2,3,4 The condition responds well to topical antifungal therapy and, in rare cases, heals spontaneously according to Bonifaz et al. 5
DISCUSSION
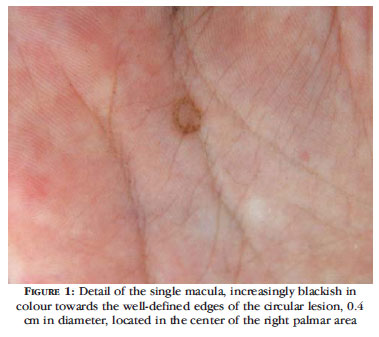
We report the case of a 4-year-old girl from Itajai, (SC) who often played on the nearby beaches. The child's mother reported noticing two months ago a small asymptomatic dark spot on her daughter's right hand which eventually became a black blemish. On dermatological examination, we observed a single, blackish round mark, with well-defined edges, 0.4 cm in diameter, located in the center of the right palmar area (Figure 1). Clinical suspicion of TN was confirmed in the laboratory by direct mycological examination which, after clarification with potassium hydroxide (10- 20%), revealed septate, branched and dematiaceous hyphae with irregular contours. Culture in Sabouraud agar showed after three weeks the growth of shiny colonies, initially white to gray in color and subsequently pigmented (Figure 2). Young colonies of Hortae werneckii were confirmed by microculture with Sabouraud agar at room temperature, where filaments pigmented with annelloconidia were identified. When the mother returned to the clinic with the child she denied any therapy or disappearance of the lesion resulting from scraping the scales in the course of the mycological examination, asserting that the hyperchromic macule had gradually turned white. We observed that the clinical symptoms had regressed completely and spontaneously after 20 days.
In the 120 years since TN was clinically observed for the first time (originally called Keratomycosis nigricans palmaris by Alexandre Cerqueira in 1891 in Bahia), 1,4,6 reports of this disease have been rare, with probably fewer than 100 cases notified in Brazil. 1,4 We found in the literature that the largest series of cases published in the Americas concerned 26 cases in Venezuela (by Alvarado and Rodriguez); and the 13 Brazilian cases published by Cerqueira in 1916. 1,4,7
During the 60th Congress of the Brazilian Society of Dermatology (SBD) in 2005, the authors reported 27 cases observed in the state of Santa Catarina over a ten-year period (1995-2004). The case described above was included in the sample. 8
The Hortae werneckii is a dermatophyte saprophytic fungus that possibly occurs in soil, plants and wood and in places with a high salt concentration such as beach sand. 2,4,6 This fungus was isolated in dry and wet sand taken from the beaches of Itajai in 2006 in an experiment conducted by the authors. 9 The isolation of H.werneckii, even two years after our diagnosis of TN followed by spontaneous healing of the child reported on above, confirmed that the region's beaches were a habitat of the fungus and the possible source of contagion.
In the study by Marques and Camargo, 63.3% of patients with TN were under 20 years of age. According to Giraldi et al, of the 65 Brazilian cases reviewed by 2001 (37 published and 28 presented at conferences, 18 made no mention of the patients'age. 4 Of the 31 patients identified under the age of 19, 18 were still at school (5-13 years old), 8 were teenagers (14-19 years old) and 5 were pre-schoolers (1-4 years). 4 Our reported case concerning a 4-year-old child is consistent with the findings by the authors in the region, especially with regard to the 27 cases where the majority (59.2%) occurred in very young children (1-5 years old). 8
TN affects both sexes. In a review of 31 pediatric patients by Giraldi et al. the female to male ratio was 3.1:1. 4 In the 27 cases observed by the authors in the region, male cases however exceeded those of females in a ratio of 2:1. 8 Our case reported above (female child) is consistent with Brazilian epidemiologic data, 4 but in disagreement with the authors' findings. 8
According to Bonifaz et al. TN rarely evolves to spontaneous healing, and over a period of eleven years (1997-2007) only two cases of spontaneous healing were observed among 22 Mexican cases. 5 In the review of cases by Brazilian authors, only Flaviano Silva (1929) mentioned that the seven-year-old son of the patient affected by the disease presented spontaneous healing of lesions on the neck, demonstrating the rarity of such cases. 10
While infectious diseases can progress to spontaneous healing, patients often do not seek medical help, thus ruling out laboratory diagnosis. In infectious diseases such as asymptomatic TN, many more cases of spontaneous regression are probably undiagnosed because of the reluctance of patients to seek medical help.
Despite the fact that few additional cases of TN were observed in the dermatology clinics (apart from the 27 cases during the 10 year period 1995-2004 mentioned above) 8, the authors nevertheless reported at the 61st SBD Conference that 11 new cases had been observed in the region in 2005 alone. 11
The authors conclude that the case reported here, confirmed by mycological examination, is probably the first time that a case of spontaneously-cured TN identified as the fungus Hortae werneckii has been reported formally in Brazil, despite the high incidence of the condition in the region.
ACKNOWLEDGEMENT
Our thanks to Prof. Vidal Haddad Júnior of the Universidade Estadual Paulista/UNESP Botucatu, SP, and the Instituto Butantan, São Paulo, for his help in revising this text.
Received on 25.03.2010.
Approved by the Advisory Board and accepted for publication on 17.04.2011.
Conflict of interest: None
Financial funding: None
- 1. Marques SA, Camargo RMP. Tinea nigra: relato de caso e revisão da literatura brasileira. An Bras Dermatol. 1996;71:431-5.
- 2. McGinnis MR. Taxonomic of Exophiala werneckii and relationship to Miscrosporum mansonii. Sabouraudia. 1979:17:145-54.
- 3. Zaitz C, Campbell I, Marques AS, Ruiz LRB, Framil VMS. Dermatomicoses por fungos filamentosos septados demácios. In: Zaitz C, Campbell I, Marques AS, Ruiz LRB, Framil VMS. Compêndio de Micologia Médica. 2 ed. Rio de Janeiro: Guanabara Koogan, 2010. p. 180-6.
- 4. Giraldi S, Abbage KT, Marinoni LP, Oliveira VC, Bertogna J. Tinea nigra: relato de seis casos no Estado do Paraná. An Bras Dermatol. 2003;78:593-600.
- 5. Bonifaz A, Badali H, de Hoog GS, Cruz M, Araiza J, Cruz MA, et al. Tinea nigra by Hortaea werneckii, a report of 22 cases from Mexico. Stud Mycol. 2008;61:77-82.
- 6. Cerqueira AG. Keratomycosis nigricans palmaris. [tese]. Salvador (BA): Faculdade de Medicina da Bahia; 1916.
- 7. Alvarado JAR, Rodeiguez H. Tiña nigra en el laboratorio de micologia del servicio de Dermatología del Hospital Universitario de Caracas 1959-1986. Dermatol Venez. 1987;25:47-50.
- 8. Rossetto AL, Cruz RCB, Angelo MV, Correa PR. Tinea nigra: estudo clínico e epidemiológico de vinte e sete casos observados no Vale do Itajaí, Estado de Santa Catarina, durante período de 10 anos. An Bras Dermatol. 2005;80(Supl 2):S124-5.
- 9. Balestieri Filho LA. Isolamento do fungo Hortaea werneckii nas areias secas e úmidas das praias oceânicas de Itajaí, SC, Brasil [monografia]. Itajaí (SC): Universidade do Vale do Itajaí; 2006.
- 10. Silva F. Tinea nigra (Clasdosporose epidérmica). Brasil Med. 1929;43:924-6.
- 11. Rossetto AL, Cruz RCB, Lisboa LC, Jahnke JC, Vargas JV. Tinea nigra: Relato de onze novos casos observados durante o ano de 2005. An Bras Dermatol. 2006;81(Supl 2):S235.
Publication Dates
-
Publication in this collection
02 Apr 2012 -
Date of issue
Feb 2012
History
-
Received
25 Mar 2010 -
Accepted
17 Apr 2011