Abstracts
Folliculitis decalvans is an inflammatory presentation of cicatrizing alopecia characterized by inflammatory perifollicular papules and pustules. It generally occurs in adult males, predominantly involving the vertex and occipital areas of the scalp. The use of dermatoscopy in hair and scalp diseases improves diagnostic accuracy. Some trichoscopic findings, such as follicular tufts, perifollicular erythema, crusts and pustules, can be observed in folliculitis decalvans. More research on the pathogenesis and treatment options of this disfiguring disease is required for improving patient management.
Dermoscopy; Hair diseases; Scalp dermatoses
Dermatoses do couro cabeludo; Dermoscopia; Doenças do cabelo
A foliculite decalvante é uma forma inflamatória de alopecia cicatricial caracterizada por pápulas e pústulas inflamatórias perifoliculares. Ocorre mais comumente em adultos do sexo masculino,envolvendo predominantemente o vértice e a região occipital do couro cabeludo. O uso da dermatoscopia nas doenças dos cabelos e do couro cabeludo melhora a precisão diagnóstica. Alguns achados tricoscópicos como tufos foliculares, eritema perifolicular, crostas e pústulas podem ser observados na foliculite decalvante.Mais pesquisas sobre patogênese e opções de tratamento desta doença desfigurante são necessárias para uma melhor gestão dos pacientes.
INTRODUCTION
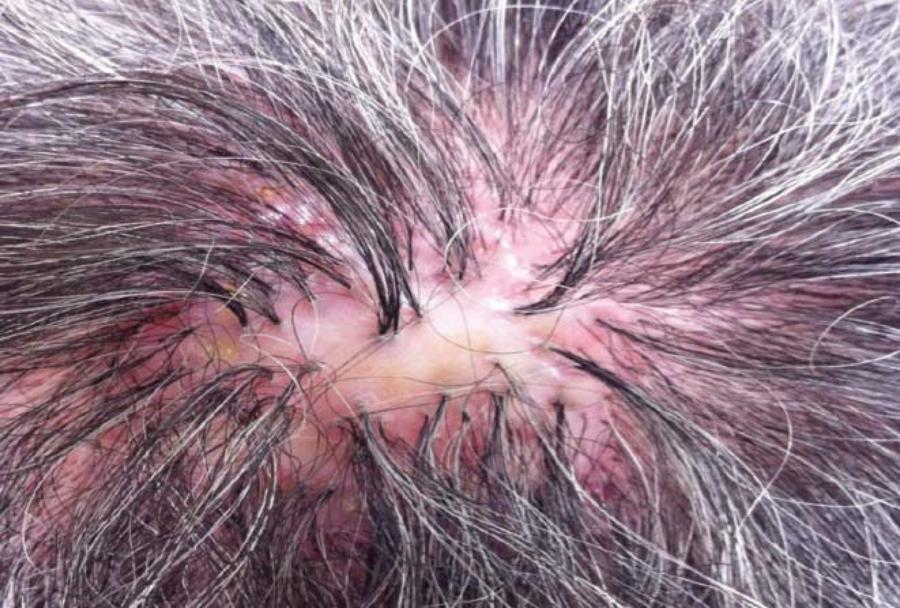
Folliculitis decalvans (FD) is an inflammatory presentation of cicatrizing alopecia characterized by inflammatory perifollicular papules and pustules. It accounts for approximately 11% of all primary cicatrizing alopecia cases. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol. 1999:140:328-33. , 22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44. The disease was first described by Quinquaud in the 19th century. In 1905, Brocq et al named Quinquaud's clinical findings as Folliculitis decalvans. 22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44. It occurs predominantly in young and middle-aged adults, with a slight preference for the male gender, and appears to be more frequent in people of Afro-American stock. 33. Ross EK, Vincenzi C, Tosti A. Videodermoscopy in the evaluation of hair and scalp disorders. J Am Acad Dermatol. 2006;55:799-806. The etiology of this inflammatory process is not fully understood. However, Staphylococcus aureus scalp colonization has been implicated as a contributing factor. It has been suggested that the mechanism of "superantigens" or cytotoxins that bind to class II MHC can play a role in the pathogenesis of the disease. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol. 1999:140:328-33. , 22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44. The theory of genetic predisposition is supported by reports of FD familial cases. 44. Douwes KE, Landthaler M, Szeimies RM. Simultaneus occurence of foliculitis decalvans capillitis in identical twins. Br J Dermatol. 2000;143:195-7. The vertex and occipital areas of the scalp are especially involved. There is usually only one focus of the disease, which begins with painful follicular papules and pustules and spreads to the back. A large erythematous, thick and hardened alopecia plaque appears, with a centrifugal progression. The hallmark of FD is the development of scars and areas of follicular pustules. Follicular keratosis, erosions and hemorrhagic crusts can be observed. Some patients occasionally report spontaneous bleeding, pain, itching or a burning sensation. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol. 1999:140:328-33. , 22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44. Tuffed folliculitis is a common finding in FD patients, characterized by multiple hairs emerging from one single dilated follicular orifice (polytrichia) (Figure 1). 55. Rudnicka L, Olszewska M, Rakowska A, Slowinska M. Trichoscopy update 2011. J Dermatol Case Rep. 2011;5:82-8 The patient's detailed clinical history, together with a thorough examination of the entire scalp, are important for diagnosis. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol. 1999:140:328-33. , 22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44. , 44. Douwes KE, Landthaler M, Szeimies RM. Simultaneus occurence of foliculitis decalvans capillitis in identical twins. Br J Dermatol. 2000;143:195-7. Pictures of the scalp should be taken at the first clinical visit. A sketch, as well as measurements of the scarred areas, is also a useful aid for monitoring disease progression. Bacterial cultures should be performed from an intact pustule, and a nasal swab with antibiotic sensitivity tests should also be done in order to identify an occult S. aureus strain. 22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44. Trichoscopy is a non-invasive method that can be used in the differential diagnosis of most diseases affecting the hair and scalp. This method improves diagnostic accuracy and may contribute to a better understanding of the pathogenesis of these disorders. 33. Ross EK, Vincenzi C, Tosti A. Videodermoscopy in the evaluation of hair and scalp disorders. J Am Acad Dermatol. 2006;55:799-806. , 55. Rudnicka L, Olszewska M, Rakowska A, Slowinska M. Trichoscopy update 2011. J Dermatol Case Rep. 2011;5:82-8 , 66. Duque-Estrada B, Tamler C, Sodré CT, Barcaui CB, Pereira FB. Dermoscopy patterns of cicatricial alopecia resulting from discoid lupus erythematosus and lichen planopilaris. An Bras Dermatol. 2010;85:179-83. , 77. Rudnicka L, Olszewska M, Rakowska A, Kowalska-Oledzka E, Slowinska M. Trichoscopy: a new method for diagnosing hair loss. J Drugs Dermatol. 2008;7:651-4. , 88. Inui S. Trichoscopy for common hair loss diseases: algorithmic method for diagnosis. J Am Acad Dermatol. 2011;38:71-5.
DISCUSSION
The technique for performing dermatoscopy of the scalp consists of using optical devices
with variable increase. For the analysis, dermatologists can use a manual dermatoscope
(magnification x10) or a videodermatoscope equipped with a range of magnifying lenses
(from X20 to X1000). 33. Ross EK, Vincenzi C, Tosti A. Videodermoscopy in the evaluation of
hair and scalp disorders. J Am Acad Dermatol. 2006;55:799-806. Both the trichoscopic dry
exam and the one with interface liquid are important, because they show different
dermatoscopic findings (Figure 2). The
trichoscopic hallmark of folliculitis decalvans is the presence of multiple hairs
emerging from one single dilated follicular orifice (polytrichia). Generally, these
tufts vary from 5-20 hair shafts per follicular orifice. Additional trichoscopic
findings include perifollicular erythema arranged in a starburst pattern, yellowish
tubular scaling, crusting and follicular pustules. In long-lasting lesions, ivorywhite
and milky-red areas without follicular orifices predominate in trichoscopic images. Dots
are rare, present in fewer than 20% of patients, and there appears to be no
characteristic vascular pattern (Figures 1, 3 and 4). 33. Ross EK, Vincenzi C, Tosti A. Videodermoscopy in the evaluation of
hair and scalp disorders. J Am Acad Dermatol. 2006;55:799-806.
,
55. Rudnicka L, Olszewska M, Rakowska A, Slowinska M. Trichoscopy update
2011. J Dermatol Case Rep. 2011;5:82-8
,
77. Rudnicka L, Olszewska M, Rakowska A, Kowalska-Oledzka E, Slowinska M.
Trichoscopy: a new method for diagnosing hair loss. J Drugs Dermatol.
2008;7:651-4.
8. Inui S. Trichoscopy for common hair loss diseases: algorithmic method
for diagnosis. J Am Acad Dermatol. 2011;38:71-5.
9. Wallace MP, de Berker DA. Hair diagnoses and signs: the use of
dermatoscopy. Clin Exp Dermatol.2010;35:416.
-
1010. Lacarrubba F, Dall'Oglio F, Rita Nasca M, Micali G.
Videodermatoscopy enhances diagnostic capability in some forms of hair loss. Am J
Clin Dermatol 2004;5:205-8. Undertaking dermatoscopy does not replace
histopathological examination, and performing a skin biopsy of an active lesion is
essential for diagnosing FD. Histopathologically, FD has been characterized as a
neutrophilic primary cicatricial alopecia. Early lesions show keratin aggregation and a
dilatation of the infundibulum, combined with numerous intraluminal neutrophils.
Sebaceous glands are destroyed early in the process, and a predominant neutrophilic,
intrafollicular and perifollicular infiltrate can be found. In advanced lesions, this
infiltrate can consist of neutrophils, lymphocytes and numerous plasma cells extending
into the dermis. The infiltrate may also be found around the blood vessels of the
superficial and mid-dermis. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including
tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol.
1999:140:328-33.
,
22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans.
Dermatol Ther. 2008;21:238-44. The differential diagnosis can be done with acne
keloidalis nuchae, erosive pustular dermatosis of the scalp, lichen planopilaris,
discoid lupus erythematous, pseudopelade of Brocq, central centrifugal cicatricial
alopecia, among others. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including
tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol.
1999:140:328-33.
,
22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans.
Dermatol Ther. 2008;21:238-44.
,
66. Duque-Estrada B, Tamler C, Sodré CT, Barcaui CB, Pereira FB.
Dermoscopy patterns of cicatricial alopecia resulting from discoid lupus
erythematosus and lichen planopilaris. An Bras Dermatol.
2010;85:179-83. FD can be very therapy resistant. Therapeutic options include oral and
topical antibiotics, oral and topical corticosteroids, antiseptics, oral isotretinoin
and dapsone. 11. Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including
tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol.
1999:140:328-33.
,
22. Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans.
Dermatol Ther. 2008;21:238-44.
,
44. Douwes KE, Landthaler M, Szeimies RM. Simultaneus occurence of
foliculitis decalvans capillitis in identical twins. Br J Dermatol.
2000;143:195-7. More research
on the pathogenesis and treatment options of this disfiguring disease is needed for
improving patient management.
A - Trichoscopic exam without interface liquid showing the crusts and scales. B - Trichoscopic exam with interface liquid showing erythema, fibrosis and vessels
REFERENCES
-
1Powell JJ, Dawber RP, Gatter K. Folliculitis decalvans including tufted folliculitis: clinical, histological and therapeutic findings. Br J Dermatol. 1999:140:328-33.
-
2Otberg N, Kang H, Alzolibani AA, Shapiro J. Folliculitis decalvans. Dermatol Ther. 2008;21:238-44.
-
3Ross EK, Vincenzi C, Tosti A. Videodermoscopy in the evaluation of hair and scalp disorders. J Am Acad Dermatol. 2006;55:799-806.
-
4Douwes KE, Landthaler M, Szeimies RM. Simultaneus occurence of foliculitis decalvans capillitis in identical twins. Br J Dermatol. 2000;143:195-7.
-
5Rudnicka L, Olszewska M, Rakowska A, Slowinska M. Trichoscopy update 2011. J Dermatol Case Rep. 2011;5:82-8
-
6Duque-Estrada B, Tamler C, Sodré CT, Barcaui CB, Pereira FB. Dermoscopy patterns of cicatricial alopecia resulting from discoid lupus erythematosus and lichen planopilaris. An Bras Dermatol. 2010;85:179-83.
-
7Rudnicka L, Olszewska M, Rakowska A, Kowalska-Oledzka E, Slowinska M. Trichoscopy: a new method for diagnosing hair loss. J Drugs Dermatol. 2008;7:651-4.
-
8Inui S. Trichoscopy for common hair loss diseases: algorithmic method for diagnosis. J Am Acad Dermatol. 2011;38:71-5.
-
9Wallace MP, de Berker DA. Hair diagnoses and signs: the use of dermatoscopy. Clin Exp Dermatol.2010;35:416.
-
10Lacarrubba F, Dall'Oglio F, Rita Nasca M, Micali G. Videodermatoscopy enhances diagnostic capability in some forms of hair loss. Am J Clin Dermatol 2004;5:205-8.
-
Financial funding: None
-
* Work performed at the Hospital Naval Marcílio Dias (HNMD), Rio de Janeiro (RJ), Brazil.
Publication Dates
-
Publication in this collection
Oct 2013
History
-
Received
15 Sept 2012 -
Accepted
24 Oct 2012