Abstracts
Early diagnosis of rheumatoid arthritis is essential for its proper management. Currently, the initial phase of rheumatoid arthritis is known to provide a window of therapeutic opportunity. Although the diagnosis is primarily clinical, the development and improvement of laboratory and imaging methods have contributed to earlier diagnosis and determination of procedures in early rheumatoid arthritis. In this article, the authors review the role of the major imaging methods used for assessing early rheumatoid arthritis, especially conventional radiography, ultrasonography, and magnetic resonance imaging.
early rheumatoid arthritis; conventional radiography; ultrasonography; magnetic resonance imaging
O diagnóstico precoce da artrite reumatoide é essencial para o manejo adequado da condição. Atualmente, considera-se que a fase inicial da doença constitui uma janela de oportunidade terapêutica para a artrite reumatoide. Embora o diagnóstico seja primordialmente clínico, o desenvolvimento e o aprimoramento de métodos laboratoriais e de imagem têm contribuído para o diagnóstico mais precoce e a determinação da conduta na artrite reumatoide inicial. Neste artigo os autores revisam o papel dos principais métodos de imagem utilizados para a avaliação da artrite reumatoide inicial, notadamente a radiologia convencional, a ultrassonografia e a ressonância magnética.
artrite reumatoide inicial; radiografia convencional; ultrassonografia; ressonância magnética
REVIEW ARTICLE
Imaging diagnosis of early rheumatoid arthritis
Licia Maria Henrique da MotaI; Ieda Maria Magalhães LaurindoII; Leopoldo Luiz dos Santos NetoIII; Francisco Aires Corrêa LimaVI; Sérgio Lopes VianaV; Paulo Sérgio MendlovitzVI; João Luiz FernandesVII
IPhD in Medical Sciences, Faculdade de Medicina, Universidade de Brasília - FM-UnB; Rheumatologist, Service of Rheumatology, Hospital Universitário de Brasília - HUB-UnB
IICollaborating Professor, Hospital das Clínicas, Faculdade de Medicina, Universidade de São Paulo - HC-FMUSP
IIIAssociate Professor of Internal Medicine and of the Service of Rheumatology, HUB-UnB
IVRheumatologist of the Service of Rheumatology, HUB-UnB
VRadiologist, Hospital da Criança de Brasília José Alencar e Clínica Vila Rica, Brasília/DF
VIRadiologist, HUB-UnB
VIIRadiologist, Image Memorial, Salvador/BA
Correspondence to Correspondence to: Licia Maria Henrique da Mota Centro Médico de Brasília. SHLS 716/916, bloco E, salas 501/502 - Asa Sul Brasília, DF, Brazil. CEP: 70390-904 Email: liciamhmota@yahoo.com.br
ABSTRACT
Early diagnosis of rheumatoid arthritis is essential for its proper management. Currently, the initial phase of rheumatoid arthritis is known to provide a window of therapeutic opportunity. Although the diagnosis is primarily clinical, the development and improvement of laboratory and imaging methods have contributed to earlier diagnosis and determination of procedures in early rheumatoid arthritis. In this article, the authors review the role of the major imaging methods used for assessing early rheumatoid arthritis, especially conventional radiography, ultrasonography, and magnetic resonance imaging.
Keywords: early rheumatoid arthritis, conventional radiography, ultrasonography, magnetic resonance imaging.
INTRODUCTION
Rheumatoid arthritis (RA) is a progressive systemic chronic inflammatory disease that affects primarily the synovial membrane and can lead to bone and cartilaginous destruction.1 It is a frequent condition (1%-2% of the world population) that affects all ethnical groups.2
In the past years, the generalization of the concept of "initial" or "early" RA and the existence of a window of therapeutic opportunity - time during which the institution of adequate therapy for the disease would result in marked clinical improvement - have strengthened the notion that early diagnosis and treatment can modify the course of disease.3
Concomitantly, laboratory and imaging tests have been developed or refined, contributing to the earlier diagnosis and prognostication of initial RA; in addition, changes in the therapeutic approach of RA have been instituted, with the use of new classes of drugs.4
The diagnosis of RAis established considering the association of clinical findings, and neither a laboratory test, nor a histological finding, nor an imaging test alone can confirm it. When RAis fully expressed with all its classic features, its recognition is simple. Its diagnosis in its early stage, however, is particularly difficult, because serological and radiological characteristics often lack.5
Although the identification of initial RA is primarily clinical, several complementary tests can be used to establish the diagnosis, make the differential diagnosis, determine prognosis, and follow disease up. This study is a brief review about the major imaging tests used for diagnosing and managing initial RA, especially conventional radiography, ultrasonography (US), and magnetic resonance imaging (MRI).
IMAGING TESTS
Several imaging tests are used to assess RA, such as conventional radiology, US, bone scan, computed tomography (CT), MRI, and bone densitometry.6
Bone scan, despite having high sensitivity to detect conditions leading to increased metabolic activity, such as joint inflammation, has low specificity and spatial resolution. Although CT has high spatial resolution, its limited contrast resolution restricts its use for soft tissue assessment and does not allow the detection of medullary bone edema, reducing its use in early RA. Bone densitometry is the best method to detect bone mass loss, which is unspecific, but provides little additional information other than that; in addition, bone densitometry still lacks standardization for the specific fi nality of assessing disease activity.7
More recently, molecular imaging methods, such as positron emission tomography (PET/CT) and single photon emission computed tomography (SPECT), have been used to diagnose, characterize, and monitor the activity of inflammatory diseases, such as RA.7-9 For example, (19)F-fluorodeoxyglucose PET/CT accurately detects inflammatory activity in large joints of patients with RA, and may be helpful for the early assessment of RA extent.7 Although the real role of those new techniques in the investigation of RA has not been established, they hold great promise, and, in the future, may play a more critical role in the diagnosis and assessment of disease activity.8
Currently, the three imaging methods most used to assess RA, because of the longer time of use and the experience accumulated, are as follows: conventional radiography; US; and MRI.
Radiography
Conventional radiography (both in its analogical and digital forms) is still the imaging modality of choice in assessing RA, being indispensable for all patients already at their first medical consultation, because radiographic changes are part of the diagnostic criteria for RA.10 In addition, the test is relatively inexpensive and almost universally available. However, the method is not sensitive to demonstrate the earliest changes of disease, mainly bone erosions; edema of the soft tissues and juxta-articular osteoporosis are some of the fi rst radiographic findings (Figure 1). On radiography, the first sites affected are usually metacarpophalangeal joints (especially the second and third ones), metatarsophalangeal joints (especially the fifth), proximal interphalangeal joints, and ulnar and radial styloid processes.11
The most characteristic lesions appear later on radiography, and include narrowing of the joint space (due to cartilage destruction) and bone erosions (Figure 2). Patients with RA assessed with conventional radiography at an early stage of disease showed erosions as follows: on the fi rst assessment, only 13%; after 12 months, 28%; after 24 months, 75%; and after 60 months of follow-up, 90%.12,13
In late stages, sequelae such as deformities, subluxations, and ankylosis can be observed. None of those changes is pathognomonic, but their presence, especially if symmetrical, in association with clinical findings strongly suggests disease. All patients should undergo a baseline initial radiography that allows radiographic follow-up, aiming at assessing disease progression and response to treatment.11
Ultrasonography
US is an inexpensive exam that allows good assessment of soft tissues. The technique detects synovial thickening; presence of fluid in joints, bursae, and tendon sheaths; structural abnormalities of tendons, ligaments, and entheses; and superficial erosions.14,15 However, it is examiner dependent, has low reproducibility, and has not been completely standardized to assess initial RA.16 It does not allow assessing changes deeply located in the joints. In addition, the ultrasound beam does not penetrate bone, and, thus, bone assessment is restricted to the cortical surface and available acoustic windows. Techniques such Doppler can be useful in assessing disease activity, differentiating between active (pannus) and inactive inflammatory tissue. US may be useful to quantify disease progression and may monitor response to treatment in RA.17 However, the quantification of inflammatory activity on US is yet to be standardized.15
Magnetic resonance
Of the imaging techniques currently available, MRI is undoubtedly the most sensitive for detecting the changes of RA. It allows assessing all structures affected, such as soft tissues, bones and cartilages, and detecting early erosions (up to three years before conventional radiography). The pattern and site of the changes might have a prognostic implication.16 The use of paramagnetic contrast agents (gadolinium compounds) is formally indicated in patients with RA, potentiating the detection of synovial thickening and anomalously enhanced areas, indicative of inflammatory activity in both soft tissues and bone; enhanced areas in medullary bone are seen even prior to the appearance of erosions and indicate increased risk for their development.16
Erosions and the tenosynovial component of RA are also properly demonstrated on MRI, even with virtually normal radiographies. The CIMESTRA study has shown that the detection of bone edema on MRI in initial RA is the best predictor of radiographic progression of bone erosion after a two-year follow-up.18 That result has been confirmed by a recent systematic review, which has suggested that performing MRI at an early stage of disease can be useful to increase its predictive value.19
In addition to its high cost and limited availability,20 the disadvantages of MRI comprise the lack of method standardization and of a cutoff point for lesion definition (changes similar to erosions and synovitis have already been described in healthy individuals with no clinical evidence of RA). Moreover, sedation might be required for claustrophobic patients; the position and the time required for the test might not be tolerated by elderly and/or debilitated patients, and some contraindications such as cardiac pacemaker holders or patients with ferromagnetic aneurysm clips still persist.21
Attempts to reduce the costs of MR include the use of new techniques. The isolated assessment of the fist of the dominant hand seems adequate to evaluate patients with initial RA, showing good sensitivity and specificity for the early detection of the typical changes of the disease.22 A new technique proposed (modified "praying hands") has proved to be, as compared with the traditional technique, equally sensitive to detect changes compatible with the early stage of disease, with a great advantage regarding the duration of the test. This would allow cost reduction and an increase in the number of exams performed in a certain time period.23
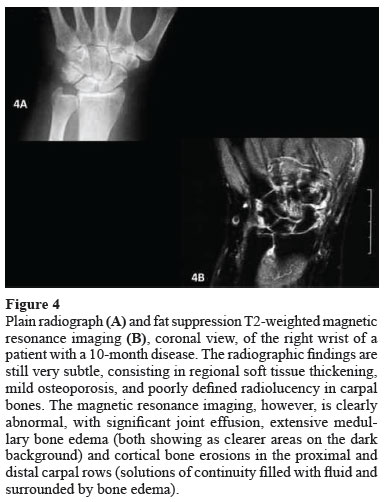
Figures 3 and 4 exemplify different imaging exams and their findings in patients with symptoms compatible with RA for up to 12 months. Table 1 compares advantages and disadvantages of the major imaging tests used to assess initial RA.24
CONCLUSIONS
The diagnosis of initial RA is primarily clinical, but several complementary tests can be used, such as imaging exams. Of the recent advances, MRI has gained increasing importance, showing high sensitivity at very early stages. In addition, methods, such as PET/CT and SPECT, have been used to diagnose, characterize and monitor the activity of inflammatory diseases such as RA.
On conventional radiography, erosions remain as the key measure for the structural outcome in initial RA, and their use has been recommended by a European committee of rheumatologists after a detailed review of all evidence available.25
Although plain radiographs remain essential for the initial assessment of patients with RA, several studies have suggested the use of ultrasonography and MRI as the imaging exams of choice for assessing early RA.26 Enhanced MRI, in particular, is extremely sensitive, allowing the detection of areas de intraosseous inflammation before overt erosions develop. Technical refining of those methods is being studied and shows promising results. However, standardizing those methods in the context of rheumatoid disease, in addition to defining their real role in prognostication and assessment of response to treatment, are still required.
REFERENCES
1. Lee DM, Weinblatt ME. Rheumatoid arthritis. Lancet 2001;358(9285):903-11.
2. Alarcón GS. Epidemiology of rheumatoid arthritis. Rheum Dis Clin North Am 1995;21(3):589-604.
3. Mota LMH. Atualização em Reumatologia: Artrite reumatoide inicial. Rev Bras Reumatol 2008;48(6):360-5.
4. Mota LMH, Carvalho JF, Santos-Neto LL.Autoantibodies and other serological markers in rheumatoid arthritis: predictors of disease activity? Clin Rheumatol 2009;28(10):1127-34.
5. Keen HI, Emery P. How should we manage early rheumatoid arthritis? From imaging to intervention. Curr Opin Rheumatol 2005;17(3):280-5.
6. Brown AK, Wakefield RJ, Conaghan PG, Karim Z, O'Connor PJ, Emery P. New approaches to imaging early inflammatory arthritis. Clin Exp Rheumatol 2004;22(5 Suppl. 35):S18-25.
7. Kubota K, Ito K, Morooka M, Mitsumoto T, Kurihara K,Yamashita H et al. Whole -body FDG-PET/CT on rheumatoid arthritis of large joints. Ann Nucl Med 2009;23(9):783-91.
8. Basu S, Zhuang H, Torigian DA, Rosenbaum J, Chen W, Alayi A. Functional imaging of inflammatory diseases using nuclear medicine techniques. Semin Nucl Med 2009;39(2):124-45.
9. Fonseca A, Wagner J, Yamaga LI, Osawa A, da Cunha ML, Scheinberg M. (18) F-FDG PET imaging of rheumatoid articular and extraarticular synovitis. J Clin Rheumatol 2008;14(5):307.
10. Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS et al. The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis.Arthritis Rheum 1988;31(3):315-24.
11. van der Heijde DM. Radiographic imaging: the "gold standard" for assessment of disease progression in rheumatoid arthritis. Rheumatology (Oxford) 2000;39(Suppl. 1):9-16.
12. Dixey J, Solymossy C, Young A; Early RA Study. Is it possible to predict radiological damage in early rheumatoid arthritis (RA)? A report on the occurrence, progression, and prognostic factors of radiological erosions over the first 3 years in 866 patients from the Early RA Study (ERAS). J Rheumatol Suppl 2004;69:48-54.
13. Lindqvist E, Jonsson T, Saxne T, Eberhardt K. Course of radiographic damage over 10 years in a cohort with early rheumatoid arthritis. Ann Rheum Dis 2003;62(7):611-6.
14. Wakefield RJ, D'Agostino MA, Iagnocco A, Filippucci E, Backhaus M, Scheel AK et al.; OMERACT Ultrasound Group. The OMERACT Ultrasound Group: status of current activities and research directions. J Rheumatol 2007;34(4):848-51.
15. Fernandes EA, Castro Júnior MR, Mistraud SAV, Kubota ES, Fernandes ARC. Ultrassonografia na artrite reumatoide: aplicabilidade e perspectives. Rev Bras Reumatol 2008;48(1):25-30.
16. Østergaard M, Pedersen SJ, Døhn UM. Imaging in rheumatoid arthritis - status and recent advances for magnetic resonance imaging, ultrasonography, computed tomography and conventional radiography. Best Pract Res Clin Rheumatol 2008;22(6):1019-44.
17. Wells AF, Haddad RH. Emerging role of ultrasonography in rheumatoid arthritis: optimizing diagnosis, measuring disease activity and identifying prognostic factors. Ultrasound Med Biol 2011;37(8):1173-84.
18. Hetland ML, Ejbjerg B, Hørslev-Petersen K, Jacobsen S, Vestergaard A, Jurik AG et al.; CIMESTRA study group. MRI bone oedema is the strongest predictor of subsequent radiographic progression in early rheumatoid arthritis. Results from a two year randomized controlled trial (CIMESTRA). Ann Rheum Dis 2009;68(3):384-90.
19. Suter LG, Fraenkel L, Braithwaite RS. Role of magnetic resonance imaging in the diagnosis and prognosis of rheumatoid arthritis. Arthritis Care Res (Hoboken) 2011;63(5):675-88.
20. Suster LG, Fraenkel L, Braithwaite RS. Cost-effectiveness of adding magnetic resonance imaging to rheumatoid arthritis management. Arch Intern Med 2011;171(7):657-67.
21. Keen HI, Brown AK, Wakefield RJ, Conaghan PG. MRI and musculoskeletal ultrasonography as diagnostic tools in early arthritis. Rheum Dis Clin North Am 2005;31(4):699-714.
22. Vitule LF. Avaliação da ressonância magnética da mão dominante na artrite reumatoide precoce: correlação com a radiologia convencional. Doutorado [tese]. São Paulo: Universidade de São Paulo; 2007.
23. Mota LMH, Mendlovitz S, Carneiro JN, Von Kircheheim RAF, Almeida LA, Lima FAC. Ressonância magnética para avaliação da artrite reumatoide inicial - proposta da técnica de "mãos em prece" modificada [abstract]. In: XXVII Congresso Brasileiro de Reumatologia; 2008 Set 17-20; Maceió . Rev Bras Reumatol 2008;48:S235. Abstract 01.020.
24. Mota LMH, Cruz BA, Brenol CV, Pereira IA, Fronza LS, Bertolo MB et al.; Brazilian Society of Rheumatology. 2011 Consensus of the Brazilian Society of Rheumatology for diagnosis and early assessment of rheumatoid arthritis. Rev Bras Reumatol 2011;51(3):199-219.
25. Combe B, Landewe R, Lukas C, Bolosiu HD, Breedvelt F, Dougados M et al. EULAR recommendations for the management of early arthritis: report of a task force of the European Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis 2007;66(1):34-45.
26. Østergaard M, Døhn UM, Ejbjerg BJ, McQueen FM. Ultrasonography and magnetic resonance imaging in early rheumatoid arthritis: recent advances. Curr Rheumatol Rep 2006;8(5):378-85.
Received on 09/06/2011.
Approved on 06/27/2012.
The authors declare no conflict of interest.
Service of Rheumatology, Hospital Universitário de Brasília, Universidade de Brasília - HUB-UnB; Service of Rheumatology, Hospital das Clínicas, Faculdade de Medicina, Universidade de São Paulo - HC-FMUSP.
-
1Lee DM, Weinblatt ME. Rheumatoid arthritis. Lancet 2001;358(9285):903-11.
-
2Alarcón GS. Epidemiology of rheumatoid arthritis. Rheum Dis Clin North Am 1995;21(3):589-604.
-
3Mota LMH. Atualização em Reumatologia: Artrite reumatoide inicial. Rev Bras Reumatol 2008;48(6):360-5.
-
4Mota LMH, Carvalho JF, Santos-Neto LL.Autoantibodies and other serological markers in rheumatoid arthritis: predictors of disease activity? Clin Rheumatol 2009;28(10):1127-34.
-
5Keen HI, Emery P. How should we manage early rheumatoid arthritis? From imaging to intervention. Curr Opin Rheumatol 2005;17(3):280-5.
-
6Brown AK, Wakefield RJ, Conaghan PG, Karim Z, O'Connor PJ, Emery P. New approaches to imaging early inflammatory arthritis. Clin Exp Rheumatol 2004;22(5 Suppl. 35):S18-25.
-
7Kubota K, Ito K, Morooka M, Mitsumoto T, Kurihara K,Yamashita H et al Whole -body FDG-PET/CT on rheumatoid arthritis of large joints. Ann Nucl Med 2009;23(9):783-91.
-
8Basu S, Zhuang H, Torigian DA, Rosenbaum J, Chen W, Alayi A. Functional imaging of inflammatory diseases using nuclear medicine techniques. Semin Nucl Med 2009;39(2):124-45.
-
9Fonseca A, Wagner J, Yamaga LI, Osawa A, da Cunha ML, Scheinberg M. (18) F-FDG PET imaging of rheumatoid articular and extraarticular synovitis. J Clin Rheumatol 2008;14(5):307.
-
10Arnett FC, Edworthy SM, Bloch DA, McShane DJ, Fries JF, Cooper NS et al The American Rheumatism Association 1987 revised criteria for the classification of rheumatoid arthritis.Arthritis Rheum 1988;31(3):315-24.
-
11van der Heijde DM. Radiographic imaging: the "gold standard" for assessment of disease progression in rheumatoid arthritis. Rheumatology (Oxford) 2000;39(Suppl. 1):9-16.
-
13Lindqvist E, Jonsson T, Saxne T, Eberhardt K. Course of radiographic damage over 10 years in a cohort with early rheumatoid arthritis. Ann Rheum Dis 2003;62(7):611-6.
-
14Wakefield RJ, D'Agostino MA, Iagnocco A, Filippucci E, Backhaus M, Scheel AK et al; OMERACT Ultrasound Group. The OMERACT Ultrasound Group: status of current activities and research directions. J Rheumatol 2007;34(4):848-51.
-
15Fernandes EA, Castro Júnior MR, Mistraud SAV, Kubota ES, Fernandes ARC. Ultrassonografia na artrite reumatoide: aplicabilidade e perspectives. Rev Bras Reumatol 2008;48(1):25-30.
-
16Østergaard M, Pedersen SJ, Døhn UM. Imaging in rheumatoid arthritis - status and recent advances for magnetic resonance imaging, ultrasonography, computed tomography and conventional radiography. Best Pract Res Clin Rheumatol 2008;22(6):1019-44.
-
17Wells AF, Haddad RH. Emerging role of ultrasonography in rheumatoid arthritis: optimizing diagnosis, measuring disease activity and identifying prognostic factors. Ultrasound Med Biol 2011;37(8):1173-84.
-
18Hetland ML, Ejbjerg B, Hørslev-Petersen K, Jacobsen S, Vestergaard A, Jurik AG et al; CIMESTRA study group. MRI bone oedema is the strongest predictor of subsequent radiographic progression in early rheumatoid arthritis. Results from a two year randomized controlled trial (CIMESTRA). Ann Rheum Dis 2009;68(3):384-90.
-
19Suter LG, Fraenkel L, Braithwaite RS. Role of magnetic resonance imaging in the diagnosis and prognosis of rheumatoid arthritis. Arthritis Care Res (Hoboken) 2011;63(5):675-88.
-
20Suster LG, Fraenkel L, Braithwaite RS. Cost-effectiveness of adding magnetic resonance imaging to rheumatoid arthritis management. Arch Intern Med 2011;171(7):657-67.
-
21Keen HI, Brown AK, Wakefield RJ, Conaghan PG. MRI and musculoskeletal ultrasonography as diagnostic tools in early arthritis. Rheum Dis Clin North Am 2005;31(4):699-714.
-
22Vitule LF. Avaliação da ressonância magnética da mão dominante na artrite reumatoide precoce: correlação com a radiologia convencional. Doutorado [tese]. São Paulo: Universidade de São Paulo; 2007.
-
23Mota LMH, Mendlovitz S, Carneiro JN, Von Kircheheim RAF, Almeida LA, Lima FAC. Ressonância magnética para avaliação da artrite reumatoide inicial - proposta da técnica de "mãos em prece" modificada [abstract]. In: XXVII Congresso Brasileiro de Reumatologia; 2008 Set 17-20; Maceió
- Rev Bras Reumatol 2008;48:S235. Abstract 01.020.
- 24. Mota LMH, Cruz BA, Brenol CV, Pereira IA, Fronza LS, Bertolo MB et al; Brazilian Society of Rheumatology. 2011 Consensus of the Brazilian Society of Rheumatology for diagnosis and early assessment of rheumatoid arthritis. Rev Bras Reumatol 2011;51(3):199-219.
- 25. Combe B, Landewe R, Lukas C, Bolosiu HD, Breedvelt F, Dougados M et al EULAR recommendations for the management of early arthritis: report of a task force of the European Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis 2007;66(1):34-45.
- 26. Østergaard M, Døhn UM, Ejbjerg BJ, McQueen FM. Ultrasonography and magnetic resonance imaging in early rheumatoid arthritis: recent advances. Curr Rheumatol Rep 2006;8(5):378-85.
Correspondence to:
Publication Dates
-
Publication in this collection
19 Oct 2012 -
Date of issue
Oct 2012
History
-
Received
06 Sept 2011 -
Accepted
27 June 2012