Abstracts
Foraminal lumbar disc herniations are extremely handicapping in relation to clinical symptoms and over the last forty years many alternatives have been put forward for treatment. Twenty patients with this radicular syndrome were operated by posterolateral access using arthroscopic microdiscectomy. Success was evaluated using pre-operative and post-operative self-evaluation questionnaires. Inclusion and exclusion criteria for surgery were rigorously followed. The mean age of the patients was 43 years old, varying between 23 and 58 years old. The group consisted of 13 women (65%) and 7 men (35%). All patients underwent operations for foraminal lumbar disc herniations between the 4th and 5th lumbar vertebrae. The success rate was 75% of the cases. No motor nerve or vascular lesions or bacterial discitis were evidenced.
Foraminal; Microdiscectomy; Arthroscopic
A hérnia discal lombar foraminal é extremamente incapacitante em relação à sintomatologia clínica. Nos últimos quarenta anos muitas alternativas foram propostas no tratamento dessa patologia. Vinte pacientes com essa síndrome radicular foram operados, via póstero-lateral, pela técnica da microdiscectomia artroscópica. O acompanhamento foi realizado com questionários de auto-avaliação pré-operatória e pós-operatória sendo obedecidos rigorosamente os critérios de inclusão e exclusão para a indicação cirúrgica. A idade média dos pacientes foi de 43 anos, com variação de 23 a 58 anos. Houve predomínio do sexo feminino (13 pacientes e freqüência percentual de 65%) em relação ao masculino (7 pacientes e freqüência percentual de 35%). Todos os pacientes foram operados de hérnia discal lombar foraminal no nível entre as 4ª e 5ª vértebras lombares. Os resultados clínicos apresentaram um percentual de 75% de sucesso. Não ocorreram nesse estudo complicações, tais como: lesão nervosa motora, vascular ou discite bacteriana.
Foraminal; Microdiscetomia; Artroscopia
ORIGINAL ARTICLE
Surgical treatment of foraminal disc herniations by arthroscopic microdiscectomy
Pedro Vilela Machado FilhoI; Alceu Gomes ChueireII
IHead of the Orthopaedics and Traumatology Service - Santa Casa de Misericórdia-São José do Rio Preto, member of SBOT - Brazilian Orthopaedics Society and SBPCV- Brazilian Spine Society
IIPhD inOrthopaedics. Head of Orthopaedics Department - Faculdade de Medicina de São José do Rio Preto - FAMERP
Correspondence Correspondence to Rua Siqueira Campos, 1820 Boa Vista 15025-055 São José do Rio Preto-SP phone: + 55 ( 17 ) 212-1500. e-mail: pedrohlv@terra.com.br
SUMMARY
Foraminal lumbar disc herniations are extremely handicapping in relation to clinical symptoms and over the last forty years many alternatives have been put forward for treatment. Twenty patients with this radicular syndrome were operated by posterolateral access using arthroscopic microdiscectomy. Success was evaluated using pre-operative and post-operative self-evaluation questionnaires. Inclusion and exclusion criteria for surgery were rigorously followed. The mean age of the patients was 43 years old, varying between 23 and 58 years old. The group consisted of 13 women (65%) and 7 men (35%). All patients underwent operations for foraminal lumbar disc herniations between the 4th and 5th lumbar vertebrae. The success rate was 75% of the cases. No motor nerve or vascular lesions or bacterial discitis were evidenced.
Key words: Foraminal; Microdiscectomy; Arthroscopic.
INTRODUCTION
Foraminal and extraforaminal lateral lumbar disc herniations have been described by Dandy (1941)(2), Lindblom (1944)(11), Harris & MacNab (1954)(4) and were rarely seen in practice.
Abdullah et al(1) described the clinical characteristics of lateral disc herniations and proposed computerized axial tomography and discography as diagnostic methods. He also established the treatment using medial facetectomy, which gave origin to lumbar segmental instability. Foraminal disc herniation is an acute radicular syndrome, with more intense pain in the leg than in the lower back, originating from a disc rupture in the extracanalicular portion of the medullary canal (within borders of the pedicles) and which compresses the longitudinal emerging root. That is, a foraminal disc between L4 and L5 causes tension on the L4 root. The extraforaminal herniation is located laterally to the pedicle.
McCulloch and Young(13) related this herniation is observed at the same rate both in men and women and is most frequently seen between the 4th and 5th lumbar vertebrae, as this is the segment with the greatest mobility. The incidence of this type of herniation is of between 5% and 10%. It most commonly affects over 50-year-old patients with normal disc spacing as seen on radiographs and the sudden start of the symptoms suggests a traumatic origin. The majority of lateral disc herniations irritates and compresses, partially or totally, the ganglia of the dorsal root provoking intensely painful symptoms.
Hijikata(5) evidenced a satisfactory evolution in 75% of his patients submitted to nuclear resection by the posterolateral endoscopic approach.
In the 1980s(6) the instruments were modified, increasing the diameter of the cannula for the passage of the special forceps, thus facilitating the resection of the lumbar disc.
Subsequently, Grenier, et al(3) described the importance of computerized axial tomography and nuclear magnetic resonance in the identification of foraminal and extraforminal herniations.
Kambin et al(9) improved the understanding of the posterolateral arthroscopic anatomy describing the working space zone of the fibrous annulus. The availability of small-caliber optic fibers permitted the entrance of the needle in the skin to the side and the perineural placing of the open end of the cannula. These authors demonstrated that the principle of arthroscopic microdiscectomy is based on resection of herniated disc fragments using illumination and intensification of the image. This technique consists of opening the intervertebral disc space, reducing the herniated volume of the nucleus pulposus. The non-migrated disc protrusion, with a clinical symptom of irritation of the nerve root, is the principal indication of this method.
The general aim of this work is to evaluate the surgical technique in the treatment of foraminal lumbar disc herniations by arthroscopic microdiscectomy, highlighting its advantages and disadvantages.
CASUISTIC AND METHOD
Twenty patients suffering from foraminal lumbar disc herniations underwent surgery by arthroscopic microdiscectomy. All were previously treated conservatively over a period of between two and 8 months (average of 4 months 25 days). After this period, surgical treatment was indicated. The mean age of the patients was 43 years with a variation of between 23 and 58 years. The group consisted of 13 women (65%) and 7 men (35%). All the patients underwent operations for foraminal lumbar disc herniations between the 4th and 5th lumbar vertebrae. There was a predominance of the right side (11 patients 55%) compared to the left (9 patients 45%).
The statistical tools utilized were: Frequency tables, exploratory data analysis, graphs and individual and mean profiles. The software STATDISK V.5.0 was employed.
Indication for surgery depended on the following inclusion criteria: 1) severe radiculopathy between the 3rd and 4th or 4th and 5th vertebrae, which did not respond to conservative treatment of at least 8 weeks; 2) more intense pain in the leg than in the lower back; 3) worsening of the reflected neurological sensitivity deficits, reflex abnormalities and paresis; 4) signs of tension of the nerve root (positive Lasegue's sign, positive contralateral Lasegue's sign, reproduction of the radicular pain under flexion load and rotation of the lumbar column); 5) study of images correlating to the clinical symptoms. The exclusion criteria were: 1) patients who did not fulfill the requisites of the pre-operative questionnaire; 2) cauda equina syndrome; 3) extrusive disc and intracanal migrated herniation (extraligamentous migrated); 4) tumors; 5) psychosocial problems.
All the patients completed the "Pre-surgery Self-assessment Questionnaire", quantifying the intensity of the pain, the frequency of paresis and paresthesia in the affected leg and the degree of capacity for work. During the follow-up in the out-patients clinic the "Post-surgery Self-assessment Questionnaire" was completed in the 3rd and 6th post-operative months. Diagnosis was confirmed by computerized axial tomography and/or nuclear magnetic resonance imaging.
The instruments utilized in the arthroscopic microdiscectomy were developed by Professor Kambin (AMD system, Smith & Nephew Dyonics Inc.) and avoid vascular lesions as they do not allow greater than 2 centimeters of penetration of the forceps, trimmer blades or trephines inside the intervertebral space.
SURGICAL TECHNIQUE
Anesthesia was achieved with sedation using diprivan during all the surgery. The positioning of the patient in a recumbent position was on four supports with the hips and knees kept in flexion to correct the lumbar curve. Following this an image amplifier was placed on the affected side of the patient and a Kirschner wire was placed in the anteroposterior position parallel to the disc space to be operated on. A cephalic image of 20º was obtained of the disc space along all its extension. A metal wire was placed in the skin and the skin was marked using a pencil at 8, 10 and 12 centimeters distance from the midline of the spinal column.
A unilateral uniportal access was utilized. Using 2% Xylocaine associated with a vasoconstrictor the surgeon anesthetized the skin, subcutaneous cellular tissue, lumbar quadrate muscles, sacrospinal, iliac psoas and the outer border of the fibrous annulus.
The positioning of the peridural needle in respect to the fibrous annulus was at an angle of 35º to 45º in relation to the horizontal plane. The guide wire was positioned in the triangular working zone which is an extrapedicular space giving a safe passage for the instruments.
The triangular working zone's anterior boundary is the spinal nerve, lower is the side of the lower lumbar segment and the posterior boundary is the proximal articular process of the inferior vertebra. An anteroposterior image was made to demonstrate that the distal end of the guide wire was medial to the pedicle, allowing, in the per-operative period, arthroscopic visualization of the nerve root and of the dura mater. To resect the migrated foraminal herniation, the wire was maintained medial to the pedicle or in the lateral extra-foraminal herniation. In the lateral projection, the end of the guide wire was observed posterior to the vertebral bodies. The cannulated obturator was used to laterally displace the nerve root giving access to the herniation. In this phase of the procedure, four quadrants of the outside of the fibrous annulus were anesthetized using 2-% Xylocaine and a mixture of 4 ml of saline solution with 1 ml of fentanyl. An arthroscopic inspection of the annulotomy was performed with a rigid arthroscope of 0º or 30º scope avoiding neural lesion and periannular bleeding. The annular fenestration was achieved with 2 trephines of external diameters of 3 and 5 mm.
The inlet and outlet of the saline solution irrigation was established inside the arthroscope. Under visualization and illumination with instruments articulating at 120º dorsal angle, herniated fragments were resected. The epidural space was checked for the existence of extraligamentous fragments. This allowed the insertion of the arthroscope and an uninterrupted visualization of the herniated nuclear material. In this phase, several types of special forceps and automated nucleotome were introduced to remove the herniated nuclear fragments. Following this, the instruments were withdrawn and a single suture was made using 5-0 mononylon and an occlusive dressing was applied.
RESULTS
In Table 1, the absolute frequencies, percentages and accumulated percentages of the variable responses (pain, weakness, numbness and capacity to work) in each of the time intervals (t1, t2 and t3) are shown. Time interval t1 refers to the pre-operative time, t2 at three post-operative months and t3 at six post-operative months. In relation to the pain, initially (t1) all the patients reported levels of 8 or greater and at t2 all the patients presented with pain levels of less than or equal to 3. By t3 all the patients presented with pain levels less than or equal to 5, that is 90% of them were less than 4, 75% less than 3, 65% less than 2 and 25% less than 1. In general an improvement was observed with the passing of time in all four variables.
Analogously what happened with pain, also happened with weakness and paresthesia. The capacity to work also improved very much at t3, with all the patients presented with at least 75% capacity and 67% with total capacity.
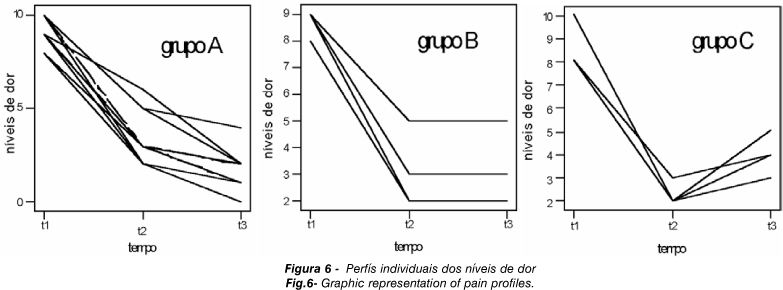
On analyzing each patient, it is possible to see that the measurements are repeated over the time and so the profile of the patients deserves special attention. For pain the graphic representation of the profiles can be seen in Figure 6. Three groups of patients can be seen denominated as:
Group A; those in which an improvement is observed at t2 and t3, representing 60% of the patients.
Group B; those who maintained the same level at t3 as at t2 representing 20% of the patients.
Group C; representing the final 20% in whom there was deterioration in the pain levels at t3.
DISCUSSION
We had dificulties to get research papers about arthroscopic microdiscectomy because the literature about this technique is a little spread by scientific vehicles.
The bad clinical results of laminectomy and discectomy encouraged more research for alternative methods of decompression. The gold standard for comparison continues to be laminectomy (or laminotomy) and discectomy. Foraminal or extraforaminal herniations are removed particularly well by arthroscopic posterolateral microdiscectomy. The foraminal herniation is the ideal type for this procedure as it is located right at the end of the cannula. Visualization and removal of the herniation using simple pituitary ronguers is very easy. The working channel scope allows visualization of the herniation during its resection without the necessity of facetary resection which can lead to segmental instability. In aged patients, the disc nuclear mass is generally dehydrated, and the mechanical compression of the nerve root is caused by protrusion of the fibers of the fibrous annulus associated with stenosis of the lateral or central recess. When these discs are dorsal-laterally approached a cavity, and in many cases little or no nuclear mass, is discovered(9). It must be emphasized that stenosis of the lateral recess is generally associated with unsuccessful arthroscopic microdiscectomy.
On the other hand, it is not possible to resect sequestered discs by the above technique. If it is not possible to differentiate between a non-dislocated sequestered fragment or partial extrusion and of the herniation from the routine computerized axial tomography images and/or magnetic resonance, then a tomography associated with discography should be performed to demonstrate the surplus radiopaque material at the site of the herniation and to clearly delimit the sequestered fragment.
Peterson(14) operated foraminal and extraforaminal hernias by arthroscopic posterolateral decompression. Of 41 patients accompanied over one year, he obtained an 88% success rate and in his casuistic there were 5 bad results, three who underwent reoperations and two who did not report any improvement.
Reynolds et al(15) achieved an 80% rate of good results using the inclusion criteria of Professor Kambin. The two different prospective studies of Kambin(7,10) demonstrated an 88.1% success rate in 275 assessed patients. Yeung(16) operated on 185 patients by the same technique and achieved a success rate of 85%. Mayer & Brock(12) presented results from prospective randomized studies of 40 patients who underwent posterior microdiscectomy or posterolateral arthroscopic microdiscectomy. Two years after the surgery, the disappearance of the sciatic pain was evidenced in 80% of the patients who made the endoscopic procedure whilst in the open access patients there was an improvement of 65%. In relation to sensitivity deficit, the arthroscopic microdiscectomy group had 92.3% and with the open microdiscectomy group there was 68.8%. A total of 95% of the arthroscopic group and 72.2% of the open surgery group were able to return to their original occupation. Our results compared with Mayer & Brock in the sixth post-operative month we evidenced that 75% of the patients had occasional pain and 65% had rare episodes. Apart from this, 95% had rare episodes of paresis and 80% of the individuals reported paresthesia disappeared completely. A total of 85% had their capacity to work reestablished. In this group of twenty patients, 3 were reoperataded due severe leg pain by open microdiscectomy after four months and recovered well.
Complications relating to the placing of the needle and the instruments occurred in five patients who had hypersensitivity of the skin in the lumbar region and the lateral face of the leg and who were conservatively treated using non-opiate analgesics, antidepressive agents and continuous physiotherapy. After this treatment there were remission of the clinical findings. One patient presented with very intense pain in the right leg and thigh. The etiology of this pain was excessive movement in the per-operative period distended vesical globe and the continuous movement of the access cannula migrating to the periannular space thus injuring the emerging root. After vesical catheterism there was consequent relief. Hyperstesia persisted for 2 months. There was no motor nerve or vascular lesions or bacterial discitis.
Kambin and Zhou(10) related the efficacy over the long term and low incidence of re-herniation after the arthroscopic disc surgery was attributed to several factors. These include the protection of the support and fine dural and neural ligamentous structures by the cannula, avoiding rupture; prevention of the formation of epidural and perineural scaring by not penetrating the lumbar canal, not injuring the epidural venous system which can lead to edema and chronic fibrosis of the nerve and preservation of the fibers of the posterolateral and posterior fibrous annulus during the surgery.
Kambin, et al(9) refered the limitations of the posterolateral approach include difficulties associated with the removal of sequestered disc fragments and access to the L5-S1 intervertebral discat the presence of elevated iliac crest that is prevalent in men. The ongoing development of research in the field of minimally invasive surgery facilitates arthroscopic access and decompression of the nerve roots in this group of patients.
CONCLUSIONS
Arthroscopic microdiscectomy was efficient in the treatment of protrusive foraminal lumbar disc herniations (between the 4th and 5th vertebrae), constituting an alternative to open surgery.
The clinical advantages observed in this technique were: reduction of pain in the local of incision, better cosmetic results and fast recovery to daily life activities.
REFERÊNCIAS BIBLIOGRÁFICAS
10. Kambin P, Zhou L. Arthroscopic discectomy of the lumbar spine. Clin Orthop 337:49-57, 1997
11. Lindblom K. Protrusions of discs and nerve compression in the lumbar region. Acta Radiol 25:195-212, 1944
Work perfomed at the Santa Casa de Misericórdia de São José do Rio Preto
- 1. Abdullah AF, Ditto E, Byrd E, Williams R. Extreme lateral lumbar disc herniation. J Neurosurg 4l:229-234, 1974.
- 2. Dandy WE. Concealed ruptured intervertebral discs. JAMA 117:821-823, 1941.
- 3. Grenier N, Greselle J, Douws C, et al. MR Imaging of foraminal and extraforaminal lumbar disc herniations. J Comput Assist Tomogr 14:243-249, 1990.
- 4. Harris RI, MacNab I. Structural changes in the lumbar intervertebral discs. Their relantionship to low back pain and sciática. J Bone Joint Surg Br 38:304-322, 1954.
- 5. Hijikata S. Percutaneous nucleotomy: a new concept. Technique and 12 years' experience. Clin Orthop 238:9-23. 1989
- 6. Kambin P, Brager M. Percutaneous posterolateral discectomy. Anatomy an mechanism. Clin Orthop 223:145-154, 1987.
- 7. Kambin P, Casey K, O'Brien E, Zhou L. Transforaminal arthroscopic descompression of lateral recess stenosis. J Neurosurg, 84:462-467, 1996.
- 8. Kambin P, O'Brien E, Zhou L. Arthroscopic microdiscectomy and fragmentectomy. Clin Orthop 347:150-167, 1998.
- 9. Kambin P, Schaffer JL, Zhou L. Incidence of complications following percutaneous posterolateral arthroscopic disc surgery. Orthop Trans 19:404-405, 1995.
- 12. Mayer HM, Brock M. Percutaneous endoscopic discectomy: surgical technique and preliminary results compared to microsurgical discectomy. J Neurosurg 78:216-225, 1993.
- 13. McCulloch JA, Young PH. Foraminal and extraforaminal lumbar disc herniation. In: Essentials of spinal microsurgery. Philadelphia: Lippincott-Raven 21:383-427, 1988.
- 14. Peterson R. Effectiveness of arthroscopic microdiscectomy in the treatment of foraminal and extraforaminal disc herniation, new horizons in spinal surgery, (notes) Allegheny University Hospitals, Philadelphia, PA, Nov. 1-2, 1996.
- 15. Reynolds J, Goldthwaite N, White A et al. Arthroscopic microdiscectomy (AMD) for lumbar disc protrusion, San Francisco Spine Institute, Daly City, California. Personal Communication.
- 16. Yeung A, A.M.D. The evolution from central nucleotomy to posterior and lateral fragmentectomy arthroscopic microdiscectomy of the lumbar spine (notes), international symposium abbott norhwestern hospital university of Minnesota, Minneapolis, Minnesota, October 6-7, 1995.
Publication Dates
-
Publication in this collection
16 June 2004 -
Date of issue
June 2004
History
-
Accepted
06 Apr 2004 -
Received
03 July 2003