Abstract
Significant changes have been witnessed in the Brazilian health system over the last 30 years. This article outlines trends in outpatient and hospital care, staffing, and health service use during this period. There was a significant expansion of the public health network, particularly of primary care services, leading to improved access to consultations and a reduction in hospital admissions. However, there is a persistent shortage of health professionals in Brazil’s public health system, particularly dentists. Despite improvements in coverage, the public system continues to face serious challenges, particularly with respect to funding, service provision, and its relationship with the private sector.
Access to health services; Use of health services; Health care networks
Resumo
Ao longo dos últimos 30 anos, o Sistema Único de Saúde brasileiro se caracterizou por importantes mudanças na atenção à saúde. No presente artigo, são apresentados dados relativos à evolução das estruturas ambulatorial e hospitalar, e dos recursos humanos, bem como acerca da utilização dos serviços de saúde. A expansão da rede pública ocorreu principalmente entre as unidades que dão suporte aos programas de atenção básica, ampliando o acesso às consultas médicas e a redução das internações para um conjunto de doenças, mas persiste uma carência de profissionais, especialmente no cuidado odontológico. Entretanto, a despeito do avanço na cobertura, permanecem os desafios à continuidade do SUS e à melhoria da qualidade do cuidado, particularmente no tocante ao financiamento público, oferta de serviços, e na relação com o setor privado.
Utilização de serviços de saúde; Acesso aos serviços de saúde; Rede assistencial
Introduction
Under the National Social Welfare Institute (Instituto Nacional de Previdência Social - INPS), the design of Brazil’s health system was based around a concentration of resources in the social welfare system, a centralized model of funding and administration, standardization of benefits, and the expansion of the social coverage of medical services to insured workers, favoring outsourcing of services to the private sector11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.. Specialized individual medical care was provided by the Ministry of Welfare and Social Assistance (Ministério da Previdência e Assistência Social), while the Ministry of Health’s role was limited primarily to regulation and preventive actions. Through the “group medicine” scheme, companies were able to outsource employee medical services, making them exempt from paying social security contributions11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434..
The movimento sanitário (health movement) that emerged in Brazil in the 1970s defended health reform based on a shift from a primarily biological approach to dealing with health problems towards an historical-structural approach that took into account the socioeconomic and political determinants of health11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.,22. Gerschman S. A democracia inconclusa: um estudo da reforma sanitária brasileira. Rio de Janeiro: Fiocruz; 2004.. Those who championed this approach argued that the state should play a key role in health promotion, health system regulation and service provision and that the democratization of access to health services and care system restructuring were an imperative33. Fleury S. Reforma sanitária brasileira: dilemas entre o instituinte e o instituído. Cien Saude Colet 2009; 14(3):743-752..
With the promulgation of the Federal Constitution in 1988, access to healthcare provided through a unified system became a social right. Law 8080/199044. Brasil. Lei 8.080, de 19 de setembro de 1990. Dispõe sobre as condições para a promoção, proteção e recuperação da saúde, a organização e o funcionamento dos serviços correspondentes e dá outras providências. Diário Oficial da União 1990; 19 set. went on to create the Unified Health System (Sistema Único de Saúde - SUS), based on the following underlying principles: universal access to health services across all levels of care; equality of care, without prejudice and privilege of any kind; comprehensiveness; public participation; and political and administrative decentralization55. Noronha JC, Lima LD, Machado CV. O Sistema Único de Saúde – SUS. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz, 2008. p. 435-472.. Also created in 1990, Law 814266. Brasil. Lei 8.142, de 28 de dezembro de 1990. Dispõe sobre a participação da comunidade na gestão do Sistema Único de Saúde (SUS) e sobre as transferências intergovernamentais de recursos financeiros na área da saúde e dá outras providências. Diário Oficial da União 1990; 31 dez. enshrined the principle of public participation in the SUS, providing for the creation of health councils and the promotion of health conferences.
While the Constitution provides that the provision of public health actions and services under the SUS should integrated, regionalized and hierarchical, it also states that health care is open to private enterprise. Furthermore, it provides that when SUS resources are not sufficient to guarantee full coverage in a particular area, the SUS may resort to outsourcing services to the private sector77. Paim J, Travassos C, Almeida C, Bahia L, Macinko J. The Brazilian health system: history, advances, and challenges. Lancet 2011; 377(9779):1778-1797..
Based on an analysis of trends in the supply of health establishments and resources and the use of health services in Brazil over the last three decades, this article explores the effects of health actions and policies and the role played by the private sector providers in the provision of NHS services.
Methodological aspects
To analyze structural changes in outpatient and hospital care, we used data from the 1981, 1986, 1990 and 1992 editions of the Medical-health Care Surveys (Pesquisa Assistência Médico-Sanitária - AMS), conducted by the Brazilian Institute of Geography and Statistics (IBGE, acronym in Portuguese)88. Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa Assistência Médico-Sanitária. Rio de Janeiro: IBGE; 1981, 1986, 1990 e 1992., and from the National Health Establishments Registry (Cadastro Nacional de Estabelecimentos de Saúde - CNES/MS)99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
from 2006, 2010 and 2017. Using the variable “Administrative Sphere”, we estimated the number of public and private establishments in each of the following groups: 1 – Family health support Centers (Centro de Apoio à Saúde da Família - CASF), health centers/primary care centers (Centro de Saúde/Unidade Básica de Saúde - UBS), health posts (Posto de Saúde) and family care centers (Unidade da Saúde da Família); 2 – Specialized clinics/specialized outpatient clinics, polyclinics (Policlínica), and mixed care centers (Unidade Mista); 3 - Hospitals; 4 – Urgent care, specialized emergency care, and general emergency care centers; 5 - Diagnosis and therapy support service units (Unidade de Serviço de Apoio de Diagnose e Terapia - SADT).
The type of service provided by the establishments was categorized as follows: “SUS” - establishments that provide services exclusively under the SUS; “Private” - establishments that provide exclusively private services via out-of-pocket payment (private), private health insurance plans (plan), or a combination of the two (plan/private); and “Mixed” - establishments that provide both public and private services (“SUS/private”, “SUS/plan”, and “SUS/plan/private”).
Changes in the way the IBGE generated data on outpatient establishments mean that the data for 1999, 2005 and 2009 is not comparable to previous periods.
Staffing trends were analyzed for the following categories of health professionals: doctors, dentists, and nurses. CNES data was used to calculate the proportion of professionals working in the SUS in the period 2007-2017, while the total number of doctors in the country between 1980 and 2017 was calculated using data obtained from the Federal Council of Medicine (CFM). The number of doctors per capita was calculated using annual population estimates produced by the IBGE between 1980 and 1999 and, for subsequent years, population projections estimated by the IBGE based on the results of the 2010 Demographic Census and information from birth and death records.
Data on access to and use of healthcare services in the 1980s was obtained from the 1981 and 1986 National Household Sample Surveys (Pesquisas Nacionais por Amostra de Domicílios - PNAD)11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.0. For subsequent years, data was obtained for successive five-year periods from the PNADs conducted between 1998 and 2008, which adopted sampling designs and questionnaires that were similar to those used in the 1981 PNAD, and from the 2013 National Health Survey (Pesquisa Nacional de Saúde - PNS)11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434..
The results of certain questions contained in the health survey questionnaires were used as indicators of access to health services, including the proportion of respondents that had visited the doctor or dentist in the 12 months prior to the survey. To analyze trends in the use of services in more recent periods of time prior to the questionnaire, we considered the following variables: proportion of respondents who had sought services in the period in question, type of service sought, reason for seeking services, type of care received, and type of payment. We also considered the proportion of respondents who had been admitted to hospital in the 12 months prior to the survey, the type of hospital, and type of payment.
Health service provision
Care network
Figure 1 shows the number of health establishments by group and broken down by type of establishment (public/private) between 1981 and 2017, demonstrating that there was a significant rise in the number of health establishments over the period.
Number of health establishments by group and broken down by type of establishment (public/private) between 1981 and 2017.
The total number of establishments increased from 21,532 to 129,544 in the period under study. Increases were particularly marked in the case of UBSs, whose number rose over the entire period levelling off in recent years, and clinics, especially since the beginning of the 1990s. There was also slight increase in the number of hospitals from 5,660 in 1981 to 6,794 in 2017. The number of emergency care centers and SADT units was limited at the beginning of the period; however, the number of SADT units grew in the 1990s.
The expansion of the primary care and urgent and emergency care network in the 2000s described by authors such as Paim et al.99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
and Braga Neto et al.11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.22. Gerschman S. A democracia inconclusa: um estudo da reforma sanitária brasileira. Rio de Janeiro: Fiocruz; 2004. is associated with the significant increase in the number of UBSs and clinics. It is interesting to note that while practically all UBSs are public (99.2% in 2017), the large majority of clinics are private (86.8% in 2017). In this respect, the percentage of public clinics declined significantly over the period, considering that it was over 50% in 1981.
Hospitals and SADT units are also predominantly private. Despite skewed regional concentration and closure of private facilities leading to an increase in the percentage of public hospitals (reaching 35.8% in 2017), hospitals in Brazil remain predominantly private. Braga Neto et al.1414. Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145. point out that the creation of small and medium-sized hospitals and federal and state incentives for the creation of beds in large hospitals account for majority of growth in public hospitals, while private hospitals, including those which are outsourced by the SUS, tend to be concentrated in areas where the possibility of sustainability and profit is greater1414. Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145.
SADT units were predominantly private throughout the period, with a slight increase in the proportion of public facilities, reaching 6.3% in 2017.
The private sector has continued to play a major role in healthcare since the middle of the twentieth century, despite the institution of the SUS at the end of the 1980s11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.,44. Brasil. Lei 8.080, de 19 de setembro de 1990. Dispõe sobre as condições para a promoção, proteção e recuperação da saúde, a organização e o funcionamento dos serviços correspondentes e dá outras providências. Diário Oficial da União 1990; 19 set., not only dominating specific areas such as SADT, but also benefitting from government support for the creation of private facilities11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.. Despite the creation of a universal public health system, public service provision therefore continues to be imbricated with the private sector.
Establishments and types of care
Private sector participation in healthcare provision in Brazil dates back to the middle of the twentieth century11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434. and has continued throughout the 30 years since the creation of the SUS. To explore public-private interdependence and how this relationship evolved during the period under study, we analyzed the type of care provided (SUS, private or mixed) in four categories of private establishments in 2006, 2010 and 2017, as shown in Figure 2. UBSs and health posts were excluded from the analysis because they are largely public.
The results show that the majority of the clinics are exclusively private and that service use occurs via private health insurance plans or out-of-pocket payments. The percentage of exclusively private establishments increased from 84.2% in 2006 to 88.5% in 2017, with a corresponding reduction in the percentage of establishments providing services exclusively through the SUS.
Although the majority of hospitals in this country are private, Figure 3 shows that the majority of private hospitals provide services exclusively to SUS patients or mixed services. The percentage of private hospitals that provide services exclusively to SUS patients decreased between 2006 and 2017, although they still accounted for almost 50% of all private hospitals in 2017. There was also a decrease in the percentage of exclusively private hospitals, with a corresponding increase in the percentage of establishments that provide mixed services, reinforcing the interdependence between the public and private sectors.
In contrast, SADT units are predominantly private, with the large majority providing exclusively private or mixed services. The trend in this type of establishment was similar to that of hospitals, with a reduction in the percentage of facilities that provide services exclusively to SUS patients and exclusively private facilities and an increase in the percentage of mixed facilities. However, in contrast to hospitals, SADT units were predominantly mixed service facilities, corroborating the findings of Martins1313. Machado MH. Trabalho e emprego em saúde. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2012. p. 259-2786..
Although emergency centers in Brazil are predominantly public, several private facilities also provide services to SUS patients. Trends were similar to those witnessed for SADT units, with an overwhelming predominance of mixed service facilities.
These findings show a significant degree of interdependence between the public and private sectors in relation to the provision of health services. While on the one hand the SUS needs private services to guarantee the right to healthcare, the majority of private establishments also depend on public resources, either because they provide services exclusively to SUS patients or are mixed facilities, particularly in the case of hospitals and SADT units.
Human Resources
The evolution of the SUS over the last 30 years is also associated with changes in human resources. The availability of staff in the health sector as a whole and, more specifically, in primary care, provides a basis for assessing increases in the provision of these services and the effects of specific policies such as the National Primary Care Policy and Programa Mais Médicos (more doctors program).
Figure 3 shows the total number of doctors and number of doctors per 1000 population, percentage of doctors, nurses and dentists working in the SUS, and their participation in primary care.
The number of doctors in the country increased from around 111,000 in 1980 to 447,000 in 2017, while the number of nurses and dentists increased from around 90,000 and 78,000, respectively, in 2007 to 230,000 and 127,000, respectively, in 2017.
The number of doctors per 1000 population also showed a marked increase, as the rate of increase in the number of doctors outstripped the population growth rate. The rate increased from under one doctor per 1000 population (0.94) in 1980 to 2.15 in 2017. This increase was proportionately greater between 2005 and 2015, when the rate increased from 1.6 to 2.15, which is slightly greater than the increase seen over the 25 years prior to this period.
The participation of the professionals that attend the SUS in the three highest professional categories (doctors, nurses and dentists)1414. Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145. also reveals interesting aspects of human resources. The percentage of nurses and doctors working in the SUS remained over 80% and 70%, respectively over the period under study. The percentage of nurses working in the SUS gradually decreased over the period, standing at 88% in 2017, while the percentage of doctors remained relatively stable at around 75%.
The percentage of dentists working in the SUS was lower than that of doctors and nurses and showed a significant reduction over the period from 62.8% in 2007 to 46.3% in 2017. Oral health has proven to be a major challenge for the SUS throughout its history11. Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.55. Noronha JC, Lima LD, Machado CV. O Sistema Único de Saúde – SUS. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz, 2008. p. 435-472., despite the existence of various programs in the area1616. Carvalho MN, Costa EMOD, Sakai MH, Gil CRR, Leite SNL. Expansão e diversificação da força de trabalho de nível superior nas Unidades Básicas de Saúde no Brasil, 2008 – 2013. Saúde Debate 2016; 40(109):154-162., and this is reflected in the low percentage of professionals working in the SUS.
The staffing of primary care centers underwent significant changes during the period. There was a notable increase in the number of professionals, especially nurses and doctors working in the Family Health Program. It is important to note here that, despite being registered in the CNES, these doctors do not necessarily have training in this area.
The number of nurses working in primary care outstripped the number doctors for the first time in 2008 and grew steadily throughout the rest of the period. The overall number of doctors decreased between 2005 and 2008, despite an increase in the number of doctors working in family health. There was a slight rise in the number of doctors between 2009 and 2012, followed by more substantial growth throughout the rest of the period especially due to an increase in the number of doctors working in family health through the Programa Mais Médicos implemented in 20131717. Brasil. Ministério da Saúde (MS). Programa Mais Médicos – dois anos: mais saúde para os brasileiros. Brasília: MS; 2015.. There was a decrease in the number of dentists working in the SUS despite an overall increase in numbers throughout the period.
Carvalho et al.1818. Viacava F, Bellido JG. Condições de saúde, acesso a serviços e fontes de pagamento, segundo inquéritos domiciliares. Cien Saude Colet 2016; 21(2):351-370. highlight that there was an increase in the proportion of other professionals resulting from the creation of the teams that make up the Family Health Support Centers (Núcleo de Apoio à Saúde da Família). These authors emphasize the importance of this diversification in enhancing the quality and diversity of care and moving towards comprehensiveness.
Machado1414. Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145. points out that the increase in the number of health professionals is a reflection of the expansion of care and is distinct from other industries where the incorporation of technology has led to a reduction in the demand for human labor. Unlike these industries, there has been a significant increase in the number of workers in the health sector despite the introduction of various new technologies over recent decades.
One of the main challenges in this respect is the multitude of different types of contractual relationships within the SUS due to the lack of a standardized human resources policy, which often results in precarious contractual arrangements and difficulties in hiring and maintaining staff in many localities1616. Carvalho MN, Costa EMOD, Sakai MH, Gil CRR, Leite SNL. Expansão e diversificação da força de trabalho de nível superior nas Unidades Básicas de Saúde no Brasil, 2008 – 2013. Saúde Debate 2016; 40(109):154-162. In this respect, it is important to highlight the striking regional disparities in the availability of professionals1616. Carvalho MN, Costa EMOD, Sakai MH, Gil CRR, Leite SNL. Expansão e diversificação da força de trabalho de nível superior nas Unidades Básicas de Saúde no Brasil, 2008 – 2013. Saúde Debate 2016; 40(109):154-162.,1919. Viacava F, Porto SM, Carvalho CC, Bellido JG. Desigualdades regionais e sociais em saúde segundo inquéritos domiciliares (Brasil, 1998-2013). Cien Saude Colet. No prelo 2018., which is just one of a wide range of persistent socioeconomic and spatial inequalities across the sector.
Access to health services
Access to health services has improved over the last three decades. Commonly used indicators such as the percentage of respondents who had visited a doctor or dentist in the past 12 months show that there was an increase in the percentage of the population seeking and obtaining health services.
The results of the PNAD and PNS show that the percentage of respondents who had visited a doctor in the past 12 months increased from 54.7% to 71.2% between 1998 and 20131919. Viacava F, Porto SM, Carvalho CC, Bellido JG. Desigualdades regionais e sociais em saúde segundo inquéritos domiciliares (Brasil, 1998-2013). Cien Saude Colet. No prelo 2018., with increases being registered in all of the major regions. In 2013, 72.8% of people aged between 18 and 59 years with at least 11 years of schooling had visited a doctor, compared to 63.7% of people with zero to three years of schooling. The difference between these two groups was greatest in the North Region, where the ratio was 1,32020. Brasil. Ministério da Saúde (MS). Sistema de Informações Hospitalares do SUS (SIH/SUS). Brasília: MS; 2017..
Access to dental services, based on the percentage of respondents who had visited a dentist in the last 12 months, increased steadily over the period from 17.3% in 1981 to 33.1% and 44.4% in 1998 and 2013, respectively1212. Braga Neto FC, Barbosa BR, Santos IS. Atenção Hospitalar: Evolução Histórica e Tendências. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p. 665-704.,1313. Machado MH. Trabalho e emprego em saúde. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2012. p. 259-2786.. However, major disparities between the North/South and Southeast Regions persisted in 2013, where only one-third and a half of respondents, respectively, had visited a dentist in the last 12 months1313. Machado MH. Trabalho e emprego em saúde. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2012. p. 259-2786.. Inequality in access to oral health care is associated with income and level of education1818. Viacava F, Bellido JG. Condições de saúde, acesso a serviços e fontes de pagamento, segundo inquéritos domiciliares. Cien Saude Colet 2016; 21(2):351-370., whereby the higher the income and level of education the lower the likelihood of never having visited a dentist. Furthermore, access to dental care remains largely dependent on ability to pay, as the percentage of patients paying for dental treatment remains high, varying between 66% in 1981 and 59% in 20131212. Braga Neto FC, Barbosa BR, Santos IS. Atenção Hospitalar: Evolução Histórica e Tendências. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p. 665-704.,1313. Machado MH. Trabalho e emprego em saúde. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2012. p. 259-2786..
According to the PNAD, the percentage of respondents who had sought some kind of health service or professional in the 30 days prior to the survey increased from 7.7% in 1981 to 11% in 1986. This percentage increased from 12.7% in 1998 to 15.3% in 2013. According to Paim et al.77. Paim J, Travassos C, Almeida C, Bahia L, Macinko J. The Brazilian health system: history, advances, and challenges. Lancet 2011; 377(9779):1778-1797., inequality in the use of services reduced between 1981 and 2008, although major disparities remained in the use of dental services. The results of the 2013 PNS show that people aged 18 years and over with less than three years of schooling were more likely to seek services than other groups and that there was no statistically significant difference between groups with four to 10 years of schooling and 11 years and over.
The type of health service sought by patients changed between 1981 and 2013, with a movement from ambulatory care (44.8% and 36.8%, respectively) towards primary care units (22.8% and 38.7%, respectively). The percentage of people who used a health post or health center on a regular basis increased from 41.8% in 1998 to 53.7% in 2013 and was higher among people with a low level of schooling2020. Brasil. Ministério da Saúde (MS). Sistema de Informações Hospitalares do SUS (SIH/SUS). Brasília: MS; 2017..
Another interesting aspect of the use of health services is the reason for seeking healthcare services (Table 1). Although the surveys differ in terms of the categories used, the results show that despite “illness” being the most frequent reason throughout the period under study, there was a significant increase in the use of health prevention and control services beginning in 1998.
In 1981, publicly funded services accounted for almost 70% of consultations made in the 15 days prior to the survey (6.3 million), including those provided under the social welfare system, which were largely federal (14.2%). In 2013, the SUS network or outsourced services accounted for 61.7% of consultations, which is equivalent to 17.6 million consultations. The percentage of consultations provided via health insurance plans increased from 9.3% in 1981 to 29.6%, peaking at 30.4% in 1998, while the percentage provided through direct payment decreased from 21% in 1981, to 13.5% in 1998 and to 8.7% in 2013 (Table 2).
Between 1995 and 2016, the annual number of hospital admissions in the SUS was around 11 million, 53% of which were in the South and Southeast2121. PROADESS – Projeto Avaliação do Desempenho do Sistema de Saúde. [acessado 2018 Jan 10]. Disponível em: http://www.proadess.icict.fiocruz.br
http://www.proadess.icict.fiocruz.br...
. According to health survey data, the proportion of respondents who had been admitted to hospital in the 12 months prior to the survey remained stable at around 7% and there was increase in annual public and private admissions from 8.6 million to 12.1 million. With respect to inequalities, the analysis shows that in recent years people with a low level of schooling were more likely to be admitted to hospital than those with higher levels1818. Viacava F, Bellido JG. Condições de saúde, acesso a serviços e fontes de pagamento, segundo inquéritos domiciliares. Cien Saude Colet 2016; 21(2):351-370..
With respect to the reasons for hospital admissions (Figure 4), the percentage of admissions for childbirth decreased from 27.2% in 1981 to 12.7% in 2013, while the percentage of admissions for surgery increased from 18.3% to 29.9%.
Types and sources of payment of the last hospitalizations referred to in the health surveys (in the 12 months which preceded the interviews).
According to survey data, the majority of admissions were paid by the public system, which accounted for 67% of admissions in 2013. However, the percentage of admissions covered by health insurance plans increased from 6.4% in 1981 to 27.6% in 2013, due to the expansion of coverage of plans, especially among higher socioeconomic status groups.
The increase in the number of public health posts and centers, changes in the point of entry to the health system, and the use of public facilities for the first entry to the system may be due to the expansion of the Family Health Strategy (Estratégia de Saúde da Família - ESF). The reduction in the percentage of hospitalizations due to ambulatory care sensitive conditions may also be credited to the expansion of the ESF, due both to improvements in the effectiveness of primary care and a reduction in the risk of patient exposure to unnecessary care.
The coverage of the ESF and primary care teams started to increase in 2000, reaching 59.9% and 63% of the population, respectively, in 2015. The ESF is particularly prominent in the Northeast, with 76% coverage, and also grew in the Southeast, where coverage was 49.2%2222. Cericato GO, Garbin D, Fernandes APS. A inserção do cirurgião-dentista no PSF: uma revisão crítica sobre as ações e os métodos de avaliação das Equipes de Saúde Bucal. RFO 2007; 12(3):18-23. in 2015. The expansion of coverage has improved access to health services, particularly among low economic status groups.
Improved access to dental care may also be associated with the incorporation of oral health teams into the Family Health program, although turnover is high due to the fact that the majority of staff are hired on temporary contracts22. Gerschman S. A democracia inconclusa: um estudo da reforma sanitária brasileira. Rio de Janeiro: Fiocruz; 2004.33. Fleury S. Reforma sanitária brasileira: dilemas entre o instituinte e o instituído. Cien Saude Colet 2009; 14(3):743-752.. The relatively low percentage of dentists working in the SUS also influences access to dental care, reducing the availability of services, especially among low-income groups. As Farias & Sampaio2424. Brasil. Emenda Constitucional nº 95, de 15 de dezembro de 2016. Diário Oficial da União 2016; 16 dez. highlight, the lack of meaningful participation of oral health professionals in the health reform process has hampered their inclusion in the system and continues to be a barrier to the effective integration of dental healthcare into the ESF.
Final considerations
The path taken by the SUS over the 30 years since its creation has been marked by important changes in healthcare. The main changes include an increase in the supply of health services and professionals working in the SUS, coupled with improved access and changing patterns of service use. However, it is important to underline the age-old challenges facing the Brazilian health system, such as public-private interdependence in health service provision, striking regional inequalities, and underfunding. Recent challenges include changes in the health status of the population, which has implications for the use of health services, and a 20-year social spending freeze approved in 20162424. Brasil. Emenda Constitucional nº 95, de 15 de dezembro de 2016. Diário Oficial da União 2016; 16 dez..
The supply of establishments also increased and has become considerably more diversified since the beginning of the 1980s99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
,1414. Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145.. The number of all types of establishments has grown significantly, with a particularly sharp rise in the number of public health posts and private SADT units and clinics. The country has also witnessed a steady increase in the number of health professionals1616. Carvalho MN, Costa EMOD, Sakai MH, Gil CRR, Leite SNL. Expansão e diversificação da força de trabalho de nível superior nas Unidades Básicas de Saúde no Brasil, 2008 – 2013. Saúde Debate 2016; 40(109):154-162., with the large majority of doctors and nurses working in the SUS. There has also been a notable increase in the number of professionals working in primary care1919. Viacava F, Porto SM, Carvalho CC, Bellido JG. Desigualdades regionais e sociais em saúde segundo inquéritos domiciliares (Brasil, 1998-2013). Cien Saude Colet. No prelo 2018. in recent years.
There was a significant improvement in access to healthcare services99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
,2020. Brasil. Ministério da Saúde (MS). Sistema de Informações Hospitalares do SUS (SIH/SUS). Brasília: MS; 2017. over the period under study, possibly related to the increased supply of health services and human resources coupled with the diversification of the workforce. The increase in the number of primary care establishments and professionals has had an impact on the patterns of use of health services, leading to a reduction in demand for primary care services associated with illnesses and an increase in demand for preventive care services. Public funding (SUS after its creation at the end of the 1980s) continued to play a major role, accounting for over 60% in consultations and admissions according to recent surveys.
It is important to stress, however, that any analysis of access, supply and use of services should be complemented by an evaluation of the quality of care. This requires a different approach that is able to assess the various dimensions of health system performance, such as adequacy, continuity, acceptability, effectiveness, efficiency, safety and respecting patient rights2222. Cericato GO, Garbin D, Fernandes APS. A inserção do cirurgião-dentista no PSF: uma revisão crítica sobre as ações e os métodos de avaliação das Equipes de Saúde Bucal. RFO 2007; 12(3):18-23..
The complex and enduring public-private relationship for the provision of health services has been a major challenge throughout the evolution of the SUS. This interdependent relationship stems from a history of government support for the expansion of private health services22. Gerschman S. A democracia inconclusa: um estudo da reforma sanitária brasileira. Rio de Janeiro: Fiocruz; 2004. and affirms itself in the structure of the SUS99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
. However, while guaranteeing access to health services to all citizens via the SUS requires private services, many of these services rely heavily on public resources for both their maintenance and expansion.
Deep regional inequalities are one of the main features of Brazilian reality and the country’s healthcare system clearly expresses these disparities. The supply of services and professionals and the various aspects of access and patterns of service use constitute challenges in this context, particularly bearing in mind the persistent nature of these inequalities2121. PROADESS – Projeto Avaliação do Desempenho do Sistema de Saúde. [acessado 2018 Jan 10]. Disponível em: http://www.proadess.icict.fiocruz.br
http://www.proadess.icict.fiocruz.br...
and the reproduction of the underlying elements that sustain them99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
,1414. Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145.,1616. Carvalho MN, Costa EMOD, Sakai MH, Gil CRR, Leite SNL. Expansão e diversificação da força de trabalho de nível superior nas Unidades Básicas de Saúde no Brasil, 2008 – 2013. Saúde Debate 2016; 40(109):154-162..
Underfunding is another structural challenge facing the SUS22. Gerschman S. A democracia inconclusa: um estudo da reforma sanitária brasileira. Rio de Janeiro: Fiocruz; 2004.,99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
. The effective implementation of the system, which depends on funding in order to increase the supply of services and professionals, incorporate technologies and democratize access to resources, has always been in dispute because of the varying interests that exist across the different spheres of government2525. Bahia L. O sistema de saúde brasileiro entre normas e fatos: universalização mitigada e estratificação subsidiada. Cien Saude Colet 2009; 14(3):753-762.. Guaranteeing improved access and gains in effectiveness depend on the availability of resources and, considering the role played by the SUS in healthcare provision, it is essential improve the funding situation.
The general health status of Brazil’s population has changed in recent years99. Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde. Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
http://cnes.datasus.gov.br...
due to population aging, an increase in morbidity and mortality due to external causes, and the emergence /reemergence of infectious and parasitic diseases. Throughout its history, the SUS has had to adapt to the resulting changed in healthcare demands. Tackling noncommunicable diseases and providing continuing healthcare constitutes a major challenge, while escalating urban and traffic violence and diseases such as Dengue and Zika virus impose a significant burden on health services.
This overview of developments in the SUS over the last three decades focused on the supply of establishments and professionals and access to services. The diversity of the sources used in this analysis, which hampers comparison of data over time, and an incomplete times series, which results in data gaps for certain periods, are the main limitations of this study. However, the results clearly show the essential role played by the SUS in the provision of healthcare to the Brazilian population.
Constitutional Amendment 95/20162424. Brasil. Emenda Constitucional nº 95, de 15 de dezembro de 2016. Diário Oficial da União 2016; 16 dez., which restricts public spending over the next 20 years is the ultimate challenge facing the SUS. A host of questions therefore remains, such as how will the health system be able to guarantee and expand healthcare given that an already challenging funding situation has become even more restrictive and how will it be able to ensure continuity and build on the achievements of the last 30 years? These questions suggest that the day-to-day challenges facing the SUS and policy and program planning may get worse.
Referências
-
1Escorel S. História das Políticas de Saúde no Brasil de 1964 a 1990: do golpe militar à Reforma Sanitária. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p.385-434.
-
2Gerschman S. A democracia inconclusa: um estudo da reforma sanitária brasileira Rio de Janeiro: Fiocruz; 2004.
-
3Fleury S. Reforma sanitária brasileira: dilemas entre o instituinte e o instituído. Cien Saude Colet 2009; 14(3):743-752.
-
4Brasil. Lei 8.080, de 19 de setembro de 1990. Dispõe sobre as condições para a promoção, proteção e recuperação da saúde, a organização e o funcionamento dos serviços correspondentes e dá outras providências. Diário Oficial da União 1990; 19 set.
-
5Noronha JC, Lima LD, Machado CV. O Sistema Único de Saúde – SUS. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz, 2008. p. 435-472.
-
6Brasil. Lei 8.142, de 28 de dezembro de 1990. Dispõe sobre a participação da comunidade na gestão do Sistema Único de Saúde (SUS) e sobre as transferências intergovernamentais de recursos financeiros na área da saúde e dá outras providências. Diário Oficial da União 1990; 31 dez.
-
7Paim J, Travassos C, Almeida C, Bahia L, Macinko J. The Brazilian health system: history, advances, and challenges. Lancet 2011; 377(9779):1778-1797.
-
8Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa Assistência Médico-Sanitária Rio de Janeiro: IBGE; 1981, 1986, 1990 e 1992.
-
9Brasil. Ministério da Saúde (MS). CNES: Cadastro Nacional de Estabelecimentos de Saúde Brasília. [acessado 2018 Jan 10]. Disponível em: http://cnes.datasus.gov.br
» http://cnes.datasus.gov.br -
10Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa Nacional por Amostra de Domicílios (PNAD) Rio de Janeiro: IBGE; 1981, 1986, 1998, 2003, 2008.
-
11Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa Nacional de Saúde (PNS) Rio de Janeiro: IBGE; 2013.
-
12Braga Neto FC, Barbosa BR, Santos IS. Atenção Hospitalar: Evolução Histórica e Tendências. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p. 665-704.
-
13Machado MH. Trabalho e emprego em saúde. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2012. p. 259-2786.
-
14Martins LO. O segmento da medicina diagnóstica no Brasil. Rev. Fac. Ciências Médicas de Sorocaba 2014; 16(3):139-145.
-
15Moysés SJ. Saúde Bucal. In: Giovanella L, Escorel S, Lobato, LVC, Noronha JC, Carvalho AI, organizadores. Políticas e Sistemas de Saúde no Brasil. Rio de Janeiro: Editora Fiocruz; 2008. p. 705-734.
-
16Carvalho MN, Costa EMOD, Sakai MH, Gil CRR, Leite SNL. Expansão e diversificação da força de trabalho de nível superior nas Unidades Básicas de Saúde no Brasil, 2008 – 2013. Saúde Debate 2016; 40(109):154-162.
-
17Brasil. Ministério da Saúde (MS). Programa Mais Médicos – dois anos: mais saúde para os brasileiros Brasília: MS; 2015.
-
18Viacava F, Bellido JG. Condições de saúde, acesso a serviços e fontes de pagamento, segundo inquéritos domiciliares. Cien Saude Colet 2016; 21(2):351-370.
-
19Viacava F, Porto SM, Carvalho CC, Bellido JG. Desigualdades regionais e sociais em saúde segundo inquéritos domiciliares (Brasil, 1998-2013). Cien Saude Colet. No prelo 2018.
-
20Brasil. Ministério da Saúde (MS). Sistema de Informações Hospitalares do SUS (SIH/SUS) Brasília: MS; 2017.
-
21PROADESS – Projeto Avaliação do Desempenho do Sistema de Saúde. [acessado 2018 Jan 10]. Disponível em: http://www.proadess.icict.fiocruz.br
» http://www.proadess.icict.fiocruz.br -
22Cericato GO, Garbin D, Fernandes APS. A inserção do cirurgião-dentista no PSF: uma revisão crítica sobre as ações e os métodos de avaliação das Equipes de Saúde Bucal. RFO 2007; 12(3):18-23.
-
23Farias MR, Sampaio JJC. Papel do cirurgião-dentista na equipe de saúde da família. RGO - Rev Gaúcha Odontol. 2011; 59(1):109-115.
-
24Brasil. Emenda Constitucional nº 95, de 15 de dezembro de 2016. Diário Oficial da União 2016; 16 dez.
-
25Bahia L. O sistema de saúde brasileiro entre normas e fatos: universalização mitigada e estratificação subsidiada. Cien Saude Colet 2009; 14(3):753-762.
Publication Dates
-
Publication in this collection
June 2018
History
-
Received
10 Jan 2018 -
Accepted
30 Jan 2018 -
Reviewed
05 Mar 2018


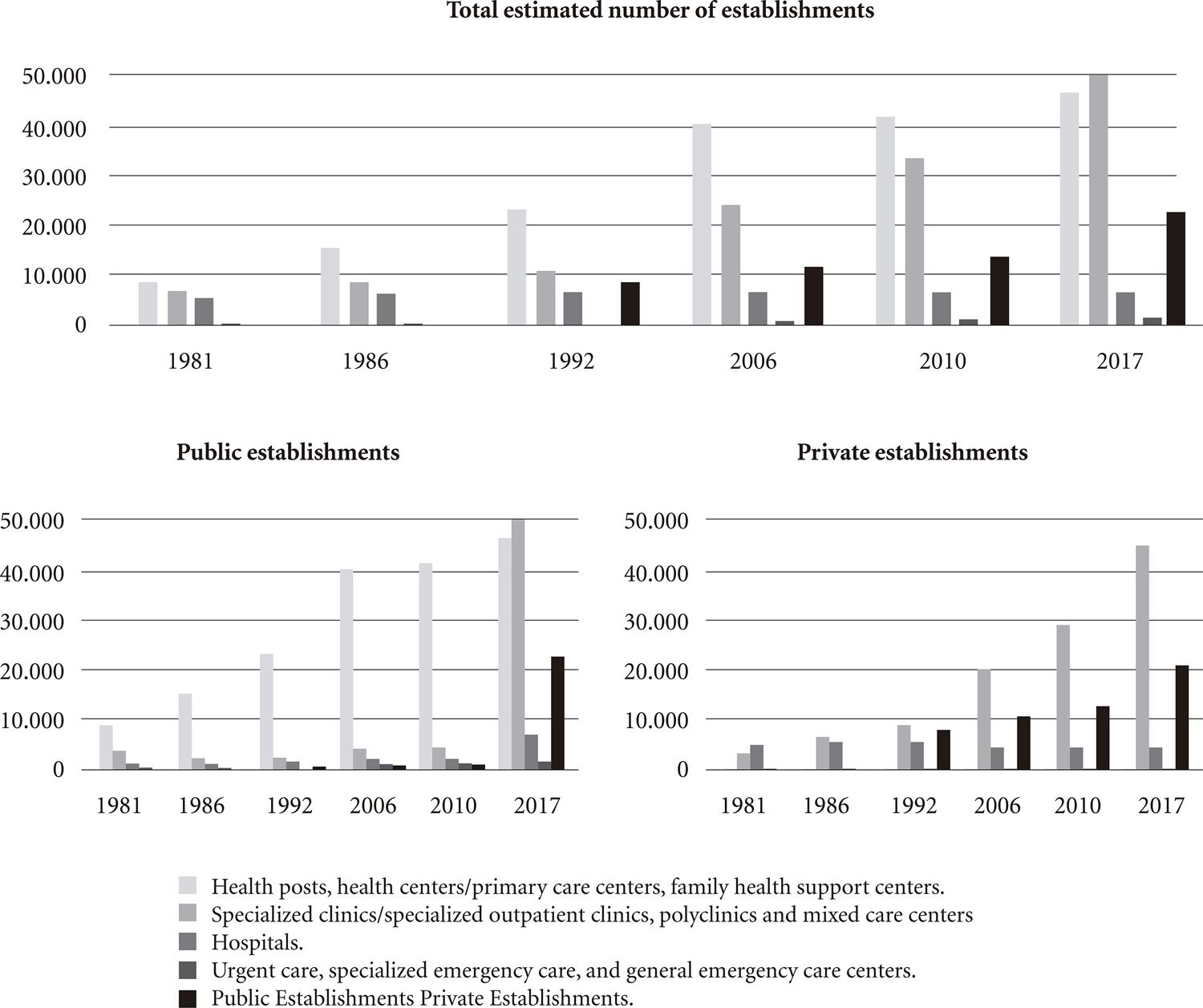 Source: AMS/IBGE (1981, 1986, 1992) e CNES/MS (2006, 2010 e 2017).
Source: AMS/IBGE (1981, 1986, 1992) e CNES/MS (2006, 2010 e 2017).
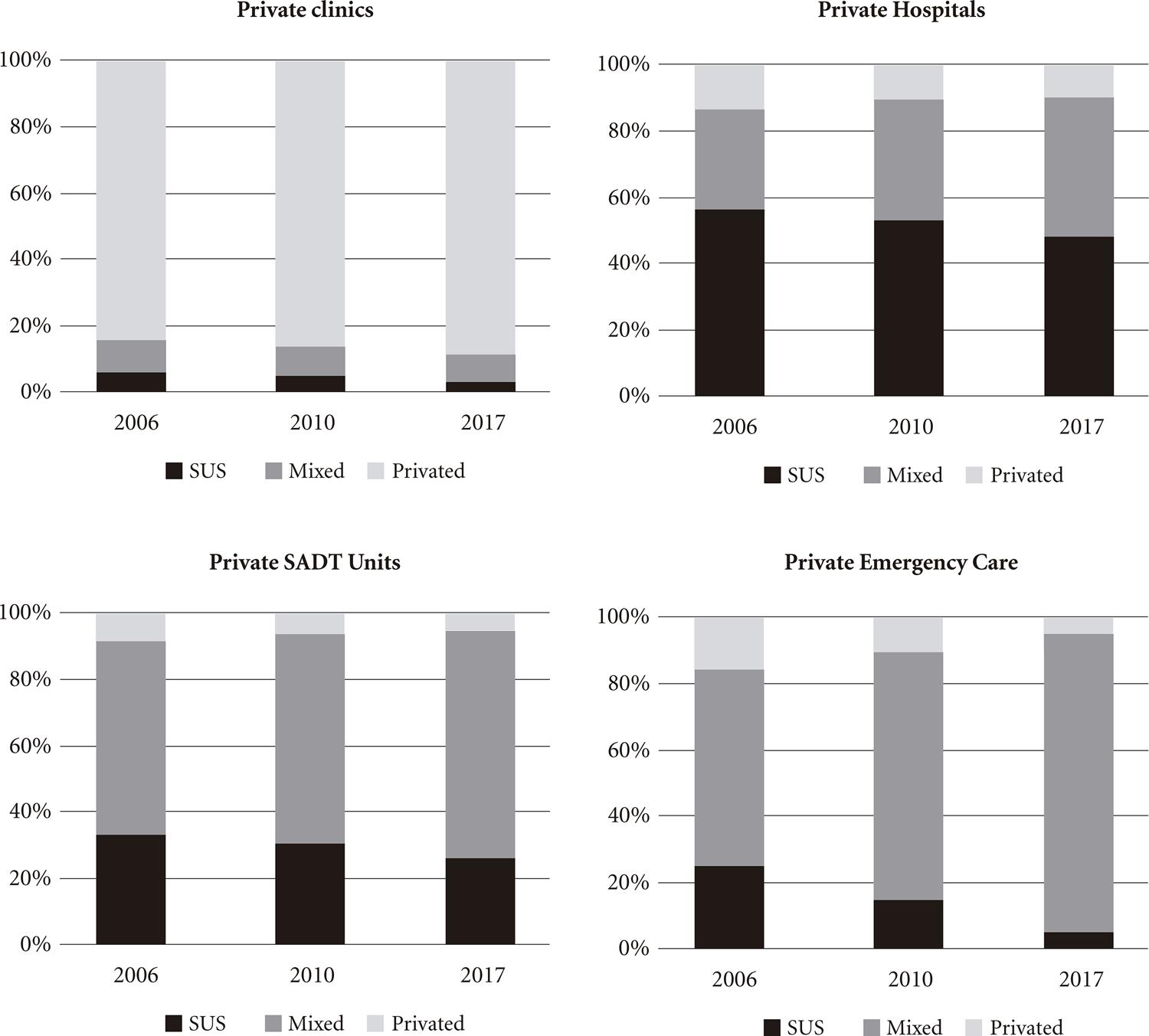 Source: CNES/MS.
Source: CNES/MS.
 Source: CNES.
Source: CNES.
 Source: PNAD 1981, PNAD 1998, PNAD 2003, PNAD 2008 e PNS 2013.
Source: PNAD 1981, PNAD 1998, PNAD 2003, PNAD 2008 e PNS 2013.