Abstract
This study evaluated oral hygiene habits and their association with sociocultural, environmental factors and factors related to the use of dental services among Quilombola and non-Quilombola rural adolescents from inland Bahia. Thiswas a cross-sectional study conducted in 2015. Prevalence and prevalence ratios were estimated for the outcomes and multiple Poisson regression analysis with robust variance was performed. We interviewed 390 adolescents, of which 42.8% were Quilombola. Poor tooth brushing and non-flossing were found in 33.3% and 46.7% of adolescents, respectively. Poor tooth brushing was increased by male gender (PR = 1.45), not living with both parents (PR = 1.45), lower hand hygiene habit (PR = 1.72) and worse oral health self-assessment (PR = 1.38). Non-flossing was associated with economic level E (PR = 1.54), older age (PR = 0.91), lower hand hygiene habit (PR = 1.53) and worse oral health self-assessment (PR = 1.33). Different associated factors were observed between Quilombola and non-Quilombola. It is necessary to consider the specificities of the populations for the promotion of adolescent oral health and the importance of the intersectoriality between education and health and care to families.
Oral health; Adolescent; Rural health; Ethnicity and health
Resumo
Este estudo avaliou os hábitos de higiene bucal e sua associação com fatores socioculturais, ambientais e relacionados à utilização de serviços odontológicos entre adolescentes rurais quilombolas e não quilombolas do interior da Bahia. Foi um estudo transversal realizado em 2015. Estimaram-se prevalências e razões de prevalências para os desfechos e foi conduzida análise múltipla por regressão de Poisson com variância robusta. Foram entrevistados 390 adolescentes, 42,8% quilombolas. Escovação dentária insatisfatória e não uso do fio dental foram encontrados em 33,3% e 46,7% dos adolescentes, respectivamente. Mostraram aumentar a escovação dentária insatisfatória: sexo masculino (RP = 1,45), não morar com ambos os pais (RP = 1,45), menor hábito de lavar as mãos (RP = 1,72) e pior autoavaliação da saúde bucal (RP = 1,38). Com o não uso de fio dental, mostraram-se associados: nível econômico E (RP = 1,54), maior idade (RP = 0,91) menor hábito de lavar as mãos (RP = 1,53) e pior autoavaliação da saúde bucal (RP = 1,33). Distintos fatores associados foram observados entre quilombolas e não quilombolas. Ressalta-se a necessidade de se considerar as especificidades das populações para a promoção da saúde bucal dos adolescentes e a importância da intersetorialidade entre educação e saúde e a atenção às famílias.
Saúde bucal; Adolescente; Saúde da população rural; Origem étnica e saúde
Introduction
Adolescence, the stage of life between childhood and adulthood, is a period in which differentiated attention is required regarding general and oral health 11. Silva Junior IF, Aguiar NL, Barros RC, Arantes DC, Nascimento LS. Saúde Bucal do Adolescente: Revisão de Literatura. Rev Adolesc. Saúde [periódico na Internet] 2016 agosto [acessado em 2017 Abr 19]; 13(Supl. 1):95-103. Disponível em: http://www.adolescenciaesaude.com
http://www.adolescenciaesaude.com...
. Physiological, psychological and social changes, typical of this stage make this population group more vulnerable to health risk situations 22. Word Health Organization (WHO). Nutrition in adolescence – Issues and Challenges for the Health Sector [Internet]. 2005. [acessado 2017 Mar 09]. Disponível em: http://apps.who.int/iris/bitstream/10665/43342/1/9241593660_eng.pdf.
http://apps.who.int/iris/bitstream/10665...
.
Oral health is a relevant aspect of adolescent life. An adverse perception of oral health influences the self-esteem and socialization of this group 33. Barbosa TB, Junqueira SR, Frias AC, Araujo ME. Interferência da Saúde Bucal em funções Biológicas e Sociais Segundo a percepção de Adolescentes Brasileiros. Rev Pesq Bras Odontoped Clin Integr [periódico na Internet]. 2013 Abr-Jun [acessado 2017 Abr 02];13(2)171-176. Disponível em: http://www.redalyc.org/articulo.oa?id=63730017006
http://www.redalyc.org/articulo.oa?id=63...
, 44. Silveira MF, Marôco JP, Freire RS, Barros Lima Martins AME, Marcopito LF. Impacto da saúde bucal nas dimensões físicas e psicossocial: uma análise através da modelagem com equações estruturais. Cad Saude Publica [periódico na Internet].2014 Jun [acessado 2017 Mar 18];30(6):1-15. Disponível em: http://www.scielo.br/pdf/csp/v30n6/pt_0102-311X-csp-30-6-1169.pdf
http://www.scielo.br/pdf/csp/v30n6/pt_01...
. Among the oral problems that may interfere with adolescents’ quality of life are untreated tooth decay, severe occlusion, tooth pain and loss, and gum bleeding 55. Peres KG, Peres MA, Araujo CLP, Menezes AMB, Hallal PC. Social and dental status along the life course and oral health impacts in adolescents: a population-based birth cohort. Health Qual Life Outcomes 2009 ; 7:95. , 66. Peres KG, Cascaes AM, Leão ATT, Côrtes MIS, Vettore MV. Aspectos sociodemográficos e clínicos da qualidade de vida relacionada à saúde bucal em adolescentes. Rev Saude Publica [periódico na Internet] 2013 [acessado 2017 Out 09]; 47(3):19-28. Disponível em: http://www.scielo.br/scielo.php?pid=S003489102013000900019&script=sci_abstract&tlng=pt
http://www.scielo.br/scielo.php?pid=S003...
.
One of the ways of preventing diseases and oral problems is proper oral hygiene, where tooth brushing and flossing are essential tools 11. Silva Junior IF, Aguiar NL, Barros RC, Arantes DC, Nascimento LS. Saúde Bucal do Adolescente: Revisão de Literatura. Rev Adolesc. Saúde [periódico na Internet] 2016 agosto [acessado em 2017 Abr 19]; 13(Supl. 1):95-103. Disponível em: http://www.adolescenciaesaude.com
http://www.adolescenciaesaude.com...
. Brazilian studies show that the prevalence of tooth brushing (≥ 3 times/day) ranges from 49.8% to 77.0% among adolescents. However, flossing is still not a consolidated habit when compared to brushing, with frequencies varying from 0.5% to 51.0% 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
, 88. Melo FGC, Cavalcanti AL. Hábitos de higiêne bucal e uso dos serviços odontológicos em estudantes de escolas públicas do município de Campina Grande, Paraíba. HU Revista [periódico na Internet].2009 Jul-Set [acessado 2017 Abr 20 ]; 35(3):191-198. Disponível em: https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721
https://hurevista.ufjf.emnuvens.com.br/h...
.
Oral hygiene habits are influenced by different factors related to individuals and their families. A higher prevalence of poorpracticesis noted in male adolescents, with lower economic level/maternal level of schooling and who report feeling alone 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
, 99. Vettore MV, Moysés SJ, Sardinha LMV, Iser BPM. Condições socioeconômicas, frequência de escovação dentária e comportamentos em saúde em adolescentes brasileiros: uma análise a partir da Pesquisa Nacional de Saúde escolar (PeNSE). Cad Saude Publica [periódico na Internet].2012 [acessado 2017 Mar 18]; 28(Supl.):S101-S113. Disponível em: http://www.scielosp.org/pdf/csp/v28s0/11.pdf
http://www.scielosp.org/pdf/csp/v28s0/11...
, 1010. Freire MCM, Jordão LMR, Malta DC, Andrade SSC, Peres MA. Desigualdades econômicas e mudanças nos comportamentos em saúde bucal de adolescente brasileiros de 2009 a 2012. Rev Saude Publica [periódico na Internet]. 2015 [acessado 2017 Abr 9]; 49:50. Disponível em: http://www.scielo.br/pdf/rsp/v49/pt_0034-8910-rsp-S0034-89102015049005562.pdf
http://www.scielo.br/pdf/rsp/v49/pt_0034...
. International studies have revealed that low prevalence of tooth brushing and flossing are associated with dwelling in rural areas 1111. Pereira C, Veiga N, Amaral O, Pereira. Comportamentos de saúde oral em adolescentes portugueses. Rev Port Saúde Pública [periódico na Internet]. 2013 Jul [acessado 2017 Mar 18]; 31(2):145-152. Disponível em: http://www.elsevier.pt/pt/revistas/revista-portuguesa-saude-publica-323/artigo/comportamentos-saude-oral-em-adolescentes-portuguesesS0870902513000278
http://www.elsevier.pt/pt/revistas/revis...
, 1212. Zhu L, Petersen PE. Oral hialita knowledge, atitudes and behaviour of children and adolescents in China. Rev. International Dental Journal [periódico na Internet]. 2003 [acessado 2017 Abr 02]; 53(5):289-298. Disponível em: http://www.who.int/oral_health/media/en/orh_knowledge_china.pdf
http://www.who.int/oral_health/media/en/...
. In Brazil, a study on rural children and adolescents aged 6-12 years showed tooth brushing (≥ 3 times/day) of 56.4% and flossing of 26.4% of respondents 1313. Menezes VA, Lorena RPF, Rocha LCB, Leite AF, Ferreira JMS, Granville-Garcia AF. Práticas de higiene bucal, uso de serviço odontológico e autopercepção de saúde bucal de escolares da zona rural de Caruaru, PE, Brasil. Rev. Odonto ciên [periódico na Internet]. 2010 [acessado 2017 Mar 02]; 25(1):25-31. Disponível em: http://www.scielo.br/pdf/roc/v25n1/06.pdf
http://www.scielo.br/pdf/roc/v25n1/06.pd...
.
The place of residence is a realm establishing the oral health situation of social groups. Individuals with similar social profiles may evidence different oral health levels, depending on the location and attributes of the dwelling place 1414. Moreira RS, Nico LS, Tomita NE. A relação entre o espaço e a saúde bucal coletiva: por uma epidemiologia georreferenciada. Cien Saude Colet [periódico na Internet]. 2007 [acessado 2017 Abr 20]; 12(1):275-284. Disponível em: http://www.scielo.br/pdf/csc/v12n1/27.pdf
http://www.scielo.br/pdf/csc/v12n1/27.pd...
.
Quilombola adolescents mostly reside in rural communities with specific territorial relationships related to resistance to the historical oppression suffered by this population 1515. Fundação Cultural Palmares. Certidões expedidas às comunidades remanescentes de quilombos (CRQs) atualizada até a portaria nº 268/2017 . 2017. [acessado 2017 Out 22]. Disponível em: http://www.palmares.gov.br/
http://www.palmares.gov.br/...
, 1616. Brasil. Decreto nº 4.887, de 20 de novembro de 2003. Regulamenta o procedimento para identificação, reconhecimento, delimitação, demarcação e titulação das terras ocupadas por remanescentes das comunidades dos quilombos de que trata o art. 68 do Ato das Disposições Constitucionais Transitórias. Diário Oficial da União 2003; 21 nov. . They coexist with social vulnerabilities related to their places of residence, such as lower coverage of water supply through a general distribution network and regular collection of garbage, low schooling and household income, when compared with other rural communities 1717. Silva EKP, Medeiros DS, Martins PC, Sousa LA, Lima GP, Rêgo MAS, Silva TO, Freire AS, Silva FM. Insegurança alimentar em comunidades rurais no Nordeste brasileiro: faz diferença ser quilombola? Cad Saude Publica [periódico na Internet]. 2017 Jun [acessado 2017 Out 22]; 33(4):e00005716. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2017000405013&lng=en
http://www.scielo.br/scielo.php?script=s...
, as well as difficult access to the dental services 1818. Silva MEA, Rosa PCF, Neves ACC, Rode SM. Necessidade protética da população quilombola de Santo Antônio do Guaporé- Rondônia- Brasil. Rev Braz Dent Sci [periódico na Internet]. 2011 Jul-Dez [acessado 2017 Mar 18]; 14(1-2)62-66. Disponível em: http://ojs.fosjc.unesp.br/index.php/cob/article/view/676
http://ojs.fosjc.unesp.br/index.php/cob/...
.
Thus, this study aimed to evaluate oral hygiene habits and its association with sociocultural and environmental factors, as well as factors related to the use of dental services among rural Quilombola and non-Quilombola adolescents from a rural area in inland Bahia.
Methods
This is a cross-sectional, population-based and home-based study conducted with adolescents aged 10-19 years of age, living in 21 Quilombola rural communities recognized by the Palmares Cultural Foundation (FCP) 1515. Fundação Cultural Palmares. Certidões expedidas às comunidades remanescentes de quilombos (CRQs) atualizada até a portaria nº 268/2017 . 2017. [acessado 2017 Out 22]. Disponível em: http://www.palmares.gov.br/
http://www.palmares.gov.br/...
and non-Quilombola communities from Vitória da Conquista, Bahia. This study is part of the study Adolescer: Adolescent Health of the Rural Area and its Conditions , approved by the Human Research Ethics Committee of the Multidisciplinary Health Institute, the Federal University of Bahia.
The sampling strategy considered the territorial extension and the population of adolescents living in rural communities, to ensure the representativeness and feasibility of the research. The following sampling principles were used: to select households proportionally to the number of adolescents per community and interview only one adolescent per household. Also, the sample was calculated separately for each stratum to facilitate valid estimates for Quilombola and non-Quilombola populations.
The research population was estimated at 811 adolescents, divided into two strata: Quilombola (n = 350) living in the Quilombola communities recognized by the FCP, and non-Quilombola (n = 461). This sample universe was obtained from a survey carried out at the Family Health Units (USF) and confirmed in a subsequent mapping of the communities.
The following criteria were considered for the sample design: prevalence of 50%, given the heterogeneity of the events measured, an accuracy of 5%, a confidence level of 95% and design effect equal to 1.0, totaling 184 Quilombola and 210 non-Quilombola adolescents. An additional 15% was added to cater for possible losses. However, considering that only one adolescent per household would be interviewed and, among the Quilombola, the number of households would be exceeded, 7.1% were added for losses in this group.
Sampling for the non-Quilombola stratum was performed by randomly selecting households that contained adolescents, followed by their proportional distribution by community. Subsequently, adolescents were randomly selected by household. Concerning the Quilombola stratum, we only proceeded with the random selection of adolescents by household. The presence of severe mental disorders with cognitive impairment among adolescents was an exclusion criterion.
The tool used to conduct interviews was a structured questionnaire based on surveys conducted in Brazil. For this study, questions were drawn from the National School Health Survey (PeNSE) 1919. Instituto Brasileiro de Geografia e Estatística (IBGE). Questionário PENSE 2012 [internet]. 2012 [acessado 2014 Jun 16]. Disponível em: http://biblioteca.ibge.gov.br/biblioteca-catalogo?view=detalhes&id=52908
http://biblioteca.ibge.gov.br/biblioteca...
, the National Health Survey (PNS) 2020. Pesquisa Nacional de Saúde (PNS). Questionário do Domicílio [internet]. 2013 [acessado 2014 Jun 16]. Disponível em: http://www.pns.icict.fiocruz.br/arquivos/Domiciliar/Modulo%20A-PNS.pdf
http://www.pns.icict.fiocruz.br/arquivos...
and the National Oral Health Survey (SBBrasil) 2121. Brasil. Ministério da Saúde (MS). Projeto SBBrasil 2010: Pesquisa Nacional de Saúde Bucal – Resultados Principais . Brasília: MS; 2011. [acessado 2016 Out 22]. Disponível em: http://dab.saude.gov.br/CNSB/sbbrasil/arquivos/projeto_sb2010_
http://dab.saude.gov.br/CNSB/sbbrasil/ar...
.
The questionnaire was divided into two blocks, the first one containing questions about household and economic characteristics was answered by the adolescent (when aged ≥ 18 years) or by the person responsible. The second block was responded to only by adolescents, containing information about them.
A pilot study was conducted in December 2014 with rural adolescents not belonging to the primaryresearch. Data were collected between January and May 2015. Re-interviews were carried out in 5% of the sample households within seven days after the first interview, toensure data quality.
Oral hygiene habits were evaluated based on the frequency of tooth brushing and flossing. The rate of tooth brushing was obtained from the question In the last 30 days, how many times a day did you usually brush your teeth ? With the following answer options: a) I have not brushed my teeth in the last 30 days; b) Once a day; c) Twice a day; d) Three times a day; e) Four or more times a day; and f) I did not brush my teeth daily. The flossing was obtained from the following question What do you use to clean your mouth ?, where one of the secondary questions was Dental floss ? (No;Yes). For purposes of bivariate and multivariate analyses, the following were considered as outcomes: (1) unsatisfactory tooth brushing frequency when less than three times a day; (2) non-flossing.
The independent variables were selected considering a conceptual model based on Petersen 2222. Petersen PE. Sociobehavioural risk factors in dental caries – international perspectives. Community Dent Oral Epidemiol 2005 ; 33(4):274-279. , organized in two blocks. The first block had sociocultural and environmental factors and the second block had variables related to the use of dental services.
Sociocultural factors were: economic level 2323. Associação Brasileira de Empresas de Pesquisa (ABEP). Critério de classificação econômica Brasil . [site da Internet] 2017. [acessado 2017 Abr 19]. Disponível em: http://www.abep.org/criterio-brasil
http://www.abep.org/criterio-brasil...
(B and C – higher levels; D and E – lower level); gender; skin color/ethnicity, classified as black (brown and black) and non-black (white, yellow and indigenous); age; schooling; one dose of alcoholic beverage; tobacco use; trying out illicit drugs; physical activity; number of close friends; family composition; feeling lonely in the last 12 months; parental understanding of personal problems in the previous 30 days.
Having as the primary source of water supply the general distribution network was considered an environmental factor, as well as the habit of hand hygiene before meals. The second block was composed of the following variables: oral health self-assessment; perception of the need for dental treatment; dental pain in the last six months; and dental consultation in the last year.
A descriptive analysis of oral health-related characteristics was made through the distribution of frequencies for the total sample and by stratum, Quilombola and non-Quilombola, as well as the estimation of the prevalence of tooth brushing and dental flossing. Differences between proportions were assessed by Pearson’s chi-square test and Fisher’s exact test.
A bivariate analysis was performed to identify the variables associated with poor tooth brushing and non-flossing. Estimates of prevalence ratios and confidence intervals were made using Poisson regression with a robust variance for the total sample and by stratum. All variables with a level of significance lower than 20% were included in the multiple analysis.
The hierarchical entry of variables in blocks was adopted in the multiple analysis. First block variables remained as adjustment factors for the second hierarchically lower block, and those with a p-value <0.05remained in the model. The comparison between models was made by the Akaike criterion and Bayesian information. The adequacy of values predicted by the models to the observed values was evaluated by chi-square. Stata, version 15.0 (Stata Corporation, College Station, USA) was used for data analysis.
Results
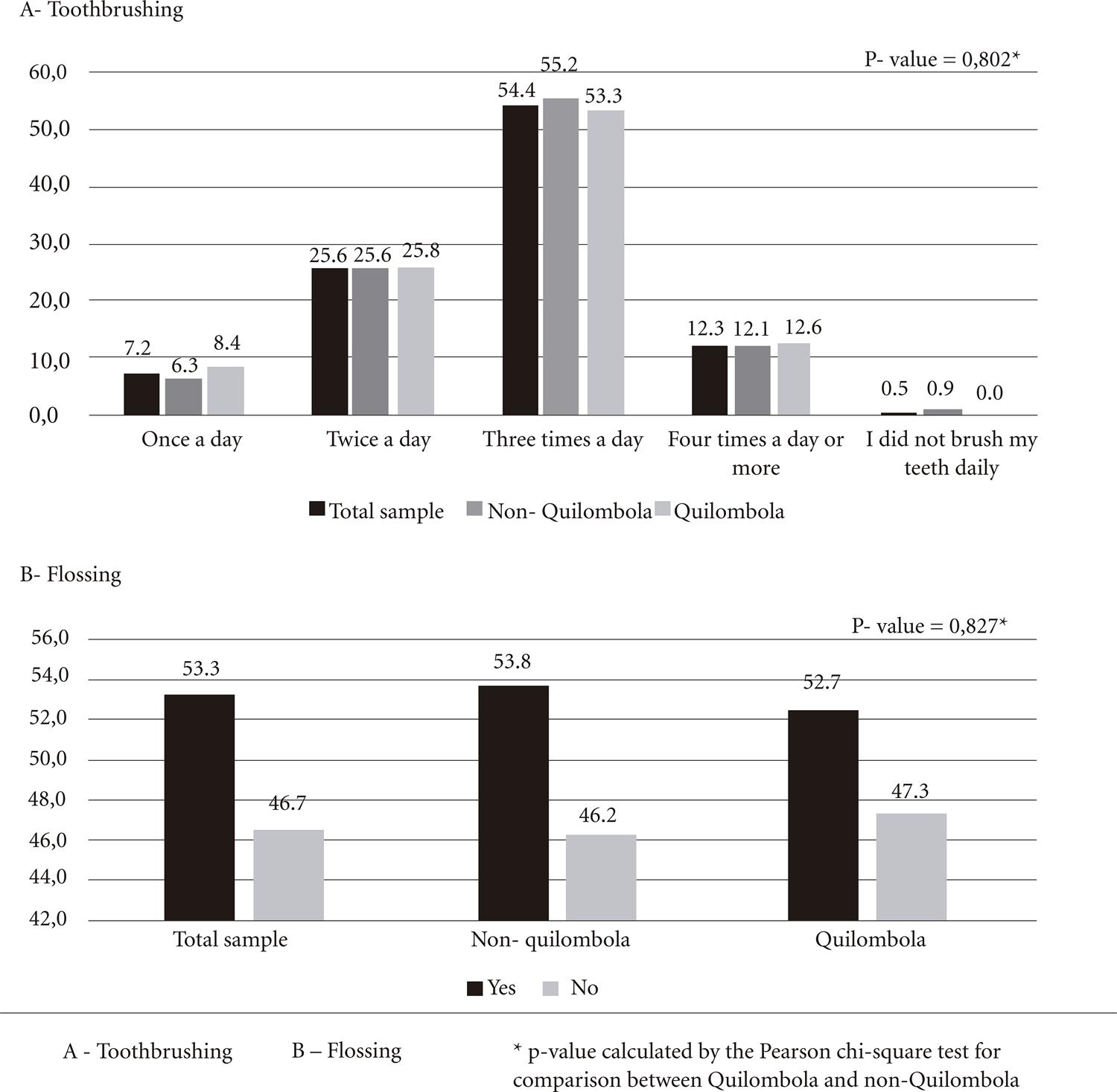
A total of 390 adolescents were interviewed, of which 42.8% (167) were Quilombola. Tooth brushing less than three times a day was observed in 33.3% of the total sample, 32.7% of non-Quilombola adolescents and 34.1% of Quilombola (Figure 1A). The prevalence of non-flossing was 46.7% for the total number of adolescents and 46.2% and 47.3% among non-Quilombola and Quilombola, respectively (Figure 1B). No significant differences were found between the two strata evaluated.
Prevalence of tooth brushing and flossing in the total sample, non-Quilombola and Quilombola. Bahia, 2015.
Most adolescents reported using toothbrush and toothpaste (99.7%) to perform oral hygiene, and 49.5% stated that they would replace the toothbrush with less than three months of use. Regarding oral health, 63.0% of adolescents considered their oral health to be good or very good, 48.1% reported a need for dental treatment and 2.6% for total dental prosthesis, 19.6% reported dental pain in the last six months and 73.1% said they were satisfied or very satisfied with their teeth and mouth ( Table 1 ).
Of the total number of adolescents, 15.6% reported no dental appointments in their lifetime and 33.2% had no dental appointments in the last year. Of the adolescents who had already had a dental appointment, 67.8% used the public service and 66.8% were attended to in anFHU, 50.8% did so for cleaning, maintenance, revision or prevention purposes, 41.9% due to tooth pain, extraction, gum problems and dental treatment and 7.3% due to orthodontic appliance maintenance or budgets, and 85.4% considered the last appointment good or very good. Differences between Quilombola and non-Quilombola adolescents were observed only for the variable dentalappointment in the lifetime, where 22.7% and 10.3% reported no consultation, respectively ( Table 1 ).
Unsatisfactory tooth brushing was significantly higher in male adolescents, who did not live with both parents, did not practice hand hygiene before meals often and considered their oral health to be either fair, poor or very poor ( Table 2 ).
Among non-Quilombola adolescents, a positive and significant association was observed between unsatisfactory tooth brushing and males, not living with both parents, with a lower frequency of hand hygiene before meals and no dental consultation in the last year. A negative association with parental understanding of their problems was sometimes observed in the last 30 days. In the Quilombola stratum, tooth brushing less than three times a day was more prevalent among those who did not wash their hands before meals frequently and those who reported worse oral health ( Table 2 ).
Regarding the non-flossing, a positive and significant association with economic level E was observed in the total sample, lack of the general distribution network as the primary form of water supply, rare or no hand hygiene before meals, and fair, poor or very poor oral health. A negative association was observed with the highest age and schooling ( Table 3 ).
The non-flossing was more prevalent among non-Quilombola adolescents of economic level E, who reported not washing their hands before meals frequently and did not consult a dentist in the last year, and less prevalent among older adolescents and higher schooling. Among the Quilombola, a positive association was observed with parents never o rarely understanding personal problems in the last 30 days and with the lack of the general network of distribution as the primary form of water supply and negative with the higher age and not having consulted the dentist in the last year ( Table 3 ).
The following factors were independently associated with unsatisfactory tooth brushing in the total sample: being male (PR = 1.45, 95% CI = 1.10-1.92); living only with one of the parents or not living with the parents (PR = 1.45, 95% CI = 1.11-1.90); hand hygiene before meals sometimes, rarely or not at all (PR = 1.72, 95% CI = 1.32-2.24); and reporting poor or very poor oral health (OR = 1.38, 95% CI = 1.05-1.82). Concerning the non-Quilombola stratum, being male (PR = 1.96, 95% CI = 1.32-2.91), living only with one of the parents or not living with the parents (PR = 1.57, 95% CI = 1.12-2.21), hand hygiene before meals sometimes, rarely or not at all (PR = 1.91, 95% CI = 1.36-2.68) and not having consulted a dentist in the last year (PR = 1.50, 95% CI = 1.04-2.16) were positively associated. Concerning the quilombola, a positive association was found with hand hygiene before meals (sometimes, frequently) (PR = 1.59, 95% CI = 1.05-2.40) and poor or very poor oral health (PR = 1.72,CI 95% = 1.12-2.62) ( Table 4 ).
The non-flossing in the total sample was independently associated with the economic level E (PR = 1.54, CI95% = 1.19-2.01), age (PR = 0.91, CI95% = 0.88-0.95), hand hygiene before meals (sometimes, rarely or not at all) (PR = 1.53, 95% CI = 1.25-1.88) and reportingpoor or very poor oral health (PR = 1.33, 95 % CI = 1.09-1.64) ( Table 4 ).
Among non-quilombola adolescents, the following were independently associated with non-flossing: economic level E (PR = 1.57, 95% CI = 1.12-2.22), age (PR = 0.91 95% CI = 0.86-0.95), hand hygiene before meals (sometimes, rarely or not at all) (PR = 1.71, 95% CI = 1.31-2.23) and not having consulted the dentist in the last year (PR = 1.31 95% CI = <1.00-1.71). In the Quilombola, a positive association was found with the parents’ understanding of personal problems – sometimes or rarely in the last 30 days (PR = 1.51, 95% CI = 1.04-2.20), sometimes and(PR = 1.64, 95% CI = 1.11-2.42) never or rarely, lack of general distribution network as the main form of water supply (PR = 1.46, 95% CI = 1.07-2.00) and reporting poor or very poor oral health (OR = 1.51, 95% CI = 1.12-2.05) and negative association with having older age (PR = 0.91, 95% CI = 0.86-0.97) ( Table 4 ).
Discussion
Satisfactory oral hygiene, tooth brushing and flossing habits were found in most of the study population. Quilombola and non-Quilombola adolescents did not differ about the prevalence of these habits. However, differences were found in sociocultural and environmental factors and factors related to the use of the dental services associated with these practices.
Freire et al. 1010. Freire MCM, Jordão LMR, Malta DC, Andrade SSC, Peres MA. Desigualdades econômicas e mudanças nos comportamentos em saúde bucal de adolescente brasileiros de 2009 a 2012. Rev Saude Publica [periódico na Internet]. 2015 [acessado 2017 Abr 9]; 49:50. Disponível em: http://www.scielo.br/pdf/rsp/v49/pt_0034-8910-rsp-S0034-89102015049005562.pdf
http://www.scielo.br/pdf/rsp/v49/pt_0034...
, in a study with Brazilian ninth-graders of elementary school, found results similar to this study for tooth brushing ≥ twotimes/day in 2009 (95.2%) and 2012 (91.7%). However, brushing ≥ 3x / day, indicated by several studies such as the recommended daily rate for adolescence, had a lower prevalence than that found among adolescents from different Brazilian regions 44. Silveira MF, Marôco JP, Freire RS, Barros Lima Martins AME, Marcopito LF. Impacto da saúde bucal nas dimensões físicas e psicossocial: uma análise através da modelagem com equações estruturais. Cad Saude Publica [periódico na Internet].2014 Jun [acessado 2017 Mar 18];30(6):1-15. Disponível em: http://www.scielo.br/pdf/csp/v30n6/pt_0102-311X-csp-30-6-1169.pdf
http://www.scielo.br/pdf/csp/v30n6/pt_01...
, 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
, 88. Melo FGC, Cavalcanti AL. Hábitos de higiêne bucal e uso dos serviços odontológicos em estudantes de escolas públicas do município de Campina Grande, Paraíba. HU Revista [periódico na Internet].2009 Jul-Set [acessado 2017 Abr 20 ]; 35(3):191-198. Disponível em: https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721
https://hurevista.ufjf.emnuvens.com.br/h...
, 2424. Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa Nacional De Saúde Escolar (PeNSE, 2015) [internet]. 2016 [acessado 2016 Set 05]. Disponível em: http://www.ibge.gov.br/home/estatistica/população/pense/2015/default.shtm
http://www.ibge.gov.br/home/estatistica/...
. Flossing was higher than reported by studies with children and adolescents (9-12 years) in rural Pernambuco (33.3%) 1313. Menezes VA, Lorena RPF, Rocha LCB, Leite AF, Ferreira JMS, Granville-Garcia AF. Práticas de higiene bucal, uso de serviço odontológico e autopercepção de saúde bucal de escolares da zona rural de Caruaru, PE, Brasil. Rev. Odonto ciên [periódico na Internet]. 2010 [acessado 2017 Mar 02]; 25(1):25-31. Disponível em: http://www.scielo.br/pdf/roc/v25n1/06.pdf
http://www.scielo.br/pdf/roc/v25n1/06.pd...
, with rural and urban adolescents in Campina Grande (PB) (0.5%) 88. Melo FGC, Cavalcanti AL. Hábitos de higiêne bucal e uso dos serviços odontológicos em estudantes de escolas públicas do município de Campina Grande, Paraíba. HU Revista [periódico na Internet].2009 Jul-Set [acessado 2017 Abr 20 ]; 35(3):191-198. Disponível em: https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721
https://hurevista.ufjf.emnuvens.com.br/h...
and urban adolescents from other Brazilian regions 44. Silveira MF, Marôco JP, Freire RS, Barros Lima Martins AME, Marcopito LF. Impacto da saúde bucal nas dimensões físicas e psicossocial: uma análise através da modelagem com equações estruturais. Cad Saude Publica [periódico na Internet].2014 Jun [acessado 2017 Mar 18];30(6):1-15. Disponível em: http://www.scielo.br/pdf/csp/v30n6/pt_0102-311X-csp-30-6-1169.pdf
http://www.scielo.br/pdf/csp/v30n6/pt_01...
, 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
. International studies showed a lower prevalence of tooth brushing and flossing 1111. Pereira C, Veiga N, Amaral O, Pereira. Comportamentos de saúde oral em adolescentes portugueses. Rev Port Saúde Pública [periódico na Internet]. 2013 Jul [acessado 2017 Mar 18]; 31(2):145-152. Disponível em: http://www.elsevier.pt/pt/revistas/revista-portuguesa-saude-publica-323/artigo/comportamentos-saude-oral-em-adolescentes-portuguesesS0870902513000278
http://www.elsevier.pt/pt/revistas/revis...
, 2525. Pengpid S, Peltzer K. Hygiene Behaviour and Associated Factors among In-School Adolescents in Nine African Countries. Int.J. Behav. Med . 2011 ; 18(2):150-159.
26. Barata C, Veiga N, Mendes C, Araújo F, Ribeiro O, Coelho I. Determinação do CPOD e comportamentos de saúde oral numa amostra de adolescentes do concelho de Mangualde. Rev Port Estomaltol Med Dent Cir Maxilofac [periódico na Internet]. 2013 [acessado em 2017 Mar 18]; 54(1):27-32. Disponível em: www.sciencedirect.com/science/article/pii/S1646289013000046
www.sciencedirect.com/science/article/pi...
27. Casanova-Rosado AJ, Medina-Solís CE, Casanova-Rosado JF, Vallejos-Sánchez AA, Minaya-Sánchez M, Mendoza-Rodríguez M, Márquez-Rodríguez S, Maupomé G. Tooth brushing frequency in Mexican schoolchildren and associated socio-demographic, socioeconomic, and dental variables. Med Sci Monit 2014 ; 20:938-944.
28. Silva RMA, Bezerra V, Medeiros DS. Experimentação de tabaco e fatores associados entre adolescentes da zona rural de Vitória da Conquista, BA, Brasil. Cien Saude Colet [periódico na Internet]. [acessado 2017 Out 22] No prelo. Disponível em: http://www.cienciaesaudecoletiva.com.br/artigos/experimentacao-de-tabaco-e-fatores-associados-entre-adolescentes-da-zona-rural-de-vitoria-da-conquista-ba-brasil/16171
http://www.cienciaesaudecoletiva.com.br/...
29. Santana KC, Teles N, Oliveira MHB, Medeiros DS. Direito à saúde: adolescentes quilombolas em comunidades rurais de Vitória da Conquista (BA). In: Oliveira MHB, Erthal RMC, Vianna MB, Matta JLJ, Vasconcellos LCF, Bonfatti RJ, organizadores. Direitos humanos e saúde: construindo caminhos, viabilizando rumos . Rio de Janeiro: Cebes; 2017 . v. 1. p. 53-68.
30. Conselho Federal de Odontologia (CFO). Código de Ética Odontológica . 2012. [acessado 2017 Out 23]. Disponível em: http://cfo.org.br/wp-content/uploads/2009/09/codigo_etica.pdf
http://cfo.org.br/wp-content/uploads/200...
31. Gomes KO, Reis EA, Guimarães MDC, Cherchiglia ML. Utilização de serviços de saúde por população quilombola do Sudoeste da Bahia, Brasil . Cad Saude Publica [periódico na Internet]. 2013 Set [acessado 2017 Out 23]; 29(9):1829-1842. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102311X2013000900022&lng=en
http://www.scielo.br/scielo.php?script=s...
32. Santos NCN, Alves TDB, Freitas VS. A saúde bucal de adolescentes: aspectos de higiene, de cárie dentária e doença periodontal nas cidades de Recife, Pernambuco e Feira de Santana, Bahia. Cien Saude Colet [periódico na Internet]. 2007 [acessado 2017 Mar 04]; 12(5):1155-1166. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-81232007000500012
http://www.scielo.br/scielo.php?script=s...
33. Freddo SL, Castro Aerts DRG, Abegg C, Davoglio R, Vieira PC, Monteiro L. Hábitos de higiene bucal e utilização de serviços odontológicos em escolares de uma cidade da Região Sul do Brasil. Cad Saude Publica [periódico na Internet]. 2008 Set [acessado 2017 Fev 20]; 24(9):1992- 2000. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2008000
http://www.scielo.br/scielo.php?script=s...
34. Brasil. Ministério da Saúde (MS). Diretrizes da Política Nacional de Saúde Bucal . [Internet]. 2004 [acessado 2017 Maio 18]. Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/politica_nacional_brasil_sorridente.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
35. Garbin CAS, Garbin AJI, Moimaz SDC, Gonçalves PE. A saúde na percepção do adolescente. Rev Physis [periódico na Internet]. 2009 [acessado 2017 Fev 08]; 19(1):227-238. Disponível em: http://www.scielo.br/scielo.php?pid=S0103-73312009000100012&script=sci_abstract&tlng=pt
http://www.scielo.br/scielo.php?pid=S010...
36. Avlund K, Pedersen PH, Morse DE, Viitanen M, Winbland B.Social relations as determinants of oral healter among persons over the age of 80 years. Rev. Comunnity Dentistry and Oral Epidemiology [periódico na Internet] 2003[acessado 2017 Maio 10]:32;454-462. Disponível em: http://onlinelibrary.wiley.com/doi/10.1046/j.1600-0528.2003.00115.x/abstract
http://onlinelibrary.wiley.com/doi/10.10...
- 3737. Dorri M, Sheiham A, Watt RG. Relationship between general hygiene behaviours and oral hygiene behaviours in Iranian adolescentes. Eur J Oral Sci 2009; 117(4):407-412. .
The literature evidences that Brazilians have a reasonable frequency in oral hygiene habits. However, the quality of this hygiene can leave something to be desired 11. Silva Junior IF, Aguiar NL, Barros RC, Arantes DC, Nascimento LS. Saúde Bucal do Adolescente: Revisão de Literatura. Rev Adolesc. Saúde [periódico na Internet] 2016 agosto [acessado em 2017 Abr 19]; 13(Supl. 1):95-103. Disponível em: http://www.adolescenciaesaude.com
http://www.adolescenciaesaude.com...
. This situation contributes to the fact that the eradication of oral diseases in the country is still a distant reality. It is emphasized that not only individual practices are responsible for oral health care but, when other types of social policies are lacking, these practices become even more crucial 11. Silva Junior IF, Aguiar NL, Barros RC, Arantes DC, Nascimento LS. Saúde Bucal do Adolescente: Revisão de Literatura. Rev Adolesc. Saúde [periódico na Internet] 2016 agosto [acessado em 2017 Abr 19]; 13(Supl. 1):95-103. Disponível em: http://www.adolescenciaesaude.com
http://www.adolescenciaesaude.com...
.
Quilombola and non-Quilombola adolescents did not differ about the prevalence of tooth brushing and flossing, but differences were found in the use of dental services during lifetime and factors associated with poor oral hygiene habits, evidencing that there are specificities among these groups.
The similar prevalence of health-related behavioral aspects between Quilombola and non-Quilombola was also reported by Silva et al. 2828. Silva RMA, Bezerra V, Medeiros DS. Experimentação de tabaco e fatores associados entre adolescentes da zona rural de Vitória da Conquista, BA, Brasil. Cien Saude Colet [periódico na Internet]. [acessado 2017 Out 22] No prelo. Disponível em: http://www.cienciaesaudecoletiva.com.br/artigos/experimentacao-de-tabaco-e-fatores-associados-entre-adolescentes-da-zona-rural-de-vitoria-da-conquista-ba-brasil/16171
http://www.cienciaesaudecoletiva.com.br/...
, in a study about tobacco experimentation in this same population. It is suggested that the social interaction of these adolescents in school could favor the mutual influence between them, transposing effects of the family, the environment and their neighborhood 1111. Pereira C, Veiga N, Amaral O, Pereira. Comportamentos de saúde oral em adolescentes portugueses. Rev Port Saúde Pública [periódico na Internet]. 2013 Jul [acessado 2017 Mar 18]; 31(2):145-152. Disponível em: http://www.elsevier.pt/pt/revistas/revista-portuguesa-saude-publica-323/artigo/comportamentos-saude-oral-em-adolescentes-portuguesesS0870902513000278
http://www.elsevier.pt/pt/revistas/revis...
, 2929. Santana KC, Teles N, Oliveira MHB, Medeiros DS. Direito à saúde: adolescentes quilombolas em comunidades rurais de Vitória da Conquista (BA). In: Oliveira MHB, Erthal RMC, Vianna MB, Matta JLJ, Vasconcellos LCF, Bonfatti RJ, organizadores. Direitos humanos e saúde: construindo caminhos, viabilizando rumos . Rio de Janeiro: Cebes; 2017 . v. 1. p. 53-68. . This interaction is even more evident in rural areas, where the supply of educational services is reduced when compared to urban ones.
The difference about performing dental consultations during lifetime can be explained, in part, by the location of USFs, which, are mostly based in non-Quilombola communities. The actions of health teams in Quilombola communities take place about once a month in satellite units that do not have the necessary infrastructure for dental consultation 2929. Santana KC, Teles N, Oliveira MHB, Medeiros DS. Direito à saúde: adolescentes quilombolas em comunidades rurais de Vitória da Conquista (BA). In: Oliveira MHB, Erthal RMC, Vianna MB, Matta JLJ, Vasconcellos LCF, Bonfatti RJ, organizadores. Direitos humanos e saúde: construindo caminhos, viabilizando rumos . Rio de Janeiro: Cebes; 2017 . v. 1. p. 53-68. . Thus, dental care is restricted to USF headquarters and educational actions are carried out in other communities. These facts add up to the obligatory presence of a responsible person over 18 years of age for the first dental care of the adolescent 3030. Conselho Federal de Odontologia (CFO). Código de Ética Odontológica . 2012. [acessado 2017 Out 23]. Disponível em: http://cfo.org.br/wp-content/uploads/2009/09/codigo_etica.pdf
http://cfo.org.br/wp-content/uploads/200...
, which increases the difficulty of the first access of Quilombola adolescents to dental services. When studying the use of health services by the adult Quilombola population of Vitória da Conquista (BA), Gomes et al. 3131. Gomes KO, Reis EA, Guimarães MDC, Cherchiglia ML. Utilização de serviços de saúde por população quilombola do Sudoeste da Bahia, Brasil . Cad Saude Publica [periódico na Internet]. 2013 Set [acessado 2017 Out 23]; 29(9):1829-1842. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102311X2013000900022&lng=en
http://www.scielo.br/scielo.php?script=s...
suggested that there is a higher difficulty in accessing services by Quilombola due to the inequities faced by this population, especially worse social and economic conditions.
Male adolescents had a higher prevalence of unsatisfactory tooth brushing, a result corroborated by other studies 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
8. Melo FGC, Cavalcanti AL. Hábitos de higiêne bucal e uso dos serviços odontológicos em estudantes de escolas públicas do município de Campina Grande, Paraíba. HU Revista [periódico na Internet].2009 Jul-Set [acessado 2017 Abr 20 ]; 35(3):191-198. Disponível em: https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721
https://hurevista.ufjf.emnuvens.com.br/h...
9. Vettore MV, Moysés SJ, Sardinha LMV, Iser BPM. Condições socioeconômicas, frequência de escovação dentária e comportamentos em saúde em adolescentes brasileiros: uma análise a partir da Pesquisa Nacional de Saúde escolar (PeNSE). Cad Saude Publica [periódico na Internet].2012 [acessado 2017 Mar 18]; 28(Supl.):S101-S113. Disponível em: http://www.scielosp.org/pdf/csp/v28s0/11.pdf
http://www.scielosp.org/pdf/csp/v28s0/11...
- 1010. Freire MCM, Jordão LMR, Malta DC, Andrade SSC, Peres MA. Desigualdades econômicas e mudanças nos comportamentos em saúde bucal de adolescente brasileiros de 2009 a 2012. Rev Saude Publica [periódico na Internet]. 2015 [acessado 2017 Abr 9]; 49:50. Disponível em: http://www.scielo.br/pdf/rsp/v49/pt_0034-8910-rsp-S0034-89102015049005562.pdf
http://www.scielo.br/pdf/rsp/v49/pt_0034...
. This behavior can be explained by a greater concern of adolescent girls regarding aesthetics and care with oral hygiene due to current social and cultural standards 3232. Santos NCN, Alves TDB, Freitas VS. A saúde bucal de adolescentes: aspectos de higiene, de cárie dentária e doença periodontal nas cidades de Recife, Pernambuco e Feira de Santana, Bahia. Cien Saude Colet [periódico na Internet]. 2007 [acessado 2017 Mar 04]; 12(5):1155-1166. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-81232007000500012
http://www.scielo.br/scielo.php?script=s...
. However, this difference between genders was not observedin the Quilombola stratum and more studies are required to understand the specificities of this group better.
The socioeconomic condition was only associated with the use of dental floss in the total sample and among non-Quilombola, a result similar to other studies with adolescents 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
, 3333. Freddo SL, Castro Aerts DRG, Abegg C, Davoglio R, Vieira PC, Monteiro L. Hábitos de higiene bucal e utilização de serviços odontológicos em escolares de uma cidade da Região Sul do Brasil. Cad Saude Publica [periódico na Internet]. 2008 Set [acessado 2017 Fev 20]; 24(9):1992- 2000. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2008000
http://www.scielo.br/scielo.php?script=s...
. Dental floss, compared to toothbrushes, is a more expensive product and its use is a less consolidated habit, which may have influenced the greater use of better-off adolescents 3636. Avlund K, Pedersen PH, Morse DE, Viitanen M, Winbland B.Social relations as determinants of oral healter among persons over the age of 80 years. Rev. Comunnity Dentistry and Oral Epidemiology [periódico na Internet] 2003[acessado 2017 Maio 10]:32;454-462. Disponível em: http://onlinelibrary.wiley.com/doi/10.1046/j.1600-0528.2003.00115.x/abstract
http://onlinelibrary.wiley.com/doi/10.10...
. The National Oral Health Policy – Programa Brasil Sorridente (Smiling Brazil Program), provides for the availability of basic dental care appropriate to the population 3434. Brasil. Ministério da Saúde (MS). Diretrizes da Política Nacional de Saúde Bucal . [Internet]. 2004 [acessado 2017 Maio 18]. Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/politica_nacional_brasil_sorridente.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
. However, not only toothbrush and fluoride dentifrice would be necessary, but also the distribution of dental floss, which would possibly reduce the effect of economic conditions on habit-forming.
The greater homogeneity of the Quilombola population about the economic level may have contributed to the absence of this variable in the final model for this stratum. Also, it is local practice to carry out educational activities with the rural population on the making of dental floss in a handmade fashion (raffia) using lineage bags, material easily accessible in rural and Quilombola communities, by professionals of the oral health teams.
The one-year age increase reduced the prevalence of non-use of dental floss by around 9%, a relationship already evidenced in a study with adolescents from Paraíba 88. Melo FGC, Cavalcanti AL. Hábitos de higiêne bucal e uso dos serviços odontológicos em estudantes de escolas públicas do município de Campina Grande, Paraíba. HU Revista [periódico na Internet].2009 Jul-Set [acessado 2017 Abr 20 ]; 35(3):191-198. Disponível em: https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721
https://hurevista.ufjf.emnuvens.com.br/h...
. The greatest attention to oral health is related to affectivity and social interaction 3535. Garbin CAS, Garbin AJI, Moimaz SDC, Gonçalves PE. A saúde na percepção do adolescente. Rev Physis [periódico na Internet]. 2009 [acessado 2017 Fev 08]; 19(1):227-238. Disponível em: http://www.scielo.br/scielo.php?pid=S0103-73312009000100012&script=sci_abstract&tlng=pt
http://www.scielo.br/scielo.php?pid=S010...
, aspects that can contribute to greater care among older adolescents.
Family aspects influenced oral hygiene habits of rural adolescents, a result corroborated by other studies. Davoglio et al. 77. Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
http://www.scielo.br/pdf/csp/v25n3/20.pd...
argue that when parents do not understand adolescents, they may assume a disinterested posture vis-à-vis their appearance and self-care as a form of protest. Also, individuals who live alone or who have low satisfaction with their social relationships tend to adopt less preventive health behaviors 3636. Avlund K, Pedersen PH, Morse DE, Viitanen M, Winbland B.Social relations as determinants of oral healter among persons over the age of 80 years. Rev. Comunnity Dentistry and Oral Epidemiology [periódico na Internet] 2003[acessado 2017 Maio 10]:32;454-462. Disponível em: http://onlinelibrary.wiley.com/doi/10.1046/j.1600-0528.2003.00115.x/abstract
http://onlinelibrary.wiley.com/doi/10.10...
.
These findings show that health care with a focus on families can bring good results to adolescents’ oral health. Considering that the Family Health Strategy is commonly present in rural areas, family core-oriented educational activities could be developed by oral health teams, as well as by community health workers, mainly through home visits.
Oral hygiene is a physical hygiene component but requires learning 3434. Brasil. Ministério da Saúde (MS). Diretrizes da Política Nacional de Saúde Bucal . [Internet]. 2004 [acessado 2017 Maio 18]. Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/politica_nacional_brasil_sorridente.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
to be carried out correctly. Studies show that oral hygieneis significantly associated with regular hygiene habits 99. Vettore MV, Moysés SJ, Sardinha LMV, Iser BPM. Condições socioeconômicas, frequência de escovação dentária e comportamentos em saúde em adolescentes brasileiros: uma análise a partir da Pesquisa Nacional de Saúde escolar (PeNSE). Cad Saude Publica [periódico na Internet].2012 [acessado 2017 Mar 18]; 28(Supl.):S101-S113. Disponível em: http://www.scielosp.org/pdf/csp/v28s0/11.pdf
http://www.scielosp.org/pdf/csp/v28s0/11...
, 3737. Dorri M, Sheiham A, Watt RG. Relationship between general hygiene behaviours and oral hygiene behaviours in Iranian adolescentes. Eur J Oral Sci 2009; 117(4):407-412. . In this study, dental brushing ≤ threetimes/day and non-use of dental floss were more prevalent among adolescents who reported not washing their hands before meals frequently.
Among the Quilombola, non-use of dental floss was more prevalent in adolescents who did not have the general distribution network as their primary source of water supply at home, which reinforces the vulnerability and need for self-care practices in this group, since it has less continuous access to fluoridated water. Public water fluoridation has been mandatory in Brazil since 1974. However, non-universal access to fluoridated water keeps an extensive number of people on the fringe of this admittedly effective and cost-effective relationship 3838. Antunes JLF, Narvai PC. Políticas de saúde bucal no Brasil e seu impacto sobre as desigualdades em saúde. Rev Saude Publica [periódico na Internet]. 2010 Abr [acessado 2017 Out 22]; 44(2): 360-365. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S003489102010000200018&lng=en.
http://www.scielo.br/scielo.php?script=s...
.
Self-assessment of oral health as fair, poor or very poor was one of the variables associated with poor oral hygiene habits. The agreement between the clinical condition and self-perceived oral health usually occurs in more severe painful and aesthetic cases, while other milder oral problems are underestimated 3939. Narvai PC, Frazão P. Saúde Bucal no Brasil: Muito Além do Céu da Boca . Rio de Janeiro: Editora Fiocruz; 2008 . . Poor oral condition has negative impacts on the daily activities of adolescents, among them, the greater difficulty in tooth brushing. Less frequent tooth brushing may, therefore, be a consequence of poor oral condition, which may influence the outcome found in this study. It should be emphasized that the perception of oral health is also related to socio-cultural and personal characteristics of individuals 3939. Narvai PC, Frazão P. Saúde Bucal no Brasil: Muito Além do Céu da Boca . Rio de Janeiro: Editora Fiocruz; 2008 . .
The lack of dental consultation in the last year was a factor that increased poor oral hygiene habits only for the non-Quilombola stratum. The contact of the dental professional with the adolescent influences the adoption of satisfactory oral hygiene habits. However, although dental work is relevant, it solves individual problems recognized by those who use it. In population terms, oral health care results from a range of factors – biological, psychological and social 3939. Narvai PC, Frazão P. Saúde Bucal no Brasil: Muito Além do Céu da Boca . Rio de Janeiro: Editora Fiocruz; 2008 . .
This work has some limitations because it is a cross-sectional study, which prevents us from inferring the temporality of some of the associations observed. The sample size was not planned to test differences between Quilombola and non-Quilombola, so there may not have been enough sampling power for some variables. However, this fact does not compromise the differences observed and described. Also, no information was collected on the clinical conditions of the adolescents, the tooth brushing and use of dental floss technique, as well as hygiene hours, hindering the analysis of these aspects.
Final considerations
Oral health policies are still recent in Brazil and aim to promote, prevent diseases and restore the oral health of individuals. However, practices aimed at recovery are again emphasized, which makes it necessary to redirect the work process to create support for comprehensive care and the needs of different population groups 3939. Narvai PC, Frazão P. Saúde Bucal no Brasil: Muito Além do Céu da Boca . Rio de Janeiro: Editora Fiocruz; 2008 . .
The National Oral Health Policy Directives provide for supervised oral hygiene activities so that autonomy is developedto self-care 3434. Brasil. Ministério da Saúde (MS). Diretrizes da Política Nacional de Saúde Bucal . [Internet]. 2004 [acessado 2017 Maio 18]. Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/politica_nacional_brasil_sorridente.pdf
http://bvsms.saude.gov.br/bvs/publicacoe...
. However, these activities are commonly geared to children, not covering adolescents, especially older ones. Collective measures facilitate savings regarding financial and human resources and are fundamental within a single health system to ensure the integrality of care, especially in more vulnerable places such as rural areas and traditional communities.
Oral health care demands intersectoral actions that consider aspects inherent to adolescents, in their social/household context, with the purpose of promoting comprehensive and resolutive adolescent oral health care. Health education actions should consider cultural traits and take into account that oral health is a component of health and transcends dentistry. The perception of oral health as a human right and not as a privilege should be increasingly strengthened, especially in populations of recognized vulnerability.
Acknowledgments
We wish to thank the rural families and adolescents, interviewers, Community Health Workers and other professionals of the Family Health Strategy teams, who have been instrumental in the implementation of this work.
Referências
-
1Silva Junior IF, Aguiar NL, Barros RC, Arantes DC, Nascimento LS. Saúde Bucal do Adolescente: Revisão de Literatura. Rev Adolesc. Saúde [periódico na Internet] 2016 agosto [acessado em 2017 Abr 19]; 13(Supl. 1):95-103. Disponível em: http://www.adolescenciaesaude.com
» http://www.adolescenciaesaude.com -
2Word Health Organization (WHO). Nutrition in adolescence – Issues and Challenges for the Health Sector [Internet]. 2005. [acessado 2017 Mar 09]. Disponível em: http://apps.who.int/iris/bitstream/10665/43342/1/9241593660_eng.pdf
» http://apps.who.int/iris/bitstream/10665/43342/1/9241593660_eng.pdf -
3Barbosa TB, Junqueira SR, Frias AC, Araujo ME. Interferência da Saúde Bucal em funções Biológicas e Sociais Segundo a percepção de Adolescentes Brasileiros. Rev Pesq Bras Odontoped Clin Integr [periódico na Internet]. 2013 Abr-Jun [acessado 2017 Abr 02];13(2)171-176. Disponível em: http://www.redalyc.org/articulo.oa?id=63730017006
» http://www.redalyc.org/articulo.oa?id=63730017006 -
4Silveira MF, Marôco JP, Freire RS, Barros Lima Martins AME, Marcopito LF. Impacto da saúde bucal nas dimensões físicas e psicossocial: uma análise através da modelagem com equações estruturais. Cad Saude Publica [periódico na Internet].2014 Jun [acessado 2017 Mar 18];30(6):1-15. Disponível em: http://www.scielo.br/pdf/csp/v30n6/pt_0102-311X-csp-30-6-1169.pdf
» http://www.scielo.br/pdf/csp/v30n6/pt_0102-311X-csp-30-6-1169.pdf -
5Peres KG, Peres MA, Araujo CLP, Menezes AMB, Hallal PC. Social and dental status along the life course and oral health impacts in adolescents: a population-based birth cohort. Health Qual Life Outcomes 2009 ; 7:95.
-
6Peres KG, Cascaes AM, Leão ATT, Côrtes MIS, Vettore MV. Aspectos sociodemográficos e clínicos da qualidade de vida relacionada à saúde bucal em adolescentes. Rev Saude Publica [periódico na Internet] 2013 [acessado 2017 Out 09]; 47(3):19-28. Disponível em: http://www.scielo.br/scielo.php?pid=S003489102013000900019&script=sci_abstract&tlng=pt
» http://www.scielo.br/scielo.php?pid=S003489102013000900019&script=sci_abstract&tlng=pt -
7Davoglio RS, Ganzo de Castro Aerts DR, Abegg C, Freddo SL, Monteiro L. Fatores associados a hábitos de saúde bucal e utilização de serviços odontológicos entre adolescentes. Cad Saude Publica [periódico na Internet]. 2009 Mar [acessado 2017 fev 12]; 25(3):665-667. Disponível em: http://www.scielo.br/pdf/csp/v25n3/20.pdf .
» http://www.scielo.br/pdf/csp/v25n3/20.pdf -
8Melo FGC, Cavalcanti AL. Hábitos de higiêne bucal e uso dos serviços odontológicos em estudantes de escolas públicas do município de Campina Grande, Paraíba. HU Revista [periódico na Internet].2009 Jul-Set [acessado 2017 Abr 20 ]; 35(3):191-198. Disponível em: https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721
» https://hurevista.ufjf.emnuvens.com.br/hurevista/article/view/721 -
9Vettore MV, Moysés SJ, Sardinha LMV, Iser BPM. Condições socioeconômicas, frequência de escovação dentária e comportamentos em saúde em adolescentes brasileiros: uma análise a partir da Pesquisa Nacional de Saúde escolar (PeNSE). Cad Saude Publica [periódico na Internet].2012 [acessado 2017 Mar 18]; 28(Supl.):S101-S113. Disponível em: http://www.scielosp.org/pdf/csp/v28s0/11.pdf
» http://www.scielosp.org/pdf/csp/v28s0/11.pdf -
10Freire MCM, Jordão LMR, Malta DC, Andrade SSC, Peres MA. Desigualdades econômicas e mudanças nos comportamentos em saúde bucal de adolescente brasileiros de 2009 a 2012. Rev Saude Publica [periódico na Internet]. 2015 [acessado 2017 Abr 9]; 49:50. Disponível em: http://www.scielo.br/pdf/rsp/v49/pt_0034-8910-rsp-S0034-89102015049005562.pdf
» http://www.scielo.br/pdf/rsp/v49/pt_0034-8910-rsp-S0034-89102015049005562.pdf -
11Pereira C, Veiga N, Amaral O, Pereira. Comportamentos de saúde oral em adolescentes portugueses. Rev Port Saúde Pública [periódico na Internet]. 2013 Jul [acessado 2017 Mar 18]; 31(2):145-152. Disponível em: http://www.elsevier.pt/pt/revistas/revista-portuguesa-saude-publica-323/artigo/comportamentos-saude-oral-em-adolescentes-portuguesesS0870902513000278
» http://www.elsevier.pt/pt/revistas/revista-portuguesa-saude-publica-323/artigo/comportamentos-saude-oral-em-adolescentes-portuguesesS0870902513000278 -
12Zhu L, Petersen PE. Oral hialita knowledge, atitudes and behaviour of children and adolescents in China. Rev. International Dental Journal [periódico na Internet]. 2003 [acessado 2017 Abr 02]; 53(5):289-298. Disponível em: http://www.who.int/oral_health/media/en/orh_knowledge_china.pdf
» http://www.who.int/oral_health/media/en/orh_knowledge_china.pdf -
13Menezes VA, Lorena RPF, Rocha LCB, Leite AF, Ferreira JMS, Granville-Garcia AF. Práticas de higiene bucal, uso de serviço odontológico e autopercepção de saúde bucal de escolares da zona rural de Caruaru, PE, Brasil. Rev. Odonto ciên [periódico na Internet]. 2010 [acessado 2017 Mar 02]; 25(1):25-31. Disponível em: http://www.scielo.br/pdf/roc/v25n1/06.pdf
» http://www.scielo.br/pdf/roc/v25n1/06.pdf -
14Moreira RS, Nico LS, Tomita NE. A relação entre o espaço e a saúde bucal coletiva: por uma epidemiologia georreferenciada. Cien Saude Colet [periódico na Internet]. 2007 [acessado 2017 Abr 20]; 12(1):275-284. Disponível em: http://www.scielo.br/pdf/csc/v12n1/27.pdf
» http://www.scielo.br/pdf/csc/v12n1/27.pdf -
15Fundação Cultural Palmares. Certidões expedidas às comunidades remanescentes de quilombos (CRQs) atualizada até a portaria nº 268/2017 . 2017. [acessado 2017 Out 22]. Disponível em: http://www.palmares.gov.br/
» http://www.palmares.gov.br/ -
16Brasil. Decreto nº 4.887, de 20 de novembro de 2003. Regulamenta o procedimento para identificação, reconhecimento, delimitação, demarcação e titulação das terras ocupadas por remanescentes das comunidades dos quilombos de que trata o art. 68 do Ato das Disposições Constitucionais Transitórias. Diário Oficial da União 2003; 21 nov.
-
17Silva EKP, Medeiros DS, Martins PC, Sousa LA, Lima GP, Rêgo MAS, Silva TO, Freire AS, Silva FM. Insegurança alimentar em comunidades rurais no Nordeste brasileiro: faz diferença ser quilombola? Cad Saude Publica [periódico na Internet]. 2017 Jun [acessado 2017 Out 22]; 33(4):e00005716. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2017000405013&lng=en
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2017000405013&lng=en -
18Silva MEA, Rosa PCF, Neves ACC, Rode SM. Necessidade protética da população quilombola de Santo Antônio do Guaporé- Rondônia- Brasil. Rev Braz Dent Sci [periódico na Internet]. 2011 Jul-Dez [acessado 2017 Mar 18]; 14(1-2)62-66. Disponível em: http://ojs.fosjc.unesp.br/index.php/cob/article/view/676
» http://ojs.fosjc.unesp.br/index.php/cob/article/view/676 -
19Instituto Brasileiro de Geografia e Estatística (IBGE). Questionário PENSE 2012 [internet]. 2012 [acessado 2014 Jun 16]. Disponível em: http://biblioteca.ibge.gov.br/biblioteca-catalogo?view=detalhes&id=52908
» http://biblioteca.ibge.gov.br/biblioteca-catalogo?view=detalhes&id=52908 -
20Pesquisa Nacional de Saúde (PNS). Questionário do Domicílio [internet]. 2013 [acessado 2014 Jun 16]. Disponível em: http://www.pns.icict.fiocruz.br/arquivos/Domiciliar/Modulo%20A-PNS.pdf
» http://www.pns.icict.fiocruz.br/arquivos/Domiciliar/Modulo%20A-PNS.pdf -
21Brasil. Ministério da Saúde (MS). Projeto SBBrasil 2010: Pesquisa Nacional de Saúde Bucal – Resultados Principais . Brasília: MS; 2011. [acessado 2016 Out 22]. Disponível em: http://dab.saude.gov.br/CNSB/sbbrasil/arquivos/projeto_sb2010_
» http://dab.saude.gov.br/CNSB/sbbrasil/arquivos/projeto_sb2010_ -
22Petersen PE. Sociobehavioural risk factors in dental caries – international perspectives. Community Dent Oral Epidemiol 2005 ; 33(4):274-279.
-
23Associação Brasileira de Empresas de Pesquisa (ABEP). Critério de classificação econômica Brasil . [site da Internet] 2017. [acessado 2017 Abr 19]. Disponível em: http://www.abep.org/criterio-brasil
» http://www.abep.org/criterio-brasil -
24Instituto Brasileiro de Geografia e Estatística (IBGE). Pesquisa Nacional De Saúde Escolar (PeNSE, 2015) [internet]. 2016 [acessado 2016 Set 05]. Disponível em: http://www.ibge.gov.br/home/estatistica/população/pense/2015/default.shtm
» http://www.ibge.gov.br/home/estatistica/população/pense/2015/default.shtm -
25Pengpid S, Peltzer K. Hygiene Behaviour and Associated Factors among In-School Adolescents in Nine African Countries. Int.J. Behav. Med . 2011 ; 18(2):150-159.
-
26Barata C, Veiga N, Mendes C, Araújo F, Ribeiro O, Coelho I. Determinação do CPOD e comportamentos de saúde oral numa amostra de adolescentes do concelho de Mangualde. Rev Port Estomaltol Med Dent Cir Maxilofac [periódico na Internet]. 2013 [acessado em 2017 Mar 18]; 54(1):27-32. Disponível em: www.sciencedirect.com/science/article/pii/S1646289013000046
» www.sciencedirect.com/science/article/pii/S1646289013000046 -
27Casanova-Rosado AJ, Medina-Solís CE, Casanova-Rosado JF, Vallejos-Sánchez AA, Minaya-Sánchez M, Mendoza-Rodríguez M, Márquez-Rodríguez S, Maupomé G. Tooth brushing frequency in Mexican schoolchildren and associated socio-demographic, socioeconomic, and dental variables. Med Sci Monit 2014 ; 20:938-944.
-
28Silva RMA, Bezerra V, Medeiros DS. Experimentação de tabaco e fatores associados entre adolescentes da zona rural de Vitória da Conquista, BA, Brasil. Cien Saude Colet [periódico na Internet]. [acessado 2017 Out 22] No prelo. Disponível em: http://www.cienciaesaudecoletiva.com.br/artigos/experimentacao-de-tabaco-e-fatores-associados-entre-adolescentes-da-zona-rural-de-vitoria-da-conquista-ba-brasil/16171
» http://www.cienciaesaudecoletiva.com.br/artigos/experimentacao-de-tabaco-e-fatores-associados-entre-adolescentes-da-zona-rural-de-vitoria-da-conquista-ba-brasil/16171 -
29Santana KC, Teles N, Oliveira MHB, Medeiros DS. Direito à saúde: adolescentes quilombolas em comunidades rurais de Vitória da Conquista (BA). In: Oliveira MHB, Erthal RMC, Vianna MB, Matta JLJ, Vasconcellos LCF, Bonfatti RJ, organizadores. Direitos humanos e saúde: construindo caminhos, viabilizando rumos . Rio de Janeiro: Cebes; 2017 . v. 1. p. 53-68.
-
30Conselho Federal de Odontologia (CFO). Código de Ética Odontológica . 2012. [acessado 2017 Out 23]. Disponível em: http://cfo.org.br/wp-content/uploads/2009/09/codigo_etica.pdf
» http://cfo.org.br/wp-content/uploads/2009/09/codigo_etica.pdf -
31Gomes KO, Reis EA, Guimarães MDC, Cherchiglia ML. Utilização de serviços de saúde por população quilombola do Sudoeste da Bahia, Brasil . Cad Saude Publica [periódico na Internet]. 2013 Set [acessado 2017 Out 23]; 29(9):1829-1842. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102311X2013000900022&lng=en
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102311X2013000900022&lng=en -
32Santos NCN, Alves TDB, Freitas VS. A saúde bucal de adolescentes: aspectos de higiene, de cárie dentária e doença periodontal nas cidades de Recife, Pernambuco e Feira de Santana, Bahia. Cien Saude Colet [periódico na Internet]. 2007 [acessado 2017 Mar 04]; 12(5):1155-1166. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-81232007000500012
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1413-81232007000500012 -
33Freddo SL, Castro Aerts DRG, Abegg C, Davoglio R, Vieira PC, Monteiro L. Hábitos de higiene bucal e utilização de serviços odontológicos em escolares de uma cidade da Região Sul do Brasil. Cad Saude Publica [periódico na Internet]. 2008 Set [acessado 2017 Fev 20]; 24(9):1992- 2000. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2008000
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0102-311X2008000 -
34Brasil. Ministério da Saúde (MS). Diretrizes da Política Nacional de Saúde Bucal . [Internet]. 2004 [acessado 2017 Maio 18]. Disponível em: http://bvsms.saude.gov.br/bvs/publicacoes/politica_nacional_brasil_sorridente.pdf
» http://bvsms.saude.gov.br/bvs/publicacoes/politica_nacional_brasil_sorridente.pdf -
35Garbin CAS, Garbin AJI, Moimaz SDC, Gonçalves PE. A saúde na percepção do adolescente. Rev Physis [periódico na Internet]. 2009 [acessado 2017 Fev 08]; 19(1):227-238. Disponível em: http://www.scielo.br/scielo.php?pid=S0103-73312009000100012&script=sci_abstract&tlng=pt
» http://www.scielo.br/scielo.php?pid=S0103-73312009000100012&script=sci_abstract&tlng=pt -
36Avlund K, Pedersen PH, Morse DE, Viitanen M, Winbland B.Social relations as determinants of oral healter among persons over the age of 80 years. Rev. Comunnity Dentistry and Oral Epidemiology [periódico na Internet] 2003[acessado 2017 Maio 10]:32;454-462. Disponível em: http://onlinelibrary.wiley.com/doi/10.1046/j.1600-0528.2003.00115.x/abstract
» http://onlinelibrary.wiley.com/doi/10.1046/j.1600-0528.2003.00115.x/abstract -
37Dorri M, Sheiham A, Watt RG. Relationship between general hygiene behaviours and oral hygiene behaviours in Iranian adolescentes. Eur J Oral Sci 2009; 117(4):407-412.
-
38Antunes JLF, Narvai PC. Políticas de saúde bucal no Brasil e seu impacto sobre as desigualdades em saúde. Rev Saude Publica [periódico na Internet]. 2010 Abr [acessado 2017 Out 22]; 44(2): 360-365. Disponível em: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S003489102010000200018&lng=en
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S003489102010000200018&lng=en -
39Narvai PC, Frazão P. Saúde Bucal no Brasil: Muito Além do Céu da Boca . Rio de Janeiro: Editora Fiocruz; 2008 .
Publication Dates
-
Publication in this collection
Sept 2018
History
-
Received
31 Oct 2017 -
Reviewed
26 Feb 2018 -
Accepted
22 Apr 2018