Abstract
Pleural tuberculosis occurs in 30% of patients with tuberculosis, and the percentage of patients with tuberculosis pleural effusions is comparable to human immunodeficiency virus HIV-positive and HIV-negative individuals, although pleural tuberculosis is rare in HIV-positive patients with CD4+ counts < 200 cells/mm³. Pleural tuberculosis in HIV-positive patients is likely to happen in young patients, and is more frequent in intravenous drug abusers, with more acid-fast bacilli identifiable in pleural tissue. We report a rare case of pleural tuberculosis in a severely immunosuppressed HIVpositive patient, presented as two parasternum pleural-cutaneous fistula.
pleural tuberculosis; parasternum pleural-cutaneous fistula; severely immunosupressed HIV-positive patient
CASE REPORT
Parasternum pleural-cutaneous fistula in a severely immunosuppressed HIV-positive patient
André Gulinelli, MDI; Diogo Oliveira Toledo, MDII; Antonio Pereira Coelho-Neto, MDIII; Roseane Pôrto Medeiros, MDIV
IInternal Medicine Department, Conjunto Hospitalar do Mandaqui, São Paulo, SP; Intensive Care Unit, Hospital e Maternidade Brasil, Santo André, SP, Brazil
IIIntensive Care Unit, Hospital do Servidor Público Estadual, São Paulo, SP, Brazil
IIIDepartment of Pneumology, Conjunto Hospitalar do Mandaqui, São Paulo, SP, Brazil
IVInternal Medicine Department, Conjunto Hospitalar do Mandaqui, São Paulo, SP; Sexually-Transmitted Diseases - Centro de Referência e Treinamento DST/Aids, São Paulo, SP, Brazil
Correspondence Correspondence to: Dra. Roseane Pôrto Medeiros Rua 13 de Maio, 1.838, apto. 91 São Paulo - SP - Brazil CEP: 01327-002 Phone: 55 11 22815218 Fax: 55 11 32622031 E-mail: roseporto@uol. com.br
ABSTRACT
Pleural tuberculosis occurs in 30% of patients with tuberculosis, and the percentage of patients with tuberculosis pleural effusions is comparable to human immunodeficiency virus HIV-positive and HIV-negative individuals, although pleural tuberculosis is rare in HIV-positive patients with CD4+ counts < 200 cells/mm³. Pleural tuberculosis in HIV-positive patients is likely to happen in young patients, and is more frequent in intravenous drug abusers, with more acid-fast bacilli identifiable in pleural tissue. We report a rare case of pleural tuberculosis in a severely immunosuppressed HIVpositive patient, presented as two parasternum pleural-cutaneous fistula.
Keywords: pleural tuberculosis, parasternum pleural-cutaneous fistula, severely immunosupressed HIV-positive patient.
INTRODUCTION
Pleural tuberculosis occurs in 30% of patients with tuberculosis, and the percentage of patients with tuberculosis pleural effusions is comparable to human immunodeficiency virus HIV-positive and HIV-negative individuals, although pleural tuberculosis is rare in HIV-positive patients with CD4+ counts < 200 cells/mm3.1
HIV infection changes the clinical presentation of tuberculosis infection, favoring atypical radiographs and extrapulmonary involvement. In a previous study, pleural tuberculosis in HIV-positive patients was more common in younger patients, who were intravenous drug abusers, had significantly more acid-fast bacilli identifiable in pleural tissue and in sputum cultures.2
We examined a rare case of parasternum pleural-cutaneous fistula from pleural tuberculosis in a HIV-positive patient with a CD4+ count of 11 cells/mm³.
CASE REPORT
A 33-year-old male patient, from the city of São Paulo, was sent to the Clinical Emergency Department of the Conjunto Hospitalar do Mandaqui due to weight loss of 19 kilograms, asthenia, weakness, cough, daily vespertine fever, night sweating, abdominal pain, and a progressively worsening dyspnea in the previous three weeks. The patient was HIVpositive for about 14 years, was an intravenous drug user, had started the antiretroviral therapy five years before this admission, and had abandoned the antiretroviral therapy. His medical history included a pulmonary tuberculosis infection treated appropriately in 2004; he was a chronic hepatitis B virus carrier and had chronic asymptomatic hepatitis C virus.
At admission, the patient was thin and had a consumptive status, oral lesions compatible with Candida albicans infection, nonspecific abdominal pain and absent pulmonary murmurs at the inferior two-thirds of the left hemithorax. Diagnostic hypothesis were AIDS, bacterial pneumonia, pulmonary tuberculosis, or Pneumocystis jiroveci pneumonia with pleural effusion. Initial exams included hemogram, electrolytes, hepatic and canalicular enzymes, coagulation tests, serum albumin, sputum, and blood cultures, which resulted negative for infection.
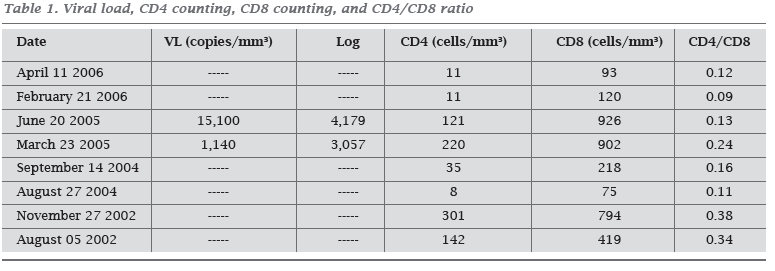
His HIV viral load had increased by approximately one log, and his CD4+ count had decreased substantially in the last two years before this admission, corresponding to transitory non-adherence to antiretroviral therapy (Table 1).
As the initial clinical symptoms were suggestive of pulmonary tuberculosis in a severely immunosuppressed HIV-positive patient, sputum samples have been collected, searching for acid-fast bacilli related to pulmonary infection, but in all samples, no bacteria or acid-fast bacilli has been identified.
A month after his admission, the patient presented a non tender mass of elastic consistency adhered to deep planes in the left parasternum region,below healthy skin,with no point of fluctuation or local warmth. Ultrasonographic evaluation revealed heterogeneous density containing liquid and dense material with septa, without clear cleavage plane in relation to the intercostal muscles, measuring 48 x 42 mm. Thoracic surgeons have performed puncture and aspiration of the mass, and the aspirate analysis revealed acid-fast bacilli in great amount (+++), with no other microbiologic elements suggestive of infection, except Mycobacterium tuberculosis. Patient received the following prescription: rifampicin, isoniazid, pyrazinamide, and ethambutol. Seven days after the first evaluation of the parasternum mass, another two thoracic masses had arisen in the intercostal spaces of left parasternum region, with irregular borders, liquid material, debris, and septations, measuring 40 x 24 mm and 25 x 13 mm, also aspirated. Both pleural aspirates revealed lymphocytic predominance, high levels of DHL (1,798 and 960 mg/dL), presence of high parasternum quantity of acid-fast bacilli (more than five bacilli per field) and negative bacterial cultures.
A thoracic CT scan has been done for a detailed analysis of the masses and their anatomic relation with the lungs, pleura, and subcutaneous thoracic tissue and revealed a clear dissemination of the masses from the left pleura to the muscular thoracic layers and to the subcutaneous tissue (Figures 1 and 2). We diagnosed pleural tuberculosis in a severely immunosupressed HIV-positive patient.
DISCUSSION
Pleural tuberculosis and HIV infection are strongly associated in HIV-infected patients. The pathogenesis of HIV-associated pleural tuberculosis involves direct bacterial invasion of pleural space, and the loss of immunity due to tuberculosis in HIV infection result from CD4+ Tcell depletion and reduction of antigen-specific cytokines responses, resulting in an uncontrolled mycobacterium replication, despite of the elevated levels of interferon-gamma and tumor necrosis factor-alpha.3
In this case report, among all clinical clues of extra pulmonary tuberculosis.4 the patient had an exudative pleural effusion, with lymphocytic predominance,negative bacterial cultures, and HIV infection. Moreover, the caseous-purulent aspect of the fistulized material, associated with the heterogenic density at the ultrasonografic evaluation, as reported elsewhere in the literature5 are typical evidence of pleural tuberculosis.
This patient presented four of the independent risk factors for pleural tuberculosis:6 history of liver disease (hepatitis B and C infection), Mycobacterium tuberculosis culture negative in sputum, chest pain, and presence of symptoms for less than 60 days. Additional suggestive symptoms were dyspnea and abdominal pain, more frequent in HIV-infected patients with pleural tuberculosis than with pulmonary tuberculosis.
Antituberculous therapy minimizes the morbimortality associated with tuberculosis infection and must be initiated empirically in most cases, once negative smear form acidfast bacillus, lack of granulomas in HIV-infected patients, and negative cultures to Mycobacterium tuberculosis are not rare in severely immunosuppressed HIV-infected patients with pleural tuberculosis.
Even with the empirical introduction of antituberculous therapy, the mortality rate in HIV-patients remains elevated.
Treatment with rifampicin, isoniazid, pyrazinamide, and ethambutol had been continued, and, after two weeks of treatment, one of the masses fistulized to the skin, exteriorizing a yellow, caseous-purulent material, rich in acid-fast bacilli. Despite introduction of the adequate treatment for pleural tuberculosis, the patient died after 32 days of treatment.
CONCLUSION
Severely immunosuppressed HIV-positive patients usually present pleural tuberculosis at a younger age than HIVnegative patients. Once their immune response is impaired, when CD4+ count is < 200 cells/mm³, they do not present granulomas and have higher quantity of acid-fast bacilli identified in both pleural effusion and pleural tissue. In this subgroup of patients, pleural tuberculosis indicates a severe immunosuppression caused by HIV infection and, despite of the prompt introduction of correct treatment against tuberculosis, the response may be too late and the patient may not survive.
Submitted on: 06/13/2009
Approved on: 12/16/2009
We declare no conflict of interest.
- 1. Ferrer J. Pleural tuberculosis. Eur Respir J 1997; 10:942-947.
- 2. Relkin F, Aranda CP, Garay SM, Smith R, Berkowitx KA, Rom WN. Pleural tuberculosis and HIV infection. Chest 1994; 105:1338-41.
- 3. Hodsdon WS, Luzze H, Hurst TJ et al. HIV-1-related pleural tuberculosis: elevated production of IFN-γ, but failure of immunity to Mycobacterium tuberculosis AIDS 2001; 15:467-75.
- 4. Golden MP, Vikram HR. Extrapulmonary tuberculosis: an overview. American Family Physician 2005; 72:1761-8.
- 5. Esquivel P, Palmieri O, Corti M. Tumoración de la pared anterior del tórax en un paciente con sida. Enferm Infecc Microbiol Clin 2002; 20(5):223-4.
- 6. Qiu L, Teeter LD, Liu Z, Ma X, Musser JM, Graviss EA. Diagnostic associations between pleural and pulmonary tuberculosis. Journal of Infection 2006; 53(4):377-86.
Publication Dates
-
Publication in this collection
18 June 2010 -
Date of issue
Apr 2010
History
-
Received
13 June 2009 -
Accepted
16 Dec 2009