Abstracts
The More Doctors Program was created in 2013 to address challenges that constrained the expansion and development of PC, mainly the insufficiency and maldistribution of physicians and the inadequate training profile related to the needs of the population. The program consists of three axes: emergency provision, improvement of infrastructure and changes in training. This paper performs documentary and literature review as well as analysis of official databases with the objective of evaluating the results achieved up to 2015 with regards to physicians supply. We identified important advances in the allocation of physicians with equity; in the expansion of PC coverage; in expanding access to basic health care for the population; its impact on health indicators; and the positive evaluation made by users, physicians and managers regarding the program. As a conclusion, challenges faced by the program to effectively achieve its objectives are pointed out.
Primary health care; Physicians shortage; More Doctors Program
O Programa Mais Médicos foi criado em 2013 para enfrentar desafios que condicionavam a expansão e o desenvolvimento da Atenção Básica (AB), sobretudo, a insuficiência e má distribuição de médicos e o perfil de formação inadequado às necessidades da população. O programa é composto por três eixos: provimento emergencial, qualificação da infraestrutura e mudança da formação. Neste artigo realizamos análise documental, análise de bancos de dados oficiais e revisão de literatura, com o objetivo de avaliar resultados do provimento de médicos alcançados até 2015. Identificamos avanços importantes na alocação dos médicos com equidade; na ampliação da cobertura da AB; na ampliação do acesso da população às ações de AB; no impacto nos indicadores de saúde; e na avaliação positiva que usuários, médicos e gestores têm do programa. Na conclusão, são apontados desafios enfrentados pelo programa para alcançar efetivamente seus objetivos.
Atenção primária à saúde; Escassez de médicos; Programa Mais Médicos
El Programa Más Médicos fue creado en 2013 para enfrentar desafíos que condicionaban la expansión y el desarrollo de la AB, principalmente la insuficiencia y la mala distribución de médicos y el perfil de formación inadecuado a las necesidades de la población. El programa se compone de tres ejes: provisión de emergencia, calificación de la infraestructura y cambio de la formación. En este artículo realizamos análisis documental, análisis de bancos de datos oficiales y revisión de literatura con el objetivo de evaluar los resultados de la provisión de médicos alcanzados hasta 2015. Identificamos avances importantes en la asignación de los médicos con equidad, en la ampliación de la cobertura de la AB, en la ampliación del acceso de la población a las acciones de atención básica, en el impacto en los indicadores de salud y en la evaluación positiva que usuarios, médicos y gestores realizan del programa. En la conclusión se señalan desafíos enfrentados por el programa para alcanzar efectivamente sus objetivos.
Atención básica de salud; Escasez de médicos; Programa Más Médicos
Introduction
The More Doctors Program (PMM) was created in July 2013 through a Provisional Measure, enacted into Law 12.87111. Presidência da República (BR). Lei nº 12.871, de 22 de outubro de 2013. Institui o Programa Mais Médicos, altera as Leis no 8.745, de 9 de dezembro de 1993, e no 6.932, de 7 de julho de 1981, e dá outras providências. Diário Oficial da União. 23 Out 2013. by the National Congress in October of the same year. It was added to a set of actions and initiatives in the background of the process in which the Federal Government assumed the task of formulating public policies to face some challenges that had been conditioning the expansion and the development of Primary Care (PC) in the country. Special challenges were the insufficiency and maldistribution of doctors and places of training and residency in medicine as well as the education profile, deemed to be inadequate to the needs of the population and the Brazilian National Health System (SUS).
Primary Care should be the preferred entry point for the SUS, as it should order equitably access to health care networks and be close to people ensuring universal quality and timely access. The National Policy of Primary Care (PNAB)22. Ministério da Saúde (BR). Portaria nº 2.488, de 21 de outubro de 2011. Aprova a Política Nacional de Atenção Básica, estabelecendo a revisão de diretrizes e normas para a organização da Atenção Básica, para a Estratégia Saúde da Família (ESF) e o Programa de Agentes Comunitários de Saúde (PACS). Diário Oficial da União. 24 Out 2011. proposes it as the priority way of organizing PC in Brazil through the Family Health Strategy ( (eSF), whose coverage stagnated in recent years, as will be shown later largely because of the difficulty of municipal managers to attract and retain doctors in Family Health teams33. Girardi SN, Carvalho CL, Araújo JF, Farah IM, Wau Der Maas L, Campos LAB. Índice de Escassez de Médicos no Brasil: estudo exploratório no âmbito da Atenção Primária. In: Pierantoni CR, Dal Poz MR, França T, organizadores. O Trabalho em Saúde: abordagens quantitativas e qualitativas. Rio de Janeiro: CEPESC/IMS/UERJ; 2011. p. 171-86..
The proportion of doctors per inhabitant in Brazil (1,8/1.000)44. OECD. Health at a Glance 2011: OECD Indicators [Internet]. Paris: OECD Publishing; 2011 [citado 20 Abr 2016]. Disponível em http://dx.doi.org/10.1787/health_glance-2011-en
http://dx.doi.org/10.1787/health_glance-...
was much smaller than the one of Argentina (3,9)55. Ministerio de Salud (AR). Médicos en Argentina Red Federal de Registros de Profesionales de la Salud [Internet]. Buenos Aires; 2014 [citado 20 Abr 2016]. Disponível em: http://www.msal.gob.ar/observatorio/images/stories/documentos_fuerza_trabajo/Adjuntos%20Fuerza%20de%20Trabajo%20FT/Informe_Medicos_2012_Argentina_04.08.2014.pdf.
http://www.msal.gob.ar/observatorio/imag...
; or of several countries that also guarantee universal health systems like Canada (2,4), United Kingdom (2,7), Spain (3,5) and Portugal (3,8); and lower than the average of the 33 countries of the Organization for Economic Cooperation and Development (3.1)44. OECD. Health at a Glance 2011: OECD Indicators [Internet]. Paris: OECD Publishing; 2011 [citado 20 Abr 2016]. Disponível em http://dx.doi.org/10.1787/health_glance-2011-en
http://dx.doi.org/10.1787/health_glance-...
.
In addition, these physicians were unevenly distributed in the national territory, in a way that the poorest and most vulnerable areas and populations were those that proportionally had fewer doctors. Aggravating the problem, from 2002 to 2012, the number of doctors trained in Brazil accounted for only 65% of all medical jobs created in the same period66. Poz MRD, Pierantoni CR, Girardi, S. Formação, mercado de trabalho e regulação da força de trabalho em saúde no Brasil. In: Fiocruz. A saúde no Brasil em 2030 – prospecção estratégica do sistema de saúde brasileiro: organização e gestão do sistema de saúde. Rio de Janeiro: Fiocruz/Ipea/Ministério da Saúde/Secretaria de Assuntos Estratégicos da Presidência da República, 2013. v. 3, p. 187-233..
Finally, it is well known the model of many countries that have greater demand than training of physicians and balance these deficits through the attraction of professionals trained in other countries.
In Brazil, the process of authorization of professional practice for doctors trained abroad, being them Brazilian or not was always protectionist and restrictive, only 1.9% of the physicians who worked in Brazil in 2012 were foreigners77. Scheffer M, Cassenotte A, Biancarelli A. Demografia Médica no Brasil: 2013. 256p cenários e indicadores de distribuição [Internet] . São Paulo: Conselho Federal de Medicina, [acesso em 20 Abr 2016]. Disponível em: http://www.cremesp.org.br/pdfs/DemografiaMedicaBrasilVol2.pdf.
http://www.cremesp.org.br/pdfs/Demografi...
, while in the US, for example, this number reached 22,4%88. Aaron Y, Chaudhry HJ, Thomas JV, Dugan M. A Census of actively licensed physicians in the United States. J Med Regulation, 2012; 99(2):11-24. and in the United Kingdom 37%99. General Medial Council. The state of medical education and practice in the UK, 2012 [Internet]. 2012 [citado 20 Abr 2016]. Disponível em: http://www.gmc-uk.org/The_state_of_medical_education_and_practice_in_the_UK_2012_0912.pdf_49843330.pdf
http://www.gmc-uk.org/The_state_of_medic...
.
The PMM is the largest initiative ever undertaken in the country and one of the largest in the world to address this set of problems. The program consists of three axes1010. Pinto HA, Sales MJT, Oliveira FP, Brizolara R, Figueiredo AM, Santos JT. O Programa Mais Médicos e o fortalecimento da Atenção Básica. Divulg Saúde Debate. 2014; 51:105-120.. The emergency provision axis is an immediate response to the problem of lack of coverage and access to the PC of an important part of the Brazilian population. The PMM selects professionals graduated in Brazil and abroad, both Brazilian and foreign, to work in the areas of greatest need and vulnerability and to develop quality health care according to PNAB guidelines1111. Oliveira FP, Vanni T, Pinto HA, Santos JTR, Figueiredo AM, Araujo SQ, et al. Mais Médicos: um Programa brasileiro em perspectiva internacional. Interface (Botucatu). 2015; 19(54):623-34..
The infrastructure axis, as stated in Article 30 of the PMM Law11. Presidência da República (BR). Lei nº 12.871, de 22 de outubro de 2013. Institui o Programa Mais Médicos, altera as Leis no 8.745, de 9 de dezembro de 1993, e no 6.932, de 7 de julho de 1981, e dá outras providências. Diário Oficial da União. 23 Out 2013., almost tripled the resources of the Requalification Program for Basic Health Units (UBS) that, since its inception in 20111212. Ministério da Saúde (BR). Portaria GM nº 2.206 de 14 de Setembro de 2011. Institui, no âmbito da Política Nacional de Atenção Básica, o Programa de Requalificação de Unidades Básicas de Saúde e o respectivo Componente Reforma. Diário Oficial da União. 19 Set 2011., increased its budget to 5.5 billion BRL for structure improvement with the aim of ameliorating the UBS environment for the patients/users, as well as the conditions of professional performance and the operation and expansion of the scope of service practices1313. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015.. In addition to increasing the target of reforms and expansions of existing UBS, the PMM forecasted the construction of new UBS through the Requalification Program jumping from just over one thousand to around 4,5 thousand UBS, for a total of 26 thousand constructions planned in five thousand municipalities1313. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015..
Finally, the third axis, Medical Training included short and long term measures such as to impact in quantitative and qualitative ways in the Brazilian medical training system. Among these measures: opening new seats in medical schools, both in undergraduate courses and residency programs along with redirecting their deployment in the country. Also it promoted shifts in the medical and specialist educational process in a way to better respond to the population and the SUS needs. The program had a planning goal of expanding the medical population until the proportion of physicians per thousand inhabitants could rise from the present 1.8 to 2.7 in 20261313. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015..
Among the axes described, the so-called “emergency provision” is what may be characterized as short term, and is able to generate positive results even within the relative short time of implementation of the program. It is worth analyzing the occurrence of these results and their relation with the objectives of the program.
Methodology
In this article, we synthesized results as they were declared officially as objectives of the axis emergency provision of the PMM11. Presidência da República (BR). Lei nº 12.871, de 22 de outubro de 2013. Institui o Programa Mais Médicos, altera as Leis no 8.745, de 9 de dezembro de 1993, e no 6.932, de 7 de julho de 1981, e dá outras providências. Diário Oficial da União. 23 Out 2013.,1010. Pinto HA, Sales MJT, Oliveira FP, Brizolara R, Figueiredo AM, Santos JT. O Programa Mais Médicos e o fortalecimento da Atenção Básica. Divulg Saúde Debate. 2014; 51:105-120.,1111. Oliveira FP, Vanni T, Pinto HA, Santos JTR, Figueiredo AM, Araujo SQ, et al. Mais Médicos: um Programa brasileiro em perspectiva internacional. Interface (Botucatu). 2015; 19(54):623-34.,1313. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015. analyzing official documents and including legislation, ordinances and related resolutions, as well as reports and articles that deal with the topic. Based on these results, we sought to identify evidence of changes produced in indicators that could describe the program using reference and methodological guidelines from the field of policy analysis studies1414. Côrtes SV. Contribuições teóricas e à pesquisa empírica da Sociologia às políticas públicas. Rev Bras Sociol. 2013; 1(1):35-56.
15. Ramos M. Aspectos conceituais e metodológicos da avaliação de políticas e programas sociais. Planej Polít Públicas. 2009; 32:95-114.-1616. Costa G, Dagnino R, organizadores. Gestão estratégica de políticas públicas. Rio de Janeiro: Editora T+8; 2008..
The search for evidence was done, both directly, through the analysis of secondary data in the databases of the Departments of Informatics of SUS (DATASUS), Primary Care (DAB), Monitoring and Evaluation of SUS (DEMAS) and Planning and Regulation of the Provision of Health Professionals (DEPREPS), and also performing reviews on the literature on the program published in articles, book chapters and research reports available. The period of analysis was from the beginning of the PMM until the end of 2015.
Results and Discussion
The emergency provision axis
The PMM provides physicians to work in PC in the most vulnerable and greater needs areas and provides its improvement through several teaching-service integration activities articulated for a period of up to three years that can be extended for up to three more years. It followed the experience of other countries and the recommendations of the World Health Organization (WHO). WHO states that it is necessary to combine the strategies of provision and retention of health professionals1111. Oliveira FP, Vanni T, Pinto HA, Santos JTR, Figueiredo AM, Araujo SQ, et al. Mais Médicos: um Programa brasileiro em perspectiva internacional. Interface (Botucatu). 2015; 19(54):623-34., and for that end the PMM provided: face-to-face and distance educational activities; training grants funded by the federal government; incentives for housing and food paid for by the municipal managers; distance clinical support; and interaction platforms through communities of virtual practices.
The teaching-service integration activities use the practice of the team as the raw material of the pedagogical process. All physicians attend the sensu lato specialization offered by a Public Higher Education Institution (IES) through the Open University of SUS (UNASUS). In addition, the permanent education of the professionals is carried out by supervisors and pedagogical tutors linked to educational institutions of the educational system or SUS. Doctors have access to the Evidence Based Health Portal of the Ministry of Health (MS) and Telehealth Brazil Networks. Finally, they develop extension activities whose intervention projects are built together with the teams.
The selection of professionals in the program takes place in stages. The first is the definition of the vacancies available, which occurs through a previous process of adhesion of the municipalities that indicate which FSs need to complete vacancies and how many will be implemented. For the occupation of the same, carried out by means of public calls for doctors, there is an order of priority defined in Law: First, doctors with registration in Brazil; second, Brazilian physicians registered only abroad; then foreign doctors, also registered only abroad; and, finally, physicians who collectively participate through the international cooperation that is being carried out between the Pan American Health Organization (PAHO) and the Ministry of Public Health of Cuba.
By December 2015, just over two years since the arrival of the first doctors in the municipalities in August 2013, it is possible to identify progress in the indicators related to results that were declared objectives of the PMM: 1- service 100% of the demand requested by municipalities, according to the rules of the program; 2 - allocation of doctors in the national territory with equity; 3 - broadening the coverage of PC in general and, in particular, the ESF; 4 - increase of population access to PC actions; 5- impact on health indicators; and 6- significant approval by users served, doctors and municipal managers. Next, evidence is systematized on each of these topics.
Provision with Equity
By the end of 2015, 73% of the municipalities in Brazil, in all states, as well as the Federal District, participated in the PMM. The program was in all the Indigenous Special Health Districts (DSEI) of the country where for the first time all the country had doctors to serve its population. Adherence to the program is voluntary and the request of doctors made by the municipalities is analyzed according to a combination of criteria: need, available supply and infrastructure1717. Resolução nº 01 da Coordenação Nacional do Projeto Mais Médicos para o Brasil, de 02 de outubro de 2015. Metodologia de autorização da quantidade de vagas para cada município do Projeto Mais Médicos para o Brasil. Diário Oficial da União. 06 Out 2015..
The need, in the period from 2013 to 2015, was calculated based on the amount eSF’s without physicians added to those needed to cover the entire population, giving a higher priority to the SUS population coverage, those, not covered by private supplementary health schemes. For this calculation the population coverage that the municipality has was estimated through consultation with the National Register of Health Establishments (CNES), subtracting that quantitative from the total population of the municipality. In this way, the amount of eSF still required for the uncovered population is obtained. Finally, it is evaluated if the structure of the existing UBS in the municipality suffices for the allocation of these professionals1717. Resolução nº 01 da Coordenação Nacional do Projeto Mais Médicos para o Brasil, de 02 de outubro de 2015. Metodologia de autorização da quantidade de vagas para cada município do Projeto Mais Médicos para o Brasil. Diário Oficial da União. 06 Out 2015..
The priority for allocation was based on criteria using both the vulnerability of the population and specific population groups and of the municipalities themselves1717. Resolução nº 01 da Coordenação Nacional do Projeto Mais Médicos para o Brasil, de 02 de outubro de 2015. Metodologia de autorização da quantidade de vagas para cada município do Projeto Mais Médicos para o Brasil. Diário Oficial da União. 06 Out 2015.
18. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Edital nº 39, de 08 de junho de 2013. Adesão de Médicos ao Projeto Mais Médicos para o Brasil. Diário Oficial da União. 08 Jun 2013.-1919. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Edital nº 02, de 15 de janeiro de 2015. Adesão de médicos aos programas de provisão de médicos do Ministério da Saúde – Projeto Mais Médicos para o Brasil e Programa de Valorização do Profissional da Atenção Básica. Diário Oficial da União. 15 Jan 2015.. In this way, the municipalities were prioritized according to their percentages of population in extreme poverty; low human development index (HDI); locations in poor regions such as the Ribeira and Jequitinhonha Valleys, the Semiarid; besides the criteria used by the DAB for the transfer of the so-called Fixed Basic Attention Floor2020. Ministério da Saúde (BR). Portaria nº 1.602, de 9 de julho de 2011. Define o valor mínimo da parte fixa do Piso de Atenção Básica (PAB), para efeito do cálculo do montante de recursos a ser transferido do Fundo Nacional de Saúde aos Fundos de Saúde dos Municípios e do Distrito Federal, e divulga os valores anuais e mensais da parte fixa do PAB. Diário Oficial da União. 11 Jul 2011.. In addition to these criteria, the periphery of large cities and indigenous population groups, rural settlers and quilombolas were prioritized within the municipalities.
Thus, by the end of 2015, the PMM had met 100% of the demand made by the municipal managers, recognized by the program according to the parameters highlighted above1313. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015..
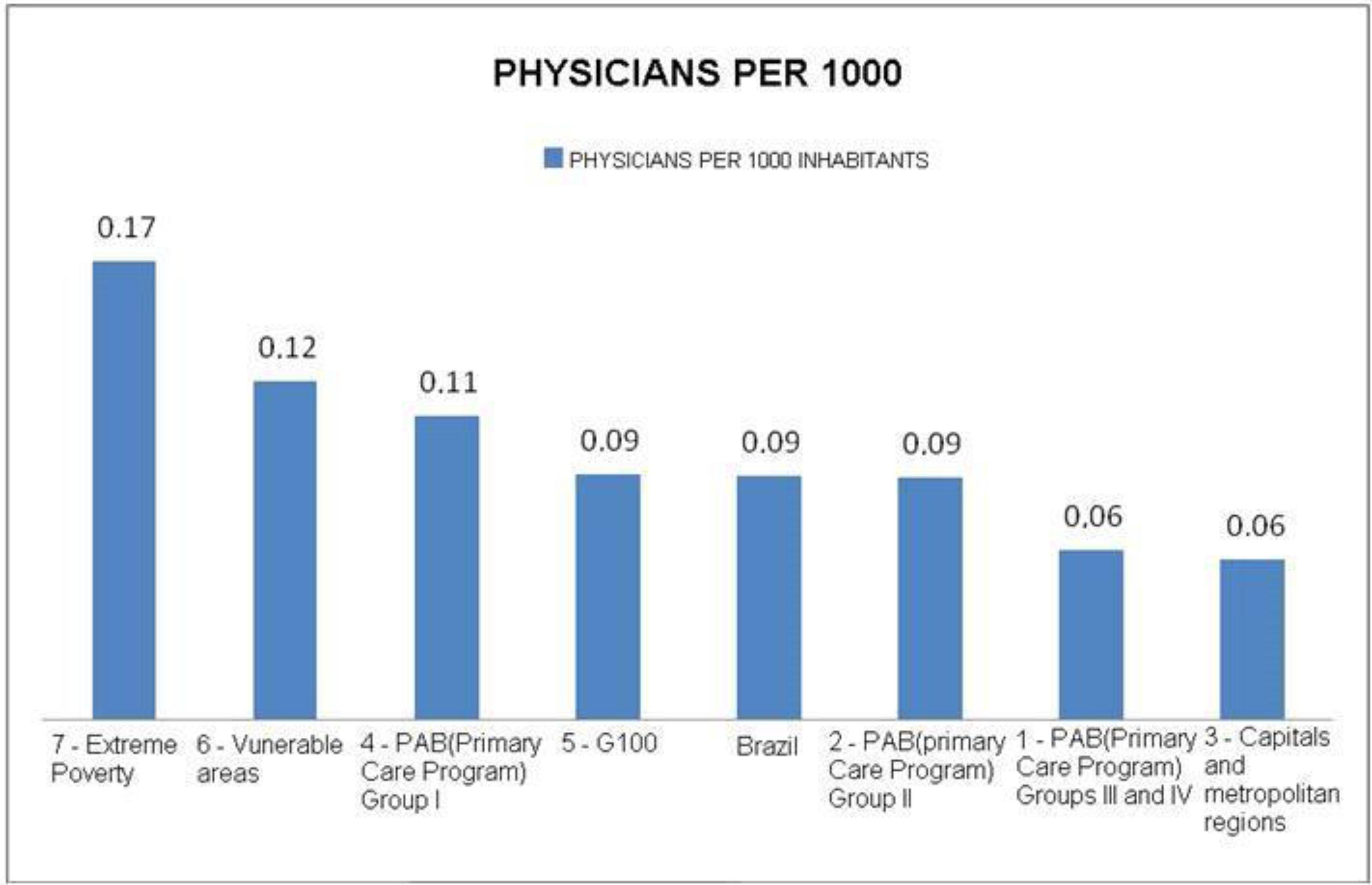
We observed that the adopted criteria had a strong equity component in the distribution of physicians considering the groups of municipalities1818. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Edital nº 39, de 08 de junho de 2013. Adesão de Médicos ao Projeto Mais Médicos para o Brasil. Diário Oficial da União. 08 Jun 2013. with which the program works, so that the proportion of PMM doctors in extremely poor municipalities was almost three times higher than in richer capitals and municipalities, according to chart 1.
Number of physicians per 1000 inhabitants per group of distribution municipalities defined by the More Doctors Program, considering only physicians registered with the program.
A similar result is found when analyzing by macro-regions, with evident priority for North and Northeast according to Chart 2.
Number of physicians per 1000 inhabitants per macro-region, considering only physicians registered with the program.
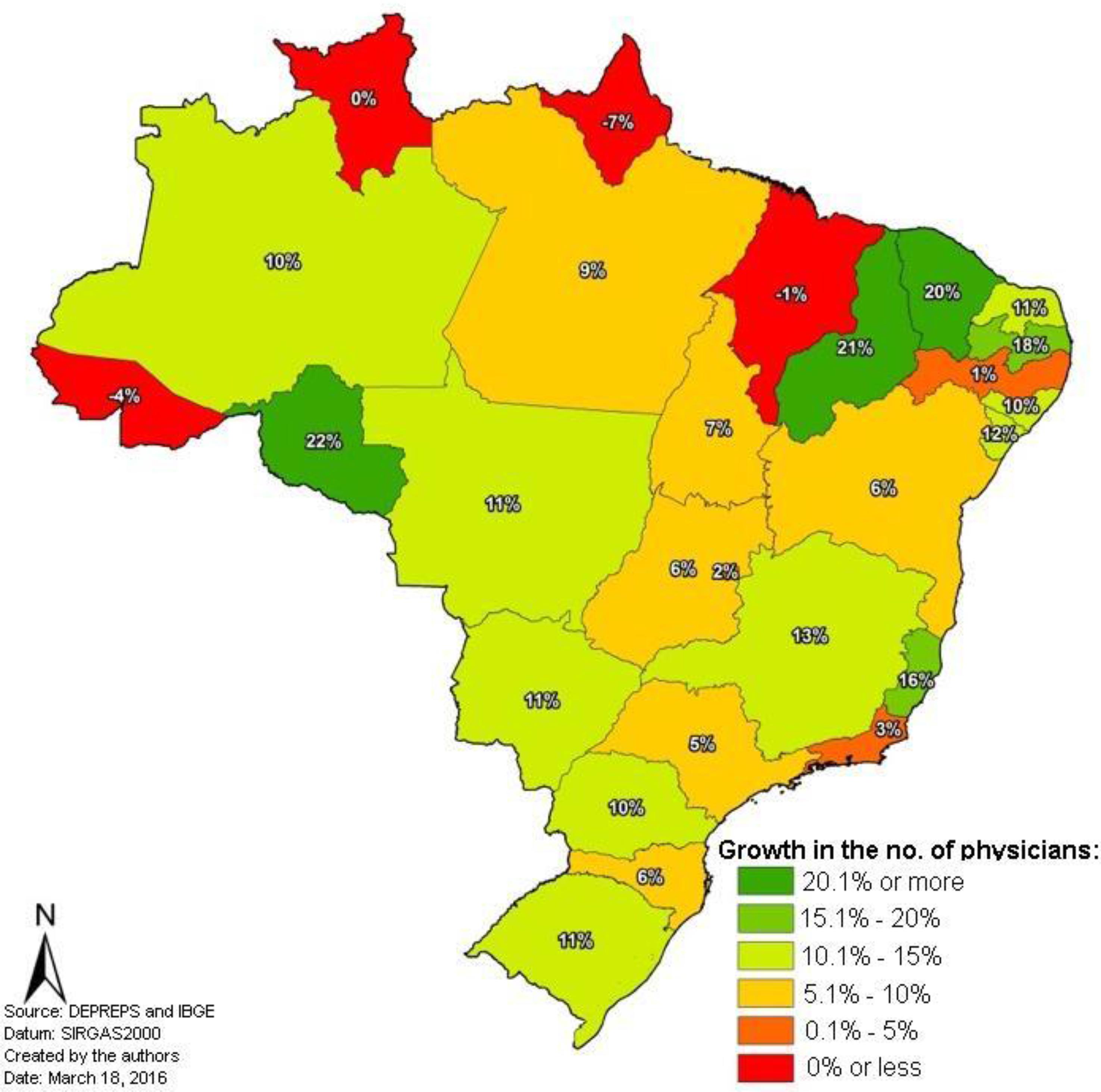
When we analyze the growth of the absolute and proportional number of doctors in Brazil and in each unit of the federation, we find that in 2012 Brazil had 388,015 doctors and by the end of 2015 this number reached 429,559, a growth of 10.7%. But most importantly, without PMM, 12 states would have had a growth rate of less than 10%; in four of them, there would have been no growth, or there would have been a reduction in the number of doctors according to map 1.
Percentage of growth in the number of physicians per federative unit without the MDP, between 2012 and 2015.
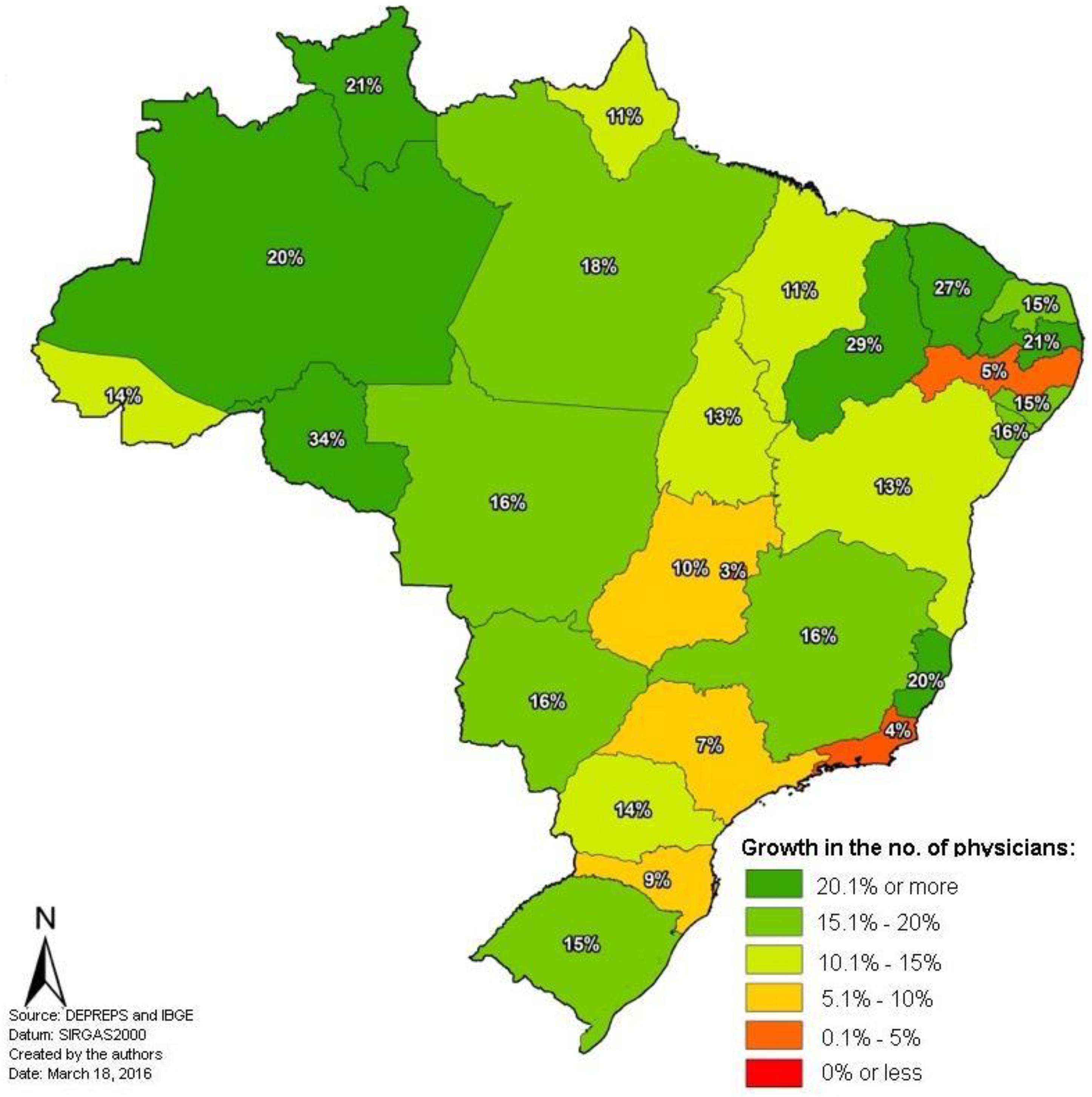
With the PMM, they all showed growth and only in five states this growth was less than 10% (map 2). In addition, all states in the North and Northeast, with the exception of Pernambuco, grew more than 15%.
Percentage in the growth in number of physicians per federative unit, with the MDP, between 2012 and 2015.
Expansion of coverage of Primary Care and ESF
There is consistent evidence of increased PC coverage since PMM implementation. To properly observe this phenomenon, it is necessary to take into account that the regulations of the program required physicians to integrate eSF or other teams provided for in PC policy. The eSFs, in turn, may be newly created, or existing teams without doctors, or even teams in which the presence of doctors was insufficient (high turnover of professionals throughout the year, irregular fulfillment of the workload, etc.).
Therefore, it is necessary to combine indicators that consider both the expansion of the ESF and PC. In effect, we selected: increase in the number of doctors (hours) in PC, increase in PC and ESF coverage, increase in the number of eSF and in the number of municipalities with eSF.
We chose to work with the medical hour indicator known in the international literature as Full Time Equivalent, and not with the absolute number of doctors, because it would not be appropriate to count in the same way a doctor with a workload of 12 hours a week with other with 40 hours. The group of doctors assigned for PC was analyzed following this criterion, and using the CNES data.
Brazilian municipalities were categorized in: municipalities that joined the program and municipalities that did not adhere. Chart 3 uses 2011 as the base year and shows this growth from 2012 to 2015.
Percentage of growth in the annual mean number of physicians – FTE – in primary care establishments, per situation of adherence to the More Doctors Program, between 2012 and 2015.
We observed that, in 2012 and 2013, municipalities that did not join the PMM - about 30% of the municipalities in Brazil - showed a greater increase in the number of doctors in PC than those who joined. In 2012, this growth was more than double that in the rest of municipalities. In the year 2013, when the Program was created, its effect was already perceived, but growth in the "non-adherents" was slightly higher. One of the reasons for the non-adherence of these municipalities may be the fact that they were easier to attract and retain doctors by their own means.
With the creation of the PMM, this growth had a reversal in the years 2014 and 2015: municipalities that previously had the most difficulty attracting and retaining doctors, the so-defined "adherents", grew by 10.8%, while the "non-adherents" grew only 1.8%., a six-fold increase. It is important to note that the national average follows the line of "adherents", precisely because the medical hours added in the PC in the participating municipalities is much higher than those added in the non-participating municipalities.
Another important data refers to the expansion of PC and ESF coverage. Here it is important to clarify the method of calculation. The DAB uses as a coverage parameter the average number of people enrolled in the Basic Attention Information System (SIAB) by eSF. In the year of definition of the parameter, 2006, the verified average was 3,450 people2121. Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Saúde da família no Brasil: uma análise de indicadores selecionados: 1998-2004. Brasília: Ministério da Saúde; 2006.. However, when applying municipality to municipality this parameter for national coverage, the algorithm used by the DAB ends up making the average a ceiling, as shown below.
A municipality “A” that has ten thousand inhabitants and two teams would register coverage of 6,900 people. A municipality B that also has ten thousand inhabitants and four teams would note, obviously, maximum coverage of 10,000 people. Thus, these six teams would cover an average of 2,817 people and not 3,450, configuring an algorithm problem.
With the reduction of the use of the SIAB from 2007 onwards - when CNES became the most important system to be updated to receive the PC financing - And with the replacement of the SIAB by the eSUS / SISAB system from 2013 onwards, the sub-registration will prevent a real count of people registered by eSF to update the actual average. Thus, until a real count is made from the data of the new information system, SISAB, the most real coverage parameter is the one that is actually verified.
Thus, for the calculations performed in this article, we constructed an algorithm that effectively applies the parameter of 3,450 people per eSF. It is important to note that this choice changes only the number of people that are theoretically covered. If at all points of the curve we have the application of the same parameter, the increase ratio is indifferent to the coverage parameter used. For people covered by non-ESF services, we use the parameter adopted by DEMAS for the Public Action Organizational Contracts, which equates 60 hours of medical time (general practitioner, family physician, clinician, gynecologist and pediatrician) in a team of PC not eSF to the coverage provided by a eSF.
As a result, we found that Brazil presented a stagnation of PC coverage growth from 2008 to 2013, from 75.8% and reaching only 80.6% (chart 4). All regions presented similar behavior, with the exception of the North region that presented, in the same period, a reduction of coverage from 72.9% to 66.2%.
From 2013, the year of creation of the PMM, in 2015, coverage in Brazil increased from 80.6% to 88.8%, which represents an average annual growth four times higher than the average growth of the previous five years. It is interesting to note also that the North region, which had the worst coverage and was the only one that had reduced it in the last period, was the one that had the greatest coverage increase after the PMM: 13.7%, practically equaling the full coverage of the Midwest and Southeast regions.
Similarly, the expansion of ESF coverage was stagnant, particularly from 2010 to 2013 (chart 5). In the last two years, with the effect of the PMM, the coverage of the ESF increased by 9%, while in the previous five years the growth was 7%. The average annual growth of the last two years was four times higher than the growth of the three years prior to the program's creation.
Estimated population covered by primary care, Family Health Strategy, and More Doctors in Brazil between 2008 and 2014.
In December 2010 the number of eSF in the country was 31,660 in 5,294 municipalities. In June 2013 (the month prior to the creation of the PMM) these figures were, respectively, 33,998 and 5,298 municipalities. That is, in a period of approximately two and a half years, 2,388 teams were deployed and only 4 other municipalities began to have eSF. As early as December 2015, approximately two and a half years after the implementation of the program, these figures were 40,162 eSF and 5,463 municipalities. An increase of 6,164 teams, two and a half times the expansion of the previous period, and 165 municipalities opted to implement eSF, forty times the result of the previous period.
Considering just teams, being them ESF and others with PMM doctors, the population coverage provided by them reaches 63 million people (31% of the population).
The difference between the coverage of teams with PMM physicians and the increase in PC and ESF coverage is precisely due to the fact that approximately one-third of the program's physicians have integrated new ESFs and the other two thirds have integrated ESFs already existed but did not have doctors or their presence was unsatisfactory, in addition to having, of course, a small number of doctors in non-ESF teams1313. Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015..
Expansion of the population's access to Primary Care
The expansion of the population's access to PC, in addition to the expansion of coverage indicated in the previous session, can both be seen in the significant increases in the number of consultations in the municipalities participating in the program and in the surveys conducted with managers and users.
In 2015, the Observatory Network of the More Doctors Program (ROPMM) was created, composed of researchers from teaching and research institutions from all regions of the country in the form of integrated multicenter studies. The report of the first phase of the ROPMM2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
identifies three findings that point to the expansion and qualification of access: the increase of the scope of practices (variety of actions and services offered) developed in the teams and UBS with program physicians; increased provision of collective procedures and home visits and stabilization of scheduled consultations with specific groups; And the increase in the number of consultations in Brazil, especially in the municipalities participating in the program2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
The increase in scope was identified from the analysis of the databases of the first and second cycle evaluations of the National Program for Improving Access and Quality in Primary Care (PMAQ), mainly in actions such as nail extraction and wound suturing. This is an important finding because it indicates the increase of the capacity to solve in the UBS, i.e. near the citizen's home, situations that would require emergency care or even hospital care, usually far away from the users2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
In addition, analyzing in a combined way the data from the SIAB, eSUS and also from the Outpatient Information System (SIA), according to established validation protocol that considers SIA for UBS without eSF and one of these systems for each eSF2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
, there was a significant increase in the number of collective actions and home visits. A significant reduction in the number of monthly consultations for users with diabetes and hypertension was also identified, indicating a greater programming of actions by the team and improvement of users' adherence to the offer of actions2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
Regarding the total number of consultations in the ESF, also calculated from the validation protocol that combines eSUS, SIAB and SIA for each eSF, the research identified a 29% increase in the number of medical consultations when compared to the months of January 2013 and January 2015. In the municipalities participating in the PMM, this growth was 33% and in the other municipalities only 15%. The increase was attributed to the implantation of new ESFs, to the fact that several ESFs that already existed had doctors attending on a regular basis, and to the finding that the eSFs of PMM offered the population more same-day medical visits2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
Reinforcing these findings, a case study coordinated by PAHO in the city of Curitiba, which, in addition to analyzing the databases of the national and municipal information systems, interviewed managers and professionals, finding that PMM physicians occupied vacancies in the most needy UBSs and Increased the number of daily consultations2323. OPAS. Implementação do Programa “Mais Médicos” em Curitiba. Experiências inovadoras e lições aprendidas [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
Another research that reinforces the same findings was carried out by the Federal University of Minas Gerais and the Institute of Social, Political and Economic Research of Pernambuco (UFMG / IPESPE)(h[1]) that interviewed users, managers and doctors participating in the program. 699 municipalities were visited. The samples for interviews totaled 14,179 users, 391 physicians and 227 managers, the latter could not necessarily be more than one in each municipality.
With regard to these managers, it was identified that among the five main factors related to the positive evaluation they make of the impact of the program, three are related to the increase of access, namely: To permanently have physicians in the UBS that effectively fulfill the defined workload; expanding access to the population; and the increase in consultations24.
Through the interviews with the users, it was identified that the two most frequent spontaneous mentions about the positive aspects of the care of the PMM physicians were precisely the increase in the number of consultations and other medical care and the fact that the unit began to have medical care every day24.
Impact on health indicators
Regarding the impact on health indicators, it is important to be clear that less than three years of implementation of this kind of intervention is insufficient to capture the effects on indicators constructed from SUS information system data. However, the ROPMM report2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
was able to identify a reduction in hospital admissions due to PC sensitive causes, analyzed from the Hospital Information System, both in Brazil and in the regions and in municipalities.
Considering that the hospitalization rate due to conditions sensitive to PC has been declining in Brazil following a permanent trend, the research showed that in the PMM participating municipalities this reduction was 4% more pronounced than in the other municipalities, comparing the hospitalizations of December 2013 And December, 2014.
Another important finding was the proportional relationship between population coverage with eSF with PMM physicians and the reduction of PC sensitive hospitalizations: in municipalities with population coverage between 17% and 36%, the reduction was 5.8% higher than in the others Municipalities, while in those with population coverage greater than 36% the reduction in the same period reached 8.9%2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
. The research stated that those were effects both from the effective increase in coverage, securing the access to people previously lacking access, regarding the resolution capacity of PC2222. Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
Also reinforcing this paper, the study case of Curitiba, using the electronic medical records and the local computerized system as a database, showed good resolubility of PMM physicians who presented hospital admission rates and referral to a care unit, respectively 1.4 per thousand consultations and four per thousand, while resident physicians presented respectively 2.3 per thousand and six per thousand and the other physicians 1.5 per thousand and six per thousand, respectively2323. OPAS. Implementação do Programa “Mais Médicos” em Curitiba. Experiências inovadoras e lições aprendidas [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
http://www.otics.org/estacoes-de-observa...
.
Users, managers and doctors assessment
The research of UFMG/IPESPE Identified that 95% of users were satisfied or very satisfied with the PMM physician's performance. Among the reasons for this extremely positive evaluation, 85% said that the quality of care improved, 87% that the doctor is more attentive and 82% that the consultation now solves their health problems better. The average rating the users gave the PMM was nine for a maximum of ten.
When asked about communication difficulties, 87% said they had no difficulties and only 3% said they were important. These numbers compared in the same survey with Brazilian physicians not participating in the program, a control group, resulted in 95% and 2%, respectively.
The research with managers showed that before the PMM they gave the average grade of 6.6 for the health care of the population and, after implementing the Program in the municipality, they gave the grade 8.7. The reasons pointed out in the research for this improvement in the evaluation are those related to the improvement of access, already mentioned in this article, together with the improvement of the quality of care and the proximity and good relationship between the Program's doctors and the patients24.
The same survey interviewed Brazilian and foreign doctors of the PMM, and found the following results: 100% said they were well received by the community; 98% would refer the Program to a friend; the mean score attributed to the relationship with the remainder of the eSF was 9.6; The grade given to program supervision was 9.0; and the evaluation of the Program as a whole received an average grade of 9.1 in a maximum of ten. Regarding the structure of the UBS, in general, considering physical structure, equipment, medications, immunobiology and working conditions; for 65% of the physicians the structure was good or excellent. For 8%, it was bad or very bad and for others it was regular24.
This positive evaluation that the participating physicians gave to the Program, the recommendation they make to their colleagues and the fact of incorporating in 2015 the Program of Appreciation of Basic Care (PROVAB) and its benefits - such as the additional 10% in the score obtained in the residence contest for those who, after one year do the same – those are facts that help to explain the significant change in Brazilian physicians' adherence to the Program.
At the end of 2013, when the Program was created, of the 3,678 vacancies filled in it, physicians registered in Brazil occupied only 22%. However, the year 2015 experienced records levels of applications from Brazilian doctors already licensed in Brazil, and the proportion reached more than ten candidates per vacancy offered, and in the three calls-for-applicants made in that year, all the vacancies were filled by Brazilian doctors: The first call of the year needed to call also Brazilian doctors with foreign registration, and in the second and third all vacancies were filled with doctors with registration in Brazil. Thus, it was not necessary to launch an international call notice for foreign doctors in 2015 and to expand cooperation with PAHO. The percentage of doctors registered in Brazil at the end of 2015 reached 29% of the more than 18 thousand physicians, according to DATASUS data.
This result is important for several reasons, among which we highlight four: it reinforces the findings that point to the importance of the approval of the Program by the Brazilian physicians who work in it and who recommend it; it shows an increasing interest in participating in the PMM; it significantly increases the number of doctors in Brazil who develop a role in the ESF and are trained for it, an important factor for the quality of professional practice, whether in PC or another area of activity; and lastly, it gives sustainability to the PMM that in this way becomes less dependent on foreign professionals.
Conclusion
The available evidence allows us to affirm that the PMM in less than three years of implementation has achieved a set of results related to the objectives of the program, such as: meeting the demand of physicians made in 2013 and, in later years, the demand of the Municipal managers to expand eSF and complete existing ones; allocate physicians in areas of greatest need improving its equitable distribution; expand PC and ESF coverage at volumes and speed significantly higher than in previous years; expand the population's access to PC actions; increase the number of consultations and diversify the scope of PC procedures; Increase the rate of reduction of PC-sensitive hospitalizations; be well evaluated by users, doctors and managers; and constitute an important alternative for Brazilian doctors.
Even with the aforementioned detailed success of the provision axis, it is worth highlighting some challenges. Brazilian doctors still choose and act in a much smaller number of municipalities in relation to the places where Brazilians trained abroad and, especially foreigners are willing to act. An example of this point is that all DSEIs now have complete teams for the first time, thanks to foreign doctors. In addition, the average length of stay and the dropout rate of Brazilian physicians in the program are higher than those of foreign doctors. These two factors still point to the need for international calls and cooperation with PAHO for quite a long time.
Another issue to be highlighted is that from 2016 on, an important action of PMM related to the training axis, namely the expansion of the Family and Community Medicine Residency with ways to universalize access to all trained doctors, will reinforce the provision axis by improving the access and quality in PC to the health of the population. In fact, if the expansion of the residence happens to be satisfactory, it is possible that the provision axis already reaches levels close to the ceiling and, from that moment it will be directed progressively to smaller municipalities and regions, that are more distant and with greater difficulties of attracting professionals.
Finally, it is important to remember that is basic to achieve the objective of the training axis in order to have physicians in the right quantity and with the training adequate to the needs of our population. Brazil needs to increase the number of doctors and improve the quality of its training in order to be able to respond to the motives that led to the creation of the PMM and to enable the country to move more and more consistently towards the right to health through a public system, that is free, universal, integral, equitable and with popular participation.
Referências
-
1Presidência da República (BR). Lei nº 12.871, de 22 de outubro de 2013. Institui o Programa Mais Médicos, altera as Leis no 8.745, de 9 de dezembro de 1993, e no 6.932, de 7 de julho de 1981, e dá outras providências. Diário Oficial da União. 23 Out 2013.
-
2Ministério da Saúde (BR). Portaria nº 2.488, de 21 de outubro de 2011. Aprova a Política Nacional de Atenção Básica, estabelecendo a revisão de diretrizes e normas para a organização da Atenção Básica, para a Estratégia Saúde da Família (ESF) e o Programa de Agentes Comunitários de Saúde (PACS). Diário Oficial da União. 24 Out 2011.
-
3Girardi SN, Carvalho CL, Araújo JF, Farah IM, Wau Der Maas L, Campos LAB. Índice de Escassez de Médicos no Brasil: estudo exploratório no âmbito da Atenção Primária. In: Pierantoni CR, Dal Poz MR, França T, organizadores. O Trabalho em Saúde: abordagens quantitativas e qualitativas. Rio de Janeiro: CEPESC/IMS/UERJ; 2011. p. 171-86.
-
4OECD. Health at a Glance 2011: OECD Indicators [Internet]. Paris: OECD Publishing; 2011 [citado 20 Abr 2016]. Disponível em http://dx.doi.org/10.1787/health_glance-2011-en
» http://dx.doi.org/10.1787/health_glance-2011-en -
5Ministerio de Salud (AR). Médicos en Argentina Red Federal de Registros de Profesionales de la Salud [Internet]. Buenos Aires; 2014 [citado 20 Abr 2016]. Disponível em: http://www.msal.gob.ar/observatorio/images/stories/documentos_fuerza_trabajo/Adjuntos%20Fuerza%20de%20Trabajo%20FT/Informe_Medicos_2012_Argentina_04.08.2014.pdf
» http://www.msal.gob.ar/observatorio/images/stories/documentos_fuerza_trabajo/Adjuntos%20Fuerza%20de%20Trabajo%20FT/Informe_Medicos_2012_Argentina_04.08.2014.pdf -
6Poz MRD, Pierantoni CR, Girardi, S. Formação, mercado de trabalho e regulação da força de trabalho em saúde no Brasil. In: Fiocruz. A saúde no Brasil em 2030 – prospecção estratégica do sistema de saúde brasileiro: organização e gestão do sistema de saúde. Rio de Janeiro: Fiocruz/Ipea/Ministério da Saúde/Secretaria de Assuntos Estratégicos da Presidência da República, 2013. v. 3, p. 187-233.
-
7Scheffer M, Cassenotte A, Biancarelli A. Demografia Médica no Brasil: 2013. 256p cenários e indicadores de distribuição [Internet] . São Paulo: Conselho Federal de Medicina, [acesso em 20 Abr 2016]. Disponível em: http://www.cremesp.org.br/pdfs/DemografiaMedicaBrasilVol2.pdf
» http://www.cremesp.org.br/pdfs/DemografiaMedicaBrasilVol2.pdf -
8Aaron Y, Chaudhry HJ, Thomas JV, Dugan M. A Census of actively licensed physicians in the United States. J Med Regulation, 2012; 99(2):11-24.
-
9General Medial Council. The state of medical education and practice in the UK, 2012 [Internet]. 2012 [citado 20 Abr 2016]. Disponível em: http://www.gmc-uk.org/The_state_of_medical_education_and_practice_in_the_UK_2012_0912.pdf_49843330.pdf
» http://www.gmc-uk.org/The_state_of_medical_education_and_practice_in_the_UK_2012_0912.pdf_49843330.pdf -
10Pinto HA, Sales MJT, Oliveira FP, Brizolara R, Figueiredo AM, Santos JT. O Programa Mais Médicos e o fortalecimento da Atenção Básica. Divulg Saúde Debate. 2014; 51:105-120.
-
11Oliveira FP, Vanni T, Pinto HA, Santos JTR, Figueiredo AM, Araujo SQ, et al. Mais Médicos: um Programa brasileiro em perspectiva internacional. Interface (Botucatu). 2015; 19(54):623-34.
-
12Ministério da Saúde (BR). Portaria GM nº 2.206 de 14 de Setembro de 2011. Institui, no âmbito da Política Nacional de Atenção Básica, o Programa de Requalificação de Unidades Básicas de Saúde e o respectivo Componente Reforma. Diário Oficial da União. 19 Set 2011.
-
13Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Programa mais médicos – dois anos: mais saúde para os brasileiros. Brasília: Ministério da Saúde; 2015.
-
14Côrtes SV. Contribuições teóricas e à pesquisa empírica da Sociologia às políticas públicas. Rev Bras Sociol. 2013; 1(1):35-56.
-
15Ramos M. Aspectos conceituais e metodológicos da avaliação de políticas e programas sociais. Planej Polít Públicas. 2009; 32:95-114.
-
16Costa G, Dagnino R, organizadores. Gestão estratégica de políticas públicas. Rio de Janeiro: Editora T+8; 2008.
-
17Resolução nº 01 da Coordenação Nacional do Projeto Mais Médicos para o Brasil, de 02 de outubro de 2015. Metodologia de autorização da quantidade de vagas para cada município do Projeto Mais Médicos para o Brasil. Diário Oficial da União. 06 Out 2015.
-
18Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Edital nº 39, de 08 de junho de 2013. Adesão de Médicos ao Projeto Mais Médicos para o Brasil. Diário Oficial da União. 08 Jun 2013.
-
19Ministério da Saúde (BR). Secretaria de Gestão do Trabalho e da Educação na Saúde. Edital nº 02, de 15 de janeiro de 2015. Adesão de médicos aos programas de provisão de médicos do Ministério da Saúde – Projeto Mais Médicos para o Brasil e Programa de Valorização do Profissional da Atenção Básica. Diário Oficial da União. 15 Jan 2015.
-
20Ministério da Saúde (BR). Portaria nº 1.602, de 9 de julho de 2011. Define o valor mínimo da parte fixa do Piso de Atenção Básica (PAB), para efeito do cálculo do montante de recursos a ser transferido do Fundo Nacional de Saúde aos Fundos de Saúde dos Municípios e do Distrito Federal, e divulga os valores anuais e mensais da parte fixa do PAB. Diário Oficial da União. 11 Jul 2011.
-
21Ministério da Saúde (BR). Secretaria de Atenção à Saúde. Departamento de Atenção Básica. Saúde da família no Brasil: uma análise de indicadores selecionados: 1998-2004. Brasília: Ministério da Saúde; 2006.
-
22Rede Observatório Programa Mais Médicos. Relatório da Pesquisa de Dados Secundários do Programa Mais Médicos até 2014 [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
» http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos -
23OPAS. Implementação do Programa “Mais Médicos” em Curitiba. Experiências inovadoras e lições aprendidas [Internet]. 2015 [citado 10 Mar 2016]. Disponível em: http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
» http://www.otics.org/estacoes-de-observacao/observatorio-mais-medicos
-
(h)
Pesquisa avaliação de política pública para saúde no Brasil: Programa Mais Médicos. UFMG e IPESPE. 2015. Mimeo.
Publication Dates
-
Publication in this collection
21 Aug 2017 -
Date of issue
2017
History
-
Received
05 July 2016 -
Accepted
06 Dec 2016