Abstract:
Objective:
To assess the quality of mortality information by analyzing the frequency of garbage codes (GC) registered as underlying cause-of-death in Belo Horizonte, Minas Gerais, Brazil.
Methods:
Data of deaths of residents from 2011 to 2013 were selected. GC causes were classified as proposed by the Global Burden of Disease Study (GBD) 2015. They were grouped into GCs from ICD-10 Chapter XVIII and GCs excluding codes of Chapter XVIII. Proportions of GC were calculated by sex, age, and place of occurrence.
Results:
In Belo Horizonte, 30.5% of the total of 44,123 deaths were GC. Higher proportion of these codes was observed in children (1 to 4 years) and in people aged over 60 years. The following leading GCs observed were: other ill-defined and unspecified causes of death (code R99), unspecified pneumonia (J18.9), unspecified stroke (hemorrhagic or ischemic) (I64), and unspecified septicemia (A41.9). The proportions of GC were 28.7% and 36.9% in deaths that occurred in hospitals and at home, respectively. An important difference occurred in the GC group from Chapter XVIII of ICD-10: 1.7% occurred in hospitals and 16.9% at home.
Conclusion:
The high proportions of GC in mortality statistics in Belo Horizonte demonstrated its importance for assessing the quality of information on causes of death.
Keywords:
Data accuracy; Mortality; Cause of death
Resumo:
Objetivo:
Avaliar a qualidade da informação sobre causas de óbito, identificando a frequência de códigos garbage (CG) em Belo Horizonte, Minas Gerais.
Métodos:
Foram selecionados óbitos de residentes, ocorridos de 2011 a 2013. As causas de óbito foram classificadas como CG, segundo a lista do estudo Global Burden of Disease (GBD) 2015. Esses códigos foram agrupados em: CG do capítulo XVIII da CID-10 e CG de outros capítulos da CID-10. Foram calculadas as proporções de CG por sexo, faixa etária e local de ocorrência.
Resultados:
Em Belo Horizonte ocorreram 44.123 óbitos no período analisado, dos quais 30,5% tiveram sua causa classificada como CG. Maiores proporções desses códigos foram observadas em crianças de 1 a 4 anos e em maiores de 60 anos. Os principais CG foram: outras causas mal definidas e as não especificadas de mortalidade (R99), pneumonia não especificada (J18.9), acidente vascular cerebral não especificado como hemorrágico ou isquêmico (I64) e septicemias (A41.9). Em 28,7% dos óbitos ocorridos em hospitais, a causa básica do óbito foi por CG, sendo essa proporção maior para óbitos domiciliares (36,9%). Maior diferença foi observada para os CG do capítulo XVIII da CID-10: 1,7% em hospitais e 16,9% para óbitos no domicílio.
Conclusão:
A magnitude dos CG nas estatísticas de mortalidade enfatiza sua importância na avaliação da qualidade da informação sobre causas de óbito.
Palavras-chave:
Confiabilidade dos dados; Mortalidade; Causas de morte
INTRODUCTION
Knowledge of the health profile of the population is fundamental for the evaluation and planning of health interventions. However, this diagnosis will only reflect the present scenario if based on high-quality information11. Mathers CD, Fat DM, Inoue M, Rao C, Lopez AD. Counting the dead and what they died from: an assessment of the global status of cause of death data. Bull World Health Organ 2005 Mar; 83(3): 171-7.. In Brazil, an important source of data for this diagnosis is the Mortality Information System (Sistema de Informação sobre Mortalidade; SIM). Implemented in the country in 1975, it became a computerized system in 1979. Since then, the use of this feature has gained strength and investments have been made to improve its quality over time22. França E, Teixeira R, Ishitani L, Duncan BB, Cortez-Escalante JJ, Morais Neto OL, et al. Causas mal definidas de óbito no Brasil: método de redistribuição baseado na investigação do óbito. Rev Saúde Pública 2014; 48(4): 671-81..
Traditionally, the quality of information on causes of death has been assessed since 1996 by the proportion of ill-defined causes from Chapter XVIII of the International Statistical Classification of Diseases and Related Health Problems (ICD), tenth revision (ICD-10)33. Rede Interagencial de Informação para a Saúde. Indicadores básicos para a saúde no Brasil: conceitos e aplicações. 2ª ed. Brasília: Organização Pan-Americana da Saúde; 2008.,44. Laurenti R, Mello-Jorge MHP, Gotlieb SLD. A confiabilidade dos dados de mortalidade e morbidade por doenças crônicas não-transmissíveis. Ciênc Saúde Coletiva 2004; 9(4): 909-20.. However, studies have indicated a tendency in considering other ill-defined causes and incomplete diagnoses from other chapters of ICD-10, defined in conjunction with those in Chapter XVIII as garbage codes (GCs). Despite still undeserving attention by health services and professionals, the importance of this group of causes has been highlighted in order to advance the discussion on the quality of the information55. Naghavi M, Makela S, Foreman K, O'Brien J, Pourmalek F, Lozano R. Algorithms for enhancing public health utility of national causes-of-death data Population Health Metrics 2010; 8: 9.,66. GBD 2015 Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016; 388: 1459-544..
The definition of GC was introduced in the Global Burden of Disease Study 1990, published in 199677. Murray CJL, Lopez AD. The global burden of disease: a comprehensive assessment of mortality and disability from diseases, injuries, and risk factors in 1990 and projected to 2020. Cambridge, MA: Harvard School of Public Health/World Health Organization/World Bank; 1996.. It consists of diagnoses that should not be considered as an underlying cause of death, as were not considered very useful in public health55. Naghavi M, Makela S, Foreman K, O'Brien J, Pourmalek F, Lozano R. Algorithms for enhancing public health utility of national causes-of-death data Population Health Metrics 2010; 8: 9., because they do not allow for adequate identification of actions for prevention and control of diseases and health disorders11. Mathers CD, Fat DM, Inoue M, Rao C, Lopez AD. Counting the dead and what they died from: an assessment of the global status of cause of death data. Bull World Health Organ 2005 Mar; 83(3): 171-7.. For example, causes such as septicemia, malignant neoplasia without specific localization, cerebral palsy, heart failure, and renal failure do not define the disease that caused the death and, according to the GBD method, should be redistributed to specific causes, according to algorithms defined in the study55. Naghavi M, Makela S, Foreman K, O'Brien J, Pourmalek F, Lozano R. Algorithms for enhancing public health utility of national causes-of-death data Population Health Metrics 2010; 8: 9.,88. Ahern RM, Lozano R, Naghavi M, Foreman K, Gakidou E, Murray CJ. Improving the public health utility of global cardiovascular mortality data: the rise of ischemic heart disease. Popul Health Metr 2011; 9: 8..
GCs therefore consist of ICD codes for underlying causes of death with ill-defined or incomplete diagnoses that do not indicate the specific cause of death. Thus, a high proportion of GCs compromises the quality of information on causes of death, which may hinder the identification of priorities and the adequate planning of actions to be taken.
Considering the importance of this group of causes in the SIM data analysis, a study was carried out in the city of Belo Horizonte aimed at identifying the frequency of GCs and their distribution in health facilities to propose appropriate interventions and consequent improvement of the information on causes of death.
METHODS
From the SIM/DATASUS database, deaths of residents of Belo Horizonte were selected in the 2011-2013 triennium, in order to reduce random variations due to small numbers. To compare GC proportions, deaths were also selected in other capitals of the country.
The classification of causes as GCs was carried out as proposed by the GBD 2015 study66. GBD 2015 Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016; 388: 1459-544.. In the Brazilian Portuguese version of this study, the authors decided not to translate the term “garbage”, since it is already widely adopted in the literature and because the translation to the Portuguese word lixo results in some distortion in the meaning of the term, as some GCs are only nonspecific - such as cerebrovascular disease, unspecified as ischemic or hemorrhagic. In contrast, a death due to septicemia in a young adult represents a GC with a different qualification, as septicemia cannot be considered the underlying cause of this death.
The causes of death classified as garbage were analyzed according to three and four characters - 3C and 4C, respectively - of ICD-10. The GCs were grouped into two categories:
-
GC-R codes: GC from Chapter XVIII of ICD-10 and
-
GC-non-R codes: GC from chapters other than Chapter XVIII.
The GCs selected for analysis were septicemia (ICD-10 A40-A41), hypertensive diseases (I10), heart failure (I50), cerebrovascular diseases, unspecified (UNS) as hemorrhagic or ischemic (I62.1, I62.9, I64, I67.4, I67.8, I67.9, I68.8, I69.4, I69.8, I69.9), UNS pneumonia (J15.9, J17.0, J17.1, J17.2, J17.3, J17.8, J18.0, J18.1, J18.2, J18.7, J18.8, J18.9), other perinatal causes (P96.9), UNS congenital anomalies (Q10.0, Q10.1, Q10.2, Q10.3, Q36.0, Q36.1, Q36.9, Q89.9, Q99.9), ill-defined causes from Chapter XVIII-ICD 10 (R00-R99), traffic accidents, unspecified (V87.0, V87.1, V87.4, V87.5, V87.6, V87.7, V87.8, V87.9, V88.0, V88.1, V88.4, V88.5, V88.6, V88.7, V88.8, V88.9, V89.0, V89.1, V89.2, V89.3, V89.4, V89.9), and external causes classified as events of undetermined intent (Y10-Y34).
In order to evaluate the relative weight of GCs in Belo Horizonte and in the other capitals of the country, GC proportions were calculated and disaggregated into two groups: GC-R codes and GC-non-R codes. The proportions were calculated for the sum of GC deaths and also for the total number of deaths from all causes during the analyzed period (2011-2013).
The deaths which occurred in Belo Horizonte were analyzed by sex, age - aged under 1 year, 1-4, 5-14, 15-29, 30-59, and 60 years or over - and the place of occurrence.
This study did not require submission to the Research Ethics Committee, as secondary data available on the Internet were used, and the data did not contain any identifying information of the research subjects.
RESULTS
Table 1 shows that of the total of 44,123 deaths reported in Belo Horizonte in the period, 30.5% (n = 13,438) corresponded to GCs, being mostly GC-non-R codes - 25.0% of total causes. Only a few other capitals had a higher GC proportion than Belo Horizonte in the period: Fortaleza and Salvador, in the Northeast; Rio de Janeiro, in the Southeast; and the capitals of the Northern region, except for Manaus and Palmas. The capitals with the lowest proportions of GCs were those of the Southern region, in addition to Vitória and Palmas. In the country, 28.3% of the total deaths that occurred in the capitals had a GC as the underlying cause of death, with 25.2% being GC-non-R codes and 3.1% GC-R codes. In all capitals, GC-R codes were responsible for the lower GC percentage. It is noteworthy that Manaus and Macapá, both from the North region, presented higher proportions of GC-R codes: 11.8 and 7.8%, respectively. In addition to this, Manaus presented the third lowest proportion of GC-non-R codes (18.5%).
Regarding age, a higher proportion of GCs were observed in Belo Horizonte among children aged 1-4 years and among the elderly. In males, this proportion was higher in the age group from 30 to 59 years; in females, the age group of 1-4 years prevailed. With the exception of the age groups of under 1 year and 30-59 years, the proportion of GCs was higher in females, with 45.3% in the age group of 1-4 years (Figure 1).
Table 2 presents the 20 main causes of death - classification by four characters of the ICD-10 - of residents in Belo Horizonte. These causes were responsible for approximately 40% of the total deaths. The following causes considered as GCs are among the main causes of death: other ill-defined and unspecified causes of mortality (ICD-10 R99 code), UNS pneumonia (J18.9), stroke UNS as hemorrhagic or ischemic (I64), UNS septicemia (A41.9), other specified cerebrovascular diseases (I67.8), essential hypertension (I10), and sequelae of stroke UNS as hemorrhagic or ischemic (I69.4). It should be noted that the first two causes are in greater proportions, responsible for 9.3% of the total deaths.
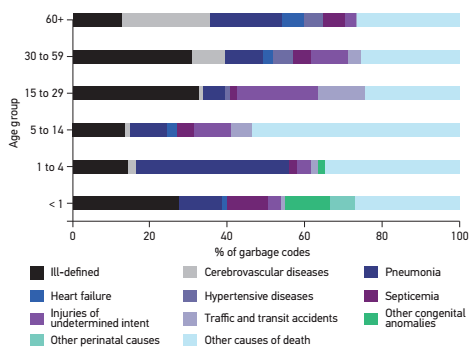
Figure 2 shows the main GC groups according to age groups. Ill-defined causes, pneumonias and septicemia stood out as the main GCs in all ages. Age groups that presented the highest proportions of GCs for ill-defined causes, exceeding 30%, were those aged 15-29 and 30-59 years. Unspecified pneumonia was highest in the age group of 1-4 years and in the elderly. Septicemia was higher in children younger than 1 year, in which UNS congenital anomalies still stand out. In the age groups of 5-14 and 15-29 years, the high proportion of events of undetermined intent and traffic accidents with type of vehicle unspecified or victim’s mode of transport unknown are also noteworthy. From the age of 30 years onwards, unspecified cerebrovascular diseases stand out, as well as heart failure in the over 60s.
The majority (74.4%) of the deaths occurred in health facilities (68.4% in hospitals) and 17.6% at home. For deaths in hospitals, the proportion of GCs (total) was 28.7%. In other health care facilities, home and other locations, this proportion was higher, around 36%. In relation to the GC-R codes group, this proportion was 16.9% for deaths occurring at home and only 1.7% for hospital cases (Table 3). Of the total GC-R codes (n = 2,410), 54.5% occurred at home. However, in the GC-non-R codes group (n = 11,028), 74.1% occurred in hospitals (data not shown).
Regarding health facilities in Belo Horizonte, it was verified that among the 21 hospitals with the highest number of GC deaths, 5 had a higher proportion than the average of the municipality (30.5% of GCs). It was observed that GC-non-R codes were the most reported, and specialized hospitals for trauma and cancer care, as well as one university hospital, were those with the lowest GC proportion (data not shown).
DISCUSSION
This study emphasizes the importance of evaluating the quality of information on mortality by focusing on GCs in the city of Belo Horizonte. This analysis is an important strategy to encourage the improvement of the quality of information11. Mathers CD, Fat DM, Inoue M, Rao C, Lopez AD. Counting the dead and what they died from: an assessment of the global status of cause of death data. Bull World Health Organ 2005 Mar; 83(3): 171-7., as it signals to health services the main problems related to filling in causes of death on the Death Certificate (DC).
In Brazil and macro-regions, a reduction in deaths due to ill-defined causes has been observed99. Costa MR, Marcopito LF. Mortalidade por causas mal definidas, Brasil, 1979-2002, e um modelo preditivo para idade. Cad Saúde Pública 2008; 24(5): 1001-12.,1010. Martins Junior DF, Costa TM, Lordelo MS, Felzemburg RDM. Tendência dos óbitos por causas mal definidas na região Nordeste do Brasil, 1979-2009. Rev Assoc Med Bras 2011; 57(3): 338-46.. However, with the exception of Manaus, which presented a proportion greater than 10% in the period, it was found that despite the small percentage of ill-defined causes - GC-R codes corresponding to Chapter XVIII of ICD-10 - other GCs stood out as important causes of death, showing that only an analysis of the percentage of ill-defined causes is not enough to evaluate the quality of information on causes of death. Kanso et al.1111. Kanso S, Romero DE, Leite IC, Moraes EN. Diferenciais geográficos, socioeconômicos e demográficos da qualidade da informação da causa básica de morte dos idosos no Brasil. Cad Saúde Pública 2011; 27(7): 1323-39., using the GC definition of the GBD 2000 study, also found a greater proportion of these causes in relation to the codes in Chapter XVIII. Interestingly, with this approach, capitals that initially presented a better quality of information show another profile when the proportion of total GC is presented, indicating the necessity to advance the discussion on the quality of the DC, which also should consider the GC-non-R codes.
Belo Horizonte is considered to be a capital with high-quality information on mortality, due to the percentage of approximately 5% of ill-defined causes (GC-R codes). This proportion was obtained due to the efforts made by the municipal health department through investigation of deaths by the surveillance team and the training of physicians in the adequate filling in of the DC, among other activities. However, when analyzing this quality through the GC approach, it is observed that the municipality is among the capitals with the highest GC percentage, which indicate the need to improve actions related to the improvement of the quality of this information.
In relation to the age groups, Naghavi et al.55. Naghavi M, Makela S, Foreman K, O'Brien J, Pourmalek F, Lozano R. Algorithms for enhancing public health utility of national causes-of-death data Population Health Metrics 2010; 8: 9. also observed a higher proportion of GCs in the ages of 1 and 14 years, with a reduction in this proportion in adulthood and with an increase in the more advanced age groups. The high proportion of GCs found in Belo Horizonte in the age group of 1-4 years may be related to the lower number of deaths. As for the age group of 60 years and over, Ngo et al.1212. Ngo AD, Rao C, Hoa NP, Adair T, Chuc NTK. Mortality patterns in Vietnam, 2006: Findings from a national verbal autopsy survey. BMC Research Notes 2010; 3(1): 78. and Costa & Marcopito99. Costa MR, Marcopito LF. Mortalidade por causas mal definidas, Brasil, 1979-2002, e um modelo preditivo para idade. Cad Saúde Pública 2008; 24(5): 1001-12. also found a higher proportion of ill-defined deaths at higher ages. Such findings may be due to the greater occurrence of comorbidities in the elderly, which make it difficult to establish the correct underlying cause that led to death1313. Mello Jorge MHP, Laurenti R, Lima-Costa MF, Gotlieb SLD, Chiavegatto Filho ADP. A mortalidade de idosos no Brasil: a questão das causas mal definidas. Epidemiol Serv Saúde 2008; 17(4): 271-81..
The lower proportion of ill-defined deaths in men of productive age compared with women may be related to the higher occurrence of external causes among them. These deaths are certified by coroners after autopsy reports and the circumstances of the injuries are investigated in police reports by the municipal health department, leading to a specific diagnosis of the cause of death1414. Matos SG, Proietti FA, Barata RCB. Confiabilidade da informação sobre mortalidade por violência em Belo Horizonte, MG. Rev Saúde Pública 2007; 41(1): 76-84. Disponível em: http://www.scielo.br/pdf/rsp/v41n1/12.pdf (Accessed on: December 12, 2016).
http://www.scielo.br/pdf/rsp/v41n1/12.pd...
.
When analyzing the occurrence of the five main GC groups - other ill-defined and unspecified causes of mortality, unspecified pneumonias, stroke unspecified as hemorrhagic or ischemic, unspecified septicemia and other specified cerebrovascular diseases - the importance of a better understanding of the concept of GC is evident given that such causes offer information of little use to support planning for specific health conditions.
Regarding the ill-defined causes of the GC-R code group, the Ministry of Health has implemented the investigation of all these deaths as a strategy for quality improvement1515. Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Departamento de Análise de Situação em Saúde. Manual para investigação do óbito com causa mal definida. Brasília: Ministério da Saúde; 2009.. Although, in these cases, the municipality searches for information by surveying outpatient medical records and hospital information systems, the underlying cause obtained often remains as a GC. Some GCs from Chapter XX of the ICD-10 (external causes) remain of undetermined intent even after investigation by health services. In the classification of external causes, the consultation of the autopsy reports, police reports, press reports, and the linkage of the SIM database with that of traffic accidents involving casualties (Reds-BH10) is often not enough to select a specific underlying cause of death. This happens, for example, in hit-and-run or collisions in which one of the vehicles involved has evaded.
Other GCs are not usually investigated. Among these, GC I64 or I67.8 includes hemorrhagic or ischemic cerebrovascular diseases, which have different procedures in their treatment and prevention. Likewise, septicemia and heart failure, when declared as underlying causes of death, do not elucidate the several diagnoses that may have triggered the sequence of events that led to death. Specific information is likely to be contained in health care records, such as imaging for cerebrovascular diseases1616. Truelsen T, Krarup LH, Iversen HK, Mensah GA, Feigin VL, Sposato LA, et al. Causes of Death Data in the Global Burden of Disease Estimates for Ischemic and Hemorrhagic Stroke. Neuroepidemiology 2015; 45(3): 152-60., as the diagnosis of the underlying disease is necessary for appropriate treatment1313. Mello Jorge MHP, Laurenti R, Lima-Costa MF, Gotlieb SLD, Chiavegatto Filho ADP. A mortalidade de idosos no Brasil: a questão das causas mal definidas. Epidemiol Serv Saúde 2008; 17(4): 271-81.. Thus, it is important to sensitize the attending physician to the adequate information of the specific cause of death during the filling in of the DC.
The different profile found in the proportion of GCs according to place of occurrence, with lower proportion in hospitals, was already expected, considering the greater ease of diagnosis after hospitalization1717. Abreu DMX, Sakurai E, Campos LN. A evolução da mortalidade por causas mal definidas na população idosa em quatro capitais brasileiras, 1996-2007. Rev Bras Est Pop 2010; 27(1): 75-88.. Despite this, the proportion of GCs in hospitals remains high. This finding also occurs when the lower percentage of GCs is verified in specialized hospitals - such as trauma and cancer centers and university hospitals. There was also a lower proportion of GC in a reference hospital for trauma in the state, as the deaths due to accidents and violence are declared by the Brazilian forensic medicine institute, Instituto Medico Legal (IML), in which an active search with systematic investigation is carried out by the municipal health department. Therefore, the underlying cause could be defined, for the majority of deaths occurring in hospitals, taking into account that this should correspond to the diagnostic hypothesis that guided the treatment1313. Mello Jorge MHP, Laurenti R, Lima-Costa MF, Gotlieb SLD, Chiavegatto Filho ADP. A mortalidade de idosos no Brasil: a questão das causas mal definidas. Epidemiol Serv Saúde 2008; 17(4): 271-81..
The fact that 54.5% of the deaths due to ill-defined causes of the GC-R codes group occurred at home shows the difficulty in defining a diagnosis in situations where death does not occur in health care facilities. This finding may be aggravated by the absence of the Death Verification Service (Serviço de Verificação de Óbitos; SVO) in Belo Horizonte. In contrast, the higher percentage of GC-non-R codes, especially in hospitals, may be due to the process of improving the filling in of the DC by physicians. Guidelines and clarifications given to health professionals by the municipal health department seem to have resulted in the reduction of causes from Chapter XVIII of ICD-10 (R00-R99) reported as the underlying cause of death. There may have been, however, a displacement to a non-specific cause from another chapter.
According to the findings of this study, based on the GC list of the GBD 2015 study, two GCs raise an important discussion. The etiological diagnosis of pneumonia (J18.9) presents a challenge, considering that the request for microbiological examinations is not routinely performed in health services and, in the short term, the implantation of this type of routine is not feasible, due to its high cost1818. Rodrigues JC, Silva Filho LVF, Bush A. Diagnóstico etiológico das pneumonias - uma visão crítica. J Pediatr 2002; 78(2): s129-40.. It would be important, however, to develop studies to evaluate the specific causes of these deaths, especially in children, given the availability of vaccines for some etiologies. These studies would also be relevant in the case of adults and elderly individuals, where pneumonia may not often be the underlying cause of death. I67.8 is considered a valid code for cerebral ischemia, according to ICD-10, and should have its inclusion reconsidered in the GC list.
Essential hypertension is considered in the GBD study as a risk factor and is classified as a GC because of its low utility when it is declared as the underlying cause of death, since it may be related to different categories of disease, such as ischemic heart disease, ischemic cerebrovascular disease, hemorrhagic cerebrovascular disease, and chronic kidney disease, among others1616. Truelsen T, Krarup LH, Iversen HK, Mensah GA, Feigin VL, Sposato LA, et al. Causes of Death Data in the Global Burden of Disease Estimates for Ischemic and Hemorrhagic Stroke. Neuroepidemiology 2015; 45(3): 152-60.. Thus, when the physician declares only essential hypertension in the DC, it is selected as the underlying cause, and information on associated diseases is lost.
In general, the results of this study indicate the need to make efforts in the investigation of GC deaths, both GC-R codes and GC-non-R codes. This procedure would make it possible to elucidate the underlying cause of death and a consequent enhancement of SIM1919. Mello Jorge MHP, Gotlieb SLD, Laurenti R. O sistema de informações sobre mortalidade: problemas e propostas para o seu enfrentamento. Mortes por causas naturais. Rev Bras Epidemiol 2002; 5(2): 197-211.. It would also allow the calculation of correction factors for more adequate estimates of the risk of mortality due to specific causes. It is also important to emphasize the importance of adequate coding for the selection of the correct underlying cause and, above all, the need to reinforce the training of physicians to correctly fill in the DC, and to ensure greater access for patients to care and diagnosis, necessary to ensure high-quality information on causes of death.
CONCLUSION
The results of this study indicate the magnitude of GCs in the municipality’s mortality statistics, pointing out the importance of adequate strategies to qualify the information on causes of death, which include both the investigation of these deaths and the training of physicians to adequately fill in the DC. It is necessary to invest in the awareness of the health professionals about the importance of the DC for health statistics that can subsidize the development of actions and programs for prevention and treatment of avoidable diseases.
REFERÊNCIAS
-
1Mathers CD, Fat DM, Inoue M, Rao C, Lopez AD. Counting the dead and what they died from: an assessment of the global status of cause of death data. Bull World Health Organ 2005 Mar; 83(3): 171-7.
-
2França E, Teixeira R, Ishitani L, Duncan BB, Cortez-Escalante JJ, Morais Neto OL, et al. Causas mal definidas de óbito no Brasil: método de redistribuição baseado na investigação do óbito. Rev Saúde Pública 2014; 48(4): 671-81.
-
3Rede Interagencial de Informação para a Saúde. Indicadores básicos para a saúde no Brasil: conceitos e aplicações. 2ª ed. Brasília: Organização Pan-Americana da Saúde; 2008.
-
4Laurenti R, Mello-Jorge MHP, Gotlieb SLD. A confiabilidade dos dados de mortalidade e morbidade por doenças crônicas não-transmissíveis. Ciênc Saúde Coletiva 2004; 9(4): 909-20.
-
5Naghavi M, Makela S, Foreman K, O'Brien J, Pourmalek F, Lozano R. Algorithms for enhancing public health utility of national causes-of-death data Population Health Metrics 2010; 8: 9.
-
6GBD 2015 Mortality and Causes of Death Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause specific mortality for 249 causes of death, 1980-2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016; 388: 1459-544.
-
7Murray CJL, Lopez AD. The global burden of disease: a comprehensive assessment of mortality and disability from diseases, injuries, and risk factors in 1990 and projected to 2020. Cambridge, MA: Harvard School of Public Health/World Health Organization/World Bank; 1996.
-
8Ahern RM, Lozano R, Naghavi M, Foreman K, Gakidou E, Murray CJ. Improving the public health utility of global cardiovascular mortality data: the rise of ischemic heart disease. Popul Health Metr 2011; 9: 8.
-
9Costa MR, Marcopito LF. Mortalidade por causas mal definidas, Brasil, 1979-2002, e um modelo preditivo para idade. Cad Saúde Pública 2008; 24(5): 1001-12.
-
10Martins Junior DF, Costa TM, Lordelo MS, Felzemburg RDM. Tendência dos óbitos por causas mal definidas na região Nordeste do Brasil, 1979-2009. Rev Assoc Med Bras 2011; 57(3): 338-46.
-
11Kanso S, Romero DE, Leite IC, Moraes EN. Diferenciais geográficos, socioeconômicos e demográficos da qualidade da informação da causa básica de morte dos idosos no Brasil. Cad Saúde Pública 2011; 27(7): 1323-39.
-
12Ngo AD, Rao C, Hoa NP, Adair T, Chuc NTK. Mortality patterns in Vietnam, 2006: Findings from a national verbal autopsy survey. BMC Research Notes 2010; 3(1): 78.
-
13Mello Jorge MHP, Laurenti R, Lima-Costa MF, Gotlieb SLD, Chiavegatto Filho ADP. A mortalidade de idosos no Brasil: a questão das causas mal definidas. Epidemiol Serv Saúde 2008; 17(4): 271-81.
-
14Matos SG, Proietti FA, Barata RCB. Confiabilidade da informação sobre mortalidade por violência em Belo Horizonte, MG. Rev Saúde Pública 2007; 41(1): 76-84. Disponível em: http://www.scielo.br/pdf/rsp/v41n1/12.pdf (Accessed on: December 12, 2016).
» http://www.scielo.br/pdf/rsp/v41n1/12.pdf -
15Brasil. Ministério da Saúde. Secretaria de Vigilância em Saúde. Departamento de Análise de Situação em Saúde. Manual para investigação do óbito com causa mal definida. Brasília: Ministério da Saúde; 2009.
-
16Truelsen T, Krarup LH, Iversen HK, Mensah GA, Feigin VL, Sposato LA, et al. Causes of Death Data in the Global Burden of Disease Estimates for Ischemic and Hemorrhagic Stroke. Neuroepidemiology 2015; 45(3): 152-60.
-
17Abreu DMX, Sakurai E, Campos LN. A evolução da mortalidade por causas mal definidas na população idosa em quatro capitais brasileiras, 1996-2007. Rev Bras Est Pop 2010; 27(1): 75-88.
-
18Rodrigues JC, Silva Filho LVF, Bush A. Diagnóstico etiológico das pneumonias - uma visão crítica. J Pediatr 2002; 78(2): s129-40.
-
19Mello Jorge MHP, Gotlieb SLD, Laurenti R. O sistema de informações sobre mortalidade: problemas e propostas para o seu enfrentamento. Mortes por causas naturais. Rev Bras Epidemiol 2002; 5(2): 197-211.
-
Financial support: Bill & Melinda Gates Foundation (GBD Global) and Ministry of Health (GBD 2015 Brazil-states), through the National Health Fund (Process No. 25000192049/2014-14).
Publication Dates
-
Publication in this collection
May 2017
History
-
Received
10 Jan 2017 -
Accepted
21 Feb 2017



 Source: SIM/DATASUS.
Source: SIM/DATASUS.
 Source: SIM/DATASUS.
Source: SIM/DATASUS.