Abstracts
Purpose
to determine whether tobacco use enhances the effects of noise caused hearing.
Methods
153 workers of both sexes, smokers and nonsmokers, from an food sector industry, randomly chosen from among 14 sectors of the company, whose band noise was presented a variation from 85 to 109 dB, answered a questionnaire about time exposure to noise as well as on smoking habits and submitted to audiometry.
Results
the hearing thresholds in the frequencies of 4000 Hz and 6000 Hz were significantly higher in the group of smokers / ex-smokers when compared to nonsmokers in both ears, these thresholds, characteristic of hearing loss induced by noise. These differences remained significant after age adjustment and exposure time.
Conclusion
through the obtained results it was possible to conclude a correlation between the use of tobacco and hearing loss.
Noise; Hearing Loss Noise-Induced; Tobacco; Hearing
Objetivo
verificar se o uso do tabaco potencializa os efeitos do ruído causados na audição.
Métodos
153 trabalhadores de ambos os sexos, fumantes e não-fumantes, de uma indústria do ramo alimentício, escolhidos aleatoriamente dentre 14 setores da empresa, cuja faixa de ruído apresentada teve uma variação de 85 a 109 dBNA, responderam a um questionário sobre tempo e exposição ao ruído bem como hábitos sobre fumo e passaram por exame de audiometria.
Resultados
os limiares auditivos da via aérea nas frequências de 4.000 Hz e 6.000Hz foram significantemente mais altos no grupo de fumantes/ex-fumantes quando comparados aos não-fumantes tanto na orelha direita quanto na orelha esquerda; limiares estes, característicos da perda auditiva induzida por ruído. Essas diferenças se mantiveram significantes após o ajuste pela idade e pelo tempo de exposição.
Conclusão
por meio dos resultados obtidos, concluiu-se que o uso do tabaco pode potencializar os danos causados pelo ruído à audição.
Ruído; Perda Auditiva Provocada por Ruído; Tabaco; Audição
INTRODUCTION
The worry with the workers’ health has increased over the years, causing several studies are performed with the intention of preventing the injuries that work can lead to the individual. Among the health problems related to work, Noise Induced Hearing Loss (NIHL) is one of the most frequent worldwide11 . Ministério da Saúde do Brasil. Doenças relacionadas ao trabalho: manual de procedimentos para os serviços de saúde. Brasília: Ministério da Saúde do Brasil, 2001..
The NIHL, also called Induced Hearing Loss High Sound Pressure Levels (HSPLIHL), it feature is sensorineural, affecting the hearing thresholds in one or more frequency band of 3 to 6 KHz.Progresses as time of exposure and is characterized be irreversible22 . Seligman J. Sintomas e sinais na PAIR. In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997..Some symptoms associated with NIHL may arise, such as tinnitus, difficulty in speech understanding, algiacusia, ear fullness and feeling of “muffled”; hearing, as well as recruitment, present in virtually all cases22 . Seligman J. Sintomas e sinais na PAIR. In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997.,33 . Lobo R, Costa EA. Classificação das perdas auditivas induzidas pelo ruído. In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997..
Currently, one of the biggest challenges in the area of occupational health constitutes in the studies on the effects of combined occupational exposures, since many physical and chemical agents can be found in the work environment44 . Morata TC, Dunn, DE, Sieber, WK. Perda auditiva e a exposição ocupacional a agentes ototóxicos. . In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997..Chemicals such as acetone, styrene, resins, cobalt, among others, associated with exposure to noise favor a higher incidence of hearing loss55 . Botelho CT, Paz APML, Gonçalves AM, Frota S. Estudo comparativo de exames audiométricos de metalúrgicos expostos a ruído e ruído associado a produtos químicos. Rev. Bras. Otorrinolaringol. 2009;75(1):51-7..Also, with respect to concomitant exposure to insecticides and noise, the average time for the development of hearing disorders is lower than when the exposure is performed only to the noise66 . Teixeira CF, Augusto LGS, Morata TC. Saúde auditiva de trabalhadores expostos a ruído e inseticidas. Rev. Saúde Pública. 2003;37(4):417-23.. Other researches indicates that carbon monoxide can have a direct effect on the cochlear metabolism77 . Lacerda A, Leroux T, Morata TC. Efeitos ototóxicos da exposição ao monóxido de carbono: uma revisão. Pró-Fono R. Atual. Cient. 2005;17(3):403-12..There are other ototoxic chemicals found in the workplace: arsenic and its compounds, lead and its compounds, ethylene glycol, hydrogen sulfide gas, mixtures of solvents, toluene, xylene, and others88 . Protocolos de procedimentos médico-periciais de doenças profissionais e do trabalho: subsídios para a implementação do anexo II do CRETO 3.048/99 pelo INSS. Informativo ANAMT (Associação Nacional de Medicina do Trabalho) nº10 vol. 2 – fevereiro de 2000.. With respect to physical agents, studies point vibration as an aggressive agent not only hearing, but the agency as a whole99 . Fernandes M, Morata TC. Estudo dos efeitos auditivos e extra-auditivos da exposição ocupacional a ruído e vibração. Rev. Bras. Otorrinolaringol. 2002;68(5): 705-13..
Other factors, not only agents found in the workplace can contribute to the onset
and worsening of hearing loss. The literature presents studies that link smoking
as a risk factor for conductive hearing loss and sensorineural1010 . Paschoal CP, Azevedo MF. O cigarro como um fator de risco para
alterações auditivas. Braz. j. otorhinolaryngol.
2009;75(6):893-902.
11 . Mohammadi S, Mazhari MM, Mehrparvar AH, Attarchi MS. Effect of
simultaneous exposure to occupational noise and cigarette smoke on binaural
hearing impairment. Noise Health. 2010;12(48):187-90.
12 . Uchida Y, Nakashima T, Ando F, Niino N, Shimokata H. Is there a
relevant effect of noise and smoking on hearing? A population-based aging study.
International Journal of Audiology. 2005;44:86-91.-1313 . Angrisani RMG, Matas CG, Furtado JRB. Análise dos potenciais
evocados auditivos em fumantes. Acta ORL. 2010;26(3):140-208..The hearing may be affected
by the effect of cigarette antioxidant mechanism or by suppressing vascular
hearing system. Some studies have also indicated that smokers show changes in
the hearing pathway in the low nerve and the central hearing pathways in
subcortical regions1313 . Angrisani RMG, Matas CG, Furtado JRB. Análise dos potenciais
evocados auditivos em fumantes. Acta ORL. 2010;26(3):140-208..
According to the literature, smoking is associated with lower blood oxygen levels, vascular obstructions and changes in blood viscosity, which may have an ototoxic effect1010 . Paschoal CP, Azevedo MF. O cigarro como um fator de risco para alterações auditivas. Braz. j. otorhinolaryngol. 2009;75(6):893-902.. However, as tobacco results in the burning of more than 4000 components, including nicotine, carbon monoxide, carbon dioxide, methanol, nitrogen and oxidants, is difficult to determine whether nicotine would be the cause of the greater adverse effect or would be combination of several components1313 . Angrisani RMG, Matas CG, Furtado JRB. Análise dos potenciais evocados auditivos em fumantes. Acta ORL. 2010;26(3):140-208..
Studies indicated that smoking is one of the most prevalent addictions throughout the world, and in Brazil, according to a survey conducted in 2005, more than 10% of the population between 12 and 65 years makes use of tobacco1414 . Azevedo RCS, Higa CMHi, Assumpção ISAM, Fernandes RF, Boscolo MM, Frazatto CRG. Atenção aos tabagistas pela capacitação de profissionais da rede pública. Rev. Saúde Pública. 2008;42(2):353-5..
Thus, with NIHL one of the biggest health problems related to work, smoking have a high prevalence worldwide and also considering that there are findings in the literature that indicate that smoking can harm hearing, this work was to check whether the use of tobacco potentiates the effects of noise caused hearing.
METHODS
This research was approved by the CEFAC Research Ethics Committee under No. 016/11.
This is a cross-sectional study of 246 workers at a food company in the state of Santa Catarina, in the period November 2010 to May 2011.The selected workers presented aged 15 to 60 years, with time of exposure to noise between 1 and 15 years and were chosen randomly from 14 sectors of the company, whose noise band had presented a variation 85-109 dB HL. The values of noise levels in each sector were obtained from the company’s Program for Prevention of Environmental Risks, that reported providing hearing protection to all employees exposed to noise, making use of the same requirement.
Before beginning the study, all subjects involved were informed of the objectives and methodology of the same receiving a letter of explanation and a term of free and informed consent to be read and signed. After this, the researcher carried out a questionnaire (Figure 1), where information were collected as: identification of the worker, working time in current role and this company, work history in other companies with exposure to noise, use of protective headset, stunted and current diseases, medication use, symptom of tinnitus and intolerance to loud sounds, type of tobacco, amount and time of use, as well as extra-occupational exposure to loud sounds.
After the questionnaire, inspection of the external auditory canal was performed to exclude patients with presence of cerumen or any abnormality that could mischaracterize the research objective. Subjects with any of these characteristics were duly referred to the ENT.
Moreover, were exclusion criteria for research: conductive or mixed hearing loss, profound hearing loss or deafness, mellittus diabetes, hypertension, and previous work with solvent and / or pesticides.
Individuals who did not have any criteria for exclusion, underwent pure tone audiometry at frequencies from 250Hz to 8kHz. Search bone conduction at frequencies between 500Hz and 4kHz and speech audiometry tests with Speech Reception Threshold (SRT) and Speech Recognition Index (SRI) were performed when the thresholds were not within the normal range (below 25dBNA). The equipment used for application of the test was 259 Interacoustics audiometer and also audiometric booth Vibrasom VSA50, both subject to the annual electroacoustic calibration.
Induced hearing loss (NIHL) were those in which auditory thresholds at 3 and / or 4 and / or 6KHz were above 25 dB HL, and higher than other tested frequencies, whether altered or not, both air conduction test as in bone conduction test, on one or both sides1515 . Ministério do Trabalho e Emprego. Portaria nº19, de 09/04/1998 – Diretrizes e Parâmetros Mínimos para Avaliação e Acompanhamento da Audição em Trabalhadores Expostos a Níveis de Pressão Sonora Elevados. Brasília, Ministério do Trabalho, 1998..
Regarding the statistical analysis, quantitative variables (thresholds) were described by median and interquartile range, by presenting skewed distribution. Qualitative variables (other) were described by absolute and relative frequencies.
To compare the hearing thresholds between groups, the Mann-Whitney test was used. Ever, to evaluate the association between qualitative variables, the Pearson’s chi-square test was applied. In case of statistical significance, the test set of residues was calculated to aid in locating associations.
In order to control for possible confounding factors (age and total exposure time), Analysis of Covariance (ANCOVA) was used to assess the association between smoking and hearing thresholds. As these thresholds showed an asymmetric distribution, the square root transformation was applied to the raw data to be possible to perform the ANCOVA data.
The level of significance was set at 5% (p ≤ 0.05), and analyzes were performed using SPSS (Statistical Package for Social Sciences) 18.0 program.
RESULTS
The sample consisted of 153 workers with female predominance (60.9%), aged between 21 and 40 years (68.0%) being allocated most of the gutting and shipping sectors (45.1%). The prevalence of smokers or ex-smokers in the sample was 20.9% (32/153). Regarding the distribution of smokers and non-smokers were similar between men and women, age groups and industry (Table 1).
The association between smoking and the variables related to the total time of noise exposure and hearing problems was presented in Table 2.
The total exposure time to the noise and the smoke had statistically significant association (p = 0.016). The group of smokers / ex-smokers had significantly longer total exposure, especially between 10 and 15 years.
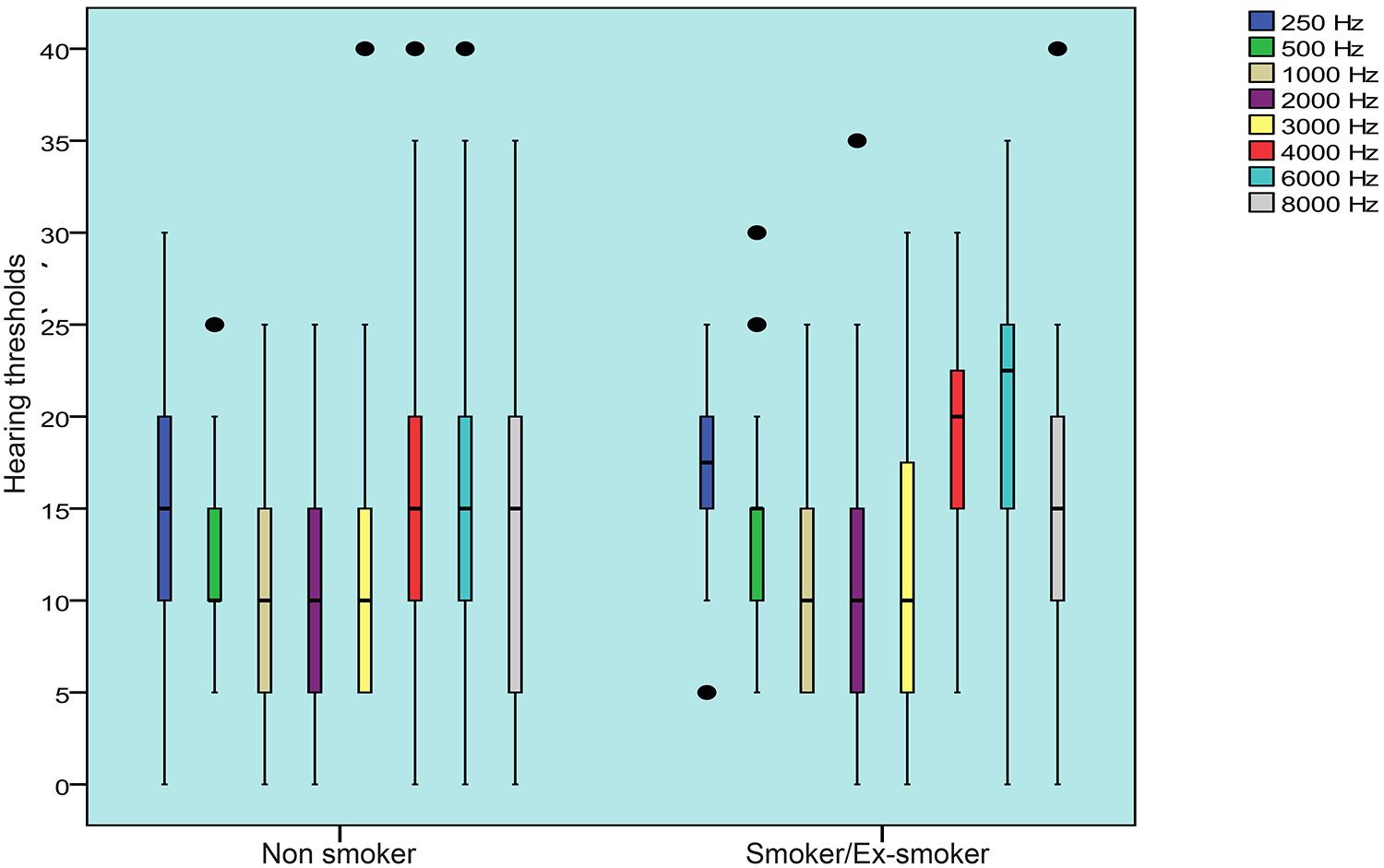
The relation between the smoking and the audiometry was shown in Table 3. Hearing thresholds of air conduction at frequencies 4,000 Hz and 6,000 Hz were significantly higher in the group of smokers / ex-smokers compared to nonsmokers both in the right ear (p = 0.034 and p = 0.018, respectively) and the left ear (p = 0.021 and 0.001, respectively). These differences remained significant after adjustment for age and time of exposure. In addition, a new statistical difference appeared after the adjustment, the frequency of 250Hz in the right ear. Thus one can say that the statistical association found between smoking and hearing thresholds, plotted in Figures 2 and 3, was independent of age and duration of exposure.
– Evaluation of hearing thresholds of the right ear at each frequency, by study group. The central line represents the median and the lower and upper limits of the box represent the 25 and 75 percentiles, respectively. The error bars represent the minimum and maximum values.
– Evaluation of hearing thresholds of the left ear at each frequency, by study group. The central line represents the median and the lower and upper limits of the box represent the 25 and 75 percentiles, respectively. The error bars represent the minimum and maximum values.
DISCUSSION
Based on the results it can be seen that the most of the sample (45.1%) of survey exercised its functions in evisceration and shipping sectors, presenting noise level equal to 88 and 91 dBA respectively. Despite the noise levels to 85dBA recommended in these sectors overcome, they are still below those found in other sectors of the company, where it was possible to observe levels of up to 109dB.
Some authors claim that the intensity of the noise seems to be the main risk factor for hearing loss, regardless of the frequency band1616 . Boger ME, Barbosa-Branco A, Ottoni AC. A influência do espectro de ruído na prevalência de perda auditiva induzida por ruído em trabalhadores. Braz J Otorhinolaryngol. 2009;75(3):328-34..
According to Regulatory Norm 15, a worker may not be exposed to a level exceeding 85 dBA noise 8 hours of work, in that case need to make use of hearing protectors1515 . Ministério do Trabalho e Emprego. Portaria nº19, de 09/04/1998 – Diretrizes e Parâmetros Mínimos para Avaliação e Acompanhamento da Audição em Trabalhadores Expostos a Níveis de Pressão Sonora Elevados. Brasília, Ministério do Trabalho, 1998.. This may explain the fact that in both groups was altered thresholds (above 25 dBA), since non-smokers also remain exposed to loud noises.
Actually, the ideal would be to reduce the noise source and implement the use of protectors since for the usage to be effective, there is need for education and training of employees continuously1717 . Gonçalves CGO, Couto CM, Carraro JM, Leonelli BS. Avaliação da colocação de protetores auriculares em grupos com e sem treinamento. Rev. CEFAC. 2009;11(2):345-52., as well as supervision of their use by checking the effectiveness of training conducted. Where it is not possible to reduce noise in the sound source, it is necessary the use of protectors. A recent study has shown effectiveness in educational activities training on the use of protectors to employees exposed to occupational noise, if well implemented1818 . Rocha CH, Santos SHD, Moreira RR, Neves-Lobo IF, Samelli AG. Verificação da efetividade de uma ação educativa sobre proteção auditiva para trabalhadores expostos a ruído. J Soc Bras Fonoaudiol. 2011;23(1):38-42..
By relating the results of audiometry with the use or nonuse of tobacco, it was noted that in the group of smokers/ex-smokers there was a significant increase in hearing thresholds of air conduction for frequencies of 4 and 6kHz, which define and characterize hearing loss as induced noise1515 . Ministério do Trabalho e Emprego. Portaria nº19, de 09/04/1998 – Diretrizes e Parâmetros Mínimos para Avaliação e Acompanhamento da Audição em Trabalhadores Expostos a Níveis de Pressão Sonora Elevados. Brasília, Ministério do Trabalho, 1998.. Despite smokers/ex-smokers do not exercise their functions in higher noise level sectors, have worse hearing thresholds for the frequencies that indicate NIHL.
A study conducted in 2005 in Japan with 2267 individuals corroborates the information found in this study, which found a significant increase in hearing thresholds in the frequency of 4 kHz in smokers compared to nonsmokers1212 . Uchida Y, Nakashima T, Ando F, Niino N, Shimokata H. Is there a relevant effect of noise and smoking on hearing? A population-based aging study. International Journal of Audiology. 2005;44:86-91..
Another study conducted in Brazil in 2009 with smokers and non-smokers, found
that the group of smokers had worse hearing thresholds at high frequencies
(12500 and 14000Hz) and worst level of otoacoustic emissions in response to the
frequency of 4 kHz in left ear, and a higher number of cases with cochlear
dysfunction1010 . Paschoal CP, Azevedo MF. O cigarro como um fator de risco para
alterações auditivas. Braz. j. otorhinolaryngol.
2009;75(6):893-902.. Some
authors suggest the use of transient evoked otoacoustic emissions in order to
identify minimal cochlear changes in individuals exposed to noise associated
with other risk factors for hearing loss, preventing damage to the hearing
system1919 . Oliveira PF, Raposo OFF, Santos ACA, Santos LA. Emissões
otoacústicas como instrumento de vigilância epidemiológica na saúde do
trabalhador. Arquivos Int. Otorrinolaringol. 2011;15(4):444-9.
20 . Coelho MSB, Ferraz JRS, Almeida EOC, Almeida Filho N. As emissões
otoacústicas no diagnóstico diferencial das perdas auditivas induzidas por
ruído. Rev. CEFAC. 2010;12(6):1050-8.-2121 . Ramos N, Aita ADC, Siqueira LP, Aita FS. O uso das emissões
otoacústicas como ferramenta auxiliar no diagnóstico de efeitos da exposição ao
ruído. Rev. bras. Saúde ocup. 2011;(124):282-7..
This study indicates that not just the use of hearing protection to prevent hearing loss, if any associated risk factors. In addition to the existing awareness against smoking campaigns, realizes the need for campaigns by employers in order to guide individuals to the hazards of tobacco use, not only the well known and as commented on by the media, but also hearing losses. Perhaps it’s necessary a more specific training more careful monitoring for those employees who take other risk than that which is already given, in the case, the noise.
Although the results of this study suggest a relationship between tobacco use and noise-induced hearing loss, it should be noted that he has a subjective character, since it does not take into consideration the time and amount of tobacco used by the worker, and even it was observed, would not be possible to measure the amount of nicotine and carbon monoxide absorbed by the individual. Perhaps a study with a larger population of smokers (with duration of use and amount of smoke approximate) exposed and not exposed to noise could help to clarify the issue.
CONCLUSION
This study suggests that tobacco use may potentiate damage to hearing caused by noise, worsening cases of NIHL, since the group of smokers/ex-smokers showed greater injury in the characteristic frequencies.
REFERÊNCIAS
-
1Ministério da Saúde do Brasil. Doenças relacionadas ao trabalho: manual de procedimentos para os serviços de saúde. Brasília: Ministério da Saúde do Brasil, 2001.
-
2Seligman J. Sintomas e sinais na PAIR. In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997.
-
3Lobo R, Costa EA. Classificação das perdas auditivas induzidas pelo ruído. In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997.
-
4Morata TC, Dunn, DE, Sieber, WK. Perda auditiva e a exposição ocupacional a agentes ototóxicos. . In: Nudelmann AA, Costa, EA, Ibañez RN, Seligman, J. PAIR: perda auditiva induzida por ruído. Porto Alegre: Bagabbem Comunicação, 1997.
-
5Botelho CT, Paz APML, Gonçalves AM, Frota S. Estudo comparativo de exames audiométricos de metalúrgicos expostos a ruído e ruído associado a produtos químicos. Rev. Bras. Otorrinolaringol. 2009;75(1):51-7.
-
6Teixeira CF, Augusto LGS, Morata TC. Saúde auditiva de trabalhadores expostos a ruído e inseticidas. Rev. Saúde Pública. 2003;37(4):417-23.
-
7Lacerda A, Leroux T, Morata TC. Efeitos ototóxicos da exposição ao monóxido de carbono: uma revisão. Pró-Fono R. Atual. Cient. 2005;17(3):403-12.
-
8Protocolos de procedimentos médico-periciais de doenças profissionais e do trabalho: subsídios para a implementação do anexo II do CRETO 3.048/99 pelo INSS. Informativo ANAMT (Associação Nacional de Medicina do Trabalho) nº10 vol. 2 – fevereiro de 2000.
-
9Fernandes M, Morata TC. Estudo dos efeitos auditivos e extra-auditivos da exposição ocupacional a ruído e vibração. Rev. Bras. Otorrinolaringol. 2002;68(5): 705-13.
-
10Paschoal CP, Azevedo MF. O cigarro como um fator de risco para alterações auditivas. Braz. j. otorhinolaryngol. 2009;75(6):893-902.
-
11Mohammadi S, Mazhari MM, Mehrparvar AH, Attarchi MS. Effect of simultaneous exposure to occupational noise and cigarette smoke on binaural hearing impairment. Noise Health. 2010;12(48):187-90.
-
12Uchida Y, Nakashima T, Ando F, Niino N, Shimokata H. Is there a relevant effect of noise and smoking on hearing? A population-based aging study. International Journal of Audiology. 2005;44:86-91.
-
13Angrisani RMG, Matas CG, Furtado JRB. Análise dos potenciais evocados auditivos em fumantes. Acta ORL. 2010;26(3):140-208.
-
14Azevedo RCS, Higa CMHi, Assumpção ISAM, Fernandes RF, Boscolo MM, Frazatto CRG. Atenção aos tabagistas pela capacitação de profissionais da rede pública. Rev. Saúde Pública. 2008;42(2):353-5.
-
15Ministério do Trabalho e Emprego. Portaria nº19, de 09/04/1998 – Diretrizes e Parâmetros Mínimos para Avaliação e Acompanhamento da Audição em Trabalhadores Expostos a Níveis de Pressão Sonora Elevados. Brasília, Ministério do Trabalho, 1998.
-
16Boger ME, Barbosa-Branco A, Ottoni AC. A influência do espectro de ruído na prevalência de perda auditiva induzida por ruído em trabalhadores. Braz J Otorhinolaryngol. 2009;75(3):328-34.
-
17Gonçalves CGO, Couto CM, Carraro JM, Leonelli BS. Avaliação da colocação de protetores auriculares em grupos com e sem treinamento. Rev. CEFAC. 2009;11(2):345-52.
-
18Rocha CH, Santos SHD, Moreira RR, Neves-Lobo IF, Samelli AG. Verificação da efetividade de uma ação educativa sobre proteção auditiva para trabalhadores expostos a ruído. J Soc Bras Fonoaudiol. 2011;23(1):38-42.
-
19Oliveira PF, Raposo OFF, Santos ACA, Santos LA. Emissões otoacústicas como instrumento de vigilância epidemiológica na saúde do trabalhador. Arquivos Int. Otorrinolaringol. 2011;15(4):444-9.
-
20Coelho MSB, Ferraz JRS, Almeida EOC, Almeida Filho N. As emissões otoacústicas no diagnóstico diferencial das perdas auditivas induzidas por ruído. Rev. CEFAC. 2010;12(6):1050-8.
-
21Ramos N, Aita ADC, Siqueira LP, Aita FS. O uso das emissões otoacústicas como ferramenta auxiliar no diagnóstico de efeitos da exposição ao ruído. Rev. bras. Saúde ocup. 2011;(124):282-7.
Publication Dates
-
Publication in this collection
Mar-Apr 2014
History
-
Received
16 May 2012 -
Accepted
04 Feb 2013