Abstracts
OBJECTIVE: There is increasing evidence that the symptoms of obsessive-compulsive disorder lie on discrete dimensions. Relatively little work has, however, explored the relationship between such factors and response to pharmacotherapy. METHOD: Data from a multi-site randomized placebo-controlled study of citalopram in obsessive-compulsive disorder were analyzed. Factor analysis of individual items and symptom categories of the Yale-Brown Obsessive-Compulsive Scale Checklist were undertaken, and the impact of symptom dimensions on treatment outcomes was analysed. RESULTS: Factor analysis of Yale-Brown Obsessive-Compulsive Scale Checklist individual items yielded 5 factors (contamination/cleaning, harm/checking, aggressive/sexual/religious, hoarding/symmetry, and somatic/hypochondriacal). Hoarding/symmetry was associated with male gender, longer duration of obsessive-compulsive disorder and early onset, whereas contamination/cleaning was associated with female gender. Citalopram was more effective than placebo, but high scores on the symmetry/hoarding and contamination/cleaning subscales predicted worse outcome at the end of study while high scores on the aggressive/religious/sexual subscale predicted better outcome. Factor analysis of Yale-Brown Obsessive-Compulsive Scale Checklist symptom clusters yielded a 4 factor solution, but confirmed that symmetry/ordering was associated with male gender, early onset, and long duration of obsessive-compulsive disorder while high scores on the hoarding subscale predicted worse response to pharmacotherapy. CONCLUSION: Citalopram shows good efficacy across the range of obsessive-compulsive disorder symptom dimensions. The relatively worse response of symmetry/hoarding to a selective serotonin reuptake inhibitor is consistent with other evidence that this symptom dimension is mediated by the dopamine system. There may be associations between symmetry/hoarding, male gender, early onset, tics, and particular genetic variants; further work is, however, needed to delineate fully obsessive-compulsive disorder subtypes and their underlying neurobiology.
Obsessive-compulsive disorder; Yale-Brown Obsessive-Compulsive Scale; Citalopram; Serotonin; Serotonin uptake inhibitors
OBJETIVO: Há crescentes evidências de que os sintomas do transtorno obsessivo-compulsivo residem em dimensões discretas. Alguns estudos têm sugerido que esses fatores possuem suportes neurobiológicos específicos. No entanto, poucos trabalhos têm explorado a relação entre tais fatores e a resposta à farmacoterapia. MÉTODO: Foi realizada a análise fatorial dos itens individuais e categorias de sintomas do checklist da Escala de Obsessão e Compulsão de Yale-Brown e foi analisado o impacto da dimensão dos sintomas no desfecho dos tratamentos. RESULTADOS: A análise fatorial exploratória dos itens individuais da Escala de Obsessão e Compulsão de Yale-Brown produziu cinco fatores (contaminação/limpeza, dano/verificação, agressividade/sexual/religioso, colecionismo/simetria e somático/hipocondríaco). Colecionismo/simetria foi associado ao sexo masculino, longa duração do transtorno obsessivo-compulsivo e início precoce, ao passo que contaminação/limpeza foi associado ao sexo feminino. O citalopram foi mais eficaz do que placebo, mas altos escores nas subescalas de simetria/colecionismo e de contaminação/limpeza predisseram desfecho pior ao final do estudo, ao passo que altos escores na subescala agressividade/sexual/religioso predisseram melhor desfecho. Uma análise fatorial de sintomas do checklist da Escala de Obsessão e Compulsão de Yale-Brown produziu uma solução com quatro fatores, mas confirmou que simetria/ordenação estava associado ao sexo masculino, início precoce e longa duração do transtorno obsessivo-compulsivo, enquanto altos escores na subescala colecionismo predisseram uma resposta pior à farmacoterapia. CONCLUSÃO: O citalopram demonstra boa eficácia ao longo das dimensões do espectro de sintomas do transtorno obsessivo-compulsivo. A resposta relativamente pior de simetria/colecionismo a um inibidor seletivo da recaptação da serotonina é consistente com outras evidências de que essa dimensão de sintomas é mediada pelo sistema dopaminérgico. Pode haver associações entre simetria/colecionismo, sexo masculino, início precoce, tiques e variantes genéticas específicas; porém, mais estudos são necessários para delinear completamente os subtipos de transtorno obsessivo-compulsivo e sua neurobiologia subjacente.
Transtorno obsessivo-compulsivo; Yale-Brown Obsessive-Compulsive Scale; Citalopram; Serotonina; Inibidores de captação de serotonina
ORIGINAL ARTICLE
Response of symptom dimensions in obsessive-compulsive disorder to treatment with citalopram or placebo
Resposta das dimensões dos sintomas no transtorno obsessivo-compulsivo ao tratamento com citalopram ou placebo
Dan J SteinI,II; Elisabeth W AndersenIII; Kerstin Fredricson OveroIII
IUniversity of Cape Town, Cape Town, South Africa
IIMt. Sinai School of Medicine, New York, USA
IIIH. Lundbeck A/S, Copenhagen
Correspondence Correspondence: Dan J. Stein UCT Dept of Psychiatry, Groote Schuur Hospital J-2 Anzio Rd, Observatory 7925 Cape Town, South Africa E-mail: dan.stein@uct.ac.za
ABSTRACT
OBJECTIVE: There is increasing evidence that the symptoms of obsessive-compulsive disorder lie on discrete dimensions. Relatively little work has, however, explored the relationship between such factors and response to pharmacotherapy.
METHOD: Data from a multi-site randomized placebo-controlled study of citalopram in obsessive-compulsive disorder were analyzed. Factor analysis of individual items and symptom categories of the Yale-Brown Obsessive-Compulsive Scale Checklist were undertaken, and the impact of symptom dimensions on treatment outcomes was analysed.
RESULTS: Factor analysis of Yale-Brown Obsessive-Compulsive Scale Checklist individual items yielded 5 factors (contamination/cleaning, harm/checking, aggressive/sexual/religious, hoarding/symmetry, and somatic/hypochondriacal). Hoarding/symmetry was associated with male gender, longer duration of obsessive-compulsive disorder and early onset, whereas contamination/cleaning was associated with female gender. Citalopram was more effective than placebo, but high scores on the symmetry/hoarding and contamination/cleaning subscales predicted worse outcome at the end of study while high scores on the aggressive/religious/sexual subscale predicted better outcome. Factor analysis of Yale-Brown Obsessive-Compulsive Scale Checklist symptom clusters yielded a 4 factor solution, but confirmed that symmetry/ordering was associated with male gender, early onset, and long duration of obsessive-compulsive disorder while high scores on the hoarding subscale predicted worse response to pharmacotherapy.
CONCLUSION: Citalopram shows good efficacy across the range of obsessive-compulsive disorder symptom dimensions. The relatively worse response of symmetry/hoarding to a selective serotonin reuptake inhibitor is consistent with other evidence that this symptom dimension is mediated by the dopamine system. There may be associations between symmetry/hoarding, male gender, early onset, tics, and particular genetic variants; further work is, however, needed to delineate fully obsessive-compulsive disorder subtypes and their underlying neurobiology.
Descriptors: Obsessive-compulsive disorder; Yale-Brown Obsessive-Compulsive Scale; Citalopram; Serotonin; Serotonin uptake inhibitors
RESUMO
OBJETIVO: Há crescentes evidências de que os sintomas do transtorno obsessivo-compulsivo residem em dimensões discretas. Alguns estudos têm sugerido que esses fatores possuem suportes neurobiológicos específicos. No entanto, poucos trabalhos têm explorado a relação entre tais fatores e a resposta à farmacoterapia.
MÉTODO: Foi realizada a análise fatorial dos itens individuais e categorias de sintomas do checklist da Escala de Obsessão e Compulsão de Yale-Brown e foi analisado o impacto da dimensão dos sintomas no desfecho dos tratamentos.
RESULTADOS: A análise fatorial exploratória dos itens individuais da Escala de Obsessão e Compulsão de Yale-Brown produziu cinco fatores (contaminação/limpeza, dano/verificação, agressividade/sexual/religioso, colecionismo/simetria e somático/hipocondríaco). Colecionismo/simetria foi associado ao sexo masculino, longa duração do transtorno obsessivo-compulsivo e início precoce, ao passo que contaminação/limpeza foi associado ao sexo feminino. O citalopram foi mais eficaz do que placebo, mas altos escores nas subescalas de simetria/colecionismo e de contaminação/limpeza predisseram desfecho pior ao final do estudo, ao passo que altos escores na subescala agressividade/sexual/religioso predisseram melhor desfecho. Uma análise fatorial de sintomas do checklist da Escala de Obsessão e Compulsão de Yale-Brown produziu uma solução com quatro fatores, mas confirmou que simetria/ordenação estava associado ao sexo masculino, início precoce e longa duração do transtorno obsessivo-compulsivo, enquanto altos escores na subescala colecionismo predisseram uma resposta pior à farmacoterapia.
CONCLUSÃO: O citalopram demonstra boa eficácia ao longo das dimensões do espectro de sintomas do transtorno obsessivo-compulsivo. A resposta relativamente pior de simetria/colecionismo a um inibidor seletivo da recaptação da serotonina é consistente com outras evidências de que essa dimensão de sintomas é mediada pelo sistema dopaminérgico. Pode haver associações entre simetria/colecionismo, sexo masculino, início precoce, tiques e variantes genéticas específicas; porém, mais estudos são necessários para delinear completamente os subtipos de transtorno obsessivo-compulsivo e sua neurobiologia subjacente.
Descritores: Transtorno obsessivo-compulsivo; Yale-Brown Obsessive-Compulsive Scale; Citalopram; Serotonina; Inibidores de captação de serotonina
Introduction
Obsessive-compulsive disorder (OCD) is in many ways a homogeneous disorder. The disorder has a prevalence of around 2% in many different countries,1 and descriptions of obsessions and compulsions have been remarkably consistent over time and place.2 Neurobiological studies have consistently found evidence that cortical-striatal-thalamic-cortical (CTSC) circuits play a crucial role in mediating the disorder,3 and treatment research has invariably demonstrated that serotonin reuptake inhibitors selectively reduce the symptoms of OCD.4
At the same time, there is growing recognition that OCD is a heterogeneous condition.5 There are different types of OCD symptoms (e.g.: washing vs checking), and OCD patients differ markedly in their severity of symptoms, degree of insight, and patterns of comorbidity. In some OCD patients the neural substrate of symptoms may include regions other than the CSTC circuits.6 Although selective serotonin reuptake inhibitors (SSRIs) are the pharmacotherapy of choice, only around 40-60% of OCD patients respond to these agents, a source of variation that remains incompletely understood. Another 50% of patients respond to augmentation of SSRIs with low doses of antipsychotics.7
Much work attempting to dissect the dimensions of OCD has been limited by not including different symptom subtypes,8-12 or by using restricted symptom scales.13-15 The Yale-Brown Obsessive-Compulsive Scale (Y-BOCS) is a clinician-rated measure that has become the most widely used primary efficacy measure in OCD medication trials, and includes a checklist of symptoms which is more comprehensive than the items of earlier scales. Factor analyses of the individual items, or of the symptom clusters, in the Y-BOCS checklist have consistently found 3 to 5 major factors, namely contamination/cleaning, aggressive/checking, symmetry/ordering, and hoarding symptoms.16,17-22
There is preliminary evidence that these OCD symptom dimensions are associated with different neuronal substrates23 and with different genetic variants.21 Some studies have suggested that washing symptoms do better with exposure therapy,24,25 and worse with serotonin reuptake inhibitors,26,27 although not all work is consistent. There is also evidence that hoarding symptoms are associated with worse response to treatment with serotonin reuptake inhibitors.20,28 Although there have been many multi-site placebo-controlled studies of the pharmacotherapy of OCD, few of these have reported whether symptom factors influence treatment outcome. In this paper we analyzed a trial of the highly selective serotonin reuptake inhibitor (SSRI), citalopram, versus placebo, in order to determine whether symptom factors significantly determined response to medication or placebo.
Method
1. Clinical trial
The trial on which the analysis is based has been previously described in detail.29 In brief, the study was a double-blind, placebo-controlled, parallel-group, fixed dose study conducted at 53 centers in 12 countries. Patients were 18-65 years and had been diagnosed according to DSM-IV criteria as suffering from OCD for at least 12 months. Age of onset of OCD was determined by clinical history.
Patients with mild depressive symptoms could be included in the study [total MADRS (Montgomery-Åsberg Depression rating scale) score d 22], but patients with moderate to severe depression and a range of other comorbid psychiatric or general medical disorders, including Tourette's syndrome, were excluded. Investigators received training on the Y-BOCS at a start-up meeting prior to the study, in order to ensure interrater reliability. The protocol was approved by the institutional review boards of the participating investigators, and subjects gave informed written consent.
Patients were randomly assigned to receive fixed daily oral doses of 20, 40 or 60 mg citalopram or placebo for 12 weeks following a 1-week run-in period. At screening, patients received the Y-BOCS symptom checklist, and at baseline and at weeks 1, 3, 5, 7, 9, and 12 OCD symptom severity was assessed using the Y-BOCS. The primary measure of efficacy was change from baseline on the Y-BOCS total score at week 12. As significant effects for citalopram were demonstrated at all doses, the citalopram data were pooled for the current analysis.
2. Statistical analysis
An exploratory factor analysis was performed on the individual symptoms from the Y-BOCS checklist (using all available patients, n = 434). A score of 2 was given if the symptom was a principal one, a score of 1 was given if the symptom was present, and otherwise 0 was given.20 As in previous factor analyses of the Y-BOCS checklist only the current symptoms were used and the two categories 'other obsessions' and 'other compulsions' were not included.16,17
Maximum likelihood was used for factor identification as this method is independent of the scales of measurement and allows comparison of factor solutions using objective criteria.30 Extracted factors were rotated using the varimax orthogonal rotation in order to ease interpretation of the results. Based on these factors, subscale scores were determined by adding the individual scores of the relevant items. As each scale consisted of a different number of items, subscale scores were standardized in terms of z-scores.
The distribution of subscale scores was compared in males and females, in patients with OCD duration more or less than 10 years, and in early (before age 15) versus late onset OCD (using the Wilcoxon two-sample test). A general linear model was used to predict the response of OCD (as measured by the Y-BOCS at endpoint), including the covariate Y-BOCS score at baseline, the factors age at onset, duration of OCD, gender, country, treatment, and the five subscale scores. The five interactions between treatment and subscale scores were also included in order to determine whether inclusion of subscale scores impacted on the efficacy of citalopram versus placebo.
Finally, given that a number of previous factor analyses have focused on the 13 main categories of symptoms in the Y-BOCS Checklist, an exploratory factor analysis was undertaken using these symptom categories, and the analysis of response to citalopram was repeated.
Results
The major symptom categories were tabulated and the most common symptoms were aggressive, contamination and symmetry obsessions, and cleaning, checking, and repeating compulsions (Table 1). In the factor analysis, Kaiser's measure of sampling adequacy (MSA) was 0.75; this is usually considered good if larger than 0.8 and unacceptable if under 0.5. A scree plot suggested that a 5-factor model was reasonable as the plot began to level out after the first five values, and using Akaike's information criteria the 5-factor model gave the best fit.
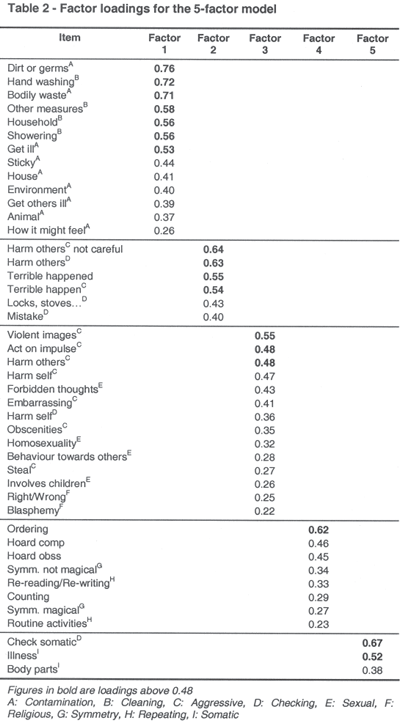
The factor loadings were tabulated (Table 2), with symptoms assigned to a factor according to the highest loading. On the basis of their component items the five factors could be labeled: factor 1 - contamination/cleaning, factor 2 - harm/checking, factor 3 - aggressive/sexual/religious, factor 4 - hoarding/symmetry, and factor 5 - somatic/hypochondriacal.
Distribution of subscale scores differed by gender, OCD duration and age of onset. Contamination/ cleaning subscale scores were higher in women [mean 5.57 (SD = 5.33)] than in men [4.54 (5.07), p = 0.0323], while hoarding/symmetry subscale scores were higher in men [4.17 (3.26)] than in women [3.25 (2.74), p = 0.0069]. The hoarding/symmetry subscale was higher in early onset (d 15 years) OCD patients [4.12 (2.89)] than in the patients with later onset [3.45 (3.05), p = 0.0088], and this subscale also was higher in patients with a long (more than 10 years) duration of OCD [4.00 (2.98)] compared to patients with a shorter duration [3.24 (2.99), p = 0.0035].
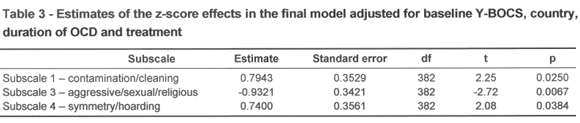
Patients with a post-baseline evaluation were included in the general linear model (n = 401). The final model for Y-BOCS score at end of study included the variables Y-BOCS score at baseline, country, duration of OCD, treatment and three of the subscales: contamination/cleaning, aggressive/forbidden and symmetry/hoarding (Table 3). High scores on the contamination/cleaning subscale and the hoarding/symmetry subscale predicted worse outcome at the end of the study while high scores on the aggressive/sexual/religious subscale predicted better results at the end of the study. Nevertheless, citalopram was still significantly superior to placebo in reducing Y-BOCS scores and there was no significant subscale by treatment interaction (that is, the subscales did not express significantly different effects in the two treatment groups). The interaction between hoarding/symmetry and treatment was the closest to becoming statistically significant (p = 0.0782) with an adjusted estimate in the placebo treated group of -0.17 (0.63) and in the citalopram treated group 1.13 (0.42). This shows a tendency for the patients with high scores on the hoarding/symmetry subscale to have worse response to treatment with citalopram.
The exploratory factor analysis of the Y-BOCS symptom clusters demonstrated that Kaiser's measure of sampling adequacy was 0.58, a result that is acceptable but which suggests that ideally more categories should be included in the identification of underlying factors. A scree plot of eigenvalues showed that the plot leveled out after the first 4 values. A 4-factor model yielded high factor loadings for hoarding, contamination/cleaning, symmetry/ordering, and aggressive/checking symptoms. Somatic symptoms fell on the contamination factor, where they had a relatively small loading.
Using four subscales based on the exploratory analysis of the symptom clusters, an attempt was made to replicate the main findings of the analyses based on exploratory factor analysis of individual Y-BOCS checklist items. Symmetry/ordering subscale scores were higher in men (p = 0.0063), in patients with long duration of OCD (p = 0.0077) and in early onset patients (p = 0.0143). The results of the general linear model were very similar to the results from the analysis using the subscales based on the items of the checklist. The main difference was a statistically significant interaction between treatment and the hoarding subscale indicating worse response to treatment for patients with a high score on the hoarding subscale.
Discussion
The frequencies of the major symptom categories of OCD reported here are similar to those recorded in previous studies. Furthermore, the 5-factor model is similar to that described in a previous investigation that also focused on individual Y-BOCS items19 as well as to a 5-factor model based on a factor analysis of the symptom clusters of the Y-BOCS Checklist.20 In the work by Feinstein et al. sexual obsessions rather somatic symptoms were a separate factor, while in the work of Mataix-Cols et al. hoarding was a separate factor.19,20 These relatively small differences are not surprising given that such symptoms are comparatively uncommon; taken together, the literature indicates that similar frequencies of OCD symptoms and similar symptom dimensions are present across a range of different OCD patient populations.
Previous studies have relied on either factor analysis of individual items or of symptoms clusters. Kaiser's measure of sampling adequacy was higher in the exploratory factor analysis of individual items than in that of symptom clusters, consistent with the argument that analysis at the level of individual items demonstrates the heterogeneity of the Y-BOCS symptom clusters. Checking, for example, includes both items related to harm avoidance and items related to undesirable impulsive acts.18 Thus, in some work based on analysis of Y-BOCS symptom clusters checking lies on the same factor as contamination,17 whereas in other studies it is grouped together with aggressive and sexual obsessions.16 Future scoring of the Y-BOCS might benefit from calculating separate summary scores for different factors based on individual items.
The relatively worse response of the hoarding/symmetry subscale to a SSRI is consistent with some previous data20,28 (but not all31), and with other evidence that this symptom dimension is mediated by the dopamine system. Animal models demonstrate that the dopaminergic system plays a key role in hoarding,32 and hoarding/symmetry symptoms are more common in patients with comorbid tic disorders17,20 which are characterized by dopaminergic dysfunction. Although patients with Tourette's disorder were excluded from the current study, it is possible that patients with motor tics alone were included. In support of a dopaminergic hypothesis of symmetry/hoarding, Jenike et al. have reported that symmetry, ordering, hoarding and unusual somatic symptoms were significantly more common in patients who responded to the monoamine oxidase inhibitor (MAOI) phenelzine than to the SSRI fluoxetine.33 Another study found that symmetry, ordering and hoarding symptoms predicted a better response in patients treated with cingulotomy.34
Previous literature has noted associations between early onset OCD, male gender, comorbid tics, and worse outcome,5 and between symmetry/ordering symptoms, male gender, and tics.20 The data here replicates the finding of Mataix-Cols et al. that symmetry/ordering symptoms are more common in males, while contamination/cleaning symptoms are more common in females. The precise interaction between these different variables requires further study; it is possible that genetic factors contribute to the inheritance of symmetry/ordering symptoms or hoarding,35-37 and that this pattern of inheritance is particularly associated with male gender, early onset, and comorbid tics.38
Several limitations of the current secondary analysis should be emphasized. In particular, OCD subjects who qualify for a clinical trial may not be representative of typical patients with this disorder. Patients in the citalopram trials did not have comorbid disorders including tic disorders, and were required to have a minimum score on the Y-BOCS. Thus both more severe subjects and subjects with more limited OCD symptoms were excluded from the analysis. This study was powered to determine the efficacy of citalopram in OCD, rather than its efficacy for particular symptom dimensions.
Although some previous factor analyses have included past symptoms,16 this approach may obscure the extent to which symptoms and symptom dimensions evolve over time.39 Conversely, however, the current data are unable to address the stability of OCD symptom dimensions. Indeed, although it seems clear that OCD is a multidimensional disorder, further work to identify a comprehensive model of symptom structure is still needed. Such work may need to include analysis not only of obsessions and compulsions assessed by the Y-BOCS, but also of other common symptoms in OCD, such as manifestations of the obsessive-compulsive spectrum disorders (Lochner and Stein, 2006).
The database on which the current study was drawn has primarily been used to demonstrate the efficacy and safety of citalopram in the treatment of OCD.29 Secondary analyses of such multi-site datasets can, however, provide useful additional clinically relevant or hypothesis-generating information. A previous predictor analysis determined that subjects with longer duration of OCD, more severe OCD symptoms, or previous SSRI use were less likely to be responders. In contrast, subjects who received adequate medication doses for sufficient periods of time were more likely to be responders.40 The current analysis focused in particular on OCD symptom dimensions. Although citalopram was effective across different symptom subscales, the data here confirm that OCD is a heterogenous disorder. In particular, additional work is needed to determine the optimal treatment of OCD patients with hoarding/symmetry symptoms (which may in turn be associated with male gender, early onset, and tics).
Submitted: December 31, 2006
Accepted: August 19, 2007
Financing: The original study on which this work is based was funded by H. Lundbeck A/S. DJS has received honoraria and grants from, and EWA and KFA are employees of H. Lundbeck A/S.
Conflict of interests: Dr. Stein has received research grants and/or consultancy honoraria from Astrazeneca, Eli-Lilly, GlaxoSmithKline, Johnson & Johnson, Lundbeck, Orion, Pfizer, Pharmacia, Roche, Servier, Solvay, Sumitomo, Tikvah, and Wyeth
- 1. Weissman MM, Bland RC, Canino GJ, Greenwald S, Hwu HG, Lee CK, Newman SC, Oakley-Browne MA, Rubio-Stipec M, Wickramaratne PJ, Wittchen HU, Yeh EK. The cross national epidemiology of obsessive compulsive disorder. J Clin Psychiatry. 1994;55S:5-10.
- 2. Stein DJ, Rapoport JL. Cross-cultural studies and obsessive-compulsive disorder. CNS Spect 1996;1:42-6.
- 3. Rauch SL, Baxter LR Jr. Neuroimaging in obsessive-compulsive disorder and related disorders. In: Jenicke MA, Baer L, Minichiello WE. Obsessive-compulsive disorders: practical management 3rd ed. St. Louis, MI: Mosby, 1998.
- 4. Ackerman DL, Greenland S. Multivariate meta-analysis of controlled drug studies for obsessive-compulsive disorder. J Clin Psychopharmacol 2002;22(3):309-17.
- 5. Lochner C, Stein DJ. Heterogeneity of obsessive-compulsive disorder: a literature review. Harv Rev Psychiatry 2003;11(3):113-32.
- 6. Hugo F, van Heerden B, Zungu-Dirwayi N, Stein DJ. Functional brain imaging in obsessive-compulsive disorder secondary to neurological lesions. Depress Anxiety 1999;10(3):129-36.
- 7. McDougle CJ, Epperson CN, Pelton GH, Wasylink S, Price LH. A double-blind, placebo-controlled study of risperidone addition in serotonin reuptake inhibitor-refractory obsessive-compulsive disorder. Arch Gen Psychiatry 2000;57:794-802.
- 8. Fals-Stewart W. A dimensional analysis of the Yale-Brown Obsessive-Compulsive Scale. Psychol Rep 1992;70(1):239-40.
- 9. Moritz S, Meier B, Kloss M, Jacobsen D, Wein C, Fricke S, Hand I. Dimensional structure of the Yale-Brown Obsessive-Compulsive Scale (Y-BOCS). Psychiatry Res 2002;109(2):193-9.
- 10. McKay D, Danyko S, Neziroglu F, Yaryura-Tobias JA. Factor structure of the Yale-Brown Obsessive-Compulsive Scale: a two dimensional structure. Behav Res Ther 1995;33(7):865-9.
- 11. Arrindell WA, de Vlaming IH, Eisenhardt BM, van Berkum DE, Kwee MG. Cross-cultural validity of the Yale-Brown Obsessive Compulsive Scale. J Behav Ther Exp Psychiatry 2002;33(3-4):159-76.
- 12. Kim SW, Dysken MW, Pheley AM, Hoover KM. The Yale-Brown Obsessive-Compulsive Scale: measures of internal consistency. Psychiatry Res 1994;51(2):203-11.
- 13. Hodgson RJ, Rachman S. Obsessional-compulsive complaints. Behav Res Ther. 1977;15(5):389-95.
- 14. van Oppen P, Hoekstra RJ, Emmelkamp PM. The structure of obsessive-compulsive symptoms. Behav Res Ther 1995;33(1):15-23.
- 15. Sanavio E, Vidotto G. The components of the Maudsley Obsessional-Compulsive Questionnaire. Behav Res Ther 1985;23(6):659-62.
- 16. Leckman JF, Grice DE, Boardman J, Zhang H, Vitale A, Bondi C, Alsobrook J, Peterson BS, Cohen DJ, Rasmussen SA, Goodman WK, McDougle CJ, Pauls DL. Symptoms of obsessive-compulsive disorder. Am J Psychiatry 1997;154(7):911-7.
- 17. Baer L. Factor analysis of symptom subtypes of obsessive compulsive disorder and their relation to personality and tic disorders. J Clin Psychiatry 1994;55(Suppl):18-23.
- 18. Summerfeldt LJ, Richter MA, Antony MM, Swinson RP. Symptom structure in obsessive-compulsive disorder: a confirmatory factor-analytic study. Behav Res Ther 1999;37(4):297-311.
- 19. Feinstein SB, Fallon BA, Petkova E, Liebowitz MR. Item-by-item factor analysis of the Yale-Brown Obsessive compulsive symptom checklist. J Neuropsychiatry Clin Neurosci 2003;15(2):187-93.
- 20. Mataix-Cols D, Rauch SL, Manzo PA, Jenike MA, Baer L. Use of factor-analyzed symptom dimensions to predict outcome with serotonin reuptake inhibitors and placebo in the treatment of obsessive-compulsive disorder. Am J Psychiatry 1999;156(9):1409-16.
- 21. Cavallini MC, Di Bella D, Siliprandi F, Malchiodi F, Bellodi L. Exploratory factor analysis of obsessive-compulsive patients and association with 5-HTTLPR polymorphism. Am J Med Genet 2002;114(3):347-53.
- 22. Calamari JE, Wiegartz PS, Janeck AS. Obsessive-compulsive disorder subgroups: a symptom-based clustering approach. Behav Res Ther 1999;37(2):113-25.
- 23. Rauch SL, Dougherty D, Shin LM, Alpert NM, Manzo P, Leahy L, Fischman AJ, Jenike MA, Baer L. Neural correlates of factor-analyzed OCD symptom dimensions: a PET study. CNS Spect 1998;3:37-43.
- 24. Rachman S, Hodgson RJ. Obsessions and Compulsions Englewood-Cliffs, NJ: Prentice-Hall; 1980.
- 25. Buchanan AW, Ko SM, Marks IM. What predicts improvement and compliance during the behavioral treatment of obsessive compulsive disorder. Anxiety 1996;2(1):22-7.
- 26. Alarcon RD, Libb JW, Spitler D. A predictive study of obsessive-compulsive disorder response to clomipramine. J Clin Psychopharmacol 1993;13(3):210-3.
- 27. Ravizza L, Barzega G, Bellino S, Bogetto F, Maina G. Predictors of drug treatment response in obsessive-compulsive disorder. J Clin Psychiatry. 1995;56(8):368-73.
- 28. Black DW, Monahan P, Gable J, Blum N, Clancy G, Baker P. Hoarding and treatment response in 38 nondepressed subjects with obsessive-compulsive disorder. J Clin Psychiatry 1998;59(8):420-5.
- 29. Montgomery SA, Kasper S, Stein DJ, Bang Hedegaard K, Lemming OM. Citalopram 20mg, 40mg and 60mg are all effective and well tolerated compared with placebo in obsessive compulsive disorder. Int Clin Psychopharmacol 2001;16(2):75-86.
- 30. Krzanowski WJ. Principles of Multivariate Analysis. A User's Perspective Oxford Science Publications; 1993.
- 31. Saxena S, Brody AL, Maidment KM, Baxter LR Jr. Paroxetine treatment of compulsive hoarding. J Psychiatr Res 2007;41(6):481-7.
- 32. Stein D J, Seedat S, Potocnik F. Hoarding: a review. Isr J Psychiatry Relat Sci 1999;36(1):35-46.
- 33. Jenike MA, Baer L, Minichiello WE, Rauch SL, Buttolph ML. Placebo-controlled trial of fluoxetine and phenelzine for obsessive-compulsive disorder. Am J Psychiatry 1997;154(9):1261-4.
- 34. Baer L, Rauch SL, Ballantine HT, Martuza R, Cosgrove R, Cassem E, Giriunas I, Manzo PA, Dimino C, Jenike MA. Cingulotomy for intractable obsessive compulsive disorder: prospective long-term follow-up of 18 patients. Arch Gen Psychiatry 1995;52(5):384-92.
- 35. Zhang H, Leckman JF, Pauls DL, Tsai CP, Kidd KK, Campos MR; Tourette Syndrome Association International Consortium for Genetics. Genomewide scan of hoarding in sib pairs in which both sibs have Gilles de la Tourette syndrome. Am J Hum Genet 2002;70(4):896-904.
- 36. Lochner C, Kinnear CJ, Hemmings SM, Seller C, Niehaus DJ, Knowles JA, Daniels W, Moolman-Smook JC, Seedat S, Stein DJ. Hoarding in obsessive-compulsive disorder: clinical and genetic correlates. J Clin Psychiatry. 2005;66(9):1155-60.
- 37. Hasler G, Kazuba D, Murphy DL. Factor analysis of obsessive-compulsive disorder YBOCS-SC symptoms and association with 5-HTTLPR SERT polymorphism. Am J Med Genet B Neuropsychiatr Genet 2006;141(4):403-8.
- 38. Hemmings SM, Kinnear CJ, Lochner C, Niehaus DJ, Knowles JA, Moolman-Smook JC, Corfield VA, Stein DJ. Early- versus late-onset obsessive-compulsive disorder: investigating genetic and clinical correlates. Psychiatry Res 2004;128(2):175-82.
- 39. Rettew DC, Swedo SE, Leonard HL, Lenane MC, Rapoport JL. Obsessions and compulsions across time in 79 children and adolescents with obsessive-compulsive disorder. J Am Acad Child Adolesc Psychiatry 1992;31(6):1050-6.
- 40. Stein DJ, Montgomery SA, Kasper S, Tanghoj P. Predictors of response to pharmacotherapy with citalopram in obsessive-compulsive disorder. Int Clin Psychopharmacol 2001;16(6):357-61.
Publication Dates
-
Publication in this collection
10 Jan 2008 -
Date of issue
Dec 2007
History
-
Accepted
19 Aug 2007 -
Received
31 Dec 2006