Abstracts
OBJECTIVE: There is growing interest in the cognitive model of psychotherapy stimulated by an extensive body of research findings demonstrating its effectiveness for a varied set of psychiatric disorders and medical conditions. This review article aims to give an overview of the historical and philosophical background to contemporary cognitive and cognitive-behavioral approaches to psychotherapy, pointing out similarities across and differences between them. A presentation of the cognitive model as designed by Aaron Beck, and some of the cognitive and behavioral techniques used in emotional disorders will be discussed. Outcome studies and meta-analyses contemplating the efficacy of cognitive and cognitive-behavioral therapies in various psychological and medical conditions will be briefly depicted. METHOD: Through review of articles and textbooks, especially the works of Aaron Beck from which this review article has heavily borrowed, the origins and foundations of the cognitive-behavioral approaches to the treatment of psychiatric and medical conditions are described. Through Medline, the search of randomized controlled trials and meta-analyses has pointed out the evidence-based efficacy of this psychotherapeutic approach. RESULTS AND CONCLUSIONS: Cognitive-behavioral therapies in general and Beckian cognitive therapy in particular hold a theoretical foundation and a varied set of techniques, whose evidence-based efficacy was demonstrated for the treatment of diverse mental and physical conditions.
Cognitive therapy; Behavior therapy; Review literature; Techniques and procedures; Research
OBJETIVO: Há um interesse crescente no modelo cognitivo de psicoterapia estimulado por grande número de resultados de pesquisa, demonstrando sua eficácia em uma série de transtornos psiquiátricos e distúrbios médicos. Este artigo de revisão objetiva dar um panorama dos fundamentos históricos e filosóficos das abordagens cognitivo-comportamentais contemporâneas, e apontar similaridades e diferenças entre elas. O modelo cognitivo, conforme delineado por Aaron Beck, e alguns dos procedimentos e técnicas cognitivas e comportamentais utilizados em transtornos emocionais serão apresentados. Ao final, resultados de pesquisas e metanálises em relação à eficácia das terapias cognitivas e cognitivo-comportamentais em vários transtornos psiquiátricos e distúrbios médicos serão relatados brevemente. MÉTODO: Por meio da revisão de artigos e livros-texto, principalmente dos trabalhos de Aaron Beck dos quais foi extraída a presente revisão, foram descritas as origens e os fundamentos das abordagens cognitivo-comportamentais no tratamento dos transtornos psiquiátricos e médicos. Através de buscas no Medline de ensaios clínicos randomizados e metanálises, foram apontadas as evidências de eficácia dessa modalidade de tratamento psicoterápico. RESULTADOS E CONCLUSÕES: As terapias cognitivo-comportamentais em geral, e a terapia cognitiva beckiana em especial, apresentam um fundamento teórico e um conjunto de técnicas cuja eficácia baseada em evidências foi demonstrada no tratamento de diversos quadros mentais e físicos.
Terapia cognitiva; Terapia comportamental; Revisão; Técnicas e procedimentos; Pesquisas
ARTICLES
Cognitive therapy: foundations, conceptual models, applications and research
Paulo KnappI; Aaron T BeckII, III
IPsychiatry doctoral student, Universidade Federal do Rio Grande do Sul (UFRGS), Porto Alegre (RS), Brasil
IIUniversity of Pennsylvania, Philadelphia (PA), USA
IIIBeck Institute for Cognitive Therapy, Philadelphia (PA), USA
Correspondence
ABSTRACT
OBJECTIVE: There is growing interest in the cognitive model of psychotherapy stimulated by an extensive body of research findings demonstrating its effectiveness for a varied set of psychiatric disorders and medical conditions. This review article aims to give an overview of the historical and philosophical background to contemporary cognitive and cognitive-behavioral approaches to psychotherapy, pointing out similarities across and differences between them. A presentation of the cognitive model as designed by Aaron Beck, and some of the cognitive and behavioral techniques used in emotional disorders will be discussed. Outcome studies and meta-analyses contemplating the efficacy of cognitive and cognitive-behavioral therapies in various psychological and medical conditions will be briefly depicted.
METHOD: Through review of articles and textbooks, especially the works of Aaron Beck from which this review article has heavily borrowed, the origins and foundations of the cognitive-behavioral approaches to the treatment of psychiatric and medical conditions are described. Through Medline, the search of randomized controlled trials and meta-analyses has pointed out the evidence-based efficacy of this psychotherapeutic approach.
RESULTS AND CONCLUSIONS: Cognitive-behavioral therapies in general and Beckian cognitive therapy in particular hold a theoretical foundation and a varied set of techniques, whose evidence-based efficacy was demonstrated for the treatment of diverse mental and physical conditions.
Descriptors: Cognitive therapy; Behavior therapy; Review literature; Techniques and procedures; Research
Introduction
The terms cognitive therapy (CT) and the generic term cognitive-behavior therapy (CBT) are frequently used as synonyms to describe psychotherapies based on the cognitive model. The term CBT is also used for a group of techniques in which a cognitive approach and a set of behavioral procedures are combined. CBT has been used as an umbrella term to include both standard CT and atheoretical combinations of cognitive and behavioral strategies.1
Since about 45 years ago, when the role of cognition in depression2 and in therapy3 was first described in the literature, there has been continuing progress in the development of cognitive theory and therapy. Empirical testing of both has refined the cognitive model throughout the years.4,5 The essential features of CT, however, have persisted, in particular the emphasis on the influence of distorted thinking and unrealistic cognitive appraisals of events on an individual's feelings and behavior.6 Aaron Beck, the founder of cognitive therapy, formulated a coherent theoretical framework before therapeutic strategies were developed. The guidelines to develop and evaluate the novel system of psychopathology and psychotherapy were:1 1) to construct a comprehensive theory of psychopathology that articulated well with the psychotherapeutic approach; 2) to investigate empirical support for the theory; and 3) to conduct empirical studies that tested the efficacy of the therapy. Research thereafter involved several stages:5 trying to identify the idiosyncratic cognitive elements derived from clinical data in various disorders; developing and testing measures to systematize these clinical observations; and preparing treatment plans and guidelines for therapy.
Research and clinical practice have shown CT to be effective in reducing symptoms and relapse rates, with or without medication, in a wide variety of psychiatric disorders. Beck applied CT's theoretical and therapeutic set of principles systematically to a sequence of disorders starting with depression,4,6 suicide,7 anxiety disorders and phobias,8 panic disorder,9 personality disorders,10 and substance abuse.11 Interpersonal problems12 and anger, hostility, and violence13 were also studied. In addition, more recent work with this approach has shown an additional effect over medication treatment of severe psychiatric disorders such as schizophrenia 14,15 and bipolar disorder.16,17 Ongoing adaptations of cognitive-behavioral protocols for an increasingly wider range of psychological and medical disorders18 have been tested for chronic pain, marital distress, childhood somatic disorders, as well as for bulimia nervosa and overeating problems.19 There are now over 330 outcome studies on cognitive-behavioral interventions, and research production has continued. 20 A few neuroimaging outcome studies21-23 have recently confirmed what was already thought: CBTs produce physiological and functional changes in many brain sites.
Historical and philosophical background to CBTs
In the early 1960s, a "cognitive revolution" began to emerge24 although the first major texts on cognitive modification appeared only in the 1970s. Albert Bandura's25 research on information-processing models and vicarious learning together with empirical evidence in the area of language development26 raised questions about the traditional behavioral model available up to that date, and pointed out the limitations of a non-mediational behavioral approach in explaining human behavior.27 An increasing number of theorists and therapists started to identify themselves as being "cognitive-behavioral" in orientation; some of the most important early proponents of a cognitive and cognitive-behavioral perspective were Beck,2,4,28 Ellis,29 Cautela,30 Meichenbaum,31 and Mahoney.27
A diversity of CBT approaches have emerged over the decades, reaching varied degrees of application and success.24 CBTs can be organized in three major divisions:32 1) coping skills therapies, which stress the development of a repertoire of skills designed to give the patient the instruments to cope with in a variety of problem situations; 2) problem-solving therapies, which emphasize the development of general strategies to deal with a broad range of personal difficulties; and 3) restructuring therapies, which emphasize the assumption that emotional problems are a consequence of maladaptive thoughts, being the goal of treatment to reframe distorted thinking and to promote adaptive thoughts. A few of these conceptual models of cognitive-behavioral modification, as presented by Dobson and Dozois24 are briefly summarized below. Aaron Beck's cognitive therapy will be discussed in a separate section in this article.
Self-instructional training was developed in the 1970s by Donald Meichenbaum,33 with a particular focus on the relationship between verbal self-instruction and behavior. Supported by extensive literature, self-instructional training has its emphasis on graded tasks, cognitive modeling, directed mediational training, and self-reinforcement, which clearly reflects Meichenbaum's behavioral background. Stress inoculation training, another CBT with a multi-component coping-skills approach, was also developed by Meichenbaum,34 and is based on the theoretical premise that in learning to deal with mild levels of stress, clients essentially become "inoculated" against uncontrollable levels of stress. Problem-solving therapy, conceptualized as self-control training, was proposed in 1971 by D'Zurilla and Goldfried;35 its purpose is to train in basic problem-solving skills that are subsequently applied to real problem situations and thus promote generalized behavior change. It has been developed and used in a variety of situations, such as stress prevention and management, anger management, depression, and coping with cancer.36
Rational emotive behavior therapy (REBT), a restructuring therapy developed by Albert Ellis, is regarded by many as one of the first cognitive-behavioral therapies. Over 45 years ago, Ellis, originally a psychoanalyst, developed the so-called ABC model, which posits that any particular experience or event activates (A) individual beliefs (B), which in turn generate emotional, behavioral or physiological consequences (C). Ellis also postulates that 12 basic irrational beliefs, which take the form of unrealistic or absolutistic expectations, underlie emotional disturbance. The goal of therapy is to identify irrational beliefs, and through logical-empirical questioning, challenging, disputing and debating forcefully modify them.37 His 1962 book Reason and Emotion in Psychotherapy remains a primary reference for this approach.
Constructivist therapy has a structural cognitive approach introduced in the early 1980s.38 While there are some parallels between the cognitive-behavioral and the constructivist perspectives, such as the identification and modification of cognitive structures through a variety of behavioral and cognitive techniques, there are important differences between CBT, termed a "rational" approach, and the constructivist perspective considered as a "post-rational" approach.33 Guidano38 expressed increasing concern with the validity value of cognitive structures over the truth value of the content of cognitive structures; rather than dealing with thought content, therapies within constructivism would emphasize the process of thinking and the generation of meaning. As pointed out by Neimeyer39 the post-rational approach may be even "radically divergent from a traditional cognitive therapy perspective".
In recent years, many other cognitive-behavioral approaches have emerged and evolved from the original cognitive and cognitive-behavioral conceptual model. Schema therapy, developed by Jeffrey Young,40 and Dialectic behavior therapy (DBT) developed by Marsha Linehan,41 are two good examples of CBT approaches being used to treat individuals with more severe psychopathology, particularly borderline personality disorder.
1. Similarities and differences between CBTs
CBT approaches share common ground, although there are considerable differences in principles and procedures between them for the fact that the pioneers in the development of cognitive-behavioral interventions came from different theoretical backgrounds. For example, while both Aaron Beck and Albert Ellis had psychoanalytic backgrounds, other theorists such as Meichenbaum, Goldfried and Mahoney were originally trained in behavior modification.
According to Dobson & Dozois,42 current CBT approaches share three fundamental propositions. The first is the mediational role of cognition, which asserts that there is always a cognitive processing and appraisal of internal and external events that can affect the response to those events; the second one, states that cognitive activity may be monitored, assessed and measured; and the third, that behavior change may be mediated by these cognitive appraisals, and may be, thus, an indirect sign of cognitive change.
CBT can be contrasted with purely behavioral treatments in which cognition is not an important explanatory variable and is not primarily targeted for intervention. Therefore, approaches aimed strictly at behavior change, such as the stimulus-response model, are not cognitive-behavioral; similarly, any therapy that focuses solely on cognitive change is not cognitive-behavioral. Any form of therapy that does not include the proposition of the mediational model as an important component of the treatment plan is not under the scope of CBT, and the label "cognitive-behavioral" cannot be applied42 In sum, a defining feature of cognitive-behavioral therapy is the concept that symptoms and dysfunctional behaviors are cognitively mediated and, hence, improvement can be produced by modifying dysfunctional thinking and beliefs.
In addition, the various cognitive-behavioral therapies share a number of commonalities that are not theoretically central.42 First, in contrast to longer-term psychoanalytic therapy, most CBTs are time-limited in nature, with many treatment manuals recommending 12-16 sessions for uncomplicated depression and anxiety. Personality disorders and other chronic disorders will take longer, maybe more than 1-2 years of treatment. Second, almost all CBTs are applied to specific problems or disorders, a characteristic that reflects their behavior therapy heritage and in part explains their time-limited nature. Rather than implying a limitation of CBTs, their problem-focused nature reflects a continuing effort to document therapeutic effects, to establish therapeutic frontiers, and to identify the most efficacious therapy for a given problem. A third commonality, the assumption of patient control, emphasizes that the patient is the active agent in his/her treatment. The assumption of patient control is made possible by the types of problems that classical CBTs typically address, which include discrete disorders and conditions, self-control problems, and general problem-solving abilities. Related to the assumption of patient control is a fourth commonality: many CBTs are explicitly or implicitly educative in nature, as the therapeutic model may be taught and the rationale for intervention communicated to the patient, which stands in contrast to other psychotherapeutic approaches. The fifth commonality extends directly from their educative process, as most CBTs set the implicit goal that the patient will learn about the therapeutic process over the course of therapy. Patients not only overcome the referral problems in therapy, and thus learn to prevent relapses, but also learn therapeutic skills, which they themselves may apply comprehensively to an array of different problems in their lives. In CBT patients become their own therapists.
As Dobson & Dozois pointed out, even though therapies identified as cognitive-behavioral share a number of theoretical and practical features, and despite their various procedural overlaps, "it is no more appropriate to state that there is really one cognitive-behavioral approach as it is to state that there is one psychoanalytic therapy".42 However, while cognitive-behavioral therapies in general involve a whole variety of approaches, cognitive therapy as developed by Beck, with its own set of principles and very specific methodologies and techniques, is fairly uniform.
Cognitive therapy
1. Theoretical foundations
The cognitive model was originally constructed following research studies conducted by Aaron Beck2,3 to explain the psychological processes in depression, in an attempt to prove Freudian's theory of depression as repressed retroflexed hostility. Instead of hostility and anger, the research on patients' dreams showed a "sense of defeat, failure and loss".43 Depressed patients' themes while dreaming were consistent with their waking themes; dreams could simply be a reflection of the person's thoughts. Based on systematic research and clinical observations, Beck proposed that the symptoms of depression could be explained in cognitive terms as biased interpretations of events attributed to the activation of negative representations of the self, the personal world, and the future (the cognitive triad).5
As a natural consequence, Beck began to increasingly question the psychoanalytic unconscious motivational model and therapeutic method, especially the psychoanalysis' emphasis on motivational-affective conceptualizations of emotional disorders, which largely ignored cognitive factors, as it was substantiated by his research findings on depression.2 Laying the grounds for cognitive theory and therapy, Beck started differentiating the cognitive from the psychoanalytic approach, focusing the treatment on present problems, as opposed to uncovering hidden traumas from the past, and on analyzing accessible, rather than unconscious, psychological experiences5,6 Nevertheless, the experience with psychoanalysis was important in the initial development of the therapeutic concepts and strategies of CT. An important contribution to the foundations of CT was given by the Freudian formulation of hierarchical structuring of cognition into a primary process (i.e., out of awareness and based on fantasies and wishes) and a secondary process (i.e., accessible to awareness and based on the principles of objective reality), as well as the concept that symptoms are based on pathogenic ideas.2 Since his psychoanalysis training and along his professional career, Beck identified himself with neo-analysts, such as Alfred Adler, Karen Horney, Otto Rank and Harry Sullivan, who emphasized the importance of understanding and dealing with patients' conscious experiences as well as the need to treat the meanings patients give to events they experience in their lives. Cognitive theory with its focus on intrapsychic processes rather than overt behavior is more a legacy from psychoanalytic theory, although therapeutic procedures are more similar to behavior therapy.44
Furthermore, the theoretical structure of CT was built on contributions from other schools, such as the phenomenological-humanistic approach to psychology. Inspired in part by philosophers such as Kant, Heidegger and Husserl, it adopted the emphasis on conscious subjective experience. Derived from the Greek stoic philosophers came the concept that human beings are disturbed by the meanings they attach to facts, not by the facts per se. Carl Rogers with his client-oriented therapy inspired the therapeutic style of gentle questioning and the unconditional acceptance of the patient. John Bowlby's45 attachment theory was a highly valuable source for the development of cognitive conceptualization.
Influences from cognitive sciences and cognitive psychology also accounted for the foundations of CT. The writings of cognitive psychologist George Kelly had a prominent impact, especially his personal construct theory, which, along with Piaget's46 idea of schemata, evolved into Beck's similar definition of schemas. The cognitive theory of emotions by Richard Lazarus,47 the problem-solving approach by Goldfried and D'Zurilla,48 the self-management models by Albert Bandura,49 and Donald Meichenbaum,50 along with cognition-oriented writers, such as Arnold Lazarus,51 also influenced cognitive theory and therapy. CT's emphasis on a problem-solving approach to conscious problems was also adopted by Ellis's rational-emotional-behavior therapy.30
The scientific approach espoused by behavior therapy contributed to diverse therapeutic procedures and strategies, such as the session structure, the greater activity by the therapist, the setting of treatment goals for the entire therapy as well as of an agenda for each session, the formulation and test of hypotheses, the elicitation of feedback, the use of problem-solving techniques and social skills training, the assignment of between-sessions homework and experiments, and the measurement of mediational variables and outcomes. However, from a philosophical point of view, CT may be seen as much more humanistic, exploratory, as it works with constructs such as the mind, and deals with feelings and thoughts, whereas many would see behavior therapy as too mechanistic.
2. Principles of CT
Again, following the information-processing approach, the major principle of CT is that the way individuals perceive and process reality will influence the way they feel and behave. Thus, the therapeutic goal of CT, since its very origins, has been to reframe and correct these distorted thoughts, and collaboratively endeavor pragmatic solutions to engender behavioral change and ameliorate emotional disorders.
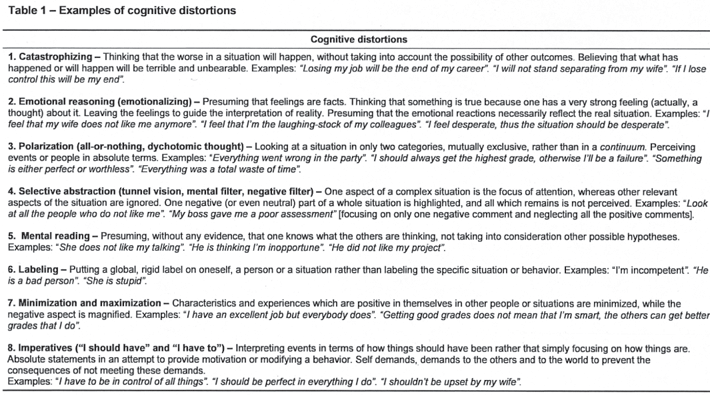
Cognitive therapy posits that there are thoughts at the fringe of awareness that occur spontaneously and rapidly, and are an immediate interpretation of any given situation.5 These are called automatic thoughts and are distinguished from the ordinary flow of thoughts observed in reflective thinking or free association. They are generally accepted as plausible, and their accuracy is taken for granted. Most people are not immediately aware of the presence of automatic thoughts, unless they are trained at monitoring and identifying them. According to Beck,52 "it is just as possible to perceive a thought, focus on it, and evaluate it as it is to identify and reflect on a sensation as pain". Some of the cognitive distortions found across different emotional disorders are summarized in Table 1.
In the roots of these distorted automatic interpretations are deeper dysfunctional thoughts called schemas (also called core beliefs, and used interchangeably by many authors). As defined by Clark, Beck & Alford53 schemas are "relatively enduring internal cognitive structures of stored generic or prototypical features of stimuli, ideas, or experiences that are used to organize new information in a meaningful way thereby determining how phenomena are perceived and conceptualized". Once a particular basic belief is formed it may influence the subsequent formation of new related beliefs, and if they persist, they are incorporated into the enduring cognitive structure or schema.54 Core beliefs embedded in these cognitive structures shape an individual's thinking style and foster the cognitive errors encountered in psychopathology.
Schemas are acquired early in an individual's development, and act as "filters" through which current information and experience is processed. These beliefs are molded by personal experiences and derived from identification with significant others and from the perception of other people's attitudes toward them. The child's environment either facilitates the emergence of particular types of schemas or tends to inhibit them. The schemas of well-adjusted individuals allow for realistic appraisals, while those of maladjusted individuals lead to distortions of reality, fostering, in turn, psychological disorder.5
Schemas have a variety of properties, such as permeability, flexibility, breadth, density, and also a degree of emotional charge,5 which may determine the difficulties or facilities encountered in the treatment process. Even though latent or inactive at given times, schemas, e.g., "I am unlovable", are activated by particular situations analogous to those early experiences that engendered the development of the schema. Associated with these dysfunctional core beliefs are subjacent individual conditional beliefs that lead to assumptions such as "If I don't have a loving wife, I'm nothing" and rules such as "A man cannot live without a wife". The activation of these schemas interferes with the capacity for objective appraisal of events, and reasoning becomes impaired. Systematic cognitive distortions (e.g., catastrophizing, emotional reasoning, and selective abstraction) occur as dysfunctional schemas are activated. As tentative coping strategies to avoid getting in contact with their core and underlying beliefs, patients may engage in compensatory strategies. Although these cognitive and behavioral maneuvers alleviate their emotional suffering momentarily, in the long run compensatory strategies may reinforce and worsen dysfunctional beliefs.
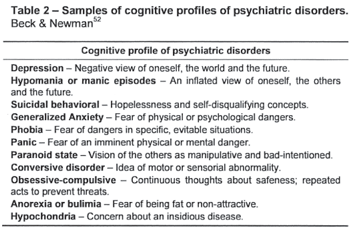
There is a reciprocal relationship between affect and cognition, as increasing emotional and cognitive impairment may result from one reinforcing the other.54 A crucial hypothesis of the cognitive model has been the notion that certain beliefs constitute a vulnerability to emotional disorders (stress-diathesis model). For example, if an individual holds a cognitive vulnerability to themes of loss and failure, the emotional and behavioral consequences will include sadness, a sense of hopelessness, and social withdrawal, as found in depression. If other individuals hold danger-oriented beliefs, anxiety will prevail and predispose them to narrow their attention to perceived threat, make catastrophic interpretations of ambiguous or even neutral stimuli,8 and engage in dysfunctional "safety behaviors"; they will be impelled to seek escapes or avoid the risk of perceived rejection, embarrassment or death. The danger-oriented biases which occur automatically and are not necessarily under conscious control are found in every phase of information processing (perception, interpretation, and recall)55 across all anxiety disorders. In patients with vulnerability to themes of humiliation, unfairness or the like, anger will be the tone, and a behavioral response in a retaliatory manner might be justified as a self-defense52 Each personality disorder is also characterized by a specific personal set of dysfunctional cognitive contents, such as defectiveness, abandonment, dependency, or need for a special status, which constitute the individual's cognitive vulnerability. When activated by external events, drugs, or endocrine factors, these schemas tend to bias the information processing and produce the typical cognitive content of a specific disorder, with its own cognitive constellation and idiosyncratic set of beliefs.1 A brief summary of cognitive profiles in psychopathology may be seen in Table 2.
Beck's model of vulnerability to depression was refined56 to suggest that predisposing beliefs could be differentiated according to whether the patient's personality was primarily autonomous or sociotropic. Autonomous individuals would more likely become depressed following an autonomous event (e.g., a perceived personal failure) than following a sociotropic event (e.g., loss of a relationship), and the reverse would be true for sociotropic individuals.
3. Procedures and techniques
CT is not a set of techniques applied mechanically as we would think at a first glance. The therapist's competence in a full range of therapeutic skills is needed to ensure efficacy to CT procedures.
As Beck points out, first and primarily, to fulfill the therapeutic endeavor, it is important to establish a good working relationship with the patient, a therapeutic procedure called collaborative empiricism. Patient and therapist work as a team of scientists in evaluating the patient's beliefs, testing them out to see whether they are accurate or not, and modifying them according to reality. Second, the therapist uses Socratic questioning as a means to guide the patient in a mindful questioning that will enable patients to have insight over their distorted thinking, a procedure called guided discovery.
Throughout the treatment, the collaborative and psychoeducational approach to treatment is used, with specific learning experiences designed to teach clients to: 1) monitor and identify automatic thoughts; 2) recognize the relationships among cognition, affect, and behavior; 3) test the validity of automatic thoughts and core beliefs; 4) correct biased conceptualizations by replacing distorted thoughts with more realistic cognitions; and 5) identify and alter beliefs, assumptions, or schemas that underlie faulty thinking patterns.5
In contrast to psychoanalytical therapies, CT sessions have a structure in which the cognitive therapist plays an active role in helping the patient identify and focus on important areas, proposing and rehearsing specific cognitive and behavioral techniques, and collaboratively planning between-sessions assignments. A treatment plan for the whole therapy and the agenda for each session are discussed with the patient, and a feedback of the patient's thoughts about the ongoing session and the whole treatment is routinely asked in order to create the opportunity to treat and handle any misconceptions and misunderstandings that might arise over the course of therapy. The cognitive therapist has to be a good strategist to devise specific therapeutic procedures that have higher chances of producing specific changes for that particular patient.
CT encourages their patients to adopt the empirical problem-solving approach of scientists, and the therapist serves as a role model for their patients by instilling self-efficacy, enthusiasm and hopefulness about the challenging work of changing maladaptive cognitions. Although transference, as defined in psychoanalytic concept, is not encouraged, its manifestation might be a valuable tool in demonstrating to patients their interpersonal distortions. Similarly, any manifestation of resistance to treatment is dealt with and treated as underlying dysfunctional beliefs.
4. Case conceptualization
From the very beginning of treatment, the therapist develops (ideally in a collaborative manner, as always) a cognitive conceptualization for the individual patient. Case conceptualization is an ongoing work throughout a treatment course; as new important clinical data are brought into therapy, cognitive conceptualization will be changed and updated as needed while the treatment progresses. To prepare a treatment plan, an individual case conceptualization is strongly needed, as it guides therapeutic interventions.
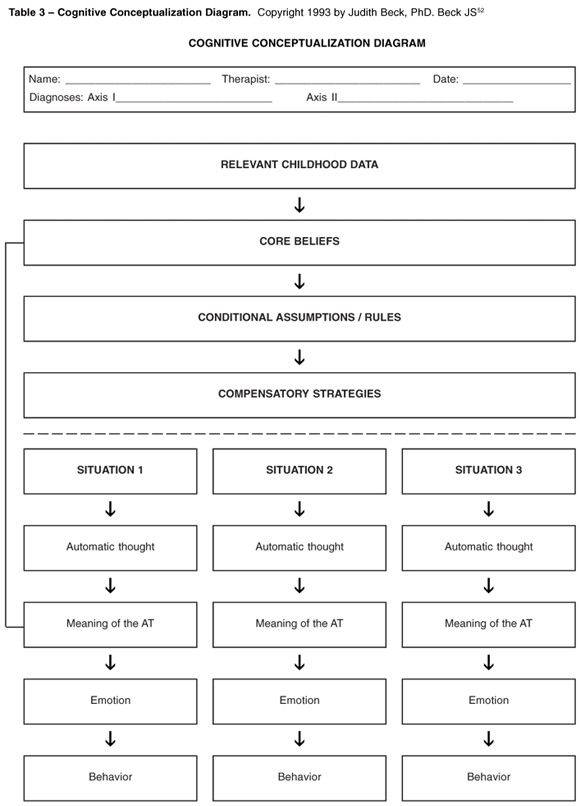
Case conceptualization holds both a historical and prospective evaluation of thought patterns and thinking styles.52 By searching and assembling common cognitive denominators across diverse life situations and the patient's evaluation of them, a cognitive pattern can be identified. It will include an understanding of the idiosyncratic set of dysfunctional beliefs, individual specific vulnerabilities, and the behavioral strategies patients use in attempting to cope with their core beliefs. A sample of the Cognitive Conceptualization Diagram, as depicted by Judith Beck,57 is presented in Table 3.
5. Cognitive and behavioral techniques
The separation of CT interventions into cognitive techniques and behavioral techniques is only for instructive purposes, in that many of the techniques affect both patient's thought processes and behavioral patterns. As we know, cognitive change fosters behavioral change, and vice-versa. A number of different techniques may be used depending on the cognitive profile of the disorder, the phase of therapy, and the specific cognitive conceptualization of a given case. Behavioral techniques might be more used in cases of severe depression in which there is a need to promote the patient's behavioral activation. Conversely, when the patient does not primarily need behavioral activation, more purely cognitively oriented procedures may be applied. For patients with anxiety disorders, an understanding of the fundamental principles of the cognitive model will probably be necessary before the introduction of any behavioral experiment.
A variety of cognitive techniques are used in CT, such as the identification, questioning, and correction of automatic thoughts, reattribution and cognitive restructuring, cognitive rehearsal, and other imagery therapeutic procedures. Among the behavioral techniques, there are, for example, activity scheduling, mastery and pleasure ratings, graded-task behavioral assignments, reality testing experiments, role-playing, social skills training, and problem-solving techniques. We will present briefly a small sample of cognitive techniques first.
Initial treatment focuses on the increase of the patients' awareness of automatic thoughts, and further work will focus on core and underlying beliefs. Treatment may start by identifying and questioning automatic thoughts, which can be done in different ways. The therapist can guide patients to assess their automatic thoughts, especially when there is a perceived emotional arousal during the session, by simply asking: "What is going through your mind?", or any variation of this question. Cognitive distortions may be unveiled by asking, for example, "What are the evidences for your conclusion?", "Are you omitting contradictory evidence?", "Does your conclusion follow logically from the observations you have made?", "Are there alternative explanations that may be more accurate in explaining this particular episode?". When asked to reflect on alternative explanations, patients may realize that their initial explanations evolved through invalid inferences, which leads them to think of different interpretations of events, thus attaching new attributions and meanings to them.52
Most people are unaware that negative automatic thoughts precede unpleasant feelings and behavioral inhibitions, and that the emotions are consistent with the content of the automatic thoughts. To increase their awareness of these thoughts, patients can learn to track them and with systematic training pinpoint what kind of thoughts occurred immediately before an emotion, a behavior, and a physiologic reaction as consequences of that thought (Ellis' ABC sequence). The Dysfunctional Thought Record (DTR), as depicted by Judith Beck57 (Table 4), may be used to help track the thoughts that were activated by the stimulus situation and that generated the consequent emotion and behavior. A DTR exercise may enable patients to discover, clarify and change the meanings they have assigned to upsetting events and compose an alternative or rational response. Sometimes, the simple task of identifying cognitive errors (Table 1), alone or in combination with the filling out of a DTR, might be a good exercise to work on at the office or as a homework assignment.
For structural changes to occur, they have to go far beyond changing cognitive errors associated with a specific syndrome. Only through the analysis and correction of the more ingrained beliefs, changing the organization of these beliefs, cognitive restructuring may be accomplished. Treatment has to focus on the patient's core beliefs, such as "I'm unlovable", and underlying beliefs, such as "If I don't have a wife, then I'm a failure" which are re-evaluated in the same way as automatic thoughts, that means, looking for evidence that supports them and correcting them with reality testing.
Cognitive rehearsal is an imagery technique devised to help patients experience their feared situations by imagining that it is occurring right at that moment. At the office or as a between-session assignment, patients are asked to "live through" the feared situation in imagery and build up the best coping strategies to overcome it successfully. In the same manner, through imagery, patients can rehearse problem solving and assertiveness training as needed to overcome their problem situations.
Behavioral techniques are integrated into a CT treatment program in many different forms. When chronic and severely depressed patients have their activity level reduced, and are reluctant to commit themselves to any goal because they have low expectations about any achievements, behavioral activation procedures should be promoted. For example, therapist and patient may assign experiments collaboratively to see whether the patient's negative expectations are valid or come from wrong inferences about him/herself, other people and the future. For instance, a depressed woman may believe she is no more capable of preparing a Sunday dessert that her grandchildren liked so much; as a matter of fact, she even believes she is unable to stay out of bed long enough to do almost anything, let alone to prepare a dessert. To gather evidence of her expected capacity of mastery on dessert preparation and expected capacity of experiencing pleasure with her cooking skills, she is stimulated to rate her mastery and pleasure expectations before performing the task on Sunday morning and compare them to what her thoughts and feelings actually were after she completed the assigned task. She will probably receive, as usual, many positive feedbacks, which will help her correct inaccurate mastery and pleasure ratings. Frequently depressed patients have dysfunctional expectations about their capabilities when feeling depressed, and are surprised at a much better outcome than they expected. As the patient puts them to test, the outcome brings a different perspective.
As patients are able to appraise their thoughts more objectively, a whole set of thoughts become hypotheses that have to be submitted to reality testing. Because most patients need to proceed in small steps, a number of graded-task behavioral assignments are tailored for individual patients to progressively promote greater successful experiences without overwhelming them with tasks greater than their present coping capacities.
Much of cognitive therapy is devoted to problem-solving techniques; patients will learn to follow the necessary steps, such as defining the problem, generating alternative ways of solving it and implementing alternative solutions. Social skills training may be a necessary tool as part of the treatment plan. A patient that fears social situations and has poor social performance will benefit from role-playing the feared situation with the therapist to build up inhibited social skills and overcome the problem. The therapist acts as a role model so that patients can learn to perform socially. After sufficient role-playing at the office, patients are stimulated to perform in real life situations what they have built in the office.
Cognitive therapy has been developed for application in individual, group, couples and family formats, for adults, adolescents and children, in a variety of clinical contexts. The indications for cognitive therapy are determined by patient and therapist variables, rather than by the nature of the disorder.52
CT/CBT outcome studies
How effective for which disorders and for how long is CBT effective compared to other procedures? Butler and Beck et al.20 reviewed the meta-analyses of treatment outcomes of CBT/CT for a wide range of psychiatric disorders and medical conditions. A search in the literature from 1967 to 2003 pooled a total of 16 methodologically rigorous meta-analyses encompassing more than 9000 subjects from 330 studies. The review focused on effect sizes that contrasted outcomes of CBT with the outcomes for control groups for each disorder, providing an overview of the efficacy of CBT/CT. Because the literature reviews generally combine studies labeled CBT and CT under the CBT scope, the findings of these reviews were pooled and, whenever possible, pinpointed the more evident CT studies. Among the limitations of the meta-analytic approach are the assumptions of uniformity across the studies in the samples, in the content of therapy, and in therapists.
Butler et al's findings reveal that large effect sizes (grand mean = 0,90) were found for adult unipolar depression, adolescent unipolar depression, generalized anxiety disorder, panic disorder with or without agoraphobia, social phobia, post-traumatic stress disorder, and childhood depressive and anxiety disorders. The comparison-weighted grand mean effect size for these disorders when compared to no-treatment, waiting list, or placebo controls is 0.95 (SD = 0.08). CBT is associated with large improvements in symptoms for bulimia nervosa, and the associated effect sizes (M = 1,27, SD = 0.11) are significantly larger than those that have been found for pharmacotherapy. Moderate effect sizes (M = 0.62, SD = 0.11) were obtained when CT was compared to controls for marital distress, anger, childhood somatic disorders, and several chronic pain variables (i.e., pain expression behavior, activity level, social role functioning, and cognitive coping and appraisal).20
CT was found somewhat superior to antidepressants in the treatment of adult unipolar depression (ES = 0.38), and was equally effective as behavior therapy in the treatment of adult depression (ES = 0.05) as well as in obsessive-compulsive disorder (ES = 0.19). The efficacy of CT for sexual offenders is relatively low (ES = 0.35); however, in combination with hormonal treatments, it is the most effective treatment for reducing recidivism in this population. Finally, the review reported that CT was found to be superior to supportive/nondirective therapy in two comparisons for adolescent depression (ES = 0.84) and two comparisons for generalized anxiety disorder (ES = 0.71).
CBT has also shown promising results as adjunct to pharmacotherapy in the treatment of schizophrenia: the average uncontrolled effect size of 1.23 for CBT compares favorably with an effect size of 0.17 for schizophrenic patients receiving only routine care. CT/CBT may also have a therapeutic role in the relapse prevention of schizophrenia as reported in a randomized controlled study of CT with very high-risk groups.
Findings from other meta-analyses also indicate that CT/CBT protocols are more effective in reducing panic and anxiety symptoms than pharmacological treatments are.58 The efficacy of specific CT for panic disorder has been supported by several studies.59,60 Two meta-analyses of CT and CBT have demonstrated the efficacy of these approaches for social phobia,61,62 and found that a "pure" CT approach was more effective than fluoxetine.63 Standard CT for generalized anxiety disorder has been shown to have a clear advantage to behavior therapy at follow-up.64
The maintenance of the effects of CT across many disorders for substantial periods beyond the cessation of treatment was supported by the meta-analyses reviewed. Significant evidence for long-term effectiveness was found for depression, generalized anxiety, panic, social phobia, OCD, sexual offending, schizophrenia, and childhood internalizing disorders. In the cases of depression and panic, there are robust and convergent meta-analytic evidence that CT produces vastly superior long-term persistence of effects, with relapse rates half those of pharmacotherapy.1
Another meta-analysis65 pooled seventeen studies with depressed patients and found that CT had a minimal superiority to antidepressant medication (ADM) with ES = 0.38. A recent study with moderately depressed subjects conducted by DeRubeis et al.66 found that CT and ADM had equivalent efficacy but CT performed better regarding relapse prevention. Severely depressed patients had as good outcomes with CT as with ADM in a meta-analysis of 4 studies.67 In addition, CT was found to be effective in the treatment of atypical depression.
For bipolar disorder, the application of CT as an adjunctive treatment in the prevention of relapse as well as its cost-effectiveness has also been reported. Lam et al.,17 in a randomized controlled trial of CBT for relapse prevention in bipolar disorder, found that patients treated with CBT experienced significantly better outcomes (e.g., fewer and shorter bipolar episodes, fewer hospital admissions, less variability in manic symptoms etc.) at 1 year follow-up. Some other empirically supported applications of CT/CBT include anorexia nervosa, body dysmorphic disorder, pathological hoarding, pathological gambling, PTSD in abused children, obsessive-compulsive disorder in children and seasonal affective disorder.20
Randomized controlled trials have also provided strong empirical support for the efficacy of cognitive interventions, often as an adjunct to therapy, in the treatment of a broad range of medical conditions including heart disease, hypertension, cancer, headaches, chronic pain, chronic low back pain, chronic fatigue syndrome, rheumatoid arthritis, premenstrual syndrome, and irritable bowel syndrome.1 Additional outcome studies have documented the beneficial role of CT for patients with various medical disorders in reducing depression and improving overall quality of life.20
In recent years, research studies found neuropsychological correlates of the dysfunctional thinking and beliefs in depression.68,69 Neuroimaging studies supporting the effects of cognitive therapy in cerebral physiological and functional changes associated with CT for depression have also been demonstrated.23 Although the very interesting findings, the subject is beyond the scope of this review article. Of note, however, is the fact that studies of this nature can greatly expand our understanding of the mind-brain relationship, and how cognitive and behavioral techniques affect brain function.70
Conclusions
There is no doubt that Beck's cognitive approach represents a theoretical shift to the understanding and treatment of emotional disorders.71 Over 40 years after the cognitive theory of depression was published, cognitive therapy has become the single most important and best validated psychotherapeutic approach, and with the recent movement towards evidence-based practice, CT has gained prominent attention. New applications of CT are developed for a wide range of psychological and medical conditions, although the theoretical foundations of the cognitive model remain unchanged.1 As Beck70 points out, "the steady progress in research and practice evidenced throughout the history of the cognitive-behavioral therapies can be taken as an indication that the future of the field will undoubtedly witness continued advancement".
Disclosures

References
- 1. Beck AT. The current state of cognitive therapy: a 40 year retrospective. Arch Gen Psychiatry. 2005;62(9):953-9.
- 2. Beck AT. Thinking and depression. I. Idiosyncratic content and cognitive distortions. Arch Gen Psychiatry 1963;9:324-33.
- 3. Beck AT. Thinking and depression: II theory and therapy. Arch Gen Psychiatry 1964;10:561-71.
- 4. Beck AT. Depression: Clinical, Experimental, and Theoretical Aspects. New York, NY: Harper and Row; 1967.
- 5. Beck AT. Cognitive Therapy and the Emotional Disorders. New York: International Universities Press; 1976.
- 6. Beck AT, Rush AJ, Shaw BF, Emery G. Cognitive therapy of depression. New York: Guilford; 1979.
- 7. Beck AT, Resnik HLP, Lettieri DJ, editors. The Prediction of Suicide. Bowie, Md: Charles Press; 1974.
- 8. Beck AT, Emery G, Greenberg RL. Anxiety Disorders and Phobias: A Cognitive Perspective. New York, NY: Basic Books; 1985.
- 9. Beck AT. Cognitive approaches to panic disorder: theory and therapy. In: Rachman S, Maser J, editors. Panic: Psychological Perspectives Hillside, NJ: Lawrence Erlbaum Associates; 1987. p. 91-109.
- 10. Beck AT, Freeman A, Davis D, Associates. Cognitive Therapy of Personality Disorders. New York, NY: Guilford; 1990.
- 11. Beck AT, Wright FW, Newman CF, Liese B. Cognitive Therapy of Substance Abuse New York, NY: Guilford; 1993.
- 12. Beck AT. Love Is Never Enough New York, NY: Harper & Row; 1988.
- 13. Beck AT. Prisoners of Hate: The Cognitive Basis of Anger, Hostility and Violence New York, NY: HarperCollins; 1999.
- 14. Beck AT, Rector NA. Cognitive approaches to schizophrenia: theory and therapy. Annu Rev Clin Psychol 2005;1:577-606.
- 15. Rector NA, Beck AT. Cognitive behavioral therapy for schizophrenia: an empirical review. J Nerv Ment Dis 2001;189(5):278-87.
- 16. Lam DH, Watkins ER, Hayward P, Bright J, Wright K, Kerr N, Parr-Davis G, Sham P. A randomized controlled study of cognitive therapy for relapse prevention for bipolar affective disorder: outcome of the first year. Arch Gen Psychiatry 2003;60(2):145-52.
- 17. Lam DH, McCrone P, Wright K, Kerr N. Cost effectiveness of relapse prevention cognitive therapy for bipolar disorder: 30-month study. Br J Psychiatry 2005;186:500-6.
- 18. Beck AT. The past and future of cognitive therapy. J Psychother Pract Res 1997;6(4):276-84.
- 19. Beck JS. The Beck Diet Solution: train your brain to think like a thin person. Des Moines: Oxmoor House; 2007.
- 20. Butler AC, Chapman JE, Foreman EM, Beck AT. The empirical status of cognitive-behavioral therapy: a review of meta-analyses. Clin Psychol Rev. 2006;26(1):17-31.
- 21. Linden DE. How psychotherapy changes the brain the contribution of functional neuroimaging. Mol Psychiatry 2006;11(6):528-38.
- 22. Liggan DY, Kay J. Some Neurobiological Aspects of Psychotherapy: a review. J Psychother Pract Res. 1999;8(2):103-14.
- 23. Goldapple K, Segal Z, Garson C, Lau M, Bieling P, Kennedy S, Mayberg H. Modulation of cortical-limbic pathways in major depression: treatment-specific effects of cognitive behavior therapy. Arch Gen Psychiatry 2004;61(1):34-41.
- 24. Dobson KS, Scherrer, MC. História e Futuro das Terapias Cognitivo-Comportamentais. In: Knapp P, editor. Terapia Cognitivo-Comportamental na Prática Psiquiátrica. Porto Alegre: Artmed; 2004.
- 25. Bandura A. Vicarious processes: a case of no-trial learning. In: Berkowitz L, editor. Advances in experimental social psychology. Vol. 2. New York: Academic Press; 1965.
- 26. Vygotsky LS. Thought and language Cambridge, MA: M.I.T. Press; 1962.
- 27. Mahoney MJ. Cognition and behavior modification. Cambridge, MA: Ballinger; 1974.
- 28. Beck AT. Cognitive therapy: nature and relation to behavior therapy. Behav Ther. 1970;1:184-200.
- 29. Ellis A. Reason and emotion in psychotherapy New York: Stuart; 1962.
- 30. Cautela JR. Covert sensitization. Psychol Rep. 1967;20(2):459-68.
- 31. Meichenbaum DH. Cognitive factors in behavior modification: modifying what clients say to themselves. In: Franks CM, Wilson GT, editors. Annual review of behavior therapy, theory, and practice. New York: Brunner/Mazel; 1973.
- 32. Mahoney MJ. Human change processes: the scientific foundations of psychotherapy. New York: Basic Books; 1995.
- 33. Meichenbaum DH. Stress inoculation training: a twenty-year update. In: Woolfolk RL, Lehrer PM, editors. Principles and practice of stress management New York: Guilford Press; 1993.
- 34. Meichenbaum DH. Stress inoculation training: a clinical guidebook New York: Pergamon Press; 1985.
- 35. D'Zurilla TJ, Goldfried MR. Problem-solving and behavior modification. J Abnorm Psychol. 1971;78:107-26.
- 36. Nezu AM. Efficacy of a social problem solving therapy approach for unipolar depression. J Consulting Clin Psychol. 1986;54(2):196- 202.
- 37. Dryden W, Ellis A. Rational emotive behavior therapy. In: Dobson KS, editor. Handbook of cognitive-behavioral therapies. 2nd ed. New York: Guilford Press; 2001.
- 38. Guidano VF, Liotti G. Cognitive processes and emotional disorders: a structural approach to psychotherapy. New York: Guilford; 1983.
- 39. Neimeyer RA. Constructivist psychotherapies: features, foundations and future directions. In: Neimeyer RA, Mahoney MJ, editors. Constructivism in Psychotherapy. Washington, DC: American Psychological Association; 1995. p. 231-46.
- 40. Young J, Klosko J, Weishaar ME. Schema therapy: a practitioner's guide. New York: Guilford; 2003.
- 41. Linehan M. Cognitive-behavioral treatment of borderline personality disorder. New York: Guilford Press; 1993.
- 42. Dobson KS, Dozois DJ. Historical and philosophical bases of the cognitive-behavioral therapies. In: Dobson KS, editor. Handbook of cognitive-behavioral therapies 2nd ed. New York: Guilford Press; 2001.
- 43. Beck AT, Ward CH. Dreams of depressed patients: characteristic themes in manifest content. Arch Gen Psychiatry. 1961;5:462-7.
- 44. Beck AT. Cognitive therapy, behavior therapy, psychoanalysis, and pharmacotherapy: a cognitive continuum. In: Williams JBW, Spitzer RL. Psychotherapy research: where are we and where should we go? New York: Guilford; 1984.
- 45. Bowlby J. Attachment and loss I: Attachment New York: Basic Books; 1969.
- 46. Piaget J. The construction of reality in the child New York: Ballantine Books; 1954.
- 47. Lazarus RS, Alfert E. Short-circuiting of threat by experimentally altering cognitive appraisal. J Abnorm Psychol. 1964;69:195-205.
- 48. Goldfried MR. Systematic desensitization as training in self-control. J Consult Clin Psychol. 1971;37(2):228-34.
- 49. Bandura A. Vicarious processes: a case of no-trial learning. In: Berkowitz L, editor. Advances in experimental social psychology. Vol. 2. New York: Academic Press; 1965.
- 50. Meichenbaum DH. Cognitive-behavior modification New York: Plenum; 1977.
- 51. Lazarus AA, Davidson GC, Polefka DA. Classical and operant factors in the treatment of a school phobia. J Abnorm Psychol 1965;70:225-9.
- 52. Beck AT, Newman CF. Cognitive therapy. In: Kaplan & Sadock's. Comprehensive textbook of psychiatry 8th ed. New York: Lippincott Williams & Wilkins; 2005.
- 53. Clark DA, Beck AT, Alford BA. Scientific foundations of cognitive theory and therapy of depression New York: Wiley; 1999.
- 54. Beck AT. Cognition, affect, and psychopathology. Arch Gen Psychiatry. 1971;24(6):495-500.
- 55. Beck AT, Clark DA. An information processing model of anxiety: automatic and strategic processes. Behav Res Ther 1997;35(1):49-58.
- 56. Clark DA, Beck AT, Brown GK. Sociotropy, autonomy and life event perceptions in dysphoric and nondysphoric individuals. Cognit Ther Res 1992;16:635-52.
- 57. Beck JS. Cognitive therapy: basics and beyond New York: Guilford Press; 1995.
- 58. Gould RA, Otto MW, Pollack MH. A meta-analysis of treatment outcome for panic disorder. Clin Psychol Rev 1995;15(8):819-44.
- 59. Sokol L, Beck AT, Greenberg RL, Greenberg RL, Wright FD, Berchick RJ. Cognitive therapy of panic disorder: a nonpharmacological alternative. J Nerv Ment Dis 1989;177(12):711-6.
- 60. Clark DM, Salkovskis PM, Hackmann A, Middleton H, Anastasiades P, Gelder MG. A comparison with cognitive therapy, applied relaxation, and imipramine for the treatment of panic disorder. Br J Psychiatry 1994;164(6):759-69.
- 61. Gould RA, Buckminster S, Pollack MH, Otto MW, Yap L. Cognitive behavioral and pharmacological treatment for social phobia: a meta-analysis. Clin Psychol Sci Pract 1997;4:291-306.
- 62. Taylor S. Meta-analysis of cognitive-behavioral treatments for social phobia. J Behav Ther Exp Psychiatry 1996;27(1):1-9.
- 63. Clark DM, Ehlers A, McManus F, Hackman A, Fennell M, Campbell H, Flower T, Davenport C, Louis B. Cognitive therapy versus fluoxetine in generalized social phobia: a randomized placebo-controlled trial. J Consult Clin Psychol 2003;71(6):1058-67.
- 64. Butler G, Fennell M, Robson P, Gelder M. Comparison of behavior therapy and cognitive behavior therapy in the treatment of generalized anxiety disorder. J Consult Clin Psychol 1991;59(1):167-75.
- 65. Gloaguen V, Cottraux J, Cucherat M, Blackburn IM. A meta-analysis of the effects of cognitive therapy in depressed patients. J Affect Disord 1998;49(1):59-72.
- 66. DeRubeis RJ, Hollon SD, Amsterdam JD, Shelton RC, Young PR, Salomon RM, O'Reardon JP, Lovett ML, Gladis MM, Brown LL, Gallop R. Cognitive therapy vs. medications in the treatment of moderate to severe depression. Arch Gen Psychiatry 2005;62(4):409-16.
- 67. DeRubeis RJ, Gelfand LA, Tang TZ, Simons AD. Medications versus cognitive behavior therapy for severely depressed outpatients: mega-analysis of four randomized comparisons. Am J Psychiatry 1999;156(7):1007-13.
- 68. Meyer JH, McMain S, Kennedy SH, Korman L, Brown GM, DaSilva JN, Wilson AA, Blak T, Eynan-Harvey R, Goulding BS, Houle S, Links P. Dysfunctional attitudes and 5-HT-sub-2 receptors during depression and self-harm. Am J Psychiatry 2003;160(1):90-9.
- 69. Meyer JH, Houle S, Sagrati S, Carella A, Hussey DF, Ginovart N, Goulding V, Kennedy J, Wildon AA. Brain serotonin transporter binding potential measured with carbon 11-labeled DASB positron emission tomography. Arch Gen Psychiatry 2004;61(12):1271-9.
- 70. Beck AT. Cognitive therapy: a 30-year retrospective. Am Psychol. 1991;46(4):368-75.
- 71. Beck AT. The evolution of the cognitive model of depression and its neurobiological correlates. Am J Psychiatry. 2008;165(8): 969-77.
Publication Dates
-
Publication in this collection
17 Nov 2008 -
Date of issue
Oct 2008