Abstracts
OBJECTIVE: The aim of this study was to evaluate the effects that a particular psychopharmacological treatment has on personality patterns in patients with panic disorder. METHOD: Forty-seven patients with panic disorder and 40 controls were included in the study. The Mini International Neuropsychiatric Interview and Minnesota Multiphasic Personality Inventory were used to assess Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, diagnoses and personality traits, respectively. Patients were treated with sertraline for 16 weeks. RESULTS: There was a significant decrease in the score on 8 of the 10 Minnesota Multiphasic Personality Inventory scales. In addition, neurotic triad and psychasthenia personality scores were higher among panic disorder patients, even during the posttreatment asymptomatic phase, than among controls. CONCLUSION: In the asymptomatic phase of the disease, panic disorder patients present a particular neurotic/anxious personality pattern. This pattern, although altered in the presence of acute symptoms, could be a focus of research.
Panic disorder; Personality; Psychopharmacology; Sertraline; Treatment outcome
OBJETIVO: O objetivo do estudo foi avaliar os efeitos do tratamento psicofarmacológico nos padrões de personalidade em pacientes com transtorno do pânico. MÉTODO: Quarenta e sete pacientes com transtorno do pânico e 40 controles foram incluídos no estudo. O Mini International Neuropsychiatric Interview e o Inventário Multifásico Minnesota de Personalidade foram usados para avaliar os diagnósticos do Manual Diagnóstico e Estatístico de Doenças Mentais - Quarta Edição e os traços de personalidade, respectivamente. Os pacientes foram tratados com sertralina por 16 semanas. RESULTADOS: Houve uma diminuição significativa nos escores de 8 das 10 escalas do Inventário Multifásico Minnesota de Personalidade. Adicionalmente, os pacientes com transtorno do pânico apresentaram maiores escores de personalidade da tríade neurótica e de psicastenia quando comparados aos controles, mesmo após o tratamento na fase assintomática. CONCLUSÃO: Pacientes com transtorno do pânico apresentam um padrão de personalidade neurótico/ansioso na fase assintomática da doença que, mesmo que influenciado pela presença de sintomas agudos, pode ser foco de pesquisa.
Transtorno de pânico; Personalidade; Psicofarmacologia; Sertralina; Resultado de tratamento
ORIGINAL ARTICLE
Can psychopharmacological treatment change personality traits in patients with panic disorder?
O tratamento psicofarmacológico pode mudar traços de personalidade em pacientes com transtorno do pânico?
Letícia KipperI, II; Cláudia WachleskiI, II; Giovanni Abrahão SalumI, II; Elizeth HeldtI, II; Carolina BlayaI, II; Gisele Gus ManfroI, II
IPostgraduate Program in Medical Sciences: Psychiatry, Universidade Federal do Rio Grande do Sul (UFRGS), Porto Alegre (RS), Brazil
IIAnxiety Disorder Program, Hospital de Clínicas de Porto Alegre (HCPA), Porto Alegre (RS), Brazil
Correspondence Correspondence: Gisele Gus Manfro, MD, PhD Luis Manoel Gonzaga, 630/11 Phone/Fax: (+55 51) 2101-8294/(+55 51 3328-9234) 90470-280 Porto Alegre, RS, Brazil E-mail: gmanfro@portoweb.com.br
ABSTRACT
OBJECTIVE: The aim of this study was to evaluate the effects that a particular psychopharmacological treatment has on personality patterns in patients with panic disorder.
METHOD: Forty-seven patients with panic disorder and 40 controls were included in the study. The Mini International Neuropsychiatric Interview and Minnesota Multiphasic Personality Inventory were used to assess Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition, diagnoses and personality traits, respectively. Patients were treated with sertraline for 16 weeks.
RESULTS: There was a significant decrease in the score on 8 of the 10 Minnesota Multiphasic Personality Inventory scales. In addition, neurotic triad and psychasthenia personality scores were higher among panic disorder patients, even during the posttreatment asymptomatic phase, than among controls.
CONCLUSION: In the asymptomatic phase of the disease, panic disorder patients present a particular neurotic/anxious personality pattern. This pattern, although altered in the presence of acute symptoms, could be a focus of research.
Descriptors: Panic disorder; Personality; Psychopharmacology; Sertraline; Treatment outcome
RESUMO
OBJETIVO: O objetivo do estudo foi avaliar os efeitos do tratamento psicofarmacológico nos padrões de personalidade em pacientes com transtorno do pânico.
MÉTODO: Quarenta e sete pacientes com transtorno do pânico e 40 controles foram incluídos no estudo. O Mini International Neuropsychiatric Interview e o Inventário Multifásico Minnesota de Personalidade foram usados para avaliar os diagnósticos do Manual Diagnóstico e Estatístico de Doenças Mentais - Quarta Edição e os traços de personalidade, respectivamente. Os pacientes foram tratados com sertralina por 16 semanas.
RESULTADOS: Houve uma diminuição significativa nos escores de 8 das 10 escalas do Inventário Multifásico Minnesota de Personalidade. Adicionalmente, os pacientes com transtorno do pânico apresentaram maiores escores de personalidade da tríade neurótica e de psicastenia quando comparados aos controles, mesmo após o tratamento na fase assintomática.
CONCLUSÃO: Pacientes com transtorno do pânico apresentam um padrão de personalidade neurótico/ansioso na fase assintomática da doença que, mesmo que influenciado pela presença de sintomas agudos, pode ser foco de pesquisa.
Descritores: Transtorno de pânico; Personalidade; Psicofarmacologia; Sertralina; Resultado de tratamento
Introduction
Panic disorder has a chronic, recurrent course, and many patients present partial remission and episodes of relapse after years of treatment.1-3 Comorbidity of panic disorder with personality disorder has received attention as a factor that might contribute to chronicity and to the difficulty of treating certain panic disorder patients.4
The reported prevalence of this comorbidity ranges from 30% to 69%, this considerable variation likely being attributable to the different methodologies employed, especially the type of instrument used to assess personality, as well as to differences among the patient samples evaluated.5-9 Grant et al. studied panic disorder patients with agoraphobia who sought treatment and found that the prevalence of at least one personality disorder was as high as 75%.10 Considering the high frequency of comorbidity of panic disorder and personality disorder, together with the fact that both tend to have a chronic course, the possible clinical impact of this association becomes important.
The most common personality disorders described in symptomatic panic disorder patients are cluster C (anxious) disorders, which include avoidant, dependent and obsessive-compulsive personality disorders, followed by histrionic, borderline and paranoid disorders.6,10-12 However, there have been few studies of the asymptomatic stage of the disorder,12 making it difficult to evaluate which of the personality characteristics reported are primary and inherent to the personality of the subjects and which are a consequence of reorganization of their functioning due to panic disorder symptoms.
The impact of personality traits on the risk for panic disorder and on its treatment, as well as the stability of a personality disorder diagnosis continue to be an object of discussion.13,14 Personality traits and disorders are by definition a highly stable behavior pattern. However, in recent years, some authors have questioned this stability, suggesting that personality characteristics can be influenced by acute symptoms and by time frame.15-17 This differentiation between Axis I and Axis II, or subsyndromal symptoms and personality traits, is a controversial issue, although there is little evidence to provide the theoretical bases for its study.18
The aim of the present exploratory study was to discuss the following question: can psychopharmacological treatment change personality traits in patients with panic disorder? We hypothesize that there is a neurotic personality pattern in patients with panic disorder that is persistent even in the asymptomatic phase after pharmacological treatment.
Method
1. Participants and study design
The study sample was composed of patients who sought medical care at the Anxiety Disorders Outpatient Clinic of the Department of Psychiatry of the Hospital de Clínicas de Porto Alegre (HCPA), in the city of Porto Alegre, Brazil, or who were selected directly for the study. Through consecutive sampling, we included patients over 18 years of age who met the Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition (DSM-IV) diagnostic criteria for panic disorder, had anticipatory anxiety and avoidance symptoms, had had at least two panic attacks in the previous month and had not undergone any type of treatment (pharmacotherapy or psychotherapy) within the last 4 months. The control group comprised normal volunteers, all of whom were employees of the HCPA and did not meet the diagnostic criteria for any Axis I psychiatric disorders.
The panic disorder patients were assigned to receive pharmacological treatment with sertraline, a selective serotonin reuptake inhibitor proven effective in treating panic disorder.19 The initial dose was 25mg/day in the first week and was increased until there was symptom remission or clinical evaluation revealed a major adverse effect. The maximum dose was 150mg/day, since patients who achieved remission did not require a higher dose and those who did not respond could not tolerate higher doses. Clonazepam was also used when deemed necessary. The mean dose of clonazepam was 1.16mg (SD = 0.6), although it was used in only 8 patients. The patients were treated for 16 weeks, evaluations being conducted at baseline, as well as at weeks 1, 2, 4, 6, 8, 10, 12, 14 and 16. The control group was evaluated at baseline and at week 16.
The following exclusion criteria were applied: mental retardation, dementia or other organic brain syndrome; alcohol or other substance dependence; psychotic disorders (schizophrenia or other psychotic diseases); disabling chronic diseases (any chronic disease that might disable the patients and could interfere with their affective or anxiety symptoms, or with their ability to complete the personality scales); and moderate to severe major depression (Hamilton scale score > 17). Mental retardation was ruled out using the Wechsler Adult Intelligence Scale-revised version. Organic brain syndrome and other disorders were ruled out using clinical interviews and the Mini International Neuropsychiatric Interview (MINI). Two of the control individuals were excluded because their tests were considered invalid on the basis of the Minnesota Multiphasic Personality Inventory (MMPI), lie and defensiveness validity scales, which evaluate attitudes related to the inventory and determine the validity of the clinical scales.
All patients and controls gave written informed consent before participating in this study, the design of which was previously approved by the Research Ethics Committee of the HCPA (no. 01-055). Part of the sample has been described in previous studies.20,21
2. Instruments
1) Diagnostic procedures
Prior to their inclusion in the study, the panic disorder patients and the control individuals were evaluated by trained psychiatrists using a clinical interview and the Mini International Neuropsychiatric Interview (MINI) Brazilian version 5.0.0 DSM IV, a standardized and structured diagnostic interview that evaluates the main Axis I psychiatric disorders according to the DSM-IV criteria.22 The MINI was also employed to evaluate comorbidity. Demographic data were collected using a structured clinical interview developed specifically for this study.
Personality characteristics were evaluated using the MMPI. The MMPI was applied by a trained psychologist in two 60-min interviews that were carried out prior to and after 16 weeks of treatment in the case of panic disorder patients and at baseline in the control group. The same psychologist applied the MMPI before and after treatment and was blind to the clinical evolution of the patients. The MMPI is an instrument widely used in clinical practice and in research. The Portuguese-language version employed in the present study has been standardized and adapted for use in Brazil. It contains 566 true-or-false questions organized into ten clinical scales in order to identify the following personality traits: hypochondriasis (Hs); depression (D); hysteria (Hy); psychopathic deviate (Pd); masculinity-femininity (MF); paranoia (Pa); psychasthenia (Pt); schizophrenia (Sc); hypomania (Ma) and introversion-extroversion (Si). It also presents four validity scales (uncertainty, lie, error and correction/defensiveness), which evaluate attitudes related to the inventory and determine the validity of the clinical scales. In accordance with classification system devised by Hathaway and McKinley,23 the MMPI scores were defined as pathological (> 70), high (55-69) or normal-to-low (< 54). The combination of hypochondriasis, depression and hysteria is known as the neurotic triad.23,24
2) Symptom severity
The response to pharmacological treatment and the severity of the disease were determined using the Panic Inventory, Clinical Global Impression (CGI) scale, Hamilton Rating Scale for Anxiety (HAM-A)25 and Hamilton Rating Scale for Depression (HAM-D),26 all applied before and after treatment in panic disorder patients. The Panic Inventory is an instrument that classifies panic attacks as spontaneous, situational, complete or incomplete. It also assesses attacks in terms of intensity (rated on a scale from 0 to 10), duration (minutes) and frequency, as well as the severity of agoraphobia and anticipatory anxiety (rated on a scale from 0 to 10, i.e., none to extreme).20,21,27 A panic-specific version of the CGI scale was used. The CGI provides a global rating of severity of panic disorder, with scores ranging from 1 (normal, not ill) to 7 (extremely ill), according to the frequency and intensity of panic attacks, level of anticipatory anxiety, level of phobic avoidance and role (familial, social or occupational) dysfunction.28 In consonance with previous studies, the criteria applied for total remission of symptoms were CGI < 2 and cessation of panic attacks by the end of the treatment.20,21,27,29
3. Statistical analysis
The sample size was based on a previous study, with an alpha of 0.05 and a power of 80%, resulting in 40 patients and 40 controls. Data are presented as number (percentage), median (interquartile range) and mean (standard deviation). The Kolmogorov-Smirnov test and Levene's test were used to evaluate Gaussian distribution and equality of variances, respectively.
Continuous clinical and sociodemographic variables were analyzed using t-tests for independent samples. In order to correlate the CGI and HAM-A scores with the personality scales measured by MMPI, Pearson's correlation coefficient was used. Comparisons between patients and controls, in terms of baseline scores, as well as between asymptomatic patients and controls, were made using t-tests for independent samples. Comparisons between pretreatment and posttreatment patient scores were made using t-tests for paired samples. In order to analyze differences in baseline MMPI scores between patients and controls, between patients who were asymptomatic after treatment and controls and between pretreatment and posttreatment patient scores, only those patients who completed the study (n = 40) were included in the data analysis. The entire statistical analysis was made with the Statistical Package for the Social Sciences, version 14.0 (SPSS Inc., Chicago, IL, USA). The level of significance was set at α = 0.05, and 95% confidence intervals were used.
Results
1. Clinical and demographic data
Forty-seven patients with panic disorder and 40 controls were included in the study. Of the 47 patients, 7 dropped out or were excluded from the analysis before week 16 (2 due to adverse effects, 1 due to pregnancy, 3 due to noncompliance with the treatment and 1 due to failure to submit to all final tests). There were no statistically significant differences between patients who completed the study and those who did not in terms of the demographic variables and clinical scores at baseline (data not shown). In addition, there were no statistically significant differences between patients and controls considering demographic data (data not shown). Of the 47 patients with panic disorder, 43 (91.5%) also had agoraphobia, 19 (40.4%) had generalized anxiety disorder, 12 (25.5%) had mild depression, 4 (8.5%) had social phobia, 2 (4.3%) had dysthymia, and 1(2.1%) had obsessive-compulsive disorder. Severity at baseline ranged from moderate to severe (mean CGI, 4.4 ± 0.87), agoraphobia intensity (on a scale of 0 to 10) was 6.9 ± 2.82, and anticipatory intensity (also on a scale of 0 to 10) was 8.2 ± 2.60. The mean HAM-A and HAM-D scores at baseline were 25.5 ± 5.68 and 11 ± 3.48, respectively. Twenty-six patients (65%) achieved total remission by the end of the 16 weeks of treatment.
2. Personality and severity in patients with panic disorder
Four of the MMPI scales correlated significantly with the CGI-scale severity of panic disorder at baseline: depression (r = 0.436; p = 0.005); paranoia (r = 0.431; p = 0.006); psychasthenia (r = 0.433; p = 0.005); and schizophrenia (r = 0.363; p = 0.021). Nine of the MMPI scales presented significant positive correlations with the baseline HAM-A scores in patients and controls: hypochondriasis (r = 0.768; p < 0.001); depression (r = 0.666; p < 0.001); hysteria (r = 0.702; p < 0.001); psychopathic deviate (r = 0.368; p = 0.001); paranoia (r = 0.521; p < 0.001); psychasthenia (r = 0.752; p < 0.001); schizophrenia (r = 0.649; p < 0.001); hypomania (r = 0.275; p = 0.014); and introversion-extroversion (r = 0.548; p < 0.001).
3. Personality comparison between PD patients and controls
Figure 1 shows the mean baseline scores on the MMPI clinical scales for the panic disorder patients (n = 40) and for the controls (n = 40). The patients differed from the controls on nine of the ten scales, presenting significantly higher mean scores for hypochondriasis, depression, hysteria, psychopathic deviate, paranoia, psychasthenia, schizophrenia and introversion-extroversion (p < 0.001), although there was no significant difference for the hypomania score (p = 0.059). On the masculinity-femininity scale, the controls presented higher mean scores than did the patients (p = 0.014).
The mean MMPI scores for the controls (n = 40) and for the patients who were asymptomatic after treatment (n = 26) are shown in Figure 2. Patients achieving remission scored higher on the hypochondriasis, depression and hysteria (neurotic triad) scales, as well as on the psychasthenia scale, than did the controls (p < 0.05).
4. Personality comparison in all PD patients pretreatment (n = 40) and posttreatment (n = 40)
In a quantitative analysis of the MMPI scores, we found that the scores on eight of the ten clinical scales were significantly lower after the 16 weeks of pharmacological treatment. The only exceptions were the masculinity-femininity and hypomania subscales. The results can be seen in Figure 3.
Discussion
The present study identified a personality pattern characterized by higher rates of pathological personality traits as compared to control subjects, in a sample of Brazilian panic patients with low rates of major psychiatric comorbidities. Most importantly, the higher and pathological traits described were the anxious and neurotic type. In addition, the panic disorder patients who were asymptomatic after the pharmacological treatment continued to present a personality pattern that differed from that of the controls in terms of the anxious and neurotic personality characteristics. These data corroborate previous findings of a higher prevalence of maladaptive defense styles, as well as the presence of neuroticism, in these patients.20,30 Furthermore, the panic disorder patients presented a significant posttreatment decrease in certain personality characteristics, whereas others remained stable.
On the basis of these data, we can suggest that these patients present a neurotic personality pattern (hypochondriasis, depression, hysteria and psychasthenia), as observed during the asymptomatic phase of the illness, and that this pattern might be reinforced by acute symptoms. The fact that patients maintain these neurotic traits indicates that these personality characteristics could increase the probability of developing panic disorder, although the study design did not allow this conclusion to be drawn. This is in accordance with the findings of studies showing psychological vulnerability prior to the onset of panic disorder31 and is in agreement with those of a recent prospective longitudinal study demonstrating that a personality disorder in early adulthood increases the risk for panic disorder in middle adulthood.15
It is difficult to evaluate personality disorders in patients with acute panic disorder due to the influence that anxiety can have on self-evaluation and self-reporting of personality traits. This influence is evidenced by the difference between pretreatment and posttreatment personality scores, which is in agreement with the findings of earlier studies.12 However, despite the fact that these differences were statistically significant, the clinical implications of most of the changes are questionable, since most of the patients who presented abnormal (pathological or high) personality trait scores at baseline continued to present abnormal scores after treatment. In our sample, it seems that anxiety exacerbated an already existing high or pathological personality trait, although the study design did not allow this conclusion to be drawn. This is in accordance with the results obtained in the study conducted by Marchesi et al., who showed that the improvement of panic disorder symptoms was related to normalization of paranoid traits and a reduction but persistence of avoidant and dependent traits.8
Thus, can psychopharmacological treatment change personality traits in panic disorder patients? There is no simple answer to this question. On the one hand, we can say yes, since we observed some changes in MMPI scale scores over a 16-week period of treatment with sertraline. However, as previously discussed, the clinical implications of our findings are unknown. Due to the study design, we cannot determine which came first: the dysfunctional personality traits or the panic disorder. On the other hand, we can say no, if we assume that the change in MMPI scores is minimal, and we were able to identify a persistent type of personality even in asymptomatic patients.
Another question that arises in this scenario is whether symptoms and personality traits are two distinct phenomena. The categorical division between Axis I and II diagnostic criteria might be antiquated and could actually be considered a spectrum that shares a common origin with overlapping symptoms and characteristics, especially in patients with anxiety disorders or depression. There is a current tendency to put symptoms and personality traits on the same level, both being considered to be determined by genetic and environment factors.32
This study has some limitations. First, the study design did not allow us to determine whether these traits developed prior to the onset of panic disorder. In addition, the evaluator of personality traits was not blinded to the MINI results. Furthermore, the control group selected might not be representative of the general population, and it might not be possible to generalize the results to other clinical or community samples of patients with panic disorder. Moreover, the small sample size and the instrument used to measure personality might also represent limiting factors. Finally, this study evaluated changes in Axis II disorders after pharmacological treatment that was short-term.
Conclusion
Our findings suggest that panic disorder patients present a particular neurotic and anxious personality pattern that can be influenced by acute symptoms. However, certain personality patterns remain unchanged in the posttreatment asymptomatic phase and could be the focus of future studies. Although we do not intend to provide definitive answers to these complex questions, we have added to the current knowledge regarding the overlap between Axis I and II disorders and their clinical implications. Therefore, it is important to continue studying factors that might be associated with higher morbidity in panic disorder, in order to develop more effective treatment strategies. If some personality traits remain stable after remission, those traits might be associated with further relapses. Since this study evaluated only psychopharmacological treatment, psychotherapeutic interventions should also be investigated in future studies. Therefore, additional long-term cohort studies are needed in order to evaluate the role of personality disorder in a population at risk for anxiety disorders (e.g., behaviorally inhibited children or high anxiety-sensitive individuals), as well as to evaluate the long-term impact of panic disorder treatment on personality traits and disorders.
Acknowledgments
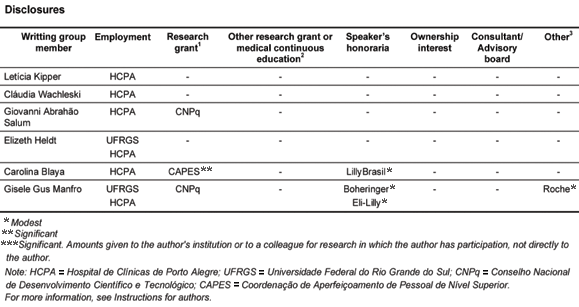
This study received financial support from the Fundo de Incentivo à Pesquisa do Hospital de Clínicas de Porto Alegre (FIPE-HCPA). Carolina Blaya is the recipient of a research grant from the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES). Cláudia Wachleski, Giovanni Abrahão Salum and Gisele Gus Manfro are the recipients of research grants from the Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq).
Submitted: January 30, 2009
Accepted: April 15, 2009
- 1. Andersch S, Hetta J. A 15-year follow-up study of patients with panic disorder. Eur Psychiatry. 2003;18(8):401-8.
- 2. Carpiniello B, Baita A, Carta MG, Sitzia R, Macciardi AM, Murgia S, Altamura AC. Clinical and pscychosocial outcome of patients affected by panic disorder with or without agoraphobia: results from a naturalistic follow-up study. Eur Psychiatry. 2002;17(7):394-8.
- 3. Manfro GG, Heldt E, Cordioli AV, Otto MW. Cognitive-behavioral therapy in panic disorder. Rev Bras Psiquiatr. 2008; 30(2):s81-7.
- 4. Pollack MH, Smoller JW. The longitudinal course and outcome of panic disorder. Psychiatr Clin North Am. 1995;18(4):785-801.
- 5. Albert U, Maina G, Bergesio C, Bogetto F. Axis I and II comorbidities in subjects with and without nocturnal panic. Depress Anxiety. 2006;23(7):422-8.
- 6. Dammen T, Ekeberg O, Arnesen H, Friis S. Personality profiles in patients referred for chest pain. Investigation with emphasis on panic disorder patients. Psychosomatics. 2000;41(3):269-76.
- 7. Latas M, Starcevic V, Trajkovic G, Bogojevic G. Predictors of comorbid personality disorders in patients with panic disorder with agoraphobia. Compr Psychiatry. 2000;41(1):28-34.
- 8. Marchesi C, Cantoni A, Fonto S, Gianelli MR, Maggini C. The effect of pharmacotherapy on personality disorders in panic disorder: a one year naturalistic study. J Affect Disord. 2005;89(1-3):189-94.
- 9. Marchesi C, De Panfilis C, Cantoni A, Fonto S, Gianelli MR, Maggini C. Personality disorders and response to medication treatment in panic disorder: a 1-year naturalistic study. Prog Neuropsychopharmacol Biol Psychiatry. 2006;30(7):1240-5.
- 10. Grant BF, Hasin DS, Stinson FS, Dawson DA, Patricia Chou S, June Ruan W, Huang B. Co-ocurrence of 12-month mood and anxiety disorders and personality disorders in the US: results from the national epidemiologic survey on alcohol and related conditions. J Psychiatr Res. 2005;39(1):1-9.
- 11. Ampollini P, Marchesi C, Signifredi R, Ghinaglia E, Scardovi F, Codeluppi S, Maggini C. Temperament and personality features in patients with major depression, panic disorder and mixed conditions. J Affect Disord. 1999;52(1-3):203-7.
- 12. Hoffart A, Hedley LM. Personality traits among panic disorder with agoraphobia patients before and after symptom-focused treatment. J Anxiety Disord. 1997;11(1):77-87.
- 13. Johnson JG, Cohen P, Kasen S, Brook JS. Personality disorders evident by early adulthood and risk for anxiety disorders during middle adulthood. J Anxiety Disord. 2006;20(4):408-26.
- 14. Mennin DS, Heimberg RG. The impact of comorbid mood and personality disorders in the cognitive-behavioral treatment of panic disorder. Clin Psychol Rev. 2000;20(3):339-57.
- 15. Rocca WA, Grossardt BR, Peterson BJ, Bower JH, Trenerry MR, Ahlskog JE, Sanft KR, de Andrade M, Maraganore DM. The Mayo Clinic cohort study of personality and aging: design and sampling, reliability and validity of instruments, and baseline description. Neuroepidemiology. 2006;26(3):119-29.
- 16. Seivewright H, Tyrer P, Johnson T. Change in personality status in neurotic disorders. Lancet. 2002;359(9325):2253-4.
- 17. Corchs F, Corregiari F, Ferrão YA, Takakura T, Mathis ME, Lopes AC, Miguel EC, Bernik M. Personality traits and treatment outcome in obsessive-compulsive disorder. Rev Bras Psiquiatr. 2008;30(3):246-50.
- 18. Crawford TN, Cohen P, First MB, Skodol AE, Johnson JG, Kasen S. Comorbid Axis I and Axis II disorders in early adolescence. Outcomes 20 Years Later. Arch Gen Psychiatry. 2008;65(6):641-8.
- 19. Rapaport MH, Wolkow R, Hackett E, Pollack M, Ota KY. Sertraline treatment of panic disorder: results of a long-term study. Acta Psychiatr Scand. 2001;104(4):289-98.
- 20. Kipper L, Blaya C, Teruchkin B, Heldt E, Isolan L, Mezzomo K, Bond M, Manfro GG. Evaluation of defense mechanisms in adult patients with panic disorder: before and after treatment. J Nerv Ment Dis. 2005;193(9):619-24.
- 21. Kipper L, Blaya C, Wachleski C, Dornelles M, Salum GA, Heldt E, Manfro GG. Trauma and defense style as response predictors of pharmacological treatment in panic patients. Eur Psychiatry. 2007;22(2):87-91.
- 22. Amorim P. Mini International Neuropsychiatric Interview (MINI): validação de entrevista breve para diagnóstico de transtornos mentais. Rev Bras Psiquiatr. 2000;22(3):106-15.
- 23. Hathaway SR, McKinley JC. Inventário Multifásico Minesota de Personalidade (MMPI). Manual de Psicologia Aplicada. Rio de Janeiro: CEPA; 1971.
- 24. Cunha JA. In: Psicodiagnóstico-V. 5a ed. rev. e ampl. Porto Alegre: Artmed; 2003. p.439-506.
- 25. Hamilton M. The assessment of anxiety states by rating. Br J Med Psychol. 1959;32(1):50-5.
- 26. Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry. 1960;23:56-62.
- 27. Heldt E, Gus Manfro G, Kipper L, Blaya C, Isolan L, Otto MW. One-year follow up of pharmacotherapy-resistant patients with panic disorder treated with cognitive-behavior therapy: outcome and predictors of remission. Behav Res Ther. 2006;44(5):657-65.
- 28. Guy W. CGI - Clinical Global Impressions. In: Guy W, editor. ECDEU Assessment Manual for Psychopharmacology. Rev Rockville, MD.: National Institute of Mental Health: 1976. p.217-22.
- 29. Pollack MH, Rapaport MH, Fayyad R, Otto MW, Nierenberg AA, Clary CM. Early improvement predicts endpoint remission status in sertraline and placebo treatments of panic disorder. J Psychiatr Res. 2002;36(4):229-36
- 30. Hettema JM, Neale MC, Myers JM, Prescott CA, Kendler KS. A population-based twin study of the relationship between neuroticism and internalizing disorders. Am J Psychiatry. 2006;163(5):857-64.
- 31. Manfro GG, Otto MW, McArdle ET, Worthington JJ 3rd, Rosenbaum JF, Pollack MH. Relationship of antecedent stressful life events to childhood history and family of anxiety and the course of panic disorder. J Affect Disord. 1996;41(2):135-9.
- 32. Smoller JW, Gardner-Schuster E, Misiaszek M. Genetics of anxiety: would the genome recognize the DSM? Depress Anxiety. 2008;25(4):368-77.
Correspondence:
Publication Dates
-
Publication in this collection
22 Jan 2010 -
Date of issue
Dec 2009
History
-
Accepted
15 Apr 2009 -
Received
30 Jan 2009