Abstracts
Objective: We aimed to assess the presence of suicidal ideation, depressive symptoms and symptoms of hopelessness in three healthcare training programs. Method: The study's population comprised all students enrolled at the Medical School of the Fundação do ABC, Brazil, from 2006 to 2007 compared to students enrolled in nursing and pharmacy programs. We applied the Beck Scale for Suicidal Ideation, the Beck Depression Inventory and the Beck Hopeless Scale to assess psychiatric symptomatology. The general response rates of the medical, nursing, and pharmacy students were 56%, 56% and 61%, respectively. Results: There was no difference regarding the presence of suicidal ideation among medical, nursing and pharmacy students. There was also no difference regarding the presence of either depression or hopelessness in medical students in comparison to nursing and pharmacy students. In comparison to nursing and pharmacy students, significantly higher severity rates in terms of hopelessness were observed only among medical students. Conclusion: Although we did not observe significant differences regarding suicidal ideation and depression among the three healthcare programs, our findings suggest that the presence of suicidal ideation is indeed a source of concern. Early identification of these symptoms is crucial in order to offer appropriate support and treatment and prevent deaths by suicide.
Depression; Symptoms, psychic; Students, medical; Cross-sectional studies; Students; health occupations
Objetivo: Objetivou-se avaliar a presença de ideação suicida, sintomas depressivos e sintomas de desesperança entre três cursos da área da saúde. Método: A população do estudo consistiu de todos os estudantes de medicina matriculados na Faculdade de Medicina da Fundação do ABC, Brasil, durante 2006 e 2007, comparados com os alunos matriculados nos cursos de enfermagem e farmácia. Aplicamos a Escala de Ideação Suicida de Beck, o Inventário de Depressão de Beck e a Escala de Desesperança de Beck para avaliar sintomatologia psiquiátrica. A taxa de resposta entre os estudantes de medicina, enfermagem e farmácia foi de 56%, 56% e 61%, respectivamente. Resultados: Não houve diferença em relação à presença de ideação suicida entre os estudantes de medicina, enfermagem e farmácia. Também não houve diferença em relação à presença de depressão ou desesperança nos estudantes de medicina em comparação com os alunos de enfermagem e farmácia. Taxas de gravidade significativamente mais elevadas foram observadas apenas em desesperança entre os estudantes de medicina em comparação com os alunos de enfermagem e farmácia. Conclusão: Embora não tenhamos observado diferenças significativas entre os três cursos da área da saúde com relação à ideação suicida e depressão, a presença de ideação suicida é um achado preocupante. A identificação precoce destes sintomas é fundamental, de modo a se oferecer apoio e tratamento adequados e prevenir mortes por suicídio.
Depressão; Sintomas Psíquicos; Estudantes de medicina; Estudos transversais; Estudantes de ciências da saúde
ORIGINAL ARTICLE
Suicidal ideation among students enrolled in healthcare training programs: a cross-sectional study
Ideação suicida entre estudantes da área da saúde: um estudo transversal
Clóvis Alexandrino-SilvaI, II; Maira Lazarini Guimarães PereiraI; Carlos BustamanteI; André Corrêa de Toledo FerrazI; Sergio BaldassinI; Arthur Guerra de AndradeI, II; Tânia Corrêa de Toledo Ferraz AlvesI, II
IDepartment of Psychiatry, Medical School, Fundação do ABC, Santo André (SP), Brazil
IIDepartment of Psychiatry, Medical School, Universidade de São Paulo (USP), São Paulo (SP), Brazil
Correspondence Correspondence : Clóvis Alexandrino-Silva Av. Lauro Gomes, 2000 09060-870 Santo André, SP, Brazil Phone/Fax: (+55 11) 4993-7295 Email: alexandrinojr@yahoo.com.br
ABSTRACT
OBJECTIVE: We aimed to assess the presence of suicidal ideation, depressive symptoms and symptoms of hopelessness in three healthcare training programs.
METHOD: The study's population comprised all students enrolled at the Medical School of the Fundação do ABC, Brazil, from 2006 to 2007 compared to students enrolled in nursing and pharmacy programs. We applied the Beck Scale for Suicidal Ideation, the Beck Depression Inventory and the Beck Hopeless Scale to assess psychiatric symptomatology. The general response rates of the medical, nursing, and pharmacy students were 56%, 56% and 61%, respectively.
RESULTS: There was no difference regarding the presence of suicidal ideation among medical, nursing and pharmacy students. There was also no difference regarding the presence of either depression or hopelessness in medical students in comparison to nursing and pharmacy students. In comparison to nursing and pharmacy students, significantly higher severity rates in terms of hopelessness were observed only among medical students.
CONCLUSION: Although we did not observe significant differences regarding suicidal ideation and depression among the three healthcare programs, our findings suggest that the presence of suicidal ideation is indeed a source of concern. Early identification of these symptoms is crucial in order to offer appropriate support and treatment and prevent deaths by suicide.
Descriptors: Depression; Symptoms, psychic; Students, medical; Cross-sectional studies; Students, health occupations
RESUMO
OBJETIVO: Objetivou-se avaliar a presença de ideação suicida, sintomas depressivos e sintomas de desesperança entre três cursos da área da saúde.
MÉTODO: A população do estudo consistiu de todos os estudantes de medicina matriculados na Faculdade de Medicina da Fundação do ABC, Brasil, durante 2006 e 2007, comparados com os alunos matriculados nos cursos de enfermagem e farmácia. Aplicamos a Escala de Ideação Suicida de Beck, o Inventário de Depressão de Beck e a Escala de Desesperança de Beck para avaliar sintomatologia psiquiátrica. A taxa de resposta entre os estudantes de medicina, enfermagem e farmácia foi de 56%, 56% e 61%, respectivamente.
RESULTADOS: Não houve diferença em relação à presença de ideação suicida entre os estudantes de medicina, enfermagem e farmácia. Também não houve diferença em relação à presença de depressão ou desesperança nos estudantes de medicina em comparação com os alunos de enfermagem e farmácia. Taxas de gravidade significativamente mais elevadas foram observadas apenas em desesperança entre os estudantes de medicina em comparação com os alunos de enfermagem e farmácia.
CONCLUSÃO: Embora não tenhamos observado diferenças significativas entre os três cursos da área da saúde com relação à ideação suicida e depressão, a presença de ideação suicida é um achado preocupante. A identificação precoce destes sintomas é fundamental, de modo a se oferecer apoio e tratamento adequados e prevenir mortes por suicídio.
Descritores: Depressão; Sintomas Psíquicos; Estudantes de medicina; Estudos transversais; Estudantes de ciências da saúde
Introduction
Studies have shown that, compared to the general population, physicians present elevated suicide rate ratios,1 a fact that represents a serious public health problem. Botega et al. investigated the life prevalence rates of suicidal ideation, suicidal plans and suicide attempts in Campinas, a city of roughly one million inhabitants located in the Southeast of Brazil.2 The authors found life prevalence rates of 17.1% for suicidal ideation, 4.8% for plans and 2.8% for suicide attempts. Several studies have supported the connection between risk for suicide and hopelessness and depression.3,4 It is known that approximately 90% of those who commit suicide have a diagnosed mental illness, with depression figuring among the major causes of suicide and suicide attempts.2,5
The high prevalence of suicides, depression, abusive use of psychotropic drugs and professional dysfunction among physicians has been extensively described.6-8 Previous studies have also indicated that a substantial proportion of medical students9-12 and students from other healthcare areas such as nursing,13 dentistry,14 and pharmacy15 experience a significant burden in the shape of psychological morbidity and distress throughout the course of their studies.16-19 However, the connection between professional psychological morbidity and suicide has not been substantiated or quantified.
Tyssen et al. investigated the presence of suicidal ideation among medical students and young physicians.20 The authors described the prevalence of 14, 8, and 1.4% of suicidal ideations, suicide plans, and suicide attempts respectively, starting at the last year of medical school down through to the end of the first year at the hospital.20 The presence of suicidal ideation is related to the development of depressive and anxiety symptomatology.21,22 On one hand, most studies conducted in this field of study have focused on medical students20,23,24 given the vicissitudes of their coursework, which exposes them to several sources of distress ranging from the admission process down to graduation, including contact with death, pathologic processes, the first physical examination of a patient, the fear of acquiring diseases and feelings of inadequacy. On the other hand, several studies on the psychological well-being of students enrolled in other healthcare programs showed that these programs were similar in terms of the psychological distress caused to students due to performance-related challenges arising from their various academic activities.13-18
Comparisons between medical students and students from other undergraduate training programs as to the existence of depressive and anxiety symptoms are scarce in numbers.25 Medical students were found to experience less stress than law students, graduate students and the general population, although medical students fare worse in terms of stress scores and depressed mood when transitioning from basic to clinical training.25 However, when assessing the specificity of psychiatric symptoms in medical students, the use of students from different fields of knowledge as a basis for comparison may not be recommended because the latter represent different populations whose curriculum characteristics and methods of teaching-learning are quite different from those seen in medical training programs. Moreover, there is a lack of studies investigating the prevalence of suicidal ideation, depressive symptoms and hopelessness among medical students in comparison to students pursuing degrees in other healthcare areas.
Therefore, considering that medical students and students from other healthcare programs do share certain courses and that some of their activities do overlap both during training and practice, we believe that the study of students enrolled in different healthcare areas can help advance studies on the risk of medical students developing depression and anxiety. The present study addresses the following questions: do medical students have suicidal thoughts more often than nursing and pharmacy students? How prevalent is depressive symptomatology among medical students in comparison to nursing and pharmacy students? Does depressive symptomatology correlate with the presence of suicidal ideation in these populations of healthcare students?
Method
The ABC region Medical School Ethics Committee (process number 129/2006) approved this study, and written consent forms were obtained from all participating students. Forms were processed anonymously. The Student Health Service was notified of the study and enlisted should the answering of the questionnaire cause any distress to any of the participants.
1. Sampling
The study population consisted of all students enrolled at the Medical School of Fundação do ABC, Brazil, between 2006 and 2007 (n = 603) compared to students enrolled in nursing (n = 187) and pharmacy (n = 199) programs during the same period. Including freshman year, the medical degree is a 6-year long program, while the nursing and pharmacy degrees are both 4-year long programs. Worldwide, medical training programs vary in length from country to country i.e., some programs involve a 4-year graduate entry programs while other programs are 5 or 6 years long. In Brazil, we have a 6-year program and the medical curriculum is divided into 3 training stages: basic (1st and 2nd years), pre-clinical/clinical-theoretical (3rd and 4th years), and internship (5th and 6th years). The curriculum for the basic stage focuses on disciplines involving the study of both the structure and function of the cell and the human body (such as anatomy and biochemistry). The pre-clinical/clinical-theoretical stage focuses on internal medicine courses and preliminary clinical experience, plus an additional set of courses on the main medical areas (general medicine, public health, surgery, pediatrics and gynecology). The internship stage takes place at a general teaching hospital and at emergency units as part of a 2-year direct supervision practical training learning program.19
2. Collected data
The questionnaire was anonymous and consent was obtained. Information on age, gender, and course and grades was also obtained. Each classroom was visited more than once with the intention of rallying all students of each of the programs. Any student who did not fill out or return the questionnaire was considered a "loss".
We used the Beck Scale for Suicidal Ideation (BSI), a 21-item self-report questionnaire that was developed to detect and measure the severity of suicidal ideation in the general population. The questionnaire assesses the following symptomatology: wish to live, wish to die, reasons to live versus reasons to die, and active and passive suicidal ideation. If the respondent denied active or passive suicidal ideation, he/she was directed to the last two items of the questionnaire, which assess past suicide attempts and the wish to die during the last attempt. If the respondent admitted to at least some active or passive suicidal ideation, he/she completed item #'s 6-19. The BSI is one of the more thorough instruments for assessing the severity of suicidal ideation and one of the only assessment devices for assessing passive suicidal ideation. The total score yields a severity score, but individual items can be used as a screen for active suicidal ideation, passive suicidal ideation, and past suicide attempts.26 The presence of depressive symptoms among medical, nursing, and pharmacy students was assessed using the Beck Depression Inventory (BDI), a 21-item self-report inventory designed to measure the severity of depressive symptomatology.27 The measurement of depression was conducted in association with the Beck Hopeless Scale (BHS), a 20-item assessment device designed to measure negative expectations about the future. Individuals completing the BHS were asked to answer the questionnaire based on their attitudes during the preceding week.28 For the BDI, the answers were dichotomized between the presence and absence of major depressive symptoms based on a cutoff of 21 points.29,30
3. Statistical analysis
Results were analyzed using the Statistical Package for the Social Sciences (SPSS, version 12.0.1). The Kolmogorov-Smirnov test (KS-test) was used to determine whether the data was normally distributed. For the quantitative variables that were normally distributed (KS-test) with homogeneity of variances (Levene's test), a t-test was used; otherwise, the Mann-Whitney U test was used. Descriptive statistics are presented in terms of counts, percentages, means and standard deviations.
Initially, Chi-square tests were used to compare the prevalence of suicidal ideation, depression and hopelessness among the three student groups i.e., medical, nursing and pharmacy. Scores from the BSI or the BHS were used for the presence or absence of suicidal ideation and hopelessness respectively, and were dichotomized according to: equal to or different than zero. For the presence/absence of significant depressive symptoms, the scores from BDI were dichotomized using a cutoff of 21 points. Using this cutoff, we obtained a ROC curve with a sensitivity of 75% and specificity at 53% for the detection of depression.30
Subsequently, in order to investigate the severity of suicidal ideation, depressive symptoms and hopelessness across the three programs, the BSI, BDI and BHS scores were treated as continuous variables. We initially approached the three variables using the Multivariable Analysis of Variance (MANOVA) covariated for gender, with post-hoc Tukey corrected for multiple comparisons in order to ascertain if a connection between the three programs (medical, nursing, and pharmacy) and the scores from BSI, BDI, and BHS could be established while taking into account our sample's gender distribution differences. We then searched each program individually for psychiatric symptomatology using the Analysis of Variance (ANOVA) with post-hoc Tukey corrected for multiple comparisons across the grades. Finally, the association of suicide thoughts and depression was investigated using Pearson correlation coefficients. The significance level used was p < 0.05.
Results
1. Study sample
The overall response rate from the medical, nursing, and pharmacy student groups were 56, 56, and 61%, respectively. The statistical power of the study was 85%. Five hundred sixty-three students of whom 78% were female (69% medical students, 94% nursing students and 88% pharmacy students) were enrolled in the study. The mean age of the entire sample was 22.21 (SD ± 3.483) years. The mean ages of the students enrolled in the three programs i.e., medical, nursing, and pharmacy were 22.42 (SD ± 2.548), 23.04 (SD ± 6.006), and 20.92 (SD ± 2.207) years, respectively.
2. Gender differences
The MANOVA investigation on the correlation between psychiatric symptomatology (BSI, BDI and BHS total scores) and the undergraduate medical, nursing and pharmacy programs covariated for gender showed that there was a significant interaction between gender and scores from BSI, BDI, and BHS (F = 3.432; p = 0.017). The BDI total scores were significantly different (p = 0.006; F = 7.802) between female (9.53 ± 8.024) and male (6.65 ± 6.009) medical students. Regarding the BSI total scores, there was a trend (p = 0.056; F = 3.663) towards higher scores by female (0.61 ± 2.474) compared to male (0.32 ± 1.260) medical students. There was no significant gender difference regarding the BHS total scores (p = 0.084; F = 3.002).
3. Investigation of the prevalence of suicidal ideation, depressive symptoms and hopelessness in health professions students
There was no difference regarding the presence of suicidal ideation among medical (n = 45 [13.4%]), nursing (n = 13 [12.3%]) and pharmacy (n = 15 [12.3%]) students (p = 0.935). There was also no difference regarding the presence of either depression or hopelessness in medical students (n = 28 [8.3%], and n = 321 [95.5%]) in comparison to nursing (n = 9 [8.5%], and n = 96 [91.4%]) and pharmacy (n = 6 [4.9%], and n = 118 [96.7%]) students (p = 0.441, and p = 0.125).
4. Investigation of the severity of suicidal ideation, depressive symptoms, and hopelessness in healthcare students
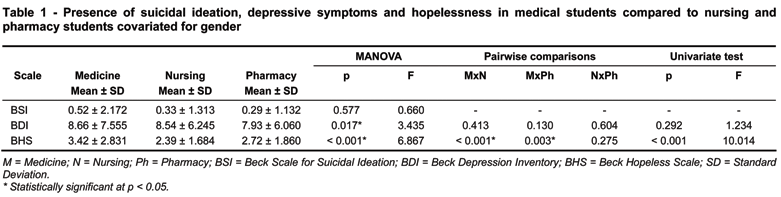
Table 1 presents the scores obtained from the medical, nursing and pharmacy students. The year-by-year scores on the BSI (Figure 1), BDI (Figure 2) and BHS (Figure 3) across the medical, nursing and pharmacy programs are shown.
The MANOVA gender-controlled investigation on the correlation between psychiatric symptomatology (BSI, BDI, and BHS total scores) and type of healthcare program (medical, nursing, and pharmacy) showed that there was a significant interaction between program type and the scores from BSI, BDI, and BHS (F = 3.77; p=0.001). After controlling for gender effect, a test on the between-subjects effects revealed that, for the corrected model, both hopelessness and depressive symptoms presented significant results (F = 6.867; df = 3; R square = 0.018; p < 0.001 and F = 3.435; df = 3; R square = 0.036; p = 0.0171, respectively), whereas suicidal ideation was not significantly associated with program type (F = 0.660; df = 3; R square = 0.004; p = 0.577). Pairwise comparisons analysis revealed that there was neither any significant difference in the severity of suicidal ideation (p > 0.214) nor in the severity of depressive symptoms (p > 0.130) among students from the three programs. We observed that medical students presented higher scores of hopelessness in comparison to both nursing (p < 0.001) and pharmacy (p = 0.003) students. However, there was no difference in the severity of hopelessness among nursing and pharmacy students (p = 0.275). Gender-controlled univariate tests showed that, across the three programs, only suicidal ideation remained significant (F = 10.014; p < 0.001) based on the linearity independent pairwise comparisons among estimate marginal tests.
Table 2 shows the year-by-year prevalence rates for each healthcare program. We did not observe significant differences in the rates of both prevalence and severity of suicidal ideation, depressive symptoms and hopelessness throughout the nursing program (Table 2). Throughout the pharmacy program, we also did not observe differences in prevalence rates of suicidal ideation, depressive symptoms and hopelessness. However, when assessing the severity of these symptoms, we observed that students in the 2nd year of the pharmacy program presented significantly higher hopelessness scores compared to students in the 3rd (p = 0.026) and 4th years (p = 0.017) of the pharmacy program. There were no other significant differences in the pharmacy program regarding suicidal ideation and depressive symptoms (p > 0.07) (Table 2).
5. Investigation of the prevalence of suicidal ideation, depressive symptoms and hopelessness during the medical program
Throughout the course of study, no difference was seen across the three major training stages i.e., basic, pre-clinical/clinical-theoretical and internship of the medical program regarding the presence of suicidal ideation, depression or hopelessness. We found a prevalence of suicide thoughts among 13% (n = 22) of the medical students at the basic stage, 11% (n = 11) at the pre-clinical/clinical-theoretical stage and 16.2% (n = 11) at the internship stage (p > 0.05). Severe depressive symptoms were found in 13% (n = 23) of the medical students at the basic stage, 6% (n = 6) at the pre-clinical/clinical-theoretical stage, and 12% (n = 8) at the internship stage (p > 0.05). Finally, we found a prevalence of hopelessness in 97% (n = 164) of the medical students at the basic stage, 95% (n = 93) at the pre-clinical/clinical-theoretical stage, and 94% (n = 64) at the internship stage (p > 0.05).
Pearson Chi-Square showed that there were no significant differences among program stages regarding the prevalence of BSI, BDI and BHS (p = 0.636, p = 0.424, p = 0.514, respectively). The MANOVA investigation revealed that there was a significant difference regarding the severity of symptoms related to BDI (p = 0.006; F = 5.144). The post hoc Tukey test showed that students at the internship stage presented significantly higher depressive scores compared to students at the basic stage (p = 0.037), as well as to students at the pre-clinical/clinical-theoretical stage (p = 0.005).
Discussion
The main purpose of our study was to identify the presence of suicidal thoughts, depressive symptoms and symptoms of hopelessness among medical students in comparison to students from other healthcare programs, namely nursing and pharmacy. Our major finding was that the presence of hopelessness was significantly greater in medical students in comparison to both nursing and pharmacy students. Furthermore, we verified a significant positive correlation between suicide risk scores and the presence of depressive symptoms and symptoms of hopelessness. Although we did not observe significant differences among medical, nursing and pharmacy students with respect to the presence of suicidal ideation or depressive symptoms, the presence of suicidal thoughts in students enrolled in healthcare programs is indeed worrying. Konick & Gutierrez suggested that both depressive symptoms and symptoms of hopelessness are predictors of suicidal ideation in undergraduate students.31
Prior to further discussing the factors involved in the absence of significant differences in the three programs in terms of the presence of suicidal ideation and depressive symptoms, the hypothetical existence of sampling errors, bias or confounding factors needs to be duly investigated.
The choice of working with the entire population of students from the three programs ruled out the possibility of a sampling error. Response rates from 56% of the medical, 56% of the nursing and 61% of the pharmacy's total medical, nursing, and pharmacy student bodies provided us with an appropriate sampling of the study population. We observed certain differences in the questionnaire's response rates across the different programs. Several reasons may account for this observation. The lower response rate by medical students serving their internships may have underestimated the prevalence of depression at this stage of the program. Nevertheless, our findings clearly show higher scores of depression in this student group, which is highly associated with suicide thoughts, suicide attempts and deaths by suicide. The poorest response rate was registered among medical students serving their internships, probably due to the fact that students in elective and external rotations could not be reached during the period in which this study was carried out. Also, this group of students undertakes clinical clerkships in several departments for varying lengths of time, thus making them less accessible when compared to nursing and pharmacy students who are fewer in number and less exposed to as many different departments.
In our study we observed that, during the medical program, students presented an increased rate of depressive symptoms while serving their internship period when compared to the basic and pre-clinical/clinical-theoretical training stages. A systematic review of the literature on depression, anxiety and other indicators of psychological distress among U.S. and Canadian medical students reported a high prevalence of depression and anxiety among medical students, with levels of psychological distress consistently higher than in the general population, especially in the later years of training (internship).32 Other studies also observed a significant elevation of both depressive symptoms and the prevalence of depression when graduating from the 1st to the 2nd years of medical education.33-35 Medical students' mental health worsens after the beginning of medical school and remains poor throughout training, thus contributing to suicide and substance abuse and affecting students' care of patients.36
A very interesting finding of our study was the fact that pharmacy students had higher rates of symptoms of hopelessness during the 2nd year. While it may be argued that pharmacy students may not be experiencing the detrimental levels of stress that affect medical students, a study conducted by Henning, Ey, & Shaw16 found a disproportionately high level of distress in pharmacy students. Even though our study did not specifically address this, such higher rates could suggest that this stage of the pharmacy program might be associated with a worsening of the students' psychological health.35 Future studies are needed in order to identify the reasons why second-year pharmacy students present higher levels of psychological symptomatology.
A possible limitation of our study was the decision to apply the Beck Inventory questionnaires, all of which are self-assessment questionnaires rather than clinically-structured interviews. We acknowledge that this decision might be associated with a bias to either minimize or maximize psychological symptomatology. However, in our view, the ensuing anonymity and the ability to assess larger samples of healthcare students clearly constitute advantages. Furthermore, considering that our study population consisted of undergraduate students from healthcare professions, we believed that they would certainly be able to fully understand the questionnaires and answer them appropriately. Besides, the application of an individual clinical interview might not have prevented students from minimizing clinical symptoms. Finally, given the cross-sectional nature of the study which prevented us from establishing a temporal cause and consequence relationship, we cannot state that the associations observed in the study are of a causal nature.
The present study represents an important addition to the current literature considering that we directly compared aspects of psychopathology present among medical students to that of other students from other healthcare professions. Hence, the importance of mental health support services to provide for such students, thus preventing the worsening of symptoms, strengthening healthy mechanisms, and increasing the ability to deal with health problems. The results presented in this study suggest that a longitudinal study design is needed to ensure continuity. We also hope that our results may promote the establishment of programs dedicated to healthcare students other than medical students. Early identification of suicidal ideation, depressive symptoms and symptoms of hopelessness in health-related programs is crucial when providing appropriate support and treatment, promoting the improvement of the students' mental health, preventing deaths by suicide and honing social and professional skills.
Acknowledgements
This research was funded by a grant received from Fundação de Amparo à Pesquisa do Estado de São Paulo (FAPESP), process numbers 06/02214-4 and 07/00720-2. We also thank the Brazilian Psychiatric Association for the "Young Psychiatrist Award" granted at the XXVI Brazilian Congress of Psychiatry, 2008 for having conducted this study.
Submitted: April 7, 2009
Accepted: June 26, 2009
- 1. Schernhammer ES, Colditz GA. Suicide rates among physicians: a quantitative and gender assessment (meta-analysis). Am J Psychiatry 2004;161(12):2295-302.
- 2. Botega NJ, Barros MB, Oliveira HB, Dalgalarrondo P, Marín-León L. Suicidal behavior in the community: prevalence and factors associated with suicidal ideation. Rev Bras Psiquiatr 2005;27(1):45-53.
- 3. Conner KR, Duberstein PR, Conwell Y, Seidlitz L, Caine ED. Psychological vulnerability to completed suicide: a review of empirical studies. Suicide Life Threat Behav 2001;31(4):367-85.
- 4. Morrison R, O'Connor RC. A systematic review of the relationship between rumination and suicidality. Suicide Life Threat Behav 2008;38(5):523-38.
- 5. Regier DA, Narrow WE, Rae DS, Manderscheid RW, Locke BZ, Goodwin FK. The de facto US mental and addictive disorders service system. Epidemiologic catchment area prospective 1-year prevalence rates of disorders and services. Arch Gen Psychiatry 1993;50(2):85-94.
- 6. Aasland OG, Ekeberg O, Schweder T. Suicide rates from 1960 to 1989 in Norwegian physicians compared with other educational groups. Soc Sci Med 2001;52(2):259-65.
- 7. Hawton K, Clements A, Sakarovitch C, Simkin S, Deeks JJ. Suicide in doctors: a study of risk according to gender, seniority and specialty in medical practitioners in England and Wales, 1979-1995. J Epidemiol Community Health 2001;55(5):296-300.
- 8. Torre DM, Wang NY, Meoni LA, Young JH, Klag MJ, Ford DE. Suicide compared to other causes of mortality in physicians. Suicide Life Threat Behav 2005;35(2):146-53.
- 9. Clark DC, Zeldow PB. Vicissitudes of depressed mood during four years of medical school. JAMA 1988;260(17):2521-8.
- 10. Mosley TH Jr, Perrin SG, Neral SM, Dubbert PM, Grothues CA, Pinto BM. Stress, coping, and well-being among third-year medical students. Acad Med 1994;69(9):765-7.
- 11. Dahlin ME, Runeson B. Burnout and psychiatric morbidity among medical students entering clinical training: a three year prospective questionnaire and interview-based study. BMC Med Educ 2007;7:6.
- 12. Dyrbye LN, Thomas MR, Eacker A, Harper W, Massie FS Jr, Power DV, Huschka M, Novotny PJ, Sloan JA, Shanafelt TD. Race, ethnicity, and medical student well-being in the United States. Arch Intern Med 2007;167(19):2103-9.
- 13. Dzurec LC, Allchin L, Engler AJ. First-year nursing students' accounts of reasons for student depression. J Nurs Educ 2007;46(12):545-51.
- 14. Gorter R, Freeman R, Hammen S, Murtomaa H, Blinkhorn A, Humphris G. Psychological stress and health in undergraduate dental students: fifth year outcomes compared with first year baseline results from five European dental schools. Eur J Dent Educ 2008;12(2):61-8.
- 15. Ried LD, Motycka C, Mobley C, Meldrum M. Comparing self-reported burnout of pharmacy students on the founding campus with those at distance campuses. Am J Pharm Educ 2006;70(5):114.
- 16. Henning K, Ey S, Shaw D. Perfectionism, the imposter phenomenon and psychological adjustment in medical, dental, nursing and pharmacy students. Med Educ 1998;32(5):456-64.
- 17. Baldwin JN, Scott DM, Agrawal S, Bartek JK, Davis-Hall RE, Reardon TP, DeSimone EM 2nd. Assessment of alcohol and other drug use behaviors in health professions students. Subst Abus 2006;27(3):27-37.
- 18. Omigbodun OO, Odukogbe AT, Omigbodun AO, Yusuf OB, Bella TT, Olayemi O. Stressors and psychological symptoms in students of medicine and allied health professions in Nigeria. Soc Psychiatry Psychiatr Epidemiol 2006;41(5):415-21.
- 19. Baldassin S, Alves TC, de Andrade AG, Martins LA. The characteristics of depressive symptoms in medical students during medical education and training: a cross-sectional study. BMC Med Educ 2008;8:60.
- 20. Tyssen R, Vaglum P, Gronvold NT, Ekeberg O. Suicidal ideation among medical students and young physicians: a nationwide and prospective study of prevalence and predictors. J Affect Disord 2001;64(1):69-79.
- 21. Placidi GP, Oquendo MA, Malone KM, Brodsky B, Ellis SP, Mann JJ. Anxiety in major depression: relationship to suicide attempts. Am J Psychiatry 2000;157(10):1614-8.
- 22. Valentiner DP, Gutierrez PM, Blacker D. Anxiety measures and their relationship to adolescent suicidal ideation and behavior. J Anxiety Disord 2002;16(1):11-32.
- 23. Hendrie HC, Clair DK, Brittain HM, Fadul PE. A study of anxiety/depressive symptoms of medical students, house staff, and their spouses/partners. J Nerv Ment Dis 1990;178(3):204-7.
- 24. Tyssen R, Hem E, Vaglum P, Gronvold NT, Ekeberg O.. The process of suicidal planning among medical doctors: predictors in a longitudinal Norwegian sample. J Affect Disord 2004;80(2-3):191-8.
- 25. Helmers KF, Danoff D, Steinert Y, Leyton M, Young SN. Stress and depressed mood in medical students, law students, and graduate students at McGill University. Acad Med 1997;72(8):708-14.
- 26. Beck AT, Kovacs M, Weissman A. Assessment of suicidal intention: the Scale for Suicide Ideation. J Consult Clin Psychol 1979;47(2):343-52.
- 27. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry 1961;4:561-71.
- 28. Beck AT, Weissman A, Lester D, Trexler L. The measurement of pessimism: the hopelessness scale. J Consult Clin Psychol 1974;42(6):861-5.
- 29. Beck AT, Steer RA, Beck JS, Newman CF. Hopelessness, depression, suicidal ideation, and clinical diagnosis of depression. Suicide Life Threat Behav 1993;23(2):139-45.
- 30. Gorenstein C, Andrade L. Validation of a Portuguese version of the Beck Depression Inventory and the State-Trait Anxiety Inventory in Brazilian subjects. Braz J Med Biol Res 1996;29(4):453-7.
- 31. Konick LC, Gutierrez PM. Testing a model of suicide ideation in college students. Suicide Life Threat Behav 2005;35(2):181-92.
- 32. Dyrbye LN, Thomas MR, Shanafelt TD. Systematic review of depression, anxiety, and other indicators of psychological distress among U.S. and Canadian medical students. Acad Med 2006;81(4):354-73.
- 33. Vitaliano PP, Maiuro RD, Russo J, Mitchell ES. Medical student distress. A longitudinal study. J Nerv Ment Dis 1989;177(2):70-6.
- 34. Stewart SM, Betson C, Marshall I, Wong CM, Lee PW, Lam TH. Stress and vulnerability in medical students. Med Educ 1995;29(2):119-27.
- 35. Aktekin M, Karaman T, Senol YY, Erdem S, Erengin H, Akaydin M. Anxiety, depression and stressful life events among medical students: a prospective study in Antalya, Turkey. Med Educ 2001;35(1):12-7.
- 36. Dyrbye LN, Thomas MR, Shanafelt TD. Medical student distress: causes, consequences, and proposed solutions. Mayo Clin Proc 2005;80(12):1613-22.
Correspondence
Publication Dates
-
Publication in this collection
16 Oct 2009 -
Date of issue
Dec 2009
History
-
Received
07 Apr 2009 -
Accepted
26 June 2009