Abstracts
OBJECTIVE: Although bipolar disorder is a major contributor to functional impairment worldwide, an independent impact of bipolar disorder and ageing on functioning has yet to be demonstrated. The objective of the present study was to evaluate the effect of bipolar disorder on age-related functional status using matched controls as a standard. METHOD: One-hundred patients with bipolar disorder and matched controls were evaluated for disability. Age-related effects controlled for confounders were cross-sectionally evaluated. RESULTS: Patients were significantly more impaired than controls. Regression showed effects for aging in both groups. The effect, size, however, was significantly stronger in patients. CONCLUSION: Bipolar disorder was an important effect modifier of the age impact on functioning. While a longitudinal design is needed to effectively demonstrate this different impact, this study further depicts bipolar disorder as a chronic and progressively impairing illness.
Bipolar disorder disability; Functioning; Ageing; Controlled study; Brazil
OBJETIVO: O transtorno bipolar é responsável por importante parcela do prejuízo funcional ao redor do mundo. Um efeito independente do transtorno bipolar e da idade no funcionamento ainda não foi demonstrado. O presente estudo tem o objetivo de avaliar o efeito do transtorno bipolar no prejuízo funcional relacionado à idade, com controles pareados como padrão. MÉTODO: Cem pacientes com transtorno bipolar e controles pareados foram avaliados para incapacidade. Efeitos relacionados à idade, com controle para confundidores, foram investigados. RESULTADOS: Pacientes tiveram significativamente mais prejuízo que controles. A regressão mostrou efeito para a idade em ambos os grupos, e o efeito foi significativamente mais forte nos pacientes. CONCLUSÃO: O transtorno bipolar foi um importante modificador de efeito no impacto da idade no funcionamento. Enquanto um desenho de estudo longitudinal é necessário para efetivamente demonstrar este impacto diferencial, este estudo caracteriza o transtorno bipolar como uma doença crônica e incapacitante.
Transtorno bipolar; incapacidade; Funcionamento; Idade; Estudo controlado; Brasil
BRIEF REPORT
Bipolar disorder and age-related functional impairment
Prejuízo funcional associado à idade e transtorno bipolar
Alice Aita CacilhasI; Pedro Vieira da Silva MagalhãesI; Keila Maria Ceresér; Julio Cesar WalzI; Fernanda WeyneI; Adriane Ribeiro RosaI, II; Eduard VietaII; Flávio KapczinskiI
IMolecular Psychiatry Laboratory & INCT Translational Medicine, Hospital de Clínicas de Porto Alegre (HCPA), Universidade Federal do Rio Grande do Sul (UFRGS), Porto Alegre (RS), Brazil
IIBipolar Disorders Program, Clinical Institute of Neuroscience, Hospital Clinic, University of Barcelona, Barcelona, Spain
Correspondence Correspondence : Flávio Kapczinski Laboratório de Psiquiatria Molecular Hospital de Clínicas de Porto Alegre Ramiro Barcelos, 2350 90035-003 Porto Alegre, RS, Brazil Phone: (+55 51) 2101-8845 Fax: (+55 51) 2101-8846 E-mail: kapcz@terra.com.br
ABSTRACT
OBJECTIVE: Although bipolar disorder is a major contributor to functional impairment worldwide, an independent impact of bipolar disorder and ageing on functioning has yet to be demonstrated. The objective of the present study was to evaluate the effect of bipolar disorder on age-related functional status using matched controls as a standard.
METHOD: One-hundred patients with bipolar disorder and matched controls were evaluated for disability. Age-related effects controlled for confounders were cross-sectionally evaluated.
RESULTS: Patients were significantly more impaired than controls. Regression showed effects for aging in both groups. The effect, size, however, was significantly stronger in patients. CONCLUSION: Bipolar disorder was an important effect modifier of the age impact on functioning. While a longitudinal design is needed to effectively demonstrate this different impact, this study further depicts bipolar disorder as a chronic and progressively impairing illness.
Descriptors: Bipolar disorder disability; Functioning; Ageing; Controlled study; Brazil
RESUMO
OBJETIVO: O transtorno bipolar é responsável por importante parcela do prejuízo funcional ao redor do mundo. Um efeito independente do transtorno bipolar e da idade no funcionamento ainda não foi demonstrado. O presente estudo tem o objetivo de avaliar o efeito do transtorno bipolar no prejuízo funcional relacionado à idade, com controles pareados como padrão.
MÉTODO: Cem pacientes com transtorno bipolar e controles pareados foram avaliados para incapacidade. Efeitos relacionados à idade, com controle para confundidores, foram investigados.
RESULTADOS: Pacientes tiveram significativamente mais prejuízo que controles. A regressão mostrou efeito para a idade em ambos os grupos, e o efeito foi significativamente mais forte nos pacientes.
CONCLUSÃO: O transtorno bipolar foi um importante modificador de efeito no impacto da idade no funcionamento. Enquanto um desenho de estudo longitudinal é necessário para efetivamente demonstrar este impacto diferencial, este estudo caracteriza o transtorno bipolar como uma doença crônica e incapacitante.
Descritores: Transtorno bipolar, incapacidade; Funcionamento; Idade; Estudo controlado; Brasil
Introduction
Ageing is often associated with progressive disability, with unique environment and genetics impacting age-related functioning.1 Among the mood disorders, bipolar disorder (BD) is associated with functioning within or below the functioning levels of the most chronic illnesses;2 moreover, it could increase age-related impairment through both genetic and environmental pathways. An increased allostatic load associated with BD would anticipate such an association.3 This concept is akin to cumulative physiologic dysregulation and allows for the prediction of changes in physical and cognitive functioning.4
To our knowledge, an independent impact of bipolar disorder on age-related functioning has yet to be demonstrated in a controlled study. We evaluated this effect, with matched healthy subjects as a standard against which age-related impairment was measured.
Method
One-hundred outpatients with a confirmed diagnosis of BD according to the Structured Clinical Interview for DSM-IV and healthy controls individually matched for gender, age and years of education were consecutively recruited from September to November 2007. The only ground for exclusion was the inability to provide informed consent. Thus, patients were representative of patients treated for bipolar disorder in a tertiary health care centre. Compared to other outpatients in the Bipolar Disorders Programme of the Hospital de Clínicas de Porto Alegre5 (n = 260), the patients in this study were not significantly different in terms of their age (44.23 vs 42.63), gender (74% vs 70% female) and number of hospitalizations (3.57 vs 3.57). All participants gave their written informed consent before entering the study, which was approved by the local ethics committee.
Functional impairment was assessed using the Functioning Assessment Short Test (FAST), an interview that evaluates disability. It includes items on autonomy, work, cognitive functioning, financial issues and interpersonal relationships. It has excellent reliability and was checked regarding content, construct and concurrent validity in Brazilian and Spanish populations.6,7
We used multiple linear regression with robust estimation of variances in the patient and control groups separately to test for age effects on functioning. In these analyses, effects were controlled for potential disability-related confounders,8 such as medications currently in use and affective symptoms, which were assessed using the Hamilton Depression Rating Scale, the Young Mania Rating Scale and the Hamilton Anxiety Rating Scale and hospitalizations. We also tested inthe model years since diagnosis and years since specific treatment, but these were not predictive of functioning. Coefficients (β) and standard errors (SE) from these regressions were used to generate effect sizes. Heterogeneity, that is, how much the groups differ was investigated with the Q statistic. When the p value for this statistic is low (below conventional levels of significance), the hypothesis of homogeneity is rejected and one can conclude that one is not measuring an effect of the same size.9 Wilcoxon's signed rank test (Z) was used to compare FAST scores in patients and controls. All tests are two-tailed.
Results
Groups were well matched (Table 1). Patients were significantly more impaired than control subjects (n = 200, Z = 8.19, p < 0.001). This effect was sustained even when only those on monotherapy (n = 30, Z = 2.33, p = 0.019), with no past hospitalizations (n = 36, Z = 3.40, p < 0.001) or with no significant depressive symptoms (HAMD < 8; n = 104, Z = 5.34, p < 0.001) were considered.
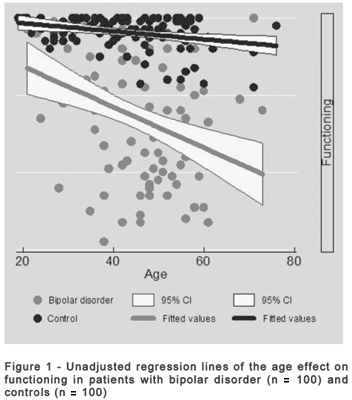
Figure 1 displays the unadjusted impact of BD on age-related functioning. In the regression analyses, age was significantly associated with functioning both in patients (β = 0.377, SE = 0.087, p < 0.001) and control subjects (β = 0.101, SE = 0.039, P = 0.013). These effects were significantly different (Q = 8.37, p = 0.004).
Discussion
Bipolar illness is characterized by a course both cyclic and recurrent, but to what extent it is progressive is still surrounded by considerable controversy. While some argue that there is a lack of evidence of progressive worsening,10 others argue that accelerated biological ageing does take place in BD.11 In this study, bipolar disorder was an important effect modifier of age effects on functioning, further characterizing BD as a chronic and impairing illness.
As this was not a population-based sample, extrapolating these findings to less severely affected patients may be problematic. Additionally, controlled longitudinal studies are needed to confirm these differential age-related effects on functioning. Notwithstanding the limitations of the cross-sectional design employed, we did find a significant, noteworthy and independent impact of BD on age-related functioning.
Emerging evidence suggests that cognition does play a role in these effects as accelerating hippocampal grey matter loss has been prospectively demonstrated in BD.12 Since an increased allostatic load creates a risk for cognitive decline,4 may be the end result of cumulative physiologic dysregulation related to medical burden,13 HPA axis dysfunction,14 altered immunity, pro-inflammatory15 and oxidative stress states.16 These factors may be partially modifiable medical risks and potential targets to reduce increasing morbidity and impairment in bipolar disorder.
Acknowledgements
Dr. Magalhães holds a doctoral scholarship awarded by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), Brazil. Dr. Kapczinski has received grant/research support from Astra-Zeneca, Eli Lilly, the Janssen-Cilag, Servier, Conselho Nacional de Desenvolviemento Científico e Tecnológico (CNPq), CAPES, National Alliance for Research on Schizophrenia and Depression (NARSAD) and the Stanley Medical Research Institute; has been a member of the speakers boards for Astra-Zeneca, Eli Lilly, Janssen and Servier; and has served as a consultant for Servier.
Submitted: November 2, 2008
Accepted: July 29, 2009
- 1. Gurland BJ, Page WF, Plassman BL. A twin study of the genetic contribution to age-related functional impairment. J Gerontol A Biol Sci Med Sci. 2004;59(8):859-63.
- 2. Morriss R, Mohammed FA. Metabolism, lifestyle and bipolar affective disorder. J Psychopharmacol. 2005;19(6 Suppl):94-101.
- 3. Kapczinski F, Vieta E, Andreazza AC, Frey BN, Gomes FA, Tramontina J, Kauer-Sant'anna M, Grassi-Oliveira R, Post RM. Allostatic load in bipolar disorder: implications for pathophysiology and treatment. Neurosci Biobehav Rev. 2008;32(4):675-92.
- 4. Karlamangla AS, Singer BH, McEwen BS, Rowe JW, Seeman TE. Allostatic load as a predictor of functional decline. MacArthur studies of successful aging. J Clin Epidemiol. 2002;55(7):696-710.
- 5. Magalhães PV, Kapczinski F, Kauer-Sant'anna M. Use of contraceptive methods among women treated for bipolar disorder. Arch Womens Ment Health 2009;12(3):183-5.
- 6. Rosa AR, Sánchez-Moreno J, Martínez-Aran A, Salamero M, Torrent C, Reinares M, Comes M, Colom F, Van Riel W, Ayuso-Mateos JL, Kapczinski F, Vieta E. Validity and reliability of the Functioning Assessment Short Test (FAST) in bipolar disorder. Clin Pract Epidemol Ment Health. 2007;3:5.
- 7. Cacilhas AA, Magalhães PV, Ceresér KM, Walz JC, Weyne F, Rosa AR, Vieta E, Kapczinski F. Validity of a short functioning test (FAST) in Brazilian outpatients with bipolar disorder. Value Health. 2009; 12(4):624-7
- 8. Huxley N, Baldessarini RJ. Disability and its treatment in bipolar disorder patients. Bipolar Disord. 2007;9(1-2):183-96.
- 9. Cochran WG. The combination of estimates from different experiments. Biometrics. 1954;10(1):101-29.
- 10. Turvey CL, Coryell WH, Solomon DA, Leon AC, Endicott J, Keller MB, Akiskal H. Long-term prognosis of bipolar I disorder. Acta Psychiatr Scand. 1999;99(2):110-9.
- 11. Simon NM, Smoller JW, McNamara KL, Maser RS, Zalta AK, Pollack MH, Nierenberg AA, Fava M, Wong KK. Telomere shortening and mood disorders: preliminary support for a chronic stress model of accelerated aging. Biol Psychiatry. 2006;60(5):432-5.
- 12. Moorhead TW, McKirdy J, Sussmann JE, Hall J, Lawrie SM, Johnstone EC, McIntosh AM. Progressive gray matter loss in patients with bipolar disorder. Biol Psychiatry. 2007;62(8):894-900.
- 13. Kupfer DJ. The increasing medical burden in bipolar disorder. JAMA. 2005;293(20):2528-30.
- 14. Daban C, Vieta E, Mackin P, Young AH. Hypothalamic-pituitary-adrenal axis and bipolar disorder. Psychiatr Clin North Am. 2005;28(2):469-80.
- 15. Kauer-Sant'anna M, Kapczinski F, Andreazza AC, Bond DJ, Lam RW, Young LT, Yatham LN. Brain-derived neurotrophic factor and inflammatory markers in patients with early- vs. late-stage bipolar disorder. Int J Neuropsychopharmacol 2008;12(4):477-58.
- 16. Kapczinski F, Frey BN, Andreazza AC, Kauer-Sant'Anna M, Cunha AB, Post RM. Increased oxidative stress as a mechanism for decreased BDNF levels in acute manic episodes. Rev Bras Psiquiatr. 2008;30(3):243-5.
Correspondence
Publication Dates
-
Publication in this collection
22 Jan 2010 -
Date of issue
Dec 2009
History
-
Received
02 Nov 2008 -
Accepted
29 July 2009