Abstracts
PURPOSE: To validate the Vocal Performance Questionnaire into Brazilian Portuguese. METHODS: The guidelines of the Scientific Advisory Committee of the Medical Outcomes Trust - SAC were followed. Initially, aspects of conceptual model and measurement, reliability, validity, sensitivity, interpretability, and demand of management and response were analyzed. The questionnaire was translated and back translated by two speech-language pathologists fluent in English. The versions were compared and the Portuguese version of the questionnaire, denominated Questionário de Performance Vocal - QPV, was generated. The QPV was administered to 325 people, 160 with vocal complaints and 165 ones without vocal complaints, with similar distribution of gender and age. The scores of both groups were calculated and compared, and the questionnaire was administered again to 39 dysphonic participants, to determine its reliability and test-retest reproducibility. A 95% confidence interval was adopted. RESULTS: All 12 questions were maintained, and the questionnaire presented reliable psychometric measures of validity, reliability and reproducibility, and sensitivity. CONCLUSION: The Brazilian version of the VPQ, the Questionário de Performance Vocal - QPV, is a reliable and valid protocol, sensitive to changes, easy to use and calculate the results, and may be an important instrument to compose the speech-language pathology assessment of dysphonic patients.
Voice; Quality of life; Validation studies; Self-assessment; Questionnaires; Brazil
OBJETIVO: Realizar a validação do Vocal Performance Questionnaire para o Português Brasileiro. MÉTODOS: Foram seguidos os passos do Scientific Advisory Committee of the Medical Outcomes Trust - SAC. Primeiramente foram analisados os aspectos de modelo conceitual e de medida, confiabilidade, validade, sensibilidade, interpretabilidade e demanda de administração e resposta. O questionário foi traduzido e também retrotraduzido por duas fonoaudiólogas fluentes na língua. As versões foram comparadas e a versão em Português do questionárion foi gerada, recebendo o nome Questionário de Performance Vocal - QPV. O questionário foi aplicado em 325 indivíduos, 160 com queixa vocal e 165 indivíduos sem queixa vocal, com distribuição semelhante de gênero e idade. Posteriormente, os escores dos dois grupos foram comparados e o questionário foi reaplicado em 39 participantes disfônicos, para avaliação da confiabilidade e reprodutibilidade do questionário. O intervalo de confiança considerado foi 95%. RESULTADOS: Todas as 12 questões foram mantidas e o questionário apresentou medidas psicométricas confiáveis de validade, confiabilidade e reprodutibilidade e sensibilidade. CONCLUSÃO: A versão brasileira chamada Questionário de Performance Vocal - QPV, é um protocolo confiável, válido, sensível a mudanças, de fácil aplicação e cálculo de resultados, podendo ser um instrumento importante para compor a avaliação fonoaudiológica do indivíduo disfônico.
Voz; Qualidade de vida; Estudos de validação; Autoavaliação; Questionários; Brasil
ORIGINAL ARTICLE
Validation of the Vocal Performance Questionnaire in Brazil
Bruna Rabelo PaulinelliI; Ana Cristina Côrtes GamaII; Mara BehlauI
ICentro de Estudos da Voz CEV São Paulo (SP), Brazil
IIDepartment of Speech-Language Pathology and Audiology, Universidade Federal de Minas Gerais UFMG Belo Horizonte (MG), Brazil
Correspondence address
ABSTRACT
PURPOSE: To validate the Vocal Performance Questionnaire into Brazilian Portuguese.
METHODS: The guidelines of the Scientific Advisory Committee of the Medical Outcomes Trust SAC were followed. Initially, aspects of conceptual model and measurement, reliability, validity, sensitivity, interpretability, and demand of management and response were analyzed. The questionnaire was translated and back translated by two speech-language pathologists fluent in English. The versions were compared and the Portuguese version of the questionnaire, denominated Questionário de Performance Vocal QPV, was generated. The QPV was administered to 325 people, 160 with vocal complaints and 165 ones without vocal complaints, with similar distribution of gender and age. The scores of both groups were calculated and compared, and the questionnaire was administered again to 39 dysphonic participants, to determine its reliability and test-retest reproducibility. A 95% confidence interval was adopted.
RESULTS: All 12 questions were maintained, and the questionnaire presented reliable psychometric measures of validity, reliability and reproducibility, and sensitivity.
CONCLUSION: The Brazilian version of the VPQ, the Questionário de Performance Vocal QPV, is a reliable and valid protocol, sensitive to changes, easy to use and calculate the results, and may be an important instrument to compose the speech-language pathology assessment of dysphonic patients.
Keywords: Voice; Quality of life; Validation studies; Self-assessment; Questionnaires; Brazil
INTRODUCTION
Literature regarding quality of life related to health have improved a lot(1) towards the perception of health as a complete state of physical, mental and social well being, and not only as the absence of disease(2).
Quality of life is defined as "the perception of the individual about his/her own position in life, in the context of culture and in system of values under which he/she lives, and regarding his/hers objectives, expectations, standards and worries" (3,4). It is a measure that takes into account many individuals aspects (feelings, circumstances)(5). Therefore, quality of life considers the individual's self-evaluation regarding symptoms of a determined disease, lived experiences, among others. On the other hand, health is a dynamic state of physical well being and absence of disease(6).
The use of these concepts, therefore, can contribute to improve the quality and integrality of health assistance(7), besides helping in taking decisions regarding treatment(8).
It is important that health professionals consider the impact of treatment on the quality of life of patients. Especially if the purpose is to make the patient feel better in all aspects of his/her life that are affected by the problem(9). Therefore, it has been observed a growth in the use of quality of life measures in practices developed in health services.
To measure quality of life related to health in the several illnesses, it has been a tendency to develop and/or adapt questionnaires(10). These tools may be generic, such as the SF-36, or specific, such as for some chronic diseases head and neck cancer, lung cancer, laryngopharingeal reflux disease, among others(11-13) or to dysphonia(9). Besides disease-specific, there is a preoccupation that they may also be specific to different types of population, such as elderly and children(14).
These tools offer the best information about the outcome of a treatment, because they have high validity and the best reliability, with good sensitivity to changes and excellent utility(15).
Protocols developed to a specific culture are useful only to that specific set and, in order to be used in different situations, they must be adequately validated. The purpose of validation is that the translated protocol is comparable to the original, therefore, the rules emphasize the linguistic, conceptual and psychometric equivalence(1), the measures of reliability, sensitivity, among others(6). An instrument is considered valid when it measures what theoretically is suppose to measure(8). They must have known reliability, validity and sensitivity, in order to prove its clinical usefulness, and to produce a reliable evaluation about the outcome of the treatment. Reliability is related to intern consistency and stability of the instrument, free of casual error or undesired variation(15).
Regarding voice problems, there are many tools to measure the impact of dysphonia in the quality of life of patients already validated into Brazilian Portuguese(14), such as the Voice-Related Quality of Life (V-RQOL)(16) Protocolo de Qualidade de Vida em Voz QVV(17), Voice Activity and Participation Profile (VAPP)(18) Perfil de Participação e Atividades Vocais PPAV(19), Voice Handicap Index (VHI)(20) Índice de Desvantagem Vocal IDV(21). All of these instruments measure the impact of dysphonia in several aspects of life related to oral communication; however each one has its own specificities and the choice of use is a prerogative of the therapist. The V-RQOL is shorter and faster; the VAPP maps the areas of greater impact of dysphonia; the VHI is focused on the handicap concept and has been more used to verify the outcome of the treatment(14).
Recently, the author of the Vocal Performance Questionnaire, along with other authors, conducted a literature review regarding the importance of the questionnaire in clinical routine, also to analyze the impact of surgery, pharmacological treatments, and mixed approaches(15). Literature shows an excellent reliability and intern consistency of the questionnaire (0.81 to 0.95), with high reproducibility (0.75). Validity was also high, and the authors highlighted that, if the patient is not satisfied with the treatment, it cannot be considered successful, even with attested improvements in perceptual and acoustic analysis. Regarding the sensitivity to change, the indexes were high both for voice therapy (1.4) and surgery (0.82). Moreover, the use of the VPQ is excellent due to its shortness, convenience and also for presenting high intern and one-dimensional consistency to measure the degree of voice deviation(15).
When the VPQ was compared with the VHI-10, the most used protocol internationally, it was verified that reliability, intern consistency, validity and utility are quite similar between them; the reproducibility of the VHI-10 is a little higher; the sensitivity of the VPQ to changes (1.04) is higher than that of the VHI-10 (0.62). The VPQ value higher than 1 was surprising, since the questionnaire has only 12 questions(15).
Thus, the purpose of this research was to validate the Vocal Performance Questionnaire into Brazilian Portuguese.
METHODS
The research was approved by the Ethics Committee of the Centro de Estudos da Voz (CEV), under protocol number 0416/08, and all participants signed the free and informed consent.
The Vocal Performance Questionnaire (VPQ) is a self-assessment protocol, derived from clinical practice(15), as all the previous instruments listed, with only 12 questions and five possible answers, that include many aspects of vocal performance, such as the characteristics of the sound of voice, physical discomfort or effort to talk, fatigue and voice worsening with usage, activities restriction due to voice problem, negative impact of voice on message intelligibility, other comments and worries regarding the problem(22). The calculation and interpretation of the score of this questionnaire are quite simple and easy to be understood by the patient.
In order to validate the questionnaire the main guidelines of the SAC Scientific Advisory Committee of the Medical Outcomes Trust(23) were followed. The validation process was conducted in six stages described as it follows:
1. Translation and linguistic and cultural adaptation: for this stage, the original questionnaire was translated by two speech-language pathologists fluent in English, one of them being an English teacher. After that, a backtranslation was made by an English teacher who was not a speech-language pathologist, did not participate in the previous stage, and did not have any knowledge about the original instrument. Then both versions were compared and the disagreement were analyzed by a group of five voice specialists, also fluent in English, who made changes by consensus and reached the final instrument, entitled, in Brazilian Portuguese, Questionário de Performance Vocal (QPV).
2. Cultural equivalence evaluation: the final questionnaire was addressed to a group of 17 subjects with voice complaints with the option "not applicable" to identify the questions that were not understood or not appropriate. None of the questions was invalid. The final version of this protocol is on Appendix 1.
3. Protocol application: the final questionnaire was then addressed to 325 Brazilian subjects, volunteers and representing various socio-cultural levels 160 with vocal complaint (dysphonia group), comprising 19 men and 141 women, mean age of 41 years (13-80 years), all without history of speech-language therapy; and 165 without vocal complaint (control group), comprising 31 men and 134 women, mean age of 33 years (19-79 years). Both groups were similar regarding gender and age. None of the subjects presented oral communication complaints other than voice disorders. The questionnaires were read and the answers were marked by the participants. The dysphonic subjects were recruited and invited to participate in the research at Speech-Language Pathology and Otorhinolaryngology clinics in Belo Horizonte (MG), Brazil, and the control group was formed by companions of the patients who attended these clinics and did not have vocal complaints. The sample calculus of this stage was done by simple random sampling with tolerable error of 0.05 with 95% reliability. To characterize the sample, a demographic and clinical descriptive statistical analysis of the population was conducted, regarding age, gender, voice deviation type, and presence or absence of vocal complaint. For the analysis of the variables gender and age between the groups, the Mann-Whitney test was used.
The VPQ is composed by 12 questions, and the subject must choose the better option among five, from "a" to "e", in which "a" represents the lower impact and "e" the higher impact. The calculus for the analysis of the questionnaire is a simple sum assigning 1 point to each answer "a", 2 points to each answer "b", and so on until de maximum of 5 points to answers "e". The maximum possible score is 60 points, and the result is considered normal when the score is 12 points(15). Any value higher than this limit indicates a decrease in vocal performance perceived by the patient. It is a short, convenient questionnaire, that presents high intern and one-dimensional consistency to measure the degree of vocal deviation(15).
4. Vocal self-evaluation and validation: to validate the questionnaire, it was requested that each subject classified their voices using a five-point Likert scale: excellent, very good, good, fair, poor. These data were used to determine the validity of the protocol, comparing the questionnaire and the self-evaluation scores, using Spearman correlation. To determine the reliability of the questionnaire, it was used the Cronbach correlation coefficients. It is important to emphasize that the self-perception analysis is a commonly used strategy to validate self-evaluation protocols of dysphonia impact(16-17,20-21).
5. Reliability and reproducibility test-retest: the questionnaire was reapplied in 39 subjects with vocal complaint after an interval of two to 14 days. This period is considered enough so that the respondents do not remember their previous answers while not having major vocal changes(24). To determine reproducibility, the Wilcoxon test was used. The reliability calculus used the Cronbach alpha test.
6. Treatment sensitivity: for this stage, the questionnaire was applied in ten dysphonic subjects before the beginning of speech-language treatment, and reapplied after ten therapy sessions. To compare the pre- and post-therapy results, the Wilcoxon test was used.
An individual analysis of the protocol questions was conducted later and, to compare the questions between groups and between pre- and post-therapy moments, the Pearson Chi-square and the Mann-Whitney tests were used.
RESULTS
Table 1 presents the difference between the mean scores of the control and dysphonia groups, showing higher values for the dysphonia group. Considering the quartiles, 50% of the participants in the control group had scores lower than 18, and 75% lower than 20; meanwhile, in the dysphonia group, only 25% of participants had scores lower than 22.
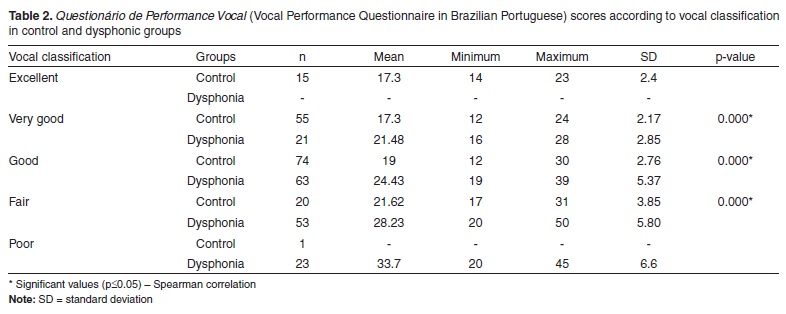
The relationship between vocal self-evaluation and mean scores on the QPV, evidencing that the more the individual realizes his/her own voice disorder, the higher the questionnaire values, indicating lower vocal performance (Table 2).
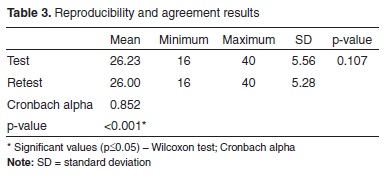
The results of reproducibility are shown in Table 3, with the mean scores, maximum and minimum in the first application and in the reapplication in a period within two to 14 days after the first one (test and retest), which was important to show that the questionnaire is reproducible and reliable, since no significant difference was found.
The questionnaire may also be considered valid, capable to reflect the impact of dysphonia on subject's vocal performance.
Table 4 presents the protocol sensitivity, indicating the decrease of QPV scores pre and post speech-language therapy, which reflects the perception of vocal performance increase with therapy; this difference was significant.
The values of the answers to the protocol questions in both groups, besides the total score, are showed in Table 5, where it is possible to observe that the dysphonia group presented higher scores in the answers to questions 11 and 12 (except for 7, which showed little difference between groups probably because, in general, the degree of dysphonia was mild or moderate, not having the need to repeat what is said to be understood), with greater difference when compared to the control group in questions 1, 2, 4, and 12. It is also presented the results of answers values in pre and post-therapy, and the QPV was able to reflect the effects of voice therapy, with a decrease in its score, showing increase in vocal performance after speech therapy.
DISCUSSION
The Vocal Performance Questionnaire VPQ is a simple instrument, quick to apply and easy to understand(15). Its translation and adaption into Brazilian Portuguese was simple, since the original version was easy to understand and the measure scales were kept the same.
In linguistic equivalence evaluation, the "not applicable" option was added to each item of the questionnaire; however, all the questions in the original version were kept in the Brazilian version, since none of them were invalid.
The mean score of control group was lower than that of the dysphonia group, but still a little high, probably because many participants in this group, even though not having dysphonia, classified their voices as fair or even poor, probably due to esthetics or the desire to have a superior quality of voice(25).
A vocal problem might reflect how the subject evaluates his/her own voice. Although not all dysphonia manifests with deviation on voice quality, the literature points out a positive correlation between self-perception of the voice problem and its negative impact on quality of life, with improvement after speech-language therapy(25-27).
The questionnaire validation was determined by the comparison between control and dysphonia groups, considering the correlation between vocal self-evaluation and the mean values of the instrument. It was possible to observe that the better the subject classifies his/her own voice, the lower the mean values of the QPV. This indicates that the questionnaire might be considered valid, capable to reflect the dysphonia impact on subject's vocal performance. This may also be found in the other voice questionnaires already validated in Brazil(14): V-RQOL(17), VAPP(19), VHI(21).
It is worth to observe that in the control group the participants who classified their voices as "very good" or "good" presented, as the minimum QPV score, 12 points, agreeing with other researches that demonstrate this value as normality limit regarding vocal performance(15). The subjects of this same group who classified their voices as "fair" presented 17 points as minimum score in the QPV. This suggests that, even though these subjects did not have the clinical diagnosis of dysphonia, they perceived their voices as not ideal, which may have reflected in the increasing of QPV values.
Reliability and reproducibility were proven by reapplying the questionnaire in 39 subjects, within a period from two to 14 days after the first application. The results demonstrate the questionnaire is reliable and reproducible, as well as other protocols already validated in Brazil(14): V-RQOL(17), VAPP(19), VHI(21).
Besides the importance to measure the impact of dysphonia on quality of life to define the basis of treatment, the comparison of pre- and post-therapy results may be valuable to measure the therapy effect from the subject's point of view(27). In this questionnaire, there was a significant difference between pre- and post-therapy. In the other questionnaires validate in Brazil(17,19,21), such as the V-RQOL(17), the statistical difference was also significant between pre- and post-therapy, that is, all of these questionnaires show the professional how the patient is feeling regarding the outcome of the treatment and, hence, help the decision of discharging the patient or the possibility to continue the intervention.
The significant difference between all questions in both groups shows how capable the questionnaire is to differentiate the studied groups, assuring the validity of the instrument.
When the pre- and post-therapy moments are compared, the questions 1, 3, 4, 6, 9, 10, 11, and 12 were capable to detect clinical alterations between moments. It was observed that, within a contextualized analysis of each patient, the QPV questions are clinically useful and enable a reliable evaluation of the treatment outcome.
When the results of this questionnaire are analyzed in view of the other protocols already validated in Brazil, it is possible to observe, again, the validity and practicality in the use of questionnaires to evaluate the impact of illnesses on subject's quality of life(10). Especially when the questionnaire is specific to a disorder, as, in this case, voice deviation(9,11-13). Besides all the advantages, the assessment of quality of life shows the point of view of the person that is being treated, and not only the therapist's point of view.
Moreover, none of the questionnaires validated in Brazil(16,18,20) have questions regarding fatigue and vocal discomfort. The QPV offers a vision of these aspects both in the beginning and in comparison between pre- and post-therapy moments, which may help the professionals in another aspect regarding the satisfaction of the patient and, therefore, in taking the decision to end the treatment.
The QPV is short, do not have redundant questions, it is addressed to physical symptoms and socio-economic impact, its questions are according to intensity of the vocal problem, and, therefore, it is an useful instrument to voice clinic.
CONCLUSION
The Vocal Performance Questionnaire in Brazilian Portuguese is valid, reliable, reproducible, and sensitive to treatment, and may be considered as another option in speech-language pathology practice regarding quality of life and voice.
REFERENCES
- 1. Novak M, Mah K, Molnar MZ, Ambrus C, Csepanyi G, Kovacs A, et al. Factor structure and reliability of the Hungrian version of the illness intrusiveness ratings scale invariance across North American and Hungarian dialysis patients. J Psych Res. 2005;58(1):103-10.
- 2. World Health Organization. Measuring quality of life – The World Health Organization Quality of life instruments. WHO/MSA/MNH/PSF. Geneva: WHO;1997. p.1-15.
- 3. Guayatt GH, Feeny DH, Patrick DL. Measuring health related quality of life. Ann Intern Med. 1993;118(8):622-29.
- 4. Gill TM, Feinstein AR. A critical appraisal of the quality of Quality-of-life Measurements. JAMA. 1994;272(2):619-26.
- 5. Rubin AD, Wodchis WP, Spak C, Kileny PR, Hogikyan ND. Longitudinal Effects of Botox Injections on Voice-Related Quality of Life (V-RQOL) for patients with adductory spasmodic dysphonia. Arch Otolaryngol Head Neck Surg. 2004;130(4):415-20.
- 6. Blas E, Kurup AS. Equity, social determinants and public health programmes. Geneva: World Health Organization; 2010.
- 7. Vido MB, Fernandes RA. Qualidade de vida: considerações sobre conceito e instrumentos de medida. Online Braz J Nurs (Online). 2007; 6(2), ago.
- 8. Guyatt G. Understanding the fundamentals of quality of life measurement. Evid Based Cardiovasc Med. 1998;2(2):35-6.
- 9. Minayo MC, Hartz ZM, Buss PM. Qualidade de vida e saúde: um debate necessário. Ciênc Saúde Coletiva. 2000;5(1):7-31.
- 10. Seidl EMF, Zannon CMLC. Qualidade de vida e saúde: aspectos conceituais e metodológicos. Cad Saúde Pública. 2004;20(2):580-8.
- 11. Amar A, Rapoport A, Franzi SA, Bisordi C, Lehn C. Qualidade de vida e prognóstico nos carcinomas epidermóides de cabeça e pescoço/ Quality of life and prognosis of squamous cell carcinoma of the head and neck . Rev Bras Otorrinolaringol. 2002;68(3):400-3.
- 12. Anant M, Guleria R, Pathak AK, Bhutani M, Pal H, Charu M, Kochupillai V. Quality of life measures in lung cancer. Indian J Cancer. 2005;42(3):125-32.
- 13. Carrau RL, Khidr A, Gold KF, Crawley JA, Hilson EM, Koufman JA, et al. Validation of a quality-of-life instrument for laryngopharyngeal reflux. Arch Otolaryngol Head Neck Sur. 2005;131(4):315-20.
- 14. Behlau M, Oliveira G, Ricarte A, Santos LM. Validação no Brasil de protocolos de autoavaliação do impacto de uma disfonia. Pró-Fono. 2009;21(4):326-32.
- 15. Carding PN, Wilson JA, MacKenzie K, Deary IJ. Measuring voice outcomes: state of the science review. J Laringol Otol. 2009;123(8):823-9.
- 16. Hogikyan ND, Sethuraman G. Validation of an instrument to measure voice-related quality of life (V-RQOL). J Voice. 1999;13(4):557-69.
- 17. Gasparini G, Behlau M. Quality of life: validation of the Brazilian Version of the Voice Related Quality of life measure (V-RQOL). J Voice. 2009;23(1):76-81.
- 18. Ma EP-M, Yiu EM-L. Voice activity and participation profile: Assessing the impact of voice disorders on daily activities. J Speech Hear Res. 2001;44(3):511-24.
- 19. Ricarte A, Gasparini G, Behlau M. Validação do Protocolo Perfil de Participação e Atividades Vocais (PPAV) no Brasil. XIV Congresso Brasileiro de Fonoaudiologia, 2006. Anais. 2006.
- 20. Jacobson HB, Johnson A, Grywalski C, Sillbergleit AK, Jacobson GP, Benninger M, et al. The voice Handicap Index (VHI): development and validation. Am J Speech Lang Pathol. 1997;6(3):66-70.
- 21. Behlau M, Santos LM, Oliveira G. Cross-Cultural Adaptation and Validation of the Voice Handicap Index Into Brazilian Portuguese. J Voice. 2011;25(3): 354-59.
- 22. Carding PN, Horsley IA, Docherty GD. A study of the effectiveness of voice therapy in the treatment of 45 patients with nonorganic dysphonia. J Voice 1999;13(1):72-104. Review.
- 23. Scientific Advisory Committee of Medical Outcomes Trust. Assessing health status and quality of life instruments: attributes and review criteria. Qual Life Res. 2002;11(3):193-205.
- 24. Hazlett DE, Duffy OM, Moorhead SA. Occupational voice demands and their impact on the call-centre industry. BMC Public Health. 2009;9:108.
- 25. Kasama ST, Brasolotto AG. Vocal perception and life quality. Pro-fono. 2007;19(1):19-28.
- 26. Buck F, Drinnan M, Wilson J, Barnard IS. What are the illness perceptions of people with dysphonia: a pilot study. J Laryngol Otol. 2007;121(1):31-9.
- 27. Zraick RI, Risner BY, Smith-Olinde L, Gregg BA, Johnson FL, McWeeny EK. Patient versus partner perception of voice handicap. J Voice. 2007;21(4):485-94.
Publication Dates
-
Publication in this collection
02 Mar 2012 -
Date of issue
Mar 2012
History
-
Received
31 Mar 2011 -
Accepted
05 July 2011