Abstracts
The isolated spontaneous dissection of the celiac artery without the concomitant dissection of the aorta is a rare condition seldomly described in the literature. The objective of the present study is to describe a case of this clinical entity in a 74-year-old, male patient, who was asymptomatic, and whose diagnosis was established by means of ultrasound and confirmed using computed angiotomography. The patient has been successfully followed up by means of clinical management for a period of 25 months.
Celiac artery; dissection; ultrasonography
A dissecção espontânea isolada do tronco celíaco sem a dissecção concomitante da aorta é uma condição rara, pouco descrita na literatura. O objetivo do presente trabalho é descrever um caso dessa entidade clínica em um paciente masculino, 74 anos, assintomático, cujo diagnóstico foi feito por ultrassonografia e confirmado com angiotomografia computadorizada. O paciente tem sido acompanhado com sucesso mediante observação clínica por um período de 25 meses.
Artéria celíaca; dissecção; ultrassonografia
CASE REPORT
IPhD; Associate professor of Angiology and Vascular Surgery at Universidade Estadual de Londrina (UEL), Londrina, PR
IIPhD; Associate professor of Angiology and Vascular Surgery at UEL, Londrina, PR
IIIPhysician in charge of CT angiography at Ultramed - Diagnóstico por Imagem, Londrina, PR
IVPhysician; Specialist in Ultrasonography at Ultramed - Diagnóstico por Imagem, Londrina, PR
VResident of Angioradiology and Endovascular Surgery, UEL, Londrina, PR
VIMedical Student at Universidade Estadual do Oeste do Paraná (UNIOESTE), Cascavel, PR
Correspondence
ABSTRACT
The isolated spontaneous dissection of the celiac artery without the concomitant dissection of the aorta is a rare condition seldomly described in the literature. The objective of the present study is to describe a case of this clinical entity in a 74-year-old male patient, who was asymptomatic, and whose diagnosis was established by means of ultrasound and confirmed using computed angiotomography. The patient has been successfully followed up by means of clinical management for a period of 25 months.
Keywords: Celiac artery, dissection, ultrasonography.
Introduction
Spontaneous dissection of a visceral artery, especially when not associated with aortic dissection, is considered to be a rare entity. Among the dissections of visceral arteries, those that compromise the superior mesenteric artery are the most common ones, while those of the celiac and inferior mesenteric arteries are very infrequent1-3.
Our objective was to describe a case of spontaneous dissection of the celiac artery in an asymptomatic patient, with satisfactory outcome after a 25-month follow-up.
Case report
A 74-year-old male patient was referred to a vascular surgeon because an image compatible with celiac artery dissection was revealed by a routine ultrasonography. The patient denied abdominal pain over the previous months. His past medical history was significant for hyperlipidemia with use of statin and smoking cessation 40 years earlier.
No significant alterations were found at physical examination: the abdomen was painless, flaccid and without palpable tumors. The peripheral pulses were present and normal.
Doppler ultrasonography of the visceral arteries demonstrated moderate fusiform dilatation of the celiac artery, (Figure 1) starting 8 mm after its origin, with an extension of 19 mm, maximum diameters of 18x18 mm and images suggesting dissection (Figure 2). The diameter of the artery proximal do the dissection was 8x8 mm. The superior and inferior mesenteric arteries had normal diameters and flow.
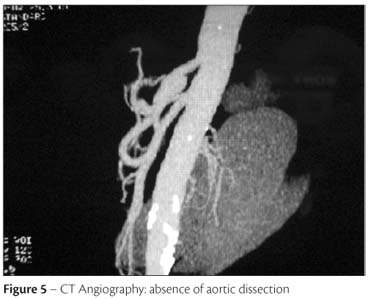
CT angiography of the abdominal aorta with multislice helical technique and tridimensional reconstruction demonstrated findings similar to those of Doppler ultrasonography, with celiac artery transverse diameters of 17.3x15.9 mm and a dissection flap inside the aneurysm (Figures 3 and 4). The abdominal aorta had calcified and non-calcified atheromatous plaques without significant stenosis, with normal diameters and no images of dissection. The superior and inferior mesenteric arteries, as well as the renal arteries, were normal (Figure 5).
As the patient was asymptomatic, we chose to follow up without medications. Doppler ultrasonography has been performed every six months and has not shown any changes, as there has been no increase in the aneurysm diameter, in the extension of the dissection or occlusion of celiac artery branches.
Discussion
Arterial dissection may be defined as a cleavage of the arterial wall between two elastic layers and local hematoma formation2.
Isolated dissection of an artery which is not associated with aortic dissection has been reported in the carotid and renal arteries, but rarely in the visceral arteries1,3-8. The extra-aortic dissections include, in decreasing order, renal, coronary, cerebral, carotid, vertebral and visceral arteries9. It is probable that these dissections were not diagnosed in the past, before the age of imaging methods.
Among visceral arteries dissections, those of the superior mesenteric artery are more frequent10, but those of the inferior mesenteric and celiac arteries and its branches are rare. In a series of 19 patients with dissection of these arteries, Takayama et al.10 found involvement of the superior mesenteric artery in 57.9%, of the celiac artery in 36%, of the isolated hepatic artery in 10.5% and of the splenic artery in only 5.3% of the cases.
Atherosclerosis is the most frequent etiologic factor. There are also reports of cystic degeneration, trauma, fungal infections, fibromuscular dysplasia, pregnancy, connective tissue diseases and periarterial inflammation accompanied by cases of cholecystitis and pancreatitis. However, in more than half of the cases, no definite cause can be found. It happened in our case, which did not present any of the previously mentioned factors.
Males aging 45 to 85 years are the most frequently affected by splanchnic arteries dissections, accounting for 88% of the cases described by Sparks et al.7 and by Takayama et al.10.
As in our patient, nearly half of all dissections of visceral arteries is asymptomatic2,3,11, being detected by imaging methods. In cases of symptomatic dissection of the celiac artery, Matsuo et al.3 reported the possibility of jaundice when the hepatic artery is involved, or of pancreatitis when there the pancreatic arcades are involved and associated with abdominal pain, the most common symptom. Due to the rich collateral circulation originating from the superior mesenteric artery, the thrombotic complications of the celiac artery dissection are often well tolerated.
CT angiography is considered the imaging method of choice. The image most frequently found is the presence of an intimal flap, which confirms the diagnosis of dissection. Other findings are the presence of hematoma in the arterial wall, which generally corresponds to false lumen thrombosis, aneurysm formation and presence of infiltration in the fat tissue surrounding the celiac artery. This last finding, which sometimes is revealed by tomography during investigation of abdominal pain, may indicate the need for CT angiography. D'Ambrosio et al.8 reported that this prognostic factor may suggest dissection extension into the adjacent vases. CT angiography may also enable assessment of dissection extension, of aneurysmal formation and dimensions, and other arteries involvement.
Doppler ultrosonography is also a valuable diagnostic modality that may be readily used without radiation exposure, besides offering precise data for diagnosis. Magnetic resonance imaging and catheter angiography may also be used.
Most authors suggest that non-complicated asymptomatic lesions must receive conservative treatment, with monitoring of the patient by imaging examinations. The use of antiplatelet or anticoagulant agents from three to six months to avoid thromboembolic complications, as well as the modification of cardiac risk factors to limit the spread of the dissection and to reduce the risk of rupture, have been suggested. Our patient did not receive medication and has been asymptomatic for 25 months.
Surgical or endovascular treatment must be carried out only when there is aneurysm formation with progressive growth to a transverse diameter of more than 20 or 24 mm, which represents 2.5 to 3.0 times the normal artery diameter.
Intervention is also indicated in the presence of complications such as arterial rupture, true lumen thrombosis with hepatic ischemia and multiple lesions compromising the lower digestive tract.
However, in a literature review, we verified that the conservative treatment may be safely indicated in patients with limited dissection who do not present evidence of rupture or expansion in a serial follow-up with imaging methods.
References
- 1. Woolard JD, Ammar AD. Spontaneous dissection of celiac artery: A case report. J Vasc Surg. 2007;45:1256-8.
- 2. Chaillou P, Moussu P, Noel SF, et al. Spontaneous dissection of celiac artery. Ann Vasc Surg. 1997;11:413-5.
- 3. Matsuo R, Ohta Y, Ohya Y, et al. Isolated dissection of celiac artery: a case report. Angiology. 2000;51:603-7.
- 4. Muller MF, Kim D. Spontaneous dissection of the hepatic artery. Abdom Imaging. 1995;20:462-5.
- 5. Yasuhara H, Shigematsu H, Muto T. Self-limited spontaneous dissection of the main trunk of the superior mesenteric artery. J Vasc Surg. 1998;27:776-9.
- 6. Suzuki S, Furui S, Kohtake H, et al. Isolated dissection of the superior mesenteric artery: CT findings in six cases. Abdom Imaging. 2004;29:153-7.
- 7. Sparks SR, Vasques JC, ergan JJ, Owens EL. Failure of nonoperative management of isolated superior mesenteric artery dissection. Ann Vasc Surg. 2000;14:105-9.
- 8. D'Ambrosio N, Friedman B, Siegel D, Katz D, Newatia A, Hines J. Spontaneous isolated dissection of the celiac artery: CT findings in adults. AJR Am J Roentgenol. 2007;188:W506-11.
- 9. Glehen O, Feugier P, Aleksic T, Delannoy P, Chealier JM. Spontaneous dissection of the celiac artery. Ann Vasc Surg. 2001;15:687-92.
- 10. Takayama T, Miyata T, Shirakawa M, Nagawa H. Isolated spontaneous dissection of the splanchnic arteries. J Vasc Surg. 2008;48:329-33.
- 11. Foord AG, Lewis RD. Primary dissection aneurysm of peripheral and pulmonary arteries: dissecting hemorrhage of media. Arch Pathol. 1959;68:553-77.
Isolated dissection of the celiac artery: a case report
Publication Dates
-
Publication in this collection
09 Feb 2011 -
Date of issue
Sept 2010
History
-
Received
27 Oct 2009 -
Accepted
19 Nov 2009