Abstract
Several different plant extracts have been evaluated with respect to their antimicrobial effects against oral pathogens and for reduction of gingivitis. Given that a large number of these substances have been associated with significant side effects that contraindicate their long-term use, new compounds need to be tested. The aim of this study was to assess the short-term safety and efficacy of a Lippia sidoides ("alecrim pimenta")-based essential oil mouthrinse on gingival inflammation and bacterial plaque. Fifty-five patients were enrolled into a pilot, double-blinded, randomized, parallel-armed study. Patients were randomly assigned to undergo a 7-day treatment regimen with either the L. sidoides-based mouthrinse or 0.12% chlorhexidine mouthrinse. The results demonstrated decreased plaque index, gingival index and gingival bleeding index scores at 7 days, as compared to baseline. There was no statistically significance difference (p>0.05) between test and control groups for any of the clinical parameters assessed throughout the study. Adverse events were mild and transient. The findings of this study demonstrated that the L. sidoides-based mouthrinse was safe and efficacious in reducing bacterial plaque and gingival inflammation.
Gingivitis; Lippia sidoides; Mouthrinse; Essential oil; Randomized controlled clinical trial
ORIGINAL ARTICLES
Effect of a novel essential oil mouthrinse without alcohol on gingivitis: a double-blinded randomized controlled trial
Marco Antonio BotelhoI; José Gomes Bezerra FilhoII; Luciano Lima CorreaII; Said Gonçalves da Cruz FonsecaIII; Danusa MontenegroIV; Ricardo GapskiV; Gerly Anne Castro BritoVI; Jörg HeukelbachII
IMSc in Public Health, Federal University of Ceará, Fortaleza, CE, Brazil
IIPhD in Public Health, Federal University of Ceará, Fortaleza, CE, Brazil
IIIMsC in Pharmacy, Federal University of Ceará, Fortaleza, CE, Brazil
IVGraduate Student, Federal University of Ceará, Fortaleza, CE, Brazil
VMSc in Periodontics, University of Missouri, Kansas City, MO, U.S.A
VIPhD in Pharmacology, Federal University of Ceará, Fortaleza, CE, Brazil
Corresponding address Corresponding address: Marco A. Botelho Departamento de Saúde Comunitária - Faculdade de Medicina - Universidade Federal do Ceará Rua Prof. Costa Mendes, 1608 - 5º Andar 60.430-170 - Fortaleza, Ceará, Brasil Phone: 55 85 3366-8044/ Fax: 55 85 3366-8050 e-mail: marcobotelho1@gmail.com
ABSTRACT
Several different plant extracts have been evaluated with respect to their antimicrobial effects against oral pathogens and for reduction of gingivitis. Given that a large number of these substances have been associated with significant side effects that contraindicate their long-term use, new compounds need to be tested. The aim of this study was to assess the short-term safety and efficacy of a Lippia sidoides ("alecrim pimenta")-based essential oil mouthrinse on gingival inflammation and bacterial plaque. Fifty-five patients were enrolled into a pilot, double-blinded, randomized, parallel-armed study. Patients were randomly assigned to undergo a 7-day treatment regimen with either the L. sidoides-based mouthrinse or 0.12% chlorhexidine mouthrinse. The results demonstrated decreased plaque index, gingival index and gingival bleeding index scores at 7 days, as compared to baseline. There was no statistically significance difference (p>0.05) between test and control groups for any of the clinical parameters assessed throughout the study. Adverse events were mild and transient. The findings of this study demonstrated that the L. sidoides-based mouthrinse was safe and efficacious in reducing bacterial plaque and gingival inflammation.
Uniterms: Gingivitis; Lippia sidoides; Mouthrinse; Essential oil; Randomized controlled clinical trial.
INTRODUCTION
Bacterial plaque and its byproducts are considered the primary cause of chronic gingival inflammation. The association between poor oral hygiene, dental plaque and the severity of periodontal diseases is also well-established21. Several surveys have demonstrated that plaque-induced gingivitis has reached epidemic proportions worldwide4,24. In Brazil, 80% of the elderly population is affected by periodontal diseases with different levels of severity6. Studies in deprived populations have demonstrated that gingivitis occurs in even greater proportions, being present in the vast majority of adults23.
Gingivitis and poor oral hygiene have been clearly associated with lower socioeconomic status, which may explain in part the high prevalence of gingivitis in resource-poor settings3. In addition, the degree of motivation and dexterity required for optimal oral hygiene may be beyond the ability of most patients, regardless of their socioeconomic status16.
From this perspective, the use of antimicrobial mouthrinses may be considered a useful adjunct to oral hygiene. Several compounds have been evaluated for their effectiveness on supragingival plaque and gingivitis, including bisbiguanides (e.g.: chlorhexidine gluconate)18, phenol-related essential oils5,7,14, triclosan13, quaternary ammonium compounds20 and herbal extract sanguinarine25. However, because of their cost, the majority of these agents are out of reach for patients in developing countries. Therefore, there is a need to develop new agents that are effective, safe and inexpensive.
Lippia sidoides (family Verbenaceae) is a medicinal herb that has been used in traditional medicine for a variety of antifungal and antimicrobial purposes17. This is a typical shrub commonly growing in the Northeast of Brazil, where it is popularly known as "alecrim-pimenta", and is available at low cost. Biochemical data have shown that oils and extracts from L. sidoides are rich in thymol and cavacrol5, which are compounds known for their antimicrobial properties19. Previous studies indicated that a L. sidoides-based mouthrinse reduced the severity of gingival inflammation, bacterial plaque in humans and histological inflammatory infiltrate in dogs7,12. The purpose of this double-blinded pilot clinical investigation was to examine the short-term efficacy and safety of L. sidoides essential oil mouthrinse on gingival inflammation and bacterial plaque in a high-caries risk population of Northeastern Brazil.
MATERIAL AND METHODS
Plant material
Lippia sidoides leaves were collected in august 2004 from the Medicinal Herb Garden "Prof. Francisco José de Abreu Matos" (Fortaleza, CE, Brazil), after approval by the Federal University of Ceará Ethics in Research Committee (#551/04). Taxonomic identification of plants was performed by botanists of the Prisco Bezerra Herbarium, Department of Biology, Federal University of Ceará, where a voucher specimen has been deposited (# 25149).
Essential oil extraction
Leaf essential oil was extracted using a modified Clevenger apparatus by the hydro-distillation technique8. Thereafter, the volume of essential oil obtained in both extractions was measured and the essential oil was stored in hermetically sealed glass receptacles with rubber lids, covered with aluminum foil to protect the contents from light, and was kept under refrigeration at 8°C until use.
Gas chromatography-mass spectrum analysis
The chemical composition of the essential oil was determined at the Technological Development Center (PADETEC) at the Federal University of Ceará by gas chromatography-mass spectroscopy (GC-MS) using a Hewlett-Packard 5971 GC/MS apparatus (Avondale, PA, USA) under the following conditions: a 0.25 mm x 30 m polydimethylsiloxane DB-1 fused silica capillary column, with a film thickness of 0.10 mm; helium as the carrier gas (1 mL/min), injector temperature of 250ºC, and detector temperature of 200ºC. The column temperature ranged from 35 to 180 ºC /min, at 4ºC V/min, and then from 180 to 280ºC, at 20 ºC V/ min; mass spectra were obtained by electronic impact 70 eV. The constituents were identified by a computer-based library search, with retention indices and visual interpretation of the mass spectra9.
L. sidoides mouthrinse preparation
L. sidoides essential oil was prepared from leaves collected from the medicinal herb garden of the Federal University of Ceará, Brazil. The botanical identification of the leaves was performed by the Department of Organic Chemistry at the same institution. The leaves were then dried under controlled conditions and a hydro-ethanolic process was used to extract the oils that were subsequently used for preparation of 1% L. sidoides mouthrinse essential oil. The mouthrinse was prepared at the School of Pharmacy of the Federal University of Ceará.
Ethics
Written informed consent was obtained from all individuals willing to participate in the research protocol approved by the Institutional Review Board of the Federal University of Ceará, Brazil. The experiments were done in accordance to the Helsinki Declaration27.
Study Design
Fifty-five patients (aged 17 to 63 years) were enrolled into a pilot, single-center, double-blinded, randomized, parallel-armed study. Patients with a minimal average gingival index of 1.2 and having at least 10 teeth in the functional dentition were included. The following individuals were excluded: patients unwilling to complete the treatment protocol, females who were pregnant, subjects with any disease that would preclude the use of the substances used in the study (e.g.: mental diseases) as well as subjects that had used any type of antibacterial mouthrinse within four weeks of enrollment into the study. Volunteers were recruited from a low socioeconomic urban area in Fortaleza city, located in the northeast of Brazil.
Eligible patients were then randomly assigned to test and control groups using a block-randomization design from a computer-generated list. The patients were submitted to a meticulous evaluation to score the visible plaque index and the gingival bleeding index (GBI) for each tooth2. The test group received a 7-day b.i.d. treatment course of Lippia sidoides-based mouthrinse (n=27) while the positive control group received the same regimen with 0.12% chlorhexidine mouthrinse (n=28). A third group was put on a regimen of an Azadirachta indica-based mouthrinse (n=26). The results from the A. indica group are presented elsewhere. The variation in the number of participants per group was a result of the randomization process.
Clinical assessment and intervention
At baseline, patients were examined clinically, including evaluation of plaque index (PI), gingival index (GI) and gingival bleeding index (GBI) scores, measured at four sites per tooth2. After baseline examination, the subjects were instructed to rinse approximately 15 mL of mouthrinse for 30 seconds, twice a day (once after breakfast and once in the late afternoon) during a 7-day period. All rinses were performed under supervision of a study assistant to guarantee standardization and correct use. The study assistant was not involved in the clinical examination of the participants. Compliance was defined as completing 50% or more of the mouthwashes. During the 4 weeks of trial, the volunteers continued to exercise their regular non-supervised, self-performed plaque control measures. The clinical exam with the same parameters was repeated 7 days after baseline, and subjects were also interviewed regarding adverse events. All clinical examinations were conducted by a single investigator, who was an experienced dentist familiar with clinical assessment of PI, GI and GBI. The investigator was blinded to the allocated treatment and did not participate in the intervention. In addition, demographic data including gender, age, smoking status, number of present teeth, level of education and yearly family income were assessed.
Statistical analysis
The treatment groups were compared to each other with respect to demographic background information (age, percentage of females, tobacco use, number of teeth present, level of education, family income) as well as to their results regarding PI, GI and GBI. For this analysis, proportions were compared using Fisher's exact test and the Mann-Whitney U-test for independent samples was used to test for significant differences.
Stata statistical software (Stata Corporation, College Station, USA) was used for data analysis. Data were first averaged within each patient, and then patient means were analyzed between treatment groups to determine baseline comparability of both groups. Significance level was set at 5%. Efficacy analyses were performed for each post-baseline visit upon an intent-to-treat population. The Wilcoxon test was used to identify which means (7- day treatment) were significantly different from baseline. The bacteriological counts were log10 transformed prior to statistical analysis to homogenized variances and eliminate the superdispersion.
RESULTS
Baseline comparison
About 30% of the initial population did not meet the inclusion criteria or were excluded. The most common reason for exclusion was the lack of a minimal number of teeth required for the study. None of the eligible patients refused to participate in the trial. The study population comprised 55 subjects, 27 assigned to the L. sidoides group and 28 assigned to the chlorhexidine group. During the study, two participants of each group were non-compliant with the treatment protocol and were excluded. In addition, 6 subjects per group could not be reached for follow-up visits, resulting in a sample size of 19 subjects in the test group and 20 subjects in the positive control group for the final data analysis.
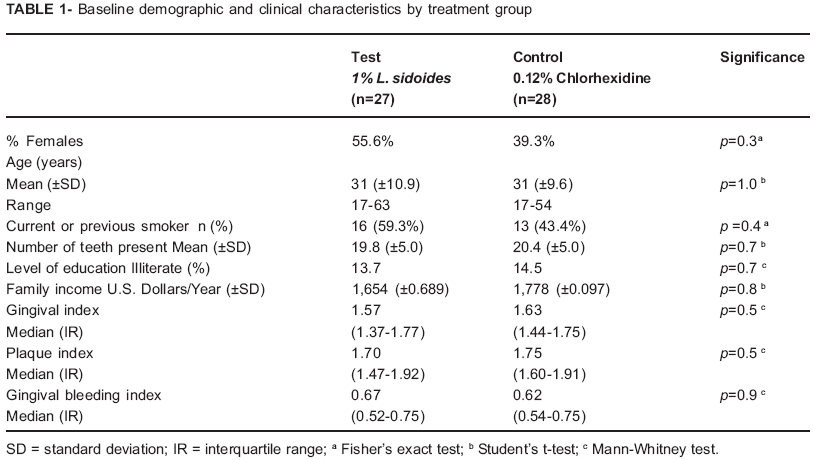
Baseline demographic and clinical data of both groups are shown on Table 1. The overall mean age for the test group was 31 ± 10.9 years (17-63 years) and 31 ± 9.6 years (17-54 years) for the control group (p=1.0). All parameters including gender, smoking status, level of education, yearly family income, number of teeth present, plaque index, gingival index and gingival bleeding index were not statistically significant between the groups at baseline (all p>0.3).
Treatment outcomes
The GI score means at baseline and 7 days are depicted on Figure 1A. Within subjects, effect data showed a statistically significant decrease in GI score means for both groups at 7 days, compared to baseline (p<0.001). Similarly, PI and GBI scores decreased significantly in both groups 7 days after baseline (Figures 1B and C ) (p<0.001).
There was no statistically significant difference between the L. sidoides-based mouthrinse and 0.12% chlorhexidine for any of the clinical parameters examined throughout the study.
Adverse events
The most commonly reported adverse event was mild burning sensation, totalizing 44% and 14% of the complaints for the test and positive control groups, respectively. Altered taste was mentioned in 22% of the test patients and 21% of the control patients and was mild and transient in nature. Two subjects in the L. sidoides group complained of nausea and 1 experienced epithelium desquamation after the treatment period. Overall, 17 (62%) subjects described adverse events in the test group and 9 (32%) in the positive control group. All adverse events were of transient nature and resolved without any specific treatment.
DISCUSSION
Reports of several medicinal herbs used empirically in the treatment and prevention of different oral conditions including toothache, caries and gingivitis5,15 have been published worldwide. Some of these substances have an effect against cariogenic and periodontal pathogens, including the Indian neem tree (Azadirachta indica)22. However, in Brazil due to the lack of adequately controlled studies, the effectiveness of these natural products and extracts remains undetermined.
L. sidoides (family of Verbanaceae) is a plant that grows virtually anywhere in northeastern Brazil and has been historically used by indigenous people. This species produces an essential oil rich in phenolic compounds, such as thymol and carvacrol, and it has been used in the traditional medicine for treatment of a variety of human diseases of bacterial and fungal origin5,12. Because of its low cost, the use of L. sidoides-based essential oil in the prevention and treatment of oral conditions could be beneficial for low socioeconomic urban and rural communities. This formulation may also be advantageous in regions where L. sidoides is a culturally accepted plant17,19.
Another advantage of this agent is the absence of any alcohol content. There has been some concern with a possible association between high-alcohol-content mouthwashes and oral and pharyngeal cancers26. Although such a correlation has not been confirmed by prospective studies, the use of an ethanol-free mouthrinse would eliminate this potential risk.
The findings of the present study showed that a 7-day treatment regimen with L. sidoides-based essential oil significantly reduced plaque, gingival and bleeding indices as compared to baseline. In addition, it was shown that such a decrease was statistically similar to the positive control, 0.12% chlorhexidine, whose choice was due to the fact that it appears to be the most effective chemical agent for plaque control1. Although chlorhexidine is considered an effective adjunct to plaque reduction measures, its use in daily practice is still limited because of several side effects10. In the present study, the most commonly related adverse event was burning and altered sensation immediately after rinsing. Interestingly, the burning sensation from the test group was three more common than that of the control group. It is difficult to speculate whether the burning sensation was related to the essential oils derivatives (thymol/carvacrol) or to other components included in the final mouthrinse formulation, such as polysorbate 80 and citric acid. Future investigations with different formulations are needed to answer this question.
In the present study, 1 patient experienced epithelium desquamation after the 7-day treatment regimen with Lippia sidoides mouthrinse. This finding was transient in nature and disappeared after 30 days (unpublished data). Mucosal desquamation has been reported after use of several oral health care products including chlorhexidine11. It is difficult to conclude from the number of patients enrolled in this trial whether this case was isolated in nature or if there is a correlation between epithelium desquamation and the tested mouthrinse. Further research with larger sample sizes are needed to assess all confounding factors (pH, flavoring, essential oils and patient predisposition). Finally, the occurrence of mild nausea in 2 patients of the test group was attributed to a gag-reflex reaction during rinsing and consequent ingestion of a small amount of the product. They reported uneventful history soon after the episodes.
CONCLUSION
Within the limitation of this trial, it was demonstrated that the Lippia sidoides-based mouthrinse was relatively safe and effective in reducing plaque index, gingival index and gingival bleeding index scores in a high-caries risk population. The reduction of the scores was statistically similar to that observed in the control group (0.12% chlorhexidine). The outcomes of the present study may have an important impact on the development of effective and inexpensive oral health interventions in low-socioeconomic communities. Future long-term prospective studies with larger sample sizes are required to confirm our findings.
ACKNOWLEDGEMENTS
The authors would like to acknowledge FUNCAP (Fundação Cearense de Apoio ao Desenvolvimento Científico e Tecnológico) for financial support and Prof. Dr. Luiz Odorico Monteiro de Andrade for assistance and support. We are also grateful for the skillful help of the Mandacaru Foundation and the Community Leaders Marilene, Luís and Antonia Valéria Assunção Santos, and Aécio Santiago, Jose Leomar and José Maria (in memoriam) Jornal Diário do Nordeste.
Received: September 13, 2006
Modification: March 16, 2007
Accepted: April 17, 2007
- 1- Addy M. Chlorhexidine compared with other locally delivered antimicrobials: a short review. J Clin Periodontol. 1986;13:957-64.
- 2- Ainamo J, Bay I. Problems and proposals for recording gingivitis and plaque. Int Dent J. 1975;25:229-35.
- 3- Baelum V, Fejerskov O, Karring T. Oral hygiene, gingivitis and periodontal breakdown in adult Tanzanians. J Periodontal Res. 1986;21:221-32.
- 4- Bhat M. Periodontal health of 14-17-year-old US schoolchildren. J Public Health Dent. 1991;51:5-11.
- 5- Botelho MA, Nogueira NA, Bastos GM, Fonseca SG, Lemos TL, Matos FJ, et al. Antimicrobial activity of the essential oil from Lippia sidoides, carvacrol and thymol against oral pathogens. Braz J Med Biol Res. 2007;40:349-56
-
6- Brasil. Ministério da Saúde. Departamento de Ação Básica. Programa Brasil Sorridente. Levantamento das condições de saúde bucal da população brasileira - SB Brasil 2003 [homepage na internet]. Brasília, DF: Ministério da Saúde; c2006 [acesso em 2006 maio 23]. Disponível em: http://www.saude.gov.br
- 7- Botelho MA, Soares JB. O óleo essencial do alecrim-pimenta (Lippia sidoides Cham) na prevenção da cárie dental [trabalho apresentado]. 13ş Simpósio de Plantas Medicinais do Brasil; 1994 set 20-23; Fortaleza, CE.
- 8- Craveiro AA, Matos FJA, Alencar JW. A simple and inexpensive steam generator for essential oils extraction. J Chem Educ. 1976;53:652.
- 9- Craveiro AA, Matos FJA, Alencar JW. Kovats indices as pre-selection routine in mass spectra library search of volatiles. J Nat Prod. 1984;47:890-92.
- 10- Flotra L, Gjermo P, Rolla G, Waerhaug J. Side effects of chlorhexidine mouth washes. Scand J Dent Res. 1971;79:119-25.
- 11- Gagari E, Kabani S. Adverse effects of mouthwash use: a review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995;80:432-9.
- 12- Girao VC, Nunes-Pinheiro DC, Morais SM, Sequeira JL, Gioso MA. A clinical trial of the effect of a mouth-rinse prepared with Lippia sidoides Cham essential oil in dogs with mild gingival disease. Prev Vet Med. 2003;59:95-102.
- 13- Gjermo P, Saxton CA. Antibacterial dentifrices: clinical data and relevance with emphasis on zinc/triclosan. J Clin Periodontol. 1991;18:468-73.
- 14- Gordon JM, Lamster IB, Seiger MC. Efficacy of Listerine antiseptic in inhibiting the development of plaque and gingivitis. J Clin Periodontol. 1985;12:697-704.
- 15- Hebbar SS, Harsha VH, Shripathi V, Hegde GR. Ethnomedicine of Dharwad district in Karnataka, Indiaplants used in oral health care. J Ethnopharmacol. 2004;94:261-6.
- 16- Koch G, Lindhe J. The effect of supervised oral hygiene on the gingiva of children. J Periodontal Res. 1967;2:64-9.
- 17- Lacoste E, Chaumont JP, Mandin D, Plumel MM, Matos FJ. Antiseptic properties of essential oil of Lippia sidoides Cham: application to the cutaneous microflora. Ann Pharm Fr. 1996;54:228-30.
- 18- Lang NP, Hotz P, Graf H, Geering AH, Saxer UP, Sturzenberger OP, et al. Effects of supervised chlorhexidine mouthrinses in children: a longitudinal clinical trial. J Periodontal Res. 1982;17:101-11.
- 19- Lemos TLG, Craveiro AA, Alencar JW, Matos FJA, Clarck AM, MacChesney JD. Antimicrobial activity of essential oil of brazilian plants. Phytother Res. 1990;4:82-4.
- 20- Lobene RR, Kashket S, Soparkar PM, Shloss J, Sabine ZM. The effect of cetylpridinium chloride on human plaque bacteria and gingivitis. Pharmacol Ther Dent. 1979;4:33-47.
- 21- Moore WE, Holdeman LV, Smibert RM, Cato EP, Burmeister JA, Palcanis KG, et al Bacteriology of experimental gingivitis in young adult humans. Infect Immun. 1982;38:651-67.
- 22- Pai MR, Acharya LD, Udupa N. Evaluation of antiplaque activity of Azadirachta indica leaf extract gel-a 6-week clinical study. J Ethnopharmacol. 2004;90:99-103.
- 23- Petersen PE. Challenges to improvement of oral health in the 21st century-the approach of the WHO Global Oral Health Programme. Int Dent J. 2004;54:329-43.
- 24- Theilade E, Wright WH, Jensen SB, Löe H. Experimental gingivitis in man. II. A longitudinal clinical and bacteriological investigation. J Periodontal Res. 1966;1:1-13.
- 25- Wennstrom J, Lindhe J. Some effects of a Sanguinarine-containing mouthrinse on developing plaque and gingivitis. J Clin Periodontol. 1985;12:867-72.
- 26- Winn DM, Blot WJ, McLaughlin JK, Austin DF, Greenberg RS, Preston-Martin S, et al. Mouthwash use and oral conditions in the risk of oral and pharyngeal cancer. Cancer Res. 1991;51:3044-7.
- 27- World Medical Association. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. Bull World Health Organ. 2001;79:373-4.
Corresponding address:
Publication Dates
-
Publication in this collection
24 Aug 2007 -
Date of issue
June 2007
History
-
Reviewed
16 Mar 2007 -
Received
13 Sept 2006 -
Accepted
17 Apr 2007