Abstract
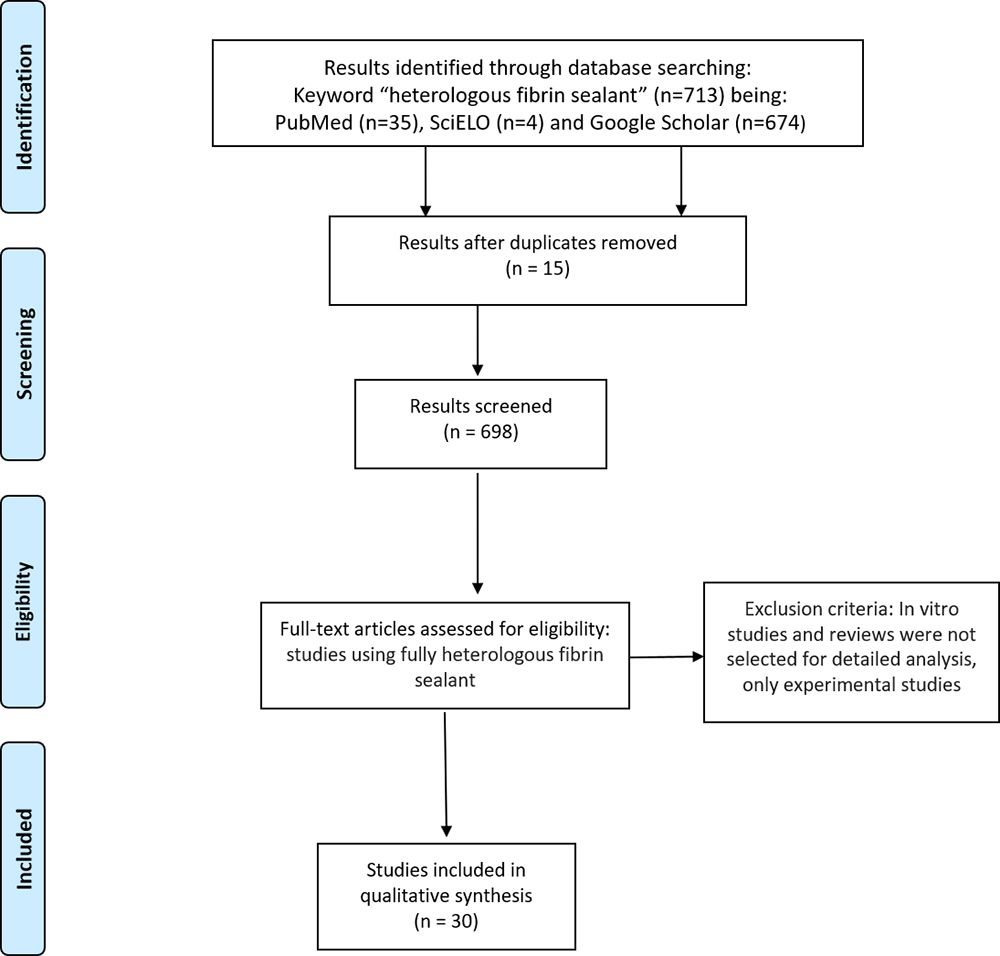
Fibrin biopolymers, previously referred as “fibrin glue” or “fibrin sealants”, are natural biomaterials with diverse applications on health. They have hemostatic, adhesive, sealant, scaffold and drug delivery properties and have become widely used in medical and dental procedures. Historically, these biomaterials are produced from human fibrinogen and human or animal thrombin, and the possibility of transmission of infectious diseases by human blood is not ruled out. In the 1990s, to overcome this problem, a new heterologous biomaterial composed of a thrombin-like enzyme purified from Crotalus durissus terrificus venom and a cryoprecipitate rich in fibrinogen extracted from buffaloes Bubalus bubalis blood has been proposed. Therefore, a systematic review of studies on exclusively heterologous fibrin sealants published between 1989 and 2018 was carried out using the following databases: PubMed, SciELO and Google Scholar. The keyword used was “heterologous fibrin sealant”. The search resulted in 35 scientific papers in PubMed, four in SciELO and 674 in Google Scholar. After applying the inclusion/exclusion criteria and complete reading of the articles, 30 studies were selected, which formed the basis of this systematic review. It has been observed that the only completely heterologous sealant is the one produced by CEVAP/UNESP. This heterologous biopolymer is proven effective by several studies published in refereed scientific journals. In addition, clinical trials phase I/II for the treatment of chronic venous ulcers authorized by the Brazilian Health Regulatory Agency (ANVISA) were completed. Preliminary results have indicated a safe and promising effective product. Phase III clinical trials will be proposed and required to validate these preliminary findings.
Keywords
Fibrin sealant; Snake venom; Thrombin-like enzyme; Cryoprecipitate coagulum
BACKGROUND
Fibrin sealants are biological materials composed of fibrinogen and thrombin. In the presence of calcium and factor XIII, thrombin converts fibrinogen to soluble fibrin, forming a stable clot and mimicking the final step of the coagulation cascade. Due to its property, this product has indications based mainly on its hemostatic and tissue adhesive properties. Thus, its recent clinical and experimental uses include drug administration and tissue engineering applicability [11. Spotnitz WD. Fibrin sealant: Past, present, and future: a brief review. World J Surg. 2010 Apr;34(4):632-4.].
The use of fibrin compounds as a hemostatic agent occurred for the first time in Germany in 1909 [22. Bergel S. Ueber Wirkungen des Fibrins. Dtsch med Wochenschr. 1909;35(15):663-5.]. In the 1940s, it was used as an adhesive in the recovery of injured peripheral nerves through the association of autologous fibrinogen and thrombin [33. Sameem M, Wood TJ, Bain JR. A systematic review on the use of fibrin glue for peripheral nerve repair. Plast Reconstr Surg. 2011 Jun;127(6):2381-90.], and also for skin graft fixation [44. Young JZ, Medawar PB. Fibrin suture of peripheral nerves. Measurement of the rate of regeneration. Lancet. 1940 Aug 3; 236 (6101):126-8.,55. Cronkite EP, Lozner EL, Deaver JM. Use of thrombin and fibrinogen in skin grafting. JAMA. 1944;124(14):976-8.].
Sutures are the conventional technique in surgical procedures; however, due to the formation of fistulas, granulomas, tissue ischemia, and lacerations in some cases, tissue engineering has been stimulating the use of fibrin-based sealants [66. Thomazini-Santos IA, Barraviera SRCS, Mendes-Giannini MJS, Barraviera B. Surgical adhesives. J Venom Anim Toxins. 2001 Dec;7(2):159-71. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000200002.
http://www.scielo.br/scielo.php?script=s...
]. Thus, these products have been used in current clinical and surgical applications, mainly to approach the edges of the skin, to produce adherence to other tissues and to provide hemostasis [66. Thomazini-Santos IA, Barraviera SRCS, Mendes-Giannini MJS, Barraviera B. Surgical adhesives. J Venom Anim Toxins. 2001 Dec;7(2):159-71. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000200002.
http://www.scielo.br/scielo.php?script=s...
-99. Ferreira RS Jr, de Barros LC, Abbade LPF, Barraviera SRCS, Silvares MRC, de Pontes LG, et al. Heterologous fibrin sealant derived from snake venom: From bench to bedside - an overview. J Venom Anim Toxins Incl Trop Dis. 2017 Apr 4; 23 (1):1-12. doi:10.1186/s40409-017-0109-8.
https://doi.org/10.1186/s40409-017-0109-...
].
Traditionally, fibrin sealants are produced in two ways: using autologous or homologous blood derivatives [1010. Matras H. Fibrin seal: The state of the art. J Oral Maxillofac Surg. 1985;43(8):605-11.,1111. Barros LC, Ferreira RS Jr, Barraviera SRCS, Stolf HO, Thomazini-Santos IA, Mendes-Giannini MJS. A new fibrin sealant from crotalus durissus terrificus venom: applications in medicine. J Toxicol Environ. 2009 Dec 2;12(8):553-71.]. Autologous sealants use the patient's own blood. Although biocompatible and presenting no risk of infectious diseases transmission, they are not feasible in emergency surgeries [1212. Ferreira Jr RS. Autologous or heterologous fibrin sealant scaffold: which is the better choice? J Venom Anim Toxins incl Trop Dis. 2014 Jul18;20:31. doi:10.1186/1678-9199-20-31.
https://doi.org/10.1186/1678-9199-20-31...
]. As an alternative, the homologous fibrin sealants produced by a pool of human blood has been used [1313. Pomini KT, Buchaim DV, Andreo JC, Rosso MPO, Colleta BBD, German IJS, et al. Fibrin sealant derived from human plasma as a scaffold for bone grafts associated with photobiomodulation therapy. Int J Mol Sci. 2019 Apr;20(7):1761.]. However, in these cases the literature suggests risks of infectious diseases transmission such as hepatitis, HIV and human parvovirus [1414. Eder G, Neumann M, Cerwenka R, Baumgarten K. Preliminary Results of a Randomized Controlled Study on the Risk of Hepatitis Transmission of a Two-Component Fibrin Sealant (Tissucol/Tisseel). In: Schlag G, Redl H, eds. Fibrin Sealant in Operative Medicine. Berlin, Heidelberg: Springer Berlin Heidelberg; 1986.-1616. Kawamura M, Sawafuji M, Watanabe M, Horinouchi H, Kobayashi K. Frequency of transmission of human parvovirus B19 infection by fibrin sealant used during thoracic surgery. Ann Thorac Surg. 2002 Apr;73(4):1098-100.].
Therefore, a group of Brazilian researchers from the Center for the Study of Venoms and Venomous Animals (CEVAP) of São Paulo State University (UNESP), Brazil, proposed a new heterologous fibrin sealant (HFS) using a snake venom fraction extracted from Crotalus durissus terrificus and a cryoprecipitate rich in fibrinogen obtained from Bubalus bubalis buffaloes blood [1111. Barros LC, Ferreira RS Jr, Barraviera SRCS, Stolf HO, Thomazini-Santos IA, Mendes-Giannini MJS. A new fibrin sealant from crotalus durissus terrificus venom: applications in medicine. J Toxicol Environ. 2009 Dec 2;12(8):553-71.,1717. Ferreira ASSBS, Barraviera B, Barraviera SRCS, Abbade LPF, Caramori CA, Ferreira RS Jr. A success in Toxinology translational research in Brazil: Bridging the gap. Toxicon. 2013 Jul;69:50-4.-1919. Ferreira Junior RS, da Silva DAF, Biscola NP, Sartori MMP, Denadai JP, Jorge AM, et al. Traceability of animal protein byproducts in ruminants by multivariate analysis of isotope ratio mass spectrometry to prevent transmission of prion diseases. J Venon Anim Toxins incl Trop Dis. 2019 May 13;25. doi.org/10.1590/1678-9199-jvatitd-1487-18.
https://doi.org/10.1590/1678-9199-jvatit...
].
Snake venoms are composed of several proteolytic enzymes, mainly serine proteases [2020. Barros LC, Soares AM, Costa FL, Rodrigues VM, Fuly AL, Giglio JR, et al. Biochemical and biological evaluation of gyroxin isolated from Crotalus durissus terrificus venom. J Venom Anim Toxins incl Trop Dis. 2011;17(1):23-33. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000100004.
http://www.scielo.br/scielo.php?script=s...
-2222. Pirkle H. Thrombin-like enzymes from snake venoms: an updated inventory. Thrombosis and Haemostasis. Scientific and Standardization Committee's Registry of Exogenous Hemostatic Factors. 1998 Mar;79(3):675-83.]. These enzymes act by activating or inhibiting the specific blood factor involved in platelet aggregation, coagulation and/or fibrinolysis [2020. Barros LC, Soares AM, Costa FL, Rodrigues VM, Fuly AL, Giglio JR, et al. Biochemical and biological evaluation of gyroxin isolated from Crotalus durissus terrificus venom. J Venom Anim Toxins incl Trop Dis. 2011;17(1):23-33. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000100004.
http://www.scielo.br/scielo.php?script=s...
,2323. Le Guéhennec L, Layrolle P, Daculsi G. A review of bioceramics and fibrin sealant. Eur Cell Mater. 2004 Sep 13;8:1-10.,2424. Palacio TZ, Santos-Filho NA, Rosa JC, Ferreira Jr RS, Barraviera B, Sampaio SV. Isolation and characterization of a novel metalloprotease inhibitor from Bothrops alternatus snake serum. Int J Biol Macromol. 2017 May;98:436-46.]. In in vitro experiments, a thrombin-like enzyme from the South American rattlesnake acts similarly to human or animal thrombins transforming fibrinogen into fibrin and forming a robust insoluble fibrin-net [2020. Barros LC, Soares AM, Costa FL, Rodrigues VM, Fuly AL, Giglio JR, et al. Biochemical and biological evaluation of gyroxin isolated from Crotalus durissus terrificus venom. J Venom Anim Toxins incl Trop Dis. 2011;17(1):23-33. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000100004.
http://www.scielo.br/scielo.php?script=s...
,2222. Pirkle H. Thrombin-like enzymes from snake venoms: an updated inventory. Thrombosis and Haemostasis. Scientific and Standardization Committee's Registry of Exogenous Hemostatic Factors. 1998 Mar;79(3):675-83.].
The first experimental studies using the HFS produced by CEVAP were performed by Juan et al. in 1995 [2525. Juan FC, Thomazini IA, Gianini MJM, Viterbo F, Toscano E, Moraes RA, et al. Reparation of peripheral nerves with fibrin glue prepared from snake venom. Preliminary results. Sao Paulo Med J. 1995 Sep-Oct;113(5):1000-2.], who presented the preparation procedures and observed good adhesive and hemostatic properties in the repair of nerve injuries in rats. In 1998, Thomazini-Santos et al. [2626. Thomazini-Santos IA, Giannini MJSM, Toscano E, Machado PEA, Lima CRG, Barraviera B. The evaluation of clotting time in bovine thrombin, Reptilase ® , and thrombin-like fraction of Crotalus durissus terrificus venom using bovine, equine, ovine, bubaline and human cryoprecipitates. J Venom Anim Toxins. 1998;4(2):120-36. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301998000200004.
http://www.scielo.br/scielo.php?script=s...
] showed that the cryoprecipitate extracted from bubaline blood had higher concentrations of fibrinogen and better performance when compared with blood from humans, bovines, ovine or equines. Additionally, they concluded that antifibrinolytic agents were not required to this sealant to achieve successful coaptation of skin surgical edges [2727. Thomazini-Santos IA. Fibrin adhesive from snake venom: the effect of adding e-aminocaproic acid, tranexamic acid and aprotinin for coaptation of wound in rat skin incisions. J Venom Anim Toxins. 2001;7(1):148-9. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000100011.
http://www.scielo.br/scielo.php?script=s...
]. Stolf et al. [2828. Stolf HO. The use of fibrin adhesive derived from snake venom and the evaluation of skin grafting using skin from the patient’s nasolabial fold. J Venom Anim Toxins. 1999;5(2):227. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301999000200011.
http://www.scielo.br/scielo.php?script=s...
] applied for the first time this new sealant in humans as an alternative to conventional suture in the nasolabial region, and described a good adhesive capacity and healing of this material. After these conclusions, the researchers standardized the unique HFS using gyroxin - a serinoprotease obtained from the South American rattlesnake - and a cryoprecipitate extracted from Bubalus bubalis buffaloes [99. Ferreira RS Jr, de Barros LC, Abbade LPF, Barraviera SRCS, Silvares MRC, de Pontes LG, et al. Heterologous fibrin sealant derived from snake venom: From bench to bedside - an overview. J Venom Anim Toxins Incl Trop Dis. 2017 Apr 4; 23 (1):1-12. doi:10.1186/s40409-017-0109-8.
https://doi.org/10.1186/s40409-017-0109-...
,1111. Barros LC, Ferreira RS Jr, Barraviera SRCS, Stolf HO, Thomazini-Santos IA, Mendes-Giannini MJS. A new fibrin sealant from crotalus durissus terrificus venom: applications in medicine. J Toxicol Environ. 2009 Dec 2;12(8):553-71.].
After these trials, several pioneering experimental studies have been carried out. Currently, the new sealant is being used in several clinical and biotechnological practices, such as in dental surgeries [88. Chiquito GCM. Comparison between suture and fibrin adhesive derived from snake venom for fixation of connective tissue graft in correction of marginal tissue recession. J Venom Anim Toxins incl Trop Dis. 2007;13(2):559.,2929. Barbosa MDS, Gregh SLA, Passanezi E. Fibrin adhesive derived from snake venom in periodontal surgery. J Periodontol. 2007 Oct;78(10):2026-31.,3030. Barbosa MDS, Stipp AC, Passanezi E, Greghi SLA. Fibrin adhesive derived from snake venom in periodontal surgery. Histological analysis. J Appl Oral Sci. 2008 Sep-Oct;16(5):310-5.], recovery of injured nervous [3131. Biscola NP, Cartarozzi LP, Ulian-Benitez S, Barbizan R, Castro MV, Spejo AB, et al. Multiple uses of fibrin sealant for nervous system treatment following injury and disease. J Venom Anim Toxins incl Trop Dis. 2017 Mar 14;23:13. doi:10.1186/s40409-017-0103-1.
https://doi.org/10.1186/s40409-017-0103-...
-3333. Buchaim RL, Andreo JC, Barraviera B, Ferreira Jr RS, Buchaim DV, Rosa Jr GM, et al. Effect of low-level laser therapy (LLLT) on peripheral nerve regeneration using fibrin glue derived from snake venom. Injury. 2015 Apr;46(4):655-60.], bone repair [3434. Cunha MR, Menezes FA, Santos GR, Pinto CAL, Barraviera B, Martins VCAM, et al. Hydroxyapatite and a new fibrin sealant derived from snake venom as scaffold to treatment of cranial defects in rats. Mat Res. 2015 Jan-Feb;18(1):196-203.-3636. de Oliveira Gonçalves JB, Buchaim DV, de Souza Bueno CR, Pomini KT, Barraviera B, Júnior RSF, et al. Effects of low-level laser therapy on autogenous bone graft stabilized with a new heterologous fibrin sealant. J Photochem Photobiol B. 2016 Sep;162:663-8.], and treatment of chronic venous ulcers [3737. Gatti MAN. Treatment of venous ulcers with surgical adhesives derived from snake venom. J Venom Anim Toxins incl Trop Dis. 2009:15(2). http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992009000200020.
http://www.scielo.br/scielo.php?script=s...
,3838. Gatti MAN, Vieira LM, Barraviera B, Barraviera SRCS. Treatment of venous ulcers with fibrin sealant derived from snake venom. J Venom Anim Toxins incl Trop Dis. 2011;17(2):226-9. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000200015.
http://www.scielo.br/scielo.php?script=s...
,3939. Abbade LPF. A new fibrin sealant derived from snake venom candidate to treat chronic venous ulcers. J Am Acad Dermatol. 2015 May;72(5):AB271.].
Thereby, due to its clinical importance and increasing use in several health areas, the aim of this systematic review was to evaluate and compare studies on exclusively heterologous fibrin sealants produced worldwide.
METHODS
A systematic review of the literature on HFS was carried out in November 2018 from PubMed, SciELO and Google Scholar databases taking into account work conducted between 1989 and 2018. The used keywords were “heterologous fibrin sealant”. The inclusion criteria were the analysis of the title and abstract, in order to identify studies that used only heterologous components in the fibrin sealant. In vitro studies and reviews were not selected for detailed analysis, only experimental studies.
RESULTS
The search resulted in 35 scientific papers in PubMed, four in SciELO and 674 in Google Scholar. After applying the inclusion/exclusion and reading criteria, a total of thirty studies were selected to form the basis of this systematic review (Figure 1). Table 1 summarizes the main articles included.
DISCUSSION
The unique heterologous fibrin sealant (HFS) produced by CEVAP was the only completely heterologous material validated and included in this review. It possesses several advantages such as: fast production process; low cost; potential to act as a scaffold for stem cells and biomaterials, and as a new drug delivery system [99. Ferreira RS Jr, de Barros LC, Abbade LPF, Barraviera SRCS, Silvares MRC, de Pontes LG, et al. Heterologous fibrin sealant derived from snake venom: From bench to bedside - an overview. J Venom Anim Toxins Incl Trop Dis. 2017 Apr 4; 23 (1):1-12. doi:10.1186/s40409-017-0109-8.
https://doi.org/10.1186/s40409-017-0109-...
,6262. Gasparotto VPO, Landim-Alvarenga FC, Oliveira ALR, Simões GF, Lima-Neto JF, Barraviera B, et al. A new fibrin sealant as a three-dimensional scaffold candidate for mesenchymal stem cells. Stem Cell Res Ther. 2014 Jun 10;5(3):78.]. Moreover, another positive point is its wide applicability in medical, veterinary and dental practice due to the possibility of custom formulation and replacement of conventional sutures. Considering all the properties described for this bioproduct, which go beyond the adhesive capacity, the name “sealant” was reconsidered and it has recently been called “fibrin biopolymer”. In Figure 2, the evolution since the 1990s of the name fibrin glue is summarized.
Standardized for more than 20 years by Brazilian researchers, the heterologous fibrin biopolymer (HFB) is composed of natural products extracted from animals, without human-blood derivatives (Fig. 3). Therefore, it does not offer risk of transmission of infectious diseases, in addition to possessing low production costs, abundant raw material and possibility of custom formulation to the procedure type [99. Ferreira RS Jr, de Barros LC, Abbade LPF, Barraviera SRCS, Silvares MRC, de Pontes LG, et al. Heterologous fibrin sealant derived from snake venom: From bench to bedside - an overview. J Venom Anim Toxins Incl Trop Dis. 2017 Apr 4; 23 (1):1-12. doi:10.1186/s40409-017-0109-8.
https://doi.org/10.1186/s40409-017-0109-...
,1111. Barros LC, Ferreira RS Jr, Barraviera SRCS, Stolf HO, Thomazini-Santos IA, Mendes-Giannini MJS. A new fibrin sealant from crotalus durissus terrificus venom: applications in medicine. J Toxicol Environ. 2009 Dec 2;12(8):553-71.]. The economic impact of this HFB is due to the reduction of surgical time with similar performance or even better when compared to traditional sutures [66. Thomazini-Santos IA, Barraviera SRCS, Mendes-Giannini MJS, Barraviera B. Surgical adhesives. J Venom Anim Toxins. 2001 Dec;7(2):159-71. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000200002.
http://www.scielo.br/scielo.php?script=s...
,1111. Barros LC, Ferreira RS Jr, Barraviera SRCS, Stolf HO, Thomazini-Santos IA, Mendes-Giannini MJS. A new fibrin sealant from crotalus durissus terrificus venom: applications in medicine. J Toxicol Environ. 2009 Dec 2;12(8):553-71.]. Thus, this systematic review aimed to gather, analyze and evaluate the available evidence on the use of HFB in the period of 30 years in in vivo experimental studies. At the end of this, it was verified by the selected studies in worldwide literature research its effectiveness in different clinical applications.
The heterologous fibrin sealant (HFS) produced by CEVAP. (A) Fractions, (B) stable clot formed after mixture of the components.
The experimental studies regarding this bioproduct began in 1995 by Juan et al. [2525. Juan FC, Thomazini IA, Gianini MJM, Viterbo F, Toscano E, Moraes RA, et al. Reparation of peripheral nerves with fibrin glue prepared from snake venom. Preliminary results. Sao Paulo Med J. 1995 Sep-Oct;113(5):1000-2.], as previously mentioned, and are being continued to date. Experiments were performed on different organs and animals such as rats, rabbits, dogs, sheep and horses. In this pioneer study, the fibrin sealant was applied in the sciatic nerve of rats, and showed similar efficacy to conventional glue. Also in an animal model, this sealant allowed the coaptation of intestinal segments and proved efficient in obtaining the anastomosis of the colon of rats [4141. Leite CVS, Naresse LE, Arantes HL, et al. An evaluation by rat colon anastomosis of the efficacy of fibrin glue derived from snake venom. J Venom Anim Toxins. 2000;6(2):180-93. http://www.scielo.br/scielo.php?pid=S0104-79302000000200004&script=sci_abstract.
http://www.scielo.br/scielo.php?pid=S010...
]. However, its use in anastomosis requires additional studies in larger animals to allow analysis in larger organs.
In 1998, Sartori Filho et al. [4040. Sartori Filho R, Prestes NC, Thomazini IA, Mendes-Giannini MJ, Toscano E, Canavessi AMO, et al. Use of fibrin glue derived from snake venom in testicular biopsy of rams. J Venom Anim Toxins. 1998;4(1):23-35. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301998000100003.
http://www.scielo.br/scielo.php?script=s...
] studied its adhesive properties in ovine, using the fibrin sealant and observing their effects on testicular biopsy. The sealant was easily applied, presenting faster repair properties. Its efficacy in hemorrhage control was important to prevent bruising that causes adhesion formation. The advantage over the traditional method (needles and suture lines, for example) was also highlighted, since these was no longer needed.
Chalhoub et al. [4242. Chalhoub M, Prestes NC, Lopes MD, Rocha NS, Thomazini-Santos IA, Mendes-Giannini MJ. The use of snake venom derived fibrin glue in hysterorrhaphy of ovine caesarean surgery. J Venom Anim Toxins. 2000;6(2):220-37. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302000000200007.
http://www.scielo.br/scielo.php?script=s...
] performed hysterorrhaphy after cesarean sections of sheep. The mortality rate of the animals was 12.5% , which was considered high. As expected, all the operated animals maintained the placenta, which compromised the healing process, having a strong influence on the results of animals in which the sealant was used. Therefore, further studies using this biomaterial on hysterorrhaphy after cesarean section in different animal species are required.
A third study in ovine was carried out. This time, the implantation of the sealant in chondral defects of cartilage was analyzed [5151. de Barros CN, Miluzzi Yamada AL, Junior RSF, Barraviera B, Hussni CA, de Souza JB, et al. A new heterologous fibrin sealant as a scaffold to cartilage repair-Experimental study and preliminary results. Exp Biol Med. 2016 Jul;241(13):1410-5.]. The applicability of the biomaterial was excellent, showed stability and did not trigger undesirable effects such as inflammation, allowing a normal repair process.
In dog models, Moraes et al. [4444. Moraes JRE, Correia PHA, Camplesi AC, Moraes FR. Experimental use of fibrin glue derived from snake venom in non-pregnant canine uterus. J Venom Anim Toxins incl Trop Dis. 2004;10(2):133-43. http://www.scielo.br/scielo.php?pid=S1678-91992004000200003&script=sci_abstract.
http://www.scielo.br/scielo.php?pid=S167...
] assessed the healing process in canine uterus hysterorrhaphy. The results indicate that fibrin sealant may have contributed to moderating the exudative phase, facilitating fibroplasia. In addition, the presence of fibrin in the sealant helps in the formation of a connective base, where the cells can proliferate and form a scar. A complementary study by the same team validated, through biomechanical tests, higher stiffness of the tissue treated with this sealant [6363. Moraes JRE, Camplesi AC, Correia PHA, Shimano AC, Ferraro GC, Moraes FR. Snake venom derived fibrin adhesive in dog uterine healing. Biomechanical study. J Venom Anim Toxins incl Trop Dis. 2005 Apr-Jun;11(2):129-42. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000200005.
http://www.scielo.br/scielo.php?script=s...
].
Moreover, the study by Rahal et al. [4343. Rahal SC, Amaral MSP, Pai VD, Barraviera SRCS, Caporal EH., Crocci AJ. Effect of fibrin glue derived from snake venom on the viability of autogenous split-thickness skin graft. J Venom Anim Toxins incl Trop Dis. 2004;10(2):161-72. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992004000200006.
http://www.scielo.br/scielo.php?script=s...
] sought to analyze the effect of the fibrin sealant derived from snake venom on skin grafts in dogs. The graft adhered to the fibrin sealant showed histological characteristics similar to the sutured graft, but tissue repair of the former was more pronounced, besides having more cells and a greater number of collagen fibers in the papillary layer of the dermis. Its use also had an important effect in reducing the time of surgery, since it minimized the use of suture materials, which is an advantage especially for patients with high surgical risk.
Ferraro et al. [4545. Ferraro G, Moraes JRE, Pereira G, Moraes FR, Bueno de Camargo MH. Clinical and morphological evaluation of snake venom derived fibrin glue on the tendon healing in dogs. J Venom Anim Toxins incl Trop Dis. 2005;11(4):433-46.,6464. Ferraro GC, Moraes JR, Shimano AC, Pereira GT, Moraes FR, Bueno de Camargo MH. Effect of snake venom derived fibrin glue on the tendon healing in dogs. Clinical and biomechanical study. J Venom Anim Toxins incl Trop Dis. 2005 Jul-Sep;11(3):261-74. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000300005.
http://www.scielo.br/scielo.php?script=s...
], evaluated the healing strength of the tendon of the thoracic limbs of dogs and their clinical evolution, using fibrin sealant as a substitute for tenorrhaphy. The assessment of four biomechanical properties (resilience, rigidity, maximum limit and stability limit) allowed observing that tendon healing achieved progressive resistance with maximum tensile strength time. Thus, fibrin sealant derived from snake venom obtained positive results, promoting healing in the flexor tendon of dogs [6464. Ferraro GC, Moraes JR, Shimano AC, Pereira GT, Moraes FR, Bueno de Camargo MH. Effect of snake venom derived fibrin glue on the tendon healing in dogs. Clinical and biomechanical study. J Venom Anim Toxins incl Trop Dis. 2005 Jul-Sep;11(3):261-74. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000300005.
http://www.scielo.br/scielo.php?script=s...
].
Sampaio et al. [4646. Sampaio RL , Ranzani JJT, Brandão CVS, Thomazini- Santos I A, Barraviera B, Barraviera SRCS. Use of fibrin glue derived from snake venom in the repair of deep corneal ulcers - experimental study in dogs (Canis familiaris, Linnaeus, 1758). J Venom Anim Toxins incl Trop Dis. 2007;13(4):857-73. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992007000400014.
http://www.scielo.br/scielo.php?script=s...
], proposed a model to repair corneal ulcers in dogs. Although fibrinolysis occurred within the first 48 hours, the healing of the eyes treated with fibrin sealant did not present complications. The sealant helped in the local repair, being evident the ease of application and the low cost.
In the assessment of peripheral nerve recovery, rat models were adopted and fibrin sealant was used for the reimplantation of dorsal spinal roots [4949. Benitez SU, Barbizan R, Spejo A, Ferreira Jr RS. Synaptic plasticity and sensory-motor improvement following fibrin sealant dorsal root reimplantation and mononuclear cell therapy. Front Neuroanat. 2014 Sep 8:1-16.] and ventral [3232. Barbizan R, Castro M., Barraviera B, Ferreira RS Jr, Oliveira ALR. Influence of delivery method on neuroprotection by bone marrow mononuclear cell therapy following ventral root reimplantation with fibrin sealant. PLoS One. 2014 Aug 26;9(8):1-13.,5454. Vidigal de Castro M, Barbizan R, Ferreira RS Jr, Barraviera B, de Oliveira ALR. Direct spinal ventral root repair following avulsion: effectiveness of a new heterologous fibrin sealant on motoneuron survival and regeneration. Neural Plast. 2016;2016:2932784.,5858. Araújo MR, Kyrylenko S, Spejo AB, Castro MV, Ferreira Junior RS, Barraviera B, et al. Transgenic human embryonic stem cells overexpressing FGF2 stimulate neuroprotection following spinal cord ventral root avulsion. Exp Neurol. 2017 Aug;294:45-57.,6161. Spejo AB, Chiarotto GB, Ferreira ADF, Gomes DA, Ferreira RS Jr, Barraviera B, et al. Neuroprotection and immunomodulation following intraspinal axotomy of motoneurons by treatment with adult mesenchymal stem cells. J Neuroinflammation. 2018 Aug 14;15(1):230.,6565. Barbizan R, Vidigal M., Ferreira Junior RS, Barraviera B, Oliveira ALR. Long-term spinal ventral root reimplantation, but not bone marrow mononuclear cell treatment, positively influences ultrastructural synapse recovery and motor axonal regrowth. Int J Mol Sci. 2014 Nov;15(11):19535-51.] after its avulsion, contributing in the process of regeneration. Benitez et al. [4949. Benitez SU, Barbizan R, Spejo A, Ferreira Jr RS. Synaptic plasticity and sensory-motor improvement following fibrin sealant dorsal root reimplantation and mononuclear cell therapy. Front Neuroanat. 2014 Sep 8:1-16.] and Barbizan et al. [3232. Barbizan R, Castro M., Barraviera B, Ferreira RS Jr, Oliveira ALR. Influence of delivery method on neuroprotection by bone marrow mononuclear cell therapy following ventral root reimplantation with fibrin sealant. PLoS One. 2014 Aug 26;9(8):1-13.,4848. Barbizan R, Castro MV, Rodrigues AC, Barraviera B, Ferreira RS, Oliveira ALR. Motor recovery and synaptic preservation after ventral root avulsion and repair with a fibrin sealant derived from snake venom. PLoS One. 2013 May 7;8(5):e63260.] also used bone marrow mononuclear cells associated with and homogenized to the fibrin sealant, respectively, which provided more lasting results for neuroprotection, significantly improving motor function. In addition, Cartarozzi et al. [5050. Cartarozzi LP, Spejo AB, Ferreira RS Jr, Barraviera B, Duek E, Carvalho JL, et al. Mesenchymal stem cells engrafted in a fibrin scaffold stimulate Schwann cell reactivity and axonal regeneration following sciatic nerve tubulization. Brain Res Bull. 2015 Mar;112:14-24.] found that the application of the association of mesenchymal stem cells and sealant improved the axonal regeneration and reactivity of Schwann cells.
Moreover, Vidigal de Castro et al. [5454. Vidigal de Castro M, Barbizan R, Ferreira RS Jr, Barraviera B, de Oliveira ALR. Direct spinal ventral root repair following avulsion: effectiveness of a new heterologous fibrin sealant on motoneuron survival and regeneration. Neural Plast. 2016;2016:2932784.] compared the treatment of axonal injury between two sealants: one composed of animal blood and snake venom (CEVAP), and another derived of human blood (fibrin sealant homologue). Both sealants were equally efficient, but the heterologous was highlighted as a safer alternative, being a biological and biodegradable product, and without human blood derivatives.
Biscola et al. [5353. Biscola NP, Politti Cartarozzi L, Ferreira Junior RS, Barraviera B, Leite Rodrigues de Oliveira A. Long-standing motor and sensory recovery following acute fibrin sealant based neonatal sciatic nerve repair. Neural Plast. 2016;2016:9028126.] also compared these two sealants, with the objective of evaluating the end-to-end coaptation of the sciatic nerve in newborn rats. The results were favorable for both sealants, promoting neuroprotection and regeneration of motor and sensory axons. However, the CEVAP fibrin sealant presented greater ease in manipulation at the time of surgery. This corroborates the study by Mozafari et al. [6060. Mozafari R, Kyrylenko S, Castro MV, Ferreira RS, Barraviera B, Oliveira ALR. Combination of heterologous fibrin sealant and bioengineered human embryonic stem cells to improve regeneration following autogenous sciatic nerve grafting repair. J Venom Anim Toxins incl Trop Dis. 2018 Apr 12;24:11. doi:10.1186/s40409-018-0147-x.
https://doi.org/10.1186/s40409-018-0147-...
], in which the fibrin sealant facilitated the repair of the sciatic nerve, allowing adhesion and nerve regeneration.
Two studies [5252. Buchaim DV, Rodrigues A de C, Buchaim RL. The new heterologous fibrin sealant in combination with low-level laser therapy (LLLT) in the repair of the buccal branch of the facial nerve. Lasers Med Sci. 2016;31(5):965-72.,5656. Rosso MPO, Rosa Júnior GM, Buchaim DV, German IJS, Pomini KT, de Souza RG, et al. Stimulation of morphofunctional repair of the facial nerve with photobiomodulation, using the end-to-side technique or a new heterologous fibrin sealant. J Photochem Photobiol B. 2017 Oct;175:20-8.] evaluated the use of fibrin sealant in the repair of facial nerve lesions with the addition of photobiomodulation therapy. The sealant allowed less manipulation of the nerve stumps compared to the suture, and when combined with the low-level laser, showed better morphofunctional results and nerve regeneration. Buchaim et al. [3333. Buchaim RL, Andreo JC, Barraviera B, Ferreira Jr RS, Buchaim DV, Rosa Jr GM, et al. Effect of low-level laser therapy (LLLT) on peripheral nerve regeneration using fibrin glue derived from snake venom. Injury. 2015 Apr;46(4):655-60.] demonstrated that the fibrin sealant was viable for nerve repair. When associated with laser therapy, the sealant showed an even more satisfactory result.
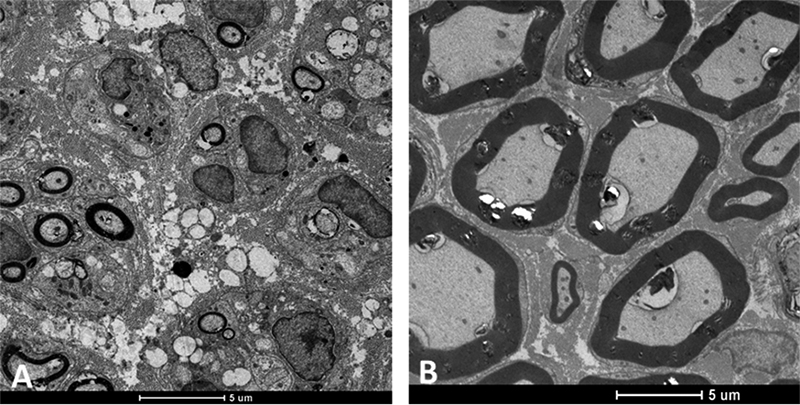
In the study by Buchaim et al. [5757. Buchaim DV, Andreo JC, Ferreira Junior RS, Barraviera B, Rodrigues AC, Macedo MC, et al. Efficacy of laser photobiomodulation on morphological and functional repair of the facial nerve. Photomed Laser Surg. 2017 Aug;35(8):442-9.], concerning qualitative, quantitative and functional aspects in the facial nerve regeneration process, the results showed that LLLT increased axonal regeneration and accelerated the functional recovery of vibrissae. Thus, both the suture and the fibrin sealant allowed the growth of axons, and the latter presented good manipulation properties, in addition to the shorter surgery time for nerve repair (Fig. 4).
Distal stump fibers of the facial nerve of rats regenerating after end-to-end neurorrhaphy by fibrin biopolymer coaptation. Transmission electronic microscopy: (A) 5 weeks post-coaptation and (B) 10 weeks post-coaptation.
The most recent study on nerve reconstruction by Leite et al. [6666. Leite APS, Pinto CG, Tibúrcio FC, Sartori AA, de Castro Rodrigues A, Barraviera B, et al. Heterologous fibrin sealant potentiates axonal regeneration after peripheral nerve injury with reduction in the number of suture points. Injury. 2019 Apr;50(4):834-47.] validated the use of the fibrin sealant as improvement to suture in sciatic repair, where a protective effect at the lesion site due to the use of HFS was observed.
In the studies that sought to evaluate the ability of the sealant in relation to bone repair in rats [3434. Cunha MR, Menezes FA, Santos GR, Pinto CAL, Barraviera B, Martins VCAM, et al. Hydroxyapatite and a new fibrin sealant derived from snake venom as scaffold to treatment of cranial defects in rats. Mat Res. 2015 Jan-Feb;18(1):196-203.-3636. de Oliveira Gonçalves JB, Buchaim DV, de Souza Bueno CR, Pomini KT, Barraviera B, Júnior RSF, et al. Effects of low-level laser therapy on autogenous bone graft stabilized with a new heterologous fibrin sealant. J Photochem Photobiol B. 2016 Sep;162:663-8.,4747. Iatecola A, Barraviera B, Ferreira RS Jr, dos Santos GR, Neves JI, da Cunha MR. Use of a new fibrin sealant and laser irradiation in the repair of skull defects in rats. Braz Dent J. 2013 Sep-Oct;24(5):456-61.], the osteogenic potential was highlighted. When combined with low-level laser therapy [3636. de Oliveira Gonçalves JB, Buchaim DV, de Souza Bueno CR, Pomini KT, Barraviera B, Júnior RSF, et al. Effects of low-level laser therapy on autogenous bone graft stabilized with a new heterologous fibrin sealant. J Photochem Photobiol B. 2016 Sep;162:663-8.,4747. Iatecola A, Barraviera B, Ferreira RS Jr, dos Santos GR, Neves JI, da Cunha MR. Use of a new fibrin sealant and laser irradiation in the repair of skull defects in rats. Braz Dent J. 2013 Sep-Oct;24(5):456-61.], or with other biomaterials such as hydroxyapatite [3434. Cunha MR, Menezes FA, Santos GR, Pinto CAL, Barraviera B, Martins VCAM, et al. Hydroxyapatite and a new fibrin sealant derived from snake venom as scaffold to treatment of cranial defects in rats. Mat Res. 2015 Jan-Feb;18(1):196-203.] and rhBMP-2 [3535. Machado EG, Issa JPM, Figueiredo FA, Santos GR, Galdeano EA, Alves MC, et al. A new heterologous fibrin sealant as scaffold to recombinant human bone morphogenetic protein-2 (rhBMP-2) and natural latex proteins for the repair of tibial bone defects. Acta Histochem. 2015 Apr;117(3):288-96.], the regeneration process was accelerated, proving the biocompatibility of the sealant with this tissue (Fig. 5).
Critical-size defects in rat calvarial bones: (A) bioadhesion of the fibrin biopolymer at the edges of the surgical bone cavity; (B) osteotomy in the center of the parietal bones and agglutination of the bone graft particles by the fibrin biopolymer before deposition; (C and D) deposition of the fibrin biopolymer mixture with different bone grafts in the surgical cavity.
In order to evaluate the osteogenic potential of the natural rubber membranes of highly bioactive clones of Hevea brasiliensis (RRIM 600 and IAN 873) and Hancornia speciosa, Floriano et al. [55] used fibrin sealant to correct membranes in bone defects in rabbit calvaria, replacing cyanoacrylate. The sealant proved to be efficient for this type of application, in which the membranes showed good adhesion to the bone surface, and there were no negative responses in the regions where the sealant was applied.
Gasparotto et al. [6262. Gasparotto VPO, Landim-Alvarenga FC, Oliveira ALR, Simões GF, Lima-Neto JF, Barraviera B, et al. A new fibrin sealant as a three-dimensional scaffold candidate for mesenchymal stem cells. Stem Cell Res Ther. 2014 Jun 10;5(3):78.] suggested for the first time the use of the new fibrin sealant in vitro as a scaffold for mesenchymal stem cells, being able to maintain cell survival without interfering with differentiation. In addition to the known advantages of its low cost of production and non-transmission of infectious diseases, Orsi et al. [5959. Orsi PR, Landim-Alvarenga FC, Justulin LA, Kaneno R, de Assis Golilm M, dos Santos DC, et al. A unique heterologous fibrin sealant (HFS) as a candidate biological scaffold for mesenchymal stem cells in osteoporotic rats. Stem Cell Res Ther. 2017 Sep 29;8(1):1-14.] evaluated for the first time the performance of the sealant as an in vivo scaffold for the transplantation of mesenchymal stem cells in the repair of critical defects of the femur in osteoporotic rats. In that present study, histological analysis revealed that at 14 days after surgery, the animals treated with HFS + MSCs and HFS + MSCs D showed a higher formation of bone cells at the lesion site than the control, suggesting that the sealant served as scaffold. Microscopy electron transmission (MET) analysis showed that fibrin sealant was non-toxic to cells, since the nucleus and cell morphology were very similar to the control group. Therefore, mesenchymal stem cells were proven to promote bone repair when associated with a biological scaffold, showing for the first time non-toxicity to cells. Recently, Cassaro et al. [6767. Cassaro CV, Justulin Junior LA, de Lima PR, Golim MA, Biscola NP, de Castro MV, et al. Fibrin biopolymer as scaffold candidate to treat bone defects in rats. J Venom Anim Toxins incl Trop Dis. 2019;25:e20190027. http://dx.doi.org/10.1590/1678-9199-JVATITD-2019-0027.
http://dx.doi.org/10.1590/1678-9199-JVAT...
] validated the osteogienic potencial of HFS+MSCs on repair of bone defect in femur of rats.
When fibrin is formed after the addition of the cryoprecipitate rich in fibrinogen extracted from buffalo blood, the fibers are randomly formed with spaces between them of different diameters. Figure 6 shows the electron microscopy of the heterologous fibrin sealant at different magnifications and a captured mesenchymal stem cell.
Electron microscopy of the heterologous fibrin sealant at different magnifications. (A) 500x; (B) 2000x; (C) 7000x and (D) 7000x with a captured mesenchymal stem cell.
In addition to the application in animal models, clinical trials with the HFB started in 1999 carried out by Stolf [2828. Stolf HO. The use of fibrin adhesive derived from snake venom and the evaluation of skin grafting using skin from the patient’s nasolabial fold. J Venom Anim Toxins. 1999;5(2):227. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301999000200011.
http://www.scielo.br/scielo.php?script=s...
]. The HFS was for the first time applied in humans as an alternative to conventional suture. Twenty-one Caucasian patients with basal cell carcinoma tumor in the nasolabial region received the product. Skin grafting of the right nasolabial fold was made using HFS, while the left nasolabial fold was sutured. The comparative study of both areas in the same patient showed erythema and edemas on the sutured areas, while dehiscence and serum-hemorrhagic exudation were seen on the glued areas 48 hours after surgery. The cosmetic evaluation of the scar formation was excellent for the glued area and good for the sutured area. The patients did not show any local or systemic adverse events, which makes the new product a valuable alternative method for skin surgery.
In 2007, Barbosa et al. [2929. Barbosa MDS, Gregh SLA, Passanezi E. Fibrin adhesive derived from snake venom in periodontal surgery. J Periodontol. 2007 Oct;78(10):2026-31.] used HFS in the dental area for the first time. They studied 15 non-smoking patients who needed bilateral gingival grafts around the bicuspid mandibular area. They concluded that the HFS is an alternative to the traditional fibrin adhesive and may represent an alternative to sutures in periodontal surgery [2929. Barbosa MDS, Gregh SLA, Passanezi E. Fibrin adhesive derived from snake venom in periodontal surgery. J Periodontol. 2007 Oct;78(10):2026-31.,3030. Barbosa MDS, Stipp AC, Passanezi E, Greghi SLA. Fibrin adhesive derived from snake venom in periodontal surgery. Histological analysis. J Appl Oral Sci. 2008 Sep-Oct;16(5):310-5.]. In addition, Chiquito et al. [88. Chiquito GCM. Comparison between suture and fibrin adhesive derived from snake venom for fixation of connective tissue graft in correction of marginal tissue recession. J Venom Anim Toxins incl Trop Dis. 2007;13(2):559.] compared HFS and conventional suture on gingival defects and considered the first as efficient as the traditional treatment.
Gatti et al. [3737. Gatti MAN. Treatment of venous ulcers with surgical adhesives derived from snake venom. J Venom Anim Toxins incl Trop Dis. 2009:15(2). http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992009000200020.
http://www.scielo.br/scielo.php?script=s...
,3838. Gatti MAN, Vieira LM, Barraviera B, Barraviera SRCS. Treatment of venous ulcers with fibrin sealant derived from snake venom. J Venom Anim Toxins incl Trop Dis. 2011;17(2):226-9. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000200015.
http://www.scielo.br/scielo.php?script=s...
] used the HFB for the first time to treat chronic venous ulcers assessing its effects on the repair process. They concluded that the application of fibrin sealant may contribute to the wound healing process. Control trials phase I/II will be necessary to evaluate the best way to apply the HFB. In 2015, Abbade et al. [3939. Abbade LPF. A new fibrin sealant derived from snake venom candidate to treat chronic venous ulcers. J Am Acad Dermatol. 2015 May;72(5):AB271.] used the HFB, previously standardized by Ferreira Jr et al. [99. Ferreira RS Jr, de Barros LC, Abbade LPF, Barraviera SRCS, Silvares MRC, de Pontes LG, et al. Heterologous fibrin sealant derived from snake venom: From bench to bedside - an overview. J Venom Anim Toxins Incl Trop Dis. 2017 Apr 4; 23 (1):1-12. doi:10.1186/s40409-017-0109-8.
https://doi.org/10.1186/s40409-017-0109-...
], in a clinical trial phase I/II treating 31 patients. They concluded that HFB was safe for the treatment of chronic venous ulcers according to the proposed dosages. Multicenter clinical trial phase III will be required to establish the definitely efficacy of the product.
Clinical trials conducted so far show that HFB is a versatile, easy to apply, low-cost preparation, which reduces pain, does not transmit infectious diseases by human blood, and does not present adverse events. Therefore, at this moment the CEVAP team is looking for opportunities and financial support to start the clinical trials phase III and registration by the Brazilian Health Regulatory Agency.
CONCLUSION
In conclusion, the studies on different tissue types showed that the fibrin biopolymer is a promising material that achieved the proposed objectives due to the ease of application (reduces surgical time), regenerative properties and biocompatibility with other materials. It is also a safer alternative, since it is a biological and biodegradable product, without human blood derivatives.
As previously mentioned, due to the properties demonstrated in studies that used the heterologous sealant produced by CEVAP, the current denomination was modified to fibrin biopolymer in accordance with other sealants and the literature. In addition to the satisfactory results presented in this review, several studies continue to be conducted to a greater understanding of its performance in different tissues and potential of clinical use.
Abbreviations
ANVISA: Brazilian Health Regulatory Agency; HFB: heterologous fibrin biopolymer; HFS: heterologous fibrin sealant; MET: microscopy electron transmission.
Acknowledgments
The authors would like to thank the Center for the Study of Venoms and Venomous Animals (CEVAP) of São Paulo State University (UNESP) and its researchers for helping on the development of this manuscript.
References
- 1. Spotnitz WD. Fibrin sealant: Past, present, and future: a brief review. World J Surg. 2010 Apr;34(4):632-4.
- 2. Bergel S. Ueber Wirkungen des Fibrins. Dtsch med Wochenschr. 1909;35(15):663-5.
- 3. Sameem M, Wood TJ, Bain JR. A systematic review on the use of fibrin glue for peripheral nerve repair. Plast Reconstr Surg. 2011 Jun;127(6):2381-90.
- 4. Young JZ, Medawar PB. Fibrin suture of peripheral nerves. Measurement of the rate of regeneration. Lancet. 1940 Aug 3; 236 (6101):126-8.
- 5. Cronkite EP, Lozner EL, Deaver JM. Use of thrombin and fibrinogen in skin grafting. JAMA. 1944;124(14):976-8.
- 6. Thomazini-Santos IA, Barraviera SRCS, Mendes-Giannini MJS, Barraviera B. Surgical adhesives. J Venom Anim Toxins. 2001 Dec;7(2):159-71. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000200002
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000200002 - 7. Spotnitz WD. Clinical Uses of Fibrin Sealant in Transfusion Therapy: Clinical Principles and Practice. 1st ed. (Press A, ed. ); 1999.
- 8. Chiquito GCM. Comparison between suture and fibrin adhesive derived from snake venom for fixation of connective tissue graft in correction of marginal tissue recession. J Venom Anim Toxins incl Trop Dis. 2007;13(2):559.
- 9. Ferreira RS Jr, de Barros LC, Abbade LPF, Barraviera SRCS, Silvares MRC, de Pontes LG, et al. Heterologous fibrin sealant derived from snake venom: From bench to bedside - an overview. J Venom Anim Toxins Incl Trop Dis. 2017 Apr 4; 23 (1):1-12. doi:10.1186/s40409-017-0109-8.
» https://doi.org/10.1186/s40409-017-0109-8 - 10. Matras H. Fibrin seal: The state of the art. J Oral Maxillofac Surg. 1985;43(8):605-11.
- 11. Barros LC, Ferreira RS Jr, Barraviera SRCS, Stolf HO, Thomazini-Santos IA, Mendes-Giannini MJS. A new fibrin sealant from crotalus durissus terrificus venom: applications in medicine. J Toxicol Environ. 2009 Dec 2;12(8):553-71.
- 12. Ferreira Jr RS. Autologous or heterologous fibrin sealant scaffold: which is the better choice? J Venom Anim Toxins incl Trop Dis. 2014 Jul18;20:31. doi:10.1186/1678-9199-20-31.
» https://doi.org/10.1186/1678-9199-20-31 - 13. Pomini KT, Buchaim DV, Andreo JC, Rosso MPO, Colleta BBD, German IJS, et al. Fibrin sealant derived from human plasma as a scaffold for bone grafts associated with photobiomodulation therapy. Int J Mol Sci. 2019 Apr;20(7):1761.
- 14. Eder G, Neumann M, Cerwenka R, Baumgarten K. Preliminary Results of a Randomized Controlled Study on the Risk of Hepatitis Transmission of a Two-Component Fibrin Sealant (Tissucol/Tisseel). In: Schlag G, Redl H, eds. Fibrin Sealant in Operative Medicine. Berlin, Heidelberg: Springer Berlin Heidelberg; 1986.
- 15. Radosevich M, Goubran HA, Burnouf T. Fibrin sealant : scientific rationale, production methods, properties, and current clinical use. Vox Sang. 1997 Jan;72(3):133-43.
- 16. Kawamura M, Sawafuji M, Watanabe M, Horinouchi H, Kobayashi K. Frequency of transmission of human parvovirus B19 infection by fibrin sealant used during thoracic surgery. Ann Thorac Surg. 2002 Apr;73(4):1098-100.
- 17. Ferreira ASSBS, Barraviera B, Barraviera SRCS, Abbade LPF, Caramori CA, Ferreira RS Jr. A success in Toxinology translational research in Brazil: Bridging the gap. Toxicon. 2013 Jul;69:50-4.
- 18. de Pontes LG, Cavassan NRV, de Barros LC, Ferreira Junior RS, Barraviera B, dos Santos LD. Plasma proteome of buffaloes. Proteomics Clin Appl. 2017 Sep;11(9-10).
- 19. Ferreira Junior RS, da Silva DAF, Biscola NP, Sartori MMP, Denadai JP, Jorge AM, et al. Traceability of animal protein byproducts in ruminants by multivariate analysis of isotope ratio mass spectrometry to prevent transmission of prion diseases. J Venon Anim Toxins incl Trop Dis. 2019 May 13;25. doi.org/10.1590/1678-9199-jvatitd-1487-18.
» https://doi.org/10.1590/1678-9199-jvatitd-1487-18 - 20. Barros LC, Soares AM, Costa FL, Rodrigues VM, Fuly AL, Giglio JR, et al. Biochemical and biological evaluation of gyroxin isolated from Crotalus durissus terrificus venom. J Venom Anim Toxins incl Trop Dis. 2011;17(1):23-33. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000100004
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000100004 - 21. Braud S, Bon C, Wisner A. Snake venom proteins acting on hemostasis. Biochimie. 2000 Sep-Oct;82(9-10):851-9.
- 22. Pirkle H. Thrombin-like enzymes from snake venoms: an updated inventory. Thrombosis and Haemostasis. Scientific and Standardization Committee's Registry of Exogenous Hemostatic Factors. 1998 Mar;79(3):675-83.
- 23. Le Guéhennec L, Layrolle P, Daculsi G. A review of bioceramics and fibrin sealant. Eur Cell Mater. 2004 Sep 13;8:1-10.
- 24. Palacio TZ, Santos-Filho NA, Rosa JC, Ferreira Jr RS, Barraviera B, Sampaio SV. Isolation and characterization of a novel metalloprotease inhibitor from Bothrops alternatus snake serum. Int J Biol Macromol. 2017 May;98:436-46.
- 25. Juan FC, Thomazini IA, Gianini MJM, Viterbo F, Toscano E, Moraes RA, et al. Reparation of peripheral nerves with fibrin glue prepared from snake venom. Preliminary results. Sao Paulo Med J. 1995 Sep-Oct;113(5):1000-2.
- 26. Thomazini-Santos IA, Giannini MJSM, Toscano E, Machado PEA, Lima CRG, Barraviera B. The evaluation of clotting time in bovine thrombin, Reptilase ® , and thrombin-like fraction of Crotalus durissus terrificus venom using bovine, equine, ovine, bubaline and human cryoprecipitates. J Venom Anim Toxins. 1998;4(2):120-36. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301998000200004
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301998000200004 - 27. Thomazini-Santos IA. Fibrin adhesive from snake venom: the effect of adding e-aminocaproic acid, tranexamic acid and aprotinin for coaptation of wound in rat skin incisions. J Venom Anim Toxins. 2001;7(1):148-9. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000100011
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302001000100011 - 28. Stolf HO. The use of fibrin adhesive derived from snake venom and the evaluation of skin grafting using skin from the patient’s nasolabial fold. J Venom Anim Toxins. 1999;5(2):227. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301999000200011
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301999000200011 - 29. Barbosa MDS, Gregh SLA, Passanezi E. Fibrin adhesive derived from snake venom in periodontal surgery. J Periodontol. 2007 Oct;78(10):2026-31.
- 30. Barbosa MDS, Stipp AC, Passanezi E, Greghi SLA. Fibrin adhesive derived from snake venom in periodontal surgery. Histological analysis. J Appl Oral Sci. 2008 Sep-Oct;16(5):310-5.
- 31. Biscola NP, Cartarozzi LP, Ulian-Benitez S, Barbizan R, Castro MV, Spejo AB, et al. Multiple uses of fibrin sealant for nervous system treatment following injury and disease. J Venom Anim Toxins incl Trop Dis. 2017 Mar 14;23:13. doi:10.1186/s40409-017-0103-1.
» https://doi.org/10.1186/s40409-017-0103-1 - 32. Barbizan R, Castro M., Barraviera B, Ferreira RS Jr, Oliveira ALR. Influence of delivery method on neuroprotection by bone marrow mononuclear cell therapy following ventral root reimplantation with fibrin sealant. PLoS One. 2014 Aug 26;9(8):1-13.
- 33. Buchaim RL, Andreo JC, Barraviera B, Ferreira Jr RS, Buchaim DV, Rosa Jr GM, et al. Effect of low-level laser therapy (LLLT) on peripheral nerve regeneration using fibrin glue derived from snake venom. Injury. 2015 Apr;46(4):655-60.
- 34. Cunha MR, Menezes FA, Santos GR, Pinto CAL, Barraviera B, Martins VCAM, et al. Hydroxyapatite and a new fibrin sealant derived from snake venom as scaffold to treatment of cranial defects in rats. Mat Res. 2015 Jan-Feb;18(1):196-203.
- 35. Machado EG, Issa JPM, Figueiredo FA, Santos GR, Galdeano EA, Alves MC, et al. A new heterologous fibrin sealant as scaffold to recombinant human bone morphogenetic protein-2 (rhBMP-2) and natural latex proteins for the repair of tibial bone defects. Acta Histochem. 2015 Apr;117(3):288-96.
- 36. de Oliveira Gonçalves JB, Buchaim DV, de Souza Bueno CR, Pomini KT, Barraviera B, Júnior RSF, et al. Effects of low-level laser therapy on autogenous bone graft stabilized with a new heterologous fibrin sealant. J Photochem Photobiol B. 2016 Sep;162:663-8.
- 37. Gatti MAN. Treatment of venous ulcers with surgical adhesives derived from snake venom. J Venom Anim Toxins incl Trop Dis. 2009:15(2). http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992009000200020
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992009000200020 - 38. Gatti MAN, Vieira LM, Barraviera B, Barraviera SRCS. Treatment of venous ulcers with fibrin sealant derived from snake venom. J Venom Anim Toxins incl Trop Dis. 2011;17(2):226-9. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000200015
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992011000200015 - 39. Abbade LPF. A new fibrin sealant derived from snake venom candidate to treat chronic venous ulcers. J Am Acad Dermatol. 2015 May;72(5):AB271.
- 40. Sartori Filho R, Prestes NC, Thomazini IA, Mendes-Giannini MJ, Toscano E, Canavessi AMO, et al. Use of fibrin glue derived from snake venom in testicular biopsy of rams. J Venom Anim Toxins. 1998;4(1):23-35. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301998000100003
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79301998000100003 - 41. Leite CVS, Naresse LE, Arantes HL, et al. An evaluation by rat colon anastomosis of the efficacy of fibrin glue derived from snake venom. J Venom Anim Toxins. 2000;6(2):180-93. http://www.scielo.br/scielo.php?pid=S0104-79302000000200004&script=sci_abstract
» http://www.scielo.br/scielo.php?pid=S0104-79302000000200004&script=sci_abstract - 42. Chalhoub M, Prestes NC, Lopes MD, Rocha NS, Thomazini-Santos IA, Mendes-Giannini MJ. The use of snake venom derived fibrin glue in hysterorrhaphy of ovine caesarean surgery. J Venom Anim Toxins. 2000;6(2):220-37. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302000000200007
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-79302000000200007 - 43. Rahal SC, Amaral MSP, Pai VD, Barraviera SRCS, Caporal EH., Crocci AJ. Effect of fibrin glue derived from snake venom on the viability of autogenous split-thickness skin graft. J Venom Anim Toxins incl Trop Dis. 2004;10(2):161-72. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992004000200006
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992004000200006 - 44. Moraes JRE, Correia PHA, Camplesi AC, Moraes FR. Experimental use of fibrin glue derived from snake venom in non-pregnant canine uterus. J Venom Anim Toxins incl Trop Dis. 2004;10(2):133-43. http://www.scielo.br/scielo.php?pid=S1678-91992004000200003&script=sci_abstract
» http://www.scielo.br/scielo.php?pid=S1678-91992004000200003&script=sci_abstract - 45. Ferraro G, Moraes JRE, Pereira G, Moraes FR, Bueno de Camargo MH. Clinical and morphological evaluation of snake venom derived fibrin glue on the tendon healing in dogs. J Venom Anim Toxins incl Trop Dis. 2005;11(4):433-46.
- 46. Sampaio RL , Ranzani JJT, Brandão CVS, Thomazini- Santos I A, Barraviera B, Barraviera SRCS. Use of fibrin glue derived from snake venom in the repair of deep corneal ulcers - experimental study in dogs (Canis familiaris, Linnaeus, 1758). J Venom Anim Toxins incl Trop Dis. 2007;13(4):857-73. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992007000400014
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992007000400014 - 47. Iatecola A, Barraviera B, Ferreira RS Jr, dos Santos GR, Neves JI, da Cunha MR. Use of a new fibrin sealant and laser irradiation in the repair of skull defects in rats. Braz Dent J. 2013 Sep-Oct;24(5):456-61.
- 48. Barbizan R, Castro MV, Rodrigues AC, Barraviera B, Ferreira RS, Oliveira ALR. Motor recovery and synaptic preservation after ventral root avulsion and repair with a fibrin sealant derived from snake venom. PLoS One. 2013 May 7;8(5):e63260.
- 49. Benitez SU, Barbizan R, Spejo A, Ferreira Jr RS. Synaptic plasticity and sensory-motor improvement following fibrin sealant dorsal root reimplantation and mononuclear cell therapy. Front Neuroanat. 2014 Sep 8:1-16.
- 50. Cartarozzi LP, Spejo AB, Ferreira RS Jr, Barraviera B, Duek E, Carvalho JL, et al. Mesenchymal stem cells engrafted in a fibrin scaffold stimulate Schwann cell reactivity and axonal regeneration following sciatic nerve tubulization. Brain Res Bull. 2015 Mar;112:14-24.
- 51. de Barros CN, Miluzzi Yamada AL, Junior RSF, Barraviera B, Hussni CA, de Souza JB, et al. A new heterologous fibrin sealant as a scaffold to cartilage repair-Experimental study and preliminary results. Exp Biol Med. 2016 Jul;241(13):1410-5.
- 52. Buchaim DV, Rodrigues A de C, Buchaim RL. The new heterologous fibrin sealant in combination with low-level laser therapy (LLLT) in the repair of the buccal branch of the facial nerve. Lasers Med Sci. 2016;31(5):965-72.
- 53. Biscola NP, Politti Cartarozzi L, Ferreira Junior RS, Barraviera B, Leite Rodrigues de Oliveira A. Long-standing motor and sensory recovery following acute fibrin sealant based neonatal sciatic nerve repair. Neural Plast. 2016;2016:9028126.
- 54. Vidigal de Castro M, Barbizan R, Ferreira RS Jr, Barraviera B, de Oliveira ALR. Direct spinal ventral root repair following avulsion: effectiveness of a new heterologous fibrin sealant on motoneuron survival and regeneration. Neural Plast. 2016;2016:2932784.
- 55. Floriano JF, Neto FC, da Mota LSLS, Furtado EL, Ferreira Jr, RS, Barraviera B, et al. Comparative study of bone tissue accelerated regeneration by latex membranes from Hevea brasiliensis and Hancornia speciosa Biomed Phys Eng Express. 2016 Jul 27;2(4):045007.
- 56. Rosso MPO, Rosa Júnior GM, Buchaim DV, German IJS, Pomini KT, de Souza RG, et al. Stimulation of morphofunctional repair of the facial nerve with photobiomodulation, using the end-to-side technique or a new heterologous fibrin sealant. J Photochem Photobiol B. 2017 Oct;175:20-8.
- 57. Buchaim DV, Andreo JC, Ferreira Junior RS, Barraviera B, Rodrigues AC, Macedo MC, et al. Efficacy of laser photobiomodulation on morphological and functional repair of the facial nerve. Photomed Laser Surg. 2017 Aug;35(8):442-9.
- 58. Araújo MR, Kyrylenko S, Spejo AB, Castro MV, Ferreira Junior RS, Barraviera B, et al. Transgenic human embryonic stem cells overexpressing FGF2 stimulate neuroprotection following spinal cord ventral root avulsion. Exp Neurol. 2017 Aug;294:45-57.
- 59. Orsi PR, Landim-Alvarenga FC, Justulin LA, Kaneno R, de Assis Golilm M, dos Santos DC, et al. A unique heterologous fibrin sealant (HFS) as a candidate biological scaffold for mesenchymal stem cells in osteoporotic rats. Stem Cell Res Ther. 2017 Sep 29;8(1):1-14.
- 60. Mozafari R, Kyrylenko S, Castro MV, Ferreira RS, Barraviera B, Oliveira ALR. Combination of heterologous fibrin sealant and bioengineered human embryonic stem cells to improve regeneration following autogenous sciatic nerve grafting repair. J Venom Anim Toxins incl Trop Dis. 2018 Apr 12;24:11. doi:10.1186/s40409-018-0147-x.
» https://doi.org/10.1186/s40409-018-0147-x - 61. Spejo AB, Chiarotto GB, Ferreira ADF, Gomes DA, Ferreira RS Jr, Barraviera B, et al. Neuroprotection and immunomodulation following intraspinal axotomy of motoneurons by treatment with adult mesenchymal stem cells. J Neuroinflammation. 2018 Aug 14;15(1):230.
- 62. Gasparotto VPO, Landim-Alvarenga FC, Oliveira ALR, Simões GF, Lima-Neto JF, Barraviera B, et al. A new fibrin sealant as a three-dimensional scaffold candidate for mesenchymal stem cells. Stem Cell Res Ther. 2014 Jun 10;5(3):78.
- 63. Moraes JRE, Camplesi AC, Correia PHA, Shimano AC, Ferraro GC, Moraes FR. Snake venom derived fibrin adhesive in dog uterine healing. Biomechanical study. J Venom Anim Toxins incl Trop Dis. 2005 Apr-Jun;11(2):129-42. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000200005
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000200005 - 64. Ferraro GC, Moraes JR, Shimano AC, Pereira GT, Moraes FR, Bueno de Camargo MH. Effect of snake venom derived fibrin glue on the tendon healing in dogs. Clinical and biomechanical study. J Venom Anim Toxins incl Trop Dis. 2005 Jul-Sep;11(3):261-74. http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000300005
» http://www.scielo.br/scielo.php?script=sci_arttext&pid=S1678-91992005000300005 - 65. Barbizan R, Vidigal M., Ferreira Junior RS, Barraviera B, Oliveira ALR. Long-term spinal ventral root reimplantation, but not bone marrow mononuclear cell treatment, positively influences ultrastructural synapse recovery and motor axonal regrowth. Int J Mol Sci. 2014 Nov;15(11):19535-51.
- 66. Leite APS, Pinto CG, Tibúrcio FC, Sartori AA, de Castro Rodrigues A, Barraviera B, et al. Heterologous fibrin sealant potentiates axonal regeneration after peripheral nerve injury with reduction in the number of suture points. Injury. 2019 Apr;50(4):834-47.
- 67. Cassaro CV, Justulin Junior LA, de Lima PR, Golim MA, Biscola NP, de Castro MV, et al. Fibrin biopolymer as scaffold candidate to treat bone defects in rats. J Venom Anim Toxins incl Trop Dis. 2019;25:e20190027. http://dx.doi.org/10.1590/1678-9199-JVATITD-2019-0027
» http://dx.doi.org/10.1590/1678-9199-JVATITD-2019-0027
-
Availability of data and material
All datasets generated or analyzed during this study are included in this published article. -
Funding
This publication was supported in part by the National Council for Scientific and Technological Development (CNPq) and Coordination for the Improvement of Higher Education Personnel (CAPES) through “Programa Editorial CNPq/CAPES” call n. 18/2018, grant n. 404770/2018-5. -
Ethics approval and consent to participate
Not applicable. -
Consent for publication
Not applicable.
Supplementary material
The following online material is available for this article:
Fibrin sealant or fibrin biopolymer: https://youtu.be/y6ho6M0amA8
Publication Dates
-
Publication in this collection
11 Nov 2019 -
Date of issue
2019
History
-
Received
21 June 2019 -
Accepted
16 Oct 2019