ABSTRACT
INTRODUCTION:
Knowledge of the different imaging tests and their appropriate indications is crucial to establish the diagnosis of temporomandibular disorders, especially in patients with overlapping signs and symptoms.
OBJECTIVE:
To present and assess the main diagnostic imaging tests for temporomandibular disorders and rationally discuss their indication criteria, advantages, and disadvantages.
METHODS:
Literature review in the Web of Knowledge, PubMed and SciELO databases, as well as manual search for relevant publications in reference lists of the selected articles.
RESULTS:
Computed tomography and magnetic resonance imaging were considered the gold standard assessments for the temporomandibular joint to evaluate hard and soft tissues, respectively. Each diagnostic method exhibited distinct sensitivity and specificity for the different subtypes of joint dysfunction.
CONCLUSION:
Selecting an evaluation examination based on its accuracy, safety, and clinical relevance is a rational decision that can help lead to an accurate diagnosis and an optimum treatment plan.
Keywords:
Temporomandibular joint disorders; Diagnostic imaging; Temporomandibular joint; Magnetic resonance imaging; X-ray computed tomography; Radiography
Resumo
Introdução:
O conhecimento dos distintos exames de imagem e sua correta indicação é fundamental para elaboração do diagnóstico das disfunções temporomandibulares, principalmente em pacientes com grande sobreposição de sinais e sintomas.
Objetivo:
Apresentar e avaliar os principais exames de diagnóstico por imagem das disfunções temporomandibulares, além de discutir racionalmente os seus critérios de indicação, vantagens e desvantagens.
Método:
Revisão da literatura nas bases de dados Web of Knowledge, PubMed e SciELO, além de busca manual por publicações relevantes nas listas de referências dos artigos selecionados.
Resultado:
Os exames de tomografia computadorizada e ressonância magnética foram considerados ''padrão-ouro'' para a avaliação dos tecidos duros e moles, respectivamente, da articulação temporomandibular. Cada método de diagnóstico pesquisado apresentou sensibilidade e especificidade distintas para os diferentes subtipos de disfunção da articulação.
Conclusão:
Considera-se como racional a indicação fundamentada na acurácia, segurança e relevância clínica do exame a ser solicitado, o que implica na adequada determinação do diagnóstico e do plano de tratamento.
PALAVRAS-CHAVE:
TRANSTORNOS DA ARTICULAÇÃO TEMPOROMANDIBULAR; DIAGNÓSTICO POR IMAGEM; ARTICULAÇÃO TEMPOROMANDIBULAR; IMAGEM POR RESSONÂNCIA MAGNÉTICA; TOMOGRAFIA COMPUTADORIZADA POR RAIOS X; RADIOGRAFIA
Introduction
The temporomandibular joint (TMJ) is a composite ginglymus-arthrodial joint, whose components are the condyle, glenoid cavity and articular tubercle, articular disc, retrodiscal tissue, synovial membrane, and joint capsule.11. Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32. It is the most frequently used joint of the human body and has simultaneous bilateral capacity to move the mandible.22. Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42.and33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.
Its components often undergo remodeling and adaptation processes. In the presence of temporomandibular disorders (TMD), structural alterations and functional disorders are commonly observed.22. Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42.and33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.
In most cases, symptoms are diffuse and imprecisely manifested as masticatory myalgia, arthralgia, headache, otalgia, and neck pain, among others.4, 5, 6, 7 and 8 Pain in more than one area is common and often leads patients to seek evaluation from various medical and dental specialists, including otorhinolaryngologists.66. Cunha SC, Nogueira RVB, Duarte AP, Vasconcelos BCE, Almeida RAC. Análise dos índices de Helkimo e craniomandibular para diagnóstico de desordens temporomandibulares em pacientes com artrite reumatoide. Braz J Otorhinolaryngol. 2007;73:19-26.and88. Silveira AM, Feltrin PP, Zanetti RV, Mautoni MC. Prevalência de portadores de DTM em pacientes avaliados no setor de otorrinolaringologia. Braz J Otorhinolaryngol. 2007;73:528-32.
For instructional purposes, the American Academy of Orofacial Pain (AAOP) has classified TMD into two major groups: muscle and joint pain.99. Leeuw R. Disfunção temporomandibular. In: Leeuw R, editor. Dor orofacial. São Paulo: Quintessence; 2010. p. 129-204. It is estimated that temporomandibular joint disorders (TMJD) affect approximately 30% of the population in asymptomatic form, as internal joint derangement, comprising disc dislocation and structural changes resulting from osteoarthritis and osteoarthrosis.2, 10 and 11 The diagnostic subtypes TMJD can be seen in Table 1.
The etiology of TMJD is not fully understood6, 8 and 12 and is related to the presence of risk factors such as trauma, parafunctional habits, postural condition, occlusal microtrauma, systemic predisposition, sleep disorders, and deleterious psychosocial alterations.6, 7, 8, 11 and 13
The diagnosis of TMJD is achieved by evaluating the medical history and by physical examination.6, 8 and 14 However, diagnostic TMJ imaging methods are used to assess the integrity of its components and their functional association, to confirm the extent or progression of an existing disease, and to assess and document the effects of an already established treatment.99. Leeuw R. Disfunção temporomandibular. In: Leeuw R, editor. Dor orofacial. São Paulo: Quintessence; 2010. p. 129-204.and1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. They are essential for assessment in cases of trauma, occlusal alterations and sudden limitation of mouth opening, presence of joint noises, systemic joint diseases, infection and failure of conservative treatments.1313. Hunter A, Kalathingal S. Diagnostic imaging for temporomandibular disorders and orofacial pain. Dent Clin North Am. 2013;57:405-18.
Objectives
This study discusses the main imaging techniques for the assessment of TMJ and adjacent structures and their indications for the diagnosis of joint alterations, rationally evaluating their advantages and disadvantages.
Method
Using the ISI Web of Knowledge, PubMed, and SciELO databases, a search was carried out for literature articles published and made available in the years 2004-2014, in English or Portuguese, that contained the keywords "temporomandibular joint disorder" and "diagnostic imaging test."
There were 51 articles found in the ISI Web of Knowledge database, 117 in PubMed, and 25 in SciELO. Basic research experimental articles, letters to the editor, and isolated case reports were excluded. A total of 23 articles, characterized as clinical trials, comparative studies, reviews, and case group studies comprised the first stage of the research.
Then, based on the same inclusion criteria, a literature search was performed in the five most frequently cited radiology journals for the years 2004-2014. In this search, six new references were found in addition to the previously selected articles. Four other relevant publications cited in the selected articles' lists of references were added, including historical ones dated prior to 2004.
According to the requirements defined in CNS Resolution 196/96, this study was submitted to the Research Ethics Committee, approved under No. 133/2009, designed to demonstrate the major changes in the TMJ as disclosed by imaging tests.
Temporomandibular joint imaging assessment
Radiographic examinations
TMJ radiographs provide information on the morphological characteristics of osseus components of the joint and certain functional associations between the condyle, articular tubercle and fossa, but are inefficient for evaluating the soft tissues.1, 14 and 16
Several anatomical and technical factors can prevent a clear and unobstructed radiographic image of the TMJ.1616. Cozzolino FA, Rapoport A, Franzi SA, Souza RP, Pereira CAB, Dedivitis RA. Correlação entre os achados clínicos e imaginológicos nas disfunções temporomandibulares. Radiol Bras. 2008;41:13-7.and1717. Almeida SM, Bóscolo FN, Pereira TCR. Estudo comparativo entre duas técnicas radiográficas transcranianas utilizando o cefalostato ACCURAD-200, nas posições padrão e corrigida, e confecção de gabaritos para delimitação dos espaços articulares. Rev Fac Odontol Univ São Paulo. 1997;11:51-60. When choosing TMJ radiography, one needs to consider the identification of boney structural details, the specific suspected clinical disorder, the amount of symptomatic information clinically available for the diagnosis, the cost of these examinations, and their radiation dose.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.and1414. Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57. The radiographic techniques most often used in the routine management of TMJD are panoramic radiography, planigraphy, and transcranial radiography1, 3, 13 and 15 (Fig. 1).
Radiographic assessments of different TMDs. (a-c) Close-up in panoramic image showing mandibular condyle hypoplasia (a), horizontal impaction of the third molar (a, b) fracture line in the region of gonial angle (b) and elongated styloid process. The transcranial images (d-f) show the presence of osteophytes (d), preservation of joint spaces in maximum habitual intercuspation (MHI) (e) and the identification of condylar hyperexcursion (f). The planography techniques (g-j) demonstrate: mandibular neck fracture and ankylosis (g) elongated styloid process (h), advanced remodeling process, superior-anterior flattening, cortical irregularities, and osteophyte formation (i) in addition to mandibular head hyperexcursion, defining TMJ hypermobility (j).
Panoramic radiography
As it provides a maxillary overview, it is useful in the differential diagnosis of odontogenic alterations whose symptoms overlap with TMJD.1313. Hunter A, Kalathingal S. Diagnostic imaging for temporomandibular disorders and orofacial pain. Dent Clin North Am. 2013;57:405-18.and1818. Hintze H, Wiese M, Wenzel A. Comparison of three radiographic methods for detection of morphological temporomandibular joint changes: panoramic, scanographic and tomographic examination. Dentomaxillofac Radiol. 2009;38:134-40. It can reveal advanced bone alterations in the condyle, such as asymmetries, erosions, osteophytes, fractures, changes in size and shape, degenerative and inflammatory processes, growth alterations, maxillary tumors, metastases, and ankylosis.1, 13, 15 and 16 However, it does not provide functional information on condylar excursion.1414. Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57. Also, only gross alterations in the articular tubercle morphology can be seen because of the superimposition of images of the skull base and the zygomatic arch.3, 14, 16 and 18 This technique is useful as a screening tool, as it allows the initial diagnosis and assessment of TMJ alterations that are not so subtle.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. It is also indicated when the patient has reduced mouth opening and the differential diagnosis of fracture is considered.11. Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32.and33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.
Planigraphy (or panoramic radiography with programs for TMJ)
This method provides considerable accuracy and produces images without much overlap. It visualizes the articular boney detail and reveals any anatomical abnormalities in structures adjacent to the TMJ, such as the styloid process, mastoid process, and zygomatic arch.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.and1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. It can be obtained in the sagittal and coronal planes, documenting the relationship of the condyle with the articular fossa in maximum habitual intercuspation (MHI) and the excursion extension during maximal mouth opening (MMO). It provides a direct comparison of both sides regarding the hypo-, normo-, or hyperexcursion of the condyle, which is useful in confirming a clinical suspicion of hypermobility.11. Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32.and33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.
In spite of the relative identification of the TMJ boney structures, it does exhibit some magnification that is inherent to the technique. However, it is useful for functional assessment of mouth opening, evaluation of morphological alteration and the joint spaces, analysis of dimension, fractures, and ankylosis.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.
Transcranial radiography
Similarly to the planigraphy, this evaluation provides good anatomical assessment of the condyle, fossa, and articular tubercle.1, 14 and 17 In this technique, an X-ray beam is obliquely directed through the skull to the contralateral TMJ, producing a sagittal view.1717. Almeida SM, Bóscolo FN, Pereira TCR. Estudo comparativo entre duas técnicas radiográficas transcranianas utilizando o cefalostato ACCURAD-200, nas posições padrão e corrigida, e confecção de gabaritos para delimitação dos espaços articulares. Rev Fac Odontol Univ São Paulo. 1997;11:51-60. Thus, the central and medial portions of the condyle are projected inferiorly and only the lateral joint contour is displayed.1717. Almeida SM, Bóscolo FN, Pereira TCR. Estudo comparativo entre duas técnicas radiográficas transcranianas utilizando o cefalostato ACCURAD-200, nas posições padrão e corrigida, e confecção de gabaritos para delimitação dos espaços articulares. Rev Fac Odontol Univ São Paulo. 1997;11:51-60. It is useful to identify bone alterations and displaced fractures of the head and neck of the mandibular condyle, as well as to assess excursion and to determine radiographic joint spaces.3, 14 and 17
This type of projection is limited by the fact that it produces an image with a large overlap of the skull bones; it also requires the use of a specific cephalostat for standardization, usually requiring complex positioning.1, 13, 14 and 17
Arthrography
Arthrography is a variant of the radiographic technique for TMJ, which aims to assess the TMJ soft tissues. In the 1970s and 1980s, arthrography was the method of choice for the identification of disc displacement.14, 15 and 19 Disc morphology, positioning, and function were indirectly identified by contrast injection into the superior and/or inferior joint spaces.1414. Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57. After the injection, dynamic images were obtained, recording mandibular movements.2020. Ramos ACA, Sarmento VA, Campos PSF, Gonzalez MOD. Articulação temporomandibular - aspectos normais e deslocamentos de disco: imagem por ressonância magnética. Radiol Bras. 2004;37:449-54.
Even though it is useful for disc position identification, arthrography is not currently recommended as it is an invasive procedure and carries a risk of iatrogenic disc perforation and facial nerve damage.1414. Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57. There are also the risks of radiation to radiosensitive structures (crystalline and thyroid), pain and limitation of movement after the injections, infections, allergies to the injected dye, and it is an examination that is considered difficult to perform.1, 14, 15 and 20
Other combined radiographic techniques
Due to the two-dimensional radiographic visualization of the TMJ, the combined use of different techniques is necessary to provide an accurate diagnosis and location of the alterations. The evaluation of the structures in different planes illuminates fracture extension, degenerative joint disease, postoperative status, ankylosis, and neoplasms.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66. Additionally, the anatomic relations of areas adjacent to the lesion can be studied with greater diagnostic accuracy, providing more efficient surgical and therapeutic planning.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. The main combined views are submental (or submento-vertex), transpharyngeal, transmaxillary, reverse Towne, posterior-anterior, and lateral teleradiography.3, 13 and 15
Despite their lower cost, technical simplicity, and lower levels of radiation, the use of combined radiographic images has become less common due to increasing use and availability of accurate images such as cone-beam computed tomography, which assess hard tissues in the three anatomical planes and are widely used in dental diagnosis.1313. Hunter A, Kalathingal S. Diagnostic imaging for temporomandibular disorders and orofacial pain. Dent Clin North Am. 2013;57:405-18.and1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.
Computed tomography (CT)
CT comprises a set of images obtained through a sophisticated and highly accurate technique, compared to plane radiographs.22. Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42. Recently, cone-beam computed tomography (CBCT) technology has been used for dental diagnosis due to its specific use for the maxillofacial region.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.and2121. Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8. Its main advantage is the observation of boney joint structures in the sagittal, coronal, and axial planes,11. Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32.and2121. Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8. in addition to the possible image manipulation at different depths and three-dimensional reconstruction1414. Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57.and2121. Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8. through specific software. The examination time varies between 10 and 70 s, and the radiation dose is much lower compared to the helical technique.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.and2121. Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8.
The main indications of CBCT include structural assessment of bone components of the TMJ, which precisely determines the location and extent of boney alterations: fractures, neoplasms, and ankylosis; erosive degenerative, pseudocystic, and osteophytic alterations; presence of asymptomatic bone remodeling; evaluation of post-surgical conditions; hyperplasia of condylar, coronoid, and styloid processes; persistent foramen of Huschke; as well as intraarticular calcification derived from synovial chondromatosis or metabolic arthritis.2, 14 and 15
Hard tissues, teeth, and bones are well demonstrated and measured in their real morphological condition, with minimal noise and artifacts.1, 18 and 22 However, few details are provided on soft tissue and it is not possible to evaluate the joint disc.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.and2222. Alkhader M, Ohbayashi N, Tetsumura A, Nakamura S, Okochi K, Momin MA, et al. Diagnostic performance of magnetic resonance imaging for detecting osseous abnormalities of the temporomandibular joint and its correlation with cone beam computed tomography. Dentomaxillofac Radiol. 2010;39:270-6.
Significant disadvantages are the cost of the examination and exposure to significant levels of radiation compared to conventional radiographic techniques.1, 14, 15 and 18
Fig. 2 shows morphological alterations in joint bone components diagnosed by the CBCT technique.
Cone-beam computed tomography (CBCT) assessment of different TMJs in the coronal (a, e) and parasagittal (b-d) views. (a) Coronal view showing extensive erosion. Note the presence of bone sclerosis, cortical irregularities, and osteophytic formation in (b), (c), and (e). The presence of subchondral cysts can be observed in (c) and (e). Advanced flattening of bone components and decreased joint space are recorded in (d). Advanced degenerative osteoarthritis alteration is observed in e. Three-dimensional reconstructions (f-h) show osteophytes (f, g), advanced erosion (g) and hyperexcursion of the mandibular condyle (h). (i) The coronal view of the right and left TMJ shows alteration of the mandibular condyle and hyperdense images in the joint spaces compatible with synovial chondromatosis.
Magnetic resonance imaging (MRI)
MRI has been the method of choice to study disease processes involving the TMJ soft tissues,2, 20 and 23 such as the articular disc, ligaments, retrodiscal tissues, intracapsular synovial content, adjacent masticatory muscles, as well as cortical and medullary integrity of bone components.1, 3, 15 and 22
The technique allows three-dimensional analysis in the axial, coronal, and sagittal planes. It is considered the gold standard for assessing disc position and is highly sensitive for intraarticular degenerative alterations.3, 20 and 23
The clinical conditions that suggest its use include persistent symptoms of joint or pre-auricular pain, presence of clicking and crepitation noises, functional alterations such as lateral projections of the condyle during mouth opening, frequent subluxations and dislocations, limited mouth opening movement with terminal stiffness, suspected neoplastic processes, and presence of osteoarthritic symptoms or asymptomatic osteoarthrosis.1, 2, 13 and 15
This diagnostic test protocols usually include the recording in the MHI and MMO position, using weighted T1, T2, and proton density (PD), in the sagittal and coronal planes.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. With T1-weighted images, it is possible to obtain excellent anatomic detail; proton density results in satisfactory spatial resolution of joint disc injuries, and is an excellent choice for the evaluation of medial and lateral disc displacements.2020. Ramos ACA, Sarmento VA, Campos PSF, Gonzalez MOD. Articulação temporomandibular - aspectos normais e deslocamentos de disco: imagem por ressonância magnética. Radiol Bras. 2004;37:449-54. T2-weighted images record the presence of joint effusion and medullary bone edema.2, 3 and 20
The main advantages include detecting soft tissue alterations, necrosis, edema, presence or absence of invasion, and lack of exposure to ionizing radiation.2, 3, 15, 16 and 20
MRI is also indicated for the assessment of the integrity and anatomical relation of neural structures, which, when compressed by tumor or vascular processes, can produce orofacial pain by demyelination and deafferentation.2, 3, 13, 14 and 16
Its disadvantages are related to the high cost and the need for sophisticated facilities. It is contraindicated in claustrophobic patients, those with pacemakers and metallic heart valves, ferromagnetic foreign bodies, and pregnant women.14, 15 and 23
Fig. 3 illustrates morphological joint disc and bone structures alterations diagnosed by MRI.
Different MRI assessments disclosing previous joint disc displacement, with no reduction in the parasagittal views. One can observe compressive deformation of the joint disc in (a), also during dynamic comparison of the mandibular condylar movement in (b) and (c). Osteophytic formations (d-f), subchondral cyst (d), and severe change in form (f) define the diagnosis of osteoarthritis degenerative alterations in bone components. The presence of hyperintense T2-weighted images defines the diagnosis of effusion in (b-f).
Other imaging techniques
Ultrasonography (US)
The use of US examination, especially by high-resolution imaging equipment, can be a useful option in the assessment of disc position in internal TMJ disorders.44. Landes CA, Goral WA, Sader R, Mack M. 3D sonography for diagnosis of disc dislocation of the temporomandibular joint compared with MRI. Ultrasound Med Biol. 2006;32:633-9.and2323. Jank S, Zangerl A, Kloss F, Laimer K, Missmann M, Schroeder D, et al. High resolution ultrasound investigation of the temporomandibular joint in patients with chronic polyarthritis. Int J Oral Maxillofac Surg. 2011;40:45-9. Although it has considerable diagnostic sensitivity, it has insufficient specificity to identify osteoarthrosis. The findings related to morphological alterations show that the method still does not have accuracy for the cortical and articular disc morphological diagnosis.2424. Bas B, Yilmaz N, Gökce E, Akan H, Turkey S. Ultrasound assessment of increased capsular width in temporomandibular joint internal derangements: relationship with joint pain and magnetic resonance grading of joint effusion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:112-7. However, the method is able to identify effusion in patients with inflammatory condition associated with pain, verified by MRI.2323. Jank S, Zangerl A, Kloss F, Laimer K, Missmann M, Schroeder D, et al. High resolution ultrasound investigation of the temporomandibular joint in patients with chronic polyarthritis. Int J Oral Maxillofac Surg. 2011;40:45-9.and2424. Bas B, Yilmaz N, Gökce E, Akan H, Turkey S. Ultrasound assessment of increased capsular width in temporomandibular joint internal derangements: relationship with joint pain and magnetic resonance grading of joint effusion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:112-7.
Even with limitations, it can become a useful option for the initial study of the internal dysfunctions of the TMJ,1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.and2323. Jank S, Zangerl A, Kloss F, Laimer K, Missmann M, Schroeder D, et al. High resolution ultrasound investigation of the temporomandibular joint in patients with chronic polyarthritis. Int J Oral Maxillofac Surg. 2011;40:45-9. particularly in patients with contraindications to MRI.1414. Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57. Moreover, it is less expensive, allows real-time visualization without the use of ionizing radiation, and is quick and comfortable.4, 23 and 24
US assessment is commonly used in the differential diagnosis of glandular and adjacent structures alterations, such as the TMJ and the masseter muscle. The symptoms present in cases of sialadenitis and sialolithiasis can be mistaken for Eagle syndrome, TMD, myofascial pain, nerve pain, and other orofacial pain conditions.
Another indication of the US assessment is the correct location of joint spaces for infiltrative therapies, arthrocentesis, and viscosupplementation (Fig. 4a and b). It shows, dynamically and in realtime, the location of joint components, providing adequate lubrication and washing, which are verified by the increase in joint space after treatment.2525. Dayisoylu EH, Cifci E, Uckan S. Ultrasound-guided arthrocentesis of the temporomandibular joint. Br J Oral Maxillofac Surg. 2013;51:667-8.
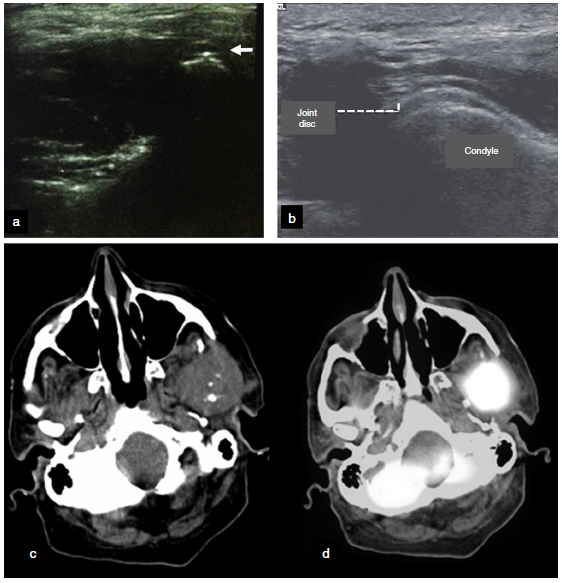
Other imaging techniques. (a) Ultrasound examination of the TMJ25 used during the arthrocentesis assessment. Note the arthrocentesis needle as a hyperechoic point (white arrow). (b) Ultrasound examination of the TMJ showing the joint disc and condyle. (c) Tomographic axial view28 showing mass of soft tissue growth in the left TMJ region extending to the ipsilateral pterygoid region. Infra-temporal space with absence of condylar process, the presence of hyperdense areas, swelling, and asymmetry. (d) PET/CT assessment in axial view28 showing high metabolic activity in the left TMJ region. Images reproduced with permission of the authors' copyrights25 and 28 by Elsevier.
Nuclear medicine evaluation
Nuclear medicine facilitates establishing a diagnosis by detecting minute concentrations of radioactive pharmacological substances that determine osteometabolic alterations expressed in imaging exams.2626. Coutinho A, FenyoPereira M, Dib LL, Lima ENP. The role of SPECT/CT with (99m) Tc-MDP image fusion to diagnose temporomandibular dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:224-30.
Bone scintigraphy is indicated to define neoplastic activity, metabolic disorders, and bone growth,14, 26 and 27 as well as to evaluate synovitis and osteoarthritis.1818. Hintze H, Wiese M, Wenzel A. Comparison of three radiographic methods for detection of morphological temporomandibular joint changes: panoramic, scanographic and tomographic examination. Dentomaxillofac Radiol. 2009;38:134-40. It is an examination with considerable sensitivity, low invasiveness, and high organ specificity, with low levels of radiation.2727. Bittencourt LP, Souza SAL, Magnanini M, Fonseca LMB, Gutfilen B. Verificação da atividade condilar em pacientes com padrão esquelético classe III por intermédio da cintilografia óssea. Radiol Bras. 2005;38:273-7. It has some advantages over radiographies, conventional CT, and MRI because it provides an estimate of metabolic and inflammatory activity.2626. Coutinho A, FenyoPereira M, Dib LL, Lima ENP. The role of SPECT/CT with (99m) Tc-MDP image fusion to diagnose temporomandibular dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:224-30.and2727. Bittencourt LP, Souza SAL, Magnanini M, Fonseca LMB, Gutfilen B. Verificação da atividade condilar em pacientes com padrão esquelético classe III por intermédio da cintilografia óssea. Radiol Bras. 2005;38:273-7. It can facilitate an early diagnosis and is less costly than CT and MRI. However, it does not differentiate among bone scar disorders, infections, osteoarthritic manifestations, or tumors.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.
Positron-emission tomography (PET) is usually indicated for the assessment and staging of metastatic tumors. It is able to provide accurate functional, morphological, and metabolic information.2828. Shintaku WH, Venturin JS, Yepes JS. Application of advanced imaging modalities for the diagnosis of metastatic adenocarcinoma of the lungs in the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107: 37-41. Three-dimensional images facilitate anatomical visualization and can significantly reduce the time required for diagnosis, in addition to properly direct treatments by ensuring that the therapies are appropriate.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.
Currently, single photon emission computed tomography with technetium-99m methylene diphosphate (SPECT/CT with 99m Tc-MDP) is largely employed.2626. Coutinho A, FenyoPereira M, Dib LL, Lima ENP. The role of SPECT/CT with (99m) Tc-MDP image fusion to diagnose temporomandibular dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:224-30. This technology allows for multiplane image acquisition and 3-D display. The radiotracer 99m Tc is able to reflect the local osteometabolic rate, while the anatomic mapping is obtained by tomographic technique.2626. Coutinho A, FenyoPereira M, Dib LL, Lima ENP. The role of SPECT/CT with (99m) Tc-MDP image fusion to diagnose temporomandibular dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:224-30. As in the PET, anatomical and functional data are fused into a single image2828. Shintaku WH, Venturin JS, Yepes JS. Application of advanced imaging modalities for the diagnosis of metastatic adenocarcinoma of the lungs in the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107: 37-41. (Fig. 4c and d). Its main advantage is its sensitivity and specificity.2626. Coutinho A, FenyoPereira M, Dib LL, Lima ENP. The role of SPECT/CT with (99m) Tc-MDP image fusion to diagnose temporomandibular dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:224-30.and2828. Shintaku WH, Venturin JS, Yepes JS. Application of advanced imaging modalities for the diagnosis of metastatic adenocarcinoma of the lungs in the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107: 37-41.
Nuclear medicine examinations differ by the radiotracers/radioisotopes used, image capture technique, radiation dose, sensitivity, and presentation of results.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.
Imaging test indication criteria in the diagnosis of temporomandibular joint disorders
One of the failures in diagnosis and treatment planning is an incorrect or unnecessary selection of unsuitable diagnostic tests. This occurs because of a lack of knowledge on the part of the professionals regarding the indications of the applicable tests.2929. Pharoah M. The prescription of diagnostic images for temporomandibular joint disorders. J Orofac Pain. 1999;13:251-4.
The correct indication of an imaging study should be based on the patient's need for legal documentation, his/her individual complaints, and the identified clinical signs and symptoms obtained during history-taking and physical examination.15, 29 and 30 The basic principle that should guide the professional is that supplementary tests are only indicated when the clinical assessment is not sufficient to arrive at a diagnosis and devise a treatment plan.2121. Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8.
For TMJD, the physical examinations of palpation, measurement of movement, functional testing and evaluation of joint noises are instruments of great diagnostic validity when performed by trained and experienced professionals.66. Cunha SC, Nogueira RVB, Duarte AP, Vasconcelos BCE, Almeida RAC. Análise dos índices de Helkimo e craniomandibular para diagnóstico de desordens temporomandibulares em pacientes com artrite reumatoide. Braz J Otorhinolaryngol. 2007;73:19-26. However, the overlapping of muscle and joint symptoms can impair diagnostic accuracy, as both conditions show functional impairment. In this case and in cases of non-specific symptoms (from, for example, inflammation, neoplasia, and trauma), complementary imaging tests are essential for diagnostic clarification and delineation of the appropriate therapy.22. Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42.and66. Cunha SC, Nogueira RVB, Duarte AP, Vasconcelos BCE, Almeida RAC. Análise dos índices de Helkimo e craniomandibular para diagnóstico de desordens temporomandibulares em pacientes com artrite reumatoide. Braz J Otorhinolaryngol. 2007;73:19-26.
Imaging tests, from the simplest to the most complex, have varying degrees of sensitivity and specificity, properties that give them their diagnostic power.3131. Calderon PDS, Reis KR, Araujo CDRP, Rubo JH, Conti PCR. Ressonância magnética nos desarranjos internos da ATM: sensibilidade e especificidade. Rev Dent Press Ortodon Ortoped Facial. 2008;13:34-9.
In general, MRI and CT are methods with higher accuracy when compared to conventional radiology, due to the higher anatomical resolution they provide. CT is considered the gold standard for the assessment of boney structures and the method of choice for facial trauma, whereas MRI is similarly regarded for the study of soft tissues.1, 2, 16, 23 and 29 The two methods often complement each other in the study of TMJ alterations, constituting important tools for muscle and joint differential diagnosis.44. Landes CA, Goral WA, Sader R, Mack M. 3D sonography for diagnosis of disc dislocation of the temporomandibular joint compared with MRI. Ultrasound Med Biol. 2006;32:633-9. Although able to diagnose all bone alterations of the TMJ, MRI is considered limited when compared to the high accuracy of CT for hard tissue.1919. Sano T. Recent developments in understanding temporomandibular joint disorders. Part 1: bone marrow abnormalities of the mandibular condyle. Dentomaxillofac Radiol. 2000;29:7-10.and2222. Alkhader M, Ohbayashi N, Tetsumura A, Nakamura S, Okochi K, Momin MA, et al. Diagnostic performance of magnetic resonance imaging for detecting osseous abnormalities of the temporomandibular joint and its correlation with cone beam computed tomography. Dentomaxillofac Radiol. 2010;39:270-6.
However, low-technical-complexity tests may possess high diagnostic accuracy,1818. Hintze H, Wiese M, Wenzel A. Comparison of three radiographic methods for detection of morphological temporomandibular joint changes: panoramic, scanographic and tomographic examination. Dentomaxillofac Radiol. 2009;38:134-40. as in the case of radiographic records of condylar hyperexcursion in patients with the clinical presentation of terminal joint clicking. These characteristics suggest a diagnosis of joint hypermobility, verified by a simple transcranial or planigraphy image.33. Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66. In this example, the image has great sensitivity, while clinical data confer specificity, ruling out other diagnostic possibilities.
Similarly, morphological alterations of the styloid, coronoid, and condylar processes can be evaluated with high diagnostic accuracy through low-cost and easy-to-perform radiographic examinations, such as planigraphy and panoramic X-rays,2929. Pharoah M. The prescription of diagnostic images for temporomandibular joint disorders. J Orofac Pain. 1999;13:251-4. even though the CT is the gold standard for assessment of these alterations.22. Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42.
The decision in choosing the examination must consider its influence on the proposed diagnosis and therapy. If the clinical indication is a conservative therapy that can control symptoms in the short term, image requests can be considered.11. Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32.and1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. Moreover, when conservative therapy has failed and an invasive therapy is indicated, highly sensitive diagnostic tests, such as CT and MRI are selected.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.and3131. Calderon PDS, Reis KR, Araujo CDRP, Rubo JH, Conti PCR. Ressonância magnética nos desarranjos internos da ATM: sensibilidade e especificidade. Rev Dent Press Ortodon Ortoped Facial. 2008;13:34-9.
Elaborate treatment plans also require complete and accurate images,2929. Pharoah M. The prescription of diagnostic images for temporomandibular joint disorders. J Orofac Pain. 1999;13:251-4.and3131. Calderon PDS, Reis KR, Araujo CDRP, Rubo JH, Conti PCR. Ressonância magnética nos desarranjos internos da ATM: sensibilidade e especificidade. Rev Dent Press Ortodon Ortoped Facial. 2008;13:34-9. for example, suspected fractures, where the CT, in addition to establishing the diagnosis, illustrates the exact location and size, and allows for the selection of the appropriate surgical therapy.22. Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42.
Similar reasoning is used for the assessment of neoplastic conditions. A study3232. Shintaku WH, Venturin JS, Langlais RP, Clark GT. Imaging modalities to access bony tumors and hyperplasic reactions of the temporomandibular joint. J Oral Maxillofac Surg. 2010;68:1911-21. that compared the accuracy of imaging tests for bone tumor detection showed that the nuclear medicine diagnostic tests had greater sensitivity and specificity than CT scans, MRI, and radiographic assessment, although the latter are useful in the initial clinical investigations.26, 28, 29 and 32
Especially for non-surgical joint conditions, one should consider the risk of injuries and the safety of diagnostic techniques.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90. Although arthrography can effectively determine disc position and perforation,3333. Liedberg J, Panmekiate S, Petersson A, Rohlin M. Evidencebased evaluation of three imaging methods for the temporomandibular disc. Dentomaxillofac Radiol. 1996;25:234-41. it is considered an invasive and potentially hazardous method. Thus, MRI has become the method of choice for such conditions.11. Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32.
Similarly, recent studies4, 5, 23, 24, 25 and 30 have recommended US as a safe, noninvasive diagnostic technique with considerable accuracy for joint disc positioning, especially for patients with contraindication to MRI or submitted to real-time interventions, such as arthrocentesis and viscosupplementation. In these techniques, the US examination is especially appropriate for the identification of the inferior joint space. Its precise identification and correct access are factors that contribute to the technique's success.1111. Grossmann E, Januzzi E, Iwaki Filho L. O uso do hialuronato de sódio no tratamento das disfunções temporomandibulares articulares. Rev Dor. 2013;14:301-6.
Long-term risks and tissue damage should also be considered for radiation exposure. As in conventional radiographs, CT should only cautiously be chosen because of its higher radiation absorption,1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.and2929. Pharoah M. The prescription of diagnostic images for temporomandibular joint disorders. J Orofac Pain. 1999;13:251-4. although CBCT has shorter radiation exposure time when compared to helical CT.2121. Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8.
Even if they pose some risk, tests that use higher doses of radiation are needed for disease staging and are essential for defining the treatment plan. Nuclear medicine examinations, for instance, are indicated to assess metabolic alterations of growth and assessment of metastases.26, 27 and 28 However, they still require confirmation of the type of growth through specific tests, such as histopathological or immunohistochemical analysis.1515. Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.
Table 2 lists and classifies information that can be obtained by several examination techniques through TMJ images, based on their indications, risks, and diagnostic power.
Conclusion
Individually, the several imaging tests have specific indications for the diagnosis of TMJD.
Despite their lower sensitivity, radiographic techniques have lower cost and employ lower radiation doses. They are indicated for the early assessment of less complex symptoms and the differential diagnosis between TMD and inflammatory dental-maxillofacial conditions.
Morphological, degenerative bone abnormalities, and fractures are precisely diagnosed, identified, and measured by CT. Mainly, CBCT has a lower radiation dose and artifact reduction, and is considered the gold standard for the assessment of maxillofacial hard tissues. Inflammatory alterations, joint disc position, and other soft tissue structures are clearly identified and evaluated by MRI, that is safer than arthrography.
US examination accurately identifies the joint disc, mainly when the MRI assessment is contraindicated. It is indicated for the differential diagnosis between TMD and painful conditions of major salivary glands, as well as pre- and post-evaluation of infiltration therapies, such as viscosupplementation and arthrocentesis.
Nuclear medicine assessments are primarily indicated for the assessment of metabolic and growth alterations, such as tumors and metastases.
Arthrography is an invasive intra-articular examination; its usual indication is the visualization of joint disc alterations. Due to the risk inherent to the technique, it has been replaced by MRI assessment.
Factors that need to be evaluated for the selection of TMJ imaging tests include the following: the need to determine the presence of the disease and its prognosis, the quality and quantity of available clinical information; uncertainty in the differential diagnosis; determining the stage of disease development; need for legal documentation; preoperative preparation; evaluation of treatment evolution; and the safety and accuracy of the proposed examination.
References
-
1Mahl CRW, Silveira MW. Diagnóstico por imagens da articulação temporomandibular: técnicas e indicações. JBA. 2002;2: 327-32.
-
2Garcia MM, Machado KFS, Mascarenhas MH. Ressonância magnética e tomografia computadorizada da articulação temporomandibular: além da disfunção. Radiol Bras. 2008;41:337-42.
-
3Ferraz Júnior AML, Guimarães JP, Ferreira LA. Técnicas de obtenção de imagens da articulação temporomandibular. In: Guimarães JP, Ferreira LA, editors. Atlas de diagnóstico por imaginologia das desordens temporomandibulares. Juiz de Fora: Editora UFJF; 2012. p. 28-66.
-
4Landes CA, Goral WA, Sader R, Mack M. 3D sonography for diagnosis of disc dislocation of the temporomandibular joint compared with MRI. Ultrasound Med Biol. 2006;32:633-9.
-
5Çakir-Özkan N, Sarikaya B, Erkorkmaz U, Aktürk Y. Ultrasonographic evaluation of disc displacement of the temporomandibular joint compared with magnetic resonance imaging. J Oral Maxillofac Surg. 2010;68:1075-80.
-
6Cunha SC, Nogueira RVB, Duarte AP, Vasconcelos BCE, Almeida RAC. Análise dos índices de Helkimo e craniomandibular para diagnóstico de desordens temporomandibulares em pacientes com artrite reumatoide. Braz J Otorhinolaryngol. 2007;73:19-26.
-
7Ferreira LA, Oliveira RG, Guimarães JP, Carvalho ACP, Paula MVQ. Laser acupuncture in patients with temporomandibular dysfunction: a randomized controlled trial. Lasers Med Sci. 2013;28:1549-58.
-
8Silveira AM, Feltrin PP, Zanetti RV, Mautoni MC. Prevalência de portadores de DTM em pacientes avaliados no setor de otorrinolaringologia. Braz J Otorhinolaryngol. 2007;73:528-32.
-
9Leeuw R. Disfunção temporomandibular. In: Leeuw R, editor. Dor orofacial. São Paulo: Quintessence; 2010. p. 129-204.
-
10Fujiwara M, Honda K, Hasegawa Y, Hasegawa M, Urade M. Comparison of joint pain in patients diagnosed with and without articular disc displacement without reduction based on the Research Diagnostic Criteria for Temporomandibular Disorders. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2013;116:9-15.
-
11Grossmann E, Januzzi E, Iwaki Filho L. O uso do hialuronato de sódio no tratamento das disfunções temporomandibulares articulares. Rev Dor. 2013;14:301-6.
-
12Güler N, Uçkan S, Imirzalioglu P, Açikgözoglu S. Temporomandibular joint internal derangement: relationship between joint pain and MR grading of effusion and total protein concentration in the joint fluid. Dentomaxillofac Radiol. 2005;34:175-81.
-
13Hunter A, Kalathingal S. Diagnostic imaging for temporomandibular disorders and orofacial pain. Dent Clin North Am. 2013;57:405-18.
-
14Vasconcelos BCE, Silva EDO, Kelner N, Miranda KS, Silva AFC. Meios de diagnóstico das desordens temporomandibulares. Rev Cir Traumat Buco-Maxilo-Facial. 2002;1:49-57.
-
15Lewis EL, Dolwick MF, Abramowicz S, Reeder SL. Contemporary imaging of the temporomandibular joint. Dent Clin North Am. 2008;52:875-90.
-
16Cozzolino FA, Rapoport A, Franzi SA, Souza RP, Pereira CAB, Dedivitis RA. Correlação entre os achados clínicos e imaginológicos nas disfunções temporomandibulares. Radiol Bras. 2008;41:13-7.
-
17Almeida SM, Bóscolo FN, Pereira TCR. Estudo comparativo entre duas técnicas radiográficas transcranianas utilizando o cefalostato ACCURAD-200, nas posições padrão e corrigida, e confecção de gabaritos para delimitação dos espaços articulares. Rev Fac Odontol Univ São Paulo. 1997;11:51-60.
-
18Hintze H, Wiese M, Wenzel A. Comparison of three radiographic methods for detection of morphological temporomandibular joint changes: panoramic, scanographic and tomographic examination. Dentomaxillofac Radiol. 2009;38:134-40.
-
19Sano T. Recent developments in understanding temporomandibular joint disorders. Part 1: bone marrow abnormalities of the mandibular condyle. Dentomaxillofac Radiol. 2000;29:7-10.
-
20Ramos ACA, Sarmento VA, Campos PSF, Gonzalez MOD. Articulação temporomandibular - aspectos normais e deslocamentos de disco: imagem por ressonância magnética. Radiol Bras. 2004;37:449-54.
-
21Rodrigues MGS, Alarcón OMV, Carraro E, Rocha JF, Capelozza ALA. Tomografia computadorizada por feixe cônico: formação da imagem, indicação e critérios para prescrição. Odontol ClínCient. 2010;9:115-8.
-
22Alkhader M, Ohbayashi N, Tetsumura A, Nakamura S, Okochi K, Momin MA, et al. Diagnostic performance of magnetic resonance imaging for detecting osseous abnormalities of the temporomandibular joint and its correlation with cone beam computed tomography. Dentomaxillofac Radiol. 2010;39:270-6.
-
23Jank S, Zangerl A, Kloss F, Laimer K, Missmann M, Schroeder D, et al. High resolution ultrasound investigation of the temporomandibular joint in patients with chronic polyarthritis. Int J Oral Maxillofac Surg. 2011;40:45-9.
-
24Bas B, Yilmaz N, Gökce E, Akan H, Turkey S. Ultrasound assessment of increased capsular width in temporomandibular joint internal derangements: relationship with joint pain and magnetic resonance grading of joint effusion. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112:112-7.
-
25Dayisoylu EH, Cifci E, Uckan S. Ultrasound-guided arthrocentesis of the temporomandibular joint. Br J Oral Maxillofac Surg. 2013;51:667-8.
-
26Coutinho A, FenyoPereira M, Dib LL, Lima ENP. The role of SPECT/CT with (99m) Tc-MDP image fusion to diagnose temporomandibular dysfunction. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101:224-30.
-
27Bittencourt LP, Souza SAL, Magnanini M, Fonseca LMB, Gutfilen B. Verificação da atividade condilar em pacientes com padrão esquelético classe III por intermédio da cintilografia óssea. Radiol Bras. 2005;38:273-7.
-
28Shintaku WH, Venturin JS, Yepes JS. Application of advanced imaging modalities for the diagnosis of metastatic adenocarcinoma of the lungs in the temporomandibular joint. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107: 37-41.
-
29Pharoah M. The prescription of diagnostic images for temporomandibular joint disorders. J Orofac Pain. 1999;13:251-4.
-
30Bas B, Yilmaz N, Gökce E, Akan H. Diagnostic value of ultrasonography in temporomandibular disorders. J Oral Maxillofac Surg. 2011;69:1304-10.
-
31Calderon PDS, Reis KR, Araujo CDRP, Rubo JH, Conti PCR. Ressonância magnética nos desarranjos internos da ATM: sensibilidade e especificidade. Rev Dent Press Ortodon Ortoped Facial. 2008;13:34-9.
-
32Shintaku WH, Venturin JS, Langlais RP, Clark GT. Imaging modalities to access bony tumors and hyperplasic reactions of the temporomandibular joint. J Oral Maxillofac Surg. 2010;68:1911-21.
-
33Liedberg J, Panmekiate S, Petersson A, Rohlin M. Evidencebased evaluation of three imaging methods for the temporomandibular disc. Dentomaxillofac Radiol. 1996;25:234-41.
-
☆
Please cite this article as: Ferreira LA, Grossmann E, Januzzi E, de Paula MVQ, Carvalho ACP. Diagnosis of temporomandibular joint disorders: indication of imaging exams. Braz J Otorhinolaryngol. 2016;82:341-52.
Publication Dates
-
Publication in this collection
May-Jun 2016
History
-
Received
23 Oct 2014 -
Accepted
16 June 2015