Abstract
Introduction
Foreign body in the oral cavity may be asymptomatic for long time and only sometimes it can lead to a typical granulomatous foreign body reaction. Some patients may complain of oral pain and present signs of inflammation with purulent discharge. A granuloma is a distinct, compact microscopic structure composed of epithelioid-shaped macrophages typically surrounded by a rim of lymphocytes and filled with fibroblasts and collagen. Nowadays, the increase of cosmetic invasive procedures such as injection of prosthetic materials in lips and cheeks may lead to unusual forms of inflammatory granulomas.
Objectives
Describe an unusual presentation of a foreign body reaction in the buccal mucosa due to previous injection of cosmetic agent.
Resumed Report
A 74-year-old woman was referred to the Department of Otorhinolaryngology, Head and Neck Surgery to investigate the presence of multiple painless, bilateral nodules in the buccal mucosa, with progressive growth observed during the previous 2months. The histologic results showed a foreign body inflammatory reaction.
Conclusion
Oral granulomatosis lesions represent a challenging diagnosis for clinicians and a biopsy may be necessary. Patients may feel ashamed to report previous aesthetic procedures, and the clinicians must have a proactive approach.
foreign body reaction; granulomatosis; orofacial; differential diagnoses; esthetic surgery
Introduction
The demand for aesthetic surgery has been increasing, and some materials, such as silicone, polymethyl methacrylate, collagen, and hyaluronic acid, are commonly used in plastic surgery.11 Puliyel D, Balouch A, Ram S, Sedghizadeh PP. Foreign body in the oral cavity mimicking a benign connective tissue tumor. Case Rep Dent 2013;2013:369510 22 Jham BC, Nikitakis NG, Scheper MA, Papadimitriou JC, Levy BA, Rivera H. Granulomatous foreign-body reaction involving oral and perioral tissues after injection of biomaterials: a series of 7 cases and review of the literature. J Oral Maxillofac Surg 2009;67(2): 280-285 When used in soft tissues, these materials can stay latent for a long time. Sometimes they may cause chronic inflammatory reaction.33 Manthey DE, Storrow AB, Milbourn JM, Wagner BJ. Ultrasound versus radiography in the detection of softtissue foreign bodies. Ann Emerg Med 1996;28(1):7-9
Granulomatous inflammation of the oral soft and hard tissues is an uncommon occurence.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x Clinically, it can be presented with a local inflammatory reaction that can be associated with purulent discharge.11 Puliyel D, Balouch A, Ram S, Sedghizadeh PP. Foreign body in the oral cavity mimicking a benign connective tissue tumor. Case Rep Dent 2013;2013:369510 Local pain can vary among patients. The incisional biopsy is the exam of choice in the diagnosing process.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x
The objective of this case report is to highlight the clinical presentation of a foreign body reaction in the oral cavity as a late effect of facial plastic procedure.
Cases that present as solid facial swellings should be differentiated especially from tuberculosis, facial erysipelas, South American blastomycosis, angioedema, orofacial granulomatosis, Crohn disease, and sarcoidosis. These diseases are detailed in the Discussion, along with the recent literature about the subject.
Case Report
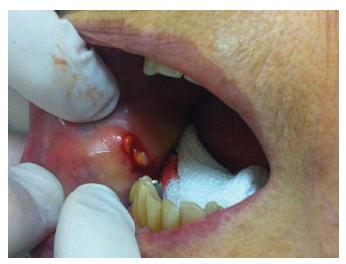
A 74-year-old woman was referred to the otorhinolaryngology department of a tertiary hospital for oral examination. At the patient's first appointment, she complained of the presence of painless hard nodules in the buccal mucosa, bilaterally, with 2 months of evolution. According with patient's report, the hard nodules were more evident during the morning, and they were always accompanied by local edema in the malar region. The nodules diminished in size during the day. Palpation of the oral tissues revealed several small nodules (1 cm diameter each) bilaterally. The nodules were not regularly distributed along the malar region and were spread out in the muscle area. During anamneses, the patient denied any plastic surgery in the past. With the probable diagnosis of deposition disease, a local incisional biopsy was performed (Fig. 1). The biopsy results showed a granulomatous reaction, caused probably by an exogenous foreign body (Fig. 2 3).
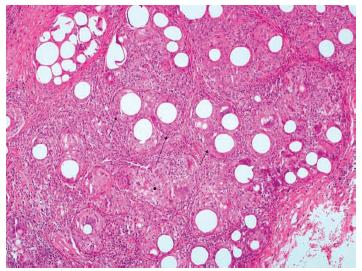
Histopathologic view (hematoxylin and eosin 10 × ) showing epithelioid-shaped macrophages surrounded by a rim of lymphocytes (full arrows), filled with fibroblasts and collagen (arrow with ball head).
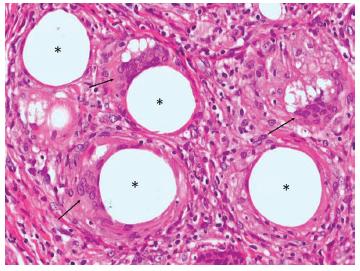
Histopathologic view (hematoxylin and eosin 40 × ): multinucleated giant cells with haphazardly/peripherally nuclei shape (arrows), associated with areas without substance, indicating foreign body particles (*).
To determine the patient's past medical history, a slide review was requested, which confirmed the previous histopathologic results. The confirmation of the previous facial filling was stated by the patient's caregiver, who said that the patient had facial plastic surgery 20 years before in a private clinic, which explained the lack of this information on the patient's medical records in our hospital.
Discussion
Foreign body inflammatory reaction can appear from a few months to several years after a surgical procedure.55 Silveira VAS, de Carmo ED, Colombo CED, Cavalcante ASR, Carvalho YR. Intraosseous foreign-body granuloma in the mandible subsequent to a 20-year-old work-related accident. Med Oral Patol Oral Cir Bucal 2008;13(10):E657-E660 It may result from local trauma or it may be iatrogenic.66 Aregbesola SB, Ugboko VI. Unusual foreign bodies in the orofacial soft tissue spaces: a report of three cases. Niger J Clin Pract 2013; 16(3):381-385 Because of the increasing number of aesthetic procedures and the use of different biomaterials, foreign body inflammatory reaction may become more frequent. These reactions show a female predilection, probably reflecting the fact that women seek cosmetic care more often than men.22 Jham BC, Nikitakis NG, Scheper MA, Papadimitriou JC, Levy BA, Rivera H. Granulomatous foreign-body reaction involving oral and perioral tissues after injection of biomaterials: a series of 7 cases and review of the literature. J Oral Maxillofac Surg 2009;67(2): 280-285
A granuloma is a distinct, compact microscopic structure composed of epithelioid-shaped macrophages typically surrounded by a rim of lymphocytes and filled with fibroblasts and collagen. Multinucleated giant cells are also present and form from coalescing epithelioid macrophages.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x
Foreign materials are composed of particles that are usually too large to be phagocytosed and are the most common source of granulomatous inflammation in the oral cavity.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x They do not evoke an immune response because they are typically inert, but there is a macrophage recruitment to eliminate the material. The identification of the foreign material is not easy and sometimes it is necessary to use polarized light to visualize them.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x
Because of the relatively nonspecific clinical findings associated with a variety of granulomatous diseases, a microscopic diagnosis of granulomatous inflammation often presents a diagnostic dilemma.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x The differential diagnosis may include a broad range of conditions. Cases that present as solid facial swellings should be differentiated especially from tuberculosis, facial erysipelas, South American blastomycosis, angioedema, orofacial granulomatosis, Crohn disease, and sarcoidosis. A clinical presentation of multiple nodules should be distinguished from Heck disease, neurofibromatosis, amyloidosis, multiple endocrine neoplasia type 2b syndrome, and lipoid proteinosis.22 Jham BC, Nikitakis NG, Scheper MA, Papadimitriou JC, Levy BA, Rivera H. Granulomatous foreign-body reaction involving oral and perioral tissues after injection of biomaterials: a series of 7 cases and review of the literature. J Oral Maxillofac Surg 2009;67(2): 280-285 44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x 77 González-García R, Rodríguez-Campo FJ, Román-Romero L, et al. Migration of aluminum silicate from the oral cavity to the submandibular region, with foreign body granuloma formation: report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;104:e45-e49
Orofacial granulomatosis is a nonspecific, descriptive term encompassing a variety of conditions that exhibit similar clinical and microscopic features. It is used as a clinical diagnosis of exclusion, and its exact cause remains unknown. The most consistent finding is a persistent, painless swelling of the orofacial tissues, with vertical fissure of the lips the most frequent involvement.44 Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x
The early diagnostic and detection of foreign bodies are based at the anamnesis and physical examination.55 Silveira VAS, de Carmo ED, Colombo CED, Cavalcante ASR, Carvalho YR. Intraosseous foreign-body granuloma in the mandible subsequent to a 20-year-old work-related accident. Med Oral Patol Oral Cir Bucal 2008;13(10):E657-E660 In long-term follow-up, patients may present with oral pain and signs of inflammation with purulent discharge, granulomas, and migration of material.11 Puliyel D, Balouch A, Ram S, Sedghizadeh PP. Foreign body in the oral cavity mimicking a benign connective tissue tumor. Case Rep Dent 2013;2013:369510 22 Jham BC, Nikitakis NG, Scheper MA, Papadimitriou JC, Levy BA, Rivera H. Granulomatous foreign-body reaction involving oral and perioral tissues after injection of biomaterials: a series of 7 cases and review of the literature. J Oral Maxillofac Surg 2009;67(2): 280-285 Migration of foreign particles is a rarely reported phenomenon that could be explained by three mechanisms: hematogenous spread of particles, lymphatic injection, and phagocytosis of the particles by macrophages that travel through the lymphatic system to the local lymph nodes.77 González-García R, Rodríguez-Campo FJ, Román-Romero L, et al. Migration of aluminum silicate from the oral cavity to the submandibular region, with foreign body granuloma formation: report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;104:e45-e49 Reports of asymptomatic foreign bodies affecting the oral cavity are rarely reported in the literature.11 Puliyel D, Balouch A, Ram S, Sedghizadeh PP. Foreign body in the oral cavity mimicking a benign connective tissue tumor. Case Rep Dent 2013;2013:369510 22 Jham BC, Nikitakis NG, Scheper MA, Papadimitriou JC, Levy BA, Rivera H. Granulomatous foreign-body reaction involving oral and perioral tissues after injection of biomaterials: a series of 7 cases and review of the literature. J Oral Maxillofac Surg 2009;67(2): 280-285
In the case reported here, the patient presented nodular lesions without pain or discharge and denied previous plastic procedures at the first visit. The oral examination was inconclusive. Imaging exams are helpful, with routine radiography being the preferred imaging modality for the initial workup. However, several types of soft tissue foreign bodies are not radiopaque and therefore remain undetected. Sonography is playing an increasing role in the diagnostic process and for accurate localization of all types of soft tissue foreign bodies, minimizing surgical exploration or, alternatively, guiding percutaneous removal of foreign body.88 Horton LK, Jacobson JA, Powell A, Fessell DP, Hayes CW. Sonography and radiography of soft-tissue foreign bodies. AJR Am J Roentgenol 2001;176(5):1155-1159
Surgical excision has been reported as the preferred option for well-circumscribed nodular lesions.66 Aregbesola SB, Ugboko VI. Unusual foreign bodies in the orofacial soft tissue spaces: a report of three cases. Niger J Clin Pract 2013; 16(3):381-385 77 González-García R, Rodríguez-Campo FJ, Román-Romero L, et al. Migration of aluminum silicate from the oral cavity to the submandibular region, with foreign body granuloma formation: report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;104:e45-e49 Surgery for widespread lesions remains controversial. Some authors argue that complete eradication of the granulomatous tissue is highly improbable and that surgery may lead to scarring and fistulas. In the other hand, González-García et al argue that surgery combined with corticoids is the preferred option for these cases.77 González-García R, Rodríguez-Campo FJ, Román-Romero L, et al. Migration of aluminum silicate from the oral cavity to the submandibular region, with foreign body granuloma formation: report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;104:e45-e49
Final Comments
Foreign body reaction as a late effect after plastic surgery may be very uncommon. However, when it occurs, biopsy is the standard diagnostic procedure, along with a good anamneses process and past medical history.
References
-
1Puliyel D, Balouch A, Ram S, Sedghizadeh PP. Foreign body in the oral cavity mimicking a benign connective tissue tumor. Case Rep Dent 2013;2013:369510
-
2Jham BC, Nikitakis NG, Scheper MA, Papadimitriou JC, Levy BA, Rivera H. Granulomatous foreign-body reaction involving oral and perioral tissues after injection of biomaterials: a series of 7 cases and review of the literature. J Oral Maxillofac Surg 2009;67(2): 280-285
-
3Manthey DE, Storrow AB, Milbourn JM, Wagner BJ. Ultrasound versus radiography in the detection of softtissue foreign bodies. Ann Emerg Med 1996;28(1):7-9
-
4Alawi F. Granulomatous diseases of the oral tissues: differential diagnosis and update. Dent Clin North Am 2005;49(1):203-221, x
-
5Silveira VAS, de Carmo ED, Colombo CED, Cavalcante ASR, Carvalho YR. Intraosseous foreign-body granuloma in the mandible subsequent to a 20-year-old work-related accident. Med Oral Patol Oral Cir Bucal 2008;13(10):E657-E660
-
6Aregbesola SB, Ugboko VI. Unusual foreign bodies in the orofacial soft tissue spaces: a report of three cases. Niger J Clin Pract 2013; 16(3):381-385
-
7González-García R, Rodríguez-Campo FJ, Román-Romero L, et al. Migration of aluminum silicate from the oral cavity to the submandibular region, with foreign body granuloma formation: report of a case. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 2007;104:e45-e49
-
8Horton LK, Jacobson JA, Powell A, Fessell DP, Hayes CW. Sonography and radiography of soft-tissue foreign bodies. AJR Am J Roentgenol 2001;176(5):1155-1159
Publication Dates
-
Publication in this collection
Oct-Dec 2015
History
-
Received
21 Nov 2014 -
Accepted
26 Jan 2015