Abstracts
The objective of this study was to prepare and evaluate chronotherapeutic drug delivery systems (ChrDDs) of torsemide. Compression coated tablets (CCT) containing torsemide in the core tablet were prepared by the compression coating technique with different grades of polyethylene oxide (PEO WSR 301 & 1105). The optimized formulations were characterised for tabletting parameters and drug polymer interaction by Fourier-Transform Infrared Spectroscopy (FTIR).The hardness of all the CCT using PEO WSR 301 & PEO WSR 1105 were in the range 6-8 kg/cm² & 5.5 to 7 kg/cm² respectively. Their friability values were <0.3%. All the CCT showed a clear lag time but finalized as per the predetermined lag time. As the amount of PEO was increased in the outer layer the drug released was delayed. The drug content of all the CCT was >99%. The FTIR studies showed no interaction throughout the process of development. Formulations of F7 and of P7 were considered optimized formulations since they yielded a predetermined lag time of 6h before burst release. Hence, these formulations can be exploited to achieve chronotherapeutic drug delivery systems of Torsemide for the treatment of hypertension at the time the patient needs it.
Torsemide; Chronotherapeutic drug; Polyethylene Oxides; Compression coated tablets; Predetermined lag time
O objetivo deste estudo foi preparar e avaliar sistemas cronoterapêuticos de liberação de fármacos (ChrDDs) de torsemida. Comprimidos revestidos por compressão (CCT) contendo torsemida no (núcleo) foram preparados pela técnica de revestimento por compressão, com diferentes categorias de óxido de polietileno (PEO WSR 301 & 1105). As formulações otimizadas foram caracterizadas por parâmetros de compressão e interação fármaco polímero por Infravermelho com Transformada de Fourier (FTIR). A dureza dos CCT utilizando PEO WSR 301 e PEO WSR 1105 foi entre 6-8 kg/cm² e 5,5 a 7 kg/cm², respectivamente. Os valores de friabilidade foram <0,3%. Todos os CCT mostraram claro tempo de retardo, mas finalizaram de acordo com o tempo de retardo pré-determinado. À medida que a quantidade de PEO aumentava na camada mais externa, a liberação do fármaco era retardada. O teor de fármaco em todos os CCT foi >99%. Os estudos de FTIR mostraram que não h[a interação durante o processo de desenvolvimento. As formulações F7 e P7 foram consideradas otimizadas, uma vez que resultaram em tempo de retardo pré-determinado de 6 h antes da liberação por meio de explosão. Dessa forma, estas formulações podem ser exploradas para se obter sistemas de liberação.
Torsemida; Sistemas de liberação cronoterapêutica; Óxidos de polietileno; Comprimidos cobertos por compressão; Tempo de retardo pré-determinado
ARTICLE
Development and evaluation of a chronotherapeutic drug delivery system of torsemide
Songa Ambedkar Sunil* * Correspondence: S. A. Sunil. University College of Pharmaceutical Sciences, Andhra University, Visakhapatnam-530003, India. E-mail: sunilsonga@gmail.com , I; Nali Sreenivasa RaoI; Meka Venkata SrikanthI; Michael Uwumagbe UhumwanghoII; Kommana Srinivas Phani KumarI; Kolaplli Venkata Ramana MurthyI
IUniversity College of Pharmaceutical Sciences, Andhra University, India
IIDepartment of Pharmaceutics and Pharmaceutical Technology, Faculty of Pharmacy, University of Benin, Nigeria
ABSTRACT
The objective of this study was to prepare and evaluate chronotherapeutic drug delivery systems (ChrDDs) of torsemide. Compression coated tablets (CCT) containing torsemide in the core tablet were prepared by the compression coating technique with different grades of polyethylene oxide (PEO WSR 301 & 1105). The optimized formulations were characterised for tabletting parameters and drug polymer interaction by Fourier-Transform Infrared Spectroscopy (FTIR).The hardness of all the CCT using PEO WSR 301 & PEO WSR 1105 were in the range 6-8 kg/cm2 & 5.5 to 7 kg/cm2 respectively. Their friability values were <0.3%. All the CCT showed a clear lag time but finalized as per the predetermined lag time. As the amount of PEO was increased in the outer layer the drug released was delayed. The drug content of all the CCT was >99%. The FTIR studies showed no interaction throughout the process of development. Formulations of F7 and of P7 were considered optimized formulations since they yielded a predetermined lag time of 6h before burst release. Hence, these formulations can be exploited to achieve chronotherapeutic drug delivery systems of Torsemide for the treatment of hypertension at the time the patient needs it.
Uniterms: Torsemide. Chronotherapeutic drug/delivery systems. Polyethylene Oxides. Compression coated tablets. Predetermined lag time.
RESUMO
O objetivo deste estudo foi preparar e avaliar sistemas cronoterapêuticos de liberação de fármacos (ChrDDs) de torsemida. Comprimidos revestidos por compressão (CCT) contendo torsemida no (núcleo) foram preparados pela técnica de revestimento por compressão, com diferentes categorias de óxido de polietileno (PEO WSR 301 & 1105). As formulações otimizadas foram caracterizadas por parâmetros de compressão e interação fármaco polímero por Infravermelho com Transformada de Fourier (FTIR). A dureza dos CCT utilizando PEO WSR 301 e PEO WSR 1105 foi entre 6-8 kg/cm2 e 5,5 a 7 kg/cm2, respectivamente. Os valores de friabilidade foram <0,3%. Todos os CCT mostraram claro tempo de retardo, mas finalizaram de acordo com o tempo de retardo pré-determinado. À medida que a quantidade de PEO aumentava na camada mais externa, a liberação do fármaco era retardada. O teor de fármaco em todos os CCT foi >99%. Os estudos de FTIR mostraram que não h[a interação durante o processo de desenvolvimento. As formulações F7 e P7 foram consideradas otimizadas, uma vez que resultaram em tempo de retardo pré-determinado de 6 h antes da liberação por meio de explosão. Dessa forma, estas formulações podem ser exploradas para se obter sistemas de liberação.
Unitermos: Torsemida. Sistemas de liberação cronoterapêutica/liberação de fármacos. Óxidos de polietileno. Comprimidos cobertos por compressão. Tempo de retardo pré-determinado.
INTRODUCTION
Hypertension is a chronic disorder and the symptoms of the disease are pronounced predominantly during the early hours of the morning (Ura et al., 1992). The treatment of this disease condition occurring in the early hours is not convenient by using the existing marketed conventional immediate release dosage form. Hence, a Chronotherapeutic drug delivery system (ChrDDs) with a predetermined lag time may be useful for such patients as the drug is released at a predetermined time and hence the maximum concentration (Cmax) of the drug can be reached when the symptoms of the disease are worse to fatal. It will be more helpful if antihypertensive patients take the medication before bed time to overcome a high level of discomfort in the morning (Smolensky et al.,1997; Efentakis et al.,2006). It is also thought that ChrDDs may be a successful tool for effective chronopharmacotherapy because of their unique drug release properties, which could take advantage of circadian rhythms in physiologic and pathologic conditions (White et al., 1992). An ideal oral ChrDDs would overcome the problem of administering the drugs frequently. The advantages of ChrDDs include convenience, reduced dosing frequency, reduced toxicity and decreased total required therapeutic or instantaneous preventive drug dose level matching exactly the biological and physiological needs to treat the disease at each point in time. Ultimately, this should lead to improved patient compliance.
Compression-coated tablets (CCT) are dosage forms that consist of an inner core immediate release tablet embedded in an outer layer compartment, which contains either a hydrophilic, hydrophobic or a mixture of both polymers. The outer layer dissolves or disintegrates slowly to release the drug after a predetermined lag time. The advantage of this technique is that it is simply achieved by minor modification of existing equipment, inexpensive, is capable of physically separating two incompatible drugs within the same dosage form, allows taste masking of bitter drugs and is not hazardous to the environment, since it does not require the use of organic solvent (Hadfield et al., 1987; Oth et al., 1993).
Previously, Conte et al., 1993 formulated a novel dry-coated device for the release of drug after a programmable period of time. It was intended to be used mainly in the therapy of those diseases which depend on circadian rhythms. CCT of aminophylline using crystalline cellulose and polyethylene glycol as coating polymers in the outer shell for timed-release dosage forms to achieve chronopharmacotherapy for asthma has also been developed (Watanabe et al., 2002). Recently, Sawada et al. (2004) also designed a CCT of nifedipine by using the dry coating technique with different polyethylene oxide-polyethylene glycol mixtures. Each formulation showed a clear lag period before the drug release. This was also followed by sustained drug release lasting up to 24 h.
Torsemide is a pyridine-sulfonylurea type loop diuretic indicated for the treatment of hypertension and edema in congestive heart failure. It may be used alone or in combination with thiazide diuretics. Its chemical name is N-[(isopropylamino)carbonyl]-4-[(3-methylphenyl)amino]pyridine-3-sulfonamide with a molecular formula of C16H20N4O3 S (Groop et al.,1989.). Its oral bioavailability is around 75-89% with a biologic half-life of about 3.5 h (Martindale, 2005).The usual initial dose is 5 mg once daily which may be increased to 10, 20 and 100 mg once daily. ChrDDs are designed such that the Cmax of the drug is reached at the maximum intensity of disease condition. Hence, the purpose of this study was to design an optimised ChrDDs of Torsemide with different grades and ratios of Polyethylene Oxide water soluble resins (PEO WSR) including PEO WSR 301 and PEO WSR 1105 to obtain the predetermined lag time of 6 hrs, after which the drug is released. PEO WSR is as a nonionic homopolymer of ethylene oxide, represented by the formula (CH2CH2O)n, where n represents the average number of oxyethylene groups. It may contain up to 3% silicon dioxide or suitable antioxidant. It is soluble in water as well as in a number of common organic solvents such as acetonitrile, chloroform, and methylene chloride. Moreover, it is insoluble in aliphatic hydrocarbons, ethylene glycol, and most alcohols.
MATERIAL AND METHODS
Materials
Torsemide, different grades of polyethylene oxides, directly compressible lactose (DCL 21), sodium starch glycolate, crospovidone, sodium croscarmellose, povidone K 30 and poloxamer 188 were Gift samples from Macleods Pvt.Ltd., Mumbai, India. Avicel pH 101 was obtained as a gift sample from FMC biopolymer and magnesium stearate was purchased from S.D. Fine Chemicals Ltd., Mumbai. All other reagents used were of analytical grade.
Methods
Preparation of an optimised core tablet
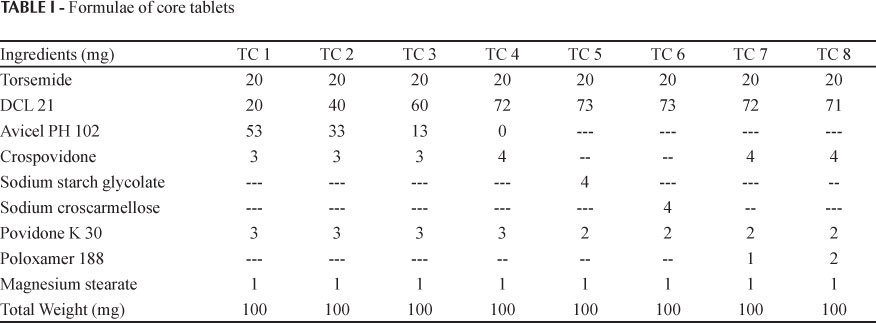
Based on preliminary studies in our laboratory, an optimized immediate release core tablet was developed by using varying concentrations and different diluents, disintegrant and binder. The drug, diluents, disintegrant and binder were weighed for a batch of 100 tablets as per formulae given in Table I. These were then passed through a # 40 (420 µm) sieve, transferred to a poly bag and blended for 5 minutes. Magnesium stearate passed through a # 60 (250 µm) sieve was added to the homogeneous mixture and blended for 2 minutes. The resulting blend was compressed with a rotary compression machine (Model Riddhi, Ahmedabad) to form a bi convex tablet with a diameter of 6mm to a hardness of 2.5±0.2 kg/cm2. The weights of the tablets were 100±0.8 mg. The batch that gave a comparable release profile with the marketed tablet (TIDE 20) was considered an optimised core tablet.
Preparation of Timed-release compression-coated tablets (CCT)
The required polymer (PEO WSR 301 or PEO WSR 1105) was weighed for a batch of 100 tablets as per formulae given in Table II and III and passed through a # 40 sieve and transferred to a poly bag. Magnesium stearate passed through # 60 sieve was added to the above mixture and blended for 2 minutes for lubrication of the blend. Half the amount of the thoroughly mixed homogeneous polymer blend was placed in the die to make a powder bed. The core tablet previously developed and optimised was carefully placed at the centre on the polymer bed and the remaining half of the homogeneous polymer blend was filled into the die. The contents were then compressed using a rotary compression machine (Model Riddhi, Ahmedabad) to form a bi convex tablet with a diameter of 9 mm & 12 mm depending on the weight.

Physicochemical evaluation of tablets
Determination of tablet hardness and friability (Banker et al., 1991; Marshall et al., 1991)
The fracture loads (kg) of ten tablets were determined individually with a Monsanto hardness tester. The mean values of the fracture loads were recorded. The friability test is to evaluate the ability of the tablet to withstand abrasion in packaging, handling and shipping. Tablets were taken, equivalent to 6.5 gm which was denoted as initial weight (w1), placed in friabilitator (Roche) and allowed to rotate at 25 rpm for 4 min. After four minutes of this treatment or 100 revolutions, the tablets were weighed and the result (w2) compared with the initial weight. The loss due to abrasion is a measure of tablet friability. The % friability was calculated by using the equation given below.
% Friability = (w1 - w2) x 100/ w1
Drug Content
In order to determine the content of Torsemide present in the tablets, five tablets were weighed and crushed to fine powder. Powder equivalent to 20 mg of drug was weighed and transferred into a 100 mL volumetric flask and diluted to 100 mL with 6.8 phosphate buffer. The resulting solution was filtered with Whatman No. 3 filter paper. The sample was suitably diluted and analyzed for drug content by using UV-spectrophotometer (Elico SL 210) at 285.5 nm.
In vitro drug release studies
The prepared core and compression coated tablets were subjected to in-vitro drug release studies in suitable dissolution media for 60 min and 8-12 h respectively to assess their ability to provide the desired release. The in-vitro drug release studies were performed using a USP Type I dissolution apparatus. The dissolution medium for the core tablets was 900 mL of 6.8 pH phosphate buffer for 60 min and for compression coated tablets was 0.1 N HCl for the first 2 h followed by 6.8 pH phosphate buffer for the remaining period. As the maximum drug release was targeted for a predetermined lag time of 6 h, after about 6 h the tablet would be in the region of the small intestine. Since the majority of drugs are well absorbed from this region, whose pH is 6.8, the 6.8 pH phosphate buffer was selected as the dissolution media. The temperature of dissolution medium was maintained at 37 ± 0.5 °C. The tablet was introduced into the basket, and then lowered such that the lower end of the basket was 25 mm above the base of the beaker which was set to rotate at 100 rpm. In all experiments, an aliquot of 5 mL sample of the leaching fluid was withdrawn at predetermined time intervals with a syringe fitted with a filter and replaced with an equal volume of drug-free dissolution fluid in order to maintain the sink condition. The samples were filtered and analyzed spectrophotometrically at 285.5 nm by using an Elico SL 210 UV-Visible double beam spectrophotometer (Elico, India). The amounts released were expressed as a percentage of the drug content in each dissolution medium. The dissolution test was carried out in triplicate and the mean results were reported.
Fourier Transform Infrared Spectroscopy (FTIR)
The FTIR spectrum of the different samples were recorded on an Infra Red spectrometer (Nicolet Magna 4R 560, MN, USA) using potassium bromide discs prepared from powdered samples. The spectrum was recorded in the region of 4000 to 400 cm-1.
RESULTS AND DISCUSSION
Physicochemical parameters of the core tablets
Core tablets were evaluated for physicochemical parameters including hardness, friability, disintegration and drug content. Hardness was in the range 2-4 kg/cm2, friability was <0.45%, disintegration (<30 sec) and drug content was >99.0%. Results are given in Table IV.
Physicochemical parameters of CCT
CCT formulations (PEO WSR 301 and 1105) were evaluated for their physicochemical parameters including hardness, friability and drug content. The tablet hardness values for formulations with PEO WSR 301 as the polymer was between 6 and 8 kg/cm2 while those prepared with PEO WSR 1105 ranged from 5.5 to 7.0 kg/cm2. The slight difference in the hardness might be attributable to the variation in tablet weight. However, these values did not vary significantly (p > 0.05). The percentage friability of all the formulations was <0.30% while the content uniformity of the tablets was >99% which indicates uniform distribution of drug in the tablets of each formulation. However, all of these values were within acceptable compendial limits. Results are given in Tables V and VI.
In vitro drug release study of Core tablet
The prepared core tablets were subjected to in vitro drug release studies in suitable dissolution media for 60 min to assess their drug release. The drug release studies were performed on an USP Type I dissolution apparatus using 900 ml of 6.8 pH phosphate buffer. The dissolution medium was kept in a thermostatically controlled water bath, maintained at 37 ± 0.5 º C. The Basket was lowered so that the lower end of the stirrer was 25 mm above the base of the beaker. The tablet was then introduced into the dissolution jar and the basket was rotated at 100 rpm. All the dissolution experiments on tablets were done in triplicate. Aliquots of 5 mL of sample were withdrawn at predetermined time intervals and replaced with an equal volume of the fresh dissolution medium to maintain the total volume constant. The samples were filtered and analyzed spectrophotometrically at 285.5 nm for the drug release. The correction factor was included in the calculation for estimation of the concentration of dissolved drug in the dissolution media. Tablets were developed in such a way that the tablets had a release that matched the marketed tablet. TC 1-7 batches were developed using different diluents and disintegrants either alone or in combination. TC 8 showed a release profile similar to that of the marketed tablet (Tide 20). 2% poloxamer 188 was used in the final formulation to achieve a release within 15 min as shown in Figure 1.
ChrDDs formulations were designed to ensure the drug is released at a predetermined lag time so that the burst release of the drug could take advantage of circadian rhythms in physiologic and pathologic conditions (White et al., 1992). This ultimately reduces toxicity and improves patient compliance. Hence, it is important that ChrDDs formulations release their drug at the time needed. Previously, (Sawada et al., 2003) reported that CCT with a greater core erosion ratio, release their drug gradually after the predetermined lag time until they have completely dissolved. In order to evaluate the performance of these formulations so as to release its medication at a predetermined lag time of 6 h, different grades and concentration of polyethylene oxide (i:e PEO WSR 301 and 1105) were used as an outer coating agent. PEO is a gel-forming polymer used to enhance water penetration into the CCT. All the dissolution experiments were done in triplicate. F 1 - 3 batches were taken by using PEO WSR 301 with core: polymer at the following ratios1:1.6, 1:1.8 and 1:2 while magnesium stearate (1.5%) was added as a lubricant in all the formulations. The dissolution profiles of torsemide CCT for batch F 1-3 is shown in Figure 2. It was observed that the lag time increased as the concentration of the PEO in the outer coat increased. For instance, formulation F 1 had a lag time of 1.5 hrs before burst release. On the other hand, F 2 and 3 had lag times of 4 and 5 hrs, respectively. It is well known that tablet hardness can affect the release rate of a drug (Capan, 1965). Katikaneni et al. (1995) reported that increase in tablet hardness is accompanied by a decrease in release rate, due to a decrease in tablet porosity. However, since there was no significant change in the tablet hardness of the all the CCT formulations with increased concentrations of the PEO, the lag time of torsemide before burst release might be attributable to the high gel-forming ability of the PEO with increase in concentration. Given the targeted predetermined lag time was 6 hrs, further batches were produced by increasing the concentrations of the PEO WSR 301. F 4 - 6 batches were produced by using PEO WSR 301 with core: polymer at the ratios 1:2.2, 1:2.4 and 1:2.6. The dissolution profile of this batch is depicted in Figure 2. The result showed that batch 4, 5 and 6 had burst releases of 7, 8 and 9 hrs respectively. Hence, the next batch F 7 was produced with a concentration of PEO WSR 301 between F 3 & 4. F 7 and was formulated with a 1:2.1 core: polymer ratio. This resulted in drug release with a predetermined lag time of 6 hrs and maximum release in 7 hrs. Hence, F 7 was considered to be the optimized formulation as the desired pre determined lag time was obtained.
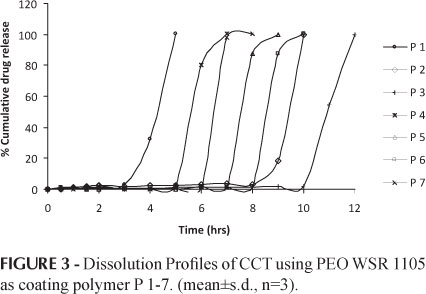
In batches P 1-3, PEO WSR 1105 polymer had core: polymer ratios of 1:4, 1:5 and 1:6. The dissolution profiles of torsemide CCT for batches P 1-3 is shown in Figure 3. Magnesium stearate (1.5%) was also incorporated as the lubricant. The results indicated that that the burst release of the drug occurred at 5, 10 and 12 hrs, respectively. As the predetermined lag time targeted was 6 hrs, further batches were also produced by changing the concentrations of the polymer to suit the drug release for the predetermined lag time of 6 hrs. Hence, P 4 - 6 batches were produced by using PEO WSR 1105 with core: polymer ratios of 1:4.3, 1:4.5 and 1:4.7. The results indicated a predetermined lag time of drug release of 6, 8 and 9 hrs for formulation 4, 5 and 6, respectively. Hence, to achieve the targeted lag time the amount of polymer was reduced in P 7 and was formulated with a core: polymer ratio of 1:4.4. The results indicated that all the physical parameters were within limits and the drug was released within 7 hrs with a predetermined lag time of 6 hrs as shown in Figure 3.
FTIR analysis
FTIR analysis of torsemide individually and in combination with other ingredients of core tablets and CCT was investigated to identify any chemical interaction between the added excipients and torsemide. The major peaks for the pure drug were observed at 1697.42.31cm-1 (C= N stretch), 1282.15 cm-1 (C-N stretch) and 3279.94 cm-1 (presence of hetero atoms). The presence of PEO WSR 301 and PEO WSR 1105 did not produce any major shift in peak characteristics of Torsemide as shown in Figure 4 and 5. This indicates that there was no chemical interaction between drug and the excipients used in the study.
CONCLUSION
In the present investigation, torsemide was selected as the drug since the symptoms of hypertension are more prevalent during the early hours of the morning and because there is no chronotherapeutic formulation presently available on the market where the immediate release dosage form cannot fulfill the needs of drug delivery at the required time. Optimized PEO WSR 301 and PEO WSR 1105 coated tablets produced the desired predetermined lag time, and all the physiochemical parameters were well within limits. Of these formulations, PEO WSR 301 obtained the predetermined lag time with a lower concentration of polymer, as the viscosity and molecular weight of PEO WSR 301(4000000 & 1650 -5500 mPas (1% sol)) is higher than that of PEO WSR 1105 (900000 & 8800 - 17600 mPas (5% sol)). Hence, these can be exploited to achieve ChrDDs of Torsemide for the treatment of hypertension at the time the patient needs it.
ACKNOWLEDGEMENTS
The author would like to thank the University Grants Commission (UGC), India, for providing the fellowship to carry out the research work. One of the authors S.A.Sunil is thankful to G.S.Sharma, B. Janaki Ram and S.Sirisha for providing valuable information during the research work.
Received for publication on 2nd October 2010
Accepted for publication on 21st February 2011
- CAPAN, Y. Influence of technological factors on formulation of sustained release tablets. Dev. Ind. Pharm., v.15, p.927-956, 1989.
- CONTE, U.; MAGGI, L.; TORRE, M. L.; GIUNCHEDI, P. L. A.; MANNA, A. Press-coated tablets for time-programmed release of drugs. Biomaterials, v.14, p.1017-1023, 1993.
- EFENTAKIS, M.; KOLIGLIATI, S.; VLACHOU M. Design and evaluation of a dry coated drug delivery system with an impermeable cup, swellable top layer and pulsatile release. Int. J. Pharm, v.311, p.147-156, 2006.
- GROOP, L.C.; LUZI, L.; DE FRANZO, R.A.; MELANDER, A. Hyperglycemia and absorption of sulfonylurea drug. Lancet, v.15, p.12-30, 1989.
- HADFIELD, P.J. D.; HOLMES, S.; YARWOOD, R. J. The potential use of compression coating in the blinding of clinical trial supplies. Drug. Dev. Ind. Pharm, v.13, p.877-1190, 1987.
- KATIKANENI, P.R.; UPADRASHTA, S.M.; NEAU, S.H.; MITRA, A.K. Ethylcellulose matrix controlled release tablets of a water-soluble drug. Int. J. Pharm, v.123, p.119-125, 1995.
- LACHMAN, L.; LIEBERMAN, H. A.; KANIG, J. L. The theory and practice of industrial pharmacy 3.ed. Bombay: Verghese Publishing House, 1991. p.88, p.297
- MARTINDALE, The complete drug reference London: Pharmaceutical Press, 2005. v.34, p.919-920, 1015.
- OTH, M.; SCOYER, R.; FRANZ, M. ARTHROTEC Part I: Conception of a product combining Misoprotol 200 mcg and EC Diclofenac Sodium 50 mg. J. Pharm. Belg, v.48, p.153,1993.
- SAWADA, T.; HIROMU, K.; HIROSHI, N.; KAZUHIRO, S.; MASAHIRO, H. Time-release compression-coated core tablet containing nifedipine for chronopharmacotherapy, Int. J. Pharm, v.280, p.103-111, 2004.
- SMOLENSKY, M.H.; LABREQUE, G. Chronotherapeutics. Pharm. News, v.2, p.10-16. 1997.
- SAWADA, T.; SAKO, K.; FUKUI, M.; YOKOHAMA, S.; HAYASHI, M. A new index the core erosion ratio of compression-coated timed-release tablets predicts the bioavailability of acetaminophen. Int. J. Pharm., v.265, p.55-63, 2003.
- URA, J.; SHIRACHI, D.; FERRILL, M. The chronotherapeutic approach to pharmaceutical treatment. California Pharmacist, v.23, p.46-53, 1992.
- WATANABE, Y.; MUKAI, B.; KAWAMURA, K.; ISHIKAWA, T.; NAMIKI, M.; UTOGUCHI, N.; FUJII, M. Preparation and evaluation of press-coated aminophylline tablet using crystalline cellulose and polyethylene glycol in the outer shell for timed-release dosage forms. Yakugaku Zasshi, v.122, p..157-162, 2002.
- WHITE, W.B.; BLACK, H.R.; WEBER, M.A.; ELLIOTT, W.J.; BRYZINSKI, B.; FAKOUHI, T.D. Comparison of effects of controlled onset extended release verapamil at bedtime and nifedipine gastrointestinal therapeutic system on arising on early morning blood pressure, heart rate, and the heart rate-blood. Am. J. Cardiol., v.81, p.424-31, 1998.
Publication Dates
-
Publication in this collection
24 Oct 2011 -
Date of issue
Sept 2011
History
-
Received
02 Oct 2010 -
Accepted
21 Feb 2011