INTERVIEW
An interview with Hugo De Clerck
• Hugo De Clerck is a graduate of the Rijksuniversiteit Gent's orthodontic program, he received his PhD in 1986 and he maintains a private practice in Brussels. He received the European Research Essay Award in 1988. He has been Professor and Chairperson of the Department of Orthodontics at the Université Catholique de Louvain from 1989 to 2006. Currently he is Adjunct Professor at the University of North Carolina at Chapel Hill. He is the former President of the Belgian Orthodontic Society and Fellow of the Royal College of Surgeons of England. His main research interests are in skeletal anchorage, biomechanics and orthopedics. He lectured extensively on these topics throughout the world.
There are rare moments in which one can be present in a revolution, a paradigm shift or a promising discovery. If we place this fact into our professional universe, chances are even smaller. Faced with a novelty, we may note optimistic reactions by some, and skeptical by others. The optimists are avid to learn and use the novelty, desiring to offer comfort to those they can be of help. On the other hand, the skeptical, suspiciously, prefer that the optimistic try first, make their mistakes first, so that, afterwards it is worthy to leave their comfort zone if possible, while the new is not yet old. If you are an optimist or a skeptical, one thing I guarantee: It is impossible to read this interview without becoming a witness of orthodontic history.
Bruno Furquim
What are the treatment effects on the maxilla produced by your approach to Class III treatment? How does this approach differ from the use of a face mask combined with a bonded palatal expansion device? (James McNamara)
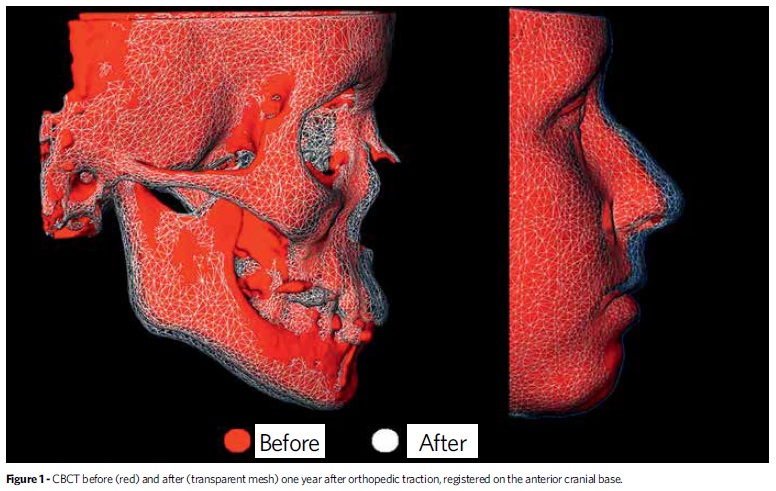
Bollard miniplates are inserted on the left and right maxillary buttresses and between the canine and lateral incisor on both sides of the mandible. Intermaxillary elastics are fixed between the upper and lower plates 24 hours a day. The application of a continuous forward traction on the maxilla results in a stretching of the fibers in the sutures and stimulation of bone apposition. Because of the complex interdigitations in the zygomatico-maxillary suture the resistance against the opening of this suture is greater than when separating the zygomatico-temporal and zygomatico-frontal sutures. This may explain why both halves of the maxilla and the left and right zygoma move forward as one unit. This has been demonstrated by the superimposition of a CBCT from the start of orthopedic traction and another after one year, registered on the anterior cranial base. The effects on the pterygo-maxillary complex are difficult to be evaluated in 3D images. However there is some evidence that supports the hypothesis that the weak transverse palatine suture, rather than the tight connection between the pyramidal process of the palatine bone and the pterygoid plates of the sphenoid bone, may be affected by the orthopedic traction. This was also observed in several maxillary protraction studies on monkeys in the late 70's.
In a sample of 25 consecutive patients treated with bone-anchored maxillary protraction, the maxilla was displaced 4 mm more forward, compared to a control group of untreated Class III patients. Also compared to a matched sample of patients treated with face mask after rapid maxillary expansion (RME), the amount of forward displacement/modeling of the maxilla was significantly greater. The continuous elastic traction may result in more bone formation than the intermittent forces generated by a face mask. Another difference compared to face mask therapy is the skeletal anchorage applying the forces directly on the bone surface of the jaws. Even when a bonded palatal expansion device is used as anchorage for the face mask, this will result in some proclination of the upper incisors and dentoalveolar compensation of the skeletal Class III. With our approach, no dental compensations of the upper incisors were observed, but some spontaneous proclination of the lower incisors occurred. Furthermore, we very exceptionally do a rapid maxillary expansion prior to the orthopedic intermaxillary traction. Mild crossbites are spontaneously corrected following the correction of the skeletal Class III. When comparing our results with the results of face mask therapy combined with RME, part of the overall effects of the face mask should be attributed to some forward projection of the anterior nasal spine during rapid maxillary expansion.
In maxillary protraction cases with Bollard miniplates, which force and time protocols do you recommend, both for correction and for retention? (Adilson Ramos)
We only tried out one single loading protocol. As we were satisfied with the initial results, we preferred to maintain the original protocol, in order to get a homogeneous sample. Originally we started with light forces, mainly to avoid overloading of the upper miniplates. Even with light forces, a good improvement of the Class III malocclusion is generally observed in the early stage of treatment. For this reason we advise to start with a loading of about 100 grams each side. Often a 5/16-in elastic is used, however the choice of elastics depends on the distance between the upper and lower plate, which is related to the severity of the skeletal Class III and the A-P position of the upper Bollard miniplates, depending on the inclination of the infrazygomatic crest. During the next three months we gradually increase the force level to 1/4-in and 3/16-in elastics. We ask the patient to augment the force a week before his next visit, so that we can change the loading shortly after the upgrade if there is increased mobility of the anchors. The patient is instructed to replace the elastics at least twice a day. The final loading is definitely smaller than generally used in combination with a face mask. Nevertheless, the orthopedic outcome is better. This may be explained by the intermittent force application with a face mask, also depending on the compliance of the patient. The wearing of the elastics is easier accepted by these young patients than the social impact of an extraoral device. The loading is started no later than 2 to 3 weeks after surgery and it is maintained for a total period of one year.
What is the force level used with the bone anchors? What happens if a higher force is applied? (James McNamara)
We are not sure that higher forces result in more growth changes. But, high forces may exceed the maximal resistance of the external cortical plate of the infrazygomatic crest and lead to bone loss and loosening of the screws. For this reason we don't use forces higher than 200 grams.
What are your clinical impressions on the stability of Class III maxillary protraction cases? In the correction of Class III which precautions do you recommended at the retention stage? (Adilson Ramos, Maurício Sakima)
There is a huge variability in growth changes of the midface observed during the active period of the orthopedic treatment. This may be due to different levels of interdigitation of the maxillary sutures, which are not always related to the chronological age. After the active orthopedic treatment the expression of Class III growth will further continue and will lead to relapse. Also an important interindividual variability is seen in the amount of remaining Class III growth during the retention period until adulthood. For this reason the miniplates are not removed after active treatment. They are used for night time intermaxillary traction when a relapse tendency of the Class III malocclusion is observed. Some cases hardly need any extra intermaxillary traction after the active period, others need more. Although treatment is started two to three years later than conventional face mask therapy, the follow-up takes a long time and total observation time is much longer than for conventional orthodontic treatment.
Which percentage of patients treated in this way had to undergo orthognathic surgery later on? (Maurício Sakima)
The majority of the patients in our sample didn't reach the end of facial growth yet. Moreover, the need for orthognathic surgery will be difficult to define. On one hand we will have the evaluation of the orthodontist and the surgeon about the severity of the remaining Class III soft tissue profile compared to a commonly accepted norm. On the other hand, the personal opinion of the patient, based on his self-esteem, will be crucial to decide whether surgery will be done or not. His self-esteem will be influenced by his experience that during growth already some improvement of his facial expression has been obtained. In the cases where orthognathic surgery is still needed, the question will remain in which degree the orthopedic treatment was able to reduce the severity of the Class III malocclusion and to reduce the amount of repositioning of the jaws needed during orthognathic surgery.
In cases with mild Class III mandibular asymmetry is there any special care needed or you do not recommend this approach? (Maurício Sakima)
True mandibular asymmetries are usually due to an asymmetric growth potential of both condyles. Based on the literature, there is little evidence that the amount of condylar growth can be permanently modified by orthopedics. For this reason we initially excluded true mandibular asymmetries from our study. However our findings showed that more than 40% of the A-P changes in the growth of the midface are due to modifications in the mandible and glenoid fossa. Therefore, more research is needed to investigate if unilateral elastic traction is able to reduce asymmetry of the mandible and chin deviation.
What surgical procedures for miniplate insertion are particularly important, as well as hygiene and medication, in order to minimize patient discomfort? (Adilson Ramos)
The surgical procedure is a very important factor in determining the failure rate. In contrary to the surgical protocol for insertion of miniscrews, a small mucoperiosteal flap has to be made. In the upper jaw the miniplate is positioned just in front of and parallel to the infrazygomatic crest. Further away from the crest, the external cortical bone is thinner. The device is positioned so that the round connecting bar of the neck penetrates the soft tissues in attached gingiva, close to the mucogingival border. Furthermore, the lower part of the neck should be in tight contact with the alveolar bone surface. In the lower jaw the miniplate is fixed between the lateral incisor and the canine. As a rule, no antibiotics or anti-inflammatory medications are prescribed. The patient is instructed to apply ice after surgery to reduce swelling, and to rinse with chlorhexidine twice a day for 12 days and several times a day with sparkling water. The first week after surgery the patient covers the intraoral extension with wax. This reduces mechanical irritation of the lip until the swelling is resolved. Ten days after surgery, the orthodontist gives appropriate hygiene instructions on how to clean the bone anchors with a conventional soft tooth brush. Before surgery and immediately after, the patient should be instructed not to touch the miniplate repeatedly by pressuring the tongue or fingers. This is the main reason why during the first weeks after surgery some mobility of the anchors may occur, without local signs of infection. Because of the smooth surface of this new object in the mouth, patients are tended to touch it repeatedly with the tongue. To reduce the adverse effects of these intermittent forces on the stability of the anchor, loading by elastics should be started no later than 2 to 3 weeks after surgery.
What are the limitations of the bone anchor protocol? Can this protocol be used in younger children? (James McNamara)
Two factors determine the ideal age to start treatment: The interdigitation degree of the sutures and the bone quality at the infrazygomatic crest. The "adaptability" of the growth potential in the sutures decreases with age. This may be explained by an increasing complexity of interdigitation of the sutures and increasing resistance against mechanical disruption. For this reason face mask therapy is usually recommended before the age of 9 years. However, at this age the thickness of the bone in the maxilla is not sufficient to obtain a solid mechanical retention of the screws. Based on our clinical experience, the best age seems to be around 11 for girls and 12 for boys. Starting the treatment two or three years later than conventional face mask therapy has the advantage that the final treatment with fixed appliance can be started immediately after the orthopedic correction. The follow-up period until adulthood will also be several years shorter.
What is the failure rate of miniplates in the maxilla in patients aged between 10 and 13? We often have bad quality bone in this region? Are these plates placed under sedation? (João Milki Neto)
In a recent study we investigated the failure rate of the Bollard miniplates in 25 consecutive Class III growing patients. They were all inserted by the same experienced surgeon. Sedation is not commonly used in Europe. Therefore, most of the miniplates were placed under a short general anesthesia (outpatient care). On a total of 100 miniplates one could not be fixed because of poor quality of the bone and insufficient mechanical retention of the screws. It was inserted three months later under local anesthesia and could be further used without problems. Five miniplates became loose after loading during the first three months. By interrupting the elastic traction, two bone plates became fixed again. However three had to be removed. After a healing period of about three months, the miniplates have been reinserted under local anesthesia and could be used again for intermaxillary traction. This high success rate is obtained by an experienced surgeon and orthodontist. However there is a learning curve for the surgeon to become familiar with the surgical protocol and the orthodontist has to learn how to deal with increasing mobility of some anchors and how to adapt the loading protocol.
Are there many cases that do not complete therapy because of complications? What are the most common technical problems encountered with your technique? (Jorge Faber/James McNamara)
The most common technical problem is loosening of the miniplate, mainly in the maxilla, in case of poor quality bone. Exceptionally a fracture of a miniplate can occur. This mainly happens after excessive bending of the round connecting bar during the surgical procedure. If a miniplate is lost, it can be replaced under local anesthesia and treatment can be completed.
Considering the timing of your treatment protocol, does the option of Rapid Maxillary Expansion + Face mask remains valid in early mixed dentition? (Leopoldino Capelozza Filho)
Because the different age range, face mask combined with RME can be started in the mixed dentition and if the outcome is not sufficient, a bone-anchored traction can still be started on a later age. However we have no evidence yet that a treatment in the early mixed dentition with RME/FM followed by a bone-anchored orthopedic treatment several years later has a better outcome than a bone-anchored orthopedic treatment alone. Then, such a two phase treatment should be avoided in order to reduce costs and discomfort for the patient.
What are the effects of the intermaxillary traction on the mandibular growth? (Leopoldino Capelozza Filho)
Besides the effects on the maxilla, the forward projection of the chin was also affected. Compared to a control group, nearly 3 mm difference in forward displacement/modeling of the bony chin was observed. However, the increase in length of the ramus and body of the mandible was not significantly different between our sample and a control group. It was concluded that the shape, rather than the size, of the mandible was modified by the continuous elastic traction. A closure of the gonial angle and posterior displacement of the ramus together with some modeling processes in the glenoid fossa are the basic effects of the force application on the mandible. In contrary to face mask therapy, no clockwise rotation of the mandible is observed. Open rotation of the mandible also results in a backward displacement of the chin, which contribute in the improvement of the facial convexity by face mask therapy.
Could adult patients benefit from this protocol when used in conjunction with surgically assisted rapid maxillary expansion (SARME)? (Bruno Furquim)
We have no experience with this procedure. The purpose of this treatment is completely different. Instead of distracting sutures, the maxilla is protracted at the level of the corticotomy. It's not sure that the light elastic traction is able to move the maxilla sufficiently forward. Moreover there will be poor vertical control and no precision in the final positioning of the maxilla, and of course no mandibular effects can be expected. If a SARME is indicated to correct a transverse deficiency of the maxilla and if also a forward displacement of the maxilla is needed, why not extending the surgical procedure by a Le Fort I osteotomy and down fracture, and position the maxilla in the 3 dimensions in an optimal relation with the rest of the face?
Submitted: March 26, 2012
Revised and accepted: April 24, 2012
Adilson Ramos
» Associate Professor, Department of Dentistry, State University of Maringá.
» MSc, FOB-USP and PhD in Orthodontics, UNESP-Araraquara.
» Former editor-in-chief of Dental Press Journal of Orthodontics (2003 2006).
Bruno Furquim
» MSc in Orthodontics, Bauru School of Dentistry / University of São Paulo.
» PhD student of Oral Rehabilitation, Bauru School of Dentistry / University of São Paulo.
James McNamara
» PhD in Anatomy, University of Michigan.
» Diplomate of the American Board of Orthodontics.
» Professor of Cell and Development Biology and Dentistry, University of Michigan.
» Researcher at the Center for Human Growth and Development, University of Michigan.
» Editor-in-chief of Craniofacial Growth Monograph Series, University of Michigan.
» Former President of Midwest Edward H. Angle Society of Orthodontists.
João Milki Neto
» Specialist in Oral and Maxillofacial Surgery by UniEVANGÉLICA (Anápolis).
» MSc in Oral and Maxillofacial Surgery, University of Brasília.
» PhD in Implantology, USC (Bauru).
» Professor of Oral and Maxillofacial Surgery, University of Brasília.
Jorge Faber
» Editor-in-chief of the Journal of the World Federation of Orthodontists and former Editor-in-chief of the Dental Press Journal of Orthodontics.
» Adjunct Professor in Orthodontics, University of Brasília.
» PhD in Biology Morphology, University of Brasília.
» MSc in Orthodontics, Federal University of Rio de Janeiro.
» Receiver of the Best Case Report in 2010 award for the best case report published in 2009 in the AJO-DO, apart from other prizes.
» Published over 70 articles in scientific journals.
Leopoldino Capelozza Filho
» MSc in Orthodontics, FOB-USP.
» PhD in Oral Rehabilitation/ Periodontics, FOB-USP.
» Coordinator of the Specialization Course in Orthodontics, Profis and USC.
» Professor of Post-graduation course in Orthodontics, USC.
» Founder and responsible for the orthodontic department "Centrinho" HRAC-USP.
» Author of Diagnóstico em Ortodontia e Metas Terapêuticas Individualizadas, also developed the individualized prescriptions for Capelozza' Straight-Wire technique.
Maurício Sakima
» Assistant Professor and PhD, Department of Child Dentistry, School of Dentistry, UNESP - Araraquara.
» MSc and PhD in Orthodontics, FOAR / UNESP.
» Post-doctorate, Royal Dental College - University of Aarhus, Denmark.
» Patients displayed in this interview previously approved the use of their images.
- 1. Nguyen T, Cevidanes L, Cornelis MA, Heymann G, de Paula LK, De Clerck H. Three-dimensional assessment of maxillary changes associated with bone anchored maxillary protraction. Am J Orthod Dentofacial Orthop. 2011 Dec;140(6):790-8.
- 2. Baccetti T, De Clerck HJ, Cevidanes LH, Franchi L. Morphometric analysis of treatment effects of bone-anchored maxillary protraction in growing Class III patients. Eur J Orthod. 2011 Apr;33(2):121-5. Epub 2010 Dec 27.
- 3. De Clerck H, Cevidanes L, Baccetti T. Dentofacial effects of bone-anchored maxillary protraction: a controlled study of consecutively treated Class III patients. Am J Orthod Dentofacial Orthop. 2010 Nov;138(5):577-81.
- 4. Cevidanes L, Baccetti T, Franchi L, McNamara JA Jr, De Clerck H. Comparison of two protocols for maxillary protraction: bone anchors versus face mask with rapid maxillary expansion. Angle Orthod. 2010 Sep;80(5):799-806.
- 5. Heymann GC, Cevidanes L, Cornelis M, De Clerck HJ, Tulloch JF. Three-dimensional analysis of maxillary protraction with intermaxillary elastics to miniplates. Am J Orthod Dentofacial Orthop. 2010 Feb;137(2):274-84.
- 6. De Clerck HJ, Cornelis MA, Cevidanes LH, Heymann GC, Tulloch CJ. Orthopedic traction of the maxilla with miniplates: a new perspective for treatment of midface deficiency. J Oral Maxillofac Surg. 2009 Oct;67(10):2123-9.
- 7. Cornelis MA, Scheffler NR, Mahy P, Siciliano S, De Clerck HJ, Tulloch JF. Modified miniplates for temporary skeletal anchorage in orthodontics: placement and removal surgeries. J Oral Maxillofac Surg. 2008 Jul;66(7):1439-45.
Publication Dates
-
Publication in this collection
16 Aug 2012 -
Date of issue
June 2012