Abstract
INTRODUCTION: An orthodontic or diagnostic setup consists in cutting and realigning the teeth in plaster models, making it an important resource in orthodontic treatment planning. OBJECTIVE: The aim of this article is to provide a detailed description of a technique to build an orthodontic setup model and a method to evaluate it. CONCLUSIONS: Although laborious, orthodontic setup procedure and analysis can provide important information such as the need for dental extractions, interproximal stripping, anchorage system, among others.
Orthodontics; Diagnosis and planning; Dental casts
SPECIAL ARTICLE
Preparation and evaluation of orthodontic setup
Telma Martins de AraújoI; Lílian Martins FonsecaII; Luciana Duarte CaldasII; Roberto Amarante Costa-PintoIII
IFull Professor of Orthodontics, Federal University of Bahia. PhD and MSc in Orthodontics, Federal University of Rio de Janeiro. Coordinator of the Center for Orthodontics and Facial Orthopedics Professor Édimo José Soares Martins, Federal University of Bahia. Former President of the Brazilian Board of Orthodontics (BBO)
IIStudents attending the Specialization Program in Orthodontics, Federal University of Bahia
IIIMSc in Orthodontics, Federal University of Rio de Janeiro. Professor of Orthodontics, EBMSP. Collaborating Faculty Member, Specialization Program in Orthodontics, Federal University of Bahia
Contact addressContact address: Telma Martins de Araújo Av. Araújo Pinho, 62 7º andar Canela, Salvador/BA Brazil Zip code: 40.110-913 E-mail: tmatelma@globo.com
ABSTRACT
INTRODUCTION: An orthodontic or diagnostic setup consists in cutting and realigning the teeth in plaster models, making it an important resource in orthodontic treatment planning.
OBJECTIVE: The aim of this article is to provide a detailed description of a technique to build an orthodontic setup model and a method to evaluate it.
CONCLUSIONS: Although laborious, orthodontic setup procedure and analysis can provide important information such as the need for dental extractions, interproximal stripping, anchorage system, among others.
Keywords: Orthodontics. Diagnosis and planning. Dental casts.
INTRODUCTION
Plaster casts of the dental arches play a key role in orthodontic diagnosis1 since, besides revealing the occlusal conditions of the patient in the three dimensions of space, they allow for the performance of many different analysis that assist in orthodontic treatment planning. These include analysis of space discrepancy in mixed and permanent dentition, dental arch symmetry, Bolton discrepancy and orthodontic setup procedure.2-6
In 1953, Kesling, after developing a tooth positioner as an aid in finishing orthodontic treatments, suggested that cutting and repositioning the teeth in duplicate study models of the malocclusions would allow simulation of the results before starting orthodontic treatment.7
Orthodontic setup is a laboratory procedure that involves cutting and mounting the teeth in dental arch casts, where a drawn up treatment plan based on the diagnosis is tested and changed until the best possible results have been achieved. While it can be quite laborious, it features considerable advantages, especially in borderline cases where there are clinical issues. Using a setup, treatment plans become less speculative, resembling a real treatment and providing orthodontists with reliable information. Research comparing the orthodontic setups of 30 patients using models obtained after treatment completion show that setups are a reliable diagnostic resource which can be used as an aid in planning orthodontic treatment.7
This article provides a detailed description of the setup procedure as well as a method for evaluating the setup, which allows professionals to extract important information to implement a proposed treatment.
ORTHODONTIC SETUP PROCEDURE
Models must be properly fabricated to faithfully reproduce the patient's malocclusion, then duplicated and polished to streamline the setup procedure. Furthermore, a treatment plan should be selected for evaluating the diagnostic setup. For a technical description of the orthodontic setup, a 14-year-old dark-skinned patient with Angle Class I malocclusion was used. She had been treated at the Bahia State Federal University (UFBA), at the Specialization Program in Orthodontics at the Édimo Jose Soares Martins Center for Orthodontics and Facial Orthopedics. A treatment plan was proposed after reviewing data collected in the clinical examination, patient history, intra and extraoral images, complementary exams, cephalometric tracing and orthodontic models (Fig 1-3). Facial analysis revealed lip incompetence, convex profile, decreased nasolabial angle and malar and paranasal deficiency. She had a Class I skeletal pattern (ANB=3º), with a good maxillomandibular relationship (SNA=82º and SNB=79º) and increased lower facial third (SN-GoGn=41º, AMF=40º and Y-axis=71º). She had a Class I dental malocclusion, bimaxillary protrusion, upper and lower anterior crowding, with discrepancy of -11.2 mm and -5.5 mm, respectively. Her incisors were in an edge-to-edge relationship, proclined (1-NA=28º and 8 mm, 1-NB=36º and 12 mm), and teeth # 12, 22, 24 and 25 in crossbite, in addition to a tooth size discrepancy9 showing 2.8 mm excess in the lower anterior region. The degree of complexity found (46 points) made it a highly complex malocclusion.10
The treatment planned for correcting this malocclusion involved the extraction of the upper and lower first premolars to eliminate the discrepancy between the teeth and basal bones, and retracting the anterior teeth to balance the facial profile.
The setup procedure comprises the steps described next (The list of materials used can be found on the website www.dentalpress.com.br/revistas).
Midline registration
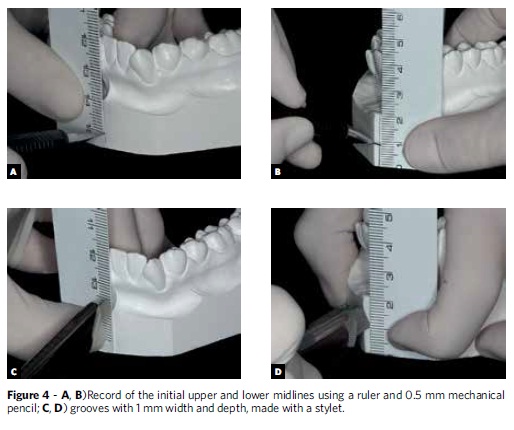
Coinciding the upper and lower dental midlines is one of the treatment objectives, be it for aesthetic and/or functional purposes, be it to accomplish adequate dental intercuspation in the posterior region of the dental arches. For this reason, the initial position of the midlines deserves utmost attention. To evaluate such position, the patient must be in a standing position during the clinical extraoral examination, with the Frankfort horizontal plane parallel to the ground, and facing the operator. One must then note the position of the upper and lower dental midlines relative to the facial midline. In a front view of the patient at rest and with lips slightly parted, one should imagine a line passing through the groove of the upper lip philtrum, and the distance from this line to a midpoint between the upper and lower central incisors should be estimated. This patient had a greater than 2 mm midline deviation to the right side while the lower midline coincided with the facial midline. The transfer of this information to the bases of the upper and lower plaster models, duly supported on a glass plate, is to be performed using 0.5 mm mechanical pencil and a ruler. Thereafter, grooves with depth and width of approximately 1 mm should be made in the demarcated sites using a ruler and stylus (Fig 4).
The grooves corresponding to the initial midlines should be filled with blue wax and heated in a dripper, and the registration of the correct midlines targeted by the orthodontic treatment should be performed using heated #7 red wax (Fig. 5). This information will guide the correct establishment of the midlines when mounting of the teeth.
First molar registration
The mesiodistal axial inclination of upper and lower posterior teeth, preferentially first molars, should also be recorded. In order to verify the axial inclination of these teeth, assuming dental crowns are intact, one can evaluate the relationship between marginal ridges and adjacent teeth, and analyze the relationship of the tooth roots in panoramic and/or periapical radiographs. Once these references have been defined, grooves with width and depth of approximately 0.5 mm should be made on the teeth and model bases. On maxillary molar teeth the grooves must be marked at the center of the mesiobuccal cusp, and on the lower molars the mark should be made on the groove between the mesiobuccal cusp and the median cusp. Both should be extended to the bases of the models using a ruler. However, should the first molars be missing, the second or third molar may be used as reference. These grooves must be filled with blue wax heated in a dripper (Fig 6). If the first molars are missing, the second or third molars can be used as reference.
Recording the position of the upper and lower molars on the model bases is important to check for changes in the movement of these teeth in the anteroposterior direction, such as loss of anchorage, distalizations or correction of dental inclinations.
Lower dental arch form registration
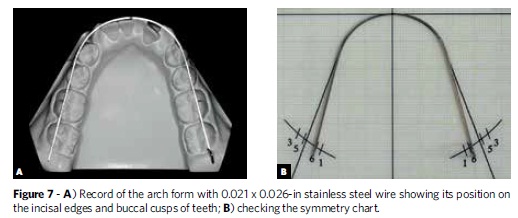
To avoid relapses, studies recommend that the original form of the lower dental arch not be changed to ensure stability of the occlusion achieved with the orthodontic treatment.11 To record the original form, a guiding arch should be prepared using thicker wires, such as stainless steel rectangular 0.021 x 0.026-in or round 0.032-in wires in order to prevent deformation during the phases of the setup procedure. This arch should be fabricated by passing it through the incisal edges of the incisors, canine cusps and buccal cusps of premolars and molars. In mounting the teeth, some modifications may be needed, since the goal is to record the form of the basal bone. Therefore, if the posterior teeth are too buccally inclined relative to the basal bone, the arch should be contracted. If, on the other hand, the teeth exhibit a very pronounced lingual inclination, the arch should have its form further expanded. It is advisable to check the symmetry of this parable in a symmetry chart before starting setup procedure (Fig 7).
Lower incisor registration
The position of the incisors at the end of treatment clearly indicates that a successful, satisfactory occlusion and a balanced profile have been achieved.
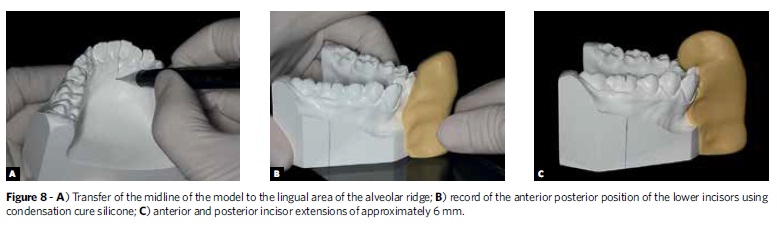
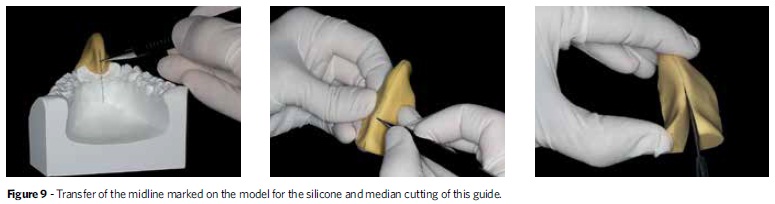
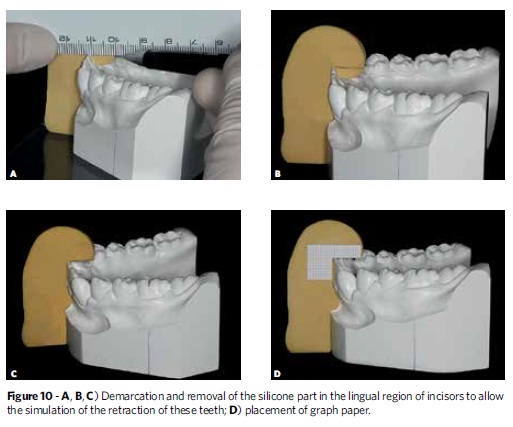
First, with the aid of a 0.5 mm mechanical pencil, one should transfer the initial lower dental midline to the lingual area of the alveolar ridge. The registration of the anteroposterior position of the incisors can be carried out with condensation or addition cure silicone. Thus, the model should be placed on a glass plate and receive the silicone, which must encompass the entire anterior vertical portion of the model base, the bottom of the vestibule and buccal and lingual surfaces of the central incisors. To facilitate planning the movement of these teeth, the silicone must be spread about 6 mm anteriorly and posteriorly, starting from the buccal surface of the incisors (Fig 8). After the silicone has set, the registration of the midline marked in the model, in the lingual region of the alveolar ridge, should be transferred to the silicone. This line will serve as a reference to the median cutting of this guide (Fig 9). Then, a piece of graph paper extending vertically and horizontally should be glued to the silicone (Fig 10). This graph paper will serve to quantify the extent to which the simulation of tooth movement is in accordance with the treatment plan, regardless of whether such movement is an intrusion, extrusion, proclination or retroclination. When the treatment plan provides for proclination or extrusion of anterior teeth, before placing the graph paper one should remove part of the silicone in the anterior or superior region to the labial incisal edge, respectively.
Another silicone cure registration must be performed in the posterior region to ensure that the vertical dimension is accurate between the upper and lower models (Fig 11). This record is particularly important in cases where there is occlusal instability, as in the presence of open bite or when many posterior teeth are missing. Thus, after removal of the teeth and while realigning them, one avoids the risk of deviations in the transverse direction and loss of vertical dimension.
Tooth identification and cutting
Before their removal from the base of the models, the teeth should be numerically identified with pencil 0.5 mm on the lingual surface, to prevent them from being confused when mounting the setup (Fig 12).
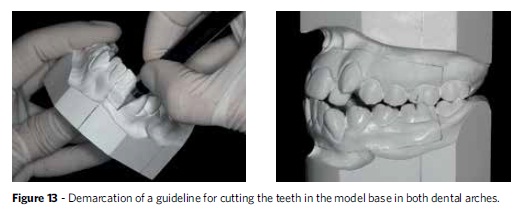
For the removal of the upper and lower teeth, a line must be drawn limiting the region of the alveolar ridge, approximately 5 mm from the cervical region of the teeth (Fig 13). Some exceptions should be considered, such as buccal ectopia and gingival recession. It is essential to ensure that the tooth stumps that result from cutting the teeth are high enough to be subsequently attached to the wax.
The models must be drilled in the buccolingual direction, with the aid of a #6 round bur mounted in a handpiece, on the limited horizontal line near the midlines of the teeth. The hole diameter should be about 2 mm, sufficient for inserting a thin spiral saw (Fig 14).
The decision regarding from which lower model quadrant one should start cutting depends on several factors, including: Midline deviation, crowding, diastemas, lateral open bites and tooth agenesis. In other words, the block of teeth to be initially highlighted should be opposite to the midline, for example. In this case, the lower dental midline was correct, but had more than 2 mm deviation to the right. Cutting was therefore started on the opposite side, so that the upper incisor on the left was properly mounted in the middle of dental arch, thus leading to the positioning of other teeth in this segment.
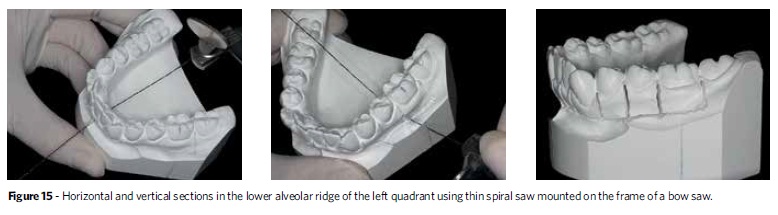
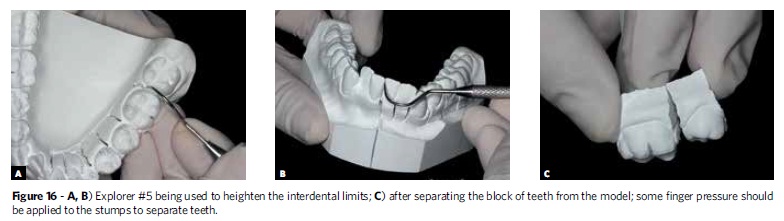
After choosing the quadrant, the spiral saw must be inserted into the hole at the base of the model and attached to a bow saw to enable horizontal cutting as far as the penultimate tooth, but only in the quadrant chosen. It is recommended that the second molars not be initially removed in order to help maintain vertical dimension. From the section in the horizontal direction, new sections between the teeth must be made in the vertical direction using a straight saw, taking care not to break the contact points in order to avoid fracturing the dental structures and compromising the mesiodistal dimension of the teeth (Fig 15). After the horizontal and vertical cutting, an explorer #5 must heighten the interdental limits, providing a guide for the fracture line. Only then should a light finger pressure be applied to weaken the embrasures and separate the teeth (Fig 16). The plaster stump of each tooth should be stripped with a steel or tungsten dental bur, slenderizing the stump while carefully preserving the mesiodistal dimension of each tooth without removing the dentogingival limit (Fig 17).
Once the teeth have been prepared, their mesiodistal dimensions should be checked with a caliper, comparing them with the sizes of the original model of the initial study, which recorded the patient's malocclusion (Fig 18).
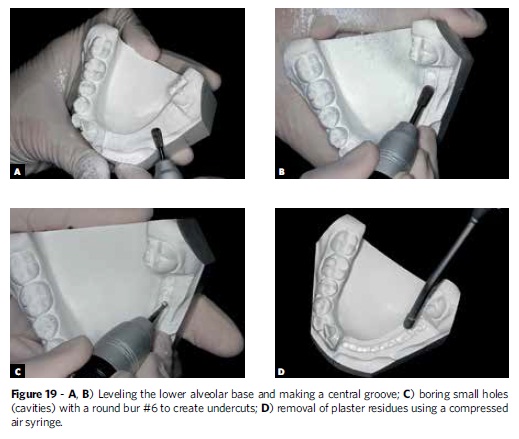
Following, the area corresponding to the base of the alveolar model should be leveled flush with a steel or tungsten carbide cutter to avoid interferences when mounting the teeth. A central groove should be made in the ridge area using the same cutter to preserve the buccal and lingual boundaries of the region, as these will be useful when carving the wax. Subsequently, small cavities should be bored with a round bur #6 in order to create retention for insertion and fixation of the wax. Soon afterwards, any debris that may interfere with the wax adhesion should be removed with a brush and/or compressed air (Fig 19). This entire sequence of procedures should be performed in the ipsilateral quadrant in the upper arch.
Tooth mounting
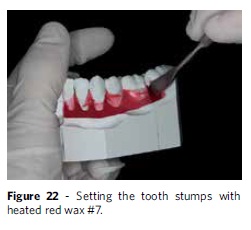
To mount the teeth, the model base should be prepared in the following sequence: Complete filling of the central groove in the alveolar base with a layer of melted red wax #7; placing of a strip of utility wax, also red, with a height of approximately 6 mm (Fig. 20). Using a silicone bite registration, the lower central incisor is positioned in the utility wax according to the changes proposed in the treatment plan, considering proclination, retraction, intrusion or extrusion. Next, the remaining teeth are positioned using as reference the archwire form which best represents the original dental arch form (Fig 21). A 3 mm retraction was planned in this case for the lower incisors. After determining the position of the teeth, excess utility wax is removed and the spaces between the teeth filled with hot wax #7 (Fig 22).
When mounting the teeth one should follow the guidelines and the six keys to a normal occlusion introduced by Robert Strang12 and Lawrence Andrews,13 whereas the arch form and intercanine and intermolar widths should be preserved.
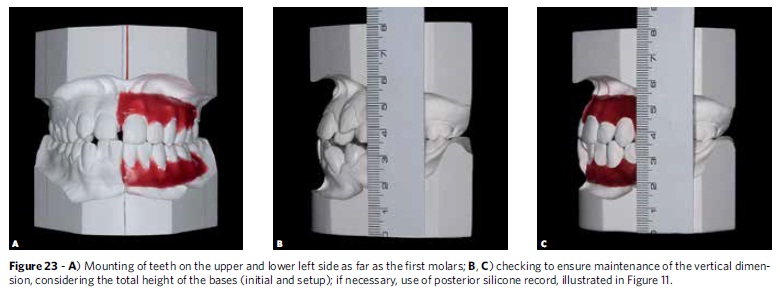
Once one of the lower quadrants has been fully mounted, the same procedures should be repeated in mounting the upper teeth on the same side, ensuring the best possible intercuspation, while maintaining the vertical and transverse dimensions (Fig 23). After mounting is completed on one side, one must repeat all procedures on the other side of the dental arch (Fig 24).
Once the vertical dimension has been preserved through the occlusion of the premolars and molars, the second molars are removed and mounted. One should, however, ascertain that posterior cutting be performed precisely on the distal surface of the second molars, thereby monitoring the amount of movement that occurs in the posterior segment of each quadrant (Fig 25). Once mounting is complete, the occlusion should be checked in its contact points, marginal ridge height and axial inclination of the anterior and posterior teeth.
Waxing, carving and finishing
Heated red wax #7 should be placed over and around the stubs, from the alveolar base to the cervical region of all teeth. This type of wax is used because of its greater strength and superior conservation of the setup. The gingival margins are then shaped using a Hollemback carver taking into account the height and shape of the crowns and original zeniths of each tooth. Maintaining the gingival margin while preparing the teeth can assist in the process of carving and waxing. The wax should be plasticized using a Hannau type lamp, rendering it thoroughly even and smooth. For finishing, the models should undergo a second procedure, namely, pearling. To this end, the setup should be dipped in a container with soap solution, with the teeth facing down, thus allowing all surfaces to submerge. Within no longer than two hours, the models must be removed from the solution, washed in running water, and rubbed with cotton soaked in the same solution. Finally, it should be allowed to dry for at least 24 hours in a ventilated, dust free environment, on absorbent paper, with the teeth facing downwards. Plaster polishing should be accomplished by rubbing a silk fabric on the teeth and model base (Figs 26, 27).
SETUP ANALYSIS
Once the setup is ready, much information is generated and if a judicious method is not used to analyze it one may not derive its full benefits. The use of an evaluation form based on the model, first suggested by Cury-Saramago and Vilella14 is recommended. The proposed method includes ten items: Extractions, changes in the basal bones, lower incisor position, leveling, midlines, dental arch form, molar and canine relationship, anchorage, interproximal stripping and cosmetic finishing (Fig 28). The manner in which data are acquired and recorded, as well as the type of information that can be obtained will be presented below, along with remarks on the analysis of the clinical case presented in this article (Fig 27).
Extractions
Under this topic one should record the extractions which were necessary for treating the malocclusion. Additionally, the mesiodistal dimensions of the extracted teeth should be recorded as these dimensions are an indication of the space gained for alignment, leveling, repositioning of the anterior teeth and correction of the midlines. In the example described above, teeth numbers 14, 24, 34 and 44 were extracted, resulting in a space gain of 16.8 mm in the upper and 17 mm in the lower arch.
Basal bones
Under this item one should record the amount of growth planned for the treatment period, and the extent of maxillary/mandibular advancement or setback determined in planning orthognathic surgery, which can be measured by the extent of wax placed on the posterior edge of the models. Since this was not a growing patient and surgery was not planned, nothing was recorded on the card.
Lower incisors
The type and amount of movement performed in mounting these teeth (retraction, proclination, intrusion, extrusion) must be recorded. In this example, there was a 3 mm retraction of the lower incisors to decrease dental protrusion (Fig 21A). It is noteworthy that in this case the space for incisor alignment and retraction was gained by extracting the first premolars.
Leveling
To assess changes in dental leveling one should note the amount of overbite and curve of Spee present in the initial malocclusion, and the correction made in the setup. It is important to stress that this leveling occurred by intrusion or extrusion of anterior or posterior teeth accomplished according to the diagnosis and treatment plan. In the case presented in this study, the edge-to-edge relationship in the anterior region identified at the beginning of treatment was corrected by extruding the upper incisors.
Midlines
One should record the changes made in the upper and lower midlines (Fig 27), and how space was obtained for this procedure, such as premolar extractions, distalization of posterior teeth or stripping. In the setup described in this study, the upper midline was corrected by deviating it 2 mm to the left; space was gained from premolar extractions.
Dental arches
In order to evaluate the lower dental arch form once the setup is complete, one should use an archwire form compatible with the original dental arch form (Fig 7). In this case, it can be observed that the form was retained to the extent possible (Fig 24C). One should also compare the distances between the upper and lower canines and molars on the setup with the measurements obtained from the models that contain the malocclusion, and record the changes. In the clinical case there was practically no changes in the intermolar distance in both arches, the intercanine width, on the other hand, increased due to the fact that these teeth were distalized to achieve leveling, alignment and incisor retraction.
Molars and canines
In this section, one should record, in addition to the initial relationship of these teeth, the position they occupy after simulating the treatment, and report whether they are in normal occlusion, Class II or III malocclusion. At this point, one can also observe if major changes were needed in molar inclination. This reading can be performed by extending the registration of the molar positions, performed at the base of the model, as far as the corresponding marks in the aforesaid teeth at their final positions (Fig 27). Intercuspation should be assessed, and any difficulty in mounting the setup, noted. This step is important as it enhances treatment predictability given the possibility that the same problems may also occur during orthodontic therapy. In this case, the relationship of the molars and canines in the anteroposterior direction was maintained. Intercuspation was improved thanks to the space obtained from the extractions.
Anchorage
Any anterior posterior movement observed in the molars must be recorded. For this purpose, a ruler is placed on the base of the model, and the registration line is extended from the starting position of the molars. Thus, one can measure with another ruler the amount and direction (mesial or distal) of tooth movement. Another form of assessment is to measure the distance between the distal end of the last tooth and the retromolar region in the upper and lower arches. However, this method is effective only if this region has been carefully cut at the distal end of the last tooth in the setup model. This information will be useful for planning the anchorage to be used in the orthodontic treatment of the malocclusion. In the case described in this article, 3.5 mm anchorage was lost in the upper right quadrant, 3 mm in the upper left quadrant, 4 mm in the lower right quadrant and 3.5 mm in the lower left quadrant. Planning the anchorage for treating the aforementioned malocclusion required the use of a Nance button and lingual bar.
Interproximal stripping
Whenever stripping is required, the mesiodistal dimensions of the teeth involved should be recorded before and after stripping. Thus, one can calculate the amount of interproximal stripping performed on each tooth to obtain proper alignment of dental and/or inter occlusal relationship, be it in the anterior or posterior segment, or both. It is important to note that this stripping should only be carried out when Bolton discrepancy9 is present, or else a Bolton discrepancy will be created in the opposing arch. Prior to stripping, one should also ascertain that the sizes of all teeth are symmetrical, since if tooth symmetry is not present, the teeth with larger mesiodistal dimensions should be stripped first, thereby establishing symmetry with the homologous teeth. In the case presented as an example, there was tooth size discrepancy with a 2.8 mm excess in the six lower anterior teeth, making it impossible to perform full space closure in the anterior maxillary arch. Stripping was therefore performed on the mesial surface of teeth 33 and 43 and on the mesial and distal surfaces of teeth 32 and 42. This procedure proved important in resolving the Bolton discrepancy and accomplishing a proper inter incisal relationship.
Cosmetic finishing
At this point, the details that were necessary for properly finishing the orthodontic treatment should be recorded, such as the stripping of the palatal marginal ridges on upper incisors so as to establish a correct overjet, or bulky or accessory cusps that may interfere with a proper posterior intercuspation. The need for gradual reshaping in the case of microteeth, asymmetries of homologous teeth, Bolton discrepancy, or large teeth showing signs of substantial incisal wear should also be noted. After achieving the best possible intercuspation it is important to record the factors that hindered the achievement of an even better intercuspation. Some such factors are the presence of eccentric or worn cusps, restorations with improper shape or size, as well as teeth with increased or decreased buccolingual dimensions. In this case, some stripping of the palatal ridges of teeth 11 and 21 was performed.
FINAL CONSIDERATIONS
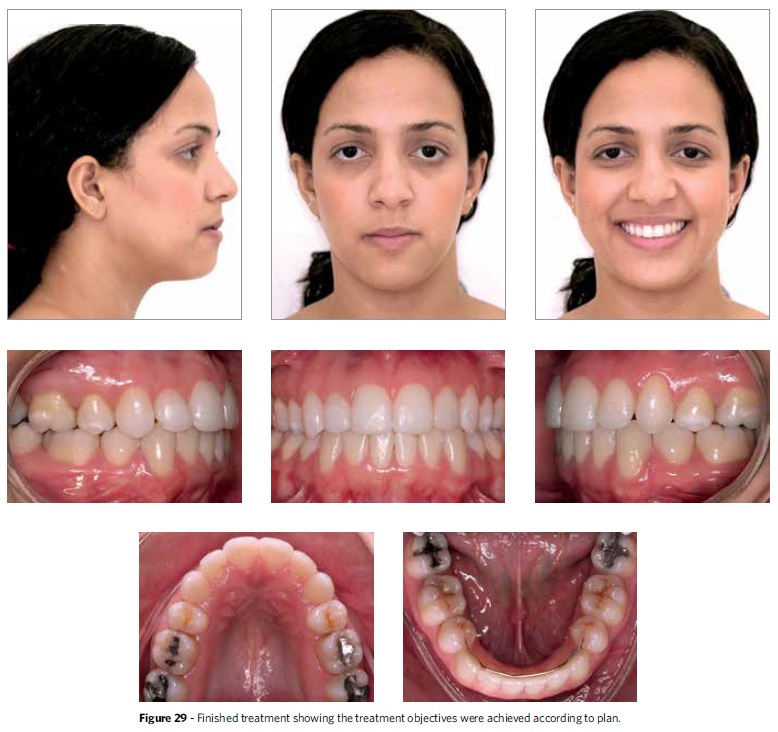
In reviewing the treatment outcome of the patient that illustrates this article, it becomes clear that the planned objectives were achieved: Pleasing face and smile, good occlusal relationship, lip competence, straight profile, the Class I skeletal pattern (ANB=2º) was preserved, with a good relationship between maxilla and mandible (SNA=81º and SNB=79º), the vertical pattern was maintained (SN-GoGn=40º, FMA=39º, Y Axis=69º) and incisor positioning improved (1-NA=28º and 6 mm; 1-NB=22º and 5 mm) (Figs 29 31). In the cephalometric superimpositions (Fig 32) one can see that incisor retraction and anchorage loss in the upper and lower arches occurred according to how the setup was planned and constructed. After performing an analysis of the manner in which the treatment was finished in dental casts and radiographs, as recommended by the American Board of Orthodontics,15 this treatment received 9 points, which is considered a good finishing score.
With the development of and reduction in the cost of three-dimensional scanning technology, along with the ability to perform computerized analyses, virtual models of the dental arches have become increasingly common in clinical orthodontics. The computer programs designed to meet this market demand are becoming increasingly effective and thorough. Today, it is possible to quickly and easily analyze asymmetries, space discrepancies, tooth size, among other features. OrthoAnalizer® software, for example, includes a tool to build digital setups (Fig 32). After scanning the model, treatment simulation is performed similarly to a conventional mounting. The teeth are separated, extractions can be performed and teeth moved in all directions. The mounting must be initiated by repositioning the lower incisors. One side should be mounted at a time and the arch form can be maintained. However, to ensure that the digital setup is reliable the operator should be skilled in the sequence and careful when simulating the tooth movements according to the manual setup construction method described in this article. Figure 33 shows the digital setup of one and the same patient.
Finally, a manual or digital reading of the setup is recommended, recording all information obtained from this diagnostic simulation on a form (Fig 28), so that no information is lost and maximum benefits can be derived. As a result, treatment planning will be more reliable and prognosis more clearly envisaged, especially in more complex cases or atypical extractions.
Submitted: April 9, 2012
Revised and accepted: April 30, 2012
» The authors report no commercial, proprietary, or financial interest in the products or companies described in this article.
» Patients displayed in this article previously approved the use of their facial and intraoral photographs.
- 1. Hou HM, Wong RWK, Hägg U. The uses of orthodontic study models in diagnosis and treatment planning. Hong Kong Dent J. 2006;3(2):107-15.
- 2. Bolognese AM, Mucha JN, Mangim VCN, Moreira TC, Goraieb SM, Menezes LM, et al. Setup: uma técnica de confecção. Rev Soc Bras Ortodon. 1995;2(8):245-9.
- 3. Tavares CAE, Zanini LK. A confecção do "Set up" de diagnóstico ortodôntico. Rev Dental Press Ortod Ortop Facial. 1999;4(5):20-3.
- 4. Ruellas ACO. Montagem de diagnóstico ortodôntico simplificado (set up). J Bras Ortodon Ortop Facial. 2000;5(30):57-60.
- 5. Vianna MS, Saga AY, Casagrande FA, Camargo ES. Setup: um auxílio no diagnóstico ortodôntico. J Bras Ortodon Ortop Facial. 2002;7(11):398-405.
- 6. Kesling HD. The diagnostic setup with consideration of the third dimension. Am J Orthod. 1956;42(10):740-8.
- 7. Andrade BNG, Almeida RC, Carvalho FAR, Quintão CCA, Almeida MAO. Avaliação da confiabilidade do setup no diagnóstico e planejamento ortodôntico. Ortodontia. 2010;43(4):389-95.
- 8. Habib F, Fleischmann LA, Gama SKC, Araújo TM. Obtenção de modelos ortodônticos. Rev Dental Press Ortod Ortop Facial. 2007;12(3):146-56.
- 9. Bolton WA. The clinical application of tooth size analysis. Am J Orthod. 1962;48(7):504-29.
- 10. Cangialosi TJ, Riolo ML, Owens SE Jr, Dykhouse VJ, Moffitt AH, Grubb JE, et al. The ABO discrepancy index: a measure of case complexity. Am J Orthod Dentofacial Orthop. 2004;125(3):270-8.
- 11. Triviño T, Siqueira DF, Scanavini MA. A forma do arco dentário inferior na visão da literatura. Rev Dental Press Ortod Ortop Facial. 2007;12(6):61-72.
- 12. Strang RH, Thompson WM. A textbook of Orthodontia. 4th. ed. Philadelphia: Lea & Febiger; 1958.
- 13. Andrews LF. The six keys to normal occlusion. Am J Orthod Dentofacial Orthop. 1972;62(3):296-309.
- 14. Cury-Saramago AA, Vilella OV. Analisando o setup. Rev Soc Bras Ortodon. 2005;5(2):107-18.
- 15. Casko JS, Vaden JL, Kokich VG, Damone J, James RD, Cangialosi TJ, et al. Objective grading system for dental casts and panoramic radiographs. Am J Orthod Dentofacial Orthop. 1998;114(5):589-99.
Contact address:
Publication Dates
-
Publication in this collection
16 Aug 2012 -
Date of issue
June 2012
History
-
Received
09 Apr 2012 -
Accepted
30 Apr 2012