Abstracts
This study had the aim to investigate the auditory and communicative abilities of children diagnosed with Auditory Neuropathy Spectrum Disorder due to mutation in the Otoferlin gene. It is a descriptive and qualitative study in which two siblings with this diagnosis were assessed. The procedures conducted were: speech perception tests for children with profound hearing loss, and assessment of communication abilities using the Behavioral Observation Protocol. Because they were siblings, the subjects in the study shared family and communicative context. However, they developed different communication abilities, especially regarding the use of oral language. The study showed that the Auditory Neuropathy Spectrum Disorder is a heterogeneous condition in all its aspects, and it is not possible to make generalizations or assume that cases with similar clinical features will develop similar auditory and communicative abilities, even when they are siblings. It is concluded that the acquisition of communicative abilities involves subjective factors, which should be investigated based on the uniqueness of each case.
Auditory perception; Communication; Language; Hearing loss, central; Child
Este estudo teve como objetivo investigar as habilidades auditivas e comunicativas de crianças diagnosticadas com Espectro da Neuropatia Auditiva, sendo a etiologia definida como mutação no gene Otoferlin. Trata-se de uma pesquisa descritivo-qualitativa, na qual foram avaliados dois irmãos que se enquadram no quadro clínico descrito. Os procedimentos realizados foram: testes de percepção de fala voltados a crianças deficientes auditivas profundas e avaliação das habilidades comunicativas por meio do Protocolo de Observação Comportamental. Por serem irmãos, as crianças voluntárias neste estudo partilham o mesmo ambiente familiar e contexto comunicativo. Apesar disso, desenvolveram habilidades comunicativas distintas, principalmente quanto ao uso da linguagem oral. O estudo mostrou que o Espectro da Neuropatia Auditiva é uma patologia muito heterogênea em todos os aspectos, não sendo possível fazer generalizações ou supor que casos com características clínicas similares desenvolverão as mesmas habilidades auditivas e comunicativas, mesmo no caso de irmãos. Conclui-se que a aquisição dessas habilidades envolve fatores subjetivos, que devem ser investigados a partir da singularidade de cada caso.
Percepção auditiva; Comunicação; Linguagem; Perda auditiva central; Criança
CASE REPORT
Auditory and communicative abilities in the auditory neuropathy spectrum disorder and mutation in the Otoferlin gene: clinical cases study
Nayara Thais de Oliveira CostaI; Ana Claudia Martinho-CarvalhoII; Maria Claudia CunhaIII; Doris Ruthi LewisIII
IGraduate Program (Masters degree) in Speech-Language Pathology and Audiology, Pontifícia Universidade Católica de São Paulo - PUC - São Paulo (SP), Brazil
IIDepartment of Physical Therapy, Speech-Language Pathology and Audiology, and Occupational Therapy, School of Medicine, Universidade de São Paulo - USP - São Paulo (SP), Brazil
IIDepartment of Clinical Speech-Language Pathology and Audiology, School of Human and Health Sciences, Pontifícia Universidade Católica de São Paulo - PUC - São Paulo (SP), Brazil
Correspondence address Correspondence address: Nayara Thais de Oliveira Costa R. Araguari, 661/102, Moema São Paulo (SP), Brasil, CEP: 04514-041 E-mail: na-thais@hotmail.com
ABSTRACT
This study had the aim to investigate the auditory and communicative abilities of children diagnosed with Auditory Neuropathy Spectrum Disorder due to mutation in the Otoferlin gene. It is a descriptive and qualitative study in which two siblings with this diagnosis were assessed. The procedures conducted were: speech perception tests for children with profound hearing loss, and assessment of communication abilities using the Behavioral Observation Protocol. Because they were siblings, the subjects in the study shared family and communicative context. However, they developed different communication abilities, especially regarding the use of oral language. The study showed that the Auditory Neuropathy Spectrum Disorder is a heterogeneous condition in all its aspects, and it is not possible to make generalizations or assume that cases with similar clinical features will develop similar auditory and communicative abilities, even when they are siblings. It is concluded that the acquisition of communicative abilities involves subjective factors, which should be investigated based on the uniqueness of each case.
Keywords: Auditory perception; Communication; Language; Hearing loss, central; Child.
INTRODUCTION
Speech perception and comprehension represent the abilities of reception and interpretation of sound models. When these abilities are affected, other impairments also occur in an individual's communicative abilities.
The Auditory Neuropathy Spectrum Disorder (ANSD) is an auditory impairment that usually results in significant difficulties in speech perception, especially in the presence of competitive noise, indicating temporal processing impairment due to the asynchrony of the cochlear auditory pathways towards the auditory cortex(1). Failures in the temporal processing resolution ability also affect verbal comprehension and, consequently, oral language development and communicative performance(2).
The ANSD is characterized by a classic clinical picture, evidenced by absence of significant alterations on the Brainstem Auditory Evoked Potential (BAEP) results, presence of Evoked Otoacoustic Emissions (EOAE) and/or cochlear microphonic (CM), and absence of stapedial acoustic reflexes. Regarding the audiological characteristics, pure-tone thresholds might present several configurations, from normal hearing to profound hearing loss, uni or bilateral, symmetric or not. Progressive cases or fluctuation of the hearing loss are also possible, and, in some of these cases, hearing functioning may vary overnight(1).
ANSD has many possible etiologies, including non-syndromic autosomal recessive inheritance, caused by mutation in the Otoferlin (OTOF) gene(3). The OTOF is composed by 48 exons, and provides instructions for the production of the protein Otoferlin, which is responsible for the liberation of neurotransmitters in the synapses of inner hair cells (IHC) in the cochlea. The Otoferlin has many C2 regions called domains, which are calcium-binding, used to interact with other molecules. Deafness is caused by an almost complete loss of calcium in the exocytosis of IHC. This alteration results in a hearing loss characterized as non-syndromic sensorineural of autosomal recessive inheritance, usually from severe to profound degree and of prelingual manifestation(3).
Since the 90s, researchers have investigated the audiological results of the ANSD; more recently, the consequences of this auditory alteration to communicative abilities have also been of interest, which has been of great value for the rehabilitation process. Bearing in mind to contribute to this research field, the present study had the aim to investigate the auditory and communicative abilities of two siblings with diagnosis of ANSD and the same OTOF mutation.
CLINICAL CASE PRESENTATION
This descriptive-qualitative research was approved by the Research Ethics Committee of the Pontifícia Universidade Católica de São Paulo, under number 131/2008. Subjects' legal guardians signed the free and informed consent term.
Participants were two children diagnosed with ANSD in a high complexity hearing health center in the city of São Paulo (Brazil).
Participants
Subject 1
Subject 1, male gender, was diagnosed with ANSD at 1 year of age. The audiological assessment conducted at the institution consisted of OAE, BAEP with CM testing, tympanometry with acoustic reflex testing, and visual reinforcement audiometry (VRA). Results obtained in the battery of tests were: presence of OAE, absence of BAEP with presence of CM, type A tympanometric curve with absence of stapedial reflexes bilaterally, and audiometric configuration indicating profound hearing loss.
After evaluation, the child went through the process of indication and adaptation of hearing aids (HA) bilaterally, and initiated speech-language therapy, which was carried out until 2 years of age. Then, he stopped attending therapy at the institution.
The subject always used HA for long periods of time during the day, removing it only to play, shower and sleep. However, the parents put the device on the child's ear, and, when they didn't, he did not miss it, and could not tell whether the HA was working or not (e.g. when it was out of batteries).
The child was enrolled in a special school for deaf children at 3 years of age, when he started using Brazilian Sign Language (LIBRAS) and undergoing therapy with the school's speech-language therapist. When this study was conducted, subject 1 was 9 years old, used HA regularly, and was enrolled in speech-language therapy. His recent audiological assessments showed presence of OAE, type A tympanometric curve with absence of stapedial reflexes, and bilateral profound hearing loss.
Subject 2
Subject 2, female gender, was submitted to audiological assessment at the institution at 2 months of age, due to the auditory alterations diagnosed in her brother (subject 1), without defined etiology. In the first audiological assessment, results showed present OAE bilaterally, absence of BAEP in the right ear (detected in screening procedure), and absence of cochleopalpebral reflex in instrumental evaluation.
At 1 year and 10 months, a new audiological assessment was conducted. At the time, the OAE responses were still present; however, the pure-tone audiometry obtained no responses. After this assessment, the child failed to attend the institution.
At 4 years of age, the subject came back to the institution. According to the parents, she was enrolled in a special school for deaf children when she was 2 years old, and started learning LIBRAS. Audiological assessments were conducted regularly at the school. From 2 to 3 years of age, the child was regularly assessed, and bilateral HA were indicated for her case. Initially, she avoided using them, and the parents supposed that was because the child obtained no benefits from the device.
At the institution, new audiological assessments were conducted, with the same results: present OAE and absence of responses in pure-tone audiometry and in BAEP. The child started audiological follow-up at th e institution, went through a new HA selection and adaptation process, and was enrolled in speech-language therapy. Until 5 years of age, the audiometric configuration showed profound hearing loss. At 6 years of age, audiometric thresholds indicated bilateral fluctuating moderate to severe hearing loss.
At the time of this study, subject 2 was 8 years old and enrolled in speech-language therapy. Recent audiological assessments indicated mild hearing loss, with presence of OAE, type A tympanometric curve with absence of acoustic reflexes, and absence of BAEP waves. Based on parents' report, the child presented fluctuating hearing abilities. According to them, the HA were used only when she had greater hearing difficulties.
The siblings with ANSD diagnosis presented mutation of the Otoferlin gene as etiological cause. According to the genetic report, both children have autosomal recessive inheritance, and are carriers of the same genetic mutation in the OTOF: c.5431A>T (K1811X) on exon 44.
Procedures
The procedures described below were carried out with both subjects.
Stage 1: Characterization of the communicative performance of the subjects, according to data collected in interviews with family members.
Stage 2: Speech perception evaluation using the "Procedure for Speech Perception Evaluation in Deaf Children with Profound Hearing Loss"(4). Tests were conducted with and without the HA, with speakerphone and in soundproof booth, keeping a one-meter distance between the child and the evaluator, eliminating the possibility of orofacial reading. Based on the results obtained, children were classified into hearing categories (Appendix 1 Appendix 1 - Click to enlarge ).
Stage 3: Assessment of communicative abilities using the Behavior Observation Protocol (PROC)(5). Children were video-recorded for 40 minutes in an interactive playful situation with the evaluator, using pre-selected toys, for posterior analysis. The PROC was used in an adapted manner, assessing only the following aspects: communicative abilities, and verbal comprehension. Based on the results obtained, general characteristics regarding communicative abilities, linguistic organization, and oral language comprehension were attributed, according to the parameter proposed by the instrument.
RESULTS
Subjects' communicative performance
According to data collected in interviews with the family members, the subjects were always within the same communicative environment, both at home and at school. However, they were very different from each other regarding communication development.
Subject 1 did not vocalize to obtain attention from others, and rarely used his voice spontaneously during communicative situations. His oral language was difficult to understand, even by familiar individuals, and his communication was based on representative gestures or LIBRAS.
Subject 2, on the other hand, always used more oral language, however, with preference for isolated words, mostly comprehended only by familiar individuals. She also used LIBRAS and symbolic gestures.
Due to her fluctuating hearing loss, it is hard to precisely determine the audibility of subject 2. Hence, in both cases, the study was based on hearing thresholds obtained when the speech perception and communicative abilities evaluations were conducted.
Speech perception
Below are presented the results obtained in the procedures of speech perception evaluation in each case.
It is emphasized that, in the speech perception evaluation, subject 1 was tested with and without the HA. However, the classification of hearing category was established based on the results obtained with the device, considering that, with its use, auditory perception is improved. Subject 2, on the other hand, was assessed without HA, considering the mean pure-tone thresholds of 500 Hz, 1 and 2 kHz within normal parameters on the day of testing. The hearing category was established based on the results obtained without the device.
The results of subject 1 in the speech perception evaluation showed no difference between responses obtained with or without the HA (Table 1). It was evidenced that the device had been improving only sound detection, vocalic discrimination, and vowel length discrimination abilities; however, little improvement was obtained regarding the abilities of word recognition and sentence comprehension. This means that the child was in hearing category 2, that is, he detected the presence of speech signal and was beginning to differentiate words using supra-segmental features.
Subject 2, even without the HA, obtained good results on the speech perception test, although she also had difficulties in more complex auditory abilities, such as sentence comprehension (Table 2).
Communicative abilities
Subject 1 was assessed with the HA, in order to have his auditory perception improved. The child responded unsystematically to oral language, but presented plurifunctional intentional communication, with great participation in dialogic activity through non-verbal symbolic means.
Subjects 2 was assessed without the HA, considering the mean pure-tone thresholds within normal parameters, registered in audiometry on the day of testing. The child comprehended orders of up to two actions related to the immediate context, and had plurifunctional intentional communication, with great participation in dialogic activity through verbal means related to the immediate context.
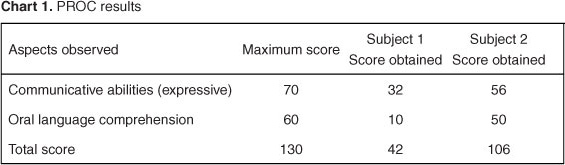
The PROC results of both children were obtained, allowing the comparison between their scores (Chart 1).
The results of all assessments conducted with both children were also registered, discriminating relevant qualitative aspects regarding auditory perception, verbal comprehension, and communicative abilities (Chart 2).
DISCUSSION
The ANSD has been the object of study of many researchers for years. However, despite of numerous findings about this condition, many issues are yet to be clarified.
The ANSD is a hearing alteration that comprises a heterogeneous population, with different etiologies and lesion sites; similarities or variations both in tests results and hearing behavior can also occur. Hence it is a challenge to propose the most efficient rehabilitation method for each case.
In the present study, both siblings presented genetic inheritance as the only etiological factor; their medical records did not register any pre-, peri- or post-natal factors that might suggest additional etiologies. A recent study with significant casuistry has also shown that this is the most evidenced etiology in cases of ANSD(6).
Both children had mutation in a single allele of the OTOF gene. However, as in another study(7), the mutations identified in the present study are not yet described in literature. Thus, even being considered one of the most common etiologies of ANSD, the exons of this gene must be researched in order to identify the greatest number of possible pathogenic mutations.
The main complaint found among cases of ANSD is speech perception difficulty, especially in the presence of noise(8). Since measuring the influence of noise on the speech perception of these children was not a purpose of this study, we opted to conduct the assessment of this ability only in silence, within a soundproof booth. The results of this assessment showed that the subjects had difficulties mainly in tasks that involved words or sentences.
Both subjects were not able to complete the Sentence Comprehension task of the speech perception test, a difficulty that was also identified on the speech comprehension item of the PROC. This might be associated to the limited benefits provided by the HA as an electronic device to be used in the habilitation and rehabilitation process of some ANSD cases, but also to the temporal resolution impairment, which is related to the competence to analyze and differentiate distinct linked sound events - an essential ability for speech comprehension and for the acquisition and development of linguistic abilities.
Since the diagnosis itself and the lesion site are still very difficult to be determined in ANSD cases, the resources for (re)habilitation are also currently very explored and discussed. There are still doubts and questions regarding methods and approaches to be used in speech-language therapy, and the moment at which cochlear implant (CI) should be indicated.
Some studies have suggested that the HA is not the most indicated intervention approach for ANSD cases, regardless the degree of hearing loss, because the amplified stimulus that reaches the cochlea is not conducted to the auditory nerve, due to the dyssynchrony found in auditory pathways. Hence, the conventional hearing aid would be able to improve only on sensitivity or audibility, contributing very little to the improvement of speech perception(9). The results found in the speech perception tests of the subjects in this study are compatible to those found in existent literature, since the use of the HA was also not effective for the development of more complex auditory abilities. Similar results were also found in a research(6) in which 85 out of 260 patients were adapted with HA, but only 15% of them obtained benefits for speech comprehension and oral language acquisition.
Studies have been showing that ANSD cases present improvements on auditory behavior with CI. However, the results on speech perception tests can be inferior when compared to cases of sensorineural hearing loss also implanted(9,10).
Some researchers recommend CI for all subjects that do not present benefits from HA(11,12). Other authors refer that caution should be taken, instead of indicating CI for all children with ANSD. There may be cases where electrical stimulation is not a good choice due to the lack of synchrony in the auditory nerve, as observed in patients with cochlear nerve deficiency (who are not candidates to implantation)(13).
In cases with mutation in the OTOF gene, there is a consensus that the lesion site is on the IHC, and that there is possibly a sufficient number of auditory nerve fibers and ganglion cells able to respond to electrical stimulation. Thus, individuals with this mutation are potential candidates to the benefits of CI, which will probably help to improve audiometric thresholds, as well as the development of auditory and linguistic abilities(14). However, one must consider that studies about this gene are still being developed, and there is no current evidence of the benefits of CI in children with the same mutation of the siblings studied.
Another aspect to be highlighted concerns the fluctuating thresholds registered in the audiometric assessment of subject 2, even though, in the last evaluations, these thresholds were close to the normal standards. This fluctuation was also noted by the family. According to parents' reports, the child started gradually and more frequently to notice the presence of sound stimuli, even those of low intensity. However, in the course of evaluations, it was possible to observe that she had limited use of oral language, apparently not compatible with the audiological results (which were next to normal).
A study(15) have reported a case of ANSD similar to our subject 2, with audiometric thresholds compatible with mild to moderate bilateral hearing loss. After being implanted in one ear, there was improvement in word recognition, even in the presence of noise. However, this conduct should be taken carefully, considering the variability found among subjects with ANSD, especially when there is fluctuating hearing loss. Hence, authors(1) have suggested the conduction of audiological monitoring for subjects with possible transitory or evolutive forms of the auditory status, with the main purpose to provide a hearing rehabilitation compatible with the conditions and necessities of each individual.
Considering the temporal resolution alteration caused by ANSD, we agree with the statement that the audiogram and the degree of hearing loss are not enough to presume speech perception abilities. This information reflects only one audibility measure in the many frequencies of the audiogram.
For the siblings studied, the HA was elected for the habilitation and rehabilitation process. However, it is clear that sound amplification was not enough for these children to develop auditory and linguistic abilities. One should consider that, at the time of diagnosis, little was known about the intervention possibilities for ANSD cases, and clinical and scientific improvement was needed to obtain the current knowledge regarding this type of hearing alteration.
Regarding the general communicative abilities, although the subjects were within the same communicative environment, they were always very different from each other in communication. Subject 1 used more gestures and LIBRAS, and avoided oral language, even when required. Subject 2, in comparison, used more oral language, however in a restrict way, usually through unintelligible sounds and/or short utterances. We also did not find in literature reports of children with ANSD who presented problems with communicative intention. In this perspective, it is observed that the siblings in this study also presented intentional interpersonal interaction.
We know that the quality of family interactions favors the communicative performance, in general. Nevertheless, it is not possible to affirm that the familiar context provides the same effects on the communicative behavior of each of its members, because factors related to individual subjective functioning may interfere in this condition.
Finally, we emphasize that the ANSD is a condition that still needs further study, both regarding its characteristics and the clinical results obtained by speech-language intervention, especially related to communicative performance.
FINAL COMMENTS
Although diagnosed with the same hearing impairment - ANSD - and with the same etiological factor - mutation in the Otoferlin gene -, and sharing consanguinity bonds, the children in this study developed diverse and peculiar auditory and communicative abilities. This finding, besides outlining the complexity of this type of clinical condition, suggests that the acquisition of these abilities is affected by singular subjective content that should not be ignored during speech-language assessment and intervention.
ACKNOWLEDGEMENTS
We thank the Child Hearing Center (Centro Audição na Criança - CeAC), Division of Education and Rehabilitation of Communication Disorders (Divisão de Educação e Reabilitação dos Distúrbios da Comunicação - DERDIC) of the Pontifícia Universidade Católica de São Paulo (PUC-SP), for their support and for allowing the conduction of this study, and the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES), for the grants provided for this research. We also acknowledge the parents that allowed the participation of their children in this study.
Received: 10/18/2011
Accepted: 1/12/2012
Study conducted at the Graduate Program in Speech-Language Pathology and Audiology, Pontifícia Universidade Católica de São Paulo - PUC - São Paulo (SP), Brazil
Conflict of interests: None
- 1. Hayes D, Sininger Y. Guidelines for identification and management of infants and young children with auditory neuropathy spectrum disorder. In: Proceedings of the Guidelines Development Conference at NHS; 2008; Como, Italy.
- 2. Rabelo CM. Avaliação eletrofisiológica e comportamental do processamento temporal [tese]. São Paulo: Universidade de São Paulo, Faculdade de Medicina; 2008.
- 3. Yasunaga S, Grati M, Chardenoux S, Smith TN, Friedman TB, Lalwani AK, et al. OTOF encodes multiple long and short isoforms: genetic evidence that the long ones underlie recessive deafness DFNB9. Am J Hum Genet. 2000;67(3):591-600.
- 4. Bevilacqua MC, Tech EA. Elaboração de um procedimento de avaliação de percepção de fala em crianças deficientes auditivas profundas a partir de cinco anos de idade. In: Marchesan IQ, Zorzi JL,Gomes IC. Tópicos em fonoaudiologia. São Paulo: Lovise; 1996. p. 411-33.
- 5. Zorzi JL, Hage SR. PROC-Protocolo de observação comportamental. São José dos Campos: Pulso; 2004.
- 6. Berlin CI, Hood LJ, Morlet T, Wilensky D, Li L, Mattingly KR, et al. Multi-site diagnosis and management of 260 patients with auditory neuropathy/dys-synchrony (auditory neuropathy spectrum disorder). Int J Audiol. 2010;49(1):30-43.
- 7. Rodríguez-Ballesteros M, Reynoso R, Olarte M, Villamar M, Morera C, Santarelli R, et al. A multicenter study on the prevalence and spectrum of mutations in the otoferlin gene (OTOF) in subjects with nonsyndromic hearing impairment and auditory neuropathy. Hum Mutat. 2008;29(6):823-31.
- 8. Raveh E, Buller N, Badrana O, Attias J. Auditory neuropathy: clinical characteristics and therapeutic approach. Am J Otolaryngol. 2007;28(5):302-8.
- 9. Gibson WP, Sanli H. Auditory neuropathy: an update. Ear Hear. 2007;28(2 Suppl):102S-106S.
- 10. Rance G, Barker EJ. Speech perception in children with auditory neuropathy/dyssynchrony managed with either hearing aids or cochlear implants. Otol Neurotol. 2008;29(2):179-82.
- 11. Postelmans JT, Stokroos RJ. Cochlear implantation in a patient with deafness induced Chacot-Marie-Tooth disease (hereditary motor and sensory neuropathies). J Laryngol Otol. 2006;120(6):508-10.
- 12. Jeong SW, Kim LS, Kim BY, Bae WY, Kim JR. Cochlear implantation in children with auditory neuropathy: outcomes and rationale. Acta Otolaryngol Suppl. 2007;(558):36-43.
- 13. Teagle HF, Roush PA, Woodard JS, Hatch DR, Zdanski CJ, Buss E, et al. Cochlear implantation in children with auditory neuropathy spectrum disorder. Ear Hear. 2010;31(3):325-35.
- 14. Rouillon I, Marcolla A, Roux I, Marlin S, Feldmann D, Couderc R, et al. Results of cochlear implantation in two children with mutations in the OTOF gene. Int J Pediatr Otorhinolaryngol. 2006;70(4):689-96.
- 15. Shallop J. Auditory neuropathy/dys-synchrony in adults and children. Semin Hear. 2002;23(3):215-24.
Appendix 1 - Click to enlarge

Publication Dates
-
Publication in this collection
20 July 2012 -
Date of issue
2012
History
-
Received
18 Oct 2011 -
Accepted
12 Jan 2012