Abstracts
Introduction:
Attentional bias, the tendency that a person has to drive or maintain attention to a specific class of stimuli, may play an important role in the etiology and persistence of mental disorders. Attentional bias modification has been studied as a form of additional treatment related to automatic processing.
Objectives:
This systematic literature review compared and discussed methods, evidence of success and potential clinical applications of studies about attentional bias modification (ABM) using a visual probe task.
Methods:
The Web of Knowledge, PubMed and PsycInfo were searched using the keywords attentional bias modification, attentional bias manipulation and attentional bias training. We selected empirical studies about ABM training using a visual probe task written in English and published between 2002 and 2014.
Results:
Fifty-seven studies met inclusion criteria. Most (78%) succeeded in training attention in the predicted direction, and in 71% results were generalized to other measures correlated with the symptoms.
Conclusions:
ABM has potential clinical utility, but to standardize methods and maximize applicability, future studies should include clinical samples and be based on findings of studies about its effectiveness.
Behavior therapy; cognitive therapy; outcome studies; experimental psychology
Introdução:
O viés atencional, definido como a tendência a direcionar ou manter a atenção focada em uma classe específica de estímulos, pode ter um papel importante na etiologia e manutenção dos transtornos mentais. A modificação do viés atencional tem sido estudada como forma adicional de tratamento dirigida ao processamento automático.
Objetivos:
Esta revisão sistemática da literatura compara e discute questões metodológicas, evidências de resultados positivos e potenciais aplicações clínicas dos estudos sobre a modificação do viés atencional (MVA) baseados em uma tarefa de atenção visual.
Métodos:
As bases de dados Web of Knowledge, PubMed e PsycInfo foram pesquisadas usando os descritores attentional bias modification, attentional bias manipulation e attentional bias training. Foram selecionados estudos empíricos sobre treinamento para MVA baseados em tarefa de atenção visual escritos em inglês e publicados entre 2002 e 2014.
Resultados:
Cinquenta e sete estudos atenderam aos critérios de inclusão. A maioria (78%) obteve sucesso no treinamento da atenção na direção prevista, e 71% tiveram seus resultados generalizados a outras medidas correlacionadas com os sintomas.
Conclusões:
A MVA tem utilidade clínica potencial, mas, para atingir a padronização de métodos e a maximização de sua aplicabilidade, estudos futuros deverão incluir amostras clínicas e ser baseados nos resultados dos estudos sobre sua eficácia.
Terapia comportamental; terapia cognitiva; resultados de estudos; psicologia experimental
Introduction
Attentional bias is the tendency to drive or maintain attention to a particular class of stimuli.11. Williams JM, Mathews A, MacLeod C. The emotional Stroop task and psychopathology. Psychol Bull. 1996;120:3-24.,22. Lopes FM, Peuker AC, Bizarro L. Viés atencional em fumantes. Psico. 2008;39:280-8. In individuals affected by emotional disorders, such as anxiety, depression, phobia, posttraumatic stress disorder, eating disorder or addiction, attention toward events (words or images) related to their pathologies is increased.11. Williams JM, Mathews A, MacLeod C. The emotional Stroop task and psychopathology. Psychol Bull. 1996;120:3-24.,33. Peuker AC, Lopes FM, Bizarro L. Viés atencional no abuso de drogas: teoria e método. Psic Teor Pesq. 2009;25:603-9. In addictions, for example, attentional bias seems to be related to greater frequency and intensity of drug use, as drug-related stimuli produce a variety of responses associated with their effects, including craving, excitement and difficulty sustaining abstinence.44. Robbins SJ, Ehrman RN. The role of attentional bias in substance abuse. Behav Cogn Neurosci Rev. 2004;3:243-60. Similarly, the attentional system of anxious patients may be distinctly sensitive and biased in favor of threats than other environmental stimuli.55. Bar-Haim Y, Lamy D, Pergamin L, Bakermans-Kranenburg MJ, van IJzendoorn MH. Threat-related attentional bias in anxious and nonanxious individuals: a meta-analytic study. Psychol Bull. 2007;133:1-24. Therefore, attentional bias may play an important role in the etiology and persistence of these mental disorders.
As attention to events associated with a pathology may complicate its treatment, attentional bias modification (ABM) has been recently studied as an implicit training strategy to disengage attention from threatening events related to anxiety66. Amir N, Beard C, Burns M, Bomyea J. Attention modification program in individuals with generalized anxiety disorder. J Abnorm Psychol. 2009;118:28-33.
7. MacLeod C, Rutherford E, Campbell L, Ebsworthy G, Holker L. Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol. 2002;111:107-23.-88. Schmidt NB, Richey JA, Buckner JD, Timpano KR. Attention training for generalized social anxiety disorder. J Abnorm Psychol. 2009;118:5-14. and to prevent relapse in individuals with alcohol dependence,99. Field M, Duka T, Eastwood B, Child R, Santarcangelo M, Gayton M. Experimental manipulation of attentional biases in heavy drinkers: do the effects generalize? Psychopharmacology (Berl). 2007;192:593-608.,1010. Schoenmakers T, Wiers RW, Jones BT, Bruce G, Jansen AT. Attentional re-training decreases attentional bias in heavy drinkers without generalization. Addiction. 2007;102:399-405. as well as among smokers.1111. Attwood AS, O'Sullivan H, Leonards U, Mackintosh B, Munafo MR. Attentional bias training and cue reactivity in cigarette smokers. Addiction. 2008;103:1875-82.,1212. Field M, Duka T, Tyler E, Schoenmakers T. Attentional bias modification in tobacco smokers. Nicotine Tob Res. 2009;11:812-22. Of the techniques to achieve ABM included in studies, the most commonly used is a modified version of a visual probe task developed in 2002.77. MacLeod C, Rutherford E, Campbell L, Ebsworthy G, Holker L. Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol. 2002;111:107-23. In the standard visual probe task to assess attentional bias,1313. MacLeod C, Mathews A, Tata P. Attentional bias in emotional disorders. J Abnorm Psychol. 1986;95:15-20. a pair of images, one related to the pathology (target) and one control, originally from the same context of the target but which does not offer any clues to the pathology, are displayed side by side simultaneously on the screen of a computer. After a short time, the two images disappear and a small stimulus (e.g., an arrow) replaces one of the two images. Participants are asked to pay attention to the arrow and indicate its direction as quickly as possible. The arrow replaces the target images and the control images with equal frequency (50%). Response latency indicates visual attention to the stimuli presented.1414. Townshed JM, Duka T. Attentional bias with alcohol cues: differences between heavy and occasional social drinkers. Psychopharmacology (Berl). 2001;157:67-74. Thus, shorter reaction times when the arrow replaces a particular class of stimuli indicate an attentional bias to this type of stimulus.
This modified version of the visual probe task differs from the standard task only in the frequency with which the probe replaces relevant and non-relevant images. The participants are randomly assigned to groups that differ in probe location, that is, in the group that was trained to increase attentional bias (attend group), most of the time (or 100% of the times) the probe replaces the relevant image, whereas in the group trained to reduce attentional bias (avoid group), the probe replaces the non-relevant image. As participants detect and respond as quickly as possible to probe location, they tend, with time and repetition, to direct their attention to relevant images (attend group) or to non-relevant images (avoid group). In training for attention modification to reduce bias, the probe always replaces non-relevant images, and the implicit rule to automatically attend to stimuli that are non-anxiogenic or unrelated to the drug is learned. The objective of attentional training is to teach patients to avoid, or "disengage" from, generalized attention to events of actual exposure to cues, so that they learn to ignore relevant stimuli. As a result, individuals with an addiction may be able to prevent increases in craving, which improves their chances of maintaining abstinence, and patients with anxiogenic disorders may not experience increases in their levels of anxiety.
Despite the great importance of this topic, studies reviewing ABM have been limited to the analysis of anxiety and mood disorders, although ABM has been investigated in other fields, such as drug addiction and eating disorders. To our knowledge, three meta-analyses of the effects of ABM have been published in recent years, and they all focused on anxiety and depression.1515. Hakamata Y, Lissek S, Bar-Haim Y, Britton JC, Fox NA, Leibenluft, E, et al. Attention bias modification treatment: a meta-analysis toward the establishment of novel treatment for anxiety. Biol Psychiatry. 2010;68:982-90.
16. Hallion LS, Ruscio AM. A meta-analysis of the effect of cognitive bias modification on anxiety and depression. Psychol Bull. 2011;137:940-58.-1717. Beard C, Sawyer AT, Hofmann SG. Efficacy of attention bias modification using threat and appetitive stimuli: a meta-analytic review. Behav Ther. 2012;43:724-40. Other critical reviews of ABM also investigated anxiety and mood disorders.1818. Bar-Haim Y. Research review: attention bias modification (ABM): a novel treatment for anxiety disorders. J Child Psychol Psychiatry. 2010;51:859-70.
19. Browning M, Holmes EA, Harmer CJ. The modification of attentional bias to emotional information: a review of the techniques, mechanisms, and relevance to emotional disorders. Cogn Affect Behav Neurosci. 2010;10:8-20.-2020. MacLeod C, Mathews A. Cognitive bias modification approaches to anxiety. Annu Rev Clin Psychol. 2012;8:198-217. Our review aimed to provide a critical appraisal about methods and results of studies about ABM using modified a visual probe task in any field. The main focus of our analysis was to discuss method discrepancies and similarities in the use of the modified visual probe task and to compare findings with those reported in the studies included in the review, which may be useful to integrate current information about this type of intervention. Moreover, evidence related to the use of this technique was collected and systematically described, which may lead to insights to be applied to future studies and clinical practice.
Method
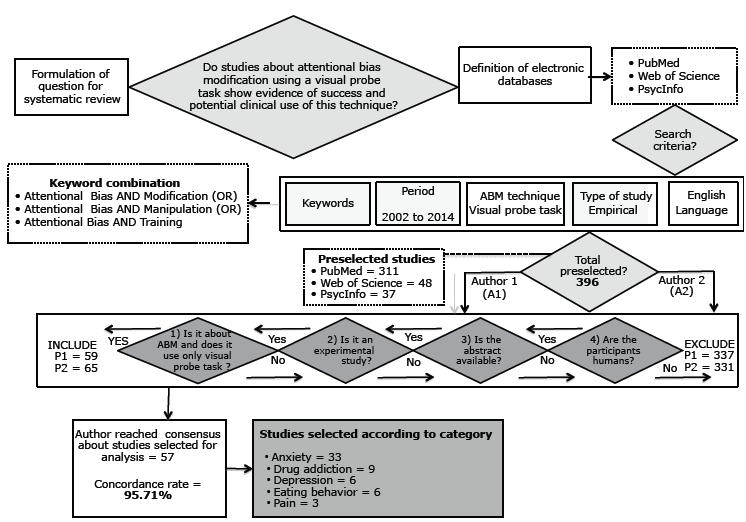
A systematic literature review was conducted in 2014 by searching PubMed, Web of Science and PsycInfo for studies published in the last twelve years (2002-2014). The following keywords were used: attentional bias modification, attentional bias manipulation and attentional bias training. The search was limited to empirical studies written in English.
Studies preselected using the search strategies described above were assessed independently by two authors, according to the following inclusion criteria: investigation of visual attentional bias modification using only a visual probe task; experimental study; abstract available; and study conducted with humans.
Duplicates and all studies that used any other interventions (except assessment) in addition to the visual probe task were excluded, and the final study selection was defined after author consensus was reached. Figure 1 shows the flowchart of the systematic search.
Results
The initial search in the three databases using the keywords listed above yielded 396 studies. After the exclusion of duplicates and the application of inclusion criteria, 57 studies were selected for the final analysis and classified according to the disorder that they investigated: anxiety (33), drug addiction (9), depression (6), eating behavior (6) and pain (3). Table 1 shows method variations, that is, discrepancies and similarities in the use of the visual probe task. Table 2 summarizes the results and the impact of the selected studies.
Anxiety
This category included 33 studies about specific topics, such as trait-anxiety, social phobia and posttraumatic stress disorder (26), as well as worrying (3) and stress (4). The analysis of bias training method revealed that, although all studies in this category included a visual probe task, not all used the same stimulus, which varied from words to faces. In addition, they did not use similar stimulus-onset asynchrony (SOA), which ranged from 20 to 1,500 ms. Besides task variations, differences in group design may also have affected results (Table 1).
Of the 14 studies that compared an avoid group (threat) with a control group, only five found no difference between groups after training.2121. Boettcher J, Berger T, Renneberg B. Internet-based attention training for social anxiety: a randomized controlled trial. Cognit Ther Res. 2012;36:522-36.
22. Carlbring P, Apelstrand M, Sehlin H, Amir N, Rousseau A, Hofmann SG, et al. Internet-delivered attention bias modification training in individuals with social anxiety disorder -- a double blind randomized controlled trial. BMC Psychiatry. 2012;12:66.
23. Julian K, Beard C, Schmidt NB, Powers MB, Smits JA. Attention training to reduce attention bias and social stressor reactivity: an attempt to replicate and extend previous findings. Behav Res Ther. 2012;50:350-8.
24. Schoorl M, Putman P, Van Der Does W. Attentional bias modification in posttraumatic stress disorder: a randomized controlled trial. Psychother Psychosom. 2013;82:99-105.-2525. Rapee RM, MacLeod C, Carpenter L, Gaston JE, Frei J, Peters L, et al. Integrating cognitive bias modification into a standard cognitive behavioural treatment package for social phobia: a randomized controlled trial. Behav Res Ther. 2013;51:207-15. In the other nine studies, there were differences between groups, and AB for threat was reduced in the avoid groups, when compared with the control group. However, only four of these studies found a correlation of AB after training with reduced symptoms of anxiety.66. Amir N, Beard C, Burns M, Bomyea J. Attention modification program in individuals with generalized anxiety disorder. J Abnorm Psychol. 2009;118:28-33.,2626. Hazen RA, Vasey MW, Schmidt NB. Attentional retraining: a randomized clinical trial for pathological worry. J Psychiatr Res. 2009;43:627-33.
27. Heeren A, Lievens L, Philippot P. How does attention training work in social phobia: disengagement from threat or re-engagement to non-threat? J Anxiety Disord. 2011;25:1108-15.-2828. See J, MacLeod C, Bridle R. The reduction of anxiety vulnerability through the modification of attentional bias: a real-world study using a home-based cognitive bias modification procedure. J Abnorm Psychol. 2009;118:65-75. The other five studies2929. Heeren A, Philippot P, Koster EH. Impact of the temporal stability of preexistent attentional bias for threat on its alteration through attention bias modification. J Behav Ther Exp Psychiatry. 2015;49(Pt A):69-75.
30. Amir N, Taylor CT, Donohue MC. Predictors of response to an attention modification program in generalized social phobia. J Consult Clin Psychol. 2011;79:533-41.
31. Eldar S, Bar-Haim Y. Neural plasticity in response to attention training in anxiety. Psychol Med. 2010;40:667-77.
32. Koster EH, Baert S, Bockstaele M, De Raedt R. Attentional retraining procedures: manipulating early or late components of attentional bias? Emotion. 2010;10:230-6.-3333. Reese HE, McNally RJ, Najmi S, Amir N. Attention training for reducing spider fear in spider-fearful individuals. J Anxiety Disord. 2010;24:657-62. found no effects of generalization on AB reduction or correlations with other variables.
Of the seven studies that compared an avoid group (threat) with an attend group, five found a difference between groups, as AB for threat increased in the attend groups and decreased in the avoid groups. A generalization to new stimuli or other measures was found in three of these five studies,77. MacLeod C, Rutherford E, Campbell L, Ebsworthy G, Holker L. Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol. 2002;111:107-23.,1919. Browning M, Holmes EA, Harmer CJ. The modification of attentional bias to emotional information: a review of the techniques, mechanisms, and relevance to emotional disorders. Cogn Affect Behav Neurosci. 2010;10:8-20.,3434. MacLeod C, Soong LY, Rutherford EM, Campbell LW. Internet-delivered assessment and manipulation of anxiety-linked attentional bias: validation of a free-access attentional probe software package. Behav Res Methods. 2007;39:533-8. which suggests a potential clinical use for the technique under study here. However, two of them did not find any correlation with other measures.3535. Van Bockstaele B, Verschuere B, Koster EH, Tibboel H, De Houwer J, Crombez G. Effects of attention training on self-reported, implicit, physiological and behavioural measures of spider fear. J Behav Ther Exp Psychiatry. 2011;42:211-8.,3636. Van Bockstaele B, Koster EH, Verschuere B, Crombez G, De Houwer J. Limited transfer of threat bias following attentional retraining. J Behav Ther Exp Psychiatry. 2012;43:794-800. The other two studies found that ABM was efficient in inducing an AB for threat, but inefficient in inducing a bias away from threat3737. Eldar S, Ricon T, Bar-Haim Y. Plasticity in attention: implications for stress response in children. Behav Res Ther. 2008;46:450-61. and that ABM was efficient in both groups only when AB was found in the pretest.3838. O'Toole L, Dennis TA. Attention training and the threat bias: an ERP study. Brain Cogn. 2012;78:63-73.
In contrast, all six studies that compared attend groups with control groups found an effect of ABM. Two of these studies manipulated the attend group to threat or negative stimuli3939. Heeren A, Peschard V, Philippot P. The causal role of attentional bias for threat cues in social anxiety: a test on a cyber-ostracism task. Cognit Ther Res. 2012;36:512-21.,4040. Krebs G, Hirsch CR, Mathews A. The effect of attention modification with explicit vs. minimal instructions on worry. Behav Res Ther. 2010;48:251-6. and four, to positive stimuli.4141. Hayes S, Hirsch CR, Mathews A. Facilitating a benign attentional bias reduces negative thought intrusions. J Abnorm Psychol. 2010;119:235-40.
42. Li S, Tan J, Qian M, Liu X. Continual training of attentional bias in social anxiety. Behav Res Ther. 2008;46:905-12.
43. Taylor CT, Bomyea J, Amir N. Malleability of attentional bias for positive emotional information and anxiety vulnerability. Emotion. 2011;11:127-38.-4444. Wadlinger HA, Isaacowitz DM. Looking happy: the experimental manipulation of a positive visual attention bias. Emotion. 2008;8:121-6. The first two found that the treated groups increased AB for threat or negative stimuli when compared with the control groups. They also found that the effects correlated with higher anxiety scores3939. Heeren A, Peschard V, Philippot P. The causal role of attentional bias for threat cues in social anxiety: a test on a cyber-ostracism task. Cognit Ther Res. 2012;36:512-21. and were potentiated by explicit instructions before training.4040. Krebs G, Hirsch CR, Mathews A. The effect of attention modification with explicit vs. minimal instructions on worry. Behav Res Ther. 2010;48:251-6. Likewise, the four studies that used positive training increased AB for positive stimuli. Moreover, they had a negative correlation with anxiety,4242. Li S, Tan J, Qian M, Liu X. Continual training of attentional bias in social anxiety. Behav Res Ther. 2008;46:905-12. stress reactivity,4343. Taylor CT, Bomyea J, Amir N. Malleability of attentional bias for positive emotional information and anxiety vulnerability. Emotion. 2011;11:127-38. fewer negative thought intrusions in a worry test4545. Amir N, Taylor CT. Combining computerized home-based treatments for generalized anxiety disorder: an attention modification program and cognitive behavioral therapy. Behav Ther. 2012;43:546-59. and generalization to other measures of stress.4444. Wadlinger HA, Isaacowitz DM. Looking happy: the experimental manipulation of a positive visual attention bias. Emotion. 2008;8:121-6.
Of the three studies that used only avoid groups, one did not conduct a post test because it did not find AB for threat at baseline,4646. Cowart MJ, Ollendick TH. Attention training in socially anxious children: a multiple baseline design analysis. J Anxiety Disord. 2011;25:972-7. whereas the other two found a reduction in the post-training AB, with effects generalized to other scales and self-reported symptoms of anxiety, worrying and depression.4545. Amir N, Taylor CT. Combining computerized home-based treatments for generalized anxiety disorder: an attention modification program and cognitive behavioral therapy. Behav Ther. 2012;43:546-59.,4747. Brosan L, Hoppitt L, Shelfer L, Sillence A, Mackintosh B. Cognitive bias modification for attention and interpretation reduces trait and state anxiety in anxious patients referred to an out-patient service: results from a pilot study. J Behav Ther Exp Psychiatry. 2011;42:258-64. However, the two studies4848. Heeren A, Reese HE, McNally RJ, Philippot P. Attention training toward and away from threat in social phobia: effects on subjective, behavioral, and physiological measures of anxiety. Behav Res Ther. 2012;50:30-9.,4949. Klumpp H, Amir N. Preliminary study of attention training to threat and neutral faces on anxious reactivity to a social stressor in social anxiety. Cognit Ther Res. 2010;34:263-71. that used avoid, attend and control group found different results. In the first study, the avoid group had less AB for threat than both attend and control groups, with no differences between avoid and control groups. Moreover, the avoid group had a greater reduction of in self-reported, behavioral and physiological measures of anxiety than did the other two groups. The second study found no differences between groups after training. Finally, the other study trained three groups: attend (to threat), attend (to positive stimulus) and control.5050. Boettcher J, Leek L, Matson L, Holmes EA, Browning M, MacLeod C, et al. Internet-based attention bias modification for social anxiety: a randomised controlled comparison of training towards negative and training towards positive cues. PLoS One. 2013;8:e71760. It found no differences between groups and no other effects after training, and the authors suggested that their results might be due to an absence of attentional bias at baseline in all groups.
Drug addiction
This category included nine studies about alcohol users (7) and tobacco smokers (5). The analysis of bias training method revealed that all used the same stimulus (drug-neutral images), and that only in SOA varied: 50, 200 and 500 ms.
The two studies that included attend (to drug) and avoid groups1111. Attwood AS, O'Sullivan H, Leonards U, Mackintosh B, Munafo MR. Attentional bias training and cue reactivity in cigarette smokers. Addiction. 2008;103:1875-82.,5151. Field M, Eastwood B. Experimental manipulation of attentional bias increases the motivation to drink alcohol. Psychopharmacology (Berl). 2005;183:350-7. found differences between groups, as AB increased in the attend groups and decreased in the avoid groups. Moreover, in one of the studies with smokers, post-training AB correlated positively with craving to smoke in the attend group, but only among men1111. Attwood AS, O'Sullivan H, Leonards U, Mackintosh B, Munafo MR. Attentional bias training and cue reactivity in cigarette smokers. Addiction. 2008;103:1875-82.; and in one of the studies about alcohol use, the urge to drink and beer consumption in the attend group was greater in the avoid alcohol.5151. Field M, Eastwood B. Experimental manipulation of attentional bias increases the motivation to drink alcohol. Psychopharmacology (Berl). 2005;183:350-7. In contrast, of the five studies that compared avoid (to drug) and control groups, only one found no differences between groups.5252. McHugh RK, Murray HW, Hearon BA, Calkins AW, Otto MW. Attentional bias and craving in smokers: the impact of a single attentional training session. Nicotine Tob Res. 2010;12:1261-4. The two studies about alcohol use1010. Schoenmakers T, Wiers RW, Jones BT, Bruce G, Jansen AT. Attentional re-training decreases attentional bias in heavy drinkers without generalization. Addiction. 2007;102:399-405.,5353. Schoenmakers TM, de Bruin M, Lux IF, Goertz AG, Van Kerkhof DH, Wiers RW. Clinical effectiveness of attentional bias modification training in abstinent alcoholic patients. Drug Alcohol Depend. 2010;109:30-6. found differences between groups in the post-test. In one of them, AB in the avoid group decreased only in the case of old stimuli and did not correlate with craving.1010. Schoenmakers T, Wiers RW, Jones BT, Bruce G, Jansen AT. Attentional re-training decreases attentional bias in heavy drinkers without generalization. Addiction. 2007;102:399-405. In the other study, AB in the avoid group decreased when compared with the control group at SOA 500 ms, but not at 200 ms, and generalized to new stimuli, but did not correlate with craving.5353. Schoenmakers TM, de Bruin M, Lux IF, Goertz AG, Van Kerkhof DH, Wiers RW. Clinical effectiveness of attentional bias modification training in abstinent alcoholic patients. Drug Alcohol Depend. 2010;109:30-6. The latter had the largest number of trials in this category, and although the AB did not correlate with craving, the participants in the avoid group took longer to relapse and were discharged earlier than those in the control group. The study that offered training to avoid smoking cues on a personal digital assistant to smokers that were not seeking to quit found differences between the avoid and control groups, which correlated with craving but did not affect smoking behavior.5454. Kerst WF, Waters AJ. Attentional retraining administered in the field reduces smokers' attentional bias and craving. Health Psychol. 2014;33:1232-40. In contrast, in the study that included smokers trying to quit, evaluated different numbers of training sessions and followed up participants for 1 year, the assessment of attentional bias revealed differences between groups in the desired direction, but results did not correlate with craving or influenced participants to stop smoking.5555. Lopes FM, Pires AV, Bizarro L. Attentional bias modification in smokers trying to quit: a longitudinal study about the effects of number of sessions. J Subst Abuse Treat. 2014;47:50-7.
Finally, of the two studies that compared attend (to drug), avoid (to drug) and control groups, the study with tobacco smokers found post-test differences between groups only for old stimuli, with a higher AB in the attend than in the other groups, but no differences between the avoid and control groups. However, this difference did not remain on the following day,1212. Field M, Duka T, Tyler E, Schoenmakers T. Attentional bias modification in tobacco smokers. Nicotine Tob Res. 2009;11:812-22. and ABM had no effects on subjective craving or behavioral measures of tobacco seeking. The study about alcohol users99. Field M, Duka T, Eastwood B, Child R, Santarcangelo M, Gayton M. Experimental manipulation of attentional biases in heavy drinkers: do the effects generalize? Psychopharmacology (Berl). 2007;192:593-608. found differences, as AB increased in the attend group (alcohol) from pre- to post-test, and this effect was clear for both old and new stimuli. In addition, craving in the attend group increased only in the group of participants that were aware of the experimental contingencies during attentional training. There were no differences in alcohol consumption between groups.
Depression
This category included six studies about depression (5) and mood (1). The analysis of the method used to train bias revealed that not all the six studies used the same stimulus, as they used words or faces, or the same SOAs, which varied from 500 to 2,000 ms. Positive results were found in both studies that used attend (to positive) and control groups.5656. Browning M, Holmes EA, Charles M, Cowen PJ, Harmer CJ. Using attentional bias modification as a cognitive vaccine against depression. Biol Psychiatry. 2012;72:572-9.,5757. Haeffel GJ, Rozek DC, Hames JL, Technow J. Too much of a good thing: testing the efficacy of a cognitive bias modification task for cognitively vulnerable individuals. Cognit Ther Res. 2012;36:493-501. Both reported differences between groups, as participants in the attend groups were much more likely to attend to adaptive stimuli relative to maladaptive stimuli than participants in the control group. In addition, positive ABM using faces (but not words) reduced two risk measures of depressive recurrence,5656. Browning M, Holmes EA, Charles M, Cowen PJ, Harmer CJ. Using attentional bias modification as a cognitive vaccine against depression. Biol Psychiatry. 2012;72:572-9. and participants in the attend group reported fewer depressive symptoms and had greater persistence on a difficult laboratory task.5757. Haeffel GJ, Rozek DC, Hames JL, Technow J. Too much of a good thing: testing the efficacy of a cognitive bias modification task for cognitively vulnerable individuals. Cognit Ther Res. 2012;36:493-501.
The study that compared attend-to-positive and attend-to-negative groups found differences in AB according to age. In the group of young adults, negative training resulted in fewer post-training fixations to the most negative areas of the images, whereas positive training seemed to be more successful in changing fixation patterns in the group of older adults. Furthermore, moods were not affected by training among young adults, whereas older adults in the attend-to-negative group had the worst moods after training.5858. Isaacowitz DM, Choi Y. The malleability of age-related positive gaze preferences: training to change gaze and mood. Emotion. 2011;11:90-100. A recent study5959. Yang W, Ding Z, Dai T, Peng F, Zhang JX. Attention Bias Modification training in individuals with depressive symptoms: a randomized controlled trial. J Behav Ther Exp Psychiatry. 2015;49(Pt A):101-11. that provided an eight-session training and compared an avoid group with a control group found a significant reduction of attentional bias to stimuli, as well as reductions in depressive symptoms at post-training. These results were confirmed at 3-month follow-up assessments, and more participants remained asymptomatic in the ABM group from immediate post-training to 7-month follow-ups. In this study, ABM also significantly reduced secondary outcome measures, such as rumination and trait anxiety. In contrast, the study that compared attend (to positive) and avoid (from negative) groups with a control group using a 10-session training program6060. Baert S, De Raedt R, Schacht R, Koster EH. Attentional bias training in depression: therapeutic effects depend on depression severity. J Behav Ther Exp Psychiatry. 2010;41:265-74. and the study that compared avoid and control groups using a single-session training6161. Tsumura H, Shimada H, Nomura K, Sugaya N, Suzuki K. The effects of attention retraining on depressive mood and cortisol responses to depression-related stimuli. Jpn Psychol Res. 2012;54:400-11. found no differences or any other impact of ABM between groups.
Eating behavior
This category included studies about eating disorders, as well as those that explored the effect of attention training on levels of satisfaction with body, considering that AB for body parts that is evaluated negatively may have a causal association with eating disorders and body dissatisfaction. Six studies were identified,6262. Kemps E, Tiggemann M, Elford J. Sustained effects of attentional re-training on chocolate consumption. J Behav Ther Exp Psychiatry. 2015;49(Pt A):94-100.
63. Kakoschke N, Kemps E, Tiggemann M. Attentional bias modification encourages healthy eating. Eat Behav. 2014;15:120-4.
64. Boutelle KN, Kuckertz JM, Carlson J, Amir N. A pilot study evaluating a one-session attention modification training to decrease overeating in obese children. Appetite. 2014;76:180-5.
65. Kemps E, Tiggemann M, Orr J, Grear J. Attentional retraining can reduce chocolate consumption. J Exp Psychol Appl. 2014;20:94-102.
66. Kemps E, Tiggemann M, Hollitt S. Biased attentional processing of food cues and modification in obese individuals. Health Psychol. 2014;33:1391-401.-6767. Smeets E, Jansen A, Roefs A. Bias for the (un)attractive self: on the role of attention in causing body (dis)satisfaction. Health Psychol. 2011;30:360-7. and their tasks did not vary substantially, as they all a SOA of 500 ms and 12-20 pairs of food as a stimulus, although five used pictures and one used words.
The three studies that compared attend and avoid groups6262. Kemps E, Tiggemann M, Elford J. Sustained effects of attentional re-training on chocolate consumption. J Behav Ther Exp Psychiatry. 2015;49(Pt A):94-100.,6565. Kemps E, Tiggemann M, Orr J, Grear J. Attentional retraining can reduce chocolate consumption. J Exp Psychol Appl. 2014;20:94-102.,6666. Kemps E, Tiggemann M, Hollitt S. Biased attentional processing of food cues and modification in obese individuals. Health Psychol. 2014;33:1391-401. found AB changes and a significant impact of training. In the study with obese participants, AB for food increased in the attend group and decreased in the avoid group, and the effects generalized to an independent measure of attentional bias.6666. Kemps E, Tiggemann M, Hollitt S. Biased attentional processing of food cues and modification in obese individuals. Health Psychol. 2014;33:1391-401. The two studies that investigated ABM for chocolate achieved the same positive outcome, as AB for chocolate cues increased in the attend group and decreased in the avoid group, and these training effects generalized to novel, previously unseen chocolate pictures. Moreover, attentional retraining affected chocolate consumption and craving, and participants in the avoid group ate less chocolate in a so-called taste test than did those in the attend group.6262. Kemps E, Tiggemann M, Elford J. Sustained effects of attentional re-training on chocolate consumption. J Behav Ther Exp Psychiatry. 2015;49(Pt A):94-100.,6565. Kemps E, Tiggemann M, Orr J, Grear J. Attentional retraining can reduce chocolate consumption. J Exp Psychol Appl. 2014;20:94-102.
Similar encouraging results were found in two other recent studies.6363. Kakoschke N, Kemps E, Tiggemann M. Attentional bias modification encourages healthy eating. Eat Behav. 2014;15:120-4.,6464. Boutelle KN, Kuckertz JM, Carlson J, Amir N. A pilot study evaluating a one-session attention modification training to decrease overeating in obese children. Appetite. 2014;76:180-5. In the first, groups were trained either to attend to healthy food or to attend to unhealthy food, and all participants showed an attentional bias toward unhealthy food cues at baseline. After training, participants in the healthy food group, but not those in the unhealthy food group, had a significant increase in AB and ate significantly more healthy snacks than participants in the other group. In the second study, AB of children decreased in the avoid group and increased in the control group. Over time, the number of calories consumed in the free access session, as well as the percent of daily caloric needs consumed in free access, increased significantly among children in the control group, but showed a slight decrease among children in the avoid group. Changes in cravings, liking, and saliva were not significantly different between groups.
Finally, the study that investigated body dissatisfaction6767. Smeets E, Jansen A, Roefs A. Bias for the (un)attractive self: on the role of attention in causing body (dis)satisfaction. Health Psychol. 2011;30:360-7. randomly assigned women to groups according to the words to which they attended: negative shape/weight words, positive shape/weight words, negative (high calorie) food words, positive (low calorie) food words, or neutral words. Participants in the control group were instructed to attend to neutral words paired with stimuli that induced body dissatisfaction. The results revealed that AB induction to negative shape/weight and negative food words increased body dissatisfaction and dietary restrictions. In contrast, AB induction to positive shape/weight and positive (low calorie) food words resulted in no significant differences from the control group. The authors suggested that their study might provide evidence of the association between selective attention and body satisfaction. Moreover, they pointed out that attention training might be an additional technique for clinical interventions.
Pain
This category included three studies6868. Sharpe L, Ianiello M, Dear BF, Nicholson Perry K, Refshauge K, Nicholas MK. Is there a potential role for attention bias modification in pain patients? Results of 2 randomised controlled trials. Pain. 2012;153:722-31.
69. McGowan N, Sharpe L, Refshauge K, Nicholas MK. The effect of attentional re-training and threat expectancy in response to acute pain. Pain. 2009;142:101-7.-7070. Schoth DE, Liossi C. Specificity and time-course of attentional bias in chronic headache: a visual-probe investigation. Clin J Pain. 2013;29:583-90. that investigated pain primarily and compared avoid and control groups. Two of them6868. Sharpe L, Ianiello M, Dear BF, Nicholson Perry K, Refshauge K, Nicholas MK. Is there a potential role for attention bias modification in pain patients? Results of 2 randomised controlled trials. Pain. 2012;153:722-31.,6969. McGowan N, Sharpe L, Refshauge K, Nicholas MK. The effect of attentional re-training and threat expectancy in response to acute pain. Pain. 2009;142:101-7. had practically the same ABM method, as both used SOA of 500 ms and 40 pairs of words (pain-neutral) as a stimulus. Both found no AB differences between groups at post training, but interestingly some benefits were seen after a longer time. In the first study,6868. Sharpe L, Ianiello M, Dear BF, Nicholson Perry K, Refshauge K, Nicholas MK. Is there a potential role for attention bias modification in pain patients? Results of 2 randomised controlled trials. Pain. 2012;153:722-31. participants in the avoid group reported fewer days in pain and less average pain at a 3-month follow-up. In the second study,6969. McGowan N, Sharpe L, Refshauge K, Nicholas MK. The effect of attentional re-training and threat expectancy in response to acute pain. Pain. 2009;142:101-7. the benefits of ABM emerged 6 months later for disability and anxiety sensitivity. This study6969. McGowan N, Sharpe L, Refshauge K, Nicholas MK. The effect of attentional re-training and threat expectancy in response to acute pain. Pain. 2009;142:101-7. also used attend (to pain) and control groups and found that participants in the attend group reported pain more quickly and strongly than those in the control group, but pain tolerance did not differ between groups. In the most recent study,7070. Schoth DE, Liossi C. Specificity and time-course of attentional bias in chronic headache: a visual-probe investigation. Clin J Pain. 2013;29:583-90. ABM to avoid pain was trained using faces and words, and SOA of 500 and 1,250 ms. Results were very similar to those described before, and although AB scores were not statistically different across time, statistically and clinically significant changes were found in pain intensity, anxiety, depression and pain interference 6 months after ABM.
Discussion
The analysis of the results of 57 studies that investigated ABM using a visual probe task revealed that most (79%, n = 45) were successful for the groups that received training, as attentional bias (AB) was successfully manipulated in the expected direction. In 71% (n = 32) of these, results that generalized to other measures were correlated with symptoms, which suggests that this technique has potential clinical utility. The studies about eating behavior (100%), drug addiction (88%) and anxiety (75%) had the highest rates of training success (Table 2), but data should be carefully analyzed to determine training impact on symptom improvement, because there are many more studies in one category than in the others.
The analysis according to categories demonstrated that most studies about ABM have focused on anxiety to this date, probably because the modified visual probe task was developed to manipulate AB for emotional vulnerability.77. MacLeod C, Rutherford E, Campbell L, Ebsworthy G, Holker L. Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol. 2002;111:107-23. Our study has opened doors for many others in the area of anxiety, stress and worrying, as well as of depression, drug addiction, pain and eating behavior. Although more studies about ABM using visual probe tasks to investigate eating behaviors and pain than studies about other categories have been published in the last 2 years, much remains to be studied in these areas to reach conclusions about the effectiveness of this technique.
Two of the three studies about pain that found no differences in attentional bias between groups immediately after training found some benefits 3 and 6 months later. Improvements may have arisen from non-specific therapeutic factors, such as expectancy. However, other possible explanation may be the fact that ABM, as an implicit training strategy,5353. Schoenmakers TM, de Bruin M, Lux IF, Goertz AG, Van Kerkhof DH, Wiers RW. Clinical effectiveness of attentional bias modification training in abstinent alcoholic patients. Drug Alcohol Depend. 2010;109:30-6.,5555. Lopes FM, Pires AV, Bizarro L. Attentional bias modification in smokers trying to quit: a longitudinal study about the effects of number of sessions. J Subst Abuse Treat. 2014;47:50-7. might have led to some late effects. A recent study5555. Lopes FM, Pires AV, Bizarro L. Attentional bias modification in smokers trying to quit: a longitudinal study about the effects of number of sessions. J Subst Abuse Treat. 2014;47:50-7. showed long-term effectiveness of ABM in a clinical population of smokers, as a positive AB at baseline became immediately negative (avoidance pattern) in the first post-training assessment, remained negative 6 months later and was progressively attenuated, reaching a near-zero level (no AB) in the last assessment 1 year after training.
Some methodological issues of the studies under analysis may raise concerns and should be discussed carefully. First, the analysis of study group design revealed that training to attend seemed to modify AB more easily than training to avoid. This was clear in studies that compared attend and avoid groups,77. MacLeod C, Rutherford E, Campbell L, Ebsworthy G, Holker L. Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol. 2002;111:107-23.,1919. Browning M, Holmes EA, Harmer CJ. The modification of attentional bias to emotional information: a review of the techniques, mechanisms, and relevance to emotional disorders. Cogn Affect Behav Neurosci. 2010;10:8-20.,3737. Eldar S, Ricon T, Bar-Haim Y. Plasticity in attention: implications for stress response in children. Behav Res Ther. 2008;46:450-61.,5151. Field M, Eastwood B. Experimental manipulation of attentional bias increases the motivation to drink alcohol. Psychopharmacology (Berl). 2005;183:350-7. or attend, avoid and control groups,99. Field M, Duka T, Eastwood B, Child R, Santarcangelo M, Gayton M. Experimental manipulation of attentional biases in heavy drinkers: do the effects generalize? Psychopharmacology (Berl). 2007;192:593-608.,1212. Field M, Duka T, Tyler E, Schoenmakers T. Attentional bias modification in tobacco smokers. Nicotine Tob Res. 2009;11:812-22. which found differences in the AB of the attend groups when compared to the other study groups. However, several studies that compared avoid and control groups2121. Boettcher J, Berger T, Renneberg B. Internet-based attention training for social anxiety: a randomized controlled trial. Cognit Ther Res. 2012;36:522-36.
22. Carlbring P, Apelstrand M, Sehlin H, Amir N, Rousseau A, Hofmann SG, et al. Internet-delivered attention bias modification training in individuals with social anxiety disorder -- a double blind randomized controlled trial. BMC Psychiatry. 2012;12:66.-2323. Julian K, Beard C, Schmidt NB, Powers MB, Smits JA. Attention training to reduce attention bias and social stressor reactivity: an attempt to replicate and extend previous findings. Behav Res Ther. 2012;50:350-8.,5252. McHugh RK, Murray HW, Hearon BA, Calkins AW, Otto MW. Attentional bias and craving in smokers: the impact of a single attentional training session. Nicotine Tob Res. 2010;12:1261-4. found no differences between groups after training. One possible explanation for this phenomenon might be that avoidance training demands a greater cognitive effort, as it goes against the trend preferred by participants, whereas training to attend reinforces this trend and does not demand any special cognitive effort. However, although attend-to-positive stimuli (e.g., attend to happy faces or healthy food) generate benefits for participants in the case of depression and eating behaviors, this type of training has no clinical utility for anxiety, drug addiction and pain, which suggests that studies about ABM in these three categories should use only avoid and control groups.
The second concern about study methods was the number of training sessions. Of the 57 studies under analysis, 50% used a single training session, whereas the other 50% used multiple sessions, but the results that indicated which frequency was more efficient were controversial. In studies about anxiety, the number of sessions did not seem to affect training success, as studies using a larger number of sessions found no substantial differences between groups when compared with those that used only one session. The same was found for studies about depression and pain. In contrast, the analysis of studies in the drug addiction category revealed that the highest number of training sessions led to the most successful results and clinical utility.5353. Schoenmakers TM, de Bruin M, Lux IF, Goertz AG, Van Kerkhof DH, Wiers RW. Clinical effectiveness of attentional bias modification training in abstinent alcoholic patients. Drug Alcohol Depend. 2010;109:30-6. The use of five ABM training sessions in a group of patients with alcohol dependence was effective and affected treatment progression, as patients in the avoid group took longer to relapse and were discharged before patients in the control group. Similarly, the study with smokers trying to quit5555. Lopes FM, Pires AV, Bizarro L. Attentional bias modification in smokers trying to quit: a longitudinal study about the effects of number of sessions. J Subst Abuse Treat. 2014;47:50-7. found that the effect of ABM training was dose-dependent. Because of the complexity and diversity of addictive habits, as well as the number of pairings of environmental cues and the act of smoking or drinking, a greater number of ABM sessions, perhaps held daily, might be necessary to reduce addictive behaviors. Intensive training sessions can be conducted concurrently and after formal treatment to reinforce motivation to achieve abstinence between sessions, as well as to reinforce abstinence maintenance. In the same direction, the study about AB toward chocolate6262. Kemps E, Tiggemann M, Elford J. Sustained effects of attentional re-training on chocolate consumption. J Behav Ther Exp Psychiatry. 2015;49(Pt A):94-100. found that training effects were maintained 1 week later only when multiple training sessions were used, and its authors emphasized the importance of administering multiple ABM re-training sessions. Therefore, at least in the area of drug addiction and eating behaviors, future studies should investigate whether multiple training sessions on consecutive or alternate days, but not on the same day, may enhance post-training success and longer-term training effects.
Although all studies analyzed used the same evaluation paradigm (modified visual probe task), our third methodological concern is the great variation in type and number of stimuli and in SOA. Differently from studies about other tasks for ABM,1515. Hakamata Y, Lissek S, Bar-Haim Y, Britton JC, Fox NA, Leibenluft, E, et al. Attention bias modification treatment: a meta-analysis toward the establishment of novel treatment for anxiety. Biol Psychiatry. 2010;68:982-90. those that use visual probe tasks have not defined a consensus about what type of stimuli is most effective, especially when investigating anxiety and depression. In contrast, most studies about drug addiction and eating behaviors use pictures, and not words, because authors argue that images have greater ecological validity. The analysis of SOA suggests that an advantage of visual probe tasks is that all attentional processes involved in AB can be evaluated, including the initial, automatic detection of stimuli (measured by shorter SOAs) and the engagement stages of attention maintained later on (measured by longer SOAs).44. Robbins SJ, Ehrman RN. The role of attentional bias in substance abuse. Behav Cogn Neurosci Rev. 2004;3:243-60.,7171. Field M, Mogg K, Zetteler J, Bradley BP. Attentional biases for alcohol cues in heavy and light social drinkers: the roles of initial orienting and maintained attention. Psychoparmacology (Berl). 2004;176:88-93. The results of most studies under analysis suggest that relatively longer stimulus duration should be preferred in ABM, because participants have time to process the content of the stimulus more fully, which may lead to a more elaborate processing of stimuli congruent with participant emotions.5959. Yang W, Ding Z, Dai T, Peng F, Zhang JX. Attention Bias Modification training in individuals with depressive symptoms: a randomized controlled trial. J Behav Ther Exp Psychiatry. 2015;49(Pt A):101-11. Future studies about these two factors in clinical populations should aim at defining the optimal ABM format to maintain improvements over time.
The fourth and final concern about study methods is training contingencies and follow-up assessments. Some studies found that awareness contingency improved efficiency,99. Field M, Duka T, Eastwood B, Child R, Santarcangelo M, Gayton M. Experimental manipulation of attentional biases in heavy drinkers: do the effects generalize? Psychopharmacology (Berl). 2007;192:593-608.,1111. Attwood AS, O'Sullivan H, Leonards U, Mackintosh B, Munafo MR. Attentional bias training and cue reactivity in cigarette smokers. Addiction. 2008;103:1875-82. and their authors suggested that explicit instructions about the purpose of training might affect results if these methods were applied clinically, and that participants should be made aware of experimental contingencies.99. Field M, Duka T, Eastwood B, Child R, Santarcangelo M, Gayton M. Experimental manipulation of attentional biases in heavy drinkers: do the effects generalize? Psychopharmacology (Berl). 2007;192:593-608. Moreover, only a few studies used new stimuli in post training and performed follow-up studies, which might have provided information about the effects of generalization and of training in the short, medium and long term. Therefore, instruments to investigate the clinical impact of ABM over time should be encouraged. Lack of standardization of method or statistical analyses may produce different results due to the use of different stimuli or statistical tests. Studies evaluating efficacy are important to guide the design and improve the standardization of future investigations.
This systematic review focused on methods and results of studies about ABM using a specific modified visual probe task, which may be a limitation of this study. Other experimental methods used to modify AB, such as touch the face,7272. Dandeneau SD, Baldwin MW. The inhibition of socially rejecting information among people with high versus low self-esteem: the role of attentional bias and the effects of bias reduction training. J Soc Clin Psychol. 2004;23:584-603. alcohol attention-control training program,7373. Fadardi JS, Cox WM. Reversing the sequence: reducing alcohol consumption by overcoming alcohol attentional bias. Drug Alcohol Depend. 2009;101:137-45. goal instructions,7474. Johnson DR. Goal-directed attentional deployment to emotional faces and individual differences in emotional regulation. J Res Pers. 2009;43:8-13. structure and semantic task,7575. Hirsch CR, MacLeod C, Mathews A, Sandher O, Siyani A, Hayes S. The contribution of attentional bias to worry: distinguishing the roles of selective engagement and disengagement. J Anxiety Disord. 2011;25:272-7. and push or pull the joystick,7676. Wiers RW, Rinck M, Kordts R, Houben K, Strack F. Retraining automatic action-tendencies to approach alcohol in hazardous drinkers. Addiction. 2010;105:279-87. were not included here, but should also be the focus of future studies. However, we chose to select studies that included a visual probe task because it was the first task originally developed to modify AB and the most widely used task in ABM studies. In addition, this study aimed at discussing method discrepancies and similarities, as well as compare findings of studies that used the same paradigm to understand the impact of this method as an additional intervention for the treatment of emotional disorders.
Finally, these results add to the growing body of literature that suggests that pursuing attention-based interventions is a novel and promising approach with potential clinical utility as an additional intervention. However, according to Field et al., based on the evidence to date about the use of ABM in drug addiction, this intervention should be evaluated in a large-scale clinical trial before it is included in treatment programs.7777. Clarke PJ, Notebaert L, MacLeod C. Absence of evidence or evidence of absence: reflecting on therapeutic implementations of attentional bias modification. BMC Psychiatry. 2014;14:8. In turn, Clarke et al., who reviewed studies that failed to modify AB, suggested that failure might be a result of task conditions and delivery modes and suggested that "absence of evidence for the effectiveness of ABM is not evidence that ABM is ineffective."7878. Field M, Marhe R, Franken IH. The clinical relevance of attentional bias in substance use disorders. CNS Spectr. 2013;19:225-30. The same authors reported that experimental psychology research about ABM using visual probe tasks has been conducted for little more than one decade, and that it has been applied to clinical samples and shown promising results since the beginning,7878. Field M, Marhe R, Franken IH. The clinical relevance of attentional bias in substance use disorders. CNS Spectr. 2013;19:225-30. which was confirmed in our review. In summary, post-training group differences are not enough to determine whether ABM training procedures lead to behavioral changes. To do that, training effects should generalize to real life events, correlate with improvement in symptoms and, especially, be maintained in the long term. Therefore, study designs should include different stimuli during training and post training, and longitudinal studies should be conducted. Method standardization should be based on the evidence of what is more effective, such as a higher number of training sessions on alternate days, stimuli with more ecological validity, assessment of the impact of the awareness of training contingencies and assessment of the presence of AB as a prerequisite for the completion of training. These suggestions may help determine the effects of training in future studies, as well as define possible applications of this technique as an addition to treatments currently available for disorders such as anxiety, depression and addiction.
References
-
1Williams JM, Mathews A, MacLeod C. The emotional Stroop task and psychopathology. Psychol Bull. 1996;120:3-24.
-
2Lopes FM, Peuker AC, Bizarro L. Viés atencional em fumantes. Psico. 2008;39:280-8.
-
3Peuker AC, Lopes FM, Bizarro L. Viés atencional no abuso de drogas: teoria e método. Psic Teor Pesq. 2009;25:603-9.
-
4Robbins SJ, Ehrman RN. The role of attentional bias in substance abuse. Behav Cogn Neurosci Rev. 2004;3:243-60.
-
5Bar-Haim Y, Lamy D, Pergamin L, Bakermans-Kranenburg MJ, van IJzendoorn MH. Threat-related attentional bias in anxious and nonanxious individuals: a meta-analytic study. Psychol Bull. 2007;133:1-24.
-
6Amir N, Beard C, Burns M, Bomyea J. Attention modification program in individuals with generalized anxiety disorder. J Abnorm Psychol. 2009;118:28-33.
-
7MacLeod C, Rutherford E, Campbell L, Ebsworthy G, Holker L. Selective attention and emotional vulnerability: assessing the causal basis of their association through the experimental manipulation of attentional bias. J Abnorm Psychol. 2002;111:107-23.
-
8Schmidt NB, Richey JA, Buckner JD, Timpano KR. Attention training for generalized social anxiety disorder. J Abnorm Psychol. 2009;118:5-14.
-
9Field M, Duka T, Eastwood B, Child R, Santarcangelo M, Gayton M. Experimental manipulation of attentional biases in heavy drinkers: do the effects generalize? Psychopharmacology (Berl). 2007;192:593-608.
-
10Schoenmakers T, Wiers RW, Jones BT, Bruce G, Jansen AT. Attentional re-training decreases attentional bias in heavy drinkers without generalization. Addiction. 2007;102:399-405.
-
11Attwood AS, O'Sullivan H, Leonards U, Mackintosh B, Munafo MR. Attentional bias training and cue reactivity in cigarette smokers. Addiction. 2008;103:1875-82.
-
12Field M, Duka T, Tyler E, Schoenmakers T. Attentional bias modification in tobacco smokers. Nicotine Tob Res. 2009;11:812-22.
-
13MacLeod C, Mathews A, Tata P. Attentional bias in emotional disorders. J Abnorm Psychol. 1986;95:15-20.
-
14Townshed JM, Duka T. Attentional bias with alcohol cues: differences between heavy and occasional social drinkers. Psychopharmacology (Berl). 2001;157:67-74.
-
15Hakamata Y, Lissek S, Bar-Haim Y, Britton JC, Fox NA, Leibenluft, E, et al. Attention bias modification treatment: a meta-analysis toward the establishment of novel treatment for anxiety. Biol Psychiatry. 2010;68:982-90.
-
16Hallion LS, Ruscio AM. A meta-analysis of the effect of cognitive bias modification on anxiety and depression. Psychol Bull. 2011;137:940-58.
-
17Beard C, Sawyer AT, Hofmann SG. Efficacy of attention bias modification using threat and appetitive stimuli: a meta-analytic review. Behav Ther. 2012;43:724-40.
-
18Bar-Haim Y. Research review: attention bias modification (ABM): a novel treatment for anxiety disorders. J Child Psychol Psychiatry. 2010;51:859-70.
-
19Browning M, Holmes EA, Harmer CJ. The modification of attentional bias to emotional information: a review of the techniques, mechanisms, and relevance to emotional disorders. Cogn Affect Behav Neurosci. 2010;10:8-20.
-
20MacLeod C, Mathews A. Cognitive bias modification approaches to anxiety. Annu Rev Clin Psychol. 2012;8:198-217.
-
21Boettcher J, Berger T, Renneberg B. Internet-based attention training for social anxiety: a randomized controlled trial. Cognit Ther Res. 2012;36:522-36.
-
22Carlbring P, Apelstrand M, Sehlin H, Amir N, Rousseau A, Hofmann SG, et al. Internet-delivered attention bias modification training in individuals with social anxiety disorder -- a double blind randomized controlled trial. BMC Psychiatry. 2012;12:66.
-
23Julian K, Beard C, Schmidt NB, Powers MB, Smits JA. Attention training to reduce attention bias and social stressor reactivity: an attempt to replicate and extend previous findings. Behav Res Ther. 2012;50:350-8.
-
24Schoorl M, Putman P, Van Der Does W. Attentional bias modification in posttraumatic stress disorder: a randomized controlled trial. Psychother Psychosom. 2013;82:99-105.
-
25Rapee RM, MacLeod C, Carpenter L, Gaston JE, Frei J, Peters L, et al. Integrating cognitive bias modification into a standard cognitive behavioural treatment package for social phobia: a randomized controlled trial. Behav Res Ther. 2013;51:207-15.
-
26Hazen RA, Vasey MW, Schmidt NB. Attentional retraining: a randomized clinical trial for pathological worry. J Psychiatr Res. 2009;43:627-33.
-
27Heeren A, Lievens L, Philippot P. How does attention training work in social phobia: disengagement from threat or re-engagement to non-threat? J Anxiety Disord. 2011;25:1108-15.
-
28See J, MacLeod C, Bridle R. The reduction of anxiety vulnerability through the modification of attentional bias: a real-world study using a home-based cognitive bias modification procedure. J Abnorm Psychol. 2009;118:65-75.
-
29Heeren A, Philippot P, Koster EH. Impact of the temporal stability of preexistent attentional bias for threat on its alteration through attention bias modification. J Behav Ther Exp Psychiatry. 2015;49(Pt A):69-75.
-
30Amir N, Taylor CT, Donohue MC. Predictors of response to an attention modification program in generalized social phobia. J Consult Clin Psychol. 2011;79:533-41.
-
31Eldar S, Bar-Haim Y. Neural plasticity in response to attention training in anxiety. Psychol Med. 2010;40:667-77.
-
32Koster EH, Baert S, Bockstaele M, De Raedt R. Attentional retraining procedures: manipulating early or late components of attentional bias? Emotion. 2010;10:230-6.
-
33Reese HE, McNally RJ, Najmi S, Amir N. Attention training for reducing spider fear in spider-fearful individuals. J Anxiety Disord. 2010;24:657-62.
-
34MacLeod C, Soong LY, Rutherford EM, Campbell LW. Internet-delivered assessment and manipulation of anxiety-linked attentional bias: validation of a free-access attentional probe software package. Behav Res Methods. 2007;39:533-8.
-
35Van Bockstaele B, Verschuere B, Koster EH, Tibboel H, De Houwer J, Crombez G. Effects of attention training on self-reported, implicit, physiological and behavioural measures of spider fear. J Behav Ther Exp Psychiatry. 2011;42:211-8.
-
36Van Bockstaele B, Koster EH, Verschuere B, Crombez G, De Houwer J. Limited transfer of threat bias following attentional retraining. J Behav Ther Exp Psychiatry. 2012;43:794-800.
-
37Eldar S, Ricon T, Bar-Haim Y. Plasticity in attention: implications for stress response in children. Behav Res Ther. 2008;46:450-61.
-
38O'Toole L, Dennis TA. Attention training and the threat bias: an ERP study. Brain Cogn. 2012;78:63-73.
-
39Heeren A, Peschard V, Philippot P. The causal role of attentional bias for threat cues in social anxiety: a test on a cyber-ostracism task. Cognit Ther Res. 2012;36:512-21.
-
40Krebs G, Hirsch CR, Mathews A. The effect of attention modification with explicit vs. minimal instructions on worry. Behav Res Ther. 2010;48:251-6.
-
41Hayes S, Hirsch CR, Mathews A. Facilitating a benign attentional bias reduces negative thought intrusions. J Abnorm Psychol. 2010;119:235-40.
-
42Li S, Tan J, Qian M, Liu X. Continual training of attentional bias in social anxiety. Behav Res Ther. 2008;46:905-12.
-
43Taylor CT, Bomyea J, Amir N. Malleability of attentional bias for positive emotional information and anxiety vulnerability. Emotion. 2011;11:127-38.
-
44Wadlinger HA, Isaacowitz DM. Looking happy: the experimental manipulation of a positive visual attention bias. Emotion. 2008;8:121-6.
-
45Amir N, Taylor CT. Combining computerized home-based treatments for generalized anxiety disorder: an attention modification program and cognitive behavioral therapy. Behav Ther. 2012;43:546-59.
-
46Cowart MJ, Ollendick TH. Attention training in socially anxious children: a multiple baseline design analysis. J Anxiety Disord. 2011;25:972-7.
-
47Brosan L, Hoppitt L, Shelfer L, Sillence A, Mackintosh B. Cognitive bias modification for attention and interpretation reduces trait and state anxiety in anxious patients referred to an out-patient service: results from a pilot study. J Behav Ther Exp Psychiatry. 2011;42:258-64.
-
48Heeren A, Reese HE, McNally RJ, Philippot P. Attention training toward and away from threat in social phobia: effects on subjective, behavioral, and physiological measures of anxiety. Behav Res Ther. 2012;50:30-9.
-
49Klumpp H, Amir N. Preliminary study of attention training to threat and neutral faces on anxious reactivity to a social stressor in social anxiety. Cognit Ther Res. 2010;34:263-71.
-
50Boettcher J, Leek L, Matson L, Holmes EA, Browning M, MacLeod C, et al. Internet-based attention bias modification for social anxiety: a randomised controlled comparison of training towards negative and training towards positive cues. PLoS One. 2013;8:e71760.
-
51Field M, Eastwood B. Experimental manipulation of attentional bias increases the motivation to drink alcohol. Psychopharmacology (Berl). 2005;183:350-7.
-
52McHugh RK, Murray HW, Hearon BA, Calkins AW, Otto MW. Attentional bias and craving in smokers: the impact of a single attentional training session. Nicotine Tob Res. 2010;12:1261-4.
-
53Schoenmakers TM, de Bruin M, Lux IF, Goertz AG, Van Kerkhof DH, Wiers RW. Clinical effectiveness of attentional bias modification training in abstinent alcoholic patients. Drug Alcohol Depend. 2010;109:30-6.
-
54Kerst WF, Waters AJ. Attentional retraining administered in the field reduces smokers' attentional bias and craving. Health Psychol. 2014;33:1232-40.
-
55Lopes FM, Pires AV, Bizarro L. Attentional bias modification in smokers trying to quit: a longitudinal study about the effects of number of sessions. J Subst Abuse Treat. 2014;47:50-7.
-
56Browning M, Holmes EA, Charles M, Cowen PJ, Harmer CJ. Using attentional bias modification as a cognitive vaccine against depression. Biol Psychiatry. 2012;72:572-9.
-
57Haeffel GJ, Rozek DC, Hames JL, Technow J. Too much of a good thing: testing the efficacy of a cognitive bias modification task for cognitively vulnerable individuals. Cognit Ther Res. 2012;36:493-501.
-
58Isaacowitz DM, Choi Y. The malleability of age-related positive gaze preferences: training to change gaze and mood. Emotion. 2011;11:90-100.
-
59Yang W, Ding Z, Dai T, Peng F, Zhang JX. Attention Bias Modification training in individuals with depressive symptoms: a randomized controlled trial. J Behav Ther Exp Psychiatry. 2015;49(Pt A):101-11.
-
60Baert S, De Raedt R, Schacht R, Koster EH. Attentional bias training in depression: therapeutic effects depend on depression severity. J Behav Ther Exp Psychiatry. 2010;41:265-74.
-
61Tsumura H, Shimada H, Nomura K, Sugaya N, Suzuki K. The effects of attention retraining on depressive mood and cortisol responses to depression-related stimuli. Jpn Psychol Res. 2012;54:400-11.
-
62Kemps E, Tiggemann M, Elford J. Sustained effects of attentional re-training on chocolate consumption. J Behav Ther Exp Psychiatry. 2015;49(Pt A):94-100.
-
63Kakoschke N, Kemps E, Tiggemann M. Attentional bias modification encourages healthy eating. Eat Behav. 2014;15:120-4.
-
64Boutelle KN, Kuckertz JM, Carlson J, Amir N. A pilot study evaluating a one-session attention modification training to decrease overeating in obese children. Appetite. 2014;76:180-5.
-
65Kemps E, Tiggemann M, Orr J, Grear J. Attentional retraining can reduce chocolate consumption. J Exp Psychol Appl. 2014;20:94-102.
-
66Kemps E, Tiggemann M, Hollitt S. Biased attentional processing of food cues and modification in obese individuals. Health Psychol. 2014;33:1391-401.
-
67Smeets E, Jansen A, Roefs A. Bias for the (un)attractive self: on the role of attention in causing body (dis)satisfaction. Health Psychol. 2011;30:360-7.
-
68Sharpe L, Ianiello M, Dear BF, Nicholson Perry K, Refshauge K, Nicholas MK. Is there a potential role for attention bias modification in pain patients? Results of 2 randomised controlled trials. Pain. 2012;153:722-31.
-
69McGowan N, Sharpe L, Refshauge K, Nicholas MK. The effect of attentional re-training and threat expectancy in response to acute pain. Pain. 2009;142:101-7.
-
70Schoth DE, Liossi C. Specificity and time-course of attentional bias in chronic headache: a visual-probe investigation. Clin J Pain. 2013;29:583-90.
-
71Field M, Mogg K, Zetteler J, Bradley BP. Attentional biases for alcohol cues in heavy and light social drinkers: the roles of initial orienting and maintained attention. Psychoparmacology (Berl). 2004;176:88-93.
-
72Dandeneau SD, Baldwin MW. The inhibition of socially rejecting information among people with high versus low self-esteem: the role of attentional bias and the effects of bias reduction training. J Soc Clin Psychol. 2004;23:584-603.
-
73Fadardi JS, Cox WM. Reversing the sequence: reducing alcohol consumption by overcoming alcohol attentional bias. Drug Alcohol Depend. 2009;101:137-45.
-
74Johnson DR. Goal-directed attentional deployment to emotional faces and individual differences in emotional regulation. J Res Pers. 2009;43:8-13.
-
75Hirsch CR, MacLeod C, Mathews A, Sandher O, Siyani A, Hayes S. The contribution of attentional bias to worry: distinguishing the roles of selective engagement and disengagement. J Anxiety Disord. 2011;25:272-7.
-
76Wiers RW, Rinck M, Kordts R, Houben K, Strack F. Retraining automatic action-tendencies to approach alcohol in hazardous drinkers. Addiction. 2010;105:279-87.
-
77Clarke PJ, Notebaert L, MacLeod C. Absence of evidence or evidence of absence: reflecting on therapeutic implementations of attentional bias modification. BMC Psychiatry. 2014;14:8.
-
78Field M, Marhe R, Franken IH. The clinical relevance of attentional bias in substance use disorders. CNS Spectr. 2013;19:225-30.
-
Financial support: Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES).
Publication Dates
-
Publication in this collection
Oct-Dec 2015
History
-
Received
20 Feb 2015 -
Accepted
09 Mar 2015