Abstracts
Mucocele of the appendix is a rare disease. It can be triggered by benign or malignant diseases, which cause the obstruction of the appendix and the consequent accumulation of mucus secretion. The preoperative diagnosis is difficult due to non-specific clinical manifestations of the disease. Imaging tests can suggest the diagnosis. The treatment is always surgical and depends on the integrity and size of the appendix base and on the histological type of the original lesion. The prognosis is good in cases of integrity of the appendix. The perforation of the appendix and subsequent extravasation of its contents into the abdominal cavity may lead to pseudomyxoma peritonei, which has very poor prognosis if not treated properly.
mucocele; appendix; pseudomyxoma peritonei; treatment
A mucocele do apêndice cecal é uma doença rara. Pode ser causada por doenças benignas ou malignas que provocam a obstrução da luz do apêndice e, consequente, acúmulo de secreção mucoide. O diagnóstico pré-operatório é difícil devido ao quadro clínico inespecífico da doença. Exames de imagem sugerem o diagnóstico. O tratamento é sempre cirúrgico e é determinado pela integridade do órgão, dimensões da base e tipo histológico da lesão. O prognóstico é bom nos casos com integridade do apêndice cecal. A perfuração do apêndice e o consequente extravasamento do seu conteúdo para a cavidade abdominal pode ocasionar o pseudomixoma peritoneal, cujo prognóstico é bastante desfavorável se não tratado adequadamente.
mucocele; apêndice cecal; pseudomixoma peritoneal; tratamento
ORIGINAL ARTICLE
Mucocele of the appendix : appendectomy or colectomy?
Janduí Gomes De Abreu Filho; Erivaldo Fernandes De Lira
Service of Coloproctology of Hospital de Base do Distrito Federal (HBDF), Secretariat of Health in Distrito Federal - Brasília (DF), Brazil
Correspondence to Correspondence to: Janduí Gomes de Abreu Filho Rua 35 Sul, Lote 9, Apto. 1204, Ed. Del Fiori CEP: 71931-180 Águas Claras (DF), Brazil. E-mail: jgabreufilho@bol.com.br
ABSTRACT
Mucocele of the appendix is a rare disease. It can be triggered by benign or malignant diseases, which cause the obstruction of the appendix and the consequent accumulation of mucus secretion. The preoperative diagnosis is difficult due to non-specific clinical manifestations of the disease. Imaging tests can suggest the diagnosis. The treatment is always surgical and depends on the integrity and size of the appendix base and on the histological type of the original lesion. The prognosis is good in cases of integrity of the appendix. The perforation of the appendix and subsequent extravasation of its contents into the abdominal cavity may lead to pseudomyxoma peritonei, which has very poor prognosis if not treated properly.
Keywords: mucocele; appendix; pseudomyxoma peritonei; treatment.
RESUMO
A mucocele do apêndice cecal é uma doença rara. Pode ser causada por doenças benignas ou malignas que provocam a obstrução da luz do apêndice e, consequente, acúmulo de secreção mucoide. O diagnóstico pré-operatório é difícil devido ao quadro clínico inespecífico da doença. Exames de imagem sugerem o diagnóstico. O tratamento é sempre cirúrgico e é determinado pela integridade do órgão, dimensões da base e tipo histológico da lesão. O prognóstico é bom nos casos com integridade do apêndice cecal. A perfuração do apêndice e o consequente extravasamento do seu conteúdo para a cavidade abdominal pode ocasionar o pseudomixoma peritoneal, cujo prognóstico é bastante desfavorável se não tratado adequadamente.
Palavras-chave: mucocele; apêndice cecal; pseudomixoma peritoneal; tratamento.
INTRODUCTION
The mucocele of the appendix was first described in 1842 by Rokitansky1. This disease is considered as a rare lesion of the appendix, which is found in 0.2 to 0.3% of the appendectomies2. It is characterized by the dilation of the organ lumen with mucus accumulation, being more frequent among individuals aged 50 years or more3,4. Gender prevalence is controversial.
Appendix mucocele may come as a consequence of obstructive or inflammatory processes, cystadenomas or cystadenocarcinomas7. Besides these causes, other tumor lesions in the appendix or cecum may present as mucocele8. Its main complication is pseudomyxoma peritonei.
Treatment is always surgery and determined by the organ's integrity, the dimensions of the base and histological type of the lesion.
Revista Brasileira de Coloproctologia has recently published two articles about this disease. The first one defends the right colectomy as a treatment9, and the second one recommends only appendectomy10. Despite the different adopted conducts, in both reported cases a cystadenoma was diagnosed in the appendix; the choice was for elective surgery.
The objective of this review is to analyze literature as to mucocele, especially regarding diagnosis and treatment, besides discussing follow-up and prognosis of the individuals who have this disease.
LITERATURE REVIEW
The mucocele of the appendix is a descriptive and unspecific term to define the cystic dilation of the appendix caused by the accumulation of mucus secretion. This process is slow and gradual, with no signs of infection inside the organ. It results from the lumen obstruction in the appendix, which is secondary to the inflammatory or neoplastic proliferation of the appendix mucosa, or of lesions in the cecum, adjacent to the appendiceal ostium.
While some articles confirm its prevalence among women3,4, others demonstrate a higher incidence among men5,6.
Mucocele in the appendix may be classified according to the histological characteristics of lumen obstruction7.
Simple mucocele (inflammatory, obstructive or retention cyst) is characterized by degenerative epithelial changes and results in the obstruction and the distension of the appendix. There is no evidence of hyperplasia or mucosal atypia.
In hyperplastic mucocele, the appendix dilation occurs due to the hyperplastic growth of the appendix or cecal mucosa, just like hyperplastic polyps in the colon.
Simple and hyperplastic mucoceles correspond to 5 to 25% of the cases, and mucus is usually acellular.
The mucinous cystadenoma is an appendix neoplasm with dysplastic epithelium similar to colon adenomatous polyps, and corresponds to 63 to 84% of the cases.
The mucinous cystadenocarcinoma presents high grade cellular dysplasia and stromal invasion, besides muscularis mucosae, and represents 11 to 20% of the cases.
In both types described, the mucus material contains epithelial adenoma cells with low or high grade of dysplasia. The rupture of the appendix may lead to the dissemination of the epithelium that produces mucins in the abdominal cavity, causing mucinous ascites or pseudomyxoma peritonei.
Stocchi et al.4 analyzed 135 patients with mucocele of the appendix. Out of these, 129 were submitted to surgery and histological analyses, and 37 presented pseudomyxoma peritonei. From the 37 cases of pseudomyxoma peridonei, 95% had malignant mucocele, and 83% of the perforated mucoceles were malignant.
Ronnet et al.11 studied 109 cases of pseudomyxoma peritonei and classified it in two types: disseminated peritoneal adenomucinosis, which is a result of mucinous adenoma, with survival rate of 84%; and peritoneal mucinous carcinomatosis, which is secondary to mucinous adenocarcinoma, with survival rate of 6.7%.
Thus, both the benign and the malignant mucocele may cause pseudomyxoma peritonei, however, this complication is more frequent and has worse prognosis for malignant cases, probably because in this situation the appendix ruptures more easily, and the celular seeding is more aggressive4,5,11.
Mucocele of the appendix can also result from alterations in the cecum, such as fecal impaction, polyps or malignant neoplasms, which, in theory, can obstruct the appendiceal ostium. Another rare cause found in literature is endometriosis, which may be established on the wall of the appendix, causing lumen obstruction8.
The classification based on histopathological standards is really important, once the progress of the disease and its prognosis are related to the subtypes.
Simple and benign mucoceles have an insidious evolution and are rarely perforated; on the other hand malignant mucocele evolution is faster, like in acute appendicitis, usually presenting as an organ perforation4.
The diameter of the non-neoplastic mucocele (simple and hyperplastic) is smaller than the neoplastic mucocele (cystadenoma and cystadenocarcinoma); however, there is no difference related to size among benign and malignant neoplastic mucoceles. Besides, no neoplastic mucocele has a diameter smaller than two centimeters4.
The clinical presentation of mucocele in the appendix is usually unspecific, with difficult preoperative diagnosis. The most common complaint is pain in the right lower quadrant of the abdomen, which may last for months, being noticed in up to 50% of the cases, associated or not with a palpable tumor. About 25 to 50% of the subjects can be asymptomatic4,5.
The carcinoembryonic antigen (CEA) level at preoperative may suggest malignity in the appendix or in the colon9,10.
Imaging tests, such as ultrasound, computed tomography and enema, besides colonoscopy, may suggest the presence of mucocele of the appendix, which helps to define the treatment.
The ultrasound shows an encapsulated cystic lesion in the lower quadrant of the abdomen with a liquid content of variable echogenicity, according to the density of the mucus12. Some tests present images of multiple echogenic layers in the dilated appendix, which may be considered as pathognomonic of appendix mucocele13.
At computer tomography, the typical feature of mucocele of the appendix is a cystic mass with a thin wall and of low density, which communicates directly with the cecum (Figure 1). The presence of punctate or curvilinear calcification in this wall confirms the mucocele diagnosis and differs from the appendicular abscess, which does not have this characteristic6.
At enema, the presence of mucocele can be characterized by a cecal filling defect, besides the lateral displacement of the cecum and terminal ileum14.
Colonoscopy may show a soft erythematous mass, with a central crater due to the protrusion of appendiceal ostium, which can increase or decrease according to the respiratory movement15. This condition is known as "volcano sign"16 (Figure 2). This examination may still show the presence of synchronic neoplastic lesions in the colon, which occur in up to 20% of the cases17.
The cytology of the mucus inside the mucocele obtained by puncture with a thin needle may distinguish benign and malignant forms, but it should not be used due to the risk of cell dissemination and evolution to pseudomyxoma peritonei18,19.
The treatment of appendix mucocele is surgeryl and determined by some factors, such as the integrity of the wall of the organ, the dimensions of its base and histopathological examination of the cause of mucocele.
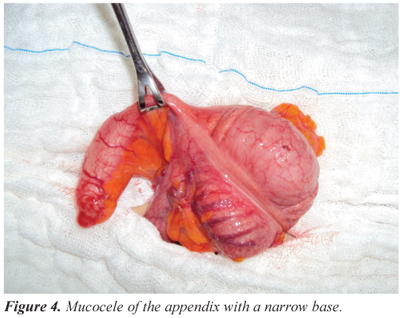
For mucocele (Figure 3), appendectomy with lymphadenectomy, including all the fat from the mesoappendix in the resection, is indicated for cases of simple or benign mucocele, when the appendicular base is not compromised by the dilation and is smaller than 2.0 cm (Figure 4).
The partial cecal resection with linear stapler cutter, including the site of implantation of the appendix, is performed in cases of mucocele with dilated appendicular base (larger than 2.0 cm), or at the presence of some cecal tumor.
This procedure prevents the dissemination of neoplastic cells to the abdominal cavity, besides ensuring a negative margin in the resection-line (Figures 5 and 6).
The release and exteriorization of the cecum should occur in order to reduce the risk of contamination in the abdominal cavity in cases of unwanted rupture during the manipulation of the cecal appendix.
In both surgical procedures, the cecal appendix is sent to frozen section. In case there is suspicion or detection of malignant neoplasm as the cause of mucocele, the resection is complemented with the right colectomy, with the objective of removing the whole lymphatic chain of the region. If the frozen section is not available at the time of the initial surgery, which is usually urgent, right colectomy should not be performed. This can prevent unnecessary abdominal incisions, since the malignant neoplasm is the cause of mucocele in only 10 to 20% of the cases7. If the lymph nodes are increased and the frozen section is positive for malignity, or even if the histopathological examination of the surgical piece confirms the malignant etiology, the patient is submitted to right colectomy. However, when the patient undergoes colonoscopy at the preoperative and a malignant neoplasm is diagnosed in the cecum, or if a cecal tumor is noticed, right colectomy is the first choice.
A complete abdominal exploration during intraoperative is indicated due to the occurrence of mucocele in synchrony with other tumors, like colon and ovaries. This conduct is mainly indicated when the surgery is performed with urgency, and preoperative examinations are not made17.
In cases of mucocele, lymphadenectomy in the mesoappendix is common to help the pathologist define the histology of the lesion. Besides, lymphadenectomy is important to define the conduct of other cecal appendix tumors, like carcinoid and adenocarcinoid tumors, which may eventually lead to mucocele19,20.
If the mucocele is simple and benign, appendectomy with lymphadenectomy is the definite treatment, as well as it is for carcinoid and adenocarcinoid tumors with favorable histology (small, with negative and well differentiated lymph nodes) and endometriosis. If the histological diagnosis points to bowel or mucinous adenocarcinoma, carcinoid or adenocarcinoid tumors larger than 2.0 cm, with positive lymph nodes or high mitotic rate, the resection is complemented with right colectomy19,20.
Even though lymphatic dissemination is not so frequent in this type of tumor, the mucinous adenocarcinoma of the non-perforated appendix has higher chances of healing with the right colectomy. This surgery has low mortality rates, especially when elective and performed in patients at a good general state21,22.
The bowel adenocarcinoma is always submitted to right colectomy because the incidence of lymphatic dissemination is high in this type of tumor23.
The performance of appendectomy by videolaparoscopy in cases of mucocele is not indicated due to the manipulation and risk of appendicular rupture and the dissemination of mucus with the possibility of peritoneal implants24. In case mucocele is diagnosed during laparoscopy, the surgery should be converted into a laparotomy. However, some authors disagree as to the recommendation to avoid laparoscopy for mucocele, by saying that laparoscopic appendectomy to handle appendix tumors has late results, similar to the open technique, in case there is a careful manipulation of the organ and the use of protective envelopes25,26. However, although it is technically possible to remove the intact appendix with free resection margins with laparoscopy, the advantage of open surgery is the release and exteriorization of the cecum, avoiding the contamination of the cavity in case of accidental rupture of the appendix.
As to follow-up, a recent study suggests histological, clinical and genetic similarities in proliferative lesions of the appendix and colonic mucosa27. So, simple and hyperplastic mucoceles would not require follow-up, benign mucocele would be followed-up as an adenomatous polyp with colonoscopies, according to the follow-up of colonic adenomas28, and the malignant one would be followed-up as a colonic adenocarcinoma, with doses of CEA and serial colonoscopies29.
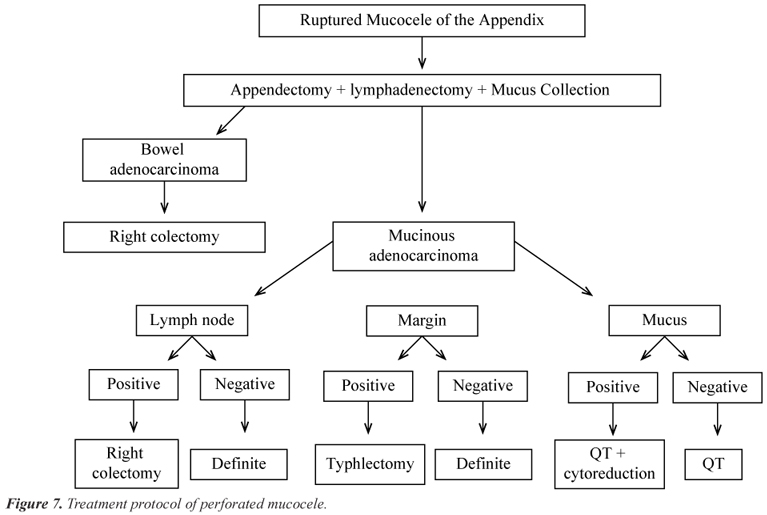
In cases of perforated mucocele of the appendix (Figure 7), there is mucus extravasation to the abdominal cavity, the pseudomyxoma peritonei. This entity was first described in 1884 by Werth30, and is characterized by implants of mucinous epithelium and mucus accumulation in the peritoneal cavity. The treatment depends on the histology of the appendix, the cytology of the ascitic fluid and the presence of positive lymph nodes in the mesoappendix23,31.
These patients may present an abrupt evolution, with symptoms that characterize acute appendicitis, or present chronic evolution, with an increased abdominal circumference, mucinous ascites, mucin within the hernia sac and ovarian tumor32.
Computed tomography can show the ascitic fluid, changes in hepatic contour and presence of nodes in the splenic capsule, corresponding to peritoneal implants, calcification of serous implantations; besides, it can also show metastatic ovarian carcinoma.
The initial surgery in cases of mucocele of the appendix is appendectomy, block resection of the appendicular fat and collection of mucinous ascitic fluid.
In patients with free mucinous fluid in the abdominal cavity, the peritoneum would work as a defense against the dissemination of epithelial cells. Thus, the initial surgery should be as minimal as possible, in order to keep the peritoneum intact23,31.
Patients with perforated mucocele who did not present positive lymph nodes or compromised margins, and who undergo right colectomy, present lower survival rates when compared to those who are only submitted to appendectomy at the time of the primary surgery23. Cases of deep invasion into paracaval retroperitoneal tissues at right colectomy have been reported, which is different from the minor superficial aggression, usually observed in patients with pseudomyxoma peritonei and an intact peritoneum33. This conduct is different from the primary colon cancer with peritoneal carcinomatosis, in which the results are better when the definite conduct is performed at the initial surgery34. However, if it is an adenocarcinoma of the intestine, or if the lymph nodes are positive as to malignity at the frozen section, right colectomy is performed at the initial surgery.
If the histopathological examination diagnoses bowel adenocarcinoma, the indication is right colectomy. If it is mucinous, the colectomy is performed if the lymph nodes of the appendicular fat are positive, and typhlectomy is indicated if the margins are compromised31. The lymphatic dissemination of the mucinous adenocarcinoma is rare, and the survival of these patients does not change when the bowel resection is magnified in cases in which the peritoneum is compromised23.
The prognosis of patients with adenocarcinoma of the appendix is controversial, depending on histological type. While some authors observe a better prognosis with bowel adenocarcinoma, others demonstrate more favorable results with the mucinous adenocarcinoma27,35,36.
As previously reported, any patient with benign or malignant mucocele of the appendix may have pseudomycoma peritonei, however, this condition is more common for the malignant mucocele4,5. There is no such risk in simple mucocele, since there are no epithelial cells in the mucus.
Mucus cytology should be immediately performed, because the result will define surgical therapy. If the cytology of the mucinous ascitic fluid is negative for adenomatous epithelial cells, the indication is hyperthermic intraoperative intraperitoneal chemotherapy. If it is positive, besides the operative chemotherapy, the cytoreductive surgery and postoperative intraperitoneal chemotherapy are performed31.
The cytoreductive surgery and intraperitoneal chemotherapy are indicated for patients with the disease limited to the peritoneum, with curative intent. This procedure is not recommended at the presence of unresectable malignant liver or distant disease. The surgery consists of trying to resect all visible peritoneal implants or, if it is not possible, of leaving only implants smaller than 2.5 mm in diameter, maximum limit for the intraperitoneal chemotherapy to work with curative intent. This may include omentectomy, splenectomy, upper quadrant and pelvic peritonectomy, cholecystectomy, partial or total colectomy, partial or total gastrectomy, besides rectosigmoidectomy and hysterectomy37-39.
After the cytoreductive surgert, the hyperthermic intraperitoneal chemotherapy is performed. Only after intraoperative chemotherapy, possible intestinal anastomoses can occur. At the end of surgery, abdominal drains are located in the cavity for postoperative chemotherapy37-39.
The extensive removal of the peritoneal surface may lead to a diffuse and deep implantation of malignant cells in the abdomen and pelvis, which would involve important structures, such as the ureter and blood vessels, if intraoperative intraperitoneal and immediate postoperative chemotherapies were not performed.
The hyperthermic intraperitoneal chemotherapy is performed with mitomycin or heated oxaliplatin (42ºC, for 60 to 120 min). Hyperthermia intensifies the cytotoxic effects of chemotherapy and increases the effect of the drug in the tissues.
The postoperative chemotherapy is performed with 5-fluorouracil in the first five postoperative days, which prevents free tumor cells to fixate on wound healing sites of peritonectomy, and also that adherences harm the uniform distribution of the drug in the abdominal cavity37-39.
Even at the unsuccessful attempt of complete cytoreduction, a better evolution is observed in these patients when compared to those who have not been submitted to any procedure38.
Only when surgical cytoreduction is minimal, there is no need for intraperitoneal chemotherapy. In this case, the option is systemic chemotherapy and palliative care39.
In patients with perforated appendix and neoplastic or epithelial cells disseminated into the peritoneal cavity, prognosis will be determined by chemotherapy and cytoreduction, and not by indication of appendectomy or right colectomy; it is important to ensure free resection margins at the base of the appendix, resection of all lymph nodes in the mesoappendix and collection of all peritoneal fluid for cytology23,31,40. If the tumor is mucinous and the resection margin is positive, the partial cecal resection is recommended, with a liner stapler cutter.
The follow-up of subjects with perforated mucocele of the appendix is valid considering that mucinous tumors of the appendix are rarely disseminated through lymphatic or hematogenic pathways, and that the dissemination limited to the peritoneal cavity would be a localized disease, with healing chances. However, there is no consensus as to the follow-up model. Medical history, physical examination and CEA dose, all performed every three months, are the main follow-up measures in patients submitted to cytoreductive surgery and intraperitoneal chemotherapy. Abdominal computed tomographies are performed every 6 to 12 months, or only in cases of CEA elevation and changes observed at clinical evaluation41.
The prognosis of patients with pseudomyxoma peritonei was very poor, with limited life expectancy and no chances of healing. The cytoreduction associated with hyperthermic intraperitoneal chemotherapy has reached survival rates in five years of 50% to 96%, in selected cases, when peritoneal cytoreduction is complete and there are no distant metastases41,42,43.
Submitted on: 13/09/2010
Approved on: 31/01/2011
Financing source: none
Conflict of interest: nothing to declare
Study carried out at the Service of Coloproctology of HBDF, Brasília (DF), Brazil
- 1. Rokitansky CF. A manual of pathological anatomy. Vol 2. English translation of the Vienna edition (1842). Philadelphia: Blancard and Lea, 1855:89.
- 2. Woodruff R, McDonald J. Benign and malignant cystic tumors of the appendix. Surg Gynecol Obstet 1940;71:751-5.
- 3. Misdraji J, Yantiss RK, Graeme-Cook FM, Balis UJ, Young RH. Appendiceal mucinous neoplasms. A clinicopathologic analysis of 107 cases. Am J Surg Pathol 2003;27(8):1089-103.
- 4. Stocchi L, Wolff BG, Larson DR, Harrington JR. Surgical treatment of appendiceal mucocele. Arch Surg 2003;138:585-90.
- 5. Ruiz-Tovar J, Teruel DG, Castineiras VM, Dehesa AS, Quindós PL, Molina EM. Mucocele of the appendix. World J Surg 2007;31(3):542-8.
- 6. Kim SH, Lim HK. Mucocele of the appendix: ultrassonographic and CT findings. Abdom Imaging 1998;23(3):292-6.
- 7. Higa E, Rosai J, Pizzimbono CA, Wise L. Mucosal hyperplasia, mucinous cystadenoma, and mucinous cystadenocarcinoma of the appendyx. A re-evalutation of appendiceal mucocele. Cancer 1973;32(6):1525-41.
- 8. Driman DK, Melega DE, Vilos GA, Plewes EA. Mucocele of the appendix secondary to endometriosis. Report of two cases, one with localized psedomyxoma peritonei. Am J Clin Pathol 2000;113(6):860-4.
- 9. Yamane YD, Yamane H, Castro Júnior PC, Marsilac A, Mesquita RB, Paulo FL. Mucolele da apêndice - relato de caso e revisão da literatura. Rev bras Coloproct 2005;25(3):256-60.
- 10. Fonseca LM, Sassine GCA, Luz MMP, Silva RG, Conceição SA, Lacerda-Filho A. Cistoadenoma de apêndice - relato de caso e revisão da literatura sobre tumores mucinosos do apêndice vermiforme. Rev bras Coloproct 2008;28(1):89-94.
- 11. Ronnett CM, Zahn CM, Kurman RJ, Kass ME, Sugarbaker PH, Shmookler BM. Disseminated peritoneal adenomucinosis and peritoneal mucinous carcinomatosis. A clinicopathologic analysis of 109 cases with emphasis on distinghishing pathologic features, site of origin, prognosis, and relationship to pseudomyxoma peritonei. Am J Surg Pathol 1995;19(12):1390-408.
- 12. Sasaki K, Ishida H, Komatsuda T, Suzuki T, Konno K, Ohtaka M, et al. Appendiceal mucocele: sonographic findings. Abdom Imaging 2003;28(1):15-8.
- 13. Caspi B, Cassif E, Auslender R, Herman R, Hagay Z, Appelman Z. The onion skin sign: a specific sonographic marker of appendiceal mucocele. J Ultrassound Med 2004; 23(1):117-21.
- 14. Pickhardt PJ, Levy AD, Rohrmann CA Jr, Kende AI. Primary neoplasms of the appendix: radiologic spectrum of disease with pathologic correlation. Radiographics 2003;23(3):645-62.
- 15. Zanati SA, Martin JA, Baker JP, Streutker CJ, Marcon NE. Colonoscopic diagnosis of mucocele of the appendix. Gastrointest Endosc 2005;62(3):452-6.
- 16. Hamilton DL, Stormont JM. The volcano sign of appendiceal mucocele. Gastrointest Endosc 1989;35(5):453-6.
- 17. Fujiwara T, Hizuta A, Iwagaki A, Matsuno T, Hamada M, Tanaka N, et al. Appendiceal mucocele with concomitant colonic cancer. Report of two cases. Dis Colon Rectum 1996;39(2):232-6.
- 18. Zuzarte JC, Liu YC, Cohen AM. Fine needle aspiration cytology of appendiceal mucinous cystadenoma: a case report. Acta Cytol 1996;40(2) 327-30.
- 19. Pahlavan PS, Kanthan R. Goblet cell carcinoid of the appendix. World J Surg Oncol 2005;3(36):1-11.
- 20. Fornaro R, Frascio M, Sticchi C, De Salvo L, Stabilini C, Mandolfino F, et al. Appendectomy or right hemicolectomy in the treatment of appendiceal carcinoid tumors? Tumori 2007;93(6):587-90.
- 21. Veyril N, Ata T, Muscari F, Couchard A, Msika S, Hay J, et al. Anastomotic leakage after elective right colectomy versus left colectomy for cancer: Prevalence and independent risk factors. J Am Coll Surg 2007;205(6):785-93.
- 22. Gurevitch AJ, Davidovitch B, Kashtan H. Outcome of right colectomy for cancer in octogenarians. J Gastrointest Surg 2009;13(1):100-4.
- 23. González Moreno S, Sugarbaker PH. Right hemicolectomy does not confer a survival advantage in patients with mucinous carcinoma of the appendix and peritoneal seeding. Br J Surg 2004;91(3):304-11.
- 24. González Moreno S, Shmookler BM, Sugarbaker PH. Appendiceal mucocele. Contraindication to laparoscopic appendectomy. Surg Endosc 1998;12(9):1177-9.
- 25. Navarra G, Asopa V, Basaglia E, Jones M, Jiao LR, Habib NA. Mucous cystadenoma of the appendix: is it safe to remove it by a laparoscopic approach? Surg Endosc 2003;17(5):833-4.
- 26. Bucher P, Mathe Z, Demirag A, Morel P. Appendix tumors in the era of the laparoscopic appendectomy. Surg Endosc 2004;18(7):1063-6.
- 27. Kabbani W, Houlihan PS, Luthra R, Hamilton SR, Rashid A. Mucinous and non-mucinous appendiceal adenocarcinomas: different clinicopathological features but similar genetic alterations. Mod Pathol 2002;15(6):599-605.
- 28. Winawer SJ, Zauber AG, Fletcher RH, Stillman JS, O'Brien MJ, Levin B, et al. Guidelines for colonoscopy surveillance after polipectomy: a consensus update by the US Multi-Society Task Force on Colorectal Cancer and the American Cancer Society. J Clin Oncol 2006;56(3):143-59.
- 29. Desch CE, Benson III AB, Somerfield MR, Flynn PJ, Krause C, Loprinzi CL, et al. Colorectal cancer surveillance: 2005 update of an American Society of Clinical Oncology practice guideline. J Clin Oncol 2005;23(33):8512-9.
- 30. Werth R. Kliniche and anastomische untersuchungen zur lehre von der bauchgeschwullsten und der laparotomy. Arch Gynecol Obstet 1884;24:100-18.
- 31. Dhage-Ivatury S, Sugarbaker PH. Update on the surgical approach to mucocele of the appendix. J Am Coll Surg 2002;202(4):680-4.
- 32. Esquivel J, Sugarbaker PH. Clinical presentation of the pseudomyxoma peritonei syndrome. Br J Surg 2000;87(10):1414-8.
- 33. Ortega-Perez G, Sugarbaker PH. Right psoas muscle/aortoiliac groove recurrence: an unusual anatomic site for progression of epithelial tumors of the appendix. Int Surg 2002;87(4):212 -6.
- 34. Pestieau SR, Sugarbaker PH. Treatment of primary colon cancer with peritoneal carcinomatosis: comparison of concomitant vs. delayed management. Dis Colon Rectum 2000;43(10):1341-8.
- 35. Ito H, Osteen RT, Bleday R, Zinner MJ, Ashley SW, Whang EE. Appendiceal adenocarcinoma: long-term outcomes after surgical therapy. Dis Colon Rectum 2004;47(4):474-80.
- 36. Cortina R, McCormick J, Kolm P, Perry RR. Management and prognosis of adenocarcinoma of the appendix. Dis Colon Rectum 1995;38(8):848-52.
- 37. Stephens AD, Alderman R, Chang D, Edwards GD, Esquivel J, Sebbag G, et al. Morbidity and mortality analysis of 200 treatments with cytoreductive surgery and hyperthermic intraoperative intraperitoneal chemotherapy using the coliseum technique. Ann Surg Oncol 1999;6(8):790-6.
- 38. Murphy EM, Sexton R, Moran BJ. Early results of surgery in 123 patients with pseudomyxoma peritonei from a perfurated appendiceal neoplasm. Dis Colon Rectum 2006;50(1):37-42.
- 39. Esquivel J, Sticca R, Sugarbaker P, Levine E, Yan TD, Alexander R, et al. Cytoreductive surgery and hyperthermic intraperitoneal chemotherapy in the management of peritoneal surface malignancies of colonic origin: a consensus statement. Ann Surg Oncol 207;14(1):128-33.
- 40. González-Moreno S, Brun E, Sugarbaker PH. Lymph nodes metastasis in epithelial with peritoneal dissemination does not reduce survival in patients treated by cytoreductive surgery and perioperative intraperitoneal chemotherapy. Ann Surg Oncol 2005;12(1):72-80.
- 41. Verwaal VJ, Zoetmulder FAN. Follow-up of patients treated by cytoreduction and chemotherapy for peritoneal carcinomatosis of colorectal origin. Eur J Surg Oncol 2004;30(3):280-5.
- 42. Loungnarath R, Causeret S, Bossard N, Faheez M, Sayag-Neaujard AC, Brigand C, et al. Cytoreductive surgery with intraperitoneal chemohyperthermia for the treatment of pseudomyxoma peritonei: a prospective study. Dis Colon Rectum 2005;48(7):1372-9.
- 43. Deraco M, Baratti D, Inglese MG, Allaria B, Andreola S, Gavazzi C, et al. Peritonectomy and intraperitoneal hyperthermic perfusion: a strategy that has confirmed its efficacy in patients with pseudomyxoma peritonei. Ann Surg Oncol 2004;11(4):393-8.
Correspondence to:
Publication Dates
-
Publication in this collection
07 May 2012 -
Date of issue
Sept 2011
History
-
Accepted
31 Jan 2011 -
Received
13 Sept 2010