Abstracts
Introduction
The prevalence of fecal incontinence (FI) has increased in recent decades, due to an aging population; and result in negative impacts on quality of life. Therefore, it is essential to search for an effective treatment in order to minimize the morbidity caused by incontinence.
Objective
To evaluate the effect of perineal training in the treatment of patients with fecal incontinence by biofeedback.
Method
This is a prospective study which evaluated 85 patients with FI from January 2009 to January 2014, at the Coloproctology outpatient clinic of the Hospital São Lucas/Cascavel, Paraná.
Results
Mean age was 47 years and the duration of treatment ranged from 5 to 25 sessions (mean, 13 sessions). From the women involved in the study, 70% (50) had vaginal deliveries and 34 (40%) participants were submitted to some orificial surgery. The FI score at baseline was 10.79 (6-17) and post-treatment FI was 2 (0-14) (p< 0.001). In the population studied, 49.4% (42) of the patients had an associated pre-BFT UI; and only 8.2% (7) had post-BFT UI (p< 0.001).
Conclusions
The data presented in this study confirm that perineal training through biofeedback was effective in the treatment of patients with fecal incontinence without immediate indication for surgery, still ensuring for this technique the advantages of being effective, painless and of low cost.
Fecal incontinence; Biofeedback; Anismus
Introdução
A prevalência de incontinência fecal (IF) vem aumentando nas últimas décadas devido ao envelhecimento da população; e resulta em impactos negativos na qualidade de vida. Logo, torna-se fundamental a busca de um tratamento efetivo, a fim de minimizar a morbidade ocasionada pela incontinência.
Objetivo
Avaliar o efeito do treinamento perineal no tratamento de pacientes portadores de incontinência fecal através do biofeedback.
Método
Estudo prospectivo, que avaliou 85 pacientes com IF no período de janeiro de 2009 a janeiro de 2014, no ambulatório de Coloproctologia do Hospital São Lucas/Cascavel, Paraná. Resultados: A média de idade foi de 47 anos e a duração do tratamento variou de 5 a 25 sessões (média de 13 sessões). Das mulheres envolvidas no estudo, 70% (50) tiveram partos vaginais e 34 (40%) indivíduos fizeram alguma cirurgia orificial. O escore de IF na avaliação inicial foi de 10,79 (6 a 17) e no pós-tratamento foi de 2 (0 a 14) (p < 0,001). Na população estudada, 49,4% (42) dos pacientes apresentaram IU associada no pré-TBF e apenas 8,2% (7) no pós-TBF (p < 0,001).
Conclusões
Os dados demonstrados neste estudo confirmam que o treinamento perineal através do biofeedback mostrou-se eficaz no tratamento de pacientes com incontinência fecal sem indicação imediata de cirurgia, assegurando ainda para essa técnica as vantagens de ser eficaz, indolor e de baixo custo.
Incontinência Fecal; Biofeedback; Anismus
Introduction
Fecal incontinence (FI) is a condition that results in significant physical and psychological disability, involving complex and multifactorial mechanisms.11. Alayne DM, Holly ER, Kathryn LB, Charlotte B, Alexandra LH, Leslee SL. Fecal incontinence in: obese women with urinary incontinence: prevalence and rol of dietary fiber intake. Am J Obstet Gynecol. 2009;200:566. It is generally defined as the involuntary loss of solid and liquid feces, with or without emission of flatus. Incontinence refers to a functional change in the anorectal area, leading to a loss of control of the passage of fecal material through the anus.22. Nelson RL. Epidemiology of fecal incontinence. Gastroenterology. 2004;126:3-7.
Although its prevalence is generally reported in females, in which epidemiological studies converge its results for the population over 65 years, there is a high prevalence in both men and women. However, women appear to be more susceptible, with the major risk factors being pudendal nerve or anal sphincter injury caused by obstetric trauma.22. Nelson RL. Epidemiology of fecal incontinence. Gastroenterology. 2004;126:3-7.,33. Ibrahim HS, Jorge NMJ, Habr-Gama A, Kiss RD, Rodrigues GJ. Avaliação da qualidade de vida na icontinência ana: validação do questionário FIQL (Fecal Incontinece Quality of Life). Arq Gastroenterol. 2004;41:2028. Regardless of its etiology, the emotional result impacts on quality of life, exceeding the limits of the physical, social, emotional and occupational domains.44. Oliveira CCL. Fisiologia Anorretal. Rio de Janeiro: Editora Rubio; 2010. It is hard to know the exact incidence of FI in the population, because in many cases the patient omits this fact. However, the effect described in the literature ranges from 0.1% to 5%.55. Oliveira L, Wexner SD. Anal Incontinence. In: Beck, Wexner, editors. Fundamentals of anorectal surgery. 2nd ed. London: W.B. Saunders; 1999. p. 115-52.
Paradoxical contraction of puborectal muscles, or anismus, is a pathology of idiopathic origin, affecting men and women; the anismus develops slowly and progressively, being usually accompanied by constipation. Clinically, anismus is manifested by the urge to defecate, without the ability to eliminate the whole rectal content, regardless of the degree of patient effort.66. Arend MGP, Fernanades WVB. Uso do biofeedback na incontinência fecal e dissinergia do assoalho pélvico- relato de caso. Revista saúde e pesquisa. 2009;2(3):433-6.
The mechanism of anal continence depends on the integrated action of: sphincter muscles; pelvic floor muscles; presence of the anorectal inhibitory reflex; of rectal capacity, sensitivity and compliance; stool consistency and intestinal transit time.77. Curi LA, Genoud MT. Causas más frecuentes de incontinencia fecal en nuestro medio. Acta Gastroenterol Latinoam. 2000;30:165-8.,88. Landefeld CS, Bowers AD, Feld BJ, Hartmann KE, Hoffman E, Ingber MJ, et al. National Institutes of Health state-of-the-science conference statement: prevention of fecal and urinary incontinence in adults. Ann Intern Med. 2008;148:449-58. As a result, any condition or disorder that alters any of these mechanisms can cause incontinence.99. Oliveira L. Incontinência Fecal. J Bras Gastroenterol. 2006;6:35-7. Therefore, it is critical to take into account the important role of the anal sphincters in preserving the continence, because with this knowledge a rehabilitation program for pelvic floor biofeedback training (BFT) can be established.
BFT is a technique that has been widespread since the late 70s, through the use of electronic equipment to inform its user, in a continuous and instantaneous way, about some of his/her internal (normal and abnormal) physiological events, in the form of visual and/or hearing signals.1010. Netinho JG, Dourado HM, Starling F, Ramalho EM. Tratamento da incontinência anal com biofeedback. Resultados preliminares. Rer Bras Coloproct. 1999;19:89-93. This technique allows the assessment and measurement of the patient progress through monitoring the tone at rest and the contractile ability of the muscle fiber and its support. Thus, BFT is effective in the course of the treatment of neuromuscular dysfunctions, improving the mobility, flexibility, and muscular coordination.1111. Pager CK, Solomon MJ, Rex J, Roberts RA. Long-term outcomes of pelvic floor exercise and Biofeedback treatment for patients with fecal incontinence. Dis Colon Rectum. 2002;45: 997-1003.
In this sense, BFT has been indicated in cases of mild to moderate incontinence; in the correction of severe defecation dysfunction; in cases of anismus, psychogenic megarectum (encopresis) and of chronic rectal pain; in incontinent patients without surgical indication; and, in some cases, in the postoperative phase of incontinence surgery, since studies demonstrate favorable results in improving the quality of life of these patients.1212. Tjandra JJ, Dykes RR, Kumar SL, Ellis CN, Gregorcyk SG, Hyman NH, et al. Normas Força-Tarefa Prática da Sociedade Americana de Cirurgiões cólon e reto. Parâmetros práticos para o tratamento da incontinência fecal. Dis Colon Rectum. 2007;50:1497-507. The aim of this study was to evaluate the effect of perineal training in the treatment of patients with fecal incontinence through biofeedback.
Patients and methods
This is a prospective study carried out between January 2009 and January 2014, involving 85 patients, 71 women and 14 men (83.5% and 16.4%, respectively), all of them with FI. These patients were attended at the Coloproctology outpatient clinic, Hospital São Lucas/Cascavel, Paraná by three colorectal surgeons. Patients were evaluated clinically, and the Fecal Incontinence Score proposed by Jorge-Wexner was applied; they also underwent physical examination.1313. Jorge JMN, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum. 1993;36:77-97. Then, these patients were evaluated by colonoscopy and anorectal electromanometry. Patients complaining of FI with and without anorectal electromanometry changes and without surgical indication at the time were included in this study. The perineal training in the treatment with BFT was performed by two physiotherapists (KR and MS).
The protocol consisted of a physiotherapeutic clinical assessment (collection of personal data, medical history and physical examination) and perineal training. The physical examination included skin inspection, presence of scars, and anal-vulvar distance; then, a digital palpation of the anus was performed to assess the voluntary contractile capacity of pelvic muscles, according to the table of Ortiz, graduated from 0 to 5 (Table 1).1414. Contreras Ortiz O, Coya Nunẽz F, Ibanẽz G. Evaluación funcional del piso pelviano femenino (classificación funcional). Bol Soc Latinoam Uroginecol Cir Vaginal. 1994;1:5-9. In the treatment with BFT, an electromyographic apparatus Miotool 400 (Miotec biomechanical equipment, Porto Alegre/Brazil) was used. This device consists of a 4-channel system with a gain of up to 8 times each, with 14-bit resolution and sampling frequency of 2000 Hz per channel. Only one channel was used, to which two differential surface sensors SDS500 were attached and connected with disposable electrodes (diameter 1.9 cm). The surface electrodes were applied in alignment over the perineum, and a reference electrode (ground) was fixed over the anterior superior iliac spine.
The patients followed the instructions for the treatment, which was divided into four phases: (1) contraction 10 times the pelvic floor muscles (PFM) with the highest possible strength and quickness, resting only for 1s between each contraction (5 repetitions); (2) contraction of PFM as hard as possible during 5 s and resting for 5 s (10 reps); (3) contraction of PFM as hard as possible during 10 s, resting for 10 s (5 reps); (4) defecation training: patient orientation during the defecation straining, in order to increase the abdominal pressure (Valsalva), in order to guide a proper puborectalis relaxation. The recommendations for maintaining the joint accessory muscles' (abdominals, glutei and adductors) non-contraction were followed. Patients were instructed and encouraged to perform home exercises and recommendations during the treatment and at its end.
All training was oriented according to the results of anorectal electronmanometry: (1) patients who had normotonia at rest and contraction and anismus: the sessions consisted entirely of BFT (group I); (2) patients presenting with contraction hypotonia: in addition of BFT, electrical stimulation was associated with the use of Neurodyn Evolution (Ibramed), a device which transmits low-amplitude electric current through a trans-anal electrode at a frequency of 50 Hz (the duration of the stimulation ranged from 15 to 30 min, and its intensity was determined in terms of patient comfort; the stimulation procedure was continued until the patient showed contractile ability of the muscles to start BFT) (group II); (3) patients who presented hypotonia at rest: in addition of BFT, the patient was submitted to 10 sessions of posterior tibial electronstimulation with Neurodyn Evolution (Ibramed), with low-amplitude current and frequency of 10 Hz and pulse duration of 200 μs. The stimulation time was 20 min for each session, with two surface electrodes: one applied over the medial malleolus and the other 10 cm above that point (group III).
The treatment protocol consisted of nine initial sessions; at the tenth session, a reassessment of the initial symptoms was performed, as a determinant factor to release the patient, or to proceed with the sessions until his/her release. The patient was released when a report of decreased frequency and/or intensity, or of absence of leakage and other associated symptoms was obtained. Then, along with the pre- and post-BFT Wexner score, the patient returned to the requesting physician.
The Student's t test was applied to evaluate the training response in relation to FI and urinary incontinence (UI).
Patients requiring surgery for incontinence, patients without cognitive understanding and those who did not agree to participate in this study were excluded. All patients signed a free informed consent and agreed to participate in the study, which was approved by the Ethics Committee of the Faculdade Assisi Gurgacz (FAG).
Results
The mean age of patients was 47 (29-81) years. The duration of treatment ranged from 5 to 25 (mean, 13) sessions. From the women involved in the study, 70% (50) had vaginal deliveries; and 34 (40%) patients had undergone at least one type of orificial surgery. The mean duration of incontinence was 14 years (range, 6 months to 43 years).
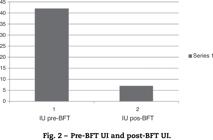
The group I was composed of 34 patients (40%); group II, 11 patients (12.9%); and group III, 40 patients (47.1%). The FI score at baseline was 10.79 (6-17) and after the treatment was 2 (0-14) (p < 0.001, Fig. 1). When the Student's t test was applied separately to these groups, it was evident that the pre- and post-treatment results were also statistically different. In the population studied, 49.4% (42) of the patients had associated UI in pre-BFT and only 8.2% (7) exhibited post-BFT UI (p < 0.001, Fig. 2).
Discussion
BFT is a well-established method for the treatment of patients with FI.1515. Norton C, Chelvanayagam S, Wilson-Barnett J, Redfern S, Kamm MA. Randomized controlled trial of biofeedback for fecal incontinence. Gastroenterology. 2003;125: 1320-9. The most common techniques used in pelvic floor muscle training include: anorectal manometry, displaying sphincter pressures; and electromyography, which can display electrical muscle activity.1616. Rao SS. Biofeedback therapy for constipation in adults. Best Pract Res Clin Gastroenterol. 2011;25:159-66.,1717. Jorge JM, Habr-Gama A, Wexner SD. Biofeedback therapy in the colon and rectal practice. Appl Psychophysiol Biofeedback. 2003;28:47-61.
The results of BFT are contradictory in the literature, especially due to the different techniques that can be used.1818. Lee HJ, Jung KW, Myung S-J. Technique of functional and motility test: how to perform biofeedback for constipation and fecal incontinence. J Neurogastroenterol Motil. 2013;19:532-7. A randomized controlled trial, in which BFT was applied in patients with FI, suggested that there was no difference between conservative treatment and/or BFT exercises.1515. Norton C, Chelvanayagam S, Wilson-Barnett J, Redfern S, Kamm MA. Randomized controlled trial of biofeedback for fecal incontinence. Gastroenterology. 2003;125: 1320-9. A meta-analysis demonstrated that muscle training was as effective as conservative treatment.1919. Enck P, Van der Voort IR, Klosterhalfen S. Biofeedback therapy in fecal incontinence and constipation. Neurogastroenterol Motil. 2009;21:1133–41. However, a recent controlled study showed that patients with an unsuccessful conservative treatment for FI and who were referred to BFT
showed 76% of successful responses.2020. Heymen S, Scarlett Y, Jones K, Ringel Y, Drossman D, Whitehead WE. Randomized controlled trial shows biofeedback to be superior to pelvic floor exercises for fecal incontinence. Dis Colon Rectum. 2009;52:1730-7. Other studies have reported positive responses ranging from 70% to 80%.2121. Jodorkovsky D, Dunbar KB, Gearhart SL, Stein EM, Clarke JO. Biofeedback therapy for defecatory dysfunction: “real life" experience. J Clin Gastroenterol. 2013;47:252-5.
In their multicenter study, Schwandner et al. reported that the combination of electrical stimulation with a prolonged muscle training (over three months) achieved the best results.2222. Schwandner T, König IR, Heimerl T, Kierer W, Roblick M, Bouchard R, et al. Triple target treatment (3T) is more effective than biofeedback alone for anal incontinence: the 3T-AI study. Dis Colon Rectum. 2010;53:1007-16. Chiarioni et al. reported that the benefits of BFT lasted for an average period of 12 months; thus, it is necessary that the training exercises are performed continuously2323. Chiarioni G, Whitehead WE. The role of biofeedback in the treatment of gastrointestinal disorders. Nat Clin Pract Gastroenterol Hepatol. 2008;5:371-82.,2424. Chiarioni S, Scarlett Y, Jones K, Ringel Y, Drossman D, Whitehead WE. Randomized controlled trial shows biofeedback to be superior to pelvic floor exercises for fecal incontinence. Dis Colon Rectum. 2009;52:1730-7. It is noteworthy, however, that the American College of Gastroenterology suggested that BFT is indicated in patients with sphincter hypotonia and/or impaired rectal sensitivity2525. Rao SS, American College of Gastroenterology Practice Parameters Committee. Diagnosis and management of fecal incontinence. American College of Gastroenterology Practice Parameters Committee. Am J Gastroenterol. 2004;99:1585-604. On the other hand, a small study reported that BFT was ineffective in patients with neurogenic FI.2626. Van Tets WF, Kuijpers JH, Bleijenberg G Biofeedback treatment is ineffective in neurogenic fecal incontinence. Dis Colon Rectum. 1996;39:992–4.
Thus, BFT should be offered to all patients who did not respond to medical interventions for FI, because this is a safe, cheap and long-term effective technique.2727. Ozturk R, Niazi S, Stessman M, Rao SS. Long-term outcome and objective changes of anorectal function after biofeedback therapy for faecal incontinence. Alim Pharmacol Ther 2004;20:667-74.
Elderly patients with normal physiology for defecation seem to respond well.2828. Fernández-Fraga X, Azpiroz F, Aparici A, Casaus M, Malagelada JR. Predictors of response to biofeedback treatment in anal incontinence. Dis Colon Rectum. 2003;46:1218-25.
Advanced anorectal physiology tests such as manometry, pelvic defecography, MRI, and pudendal nerve terminal motor latency testing do not seem to predict who will respond best to BFT2929. Terra MP, Deutekom M, Dobben AC, Baeten CG, Janssen LW, Boeckxstaens GE, et al. Can the outcome of pelvic-floor rehabilitation in patients with fecal incontinence be predicted? Int J Colorectal Dis. 2008;23:503-11. Patients with mild to moderate FI and who have not responded well to medical treatments are probably the best candidates for BFT3030. Boselli AS, Pinna F, Cecchini S, Costi R, Marchesi F, Violi V, et al. Biofeedback therapy plus anal electrostimulation for fecal incontinence: prognostic factors and effects on anorectal physiology. World J Surg. 2010;34:815-21.
In this study, patients who underwent treatment with a mixed technique, chosen from the results of anorectal elec-tronmanometry, showed a fall of FI score, from 10.76 to 2, with statistically significant difference. The techniques associated with biofeedback were: intracavitary (anal) electric stimulation and posterior tibial nerve stimulation. And even when the groups were separated, the difference was statistically significant. These data allow the achievement of better rates of success than those reported in the literature. This may be due to the fact that the technique was chosen because of a prior correct evaluation of the sphincteric apparatus by the colorectal surgeon.
Conclusion
The data presented in this study confirm that the perineal training through biofeedback was effective in the treatment of patients with fecal incontinence without immediate indication for surgery, as this is a technique with the advantages of being effective, painless and of low cost.
-
☆
This study was conducted at Coloproctology Outpatient Clinic, Hospital São Lucas, Cascavel, PR, Brazil.
REFERENCES
-
1Alayne DM, Holly ER, Kathryn LB, Charlotte B, Alexandra LH, Leslee SL. Fecal incontinence in: obese women with urinary incontinence: prevalence and rol of dietary fiber intake. Am J Obstet Gynecol. 2009;200:566.
-
2Nelson RL. Epidemiology of fecal incontinence. Gastroenterology. 2004;126:3-7.
-
3Ibrahim HS, Jorge NMJ, Habr-Gama A, Kiss RD, Rodrigues GJ. Avaliação da qualidade de vida na icontinência ana: validação do questionário FIQL (Fecal Incontinece Quality of Life). Arq Gastroenterol. 2004;41:2028.
-
4Oliveira CCL. Fisiologia Anorretal. Rio de Janeiro: Editora Rubio; 2010.
-
5Oliveira L, Wexner SD. Anal Incontinence. In: Beck, Wexner, editors. Fundamentals of anorectal surgery. 2nd ed. London: W.B. Saunders; 1999. p. 115-52.
-
6Arend MGP, Fernanades WVB. Uso do biofeedback na incontinência fecal e dissinergia do assoalho pélvico- relato de caso. Revista saúde e pesquisa. 2009;2(3):433-6.
-
7Curi LA, Genoud MT. Causas más frecuentes de incontinencia fecal en nuestro medio. Acta Gastroenterol Latinoam. 2000;30:165-8.
-
8Landefeld CS, Bowers AD, Feld BJ, Hartmann KE, Hoffman E, Ingber MJ, et al. National Institutes of Health state-of-the-science conference statement: prevention of fecal and urinary incontinence in adults. Ann Intern Med. 2008;148:449-58.
-
9Oliveira L. Incontinência Fecal. J Bras Gastroenterol. 2006;6:35-7.
-
10Netinho JG, Dourado HM, Starling F, Ramalho EM. Tratamento da incontinência anal com biofeedback. Resultados preliminares. Rer Bras Coloproct. 1999;19:89-93.
-
11Pager CK, Solomon MJ, Rex J, Roberts RA. Long-term outcomes of pelvic floor exercise and Biofeedback treatment for patients with fecal incontinence. Dis Colon Rectum. 2002;45: 997-1003.
-
12Tjandra JJ, Dykes RR, Kumar SL, Ellis CN, Gregorcyk SG, Hyman NH, et al. Normas Força-Tarefa Prática da Sociedade Americana de Cirurgiões cólon e reto. Parâmetros práticos para o tratamento da incontinência fecal. Dis Colon Rectum. 2007;50:1497-507.
-
13Jorge JMN, Wexner SD. Etiology and management of fecal incontinence. Dis Colon Rectum. 1993;36:77-97.
-
14Contreras Ortiz O, Coya Nunẽz F, Ibanẽz G. Evaluación funcional del piso pelviano femenino (classificación funcional). Bol Soc Latinoam Uroginecol Cir Vaginal. 1994;1:5-9.
-
15Norton C, Chelvanayagam S, Wilson-Barnett J, Redfern S, Kamm MA. Randomized controlled trial of biofeedback for fecal incontinence. Gastroenterology. 2003;125: 1320-9.
-
16Rao SS. Biofeedback therapy for constipation in adults. Best Pract Res Clin Gastroenterol. 2011;25:159-66.
-
17Jorge JM, Habr-Gama A, Wexner SD. Biofeedback therapy in the colon and rectal practice. Appl Psychophysiol Biofeedback. 2003;28:47-61.
-
18Lee HJ, Jung KW, Myung S-J. Technique of functional and motility test: how to perform biofeedback for constipation and fecal incontinence. J Neurogastroenterol Motil. 2013;19:532-7.
-
19Enck P, Van der Voort IR, Klosterhalfen S. Biofeedback therapy in fecal incontinence and constipation. Neurogastroenterol Motil. 2009;21:1133–41.
-
20Heymen S, Scarlett Y, Jones K, Ringel Y, Drossman D, Whitehead WE. Randomized controlled trial shows biofeedback to be superior to pelvic floor exercises for fecal incontinence. Dis Colon Rectum. 2009;52:1730-7.
-
21Jodorkovsky D, Dunbar KB, Gearhart SL, Stein EM, Clarke JO. Biofeedback therapy for defecatory dysfunction: “real life" experience. J Clin Gastroenterol. 2013;47:252-5.
-
22Schwandner T, König IR, Heimerl T, Kierer W, Roblick M, Bouchard R, et al. Triple target treatment (3T) is more effective than biofeedback alone for anal incontinence: the 3T-AI study. Dis Colon Rectum. 2010;53:1007-16.
-
23Chiarioni G, Whitehead WE. The role of biofeedback in the treatment of gastrointestinal disorders. Nat Clin Pract Gastroenterol Hepatol. 2008;5:371-82.
-
24Chiarioni S, Scarlett Y, Jones K, Ringel Y, Drossman D, Whitehead WE. Randomized controlled trial shows biofeedback to be superior to pelvic floor exercises for fecal incontinence. Dis Colon Rectum. 2009;52:1730-7.
-
25Rao SS, American College of Gastroenterology Practice Parameters Committee. Diagnosis and management of fecal incontinence. American College of Gastroenterology Practice Parameters Committee. Am J Gastroenterol. 2004;99:1585-604.
-
26Van Tets WF, Kuijpers JH, Bleijenberg G Biofeedback treatment is ineffective in neurogenic fecal incontinence. Dis Colon Rectum. 1996;39:992–4.
-
27Ozturk R, Niazi S, Stessman M, Rao SS. Long-term outcome and objective changes of anorectal function after biofeedback therapy for faecal incontinence. Alim Pharmacol Ther 2004;20:667-74.
-
28Fernández-Fraga X, Azpiroz F, Aparici A, Casaus M, Malagelada JR. Predictors of response to biofeedback treatment in anal incontinence. Dis Colon Rectum. 2003;46:1218-25.
-
29Terra MP, Deutekom M, Dobben AC, Baeten CG, Janssen LW, Boeckxstaens GE, et al. Can the outcome of pelvic-floor rehabilitation in patients with fecal incontinence be predicted? Int J Colorectal Dis. 2008;23:503-11.
-
30Boselli AS, Pinna F, Cecchini S, Costi R, Marchesi F, Violi V, et al. Biofeedback therapy plus anal electrostimulation for fecal incontinence: prognostic factors and effects on anorectal physiology. World J Surg. 2010;34:815-21.
Publication Dates
-
Publication in this collection
Oct-Dec 2014
History
-
Received
24 Feb 2014 -
Accepted
11 Aug 2014