Abstracts
ABSTRACT
Buschke-Loewenstein Tumor or giant condyloma acuminatum is a disease caused by a DNA virus, the self-inoculable human papilloma virus (HPV), being sexually transmitted. Histologically BLT is a benign tumor, but with malignant clinical behavior and a high propensity for local recurrence and malignant degeneration. The clinical picture consists of the presence of a cauliflower-like bulky condylomatous perianal mass with multiple fistulous tracts, which can cause great destruction of the anal canal, with invasion of adjacent tissues. Bleeding, foul odor, local pain and weight loss are also described. The diagnosis is established by biopsy, that should exclude the presence of malignant transformation, which occurs in 30-50% of cases. Associated with a biopsy, the hybridization test may be performed to diagnose HPV infection, especially subtypes 6 and 11, that are commonly related. The treatment of choice is radical surgical excision; however, those patients presenting with extensive fistulous lesions may require a temporary colostomy. Some authors advocate an abdominoperineal resection in cases of infiltration of the sphincter or rectum. This study was designed to evaluate the experience of the service of Coloproctology at a referral hospital in Northeastern Brazil with this rare entity, contributing to world literature in addressing this disease.
Giant condyloma acuminatum; Buschke-Loewenstein Tumor; Verrucous carcinoma; Human papillomavirus
RESUMO
Tumor de Buschke-Loewenstein ou condiloma acuminado gigante é uma doença causada por um vírus de DNA, o papilomavírus humano (HPV), auto-inoculável, sendo transmi-tido sexualmente. Histologicamente, são tumores benignos, porém, de comportamento clínico maligno, apresentando alta propensão à recorrência local e a degeneração maligna. O quadro clínico consiste na presença de uma volumosa massa condilomatosa perianal, com aspecto de couve-flor, com numerosos trajetos fistulosos, podendo provocar grande destruição do canal anal e invasão dos tecidos adjacentes. Sangramento, odor fétido, dor local e perda ponderal são também descritos. O diagnóstico é feito por biópsia, que deve afastar a presença de transformação maligna, que ocorre em 30-50% dos casos. Associado à biópsia, pode ser realizado um teste de hibridização para diagnosticar a infecção por HPV, principalmente os subtipos 6 e 11 que são comumente relacionados. O tratamento de escolha é a excisão cirúrgica radical, entretanto, os pacientes que apresentam lesão extensa com fístula, podem requerer colostomia temporária. Alguns autores advogam a amputação abdominoperineal do reto nos casos de infiltração dos esfíncteres ou do reto. O estudo foi designado para se avaliar a experiência do serviço de coloproctologia de um hospital de referência no Nordeste brasileiro com esta rara entidade, contribuindo com a literatura mundial na abordagem desta enfermidade.
Condiloma acuminado gigante; Tumor de Buschke-Loewenstein; Carcinoma verrucoso; Papilomavírus humano
Introduction
In 1894, Buschke drew attention to the existence of a variety of condyloma acuminatum of the penis, whose clinical behavior was invasive.11. Bessone A, Abeldano A, Sanguinetti O, Zorzopulos J. Condiloma acuminado gigante de Buschke y Lowenstein HPV tipo 16-18 tratado com metotrexato. Arch Argent Dermat. 1993;XLIII:397–404.–55. Vattimo A, Leite CC, Formiga GJS, Silva JH. Condiloma Gigante Acuminado Perianal (Tumor de Buschke-Loewenstein) Relato de um Caso. Rev Bras Coloproct. 1987;7:63-5. Later, in 1925, the same Buschke and Loewenstein described the condition as a well-defined clinical entity, the giant condyloma acuminatum, that received, since then, the name of Buschke-Loewenstein Tumor (BLT).66. Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40.–1010. Trombetta LJ, Place RJ. Giant condyloma acuminatum of the anorectum: trends in epidemiology and management. Dis Colon Rectum. 2001;44:1878-86.
BLT is a self-inoculable disease caused by a DNA virus, the human papilloma virus (HPV), and is sexually transmitted. Histologically, these are benign tumors, but with malignant clinical behavior, with a high propensity for local recurrence and malignant degeneration.55. Vattimo A, Leite CC, Formiga GJS, Silva JH. Condiloma Gigante Acuminado Perianal (Tumor de Buschke-Loewenstein) Relato de um Caso. Rev Bras Coloproct. 1987;7:63-5.
Since the description of the first case of this disease in the anal region in 1963 by Knoblich and Failig, until 2003 only 52 cases had been reported in the English literature.1010. Trombetta LJ, Place RJ. Giant condyloma acuminatum of the anorectum: trends in epidemiology and management. Dis Colon Rectum. 2001;44:1878-86.–1212. Gilbert SM, Lambert SM, Weiner D. Extensive condylomata acuminata of the penis: medical and surgical management. Infect Urol. 2003;16:65-76.
There is no treatment defined for the Buschke-Loewenstein Tumor; topical agents, immunotherapy, surgery and chemora-diotherapy are tentatively used. Surgery, alone or in conjunction with other methods, involves extensive resections; and in cases of invasion of the anal sphincter, an abdominoperineal resection of the rectum is required.1313. Bertram P, Treutner KH, Rubben A, Hauptmann S, Schumpelick V. Invasive squamous-cell carcinoma in giant anorectal condyloma (Buschke-Loewenstein tumor). Langenbecks Arch Chir. 1995;380:115-8.–1515. Braga JCT, Nadal SR, Stiepcich M, Framil VMS, Muller H. Buschke-Loewenstein tumor: identification of HPV type 6 and 11. An Bras Dermatol. 2012;87:131–4.
This study was designed to evaluate the experience of the service of Coloproctology at a referral hospital in Northeastern Brazil with this rare entity, contributing to world literature in addressing this disease.
Method
This is a retrospective longitudinal study, a series of cases treated at the Hospital of Coloproctology Barão de Lucena - SES/PE through the medical records of all patients who underwent biopsy for suspicion of anal condyloma, obtained from the surgery register in the period from February 1996 to February 2006. The authors identified six cases diagnosed as Buschke-Loewenstein Tumor. Then, an analysis of the clinical picture, treatment instituted and patient outcome was carried out.
Those patients lost to follow-up were contacted through telegrams, phone calls or by an active search of their home.
Clinical case 1
A 48-year-old male patient with a history of perianal tumor and purulent discharge from the perineum, pain and weight loss for ±2 months. On physical examination, an ulcerated lesion in the anal margin was observed, invading the rectum and anal canal up to ±6 cm from the anal margin, with fis-tulization to the perineum. Laboratory tests: VDRL - negative; HIV - negative; CEA = 2.0ng/mL, whole abdomen USG - normal. The histopathology was suggestive of anal condyloma of viral origin with secondary suppurative chronic inflammation in the corium.
Intralesional interferon has been proposed, but the patient refused treatment, returning to the outpatient clinic only after a period of 4 months. On this occasion, he showed progression of the lesion, with the rectum and anal canal almost completely obstructed by an ulcerative-vegetative tumor, invading the prostatic cavity and ischiorectal fossa, with multiple fis-tulae to the perineum and gluteal region. The upper limit of the tumor was not reached by the examiner's finger. This patient also had severe leukocytosis (30,000 cells/mm33. Hyacinthe M, Karl R, Coppola D, Goodgame T, Redwood W, Goldenfarb P, et al. Squamous-cell carcinoma of the pelvis in a giant condyloma acuminatum: use of neoadjuvant chemoradiation and surgical resection. Dis Colon Rectum. 1998;41:1450-5.) with a left shift. Antibiotics and drainage of abscesses and fistulae, including the scrotum, were established and a new biopsy was performed, that was consistent with Buschke-Loewenstein Tumor.
Then, we proposed an abdominoperineal resection, but it was decided that only a terminal sigmoid colostomy would be performed, because the tumor was considered unresectable. The patient was discharged and his last contact with the service was at the urgency unit, when he was seen with complaints of fever and dysuria, being medicated and released home.
Clinical case 2
A 27-year-old female patient with complaints of perianal tumor for 8 months, in association with elimination of a purulent drainage, difficulty to defecate and pain. On physical examination, multiple (eight) fistulous openings were observed in the right gluteal region with elimination of a purulent drainage, besides a circumferential mass in the anal margin and canal, with partial stenosis. The patient was hospitalized and underwent debridement of perianal tumor tissue with curettage of the fistulous tracts.
The histopathology demonstrated an absceded, fistulous, nonspecific chronic inflammation. HIV and VDRL tests were negative. The patient underwent a loop colostomy, returning months later with worsening of the disease, when was evidenced a vegetating, absceded and ulcerated tumor that began at ±7 cm from the anal margin externally, reaching the right hemicircumference of the rectum and with invasion into the ischiorectal fossa. The histopathology revealed condyloma acuminatum with areas of ulceration and hyperplasic granulation tissue.
The patient underwent local excision, and the result of the histopathological examination was consistent with a keratinizing, vegetative and infiltrating squamous cell carcinoma of the anal margin, showing moderate differentiation.
We opted for radiation and chemotherapy with 5-fluorouracil at a dose of 1g/m2 of body surface area/day/ continuous infusion for 4 days, starting on the 1st and 21st days of radiation therapy, and cisplatin at a dose of 75 mg/m2 of body surface area/infusion of 2 h on the 2nd and 22nd days of radiation therapy. The total dose of radiotherapy was 4500 cGy with 180 cGy/day for 28 days. The patient was discharged after the second cycle; however, she died at home before being evaluated as to the treatment outcome.
Clinical case 3
A 38-year-old female patient with a picture of rectal bleeding, elimination of purulent drainage associated with perianal tumor, pain and weight loss of 5 kg about 6 months ago. A physical examination identified a large ulcerated, hard and brittle lesion, which extended up to 2 cm from the anal margin, occupying the entire right hemicircumference, with the presence of pus, blood and cellulitis in the gluteal region. The patient was hospitalized and underwent endovaginal US, when a bulky mass to the right of the anal canal measuring 4.1cm × 2.4 cm was demonstrated, with no signs of abscess. The histopathological examination revealed presence of a giant condyloma of Buschke-Loewenstein. The lesion was affecting part of the right gluteal region and anal canal in right lower quadrant (RLQ) and right upper quadrant (RUQ). Then, we decided by performing a loop colostomy. The patient developed a pericolostomic abscess, which was drained prior to her discharge.
The patient was re-admitted after 2 months with a weight loss of 15 kg and severe anemia (Hb = 8.1mg/dl and Ht = 27%), being treated with hemotransfusion; then, she underwent a local resection of part of the gluteal region bilaterally, perianal region, posterior wall of the vagina and coccyx, in a monoblock procedure. The histopathological examination confirmed presence of giant condyloma acuminatum and an absceded chronic inflammation.
The patient is well after a follow-up of 20 months, with her wound healed and with only one paracolostomic hernia, for which she refuses a surgical correction.
Clinical case 4
A 36-year-old male patient presenting perianal vegetating lesion involving the entire sphincter muscle, associated with pain for about 5 months.
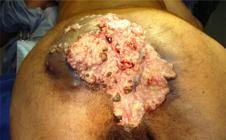
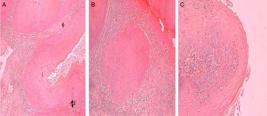
The patient underwent partial resection of the lesion (superficial hygienic resection). The histopathological findings were consistent with verrucous carcinoma. One month later, the patient was seen with extensive and invasive condylomatous lesion with important anterior fixation, with fetid odor and a purulent drainage and myiasis (Fig. 1). On physical examination, the lesion was considered unresectable; on that occasion, the patient received local care and was prescribed a blood transfusion. After defining the unresectability, the patient was discharged and sent for care at a Support Home with outpatient follow-up. The patient returned after 7 months in a state of important cachexia, dehydration and anemia, with a vegetating giant lesion causing great destruction of the anal sphincter and gluteal region, with fistulization and several necrotic areas with an extremely foul odor. The histopathology demonstrated a verrucous carcinoma (Fig. 2). The patient died before performing the scheduled colostomy.
Extensive condylomatous lesion with large tissue destruction in the gluteal region, perineum and base of the scrotum; multiple fistulas and purulent discharge.
(A and B) Stromal invasion (of corium) with inflammatory reaction is demonstrated. (C) Hyperkeratosis and parakeratosis, hyperchromasia and irregularity, binucleation, change in nucleus/cytoplasm ratio and koilocytes are evidenced (HE stain, 10 x).
Clinical case 5
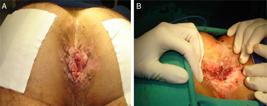
A 23-year-old male patient with complaints of small perianal tumors about 7 months ago, showed significant bleeding in stools in recent days, pain and difficulty to evacuate. HIV-positive, asymptomatic, on antiretroviral treatment. On physical examination, a cauliflower-like vegetative mass bleeding easily to the touch, with drainage and fistulization was observed, affecting the entire anal margin in a radial extent of ±15 cm (Fig. 3A). Treated with local resection with electrocautery, after infiltration with adrenaline solution (Fig. 3B).
(A) Cauliflower-like giant condyloma acuminatum (GCA) in association with microsatellite lesions and with spontaneous bleeding. (B) The final appearance after electrofulguration.
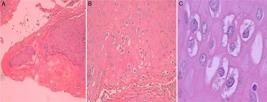
The histopathological examination confirmed the presence of condyloma acuminatum (Fig. 4).
(A-C) Hyperkeratosis, dyskeratosis, nuclear hyperchromasia and irregularity, changes in the nucleus/cytoplasm ratio and koilocytes are evidenced (HE staining, 10x, 40x and 60x, respectively).
The patient had been receiving outpatient treatment when, after 4 months, suffered a recurrence of the lesion in the anal margin of ±8 cm in diameter, extending to the entire anal canal. A new local resection was performed, with preservation of the anal sphincter (Fig. 5A and B).
(A) Disease recurrence 4 months after the first surgery; (B) postoperative appearance after a new local resection.
The histopathological examination confirmed the presence of condyloma acuminatum. After 7 months, the patient returned with a history of perianal tumor associated with pruritus for ±60 days. On physical examination, a vegetating lesion of ±3 cm in diameter was observed in the anal margin, occupying the right hemicircumference, exactly at the anodermal junction without apparent involvement of the anal canal (Fig. 6). A new surgical resection was performed and, to date, the patient has no signs of recurrence.
Clinical case 6
A 27-year-old male patient with perianal lesions with blood in stools, pain and difficulty to defecate, unaware of the duration of these symptoms. The patient exhibited cognitive impairment, and the communication between family members and himself was markedly impaired.
On physical examination, a bulky, vegetative, bleeding, condylomatous lesion around the anal canal was observed, with no signs of invasion of deep structures. Patient HIV- and VDRL-negative. A local resection of the tumor with a margin of ±2 cm was performed, saving the sphincter muscles and leaving the wound open.
The histopathological examination revealed a giant condyloma (Buschke-Loewenstein Tumor) (Fig. 7).
(A-C) Hyperkeratosis, parakeratosis, hyperchromasia and nuclear irregularity, changes in the nucleus/cytoplasm ratio and koilocytes are evidenced. (A) Acanthosis and papillomatosis are still observed (HE staining, 10 x, 40 x and 60 x, respectively).
Thirteen months after surgery, the patient returned to the clinic with no complaints and with complete healing of his wound, without deformity or retraction, an intact sphincter and in a state of continence. On the other hand, exhibited Oxiurus in his anal margin, which was treated with Albendazole (Fig. 8).
Table 1 summarizes the main demographic data, symptoms, physical examination, therapeutic regimens and evolution of the six cases.
Demographic data, symptoms, lesion characteristics, therapeutic regimens and patient outcomes.
Discussion
Since the first description of a giant condyloma by Buschke-Loewenstein, few cases have been reported in the perianal and anal location.55. Vattimo A, Leite CC, Formiga GJS, Silva JH. Condiloma Gigante Acuminado Perianal (Tumor de Buschke-Loewenstein) Relato de um Caso. Rev Bras Coloproct. 1987;7:63-5.
Although there are no prospective randomized studies on giant condyloma acuminatum, numerous case reports exist in the literature. From these, speculations about the best treatment strategy have been drawn.1010. Trombetta LJ, Place RJ. Giant condyloma acuminatum of the anorectum: trends in epidemiology and management. Dis Colon Rectum. 2001;44:1878-86.
In the present study, the patients' age ranged from 23 to 48 years, predominantly in the third decade of life (3 cases). According to the literature, GCA is found in the age group from 18 to 70 years, with a mean age of 43 years, especially between the 4th and 6th decades of life.11. Bessone A, Abeldano A, Sanguinetti O, Zorzopulos J. Condiloma acuminado gigante de Buschke y Lowenstein HPV tipo 16-18 tratado com metotrexato. Arch Argent Dermat. 1993;XLIII:397–404.,66. Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40.,1212. Gilbert SM, Lambert SM, Weiner D. Extensive condylomata acuminata of the penis: medical and surgical management. Infect Urol. 2003;16:65-76. Studies have shown a tendency to GCA onset in an increasingly early age,1010. Trombetta LJ, Place RJ. Giant condyloma acuminatum of the anorectum: trends in epidemiology and management. Dis Colon Rectum. 2001;44:1878-86. which was also observed in our study.
Regarding gender, our series consisted of 4 males and 2 females, with a male-female ratio of 2:1. The predominance of males is in agreement with most studies, showing a higher incidence in males, with a ratio of 2.2:1.11. Bessone A, Abeldano A, Sanguinetti O, Zorzopulos J. Condiloma acuminado gigante de Buschke y Lowenstein HPV tipo 16-18 tratado com metotrexato. Arch Argent Dermat. 1993;XLIII:397–404.,66. Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40.,1212. Gilbert SM, Lambert SM, Weiner D. Extensive condylomata acuminata of the penis: medical and surgical management. Infect Urol. 2003;16:65-76.
The most frequent symptoms were: presence of perianal mass and pain, which were observed in all patients, discharge of pus (four patients), bleeding (three patients), difficulty of defecation (three patients), weight loss (three patients) and rash (one patient). These findings were similar to those found in most series, that report: perianal mass in 47% of cases, perianal pain in 32%, fistula or abscess in 32%, bleeding in 18%, weight loss in 10% and rash in 4%.1010. Trombetta LJ, Place RJ. Giant condyloma acuminatum of the anorectum: trends in epidemiology and management. Dis Colon Rectum. 2001;44:1878-86.
In this series, fistulas were present in five cases, with invasion of the anal canal demonstrated in five patients and invasion of the rectum in three, besides other structures (scrotum, perineum, prostatic cavity, ischiorectal fossa, gluteus or vagina), being considered locally advanced in four patients. As the literature shows, the clinical course of perianal GCA can be very aggressive, causing fistulas and infiltration of deep tissues,1111. Cerdán FJ, Martin J, De Loa Morena MT, Furió V, Ruiz De Leon A, Balibrea JL. Condiloma acuminado anorrectal gigante (Tumor de Buschke-Loewenstein). Rev Esp Enf Ap Digest. 1987;71:525-8. as shown in most of our patients.
Diagnoses were obtained based on histopathological examinations, with many patients requiring multiple studies to confirm the diagnosis. Thanks to its appearance and size, the Buschke-Loewenstein Tumor can be confused with malignant tumors of the perianal region. Therefore, the histological diagnosis is very important. When a malignant tumor is not found, there is a trend to obtain a new biopsy to confirm the absence of neoplasia, because of fear that the material may not have been representative. In the same tumor, one can find a very wide spectrum, from areas of condyloma acuminatum, severe dysplasia and carcinoma in situ, to a frankly invasive squamous cell carcinoma.
The difficulty for the establishment of a diagnosis lies primarily in the importance in ruling out the presence of malignant transformation, because the confirmation of BLT does not necessarily exclude the possibility of squamous cell carcinoma. Given this, multiple biopsies involving the entire depth of the lesion should be made, because superficial samples may cover only inflammatory tissue or maybe condy-lomatous tissue, with superficial thickening, without offering the pathologist the opportunity to assess a possible invasion of the basal lamina.
The malignant transformation is revealed in the areas that show the squamous cell carcinoma associated with condyloma, which was observed on one of our patients. According to the literature, the malignant transformation of Buschke-Loewenstein Tumor has been reported in 30-56% of cases.33. Hyacinthe M, Karl R, Coppola D, Goodgame T, Redwood W, Goldenfarb P, et al. Squamous-cell carcinoma of the pelvis in a giant condyloma acuminatum: use of neoadjuvant chemoradiation and surgical resection. Dis Colon Rectum. 1998;41:1450-5.,66. Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40.,77. Chu DQ, Vezeredis MP, Libbey NP, Wanebo HJ. Giant condyloma acuminatum (Buschke-Loewenstein Tumor) of the anorectal and perianal regions. N Engl Cancer Soc. 1993;37:950-8.,99. Gonzales GA, Zavala LCE, La Mora FC, Arriaga AO, Zamora AC, Nakamura AC, et al. Buschke-Loewenstein tumor in childhood: a case report. J Pediatr Surg. 2005;40:E25-7.
The giant condyloma appears to be histologically similar to simple condyloma acuminatum.11. Bessone A, Abeldano A, Sanguinetti O, Zorzopulos J. Condiloma acuminado gigante de Buschke y Lowenstein HPV tipo 16-18 tratado com metotrexato. Arch Argent Dermat. 1993;XLIII:397–404.,88. Elke I, Grussendorf C. Anogenital premalignant and malignant tumors (including Buschke-Loewenstein Tumors). Clin Dermatol. 1997;15:377-88.,1212. Gilbert SM, Lambert SM, Weiner D. Extensive condylomata acuminata of the penis: medical and surgical management. Infect Urol. 2003;16:65-76.,1616. Qarro A, Ali AA, Choho A, Alkandry S, Borki K. Tumeur de Buschke-Loewenstein à localisation anorectale (Àpropôs de trois cas). An Chir. 2005;130:96-100. An invasive clinical behavior is the critical factor for the diagnosis. Many authors consider the Buschke-Loewenstein Tumor as a variant of the verrucous carcinoma, but others believe it is just a different nomenclature for the same disease. This confusion regarding nomenclature is another difficulty for its diagnosis. Often the result of histopathology is a verrucous carcinoma (as in our patients), but we only consider the presence of malignancy if there is an invasion of the basal lamina.
There are several treatments that can be used in GCA, from topical agents (podophyllin, ATA, 5-fluorouracil) to immunotherapy, interferon, radiotherapy, chemotherapy, cryotherapy, laser, electrocautery and surgery (local excision or amputation of the rectum and anus). The choice will depend on the number of lesions, their extent, degree of infiltration, the involvement of the anal canal or rectum and the presence (or non-presence) of malignant transformation.1717. Sobrado CW, Andraus W, Marques CFS, Nahas SC, Bochini SF, Nadalin V, et al. Condiloma Acuminado Perianal Gigante Recidivante Tratado com Radioterapia. Experiência inicial e Relato de Caso. Rev Bras Coloproct. 1999;19:103-7.
The standard approach to the giant condyloma acuminatum is radical surgical excision. Patients with extensive lesions, complicated by severe local infection, require a temporary colostomy. The abdominal-perineal amputation of the rectum is reserved for those patients with invasion of the rectum and anal sphincter, especially the external sphincter muscle.66. Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40.,1616. Qarro A, Ali AA, Choho A, Alkandry S, Borki K. Tumeur de Buschke-Loewenstein à localisation anorectale (Àpropôs de trois cas). An Chir. 2005;130:96-100.
In those cases where there is a malignant transformation, the optimal treatment is not well defined; however, studies have shown that chemoradiotherapy can be used prior the radical surgical treatment.22. Gomes CLR, Cruvinel RCF, Almeida JLM, et al. Condiloma acuminado gigante (tumor de Buschke-Loewenstein). Rev Bras Med. 2003;60:860–4.,33. Hyacinthe M, Karl R, Coppola D, Goodgame T, Redwood W, Goldenfarb P, et al. Squamous-cell carcinoma of the pelvis in a giant condyloma acuminatum: use of neoadjuvant chemoradiation and surgical resection. Dis Colon Rectum. 1998;41:1450-5.,66. Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40. In the single case of malignant degeneration in our series, the chemoradiotherapy was not followed by radical surgery, because the lesion was already well advanced and the patient died shortly after the end of treatment.
According to the literature, mortality occurs in 20% of patients and relapse in 50% of cases treated with radical surgery. In our study, death occurred in two patients (33.3%), among those regularly followed, in the period of 8 months and 2 years after diagnosis, respectively. Recurrence was observed in one patient among the three who underwent curative surgery. In this same patient, there were two recurrences at a mean time of 4.5 months. The follow-up time for the three patients who underwent curative surgery was 11, 13 and 20 months. Two patients were lost to follow-up, and it was not possible to assess the actual number of deaths and relapses.
The aggressive behavior of the tumor, with invasion of adjacent tissues, determined, in most of our patients, difficulties in handling the injury. The primary factor implicated for this behavior was the slowness between the onset of symptoms, the first consultation and the initiation of treatment.
Conclusions
As can be seen from this review, the Buschke-Loewenstein Tumor is a rare disease in which only six cases were diagnosed within 10 years.
Although considered a benign lesion, BLT is locally aggressive, with fistulization and invasion of adjacent tissues, with the outstanding feature of high rates of relapse, which was observed in one third of the operated cases. A high mortality rate (1/3 of patients) among those patients regularly followed was observed in this survey, as also reported in the literature.
References
-
1Bessone A, Abeldano A, Sanguinetti O, Zorzopulos J. Condiloma acuminado gigante de Buschke y Lowenstein HPV tipo 16-18 tratado com metotrexato. Arch Argent Dermat. 1993;XLIII:397–404.
-
2Gomes CLR, Cruvinel RCF, Almeida JLM, et al. Condiloma acuminado gigante (tumor de Buschke-Loewenstein). Rev Bras Med. 2003;60:860–4.
-
3Hyacinthe M, Karl R, Coppola D, Goodgame T, Redwood W, Goldenfarb P, et al. Squamous-cell carcinoma of the pelvis in a giant condyloma acuminatum: use of neoadjuvant chemoradiation and surgical resection. Dis Colon Rectum. 1998;41:1450-5.
-
4Nazário ACP, Bernardo A, Lima GR, Nicolau SM, Schivartche V. Condiloma acuminado gigante (tumor de Buschke-Loewenstein) com transformação maligna. Relato de caso. Rev Bras Cancerol. 1993;39:205-7.
-
5Vattimo A, Leite CC, Formiga GJS, Silva JH. Condiloma Gigante Acuminado Perianal (Tumor de Buschke-Loewenstein) Relato de um Caso. Rev Bras Coloproct. 1987;7:63-5.
-
6Chao MWT, Gibbs P. Squamous cell carcinoma arising in a giant condyloma acuminatum (Buschke-Loewenstein Tumour). Asian J Surg. 2005;28:238–40.
-
7Chu DQ, Vezeredis MP, Libbey NP, Wanebo HJ. Giant condyloma acuminatum (Buschke-Loewenstein Tumor) of the anorectal and perianal regions. N Engl Cancer Soc. 1993;37:950-8.
-
8Elke I, Grussendorf C. Anogenital premalignant and malignant tumors (including Buschke-Loewenstein Tumors). Clin Dermatol. 1997;15:377-88.
-
9Gonzales GA, Zavala LCE, La Mora FC, Arriaga AO, Zamora AC, Nakamura AC, et al. Buschke-Loewenstein tumor in childhood: a case report. J Pediatr Surg. 2005;40:E25-7.
-
10Trombetta LJ, Place RJ. Giant condyloma acuminatum of the anorectum: trends in epidemiology and management. Dis Colon Rectum. 2001;44:1878-86.
-
11Cerdán FJ, Martin J, De Loa Morena MT, Furió V, Ruiz De Leon A, Balibrea JL. Condiloma acuminado anorrectal gigante (Tumor de Buschke-Loewenstein). Rev Esp Enf Ap Digest. 1987;71:525-8.
-
12Gilbert SM, Lambert SM, Weiner D. Extensive condylomata acuminata of the penis: medical and surgical management. Infect Urol. 2003;16:65-76.
-
13Bertram P, Treutner KH, Rubben A, Hauptmann S, Schumpelick V. Invasive squamous-cell carcinoma in giant anorectal condyloma (Buschke-Loewenstein tumor). Langenbecks Arch Chir. 1995;380:115-8.
-
14Coelho FMP, Mano AL, Bacellar MS, Codes LMG, Souza ELQ, Filho EMA. Tumor de Buschke-Loewenstein: tratamento com imiquimod para preservação esfincteriana. Relato de caso. Rev Bras Coloproct. 2008;28:342-6.
-
15Braga JCT, Nadal SR, Stiepcich M, Framil VMS, Muller H. Buschke-Loewenstein tumor: identification of HPV type 6 and 11. An Bras Dermatol. 2012;87:131–4.
-
16Qarro A, Ali AA, Choho A, Alkandry S, Borki K. Tumeur de Buschke-Loewenstein à localisation anorectale (Àpropôs de trois cas). An Chir. 2005;130:96-100.
-
17Sobrado CW, Andraus W, Marques CFS, Nahas SC, Bochini SF, Nadalin V, et al. Condiloma Acuminado Perianal Gigante Recidivante Tratado com Radioterapia. Experiência inicial e Relato de Caso. Rev Bras Coloproct. 1999;19:103-7.
Publication Dates
-
Publication in this collection
Oct-Dec 2014
History
-
Received
26 Nov 2013 -
Accepted
12 Aug 2014