Abstracts
Plasmodium parasites degrade host hemoglobin to obtain free amino acids, essential for protein synthesis. During this event, free toxic heme moieties crystallize spontaneously to produce a non-toxic pigment called hemozoin or ß-hematin. In this context, a group of azole antimycotics, clotrimazole (CTZ), ketoconazole (KTZ) and fluconazole (FCZ), were investigated for their abilities to inhibit ß-hematin synthesis (IßHS) and hemoglobin proteolysis (IHbP) in vitro. The ß-hematin synthesis was recorded by spectrophotometry at 405 nm and the hemoglobin proteolysis was determined by SDS-PAGE 12.5%, followed by densitometric analysis. Compounds were also assayed in vivo in a malaria murine model. CTZ and KTZ exhibited the maximal effects inhibiting both biochemical events, showing inhibition of β-hematin synthesis (IC50 values of 12.4 ± 0.9 µM and 14.4 ± 1.4 µM respectively) and inhibition of hemoglobin proteolysis (80.1 ± 2.0% and 55.3 ± 3.6%, respectively). There is a broad correlation to the in vivo results, especially CTZ, which reduced the parasitemia (%P) of infected-mice at 4th day post-infection significantly compared to non-treated controls (12.4 ± 3.0% compared to 26.6 ± 3.7%, p = 0.014) and prolonged the survival days post-infection. The results indicated that the inhibition of the hemoglobin metabolism by the azole antimycotics could be responsible for their antimalarial effect.
ß-hematin synthesis; Azole antimycotics; Hemoglobin degradation; Plasmodium berghei
Los parásitos del género Plasmodium degradan la hemoglobina hospedera obteniendo aminoácidos libres para su síntesis proteica. Durante este evento, unidades de hemo libre tóxicas cristalizan espontáneamente formando un pigmento no tóxico denominado ß-hematina. En este trabajo, se investigó la capacidad de un grupo de azoles antimicóticos: clotrimazol (CTZ), ketoconazol (KTZ) y fluconazol (FCZ), en inhibir la síntesis de ß-hematina y la proteólisis de la globina. La síntesis de ß-hematina se registro por espectrofotometría a 405 nm y la proteólisis de la hemoglobina se determino por SDS-PAGE 15% seguido por análisis densitométrico de las bandas de hemoglobina intactas. Los compuestos fueron también ensayados in vivo en un modelo de malaria murina. CTZ y KTZ inhibieron la síntesis de ß-hematina con CI50 entre 10 y 15 µM y bloquearon la proteólisis de la hemoglobina (80.01 ± 2.04% y 55.33 ± 3.57%, respectivamente). En relación directa con los resultados encontrados in vitro, el CTZ redujo la parasitemia de ratones infectados en forma significativa, así como prolongó lo días de sobrevivencia post-infección en comparación con animales controles no tratados. Se sugiere así que la inhibición del metabolismo de la hemoglobina por los antimicóticos azólicos pudiera ser el mecanismo responsable de su actividad antimalárica.
MALARIA
Disturbance in hemoglobin metabolism and in vivo antimalarial activity of azole antimycotics
Alteración en el metabolismo de la hemoglobina y actividad antimalárica in vivo de azoles antimicóticos
Juan Ricardo Rodrigues; Diana Lourenco; Neira Gamboa
Correspondence to Correspondence to: Dr. Juan Ricardo Rodrigues H. and/or Dr. Neira Delina Gamboa de D. Unidad de Bioquímica, Facultad de Farmacia, Universidad Central de Venezuela Apartado 47206, Los Chaguaramos Caracas 1051-A, Venezuela Phone: + 58-212-6052717. Fax: + 58-212-6052707. E-mail: juanricardorodrigues@yahoo.es; neira.gamboa@ucv.ve
SUMMARY
Plasmodium parasites degrade host hemoglobin to obtain free amino acids, essential for protein synthesis. During this event, free toxic heme moieties crystallize spontaneously to produce a non-toxic pigment called hemozoin or ß-hematin. In this context, a group of azole antimycotics, clotrimazole (CTZ), ketoconazole (KTZ) and fluconazole (FCZ), were investigated for their abilities to inhibit ß-hematin synthesis (IßHS) and hemoglobin proteolysis (IHbP) in vitro. The ß-hematin synthesis was recorded by spectrophotometry at 405 nm and the hemoglobin proteolysis was determined by SDS-PAGE 12.5%, followed by densitometric analysis. Compounds were also assayed in vivo in a malaria murine model. CTZ and KTZ exhibited the maximal effects inhibiting both biochemical events, showing inhibition of β-hematin synthesis (IC50 values of 12.4 ± 0.9 µM and 14.4 ± 1.4 µM respectively) and inhibition of hemoglobin proteolysis (80.1 ± 2.0% and 55.3 ± 3.6%, respectively). There is a broad correlation to the in vivo results, especially CTZ, which reduced the parasitemia (%P) of infected-mice at 4th day post-infection significantly compared to non-treated controls (12.4 ± 3.0% compared to 26.6 ± 3.7%, p = 0.014) and prolonged the survival days post-infection. The results indicated that the inhibition of the hemoglobin metabolism by the azole antimycotics could be responsible for their antimalarial effect.
Keywords: ß-hematin synthesis; Azole antimycotics; Hemoglobin degradation; Plasmodium berghei.
RESUMEN
Los parásitos del género Plasmodium degradan la hemoglobina hospedera obteniendo aminoácidos libres para su síntesis proteica. Durante este evento, unidades de hemo libre tóxicas cristalizan espontáneamente formando un pigmento no tóxico denominado ß-hematina. En este trabajo, se investigó la capacidad de un grupo de azoles antimicóticos: clotrimazol (CTZ), ketoconazol (KTZ) y fluconazol (FCZ), en inhibir la síntesis de ß-hematina y la proteólisis de la globina. La síntesis de ß-hematina se registro por espectrofotometría a 405 nm y la proteólisis de la hemoglobina se determino por SDS-PAGE 15% seguido por análisis densitométrico de las bandas de hemoglobina intactas. Los compuestos fueron también ensayados in vivo en un modelo de malaria murina. CTZ y KTZ inhibieron la síntesis de ß-hematina con CI50 entre 10 y 15 µM y bloquearon la proteólisis de la hemoglobina (80.01 ± 2.04% y 55.33 ± 3.57%, respectivamente). En relación directa con los resultados encontrados in vitro, el CTZ redujo la parasitemia de ratones infectados en forma significativa, así como prolongó lo días de sobrevivencia post-infección en comparación con animales controles no tratados. Se sugiere así que la inhibición del metabolismo de la hemoglobina por los antimicóticos azólicos pudiera ser el mecanismo responsable de su actividad antimalárica.
INTRODUCTION
Malaria remains one of the major infectious diseases in tropical countries and the emergence of resistance to the main antimalarial drugs along with the absence of a successful vaccine have led to a bigger risk of death in those areas11. Therefore, there is a compelling and urgent necessity for the discovery of new antimalarials13.
Hemoglobin degradation in intraerythrocytic malaria parasites is a biochemical event which occurs in the parasite acidic digestive vacuole by different proteases to provide free amino acids necessary for protein synthesis10. In this process, the oxidant heme group is separated from the globin chains and the parasite is protected from the deleterious effects of this porphyrin by its crystallization into an insoluble non-toxic pigment called hemozoin or ß-hematin4.
Azole antifungals clotrimazole (CTZ) and ketoconazole (KTZ) seem to act by preventing the synthesis of this pigment, an effect which is shared by quinoline compounds12. Moreover, CTZ has exhibited antimalarial activity in cultures of P. falciparum18. In this context we have evaluated the ability of the azole antimycotics, CTZ, KTZ and fluconazole (FCZ) to inhibit ß-hematin synthesis and globin proteolysis in vitro together with the evaluation of their effects on a Plasmodium berghei-murine model.
MATERIAL AND METHODS
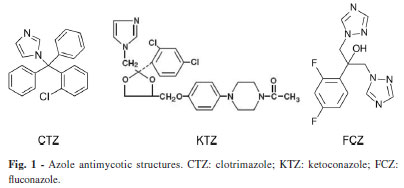
Reagents: CTZ, KTZ and FCZ (Fig. 1) were a generous gift given by Calox de Venezuela C.A. For in vitro assays, drugs were prepared as 100mM stock solution. CTZ and FCZ were dissolved in ethanol while KTZ was dissolved in methanol. All of the stock solutions were stored at 4 ºC. These solutions were diluted before the assays to reach final concentrations. For in vivo experiments, the dissolved azole compounds were diluted in Saline-Tween 20 (2%) and adjusted to a final concentration of 20 mg/kg/mouse.
Inhibition ofß-hematin synthesis: The inhibition of ß-hematin synthesis assay was performed according to a previous procedure3. In short, a solution of hemin chloride in DMSO (50 µL, 5.2 mg/mL) was distributed in 96-well micro plates. Different concentrations of dissolved compounds in DMSO (100-5 µM) were added in triplicate in test wells (50 µL) at final concentrations between 25 and 0.25 µM. Controls contained water (50 µL), DMSO (50 µL) or chloroquine (50 µL, 25-0.25 µM). The β-hematin synthesis was initiated by the addition of acetate buffer (100 µL, 0.2M, pH 4.4). Plates were incubated at 37 ºC for 48 h to allow completion of the reaction and centrifuged (20000 g x 15 min). After discarding the supernatant, the pellet was washed three times with DMSO (200 µL), dissolved in NaOH (200 µL, 0.2N) and diluted 1:2 with NaOH (0.1N), recording the absorbances at 405 nm (Microplate Reader, BIORAD-550). The obtained results were expressed as percentage of inhibition of ß-hematin synthesis relative to the drug-free control.
Experimental host and strain maintenance: Male albino mice (BALB/c, 18-22 g, were maintained on a commercial pellet diet and housed under conditions approved of by the Ethics Committee, School of Pharmacy, Central University of Venezuela. Plasmodium berghei (ANKA strain), a rodent malarial parasite, was used for infection. Mice were infected intraperitoneally with 107 infected erythrocytes diluted in phosphate buffer saline solution (PBS 10 mM, pH 7.4, 0.1 mL). Parasitemias were monitored by microscopic examination of Giemsa stained smears.
Mice native hemoglobin: Native hemoglobin from non-infected mice was obtained by mixing one volume of pellet erythrocytes and two volumes of water. The resulting lysate was used as the substrate in the hemoglobin proteolysis assay.
Parasite extracts: Blood of infected animals with high levels of parasitemia (30-50%) was collected via cardiac puncture. After centrifugation (500g x 10 min, 4 ºC), plasma and buffy coat were removed, and the red blood cells (RBCs) pellet was washed twice with chilled PBS-glucose (5.4%). The washed RBCs were centrifuged on a discontinuous percoll gradient (80-70% percoll in PBS-Glucose, 20000 g x 30 min, 4 ºC). The resulted upper band (erythrocytes infected with the mature forms of the parasites) was removed by aspiration, and washed twice with chilled PBS-glucose and lysed with saponin (0.1% in PBS x 10min). After adding cold PBS (1 mL) the samples were centrifuged (13000 g x 5 min, 4 ºC) to remove erythrocyte cytoplasmic material. Free parasites were suspended in PBS-glucose (5.4%) and subjected to three freeze-thaw cycles (-70 ºC / + 37 ºC) to obtain the final parasite extract which was used for the hemoglobin proteolysis assay17.
Hemoglobin proteolysis assay: The proteolytic effect of the parasite extract on the mouse hemoglobin was assayed using 96-well tissue culture plate. The assay mixture contained: mouse native hemoglobin (10 µL), parasite extract (50 µL), GSH (10 µL, 10 µM) and buffer acetate (0.2M, pH 5.4) to a final volume of 200 µL. The dissolved compounds (10 µL) were incorporated into the incubation mixture (5 µM final concentration). The incubations were carried out at 37 ºC for 18 hours and the reaction was stopped by addition of buffer (Tris base 0.125M, SDS 2%, ß-mercaptoethanol 5%, glycerol 20%, Bromophenol Blue 0.0025 %). The degree of digestion was evaluated electrophoretically by SDS-PAGE-15%17 followed by densitometric analysis of intact globin bands. Results were expressed as percentage of inhibition of hemoglobin proteolysis.
Four-day suppressive test (Peters' test): Azole antimycotics were also evaluated in a malaria murine model by the four-day suppressive test15 using chloroquine as a positive control (20 mg/kg). In short, native BALB/c mice (18-23 g) were infected intraperitoneally (ip) with 107 parasitized RBCs on day 0. Antimycotics were freshly prepared, dissolved in DMSO (0.1 M) and diluted with Saline-Tween 20 solution (2%). Two hours after the infection, mice received the first treatment (20 mg/kg, ip) and then every 24 hours for four consecutive days. Blood smears from the tails were prepared on the fourth day and parasitemias were determined by microscopic examination of Giemsa-stained blood films. Survivals were followed up until day 30th post-infection. The results were expressed as percentage of parasitemia on the fourth day post-infection and as survival days post-infection.
Data were presented as the average of four independent experiments (n = 4) and tested for statistical significance using unpaired t-tests for specific group comparisons assuming 95% confidence limits using GraphPad Prism 4.02 software. The maintenance of the experimental animals complied with the guidelines of the human use of laboratory animals.
RESULTS
Quinoline antimalarials as chloroquine are well known to inhibit β-hematin synthesis. In this study we confirmed that CTZ and KTZ exhibited a marked inhibition of β-hematin production. Special attention was paid to CTZ which reported no difference compared to positive control of chloroquine at the maximal dose tested (Table 1). On the other hand, the compounds alone (control without hemin) did not absorb at the same wavelength of β-hematin absorption (405 nm), which showed that the results represented a positive inhibition of this biochemical event.
Additionally, the study of the intact hemoglobin bands by electrophoretic analysis indicated that CTZ, KTZ and FCZ inhibited globin proteolysis (intact band at 14.4 kDa). CQ-treatment of trophozoites cultured with hemoglobin partially inhibited globin proteolysis (Fig. 2).
Moreover, the densitometric analysis showed more than 50% of inhibition of globin proteolysis for each of the azole compounds tested. These structures were more than twice as active as CQ (Fig. 3). This evidence supports a possible new mechanism of antimalarial action of these antimycotic compounds whereby parasites are deprived of the amino acids required for protein synthesis.
The in vivo results demonstrated that CTZ and KTZ were able to reduce the parasitemia levels at 4th day post-infection with significant differences compared to non treated infected animals (Fig. 4a). CTZ-treated mice also showed a prolongation of their survival rates; however, this drug did not clear the infection at the tested dose (Fig. 4b). Parasitemias of CQ-treated mice were cleared at the end of the assay and no deaths were registered in this group of animals. In this context, it is possible that the effects we observed in vivo could be correlated to the inhibition of β -hematin formation and globin proteolysis.
DISCUSSION
Plasmodium parasites degrade host hemoglobin through their aspartic and cysteine proteases as a source of nutrients8. In this process, free toxic heme moieties crystallize spontaneously in the acid environment of the digestive vacuole to an insoluble pigment called hemozoin or ß-hematin14. Chloroquine has been shown to inhibit hemozoin formation6 and this process is also thought to be the molecular target of other quinoline antimalarials19. Moreover the bisquinoline compound dequalinium has demonstrated antimalarial activity also through the inhibition of the globin proteolytic degradation16. Thus, ß-hematin synthesis and hemoglobin proteolysis, unique events occurring within the malaria parasites, offer a logical and valuable potential target for the development of new antimalarials.
TIFFERT et al.18 showed that CTZ inhibits P. falciparum growth in vitro, alters its morphology and interferes with parasite development and replication. Moreover, a series of heterocyclic azole-based compounds were described as inhibitors of P. falciparum lactate dehydrogenase at micromolar concentrations and these compounds displayed modest activity against parasitized erythrocytes, including parasite strains with known resistance to existing antimalarials and against Plasmodium berghei in BALB/c mice7.
Mechanisms of the antimalarial activity of CTZ have been proposed in relation to Ca2+ ions. This drug inhibits the sarcoplasmic reticulum Ca+2 pump, causing the depletion of intracellular Ca2+ stores5,18. This effect produces the activation of protein kinase R and phosphorylation of eukaryotic translation initiation factor 2α, which in consequence, inhibits protein synthesis1. However, the effects of CTZ and other azolic antifungal compounds on the hemoglobin proteolysis in malaria parasites are not known.
Our results confirmed that the imidazole compounds CTZ and KTZ inhibit ß-hematin formation, which might be due to the ability of these structures to form complexes with free heme moieties as it has been demonstrated with other antimalarials8. CHONG & SULLIVAN8 showed that these compounds also inhibited this event; however, we reported a stronger inhibition by CTZ compared to KTZ. Indeed, HUY et al.12 observed that the hydrophobic group of CTZ, three aromatic rings with a chlorine atom, should stabilize axial ligation to heme and forms a stable six-coordinate iron porphyrin complex with a high equilibrium association constant, which could explain the strong effects of this drug inhibiting the β-hematin formation in our results. When the amount of heme-CTZ complexes becomes critical, malaria-infected erythrocytes are expected to be hemolyzed, leading to parasite death. On the other hand, FCZ did not show activity inhibiting ß-hematin synthesis. This compound has a triazolic structure and it is possible that three nitrogen atoms are not favorable for the complex formation with free heme. Moreover, in this study we did not observe 100% of inhibition at the maximal dose tested and this could be due to the saturation of the compounds in the biological system.
These azole compounds were also tested for inhibition of globin proteolysis. The electrophoretic analysis indicated that the antimycotics were effective as inhibitors of hemoglobin degradation. Special attention should be paid to CTZ, which demonstrated the strongest effect inhibiting this event. Therefore, azole compounds exhibited activity avoiding free amino acid production by P. berghei from host hemoglobin. The mechanism of action of these drugs seems to be directly dependent on cysteine and/or aspartic protease inhibition since these proteases can degrade native globin during the initial steps of the hemoglobin degradation and leupeptin and pepstatin (cysteine and aspartic protease inhibitors) also inhibit this event10. The antimycotics were not tested as falcipain or plasmepsin inhibitors in vitro; however, the mechanism of action of these compounds on hemoglobin degradation could be related to the inhibition of one or both proteases. In this context, it would be necessary to examine the effect of the compounds on plasmepsin and cysteine proteases directly in further investigations.
GEMMA et al.9 previously described the in vivo antimalarial activity of CTZ orally by the decrease of the parasitemia levels in treated animals. In this context, we confirmed the activity of this compound and also KTZ in a malaria murine model. Both compounds were able to reduce the parasitemias at 4th day post-infection and CTZ increased the survival rate with significant differences compared to non-treated infected mice. These results could be the consequence of a dual mechanism of action, correlating the in vivo activity with the inhibition of ß-hematin formation and the inhibition of hemoglobin proteolysis. KTZ was also described to be active in vivo in a multidrug resistant Plasmodium yoelii nigeriensis murine model at high doses and enhanced the protective effect of mefloquine against the infection2.
It is important to note that the in vivo antimalarial activity of CQ is much stronger than that of the azole compounds and this could be due to dosage or bioavailability factors. It would therefore be interesting to assay different dose regimens or to develop some water soluble derivatives, which may provide a new medicinal chemistry route for research into this infectious disease. It would be important to test these compounds against chloroquine-resistant strains to determine their true value as antimalarials.
In conclusion, we propose that azole antimycotics, especially CTZ and KTZ could show antimalarial properties by the inhibition of two biochemical events occurring in the malaria parasite: the β-hematin synthesis and the globin proteolysis; the last one representing an alternative and new mechanism of action against the malaria parasites by these structures. Further enhancement of these structures might yield candidates suitable for consideration as new therapeutic compounds for the treatment of malaria.
ACKNOWLEDGEMENTS
This study was supported by Consejo de Desarrollo Científico y Humanístico, Central University of Venezuela (PG-CDCH-06.30.5125-2007). CTZ, KTZ and FCZ were a generous gift from CALOX-International. The experiments complied with the current laws in Venezuela.
Received: 29 August 2009
Accepted: 19 October 2010
Unidad de Bioquímica, Facultad de Farmacia, Universidad Central de Venezuela, Apartado 47206, Los Chaguaramos, Caracas 1051-A, Venezuela.
- 1. Aktas H, Flückiger R, Acosta JA, Savage JM, Palakurthi SS, Halperin JA. Depletion of intracellular Ca2+ stores, phosphorylation of eIF2alpha, and sustained inhibition of translation initiation mediate the anticancer effects of clotrimazole. Proc Natl Acad Sci USA. 1998;95:8280-5.
- 2. Awasthi A, Dutta GP, Bhakuni V, Tripathi R. Resistance reversal action of ketoconazole against mefloquine resistance of Plasmodium yoelii nigeriensis Exp Parasitol. 2004;107:115-9.
- 3. Baelmans R, Deharo E, Muñoz V, Sauvain M, Ginsburg H. Experimental conditions for testing the inhibitory activity of chloroquine on the formation of beta-hematin. Exp Parasitol. 2000;96:243-8.
- 4. Bendrat K, Berger BJ, Cerami A. Haem polymerization in malaria. Nature. 1995;378:138-9.
- 5. Benzaquen LR, Brugnara C, Byers HR, Gatton-Celli S, Halperin JA. Clotrimazole inhibits cell proliferation in vitro and in vivo Nat Med. 1995;1:534-40.
- 6. Blauer G, Akkawi M. β-hematin. Biochem Mol Biol Int. 1995;35:231-5.
- 7. Cameron A, Read J, Tranter R, Winter VJ, Sessions RB, Brady RL, et al. Identification and activity of a series of azole-based compounds with lactate dehydrogenase-directed anti-malarial activity. J Biol Chem. 2004;279:31429-39.
- 8. Chong CR, Sullivan DJ. Inhibition of heme crystal growth by antimalarials and other compounds: implications for drug discovery. Biochem Pharmacol. 2003;66:2201-12.
- 9. Gemma S, Campiani G, Butini S, Kukreja G, Coccone SS, Joshi BP, et al. Clotrimazole scaffold as an innovative pharmacophore towards potent antimalarial agents: design, synthesis and biological and structure-activity relationship studies. J Med Chem. 2008;51:1278-94.
- 10. Goldberg DE, Slater AF, Cerami A, Henderson GB. Hemoglobin degradation in the malaria parasite Plasmodium falciparum: an ordered process in a unique organelle. Proc Natl Acad Sci USA. 1990;87:2931-35.
- 11. Greenwood B, Mutabingwa T. Malaria in 2002. Nature. 2002;415:670-8.
- 12. Huy NT, Kamei K, Yamamoto T, Kondo Y, Kanaori K, Takano R, et al. Clotrimazole binds to heme and enhances heme-dependent hemolysis: proposed antimalarial mechanism of clotrimazole. J Biol Chem. 2002;277:4152-8.
- 13. Miller LH, Baruch DI, Marsh K, Doumbo OK. The pathogenic basis of malaria. Nature. 2002;415:673-9.
- 14. Orjih AU, Fitch CD. Hemozoin production by Plasmodium falciparum: variation with strain and exposure to chloroquine. Biochim Biophys Acta. 1993;1157:270-4.
- 15. Peters W. The chemotherapy of rodent malaria, XXII. The value of drug-resistant strains of P. berghei in screening for blood schizontocidal activity. Ann Trop Med Parasitol. 1975;69:155-71.
- 16. Rodrigues JR, Gamboa de Dominguez N. Plasmodium berghei: in vitro and in vivo activity of dequalinium. Exp Parasitol. 2007;115:19-24.
- 17. Rosenthal PJ. Plasmodium falciparum: effects of proteinase inhibitors on globin hydrolysis by cultured malaria parasites. Exp Parasitol. 1995;80:272-81.
- 18. Tiffert T, Ginsburg H, Krugliak M, Elford BC, Lew VL. Potent antimalarial activity of clotrimazole in in vitro cultures of Plasmodium falciparum Proc Natl Acad Sci USA. 2000;97:331-6.
- 19. Tilley L, Loria P, Foley M. Chloroquine and other quinoline antimalarials. In: Rosenthal PJ, editor. Antimalarial chemotherapy. Totowa: Humana Press; 2001. p. 87.
Correspondence to:
Publication Dates
-
Publication in this collection
04 Mar 2011 -
Date of issue
Feb 2011
History
-
Received
29 Aug 2009 -
Accepted
19 Oct 2010