Abstracts
PURPOSE: To describe the epidemiological profile of basal cell carcinoma patients at a private hospital in São Paulo and to evaluate the treatment adopted. METHODS: A prospective study of 202 patients, on which 253 lesions were diagnosed for histopathological exam as basal cell carcinoma within the period of January 2001 to September 2003, in the Plastic Surgery Residency Program at the Hospital Jaraguá. The susceptibility factor of the host, the environment variables, the characteristics of the lesions and the efficacy of the treatment were examined. The data were statistically evaluated. RESULTS: The incidence of basal cell carcinoma was 126 cases per 100,000 patients in a period of 32 months (36 cases per 100,000 patients/year). The patients were evenly distributed in terms of sex: 48% male and 52% female. The greater incidence was in patients between the ages of 60 and 80 years and the average was 64 years. The survey revealed susceptibility factors such as white race and phototypes I and II in 95.5% of the patients. Exposition to ultraviolet radiation was reported by 77% of the patients and the most frequent location of tumors was on the face (71.2% of the cases). Actinic keratosis and a history of skin cancer were reported in 43.6% and in 25% of the cases, respectively. The adopted treatment was surgery in 99.4% of the cases and only one patient was treated with radiotherapy. Twenty lesions (8%) had incomplete excision.The recurrence rate was 2% (5 cases). There were no cases with metastasis or fatal outcome. CONCLUSIONS: The factors related to the development of basal cell cancer which were significantly present in the population surveyed were: older age, white individuals, phototypes I and II, presence of actinic keratosis, previous history of non-melanoma skin cancer and exposure to ultra-violet rays both in recreational and in occupational form.The surgical treatment employed was effective with a rate of incomplete excision and recurrence similar to those found in the literature.
Neoplasms, Basal Cell; Skin Neoplasms; Epidemiologic Studies; Urban Population
OBJETIVO: Traçar o perfil epidemiológico dos portadores de carcinoma basocelular e , avaliar o tratamento instituído no Serviço de Residência de Cirurgia Plástica do Hospital Jaraguá. MÉTODOS: Foi realizado um estudo prospectivo de 202 pacientes, nos quais foram diagnosticados 253 lesões por exame anátomo-patológico como carcinoma basocelular no período de janeiro de 2001 a setembro de 2003, no Serviço de Residência de Cirurgia Plástica do Hospital Jaraguá. Foram abordados fatores de susceptibilidade do hospedeiro, fatores ambientais, características das lesões, o tratamento instituído e sua eficácia. Os dados encontrados foram submetidos à análise estatística. RESULTADOS: A incidência de carcinoma basocelular encontrada foi de 126 casos/ 100.000 pacientes em 32 meses (36casos/100.000 pacientes/ano). Os pacientes se distribuíram de forma semelhante entre os sexos masculino (48%), e feminino (52%), com uma incidência maior na faixa etária entre 60 e 80 anos (69%), com média de 64,0 anos. A amostra apresentou fatores de susceptibilidade como a raça branca e fototipos I e II em 95,5% dos pacientes. A exposição à radiação ultravioleta foi informada por 77% dos pacientes, e a localização mais freqüente dos tumores foi a face, em 71,2% dos casos. A ceratose actínica e a história de câncer de pele anterior estavam presentes em 43,6% e 25,8%, respectivamente. O tratamento instituído foi o cirúrgico em 99,4% dos casos, sendo que um caso foi tratado com radioterapia por falta de condições clínicas. No anátomo-patológico foram encontradas 20 lesões (8%) com margens comprometidas pelo tumor. A taxa de recidiva no acompanhamento pós-operatório foi de 2% (5 casos). Não houve casos de metástase ou óbito. CONCLUSÕES: Os fatores relacionados ao desenvolvimento do carcinoma basocelular que estão presentes de forma significante na população estudada são: idade avançada,raça branca, fototipos I e II, presença de ceratose actínica, história anterior de câncer de pele não-melanoma e exposição aos raios ultra-violetas tanto de forma recreacional quanto ocupacional.O tratamento instituído foi efetivo com taxas de margens comprometidas e recidivas comparáveis com as da literatura.
Neoplasia de Células Basais; Neoplasias Cutâneas; Estudos Epidemiológicos; População Urbana
ORIGINAL ARTICLE
Basal cell carcinoma: an updated epidemiological and therapeutically profile of an urban population1 1 . Plastic Surgery Residence Program at the Hospital Jaraguá (São Paulo) and Federal University of São Paulo (UNIFESP), Brazil.
Carcinoma basocelular: perfil epidemiológico e terapêutico de uma população urbana
Roberta Lopes BarianiI; Fábio Xerfan NahasII; Marcus Vinícius Jardini BarbosaIII; Andréia Bufoni FarahIV; Lydia Masako FerreiraV
IPlastic Surgeon member of the Brazilian Society of Plastic Surgery. Brazil
IIAssociate Professor of the Division of Plastic Surgery -UNIFESP-EPM. Brazil
IIIPlastic Surgeon, Master Degree in Medicine of UNIFESP. Brazil
IVPlastic Surgeon, Master Degree in Medicine of UNIFESP. Brazil
VFull Professor of the Division of Plastic Surgery of UNIFESP. Brazil
Correspondence Correspondence: Roberta Lopes Bariani Rua Inhambu, 332 04520-010 São Paulo SP Brazil r.bariani@uol.com.br
ABSTRACT
PURPOSE: To describe the epidemiological profile of basal cell carcinoma patients at a private hospital in São Paulo and to evaluate the treatment adopted.
METHODS: A prospective study of 202 patients, on which 253 lesions were diagnosed for histopathological exam as basal cell carcinoma within the period of January 2001 to September 2003, in the Plastic Surgery Residency Program at the Hospital Jaraguá. The susceptibility factor of the host, the environment variables, the characteristics of the lesions and the efficacy of the treatment were examined. The data were statistically evaluated.
RESULTS: The incidence of basal cell carcinoma was 126 cases per 100,000 patients in a period of 32 months (36 cases per 100,000 patients/year). The patients were evenly distributed in terms of sex: 48% male and 52% female. The greater incidence was in patients between the ages of 60 and 80 years and the average was 64 years. The survey revealed susceptibility factors such as white race and phototypes I and II in 95.5% of the patients. Exposition to ultraviolet radiation was reported by 77% of the patients and the most frequent location of tumors was on the face (71.2% of the cases). Actinic keratosis and a history of skin cancer were reported in 43.6% and in 25% of the cases, respectively. The adopted treatment was surgery in 99.4% of the cases and only one patient was treated with radiotherapy. Twenty lesions (8%) had incomplete excision.The recurrence rate was 2% (5 cases). There were no cases with metastasis or fatal outcome.
CONCLUSIONS: The factors related to the development of basal cell cancer which were significantly present in the population surveyed were: older age, white individuals, phototypes I and II, presence of actinic keratosis, previous history of non-melanoma skin cancer and exposure to ultra-violet rays both in recreational and in occupational form.The surgical treatment employed was effective with a rate of incomplete excision and recurrence similar to those found in the literature.
Key words: Neoplasms, Basal Cell. Skin Neoplasms. Epidemiologic Studies. Urban Population.
RESUMO
OBJETIVO: Traçar o perfil epidemiológico dos portadores de carcinoma basocelular e , avaliar o tratamento instituído no Serviço de Residência de Cirurgia Plástica do Hospital Jaraguá.
MÉTODOS: Foi realizado um estudo prospectivo de 202 pacientes, nos quais foram diagnosticados 253 lesões por exame anátomo-patológico como carcinoma basocelular no período de janeiro de 2001 a setembro de 2003, no Serviço de Residência de Cirurgia Plástica do Hospital Jaraguá. Foram abordados fatores de susceptibilidade do hospedeiro, fatores ambientais, características das lesões, o tratamento instituído e sua eficácia. Os dados encontrados foram submetidos à análise estatística.
RESULTADOS: A incidência de carcinoma basocelular encontrada foi de 126 casos/ 100.000 pacientes em 32 meses (36casos/100.000 pacientes/ano). Os pacientes se distribuíram de forma semelhante entre os sexos masculino (48%), e feminino (52%), com uma incidência maior na faixa etária entre 60 e 80 anos (69%), com média de 64,0 anos. A amostra apresentou fatores de susceptibilidade como a raça branca e fototipos I e II em 95,5% dos pacientes. A exposição à radiação ultravioleta foi informada por 77% dos pacientes, e a localização mais freqüente dos tumores foi a face, em 71,2% dos casos. A ceratose actínica e a história de câncer de pele anterior estavam presentes em 43,6% e 25,8%, respectivamente. O tratamento instituído foi o cirúrgico em 99,4% dos casos, sendo que um caso foi tratado com radioterapia por falta de condições clínicas. No anátomo-patológico foram encontradas 20 lesões (8%) com margens comprometidas pelo tumor. A taxa de recidiva no acompanhamento pós-operatório foi de 2% (5 casos). Não houve casos de metástase ou óbito.
CONCLUSÕES: Os fatores relacionados ao desenvolvimento do carcinoma basocelular que estão presentes de forma significante na população estudada são: idade avançada,raça branca, fototipos I e II, presença de ceratose actínica, história anterior de câncer de pele não-melanoma e exposição aos raios ultra-violetas tanto de forma recreacional quanto ocupacional.O tratamento instituído foi efetivo com taxas de margens comprometidas e recidivas comparáveis com as da literatura.
Descritores: Neoplasia de Células Basais. Neoplasias Cutâneas. Estudos Epidemiológicos. População Urbana.
Introduction
The incidence of skin cancer has been increasing in great proportions, especially in tropical countries.1 It was estimated that 2.75 million new cases of non- melanoma skin cancer (NMSC) are diagnosed every year all over the world 2. The American Skin Cancer Foundation estimates that one in every six Americans will develop this type of cancer in their lifetimes 3,4. In Brazil, the National Cancer Institute estimated that in 2003 the NMSC will continue to be the main type of cancer to affect the Brazilian population. In São Paulo city itself there is an annual incidence of 29.265 new cases of this type of cancer 5. NMSC are divided into two main histological types : the basal cell carcinoma (BCC) and squamous cell carcinoma (SCC). Considering all NMSC, 75% of them correspond to BCC whereas 20% are SCC 3,6. The incidence of BCC is very high all over the world, especially in regions close to the Equator 3,7 and in fair-skinned individuals with previous history of solar exposure6. The importance of NMSC as a public health problem has been underestimated mainly due to its good prognosis when detected and treated precociously, having a low mortality rate 8. It can, however, evolve with considerable morbidity and may be even fatal when well advanced. The purpose of this paper is to describe the epidemiological profile of the Basal Cell Carcinoma, identifying the factors related to the development of this condition and evaluate the treatment carried out in a service treating private patients in the city of São Paulo.
Methods
Between January 2001 and September 2003, 202 patients with 253 neoplasias diagnosed as basal cell carcinoma through histopathological exam were studied prospectively. The population under study was treated by the Plastic Surgery Residency Program medical team at the Hospital Jaraguá. This hospital is responsible for the health care of a population of 200,865 private patients.The age distribution of this group is shown in Table 1 on which 45.59% of these patients were males and 54.41% were females.
The epidemiological characteristics of this population were analyzed according to the individual susceptibility of the patient, environmental conditions and characteristics of the lesions. These data were collected by the author using a questionnaire.The types of treatment and their efficacy were also evaluated. Characteristics of the patient such as age, sex, race (white, black, mulatto, asian) and phototype according to Fitzpatrick´s classification9 were also analyzed. Factors of individual predisposition such as the presence of genetic syndromes related to a greater incidence of skin cancer, actinic keratosis, previous history of skin cancer, causal factors of the decreasing of immunity such as neoplasic illnesses, use of immunosuppressants and organ transplantation were also investigated. Environmental factors such as exposure to ultraviolet radiation and type of exposure (in working or leisure time), exposure to ionic radiation and to chemical agents were also analyzed. Patients were asked about their exposure to the sun and were classified as exposed and not exposed. The exposed patients were those with prolonged exposure to solar radiation as during outdoor work or those who had history of sunburns with frequency during outdoor activities on holidays, weekends and sports. Characteristics of the lesion and length of evolution from the time elapsed between its perception and the consultation with a doctor as well as the symptoms of the lesion were questioned. The macroscopy and the location were described by the junior author (R.L.B.). The tumor was measured with a ruler and its largest diameter was registered. Previous treatment such as surgery, radiotherapy, local chemotherapy and others were also investigated. Patients who presented lesions with difficult clinical diagnosis or lesions which could cause deformity if removed within the preconized margins were submitted to incisional biopsy, so that a histological evaluation could confirm the diagnosis. The other cases were submitted to resection of the tumor, followed by reconstruction. The surgical margins were defined according to size, macroscopy and location of the lesion. Lesions under 20 mm were excised with a 3mm margins if the tumor presented well-defined edges such as the nodular type or 5mm margins if the tumor had poorly defined edges such as the infiltrative and superficial types. In lesions larger than 20mm, the margin utilized was over 5mm. Primary suture was the first option, followed by graft or flap, depending on the surgeon´s indication. In patients with poor clinical condition, radiotherapy was indicated. Surgical procedures were carried out in the outpatient facility. Only patients who had clinical indication for monitoring and those who needed frozen biopsy were operated at the operating room in the hospital environment. Frozen biopsy was indicated in lesions on which resection involved a functional risk, also in cases of reoperation of incomplete excision and infiltrative lesions. All specimens were submitted to a histopathological exam and only those which were diagnosed as basal cell carcinoma were considered in this study. The efficacy of the treatment was evaluated according to the results of the margins in histopathological exams, depending on the presence of tumor in the skin edges. The incidence of recurrence was also investigated in the three-month and one-year follow up and, after that, the patient was seen every six months. Chi-squared test was used to verify the association between the qualitative variables and those of Mann-Whitney test, in order to check if there was a difference between the average of independent and continuous variables. Spearman correlation tests were also applied. The level of statistical significance used in the results was p<0.05. The software Statistica version 5.1 was used for all the analysis.
Results
Along the period of 32 months, 202 patients had 253 basal cell carcinoma among the 200.865 patients surveyed. Therefore, the incidence of this type of cancer in the population was approximately 126 cases for 100.000 patients in this period. Therefore,the annual incidence was 36 cases per 100.000 patients.
Host factors
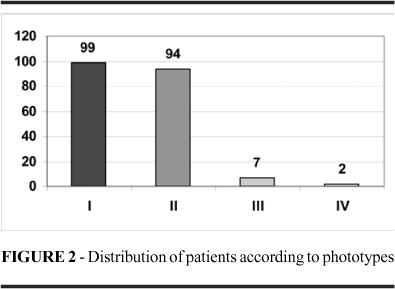
The distribution of the patients according to sex was similar, being 52% female and 48% male, with a greater incidence in the age range of 60 to 80 (59%) (Figure 1). The average age of the patients with BCC was 64.04, varying from 26 to 90 years old. The average age of the women was 65.4 and 62.5 for men. There was no statistically significant difference when the distribution of age was compared between the male and female groups (Table 2). One hundred and three patients were white (95.5%), seven (3.5%) were mullatos and only two were Asians (1%). The majority of the patients was classified as phototype I and II (95.5%) according to Fitzpatrick 's classification (Figure 2). Fifty two patients (25.8%) had a previous history of skin carcinoma. In the physical exam, 88 patients (43.6%) presented actinic keratosis, and 22 patients (10.9%) presented both: previous history of skin cancer and actinic keratosis. Seven patients had another malignant neoplasia, one patient had mielofibroplasia, and another had a previous kidney transplantation.
Environmental factors
A hundred and fifty six patients (77.2%) had a positive history of solar exposure (ultra violet radiation). Among these, 91 (58.3%) had had occupational exposure and 65 patients (41.7%) had had leisure exposure (Figure 3). There was no statistically significant difference when patient's sex was considered for solar exposure. (Table 3).
Characteristics of the BCC
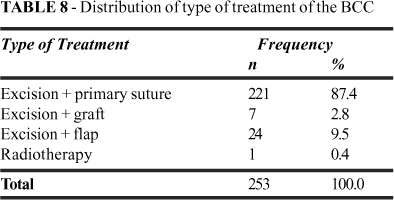
In the two hundred and two patients, 253 BCC were found. The great majority of the patients presented only one tumor (82.2%) (Table 4). Macroscopically the BCC were diagnosed as nodular in 118 tumors (47%) (Figure 4). The average of the largest diameter of the BCC was 9.54 mm, varying from 3 to 40 mm. The greater incidence ranged from 6 to 15 mm, representing 149 cases (58.9%) (Table 5). The average time elapsed between the initial growth of the lesion reported by the patient and the moment on which the patient searched for medical evaluation was 19.8 months, ranging from one to 120 months (Table 6). In most of the cases the tumors were located in the cephalic segment and the remaining ones were distributed according to Figure 5. The most frequent location of the tumors in the cephalic segment was the nose for both sexes (Table 7). The symptoms that prompted patients to look for a doctor were identified in 167 patients and are described in Figure 6. In 218 cases (86.2%), there had been no previous medical treatment. However, 17 cases (6.7%) had previously undergone surgery (recurrent BCC) and 18 cases (7.1%) had undergone another previous treatment, as shown on Figure 7. Incision biopsy was carried out in 16 (3%) of the cases. The chosen treatment was surgery in 99.6% of the cases, and only one case was treated with radiotherapy (0.4%) due to lack of clinical conditions (Table 8). The histopathological exam revealed 20 BCC (8%) incompletely excised. The excision was incomplete at the lateral margin in 40%, at the deep margin in 35% and at both in 25%. Among the patients with incomplete excision, eight cases were reoperated (40%) and the other 12 cases (60%) have either been scheduled for another surgery or gave up treatment. In one of the eight cases of reoperation no tumor evidence was found. In the other seven cases, the specimen revealed BCC with margins free of tumor. Most of the BCC with incomplete excision were located on the nose (65%) (Figure 8). The tumors that presented positive surgical excision margins varied between 3 and 10 mm. Seventeen of these cases (85%) were histologically diagnosed as nodular and as morphoeic in only three cases. The average time of evolution of the BCC in this group was 16.4 months. When this value was compared with the time of evolution of the BCC of the complete excision group, there was no statistically significant difference. The recurrence rate in the post-surgical follow up was 2% (5 cases).
It occurred between 2 and 22 months after the surgery. The place of recurrence was heterogeneously distributed, as shown in Figure 9. There were no cases of metastasis or death.
Discussion
Basal Cell Carcinoma is the most common type of skin cancer. It is the most common malignant tumor among white individuals10. In Brazil the incidence rate should be analyzed with caution since the national population database is not generally available. The treatment of BCC is carried out mainly in outpatient facilities or in private clinics, making the notification to the national cancer register more difficult11. The place with the highest incidence rate of non-melanoma skin cancer is Queensland, in Australia, with an incidence of de 2.389/100.000 men and 1.908/100.000 women 1. In Blumenau (a Brazilian city with a large population with German origin), between 1980 and 1990, the annual rate of CPNM was 330/100.000 inhabitants 12. In the population treated at Hospital Jaraguá (São Paulo), the annual incidence of BCC was 36/100.000 patients less than expected when compared to the values estimated for the year 2003 by the National Cancer Institute that was 196/100.000 inhabitants for Southeast region of Brazil5 (in the same region where the city of São Paulo is located). In the last few years, the interest on the study of the etiology, biology and treatment of non-melanoma skin cancer has been growing, mainly due to the world-wide increase of incidence of this illness, as well as due to the destruction of the ozone layer 7,13.
Host factors
According to the current literature the male sex is at greater risk of developing skin cancer 10,12,14,15,16. Men develop basal cell cancer two to three times more frequently than women. This may be explained by occupational exposure 16. Among younger people, the incidence of BCC is equivalent for men and women. After 45 years of age, the incidence is higher among men1. In this study, the basal cell cancer was distributed in a similar fashion among the sexes, displaying a slightly higher incidence among women (52%), with no difference in the age range. This is different from what was found in the literature. Two other studies carried out in Brazil, by Machado et al.11 and Bandeira et al.17, found a higher incidence of BCC among women, at the rate of 1.7:1 and 1.2:1, respectively. In Machado et al. 11, they justify the higher incidence among women by the fact that the female population corresponds to 63% of the studied population. In the population of the present study, 54.4% are female. These studies show a different characteristic of the incidence of BCC in the Brazilian population, demonstrating a higher incidence in women as compared to other world series. Old age is a well-known risk factor 15,18. In the patients studied here the higher incidence was between 60 and 80 years of age, corresponding to 59 % of the cases. Elderly individuals have a less efficient immune system and have a diminished DNA repair capacity what increases the risk of developing NMSC 18. The incidence of non-melanoma skin cancer depends on individual susceptibility. This susceptibility is related to the amount of melanin in the skin and to the capacity of the skin to tan when exposed to ultraviolet radiation. In order to evaluate the susceptibility of the samples used in this study, patients were classified based on their skin color, employing the Fitzpatrick system of phototype. This system classifies individual skin type according to the skin reaction to solar exposure 9. The population under survey was susceptible to BCC, as it was constituted by phototype I patients in 99 cases and type II in 94 cases. These two groups corresponded to 95.5% of the cases. Nine patients (4.5%) were photoype III and IV, who correspond in these study to mullatoes and asians. None of them was black. These data are similar to those found in the literature, which show a greater incidence in the white race14. None of the patients had any genetic syndrome, such as Xeroderma pigmentosum, Albinism and Nevoid Basall cell carcinoma syndrome, which present a higher risk of incidence of BCC. Though there are no pre-malignant skin lesions identified for BCC , the presence of actinic keratosis in the clinical exam is an indicator that the individual has been exposed to a significant quantity of ultraviolet B rays 3,19. This condition is also useful to identify individuals with a high risk of developing specially squamous cell carcinoma, and less frequently, BCC20. In a histopathological exam revision study of actinic keratosis (AK), BCC was identified in 4%, what reflects a similar pathogenesis between AK and BCC 19. In the present study, 88 patients (43.6%) presented actinic keratosis in the physical exam, showing skin damage caused by the sun, thus corroborating the notion that AK is a marker for increased skin cancer risk. Fifty two patients (25.8%) had a previous history of NMSC, thus demonstrating a higher risk of BCC 10,20 since the risk of developing NMSC 5 years after the diagnosis of the first one ranges between 36 and 52% 3. Conditions that lead to decrease of immunity are another factor that predisposes the incidence of BCC. The decreased mechanism of immunologic vigilance may fail to destroy potentially malignant cells1. This condition was identified in 4.5% of the patients, where seven presented another type of cancer and two were using immunosuppressant drugs (one due to mielofibroplasia and another to a kidney transplant). The risk in the use of such drugs is due to the possible potencialization of the carcinogenic effect of ultraviolet rays1.
Environmental factors
There is ample evidence that once the genetic susceptibility is excluded, the exposition to ultraviolet rays is the most important risk factor in the development of NMSC 6,10,14,21. Besides UVA and UVB rays, which have already been proved to be carcinogenic factors, the UVC, filtered by the ozone layer has a great oncogenic capacity. The ozone layer is being destroyed every day. Mathematical models have estimated an increase of 2 to 4% of incidence of skin cancer for each 1% in the reduction of the ozone layer13. The relationship of skin cancer and solar radiation has been investigated and the data showed that not only the accumulated quantity, as it was formerly believed, but also the way and the period of exposure increase the risk of basal cell cancer 21,22. In most cases, the solar exposure accumulated in life has a clearer effect in the occurrence of squamous cell carcinoma than in the occurrence of BCC. On the other hand, intermittent exposure, generally recreational, seems to be more relevant for BCC 21. This difference may be explained by the type of exposition in certain times of the year, generally at weekends or during yearly vacation weeks, in which cases individuals do not have the opportunity to develop natural skin protection. However, in individuals with continuous occupational exposition, there is time for the skin to develop its natural protection 21. In the samples surveyed, 77.2% of the patients mentioned that they had had intense solar exposure throughout their lives. Both occupational (58.3%), and recreational (41.7%) exposure were proven to be relevant for the development of BCC. One of the indicators of the relation between an intermittent pattern of exposure and the development of BCC, is the increase in the incidence of BCC on the trunk in the last decade 6.This pattern of incidence on the trunk was not evident in the present study, where only 6% of the BCC were located on the trunk. Once the hazards of other environmental factors such as exposure to ionic radiation and to chemicals, either in occupational or therapeutic forms, are well known, there has been a decrease in their influence in the development of CPNM due to the decrease in the number of people exposed 1. None of the patients on the present study were exposed to ionic radiation or to chemicals.
Characteristics of the BCC
The majority of the patients presented a single BCC (82.2%), and the highest number of BCC per patient was 5, in 0.5% of the patients. These numbers reveal an average of 1.25 lesions per individual, a low rate when compared to the relation of 1.4 15 and 1.7 16found in the literature. Patients who have private medical care have an easier access to medical consultations and this may explain the small dimension of the BCC, most of them were in the range of 6 to 15 mm (58.9%), only 10.7% were larger than 15 mm, and the largest BCC was 40mm. However, the average time between the growth of the BCC and the moment on which the patient looked for medical assistance was 19.8 months, varying between 1 and 120 months. This elapsed time may be explained because the symptoms of these tumors are few. Also, BCC present slow growth, taking one year and longer to duplicate its size. The period of 19.8 months to look for medical help was shown to be shorter when compared to data of public medical care in Brazil, on which the average elapsed time is 48 months15. One hundred and sixty seven (82.7%) patients had symptoms and the most frequent ones were growth, itching, bleeding and ulcerations. This confirms the data found by Machado et al 11. It is not easy to define the clinical types of BCC using the macroscopic aspect of the BCC. The accuracy rate is, on average, of 60 to 70% 22. The macroscopy of the BCC was divided in accordance with the histological classification found in the literature. The nodular pattern was present in 47%, superficial in 19%, infiltrative in 9%, ulcerated in 20% and pigmented in 9%. Those data confirm the distribution of the histological type found in the literature 23. The site of occurrence of BCC with the greater incidence was at the head and neck (85%). This value is similar to those found in the literature that ranges between 73.2 and 85% 6,10,11,14,15,21,24. The incidence of BCC in the trunk corresponded to 6%, thus going against the tendency in the last decade when there has been an increase of the incidence of lesions in that area. Castro et al 16 verified that 40.1% of the BCC occurred in the trunk while 39.7% were in the cephalic segment. Irebarren et al 25 also verified a high incidence of BCC in the trunk (33.5%). The low incidence of BCC in this area may be explained because most of these patients live in the city of São Paulo and usually work with the trunk covered. Biopsy is the best method for the diagnosis of BCC, even though the majority of these tumors presents a typical history and can be recognized through macroscopy 3. This is the reason why only cases with a histological diagnosis were included in this study. Incisional biopsy is well indicated for larger tumors whereas excisional biopsy is the treatment of choice for smaller lesions3. In the cases in which the excisional biopsy using the recommended margins would cause local deformity, the incisional biopsy was made to confirm the diagnosis. The treatment of choice was surgical excision, which was used in 99.4% of the cases. It is the most common intervention made by surgeons 10. According to the literature, the cure rate is 95%, getting close to 99% when the histopathological margins are negative4. Radiotherapy was used only in one case (0.6%) due to the patient's advanced age and lack of adequate clinical conditions for surgery. The indication of radiotherapy is reserved for selected cases because it does not allow access to histology and control of the margins of the tumor, and it may also cause dermatitis 26. The purpose of the treatment is the eradication of the BCC with a satisfactory cosmetic result. This is why to determine the exact margin excision is so important 10. In most cases it is the surgeon who determines the adequate excision margin 4,27. However, it is important to consider the tumor size, the histological type, the anatomic location and the presence of recurrence for a better planning of the area of excision 26. The margin macroscopically free of tumor recommended for the resection of a BCC varies greatly, from 2 to 10 mm, according to the literature 27. For tumors smaller than 2 cm, the margin varies between 2 to 5 mm 26, with a preference for the margin of 4mm 4. Thus, in this study, the margin was planned according to the dimension of the lesion. Rippey et al 23 consider margins smaller than 0.38mm as a risk factor for recurrence. Kumar et al 27 reported 4.7% of incomplete excision using margins of 1 to 2.5mm, 4.1% with margins of 3 to 4 mm and 2.9% with margins of 5 or more mm . The incidence of incomplete excision in the present study was 8%, corresponding to 20 patients. This result is similar to some of the data found in the literature which vary from 0.7% in Australia 28, from 4.1% to 13.7% in England 27, 4.2% in Portugal 29, and 15.4% in Brazil 15. Kumar et al.26 reported a recurrence rate when the tumor is completely excised of 1% in 3 years, whereas on average 31% of the tumors with incomplete excision recurred from 6 to 33 months 27. When reexcision is performed, this rate drops to 12% 26. There is a smaller chance of recurrence when tumor remains at the lateral margin after the BCC removal, when compared to the deep margin or when both are affected 30. In the present study the affected margins presented a similar distribution, being 40% on the lateral margin, 35% on the deep one, and 25% on both, what differs from the literature that shows a greater compromise of the lateral margin 25. The predominant histological type of the cases with incomplete excision was nodular (85%) and only 15% was diagnosed as morphoeic, whereas the literature search showed a greater incidence of incomplete excision in infiltrative tumors and morphoeic type30. Considering the 20 cases that were incompletely excised, thirteen cases (65%) of the lesions were located on the nose. This high rate may be explained because of the high incidence of BCC in this region (75.7%). Also, patients who had BCC previously removed may have a higher risk of recurrence. In this study there were 17 cases (6.7%) previously operated, and though it was expected a more aggressive behavior, these individuals were free of tumor as demonstrated by the histological exam and presented no recurrence in the follow-up. The treatment of incomplete excised tumors is still a controversial matter. There are many studies that support observation and follow up and others that recommend the reexcision 28. Even though re-operation was recommended to all the patients (20) who presented incomplete excision, only eight of them undertook the surgery and in only one case there was no residual tumor. The remaining 12 patients were scheduled for surgery; and eight of them did not come back for follow up, even though they were fully informed of the risk of recurrence and dissemination. In the cases of histologically proved complete excision of the tumor, there was recurrence in 5 patients (2%), in the period between 2 and 22 months after the surgery. This value was similar to the data found in the literature (1%) 27. Both cases with incomplete excision and the recurrence cases were re-operated using frozen sections of the margins in the intra-operatory, aiming at the complete resection of the tumor. In all cases the specimen margin was free of tumor. Metastasis in BCC is rare and the incidence varies between 0.00285 and 0.1% 26. No case of metastasis or death occurred in the patients surveyed in the present study. Prevention is an important weapon against this tumor. The cost of screening of the whole population is very high. Prevention by early detection could be done by identifying individuals that present the risky characteristics observed in this study. Therefore, the screening of the high risk population would decrease the cost. These patients should also be informed about their risky situation and carry out a professional follow-up throughout their lives.
Conclusions
The factors related to the development of basal cell cancer which were significantly present in the population surveyed are: older age, white individuals, phototypes I and II, presence of actinic keratosis, previous history of non-melanoma skin cancer and exposure to ultra-violet rays both in recreational and in occupational form. A similar incidence between the genders suggests a specific pattern of the São Paulo city population. Most of the BCC were nodular, preferably located on the nose, with an average size of 9,54 mm, with an average time of evolution of 19,8 months. The surgical treatment employed was effective with a rate of incomplete excision and recurrence similar to those found in the literature.
Received: October 02, 2005
Review: November 10, 2005
Accepted: December 18, 2005
Conflict of interest: none
Financial source
How to cite this article: Bariani RL, Nahas FX, Barbosa MVJ, Farah AB, Ferreira LM. Basal cell carcinoma: an updated epidemiological and therapeutically profile of an urban population. Acta Cir Bras. [serial on the Internet] 2006 Mar-Apr;21(2). Available from URL: http://www.scielo.br/acb
- 1. Strom SS, Yamamura Y. Epidemiology of nonmelanoma skin câncer. Clin Plast Surg. 1997 ; 24(4): 627-36.
- 2. Armstrong BK, Kricker A. Skin cancer. Dermatoepidemiology. 1995; 13: 583.
- 3. Gloster HM, Brodland DG. The epidemiology of skin cancer. Dermatol Surg. 1996; 22: 217-26.
- 4. Garner KL, Rodney WM. Basal and squamous cell carcinoma. Clin Plast Surg. 1997 ; 24(4): 447-58.
-
5Cancer incidence and mortality in Brazil-2003. Available from www.inca.gov.br
- 6. Zanetti R, Rosso S, Martinez C, Navarro C, Schraub S, Sancho-Garnier H, Franceschi S, Gafa L, Perea E, Tormo MJ, Laurent R, Schrameck C, Cristofolini M, Tumino R, Wechsler J. The multicentre south European study Helios I: skin characteristics and sunburns in basal cell and squamous cell carcinomas of the skin. Br J Cancer. 1996; 73: 1440-6.
- 7. Raasch B, Maclennan R, Wronski I, Robertson I. Body site specific incidence of basal and squamous cell carcinoma in an exposed population, Townsville, Australia. Mutation Res. 1998; 422: 101-6.
- 8. Kaldor J, Shugg D, Young B, Dwyer T, Wang YG. Non-melanoma skin cancer: ten years of cancer-registry-based surveillance. Int J Cancer. 1993; 53: 886-91.
- 9. Fitzpatrick TB, Sober AJ. Sunlight and skin cancer. N Engl J Med.1985; 313: 818.
- 10. Lear JT, Smith AG. Basal cell carcinoma. Postgrad Med J. 1997; 73: 538-42.
- 11. Machado CDS, Fagundes DS, Sender F, Saraiva GL, Paschoal LHC, Costa MCC, Cunha RMES, Carazzato SG. Neoplasias malignas cutâneas: estudo epidemiológico. An Bras Dermatol. 1996 ; 71(6): 479-84.
- 12. Nasser N. Incidência de câncer de pele em Blumenau/ SC - 1980-1990. An Bras Dermatol. 1993; 68(3): 77-8.
- 13. Diffey BL. Stratospheric ozone depletion and the risk of non-melanoma skin câncer in a British population. Phys Med Biol. 1992; 37(12): 2267-79.
- 14. Wennberg AM. Basal cell carcinoma: new aspects of diagnosis and treatment. Acta Derm Venereol. 2000;(Suppl 209): 5-25.
- 15. Magliavacca A, Guimarães JR, Melo LL, Vecino MCA, Araújo HM. Carcinoma basocelular: revisão de 381 casos no Hospital de Clínicas de Porto Alegre. Rev HCPA. 1990; 10(2): 95-8.
- 16. Castro LGM, Toyama CL, Gomes AP, Freire MA, Britto TF. Câncer de pele em clínica particular em São Paulo SP. An Dermatol. 1996 ; 71(6): 471-6.
- 17. Bandeira AM, Bandeira V, Silva JF, Mazza E. Carcinomas basocelulares: estudo clínico e anatomopatológico de 704 tumores. An Bras Dermatol. 2003 ; 78(1): 23-34.
- 18. Wei Q, Matanoski GM, Farmer ER, Hedayati MA, Grossman L. DNA repair and aging in basal cell carcinoma: A molecular epidemiology study. Proc Natl Acad Sci USA. 1993 ; 90: 1614-8.
- 19. Carag HR, Prieto VG, Yballe LS, Shea CR. Demonstration of additional pathological findings in biopsy samples initially diagnosed as actinic keratosis. Arch Dermatol. 2000 ; 136: 471-5.
- 20. Schwartz RA. The actinic keratosis: a perspective and update. Dermatol Surg. 1997; 23: 1009-19.
- 21. Rosso S, Zanetti R, Martinez C, Tormo MJ, Schraub S, Sancho-Garnier H, Franceschi S, Gafa L, Perea E, Navarro C, Laurent R, Schrameck C, Talamini R, Tumino R, Wechsler J. The multicentre south European study Helios II: different sun exposure patterns in the aetiology of basal cell carcinomas of the skin. Br J Cancer. 1996; 73: 1447-54.
- 22. Kricker A, Armstrong BK, English DR, Heenan PJ. Does intermittent sun exposure cause basal cell carcinoma? A case-control study in Western Australia. Int J Cancer. 1995; 60: 489-94.
- 23. Rippey JJ. Why classify basal cell carcinomas? Histopathology.1998; 32: 393-8.
- 24. Levi F, Vecchia C, Te VC, Mezzanotte G. Descriptive epidemiology of skin cancer in the Swiss Canton of Vaud. Int J Cancer. 1988; 42: 811-6.
- 25. Iribarren O, San Martin J, Alcazar A, Larenas E, Fischer J, Gallegos E.Carcinoma basocelular: epidemiologia y factores de riesgo. Rev Chil Cir. 1995 ; 47(2): 123-7.
- 26. Goldberg DP. Assessment and surgical treatment of basal cell skin cancer. Clin Plast Surg. 1997; 24(4): 673-86.
- 27. Kumar P, Watson S, Brain NA, Davenport PJ, McWilliam LJ, Banerjee SS. Incomplete excision of basal cell carcinoma: a prospective multicentre audit. Br J Plast Surg. 2002; 55: 616-22.
- 28. Emmett AJJ, Bradbent GG. Basall cell carcinoma in Queensland. Aust N Z J Surg. 1981; 51: 576-90.
- 29. Ferreira PJS, Correia PM. Basaliomas incompletamente excisados: significado prognóstico a curto prazo. An Bras Dermatol. 1998; 73(1): 7-10.
- 30. Grabski WJ, Salasche SJ. Positive surgical excision margins of a basal cell carcinoma. Dermatol Surg. 1998; 24: 921-4.
Publication Dates
-
Publication in this collection
21 Mar 2006 -
Date of issue
Apr 2006
History
-
Received
02 Oct 2005 -
Reviewed
10 Nov 2005 -
Accepted
18 Dec 2005