Abstracts
PURPOSE: To investigate the function of the bronchial mucociliary system in transplanted rat lungs with and without the influence of immunosuppression. METHODS: Thirty-six rats underwent single-lung transplantation and were divided into two groups, one of which received cyclosporine treatment, and the control group which did not. Cyclosporine was administered subcutaneously in doses of 10 mg/kg daily. The rats were sacrificed 2, 15 or 30 days after transplantation. In situ bronchial mucociliary transport (MCT) and ciliary beat frequency (CBF) were determined proximal and distal to the bronchial anastomosis. RESULTS: Significant progressive improvement on MCT, proximal and distal to the anastomotic site, was also found in the cyclosporine-treated group at 15 and 30 days (p<0.01). No significant change in MCT was found in the control group. CBF behavior in the two groups. Histological analysis showed that rejection was significantly higher in the control group (p<0.05). CONCLUSION: Cyclosporine has a positive influence on bronchial mucociliary transport but not on CBF due to the effect of the rejection mechanism.
Lung Transplantation; Cyclosporine; Immunosuppression; Mucociliary Clearance; Rats
OBJETIVO: Investigar a função do sistema mucociliar em ratos transplantados sob a influência de imunossupressores. MÉTODOS: Trinta e seis ratos foram submetidos ao transplante pulmonar unilateral e divididos em dois grupos, onde um grupo foi tratado com ciclosporina e outro foi controle. Administrada ciclosporina por via subcutânea na dose de 10 mg/kg diariamente. Os ratos foram sacrificados 2, 15 e 30 dias após o transplante pulmonar. O transporte mucociliar brônquico (TMC) in situ e a freqüência de batimento ciliar (FBC) foram analisados na porção proximal e distal à anastomose brônquica. Realizada correlação dos achados com parâmetros gasométricos e histologia. RESULTADOS: Foi encontrada melhora progressiva e significante no TMC na região proximal e distal a anastomose no grupo que recebeu ciclosporina em 15 e 30 dias (p<0,01). Não houve diferença na FBC nos dois grupos estudados. A análise histológica mostrou que a rejeição foi significantemente maior no grupo controle (p<0,05). A oxigenação foi melhor nos animais que receberam a ciclosporina. CONCLUSÃO: A ciclosporina exerceu influência positiva no transporte mucociliar brônquico, provavelmente por sua ação imunossupressora.
Transplante de Pulmão; Ciclosporina; Imunossupressão; Depuração Mucociliar; Ratos
ORIGINAL ARTICLE
TRANSPLANTATION
Influence of cyclosporine A on mucociliary system after lung transplantation in rats1 1 . Research performed at the Laboratory of Thoracic Surgery Research (LIM 61), University of São Paulo, Medical School, Post Graduate Program in Thoracic and Cardiovascular Surgery, Heart Institute (InCor), Clinics Hospital, São Paulo, Brazil.
Influência da ciclosporina A sobre o sistema mucociliar após-transplante pulmonar em ratos
Alexandre Martins XavierI; Paulo Manuel Pêgo-FernandesII; Aristides Tadeu CorreiaIII; Rogerio PazettiIV; Rosangela MonteiroV; Mauro CanzianVI; Fabio Biscegli JateneVII
IPhD, Staff Surgeon, Thoracic Surgery Division, Department of Surgery, Federal University of São Paulo (UNIFESP), Brazil
IIAssociate Professor, Thoracic Surgery Division, Department of Cardiopneumology, University of São Paulo, Medical School, Brazil
IIIBiologist, Thoracic Surgery Division, Department of Cardiopneumology, InCor, Clinics Hospital, University of São Paulo, Medical School, Brazil
IVPhD, Biologist, Laboratory of Thoracic Surgery Research, University of São Paulo, Medical School, Brazil
VPhD, Chief Biologist, Thoracic Surgery Division, Department of Cardiopneumology, InCor, Clinics Hospital, University of São Paulo, Medical School, Brazil
VIPhD, Staff Physician, Pathology Laboratory, InCor, Clinics Hospital, University of São Paulo, Medical School, Brazil
VIIFull Professor, Thoracic Surgery Division, Department of Cardiopneumology, University of São Paulo, Medical School, Brazil
Correspondence Correspondence: Paulo Manuel Pêgo-Fernandes Av. Dr. Enéas de Carvalho Aguiar, 44 / Bloco 2, Sala 9 05403-900 São Paulo SP Brazil Phone: (55 11)3069-5248 paulopego@incor.usp.br
ABSTRACT
PURPOSE: To investigate the function of the bronchial mucociliary system in transplanted rat lungs with and without the influence of immunosuppression.
METHODS: Thirty-six rats underwent single-lung transplantation and were divided into two groups, one of which received cyclosporine treatment, and the control group which did not. Cyclosporine was administered subcutaneously in doses of 10 mg/kg daily. The rats were sacrificed 2, 15 or 30 days after transplantation. In situ bronchial mucociliary transport (MCT) and ciliary beat frequency (CBF) were determined proximal and distal to the bronchial anastomosis.
RESULTS: Significant progressive improvement on MCT, proximal and distal to the anastomotic site, was also found in the cyclosporine-treated group at 15 and 30 days (p<0.01). No significant change in MCT was found in the control group. CBF behavior in the two groups. Histological analysis showed that rejection was significantly higher in the control group (p<0.05).
CONCLUSION: Cyclosporine has a positive influence on bronchial mucociliary transport but not on CBF due to the effect of the rejection mechanism.
Key words: Lung Transplantation. Cyclosporine. Immunosuppression. Mucociliary Clearance. Rats.
RESUMO
OBJETIVO: Investigar a função do sistema mucociliar em ratos transplantados sob a influência de imunossupressores.
MÉTODOS: Trinta e seis ratos foram submetidos ao transplante pulmonar unilateral e divididos em dois grupos, onde um grupo foi tratado com ciclosporina e outro foi controle. Administrada ciclosporina por via subcutânea na dose de 10 mg/kg diariamente. Os ratos foram sacrificados 2, 15 e 30 dias após o transplante pulmonar. O transporte mucociliar brônquico (TMC) in situ e a freqüência de batimento ciliar (FBC) foram analisados na porção proximal e distal à anastomose brônquica. Realizada correlação dos achados com parâmetros gasométricos e histologia.
RESULTADOS: Foi encontrada melhora progressiva e significante no TMC na região proximal e distal a anastomose no grupo que recebeu ciclosporina em 15 e 30 dias (p<0,01). Não houve diferença na FBC nos dois grupos estudados. A análise histológica mostrou que a rejeição foi significantemente maior no grupo controle (p<0,05). A oxigenação foi melhor nos animais que receberam a ciclosporina.
CONCLUSÃO: A ciclosporina exerceu influência positiva no transporte mucociliar brônquico, provavelmente por sua ação imunossupressora.
Descritores: Transplante de Pulmão. Ciclosporina. Imunossupressão. Depuração Mucociliar. Ratos.
Introduction
As of the mid 1980s, lung transplantation became an established and accepted treatment for patients with advanced pulmonary disease1-4. As a consequence of the advances in the transplantation field, we have increasingly been faced with a population of patients who present complications related to the surgical procedure 5, 6, opportunistic infections, 7, 8 and immunosuppression 9, thus generating a greater need to understand the post-transplantation immunological and clinical aspects. Alterations in the mucociliary clearance can be a predisposing factor for bacterial colonization and, consequently, for the development of pulmonary infection 10. The decrease of post-pulmonary transplantation bronchial clearance may be due to ciliary dysfunction 11, and to the quantity and/or qualitative alteration of the mucus. These factors can be related to non-specific bronchial alterations, due to bronchial denervation and devascularization, or to infection and rejection episodes. Another cause could be the use of immunosuppressive medication used on transplanted patients. However, only the drug-induced immunosuppression effect does not explain the significant prevalence of pulmonary infections, when compared with the transplantation of other organs which suffer comparable 12 immunosuppression. To the present, there has been no report in the literature on the effect of cyclosporine or azathioprine on the mucociliary system. The better understanding of the alterations in the mucociliary clearance can lead to solutions which aim at reducing the high levels of pulmonary infections in lung transplant recipients. As of this conclusion, the decision was made to investigate the immunosuppression effect on the mucociliary system in an experimental model of rat lung transplantation.
Methods
An experimental study was carried out in a model of orthotopic left lung transplantations in rats, with vascular anastomosis by utilizing a cuff technique, according to Mizuta 13. Fischer rats were used in 36 single orthotopic left lung transplantations. The transplantations were divided into 2 groups; one of which was administered cyclosporine, which was called the treated group and one of which cyclosporine was not administered, the control group. Each group had 18 rats, divided into three subgroups with 6 rats each. This subdivision was according to the date of sacrifice, which was established at 2, 15, and 30 days. The animals of the control group received daily placebo doses of 100 ml of saline solution subcutaneously. The animals of the treated group received doses of 10 mg/kg/day of Cyclosporin A (Sandimmun, 50 mg/ml, Novartis), until the date of sacrifice.
Determining in situ mucociliary transport velocity
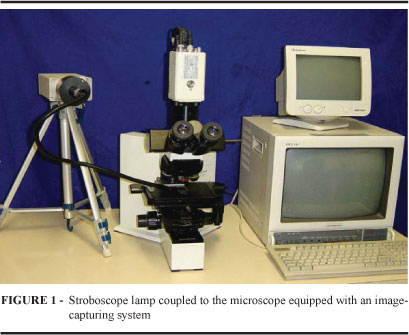
Mucociliary transport velocity was measured with the help of an Olympus BX50 microscope, equipped with reticulated eyepiece, magnification x10. A homogenized solution was formed with the use of talc particles mixed with India ink. This solution was inserted in the internal wall of the bronchus for direct observation 14, 15,16. The reticle in the x100 magnification measures a distance of 1mm. The progression of this solution on the bronchial epithelium was timed and reported as velocity, that is, the distance the solution traveled in the reticle, in millimeters, by the time space, in minutes (mm/min). The analysis of the sites of preanastomotic and post-anastomotic bronchial segments was carried out (Figure 1).
Determining ciliary beat frequency
By using a video camera (Sony, mod. 3CCD Iris), coupled to the microscope, the image of the bronchial ciliary epithelial was captured and sent to a monitor (Sony Trinitron). A stroboscope (Machine Vision Strobe, mod.5000, U.S.A.) was placed in front of the ciliary epithelial, and started to emit flashes at a specific frequency which was expressed numerically by a computer coupled to the stroboscope. Thus, it was possible to determine the ciliary beat frequency by observing the ciliary epithelial beating at the same frequency as the stroboscope lamp (Figure 1). The ciliary beat was studied before bronchial anastomosis, named preanastomosis and after bronchial anastomosis, or post-anastomosis. The preanastomotic segment evaluates the native bronchus, that is, that of the recipient animal, and the post-anastomotic segment evaluates the transplanted bronchus, or that of the donor.
Histology
The lungs were preserved in 10% formaldehyde and submitted to sagittal section. The slides were stained in hematoxylin and eosin for optical microscopy analysis to detect the presence of rejection and infection. The material was labeled in such a way that the pathologist didnt know the identification of the studied groups. The classification of rejection described in 1996 by the Lung Rejection Study Group was used17.
Results
Thirty-three samples were analyzed obtained with the model of single left lung transplantation of a total of 36 transplants, 17 of which of the control group and 16 of the treated group. Three animals were excluded due to the technical impossibility of carrying out beat frequency and/or mucociliary transport analyses, two of which were from the treated group (2 and 15 days) and one rat from the control group (2 days). The macroscopic examination of all the bronchial anastomoses at the moment of sacrifice revealed there was no obstruction or dehiscence. In addition, no alteration on the mucus or bronchial secretion was observed. There was no statistical difference in the comparisons carried out between the two groups when the weight of the animals and the total time of ischemia of the lung transplantation were analyzed.In Situ ciliary beat frequency showed at moments, a clear difference in the comparisons carried out between the pre and post-bronchial anastomotic sites (Figure 2), however, with no correlation with the use of cyclosporine (p > 0.05).In the mucociliary velocity measurements, the velocity was less when comparing the pre and post-anastomotic sites in two days (p < 0.01) and 15 days (p < 0.001); however, with no statistical difference when comparing with the use of cyclosporine. There was significant statistical difference in the 30-day group when comparing the treated group with the control group (p < 0.01) in the post-anastomotic site (Figure 3). The histological analysis of the stained slides by using the hematoxylin and eosin technique certified there was no statistical difference between the animals in the control and treated groups in a 2-day period, in relation to the classification of rejection (Table 1). In the 15-day group, there was a greater degree of rejection in the animals of the control group, where p = 0.048 (83% of the animals obtained grades 3 or 4 rejection), similar to what was found in the 30-day group where p = 0.015 (83% of the animals of the control group, presented grade 3 rejection). Evidence of infection was found in two animals, one of which from the 15-day (control) group and the other from the 30-day (treated) group.
Discussion
Cyclosporine has been used in several studies related to organ transplantation since its introduction in clinical practice. Pinsker et al. 18 studied bronchial anastomoses in dogs which were transplanted and treated with cyclosporine. The authors concluded that cyclosporine does not interfere in bronchial anastomosis and suggested that the use of cyclosporine reduced the number and the seriousness of the anastomotic complications of the transplanted animals. This occurred due to the prevention or the reduction of rejection present, especially during the initial phase of the transplant. Several studies were carried out to analyze mucociliary clearance with quite varied methodologies and different results. In this study, by means of an experimental model of rat lung transplantation, we sought to create conditions which were most similar to clinical situations and decided to analyze the influence of two factors described in the literature as co-responsible for pulmonary infection after lung transplantation, as of post-operative complications. The first factor studied was bronchial denervation, in the study carried out by Rivero et al.14 significantly different values were found when comparing the post-anastomotic bronchial site with the control bronchial site (not operated), in that there was decrease in post-anastomotic mucociliary transport velocity. The main factor in this study was bronchial denervation since neither the influence of drugs nor the presence of rejection was analyzed, because it was not a transplantation model. Many papers ascribe to immunosuppression an important cause of predisposition to lung infection 11, 19, 20, however, no study, until today, has analyzed this aspect. We have observed that in the model of lung transplantation, there is clear evidence that bronchial denervation is, in itself, a factor responsible for the decrease of mucociliary transport velocity, thus confirming what was described by Rivero et al 14. This observation is well described in Figure 3, where on the second post-transplantation day, only the denervation effect is found since both rejection and infection are not manifested at that point. Even when we compare the use of cyclosporine, this group presents similar results, that is, the drug causes no influence at that specific moment. On analyzing mucociliary transport velocity after 15 days, a slight recovery tendency was observed in the treated group; however, it did not reach statistical significance. The animals sacrificed after 30 days showed the most effective mucociliary transport velocity in the post-anastomotic site in the treated group (p < 0.01). Upon analyzing the preanastomotic site of the two groups, a better performance in the animals in the treated group (p < 0.01) when compared with the control group was reported. This finding has shown that cyclosporine did not exert influence solely on the donor region, but also on the preanastomotic site of the recipient animal. The histological analysis of the transplanted lung described in this study, has shown that in both animals sacrificed after 15 days and those sacrificed after 30 days, there was greater rejection in the group which did not receive cyclosporine (p < 0.05), thus suggesting that the drug improved mucociliary clearance, probably due to its immunosuppressive action and not due to direct action on the bronchial epithelium. Therefore, probably, due to this reason, there was improvement even in the mucociliary transport velocity in the preanastomotic site. This finding leads us to believe that immunosuppression contributes in a broader way and not only in the donor area, thus reducing the predisposition to lung infections because it improves mucociliary clearance through the control of rejection. Only two animals presented histological characteristics of infection, one of which was a rat from the control group after 15 days, and the other from the treated group after 30 days.
Conclusion
There was positive influence from cyclosporine, improving in situ mucociliary transport velocity after 30 days and less evidence of rejection in the animals which received cyclosporine, after 15 and 30 days.
Received: April 12, 2007
Review: June 14, 2007
Accepted: July 18, 2007
Conflict of interest: none
Financial source: FAPESP
- 1. Toronto Group LT. Unilateral lung transplantation for pulmonary fibrosis. N Engl J Med. 1986;314(18):1140-5.
- 2. Cooper JD. Lung transplantation for chronic obstructive lung disease. Ann N Y Acad Sci. 1991;624:209-11.
- 3. de Hoyos AL, Patterson GA, Maurer JR, Ramirez JC, Miller JD, Winton TL. Pulmonary transplantation. Early and late results: The Toronto lung transplant group. J Thorac Cardiovasc Surg. 1992;103(2):295-306.
- 4. Trulock EP. Lung transplantation. Am J Respir Crit Care Med. 1997;155(3):789-818.
- 5. Cochrane LJ, Mitchell ME, Raju S, Mansel JK. Tension pneumopericardium as a complication of single-lung transplantation. Ann Thorac Surg. 1990;50(5):808-10.
- 6. Maziak DE, Maurer JR, Kesten S. Diaphragmatic paralysis: a complication of lung transplantation. Ann Thorac Surg. 1996;61(1):170-3.
- 7. Kubak BM. Fungal infection in lung transplantation. Transpl Infect Dis. 2002; 4(Suppl 3):24-31.
- 8. Holt ND, Gould FK, Taylor CE, Harwood JF, Freeman R, Healy MD, et al. Incidence and significance of noncytomegalovirus viral respiratory infection after adult lung transplantation. J Heart Lung Transplant. 1997;16(4):416-9.
- 9. Fisher AJ, Wardle J, Dark JH, Corris PA. Non-immune acute graft injury after lung transplantation and the risk of subsequent bronchiolitis obliterans syndrome (BOS). J Heart Lung Transplant. 2002;21(11):1206-12.
- 10. Johanson WG Jr., Pierce AK, Sanford JP, Thomas GD. Nosocomial respiratory infections with gram-negative bacilli. The significance of colonization of the respiratory tract. Ann Intern Med. 1972; 77(5):701-6.
- 11. Read RC, Shankar S, Rutman A, Feldman C, Yacoub M, Cole PJ, et al. Ciliary beat frequency and structure of recipient and donor epithelia following lung transplantation. Eur Respir J. 1991;4(7):796-801.
- 12. Brooks RG, Hofflin JM, Jamieson SW, Stinson EB, Remington JS. Infectious complications in heart-lung transplant recipients. Am J Med. 1985;79(4):412-22.
- 13. Mizuta T, Kawaguchi A, Nakahara K, Kawashima Y. Simplified rat lung transplantation using a cuff technique. J Thorac Cardiovasc Surg. 1989; 97(4):578-81.
- 14. Rivero DH, Lorenzi-Filho G, Pazetti R, Jatene FB, Saldiva PH. Effects of bronchial transection and reanastomosis on mucociliary system. Chest. 2001;119(5):1510-5.
- 15. Macchione M, Guimaraes ET, Saldiva PH, Lorenzi-Filho G. Methods for studying respiratory mucus and mucus clearance. Braz J Med Biol Res. 1995;28(11-12):1347-55.
- 16. Pazetti R, Pęgo-Fernandes PM, Ranzani OT, Parra ER, Lorenzi-Filho G, Jatene FB. Cyclosporin A reduces airway mucus secretion and mucociliary clearance in rats. Clinics. 2007;62(3):345-52.
- 17. Yousem SA, Berry GJ, Cagle PT, Chamberlain D, Husain AN, Hruban RH, et al. Revision of the 1990 working formulation for the classification of pulmonary allograft rejection: lung rejection study group. J Heart Lung Transplant. 1996;15(1 Pt 1):1-15.
- 18. Pinsker KL, Veith FJ, Kamholz SL, Emeson EE, Norin A, Montefusco C. Bronchial anastomotic healing in canine lung allotransplants treated with cyclosporine. Transplantation. 1985;40(2):143-6.
- 19. Herve P, Silbert D, Cerrina J, Simonneau G, Dartevelle P. Impairment of bronchial mucociliary clearance in long-term survivors of heart/lung and double-lung transplantation: the Paris-Sud lung transplant group. Chest. 1993;103(1):59-63.
- 20. Veale D, Glasper PN, Gascoigne A, Dark JH, Gibson GJ, Corris PA. Ciliary beat frequency in transplanted lungs. Thorax. 1993;48(6):629-31.
Publication Dates
-
Publication in this collection
22 Jan 2008 -
Date of issue
Dec 2007
History
-
Accepted
18 July 2007 -
Reviewed
14 June 2007 -
Received
12 Apr 2007