Abstracts
OBJECTIVES: to determine the prevalence and key factors associated with fatigue in chronic low back pain patients. METHODS: cross-sectional study of 215 chronic low back pain patients from three health care centers and two industrial corporations. The crude prevalence of fatigue and its 95% confidence interval (CI) were calculated. Associations between fatigue and the independent variables were measured. RESULTS: the prevalence of fatigue among the participants was 26.0% [95% CI: 20.3 - 32.5]. Fatigue was independently associated with depression and self-efficacy. An increase of one unit in the score of depression increased the risk of fatigue by 9%; an increase of one unit in the score of self-efficacy reduced the risk of fatigue by 2%. CONCLUSIONS: fatigue was prevalent in chronic low back pain patients and associated with depression and self-efficacy. Knowing these factors can direct strategies for prevention and control of fatigue in chronic low back pain patients.
Fatigue; Low Back Pain; Self Efficacy; Depression
OBJETIVOS: Determinar la prevalencia y factores asociados con la fatiga en pacientes con dolor lumbar crónico. MÉTODOS: Estudio transversal con 215 pacientes con dolor lumbar crónico en tres servicios de salud y dos industrias. La prevalencia de la fatiga y su intervalo de confianza (IC) se calcularon. Las asociaciones entre variables independientes y la fatiga se calcularon. RESULTADOS: La prevalencia de la fatiga en los pacientes con dolor lumbar crónico fue del 26% [20,3 a 32,5, IC 95%]. La fatiga se asocia con la depresión y la autoeficacia. El aumento de un punto en la puntuación de depresión aumentó un 9% el riesgo de fatiga y un aumento de un punto en la auto-eficacia reduce el riesgo de la fatiga en el 2%. CONCLUSIONES: La fatiga es frecuente en pacientes con dolor lumbar crónico y se asocia con la depresión y la autoeficacia. Conocer estos factores puede dirigir las estrategias de prevención y control de la fatiga en pacientes con dolor lumbar crónico.
Fatiga; Dolor de La Región Lumbar; Autoeficacia; Depresión
OBJETIVOS: determinar a prevalência e os principais fatores relacionados à fadiga em pacientes com dor lombar crônica. MÉTODOS: trata-se de estudo transversal, com a participação de 215 pacientes com dor lombar crônica, em três centros de saúde e duas indústrias. Foram calculadas a prevalência bruta de fadiga e seu intervalo de confiabilidade de 95% (IC). RESULTADOS: a prevalência de fadiga entre os participantes com dor lombar crônica foi de 26% [20,3-32,5; IC 95%]. A fadiga foi associada à depressão e à autoeficácia de forma independente. O aumento de um ponto no escore de depressão aumentou o risco de fadiga em 9% e o aumento de um ponto no escore de autoeficácia reduziu o risco de fadiga em 2%. CONCLUSÕES: fadiga foi um fator predominante em pacientes com dor lombar crônica e indicou relação com depressão e autoeficácia. O conhecimento desses fatores pode orientar estratégias para prevenção e controle da fadiga em pacientes com dor lombar crônica.
Fadiga; Dor Lombar; Auto-Eficacia; Depressão
ORIGINAL ARTICLE
Prevalence of fatigue and associated factors in chronic low back pain patients1 1 Paper extracted from Doctoral Dissertation "Incapacidade em pessoas com dor lombar cronica: prevalência e fatores preditores", presented to Escola de Enfermagem, Universidade de São Paulo, Brazil. This research was supported by Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) and Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Brazil. Process # 471457/2010-8
Prevalencia y factores asociados con la fatiga en pacientes con dolor lumbar crónico
Marina de Góes SalvettiI; Cibele Andrucioli de Mattos PimentaII; Patrícia Emília BragaIII; Michael McGillionIV
IProfessor, Departamento de Enfermagem, Faculdade de Ciências Medicas da Universidade Estadual de Campinas, Brazil
IIFull Professor, Escola de Enfermagem, Universidade de São Paulo, Brazil
IIIMathematician, Professor, Centro Universitário São Camilo, Brazil
IVRN, Assistant Professor, Bloomberg Faculty of Nursing, University of Toronto, Canada
Corresponding Author Corresponding Author: Marina de Góes Salvetti Rua D. Pedro II, 20, Apto. 12 Vila Marques CEP: 18130-535, São Roque, SP, Brasil E-mail: mgsalvetti@usp.br
ABSTRACT
OBJECTIVES: to determine the prevalence and key factors associated with fatigue in chronic low back pain patients.
METHODS: cross-sectional study of 215 chronic low back pain patients from three health care centers and two industrial corporations. The crude prevalence of fatigue and its 95% confidence interval (CI) were calculated. Associations between fatigue and the independent variables were measured.
RESULTS: the prevalence of fatigue among the participants was 26.0% [95% CI: 20.3 - 32.5]. Fatigue was independently associated with depression and self-efficacy. An increase of one unit in the score of depression increased the risk of fatigue by 9%; an increase of one unit in the score of self-efficacy reduced the risk of fatigue by 2%.
CONCLUSIONS: fatigue was prevalent in chronic low back pain patients and associated with depression and self-efficacy. Knowing these factors can direct strategies for prevention and control of fatigue in chronic low back pain patients.
Descriptors: Fatigue; Low Back Pain; Self Efficacy; Depression.
RESUMEN
OBJETIVOS: Determinar la prevalencia y factores asociados con la fatiga en pacientes con dolor lumbar crónico.
MÉTODOS: Estudio transversal con 215 pacientes con dolor lumbar crónico en tres servicios de salud y dos industrias. La prevalencia de la fatiga y su intervalo de confianza (IC) se calcularon. Las asociaciones entre variables independientes y la fatiga se calcularon.
RESULTADOS: La prevalencia de la fatiga en los pacientes con dolor lumbar crónico fue del 26% [20,3 a 32,5, IC 95%]. La fatiga se asocia con la depresión y la autoeficacia. El aumento de un punto en la puntuación de depresión aumentó un 9% el riesgo de fatiga y un aumento de un punto en la auto-eficacia reduce el riesgo de la fatiga en el 2%.
CONCLUSIONES: La fatiga es frecuente en pacientes con dolor lumbar crónico y se asocia con la depresión y la autoeficacia. Conocer estos factores puede dirigir las estrategias de prevención y control de la fatiga en pacientes con dolor lumbar crónico.
Descriptores: Fatiga; Dolor de La Región Lumbar; Autoeficacia; Depresión.
Introduction
Low Back Pain (LBP) is a health crisis in developed and developing countries. Current estimates of its prevalence in the general adult population across countries range from 10.2% to 16.3%(1-2). LBP has a major negative impact on individuals' health-related quality of life, including poor general health, psychological distress, sleep disturbances, disability and fatigue(3). Fatigue limits functionality and can lead to social and psychological impairments(4). Fatigue is a symptom that can be particularly problematic for LBP patients, as it negatively affects physical and mental health perception, can complicate and disrupt recovery and delays optimal return to daily life and work(5-6).
Fatigue is defined as a persistent tiredness that is not alleviated by rest(5). The etiopathogenesis of this symptom is not well known but recent neuroimaging studies have raised some hypotheses that relate the involvement of the central nervous system with the presence of this symptom. The findings of these studies are not conclusive but suggest some abnormalities related to cerebral hypoperfusion and inflammatory processes that could explain the fatigue(7).
Although fatigue is a common problem across pain populations, little is known about the factors associated with fatigue in chronic low back pain patients(8). A study of fatigue among patients with recurrent low back pain found that fatigue was associated with anxiety, tension, episodes of pain, and lower levels of vigor(9). Considering that fatigue limits functionality and could hamper the involvement of low back pain patients in rehabilitation and pain management strategies, this study aimed to determine the prevalence of fatigue and key factors associated with fatigue in chronic LBP patients. Knowing these factors can direct strategies to prevent and control fatigue in chronic low back pain patients.
Methods
This study was a cross-sectional survey of 215 chronic LBP patients, conducted at three health care centers and two industrial corporations in Sao Paulo State, Brazil, over a period of 10 months, between January and November 2008. The decision to include patients from health services and industry was made to explore fatigue in employed and not employed individuals, so as to include different levels of fatigue and increase the external validity of the data.
During the data collection period, potential participants were assessed for inclusion across the study sites (health care centers and industrial corporations). The inclusion criteria were: a) chronic LBP (six months or longer); b) ages between 18 and 65 years; c) at least six years of formal education, and d) preserved communication. The exclusion criteria were: a) cancer, b) acute medical conditions, or c) a major cognitive disorder that would preclude informed consent. Of the potential participants, 368 met the inclusion criteria and 215 agreed to enroll in the study, with an acceptance rate of 58.4%. One hundred and fifty three (n=153) eligible individuals declined; they provided various reasons for their refusal to participate, including: they were too busy (85.0%), experienced physical discomfort related to pain (4.0%), and other reasons (11.0%). There were no significant differences between those who agreed to participate in the study and those who declined in relation to sex (p=0.753), age (p=0.473), education (p=0.056) and pain duration (p=0.056).
The principal investigator assessed participant eligibility and informed consent was obtained before participants enrolled in the study. Once enrolled, participants completed the study questionnaires in a private room. The study received ethical approval from the Research Ethics Committee, School of Nursing, University of Sao Paulo and the Health Services (no 684/2007/CEP-EEUSP).
In this study, the dependent variable was fatigue and the independent variables were sex, age, education, income, occupation, pain duration, pain intensity, body mass index, disability, depression, self-efficacy, and pain-related fear.
Fatigue was measured using the Brazilian version of the revised-Piper Fatigue Scale (rPFS), a multidimensional self-report instrument designed to measure fatigue that showed very good internal consistency and reliability for the total scale and dimensions, with alpha coefficients ranging from 0.84 to 0.94(10-11).
The rPFS it is composed of 22 items, ranging from 0 to 10, and assesses the presence of fatigue across four dimensions: behavioral/severity, affective meaning, sensory, and cognitive/mood. In this study the cutoff point adopted was 4.5, based on the 25th percentile of the study sample. Considering that mild fatigue (< 4.5) could have minimal clinical impact, those who scored 4.5 or higher were considered fatigued and those who reported no fatigue or scored < 4.5 were considered no fatigue.
Socio-demographic information and chronic LBP characteristics were obtained via a questionnaire developed for this study. The questionnaire included questions about the participants' age, sex, education, marital status, work situation, self-reported height and weight, LBP location, and pain duration. Additional measures were employed to obtain data on participants' pain intensity, disability, self-efficacy, pain-related fear and depression.
Pain Intensity
An 11-point Numerical Rating Scale (NRS) was employed to assess pain intensity. The NRS involves asking patients to rate their pain from 0 - 10, with endpoint anchors labeled "no pain" and "worst possible pain". The NRS is easy to administer and has been widely used in pain research. The validity of NRS has been well-documented and studies demonstrate positive and significant correlations with other measures of pain intensity(12).
Disability
Disability was assessed using the Oswestry Disability Index (ODI), an effective method for measuring disability among low back pain patients. This index includes 10 six-point scales. The first section rates the intensity of pain, and the others cover the disabling effect of pain on typical daily activities. The total ODI score ranges from 0 (no disability) to 100 (maximum disability). The ODI was validated in Brazil and showed good internal consistency (alpha=0.87) and test-retest reliability (r=0.99)(13).
Self-efficacy
Self-efficacy was assessed using the Chronic Pain Self-efficacy Scale (CPSS). The CPSS is composed of 22 items across three dimensions: Self-efficacy for Pain Management (PSE), Self-efficacy for Physical Function (FSE) and Self-efficacy for Coping with Symptoms (CSE). Each belief is assessed via a Likert scale, ranging from 10 to 100, which reflects respondents' level of confidence according to each item. The sum of the three dimensions provides the total score, ranging from 30 to 300. The psychometric properties of the Brazilian version showed very good internal consistency and reliability, with reliability coefficients ranging from 0.76 to 0.92 across the three dimensions, and 0.94 for the total scale(14).
Pain-related fear
The Tampa Scale for Kinesiophobia (TSK) was employed to assess pain-related fear (kinesiophobia), which is defined as irrational fear of physical movement resulting from a feeling of vulnerability to painful injury or reinjury(15). This scale requires respondents to rate 17 items on a 4-point Likert scale, with scores ranging from strongly disagree (0) to strongly agree. Total scores range from 17 to 68, with higher scores reflecting greater pain-related fear. The Brazilian version showed strong psychometric properties; Rasch analysis indicated excellent reliability, with a reliability coefficient of 0.95 on the items(16).
Depression
The Beck Depression Inventory (BDI) is a 21-item self-report instrument that has been employed to assess depressive symptoms. Each item is rated on a 4-point scale (0-3) with total scores ranging from 0 63. The Brazilian version was validated and the cutoff points adopted for populations without previous depression diagnoses are: scores higher than 15 to indicate mild depression, and 21 or higher to indicate depression(17). The psychometric properties of the BDI confirm the construct validity of the Brazilian version with good internal consistency (Cronbach's alpha = 0.81)(17).
Data Analysis
The data were entered into a database using the SPSS-version 13, statistical program and were analyzed using STATA 9.0 (StataCorp LP, College Station, Texas, USA). The prevalence rate of fatigue among patients reporting CLBP and its 95% confidence interval (95% CI) were determined. In the univariate analysis, associations between fatigue and the independent variables were measured using Pearson´s chi-square test for categorical variables and the Mann-Whitney test for continuing variables, at an alpha level of 0.05. Relevant variables (p<0.25 in univariate analysis) were then selected for multivariate analysis in a logistic regression model, in a stepwise forward procedure.
Variables independently associated with the outcome and confounding factors were kept in the final regression model, considering plausibility and maximum likelihood estimates during the modeling process. Adjusted Odds Ratios (ORs) by sex in multivariate analysis and their 95% CIs were calculated.
Results
This study comprised 215 participants between the ages of 19 and 65 years (mean=44.7; SD=11.1); most participants were female (65.1%) and the average education was 11.2 years (SD=3.5). The majority of participants reported living with a partner (66.4%) and 44.1% were employed in a full-time job, and most gained a low monthly family income. Most reported their pain intensity as moderate to severe (87%) and, for 45.6%, the presence of LPB has lasted 6 years or more. Overall, 56 participants (26.0%) [95%CI: 20.3 - 32.5] presented Piper Fatigue scores > 4.5 and were therefore classified as fatigued. The mean fatigue score for these respondents was 7.1 (SD: 1.4), with an average duration of 44 months. The majority (95%) reported chronic fatigue (lasting more than 6 months).
Tables 1 and 2 outline the results of the univariate analysis of factors associated with fatigue in chronic LBP patients.
Sex, occupational status and place of enrollment were significantly associated with fatigue. Men showed a lower risk for fatigue than women (p=0.029); and sick listed participants had a higher risk of fatigue compared to participants who were employed (p<0.001). Moreover, participants interviewed in health care centers (private or public) were more fatigued than those enrolled at industrial corporations (p=0.019).
Fatigue in chronic LBP was also significantly associated with pain intensity, depression, disability, self-efficacy and pain-related fear. Participants with higher levels of pain intensity (p<0.001), higher depression scores (p<0.001), higher disability scores (p<0.001), lower self-efficacy scores (p<0.001), and higher levels of pain-related fear (p<0.001) showed higher risks to be fatigued than others.
In addition, sex was significantly associated with self-efficacy (p=0.006), disability (p<0.001), and depression (p=0.050). The majority of female participants presented low self-efficacy (75%), moderate to severe disability (77%) and had depressive symptoms (63%). Among men, 63% reported high self-efficacy, 49% reported minimum disability and 76% had no depressive symptoms. Based on this finding, we conducted a multivariate analysis controlled by sex.
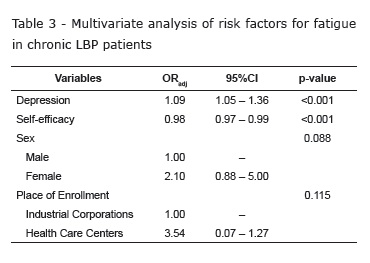
Table 3 presents the logistic regression model, identifying variables independently associated with fatigue in chronic LBP patients. After controlling for sex and place of enrollment, fatigue was shown to be independently associated with higher depression scores (p<0.001) and lower self-efficacy scores (p=0.004). It was noted that an increase of one unit in the score of depression increased the risk of fatigue by 9% and an increase of one unit in the self-efficacy score reduced the risk of fatigue by 2%.
Discussion
This study explored the prevalence of fatigue and its associated factors among chronic LBP patients. The findings reveal that fatigue is a significant problem in this group of patients. The prevalence of fatigue in this sample was slightly higher than the prevalence in the general population (18% - 22%)(18-19) and very similar to the prevalence of fatigue among nursing professionals (25.7%)(20). In addition, among the fatigued patients, most experienced chronic fatigue (95%) and their fatigue severity scores were higher than those observed in a study of cancer patients and healthy people(11).
Comparing the fatigued and non-fatigued group, the majority of non-fatigued individuals were employed, showed lower pain intensity, shorter pain duration, lower depression scores, lower disability level, lower pain-related fear and higher self-efficacy. These characteristics suggest that non-fatigued individuals seem to have more self-confidence and maintain activities like work, besides the presence of pain. On the other hand, fatigue is one of the characteristics of depression and it could increase the perception of disability and could be related to longer pain duration and severe pain.
The univariate analysis revealed that women experienced significantly more fatigue than men, in accordance with previous studies in the area(19,21-23). This finding may be the result of factors like the prevalence of depressive symptoms among women, female physical characteristics and gender-specific workloads.
Occupational status and disability have been the focus in a number of studies. In the present study, sick listed participants showed greater risk of fatigue than those who were employed; higher disability scores were also associated with fatigue in the univariate analysis. Similarly, in a study conducted in Norway, disabled people were more fatigued than subjects at work(21); and in a study on rheumathoid arthritis patients, disability was also a predictor of fatigue(23). Unfortunately, in the present study, it was not possible to determine whether or not the occupational status of sick-listed patients increased their fatigue. These associations were not supported in the final model.
The relationship between fatigue and pain demonstrated in this study supports the findings of previous research in this area. Pathophysiological processes of fatigue involve metabolic and structural lesions that disrupt the usual process of activations in pathways interconnecting the basal ganglia, thalamus, limbic system and higher cortical centre(24), which are all structures related to the physiology of pain. These similarities explain the close relationship between fatigue and pain observed in the literature, which was confirmed in this study.
In the univariate analysis, higher levels of pain intensity were associated with fatigue; however, this relationship did not appear in the multivariate analysis. An evidence-based review concluded that the etiology of fatigue was related to the presence of pain(8). Moreover, studies that explored fatigue in low back pain patients concluded that low back pain was a predictor of fatigue(9,21).
The research data in the present study showed no significant association between fatigue and age, which is consistent with some studies(18) but not with others(19); nor was there an association between fatigue and Body Mass Index (BMI). No association was found between education and fatigue, in contrast with studies that showed that low educational levels were associated with higher levels of fatigue(19). Family income and marital status were not associated with fatigue in the present study, consistent with another study(19).
The findings confirm the relationship between depression and other psychological factors and fatigue. Psychological morbidity and distress have been associated with fatigue in previous studies on the general and working population(18-19,22,25-26). A longitudinal study of chronic fatigue syndrome concluded that psychological factors, such as illness attitudes and coping styles, seem to be more important predictors of long term outcomes than immunological or demographic variables to fatigue(27).
In this investigation, depression was independently associated with fatigue. An increase of one unit in the score of depression increased the risk of fatigue to CLBP patients by 9%. Research has shown that depression is a predictor of fatigue among CLBP and neck pain patients(21) and in healthy women(26). Studies that used multiple regression analysis confirm the significance of depression in fatigue(21-22); however, the relationship between self-efficacy and fatigue has received little attention(28).
In this study, pain-related fear was associated with fatigue in the univariate analysis, but not in the logistic regression analysis. Taking into account that self-efficacy beliefs and fear-avoidance beliefs are interrelated, it is possible that self-efficacy represented fear-voidance beliefs in the final model. This study found that, in addition to depression, self-efficacy was independently associated with fatigue. An increase of one unit in the score of self-efficacy reduced the risk of fatigue among CLBP patients by 2%. In a study on the role of self-efficacy in fatigue among rheumatoid arthritis patients, a strong correlation was found between self-efficacy and fatigue(28), confirming these findings.
A study that explored the results of a multidisciplinary pain facility treatment, which included a multimodal treatment, massage therapy, educational groups and biofeedback, employed to control pain-associated fatigue, showed good results(29). Considering that depression and self-efficacy are associated with fatigue, multidisciplinary pain treatments designed to reduce depressive symptoms and improve self-efficacy could also be helpful to control pain-associated fatigue, but more studies must be developed to verify this hypothesis.
This study has limitations: the cross-sectional design of this study does not provide data on causal relationships that may occur, thus limiting the scope of the analysis and the findings. The use of a convenience sample hinders the ability to make generalizations based on the findings. Future studies could address these limitations, using a different study design that permits confirming this relationship in a linear manner.
Conclusion
This study explored the prevalence of fatigue among chronic low back pain patients and fatigue associated factors, including cognitive variables (such as self-efficacy and pain-related fear) that have yet to be studied in depth. The findings suggest a strong correlation between fatigue, depression and self-efficacy among the CLBP patients in this sample. Self-efficacy beliefs can be enhanced by self-management interventions and, as such, can be used to improve treatment outcomes in many chronic health situations. Self-efficacy may have implications for fatigue treatment as well. Interventions designed to reduce depression symptoms and improve self-efficacy beliefs may have a positive impact on fatigue among chronic LBP patients.
Received: July 19th 2012
Accepted: Oct. 10th 2012
- 1. Sa KN, Baptista AF, Matos MA, Lessa I. Chronic pain and gender in Salvador population, Brazil. Pain. 2008;139:498-506.
- 2. Freburger JK, Holmes GM, Agans RP, Jackman AM, Darter JD, Wallace AS, Castel LD, Kalsbeek WD, Carey TS. The rising prevalence of Chronic Low Back Pain. Arch Intern Med. 2009;169(3):251-8.
- 3. Kovacs, FM; Abraira, V; Zamora, J; Fernández, C. The transition from acute to subacute and chronic low back pain: A study based on determinants of quality of life and prediction of chronic disability. Spine. 2005;30(15):1786-92.
- 4. Fini A, Cruz DALM. Características da fadiga de pacientes com insuficiência cardíaca: revisão de literatura. Rev. Latino-Am. Enfermagem. 2009;17(4):557-65.
- 5. Mota DDCF, Cruz DALM, Pimenta CAM. Fadiga: uma análise do conceito. Acta Paulista de Enfermagem. 2005;18:285-93.
- 6. Oliveira JRS, Vigano MG, Lunardelli MCF, Caneo LC, Goulart Jr E. Fadiga no trabalho: como o psicólogo pode atuar. Psicol Estudo. 2010;15(3):633-8.
- 7. Ortega F, Zorzanelli R. Imagens cerebrais e o caso da síndrome da fadiga crônica. Ciência Saúde Coletiva. 2011;16(4):2123-32.
- 8. Fishbain DA, Cole B, Cutler RB, Lewis J, Rosomoff HL, Rosomoff RS. Is pain fatiguing? A structured evidence-based review. Pain Med. 2003;4(1):51-62.
- 9. Feuerstein M, Carter RL, Papciak AS. A prospective analysis of stress and fatigue in current low back pain. Pain. 1987;31:333-44.
- 10. Piper BF, Dibble SL, Dodd MJ, Weiss MC, Slaughter RE, Paul SM. The revised Piper Fatigue Scale; psychometric evaluation in women with breast cancer. Oncol Nurs Forum. 1998;25(4):677-84.
- 11. Mota DCF, Pimenta CAM, Piper BF. Fatigue in Brazilian cancer patients, caregivers and nursing students: a psychometric validation study of the Piper Fatigue Scale-Revised. Support Care Cancer. 2009;17:645-52.
- 12. Jensen MP, Karoly P. Self-Report Scales and procedures for Assessing Pain in Adults. In: Turk DC, Melzack R, editors. Handbook of Pain Assessment. 2nd ed. New York: Guilford Press; 2001. p. 19-44.
- 13. Vigatto R, Alexandre NMC, Filho HRC. Development of a Brazilian Portuguese Version of the Oswestry Disability Index: Cross-Cultural Adaptation, Reliability and Validity. Spine. 2007;32(4):481-6.
- 14. Salvetti MG, Pimenta CAM. Validação da "Chronic Pain Self-efficacy Scale" para a língua portuguesa. Rev Psiquiatr Clin. 2005;32(4):202-10.
- 15. Goubert L, Crombez G, Van Damme S, Vlaeyen JW, Bijttebier P, Roelofs J. Confirmatory factor analysis of the Tampa Scale for Kinesiophobia: Invariant two factor model across low back pain patients and fibromyalgia patients. Clin J Pain. 2004;20(2):103-10.
- 16. Siqueira FB, Teixeira-Salmela LF, Magalhães LC. Análise das propriedades psicométricas da versão brasileira da Escala Tampa de Cinesiofobia. Acta Ortopédica Bras. 2007;15(1):19-24.
- 17. Gorenstein C, Andrade L. Inventário de depressão de Beck: propriedades psicométricas da versão em português. Rev Psiquiatr Clín. 1998;25(5):245-50.
- 18. Pawlikowska T, Chalder T, Hirsch SR, Wallace P, Wright DJM, Wessely SC. Population based study of fatigue and psychological distress. BMJ. 1994;308:763-6.
- 19. Loge JH, Ekeberg O, Kaasa S. Fatigue in the general Norwegian population: normative data and associations. J Psychosom Res. 1998;45(1):53-65.
- 20. Vasconcelos SP, Fischer FM, Reis AOA, Moreno CRC. Fatores associados à capacidade para o trabalho e percepção de fadiga em trabalhadores de enfermagem da Amazônia Ocidental. Rev Bras Epidemiol. 2011;14(4):688-97.
- 21. Fishbain DA, Cutler RB, Cole B, Lewis J, Smets E, Rosomoff HL, Rosomoff RS. Are patients with chronic low back pain or chronic neck pain fatigued? Pain Med. 2004;5(2):187-95.
- 22. Hardy GE, Shapiro DA, Borril CS. Fatigue in the workforce of national health service trusts: levels of symptomatology and links with minor psychiatric disorder, demographic, occupational and work role factors. J Psychosom Res. 1997;43(1):83-92.
- 23. Repping-Wuts H, Fransen J, van Achterberg T, Bleijenberg G, van Riel P. Persistent severe fatigue in patients with rheumatoid arthritis. J Clin Nurs. 2007;16(11):377-83.
- 24. Chaudhuri A, Behan PO. Fatigue in neurological disorders. Lancet. 2004;363:978-88.
- 25. Mininel VA, Baptista PCP, Felli VEA. Psychic workloads and strain processes in nursing workers in brazilian university hospitals. Rev. Latino-Am. Enfermagem. 2011;19(2):340-7.
- 26. Libbus K, Baker JL, Osgood JM, Philips TC, Valentine DM. Persistent fatigue in well women. Women and Health. 1995;23(1):57-72.
- 27. Wilson A, Hickie I, Lloyd A, Hadzi-Pavlovic, Boughton C, Dwyer, Wakefield D. Longitudinal study of outcome of chronic fatigue syndrome. BMJ. 1994;308:756-9.
- 28. Riemsma RP, Rasker JJ, Taal E, Griep EN, Wouters JMGW, Wiegman O. Fatigue in rheumatoid arthritis: the role of self-efficacy and problematic social support. Br J Rheumatol. 1998;37:1042-6.
- 29. Fishbain DA, Lewis J, Cole B, Cutler B, Smets E, Rosomoff H, Rosomoff RS. Multidisciplinary pain facility treatment outcome for pain-associated fatigue. Pain Med. 2005;6(4):299-304.
Corresponding Author:
Publication Dates
-
Publication in this collection
01 Mar 2013 -
Date of issue
Feb 2013
History
-
Received
19 July 2012 -
Accepted
10 Oct 2012